Total Hip Replacement
|
|
|
- Coral Page
- 8 years ago
- Views:
Transcription
1 Total Hip Replacement INTRODUCTION T he following information is a guide to your upcoming surgery. It describes what is likely to happen at the time of surgery. This is a guide only and there may be some individual variations, depending on your individual circumstances and Dr Lawrie will discuss these with you. Please become familiar with this guide and discuss any aspects that you wish to with Dr Lawrie, the anaesthetist and/or the nursing staff. You will be admitted to the ward either the morning of surgery or the night before, depending on the time of day of your surgery. A typical hospital stay is 5-7 days. You will need to travel home in an ambulance on the day of your discharge to protect your new hip joint. BEFORE SURGERY Y ou should stop taking anti-inflammatory drugs at least five days prior to surgery as they can increase the chance of bleeding (e.g. Voltaren, Naprosyn, Nurofen, Brufen, Feldene, Naprosyn and Indocid. Celebrex, Vioxx and Mobic are not a problem). It is extremely important that you have no cuts, scratches or sores on your lower limb at the time of your surgery as this can increase the chances of infection. If you do have any cuts, scratches or sores then your surgery will be postponed until these are well and truly healed. On the day of your surgery a nurse will inspect your leg for any lesions. The nurse will then use clippers to remove any long hair from the hip and dress the hip with an antiseptic solution. Dr Lawrie will also inspect the leg and mark the appropriate leg to be operated on with an indelible marking pen. You should stop smoking prior to your surgery as smoking increases the risks associated with an anaesthetic and the risk of blood clots (DVT) following surgery
2 ADMISSION Y ou should not eat or drink 6 hours prior to surgery. You should bring with you: Personal effects (nightgown or pyjamas, slippers, dressing gown, toiletries) Any medication you are taking All relevant x-rays, scans and reports Medicare and private health fund membership cards This paperwork Prior to going to the operating room, the ward staff will direct you to Have a shower with an antiseptic soap Be dressed in a theatre gown and disposable underwear Have the limb inspected and dressed with an antiseptic solution and sterile drape If you wish Dr Lawrie to speak to a family member after the operation please notify the nursing staff with contact details. THE PROCEDURE Y ou will be taken into the operating room on a trolley by the nursing staff The operation will take about minutes, but you may spend up to two and a half to three hours in the theatre complex by the time you wait in the pre-operative area, are prepared from your anaesthetic and then woken up in the recovery area. THE ANAESTHETIC Y ou will meet the anaesthetist prior to your admission when he will discuss with you the different anaesthetic options. The type of anaesthetic you have will be tailored to your needs, taking into account any medical condition that you may have. You may be given a general anaesthetic (where you are completely asleep) or a regional anaesthetic such as an epidural or spinal anaesthetic where the nerves to the limb are numbed from a needle placed in your back.
3 THE SURGERY You will be placed on the operating table lying on your side. Your position on the operating table will be held by a number of bolsters to maintain your position. You will be covered in sterile drapes so that only the operation site is exposed. Dr Lawrie will check your x-rays and use those to ensure that your new hip is placed in exactly the right position and at the right angle for your hip. Any deformities due to your hip condition can often be corrected by your new hip. An incision will be made over the hip joint which will best address the pathology in your hip. The typical incision is about 10cm long, but it may be greater if more access is needed due to individual circumstances. Great care is taken to ensure that the major nerves and vessels about the hip joint are protected. The soft tissue envelope about the hip is carefully retracted exposing the capsule of the hip joint. The capsule is then entered; exposing the hip joint itself and an instrument is used at this point to mark your leg lengths so that, at the end of the procedure, we can be sure the leg lengths are satisfactory. The hip joint is then dislocated and the ball at the end of the femur is removed. The socket is then assessed and the position of the new socket is determined by consulting the x-rays. The socket is reshaped with a special tool on the end of a drill which prepares the socket to a hemispherical shape. Any large bone spurs are removed and any bone cysts seen on your x-ray are plugged with bone from the ball of the femur. A dummy socket is placed to make sure the position is correct. The femur is then prepared to accept the femoral component. A hole down the centre of the shaft of the femur is prepared which mirrors the shape of the femoral component. A dummy femoral component is then placed into the hole and a ball is placed on the end of it. The dummy hip is then reduced or brought together and the final position of the components is then decided upon. This takes into account the stability of the hip joint (of most importance) the range of motion and the leg lengths. Occasionally the leg lengths of the components and subsequently the patient s legs need to be adjusted so as to maintain the stability of the joint and not allow the joint to dislocate. This is a very important concept and one that Dr Lawrie will spend some time explaining to you. Once we are happy with the position of the dummy components, the real components will be put into place. Both the socket and the femoral stem can then be put in place, with or without cement.
4 The decision as to which method of fixation to use will depend upon the size, shape and quality of the bone in your hip and the type of pathology in your hip (e.g. osteoarthritis vs. rheumatoid arthritis vs. fracture). Dr Lawrie will discuss this with you prior to your surgery. If bone cement is to be used, its role is to act as a grout to get into all the small spaces within the bone itself. It is not an adhesive and it does not glue the components to the bone. It acts to transmit forces from the components to the bone and load the bone evenly. If cement is not used then the components themselves are fixed to the bone via the surface texture which encourages bone to grow onto the component. These components are typically made of titanium which encourages bone growth. The components are initially stable due to the precise nature of how the bone is prepared to fit the components; they get a mechanical interlock initially. Over time the bone grows onto the implant to give a biological stability. The ball and lining of the socket will then be secured. There are a number of different ball/liner combinations that can be used (this is called the bearing surface). Traditionally a metal ball on a hard plastic liner has been used. This works extremely well in the majority of cases, however in the situation of high loading it may wear more quickly than we would hope and it can lead to early failure of the joint. Therefore, a number of alternative bearings have been developed. These include all metal bearing surfaces, ceramic bearing surfaces, new cross-linked plastic bearings and a new ceramic metal called Oxinium. Each have unique characteristics and are useful in certain situations. Dr Lawrie will discuss with you what bearing surface is appropriate for your situation. Once the ball and socket are secured, the capsule can be repaired in such a way that will help with stability of the joint. The different muscle layers are then repaired and the skin is closed with staples; occasionally a drain will be placed in the muscle layers and a sterile dressing is then applied. You are rolled onto your back and the anaesthetic will be withdrawn by your anaesthetist. A catheter will be placed into your bladder at the end of the operation to prevent any problems with the bladder post-operatively. THE RECOVERY Y ou will then be wheeled into recovery and the nurse will monitor your blood pressure, pulse and breathing as you recover from your anaesthetic. A triangular pillow will be placed between your legs so as to control the position of your hip as the anaesthetic wears off. The nurse will check on the sensation and circulation of your limbs.
5 AFTER SURGERY D r Lawrie will see you and explain the operative findings to you. A copy of the operative report will be sent to your local doctor. On returning to the ward you will have a drip placed into your arm; this will keep you well hydrated until you are eating and drinking normally. Your blood level will be checked and you may need a blood transfusion. You will have tight stockings around both legs which will help to prevent blood clots; these need to be worn for six weeks following your surgery. Your usual medications will be given to you. You will be placed on antibiotics through the drip for 24hrs to reduce the risk of infection. Aspirin will be added to your medications and you should continue to take this for six weeks from the time of surgery to help prevent clots. The triangular pillow will be put between your legs while you are in bed to prevent your hip from being put into a position that may dislocate the hip. You will be given morphine type medication for pain relief, which may make you drowsy and nauseated. Your anaesthetist will keep a close eye on your pain relief and will endeavour to keep you comfortable. Commonly patients will be given a PCA (Patient Controlled Analgesia) which allows you to control the amount of pain killer that is administered through your drip. An x-ray of your hip will be taken following your surgery to check on the position of your components. Your blood levels will be checked the following day. A physiotherapist will be in charge of your mobility and will visit you following your surgery The most important thing you can do after returning to the ward is to get moving as soon as possible. This will help to prevent clots and to maximise your new hip s flexibility and minimise muscle weakness post surgery. You should start with toe wiggling immediately after surgery and progress to sitting out of bed the day after surgery; then walking with the aid of a frame a day or two following your surgery. You will be given a number of hip exercises by the physiotherapist, which will aid in getting back your muscle strength and getting you back on your feet. You will be ready to leave when you can walk about 30 metres on your own, get in and out of bed, access the toilet and shower, and get up and down stairs successfully.
6 T WHEN YOU GET HOME he risk of dislocation of your new hip joint is highest in the first three months following surgery. Your new hip will feel very good when you are discharged. Often a patient is not aware of their new hip as the pain relief is so good following hip replacement surgery. However, it is very important that you are aware of the risks to your hip and that you follow your hip precautions as described by the physiotherapist. FOR THE FIRST THRRE MONTHS DON T FLEX YOUR HIP GREATER THAN 90 DON T PIVOT OR TWIST ON THE OPERATED LEG DON T SIT FOR LONG PERIODS OF TIME DON T SIT ON CHAIRS WITHOUT ARMS DON T SIT ON OVERSTUFFED FURNITURE DON T CROSS YOUR KNEES OR ANKLES DON T TURN YOUR KNEES TOGETHER DON T SLEEP ON YOUR SIDE DON T BEND TO PICK ANYTHING UP DON T LIE WITHOUT A PILLOW BETWEEN YOUR LEGS DON T SIT IN THE BATH Once you have your new hip replacement it is up to you to take care of it. Although the new hip replacement may feel much like a normal hip, it is not. It is much like the bearings in a car and it can wear out if too much force is applied to it. Avoiding excessive and undue stresses on the new hip will give it the best chance of having a long life. You will have to avoid sports involving running or jumping. However, it is important to stay as healthy as possible. Activities such as walking, swimming, golf, lawn bowls and social tennis (preferably doubles) are all encouraged. It is very important to treat any infections of other areas aggressively such as the urinary tract or dental infections. Many invasive procedures require antibiotics prior to the procedure. It is always best to warn your doctor beforehand that you have a hip replacement as the consequences of an infected hip replacement can be dire. Surgery on
7 infected hip replacements is extremely difficult and is not always successful at eradicating the infection. One can be left without a hip joint with a painful hip and the leg may be shorter as a result. There is about a 1% chance per year that you will require a revision hip replacement. A hip revision is much more difficult, they tend to have more complications and they have a less successful outcome than the original surgery. This is why it is so important to look after your new hip forever more. By looking after your hip, you will be able to substantially improve the longevity of your it and hopefully avoid the need for a hip revision in the future. COMMONLY ASKED QUESTIONS What are the risks of surgery? The risks of Hip Replacement Surgery can be thought of as general risks of the procedure and local risks to the hip and leg General Risks Death is possible from the procedure There is the risk of having a problem with the heart such as a heart attack, heart failure or arrhythmia There is the risk of having a stroke o These events are very rare Clots in the legs may occur with pain and swelling of the legs; rarely parts of the clots can break off and travel to the lungs and this can be fatal. Many steps are taken to avoid this from happening. Small areas of the lungs can collapse following surgery which may cause infection in the lungs requiring antibiotics and physiotherapy. Bladder and prostate problems can be exacerbated by your surgery, but a catheter is routinely placed in your bladder at the time of surgery to avoid this. This will be removed once you are comfortable and mobile. The bowel may become paralysed after surgery. This may result in pain, bloating, nausea and vomiting for a short time. Local Risks Infection after hip replacement can occur at any time. Therefore it is very important to be vigilant to the risk of infection. Infection may result in revision of your hip replacement, or you may even be left without a hip; which can often result in a painful and short limb. Sometimes the infection cannot be eradicated, even with further surgery.
8 The hip can dislocate and it is most at risk in the first three months after surgery, but there is also a lifelong risk. If the hip dislocates it can often be put back in without surgery. Sometimes a brace will need to be worn for a period of time. If the hip continues to dislocate than surgery may become necessary. Surgery for dislocation is extremely difficult with a relatively low success rate. Once again, this shows how important it is to look after your hip replacement. The leg length may be different to the opposite side and this may require treatment. Typically a shoe build up is needed, but sometimes further surgery is required. There are many reasons why the leg lengths may be different following surgery. The goal of the operation is to give a pain-free, mobile hip that does not dislocate, and on occasion the leg lengths may need to be altered to achieve this. When the joint is arthritic, cartilage and bone can be lost from the joint; this shortens the leg. When the new hip is put in place, an attempt is made to restore this bone and cartilage loss, therefore the hip is often longer. There may be arthritis of the other hip, which is now shorter due to the same process, and once a new hip is in place this leg will be longer. If the hip was very short pre-operatively it can be too dangerous to lengthen the hip to any great degree, so the leg will still be short following surgery. The operated hip often feels long initially, even if it is not. In an arthritic hip the soft tissues about the hip joint are scarred and contracted due to the loss of bone and cartilage and with the inflammation about the joint. When the new hip is in place these tissues are initially stretched out of there contracted state and this can feel to you as if the leg is now longer, even if it is not. The nerves about the hip joint can be injured at the time of surgery; this can result in pain or weakness or permanent disability. The most common nerve affected is the nerve which supplies the muscles to the top of the foot; damage here can result in foot drop. The new hip joint itself may loosen and/or wear over time. This can result in pain and instability over time. The socket, the liner, the head or the stem may fail individually or in combination, which may require revision surgery in the future. Sometimes it can result in bone loss about the hip joint. This can result in fracture of the socket or thigh bone in future years; but a number of steps are taken to reduce the risks of this. Individual circumstances will dictate what type of hip replacement is used so as to get the best result for you. There is a risk that the new hip may fail within the first five years. This will require further surgery Occasionally the bone of the socket or femur may break at the time of surgery. This is often recognised at the time and can be corrected during the hip replacement. This may mean that you are not able to walk on the hip for a period of time following the
9 surgery. Rarely you may need further surgery to treat the fracture. The wound may not heal properly and can become red, thickened and painful; steps are taken to avoid this. Possible bleeding into the wound after surgery can occur. This may become painful and require surgical drainage, or it may become infected and require antibiotics. There is a risk that the leg may have to be amputated due to poor blood supply or infection. There is an increased risk of complications in obese people of wound infection, heart and lung complications and blood clots. There is an increased risk of complications with patients who have diabetes. There is an increased risk of complications with smokers. There is an increased risk of complications for patients with multiple medical problems. There is an increased risk of complications in the very elderly and infirm. Will my surgery be successful? Hip Replacement surgery is extremely successful; with a very high chance it will substantially improve or completely relieve your pain. There is about a 1% chance per year that you will require a revision hip replacement. Hip revisions are much more difficult, tend to have more complications and will have a less successful outcome than the original surgery. That is why it is so important to look after your new hip forever more. When can I drive? You may drive when you are walking without crutches, when you have good quadriceps function and when you no longer require pain killers which may cause drowsiness. This will be approximately six weeks to three months after your surgery.
10
11
12
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Procedure Information Guide
 Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Total Hip Arthroplasty (Hip Replacement) PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
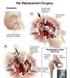 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9336 Facility: Total Hip
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9336 Facility: Total Hip
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
HIP JOINT REPLACEMENT
 HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
This information is for patients who are considering having a hip replacement.
 Directorate of Surgical Care Department of Orthopaedics Hip Replacement: Information for Patients and Carers This information is for patients who are considering having a hip replacement. What is a hip
Directorate of Surgical Care Department of Orthopaedics Hip Replacement: Information for Patients and Carers This information is for patients who are considering having a hip replacement. What is a hip
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Total Knee Replacement
 Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Total Knee Arthroplasty (Knee Replacement) PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9337 Total Knee Arthroplasty
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9337 Total Knee Arthroplasty
A Guide. To Revision Total Knee Replacement. Patient Information Leaflet
 A Guide This leaflet is available in large print, Braille and on tape. Please contact Geoff Pennock on 0151 604 7289. To Revision Total Knee Replacement Wirral University Teaching Hospital NHS Foundation
A Guide This leaflet is available in large print, Braille and on tape. Please contact Geoff Pennock on 0151 604 7289. To Revision Total Knee Replacement Wirral University Teaching Hospital NHS Foundation
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Knee Replacement: Information for Patients and Carers
 Directorate of Surgical Care Department of Orthopaedics Knee Replacement: Information for Patients and Carers This information is for patients who are considering having a knee replacement. What is a Knee
Directorate of Surgical Care Department of Orthopaedics Knee Replacement: Information for Patients and Carers This information is for patients who are considering having a knee replacement. What is a Knee
Total knee replacement Uni-compartmental knee replacement
 Your Knee Replacement at the Nuffield Orthopaedic Centre A patient s guide to: Total knee replacement Uni-compartmental knee replacement Welcome to Team Two at the NOC. Together you and your surgeon have
Your Knee Replacement at the Nuffield Orthopaedic Centre A patient s guide to: Total knee replacement Uni-compartmental knee replacement Welcome to Team Two at the NOC. Together you and your surgeon have
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
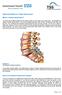 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
Patient Labeling Information System Description
 Patient Labeling Information System Description The Trident Ceramic Acetabular System is an artificial hip replacement device that features a new, state-of-the-art ceramic-on-ceramic bearing couple. The
Patient Labeling Information System Description The Trident Ceramic Acetabular System is an artificial hip replacement device that features a new, state-of-the-art ceramic-on-ceramic bearing couple. The
Delivering Excellence. Nuffield Orthopaedic Centre NHS Trust. Information for Patients. Hip and Knee service. Total Knee Replacement NHS
 www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
Ankle Stabilisation Procedure
 Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Recovering from a broken hip
 Recovering from a broken hip Information for patients, relatives and carers Who will will look look after after me me during during my hospital my hospital stay? stay? A multidisciplinary team of healthcare
Recovering from a broken hip Information for patients, relatives and carers Who will will look look after after me me during during my hospital my hospital stay? stay? A multidisciplinary team of healthcare
Arthroscopic Ankle Fusion (Arthrodesis)
 Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
PATIENTS GUIDE TO SPINAL SURGERY
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY PATIENTS GUIDE TO SPINAL SURGERY The Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY PATIENTS GUIDE TO SPINAL SURGERY The Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Hernia- Open Inguinal Hernia Repair PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
 DO NOT WRITE IN THIS BINDING MARGIN v5.00-04/2011 SW9317 Hernia- Open Inguinal Hernia Repair Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
DO NOT WRITE IN THIS BINDING MARGIN v5.00-04/2011 SW9317 Hernia- Open Inguinal Hernia Repair Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
PALM BEACH ORTHOPAEDIC INSTITUTE, P.A. FAQ: OUT-PATIENT SURGERY
 DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
Introduction. Welcome to the Orthopaedic Outpatients Department at the Hartshill Orthopaedic and Surgical Unit.
 Patient information Total Knee Replacement Introduction This booklet is designed to provide information about total knee replacement and what to expect before and after this operation. It has been compiled
Patient information Total Knee Replacement Introduction This booklet is designed to provide information about total knee replacement and what to expect before and after this operation. It has been compiled
Ganz (PAO) Operation for hip dysplasia Patient Information
 Ganz (PAO) Operation for hip dysplasia Patient Information FOCUSED PATIENT CARE Welcome to the private hospital Mølholm This brochure informs you of the pre- and post-operative procedures of your hip dysplasia
Ganz (PAO) Operation for hip dysplasia Patient Information FOCUSED PATIENT CARE Welcome to the private hospital Mølholm This brochure informs you of the pre- and post-operative procedures of your hip dysplasia
Patient information for cervical spinal fusion.
 Patient information for cervical spinal fusion. Introduction This booklet has been compiled to help you understand spinal cervical fusion surgery and postoperative rehabilitation. Anatomy The cervical
Patient information for cervical spinal fusion. Introduction This booklet has been compiled to help you understand spinal cervical fusion surgery and postoperative rehabilitation. Anatomy The cervical
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
TOTAL HIP JOINT REPLACEMENT
 TOTAL HIP JOINT REPLACEMENT Journey through your new HIP JOINT CONTENTS... 1 What is a Total Hip Joint Replacement (THJR)? 2 What you can do to prepare for surgery? 3 The operation and your stay in hospital
TOTAL HIP JOINT REPLACEMENT Journey through your new HIP JOINT CONTENTS... 1 What is a Total Hip Joint Replacement (THJR)? 2 What you can do to prepare for surgery? 3 The operation and your stay in hospital
Understanding Total Hip Replacement
 Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Surgery for hip fracture: Hemi-arthroplasty
 Surgery for hip fracture: Hemi-arthroplasty This leaflet aims to answer your questions about having surgery for a hip fracture. It explains the benefits, risks and alternatives, as well as what you can
Surgery for hip fracture: Hemi-arthroplasty This leaflet aims to answer your questions about having surgery for a hip fracture. It explains the benefits, risks and alternatives, as well as what you can
Arthroscopic subacromial decompression and rotator cuff repair
 Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Further sources of information http://www.patient.co.uk/showdoc/553/ http://www.shoulderdoc.co.uk/article.asp?section=11 http://www.medic8.com/healthguide/articles/painfulshoulder.html http://www.cks.nhs.uk/patientinformationleaflet/shoulderpainarc/st
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Should I have a knee replacement?
 Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Elbow Joint Replacement A guide for patients
 Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Arthroscopic shoulder stabilisation. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Posterior Lumbar Decompression for Spinal Stenosis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent MRI scan and consultation with your spinal surgeon
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle
 A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION. Under the Care of Mr M Paterson - 11 -
 ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
ADVICE TO PATIENT DUE TO HAVE MICRODISCECTOMY / SPINAL STENOSIS DECOMPRESSION Under the Care of Mr M Paterson Acknowledgement: Drawings by Jean Paterson Perth Australia 2006 Brochure: R. Grubb Amended:
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Guide Total Hip Replacement
 A Guide To Total Hip Replacement Surgical Services treating you well Introduction This booklet has been written to help you prepare for your operation. Specific practice may vary slightly from surgeon
A Guide To Total Hip Replacement Surgical Services treating you well Introduction This booklet has been written to help you prepare for your operation. Specific practice may vary slightly from surgeon
Total Knee Replacement
 Total Knee Replacement A Guide for Patients Produced by the British Association for Surgery of the Knee and The British Orthopaedic Association (adapted) KNEE ARTHRITIS If your knee is affected by severe
Total Knee Replacement A Guide for Patients Produced by the British Association for Surgery of the Knee and The British Orthopaedic Association (adapted) KNEE ARTHRITIS If your knee is affected by severe
Cheltenham Hip Clinic
 Hip surgery At Cheltenham, we treat a wide range of hip conditions. It s important to note that not all hip problems require surgery and we will always look for a non-surgical solution where possible.
Hip surgery At Cheltenham, we treat a wide range of hip conditions. It s important to note that not all hip problems require surgery and we will always look for a non-surgical solution where possible.
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
A Guide Total Knee Replacement
 A Guide To Total Knee Replacement Surgical Services treating you well Introduction This booklet has been written to help you prepare for your operation. Specific practice may vary slightly from surgeon
A Guide To Total Knee Replacement Surgical Services treating you well Introduction This booklet has been written to help you prepare for your operation. Specific practice may vary slightly from surgeon
Total Hip Replacement PATIENT INFORMATION
 DEPARTMENT OF ORTHOPAEDICS Total Hip Replacement PATIENT INFORMATION Welcome to Orthopaedic Department at Warwick Hospital TOTAL HIP REPLACEMENT Welcome to the Orthopaedic Department at Warwick Hospital.
DEPARTMENT OF ORTHOPAEDICS Total Hip Replacement PATIENT INFORMATION Welcome to Orthopaedic Department at Warwick Hospital TOTAL HIP REPLACEMENT Welcome to the Orthopaedic Department at Warwick Hospital.
Total Knee Replacement
 Manchester Royal Infirmary Total Knee Replacement Department of Orthopaedic Surgery 2 What is a Total Knee Replacement? Total knee replacement is one of the most commonly performed orthopaedic operations
Manchester Royal Infirmary Total Knee Replacement Department of Orthopaedic Surgery 2 What is a Total Knee Replacement? Total knee replacement is one of the most commonly performed orthopaedic operations
MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty MAKOplasty
 Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Pre-op Patient Guide to Partial Knee Resurfacing Your Guide to Partial Knee Resurfacing Page I 1 Partial Knee Resurfacing...2 Benefits Possible with the Procedure...4 Your Guide to Surgery...5 Frequently
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS)
 SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Anterior Approach. to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Varicose Vein Surgery
 Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Information for patients Varicose Vein Surgery Northern General Hospital You have been diagnosed as having varicose veins and your specialist has recommended varicose vein surgery. This leaflet explains
Total Knee Replacement
 Total Knee Replacement Patient Information Author ID: AW Leaflet Number: Musc 012 Name of Leaflet: Total Knee Replacement Date Produced: April 2014 Review Date: April 2016 Total Knee Replacement Page 1
Total Knee Replacement Patient Information Author ID: AW Leaflet Number: Musc 012 Name of Leaflet: Total Knee Replacement Date Produced: April 2014 Review Date: April 2016 Total Knee Replacement Page 1
HIP & KNEE SURGERY PATIENTS
 HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
Minimally Invasive Total Hip Replacement Using a Direct Anterior Approach & Accelerated Rehabilitation
 Bruce White Orthopaedic Surgeon Specialising in Hip and Knee Surgery Minimally Invasive Total Hip Replacement Using a Direct Anterior Approach & Accelerated Rehabilitation Hip Replacement Folder This brochure
Bruce White Orthopaedic Surgeon Specialising in Hip and Knee Surgery Minimally Invasive Total Hip Replacement Using a Direct Anterior Approach & Accelerated Rehabilitation Hip Replacement Folder This brochure
