|
|
|
- Paul Summers
- 8 years ago
- Views:
Transcription
1 icommuni cate SPEECH & COMMUNICATION THERAPY Dysarthria and Dysphonia Dysarthria Dysarthria refers to a speech difficulty that may occur following an injury or disease to the brain, cranial nerves or nervous system. Injury or disease to the speech musculature may also cause dysarthric like symptoms. When the part of the brain that controls speech production is damaged, the link from the brain to the muscles of speech is affected. Dysarthria can present in varying degrees of severity depending on localization and severity of brain damage. The production of speech sounds may be very difficult and in some cases speech may not be possible. The lips, tongue, palate, facial muscles, and the vocal folds (chords) may be uncoordinated or immobile. Further difficulties may occur if breathing is also affected as the lungs provide the energy for speech. An individual with dysarthria may have slurred, hoarse, jerky or strained speech and may be difficult to understand or completely unintelligible. Intelligibility may be further hindered by low volume, variable rate and rhythm, and irregular pitch. As well as traumatic brain injury, dysarthria can be caused by brain tumour, stroke, cerebral palsy, long term use of certain medication, and degenerative diseases such as Parkinsons. Other co-occuring problems may include difficulties with swallowing and saliva control. Types of dysarthria Ataxic dysarthria can cause poor coordination of the speech muscles meaning that speech and volume is slow, erratic and irregular. Speech maybe explosive and extra stress may be put on syllables. Flaccid dysarthria can cause a breathy voice that is often nasal in quality (because of poor control of the soft palate). There is often an obvious paralysis or weakness of the facial muscles. Spastic dysarthria can cause a very slow, indistinct, monotone voice, and at times it may seem strained with some sounds being difficult to articulate. Hyperkinetic dysarthria presents with a harsh, strained voice. Hypokinetic dysarthria presents with a hoarse voice and low volume. A Mixed dysarthria can have a mix of the symptoms mentioned above, and will depend on the type of neuron damage as to whether speech is more harsh or breathy.
2 Treatment of Dysarthria A speech and language pathologist / therapist (SLPT) can work on improving speech difficulties caused by dysarthria. Depending on the severity of the brain damage, speech may not return to normal. However, the SLPT can focus on exercises and compensatory strategies to help improve speech production and intelligibility. The SLPT may also focus on alternative forms of communication or assistive communication to help the individual with dysarthria express themselves and be understood. For those with a mild to moderate dysarthria, speech should still be their main form of communication. For those with severe dysarthria, looking at other ways to communicate may be appropriate. Muscle Exercises There are a wide variety of exercises and approaches, and their use will depend on the patient, severity and location of the brain lesion or disorder (cerebral palsy, traumatic brain injury, stroke etc), and the type of dysarthria. For instance, with flaccid dysarthria, muscle strengthening exercises may be appropriate, but for dysarthria that presents with increased muscle tone and poor coordination, relaxation exercises may need to be performed. Muscle strengthening exercises may involve a series of movement and stretching exercises of the face, jaw, lips and tongue. Other exercises may include isometric exercises, where the muscles push against other stationary objects with force e.g. pushing your tongue against a spoon etc. Breathing Exercises Breathing exercises may also be helpful, as poor breath control will effect volume and sentence length. Our lungs are the bellows, the power source that creates the energy for speech. Not only has our breath got to be powerful enough, but it also has to be timed right. The execution of speech is a precise coordination of many muscles and if our breathe is out of sync, then speech production does not work very effectively. Speech will also be affected if you speak till your breath runs low, as your speech will tend to decrease in volume and intelligibility. There are many exercises to improve breath control and timing. See for more information on breathing and muscle exercises for speech.
3 Compensatory Strategies Compensatory strategies may include, slowing speech (this is probably the most obvious way to become more intelligible), or producing each word, or syllable individually, rather than in a stream of connected speech. This does not present with very natural sounding speech, but can increase intelligibility. Speaking by pronouncing each syllable can be taught using a metronome or teaching the clients to tap their fingers to keep in time. Some people just choose to use key words to get their message across. Over emphasizing facial and articulatory movement and over emphasizing consonants in speech has also been shown to improve intelligibility. Stopping for a breath every few words is another strategy that works for some people, as speech will be slowed and extra power will be given to voice. Gesture or visuals Add gesture to your speech to give the listener another cue to help them understand. Have a book or sheet of visuals of core subjects. This can help cue people into what you are saying by putting them in the context of your conversation. Alphabet Chart Evidence has shown that using an alphabet chart can greatly enhance intelligibility. Not just by spelling out entire words, but by just pointing to the initial letter/sound of a word often cues in the listener to the word you are trying to pronounce. Alternatively, writing or drawing a diagram may also help to communicate a message. Go to for a free alphabet and number chart. Hi-tech Augmentative / Assistive communication aids Depending on the degree of your dysarthria, it may be beneficial to use a hi-tech communication device. There are a range of these machines that offer speech output, either by typing your message or accessing visual symbols on a screen via touch or scanning. Some also offer predictive text, so when you type in a letter, you are provided with a number of common words starting with that letter (this saves you typing the whole word). Lo-tech options such as an E-tram frame and partner assisted scanning, can also work well for communication. See for more examples of assistive technology, software, and lo-tech options to facilitate communication following a stroke, brain injury or degenerative disease.
4 Adapting the environment to help the dysarthric person To facilitate communication ensure that you communicate in an environment that is free from noise and distractions. Look at the dysarthric person when they are talking to see lip movements, facial expression and gesture, all of which will give you cues to facilitate intelligibility. Allow the individual time to get their message across and have a pen and paper at hand for words or diagrams if they are needed. Factors that Influence prognosis Obviously general health and the extent of the illness or trauma will have an effect on the outcome, especially if the disease is progressive, but there are other factors that can influence prognosis. Younger patients generally have a better prognosis, as do those who get good medical treatment and follow-up Speech and Language Therapy input. A positive and motivated disposition prior to, and following the diagnosis of dysarthria, and having good support systems in the form of family and friends usually provides the basis for a better prognosis. Dysphonia Dysphonia is a hoarseness, weakness or loss of voice. Following a stroke, disease, or trauma to the larynx, there can be a paralysis of the vocal folds (often called the vocal cords) and weakness of the muscles relating to phonation. This can cause a change or loss of voice. Organic Dysphonia occurs when there is a physical problem with the vocal apparatus which effects the voice, such as an infection like laryngitis, a structural abnormality such as a nodule, a tumorous growth, or a trauma to the larynx. Functional Dysphonia relates to a voice disorder where there is not a structural abnormality of the larynx, such as a polyp, or any paralysis, but a voice problem exists. This dysphonia usually occurs because of the incorrect use of voice or a psychogenic reason. How the voice works Voice is powered by air from the lungs, the air passes through the larynx which contains the vocal folds. The vocal folds are 2 folds of muscle that meet together many times per second (approximately 125 per second for men and 210 times for woman) when we want to produce voice. The meeting together of the vocal folds creates the voice which resonates in the pharynx, oral and nasal cavities, and is then shaped into words by the speech apparatus, the tongue, lips, facial muscles etc.
5 What goes wrong? A number of things can cause voice problems and these are usually associated with the larynx. Within the larynx are the vocal folds If these get damaged or a growth develops on one of them it will affect the voice. If the vocal folds cannot come together properly, then air can escape between them causing croaky or breathy speech. Weak breath control can also cause voice to be weak or at a low volume. Following a stroke, injury, brain injury or the development of a degenerative disease, the vocal folds may become paralysed. One or both vocal folds may be paralysed, and this will affect the voice and intelligibility. Compensatory strategies or alternative forms of communication may have to be considered to allow the individual to communicate effectively. When one vocal fold is damaged or paralysed surgery can sometimes improve voice. The paralysed vocal fold can be bulked up with another substance such as Teflon, collagen or body fat, and this reduces the space between the 2 folds allowing the working fold to meet the paralysed fold. Alternatively, surgery involving to push the paralysed vocal fold closer to the centre of the larynx may be performed. The working fold can then make better contact with the paralysed fold and voice is improved.. Vocal hygience If you have a voice problem of any sort there are a few things that you can do to look after your voice: Breathing correctly is one of the best ways to improve your voice. Breath from the diaphragm and take deep breathes before you speak. Do not continually talk until you run out of air. If you breath rom your chest, rather than from your stomach (shallow breathing), you are not using your breath for speech correctly and not supplying as much power for speech as you could. Having a good posture will help with your breathing technique. Stay hydrated and drink lots of water continually through the day. Avoid drinking too many caffeinated drinks or too much alcohol. Try to relax and reduce excess tension because this will effect your posture, your breathing, and the muscles of your throat and neck which will impact on your voice. Avoid clearing your throat or whispering. Many people with voice difficulties feel the need to constantly clear their throat, and are often doing this without thinking about it. Throat clearing can really aggravate voice difficulties. Some suggest either doing a hard swallow or taking a sip of water rather than throat clearing. Contrary to what many people believe, whispering is not good for protecting your voice, because the vocal folds have to work harder when whispering.
6 Try to stop or reduce smoking as the smoke passes directly over the vocal folds. Smoking can respiratory illness, laryngeal cancer and other health problems which can all impact on voice. Medications such as inhalers can coat the pharynx and vocal folds, drying them out. One way to help with this is to stay well hydrated and drink lots of water. Talk to your doctor if you feel that your medication may be effecting your voice. Reflux at night this can also cause voice problems. If you think this might be causing your problems, see your doctor for some relevant medication. Avoid work environments that are smoky or dusty. For more information about dysarthria, dysphonia, stroke or brain injury, and activities and exercises to facilitate communication see our website.
7 To learn more about voice and voice problems go to our website, or read about and purchase books from our Online Resource centre by clicking this link: Book Shop Suggested Reading: Motor Speech Disorders by James Paul Dworkin Motor Speech Disorders: Substrates, Differential Diagnosis, and Management by Joseph R. Duffy PhD, Mayo Clinic Clinical Management of Sensorimotor Speech Disorders by Malcolm McNeil Introduction to Neurogenic Communication Disorders by Robert H. Brookshire PhD CCC/SP Language Intervention Strategies in Aphasia and Related Neurogenic Communication Disorders by Roberta Chapey (Editor) Manual of Aphasia and Aphasia Therapy by Nancy Helm-Estabrooks Voice and Voice Therapy (with Free DVD), 7th Edition by Daniel R. Boone, Stephen C. McFarlane, and Shelley L. Von Berg Treatment of Voice Disorders by Robert Thayer Sataloff Greene and Mathieson's The Voice and its Disorders, 6th Ed. by Lesley Mathieson Voice and Laryngeal Disorders: A Problem-Based Clinical Guide with Voice Samples by Sally K. Gallena Laryngeal Cancer - A Medical Dictionary, Bibliography, and Annotated Research Guide to Internet References by ICON Health Publications The Voice Clinic Handbook by Harris, Tom Harris, John S. Rubin, and David M. Howard Voice Disorders and Their Management by Margaret Freeman and Margaret Fawcus Clinical Assessment of Voice by Robert Thayer Sataloff
Neurogenic Disorders of Speech in Children and Adults
 Neurogenic Disorders of Speech in Children and Adults Complexity of Speech Speech is one of the most complex activities regulated by the nervous system It involves the coordinated contraction of a large
Neurogenic Disorders of Speech in Children and Adults Complexity of Speech Speech is one of the most complex activities regulated by the nervous system It involves the coordinated contraction of a large
MS Learn Online Feature Presentation Speech Disorders in MS Featuring Patricia Bednarik, CCC-SLP, MSCS
 Page 1 MS Learn Online Feature Presentation Speech Disorders in MS Featuring, CCC-SLP, MSCS >>Kate Milliken: Hello. I'm Kate Milliken, and welcome to MS Learn Online. There are many symptoms associated
Page 1 MS Learn Online Feature Presentation Speech Disorders in MS Featuring, CCC-SLP, MSCS >>Kate Milliken: Hello. I'm Kate Milliken, and welcome to MS Learn Online. There are many symptoms associated
Who am I? 5/20/2014. Name: Michaela A. Medved. Credentials: MA, TSSLD, CCC SLP. Certifications: LSVT
 Interventions for Treatment of Respiratory Issues in Rehab Michaela A. Medved, MA, TSSLD, CCC SLP Speech Language Pathologist Director of Patient Care Services, Aspire Center for Health and Wellness Who
Interventions for Treatment of Respiratory Issues in Rehab Michaela A. Medved, MA, TSSLD, CCC SLP Speech Language Pathologist Director of Patient Care Services, Aspire Center for Health and Wellness Who
Speech & Swallowing The ba sic fac t s
 Speech & Swallowing The ba sic fac t s Multiple sclerosis If people are asking you to repeat words; if it s getting harder to carry on conversations because your speech is slurred, slow, or quiet; if you
Speech & Swallowing The ba sic fac t s Multiple sclerosis If people are asking you to repeat words; if it s getting harder to carry on conversations because your speech is slurred, slow, or quiet; if you
Adult Speech-Language Pathology Services in Health Care
 Adult Speech-Language Pathology Services in Health Care How do speech-language pathologists (SLPs) help people? SLPs work with people who have trouble speaking listening reading writing thinking swallowing
Adult Speech-Language Pathology Services in Health Care How do speech-language pathologists (SLPs) help people? SLPs work with people who have trouble speaking listening reading writing thinking swallowing
By Brittany White, PT and Kathy Adam, SLP
 By Brittany White, PT and Kathy Adam, SLP Myasthenia Gravis Weakness and rapid fatigue of muscles under your voluntary control. Caused by a breakdown in the normal communication between nerves and muscles.
By Brittany White, PT and Kathy Adam, SLP Myasthenia Gravis Weakness and rapid fatigue of muscles under your voluntary control. Caused by a breakdown in the normal communication between nerves and muscles.
Guidelines for Medical Necessity Determination for Speech and Language Therapy
 Guidelines for Medical Necessity Determination for Speech and Language Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Speech and Language Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
What is aphasia? Aphasia is a language disorder. It can cause problems with. Thinking (cognitive) skills are usually good.
 Adult Aphasia What is aphasia? Aphasia is a language disorder. It can cause problems with understanding speaking reading writing Thinking (cognitive) skills are usually good. What causes aphasia? Aphasia
Adult Aphasia What is aphasia? Aphasia is a language disorder. It can cause problems with understanding speaking reading writing Thinking (cognitive) skills are usually good. What causes aphasia? Aphasia
a guide to understanding moebius syndrome a publication of children s craniofacial association
 a guide to understanding moebius syndrome a publication of children s craniofacial association a guide to understanding moebius syndrome this parent s guide to Moebius syndrome is designed to answer questions
a guide to understanding moebius syndrome a publication of children s craniofacial association a guide to understanding moebius syndrome this parent s guide to Moebius syndrome is designed to answer questions
Speech therapy in treatment of Vocal cord Nodules
 Speech therapy in treatment of Vocal cord Nodules Definition Small benign swellings/ Edema of the subepithelial tissue Along margins of the vocal cords At the junction of the anterior and middle thirds.
Speech therapy in treatment of Vocal cord Nodules Definition Small benign swellings/ Edema of the subepithelial tissue Along margins of the vocal cords At the junction of the anterior and middle thirds.
What is cerebral palsy?
 What is cerebral palsy? This booklet will help you to have a better understanding of the physical and medical aspects of cerebral palsy. We hope it will be a source of information to anyone who wishes
What is cerebral palsy? This booklet will help you to have a better understanding of the physical and medical aspects of cerebral palsy. We hope it will be a source of information to anyone who wishes
Oral Motor Exercises for the Treatment of Motor Speech Disorders: Efficacy and Evidence Based Practice Issues
 Oral Motor Exercises for the Treatment of Motor Speech Disorders: Efficacy and Evidence Based Practice Issues A literature review based on a tutorial by Heather M. Clark (2003) Presented by Leslie Kubacki
Oral Motor Exercises for the Treatment of Motor Speech Disorders: Efficacy and Evidence Based Practice Issues A literature review based on a tutorial by Heather M. Clark (2003) Presented by Leslie Kubacki
The Role of the SLP in Schools. A Presentation for Teachers, Administrators, Parents, and the Community 1
 The Role of the SLP in Schools A Presentation for Teachers, Administrators, Parents, and the Community 1 Speech-Language Pathologists (SLPs) Are Specially Trained Professionals Who Have Earned: A master
The Role of the SLP in Schools A Presentation for Teachers, Administrators, Parents, and the Community 1 Speech-Language Pathologists (SLPs) Are Specially Trained Professionals Who Have Earned: A master
SPEECH, SWALLOWING, AND COMMUNICATION IN HD. Cheryl Gidddens, Ph.D. Associate Professor Oklahoma State University cheryl.giddens@okstate.
 SPEECH, SWALLOWING, AND COMMUNICATION IN HD Cheryl Gidddens, Ph.D. Associate Professor Oklahoma State University cheryl.giddens@okstate.edu The information provided by speakers in workshops, forums, sharing/networking
SPEECH, SWALLOWING, AND COMMUNICATION IN HD Cheryl Gidddens, Ph.D. Associate Professor Oklahoma State University cheryl.giddens@okstate.edu The information provided by speakers in workshops, forums, sharing/networking
Speech and language therapy after stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Speech and language therapy after stroke Speech and language therapy (SLT) can help if you have communication problems or swallowing problems after
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Speech and language therapy after stroke Speech and language therapy (SLT) can help if you have communication problems or swallowing problems after
School-Based Health Services: Speech and Language Therapy. Brenda Addington, MA, CCC-SLP Jessamine County Schools August 29, 2013
 School-Based Health Services: Speech and Language Therapy Brenda Addington, MA, CCC-SLP Jessamine County Schools August 29, 2013 Session Objectives: 1. Overview of the areas of communication served in
School-Based Health Services: Speech and Language Therapy Brenda Addington, MA, CCC-SLP Jessamine County Schools August 29, 2013 Session Objectives: 1. Overview of the areas of communication served in
Cerebral Palsy. 1 - Introduction. An informative Booklet for families in the Children and Teens program
 Cerebral Palsy 1 - Introduction An informative Booklet for families in the Children and Teens program Centre de réadaptation Estrie, 2008 Preface Dear parents, It is with great pleasure that we present
Cerebral Palsy 1 - Introduction An informative Booklet for families in the Children and Teens program Centre de réadaptation Estrie, 2008 Preface Dear parents, It is with great pleasure that we present
Pneumonia Education and Discharge Instructions
 Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
Pneumonia Education and Discharge Instructions Pneumonia Education and Discharge Instructions Definition: Pneumonia is an infection of the lungs. Many different organisms can cause it, including bacteria,
The Road to Rehabilitation
 The Road to Rehabilitation Part 5 Crossing the Communication Bridge: Speech, Language & Brain Injury Written by Jean L. Blosser, EdD, CCC/SCLP Roberta DePompei, PhD, CCC/SCLP Content reveiwed by Gregory
The Road to Rehabilitation Part 5 Crossing the Communication Bridge: Speech, Language & Brain Injury Written by Jean L. Blosser, EdD, CCC/SCLP Roberta DePompei, PhD, CCC/SCLP Content reveiwed by Gregory
Ph.D in Speech-Language Pathology
 UNIT 1 SPEECH LANGUAGE PRODUCTION Physiology of speech production. Physiology of speech (a) Respiration: methods of respiratory analysis (b) Laryngeal function: Laryngeal movements, vocal resonance (c)
UNIT 1 SPEECH LANGUAGE PRODUCTION Physiology of speech production. Physiology of speech (a) Respiration: methods of respiratory analysis (b) Laryngeal function: Laryngeal movements, vocal resonance (c)
AUGMENTATIVE COMMUNICATION EVALUATION
 AUGMENTATIVE COMMUNICATION EVALUATION Date: Name: Age: Date of Birth: Address: Telephone: Referral Source: Diagnosis: Participants: Social History and Current Services: lives with his in a private home
AUGMENTATIVE COMMUNICATION EVALUATION Date: Name: Age: Date of Birth: Address: Telephone: Referral Source: Diagnosis: Participants: Social History and Current Services: lives with his in a private home
The Pediatric Program at Marianjoy
 MARIANJOY Rehabilitation Hospital Wheaton Franciscan Healthcare The Pediatric Program at Marianjoy Celebrating Even the Smallest Steps, One Step at a Time The Pediatric Program at Marianjoy Celebrating
MARIANJOY Rehabilitation Hospital Wheaton Franciscan Healthcare The Pediatric Program at Marianjoy Celebrating Even the Smallest Steps, One Step at a Time The Pediatric Program at Marianjoy Celebrating
Critical Review: Sarah Rentz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
 Critical Review: In children with cerebral palsy and a diagnosis of dysarthria, what is the effectiveness of speech interventions on improving speech intelligibility? Sarah Rentz M.Cl.Sc (SLP) Candidate
Critical Review: In children with cerebral palsy and a diagnosis of dysarthria, what is the effectiveness of speech interventions on improving speech intelligibility? Sarah Rentz M.Cl.Sc (SLP) Candidate
SAM KARAS ACUTE REHABILITATION CENTER
 SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
SAM KARAS ACUTE REHABILITATION CENTER 1 MEDICAL CARE Sam Karas Acute Rehabilitation The Sam Karas Acute Rehabilitation Center is a comprehensive and interdisciplinary inpatient unit. Medical care is directed
Treatment for Acquired Apraxia of Speech. Kristine Stanton Grace Cotton
 Treatment for Acquired Apraxia of Speech Kristine Stanton Grace Cotton What is Apraxia of Speech (AOS)? a disturbed ability to produce purposeful, learned movements despite intact mobility, secondary to
Treatment for Acquired Apraxia of Speech Kristine Stanton Grace Cotton What is Apraxia of Speech (AOS)? a disturbed ability to produce purposeful, learned movements despite intact mobility, secondary to
EARLY INTERVENTION: COMMUNICATION AND LANGUAGE SERVICES FOR FAMILIES OF DEAF AND HARD-OF-HEARING CHILDREN
 EARLY INTERVENTION: COMMUNICATION AND LANGUAGE SERVICES FOR FAMILIES OF DEAF AND HARD-OF-HEARING CHILDREN Our child has a hearing loss. What happens next? What is early intervention? What can we do to
EARLY INTERVENTION: COMMUNICATION AND LANGUAGE SERVICES FOR FAMILIES OF DEAF AND HARD-OF-HEARING CHILDREN Our child has a hearing loss. What happens next? What is early intervention? What can we do to
Developmental Verbal Dyspraxia Nuffield Approach
 Developmental Verbal Dyspraxia Nuffield Approach Pam Williams, Consultant Speech & Language Therapist Nuffield Hearing & Speech Centre RNTNE Hospital, London, Uk Outline of session Speech & language difficulties
Developmental Verbal Dyspraxia Nuffield Approach Pam Williams, Consultant Speech & Language Therapist Nuffield Hearing & Speech Centre RNTNE Hospital, London, Uk Outline of session Speech & language difficulties
Speech Therapy for Cleft Palate or Velopharyngeal Dysfunction (VPD) Indications for Speech Therapy
 Speech Therapy for Cleft Palate or Velopharyngeal Dysfunction (VPD), CCC-SLP Cincinnati Children s Hospital Medical Center Children with a history of cleft palate or submucous cleft are at risk for resonance
Speech Therapy for Cleft Palate or Velopharyngeal Dysfunction (VPD), CCC-SLP Cincinnati Children s Hospital Medical Center Children with a history of cleft palate or submucous cleft are at risk for resonance
The Speech-Language Pathologist s Role in Geriatric Care
 The Speech-Language Pathologist s Role in Geriatric Care Mario A. Landera, M.A., CCC-SLP, BRS-S Clinical Instructor Department of Otolaryngology University of Miami Miller School of Medicine What is a
The Speech-Language Pathologist s Role in Geriatric Care Mario A. Landera, M.A., CCC-SLP, BRS-S Clinical Instructor Department of Otolaryngology University of Miami Miller School of Medicine What is a
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
Preparation "Speech Language Pathologist Overview"
 Speech Language Pathologist Overview The Field - Preparation - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Speech-language pathologists, sometimes
Speech Language Pathologist Overview The Field - Preparation - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Speech-language pathologists, sometimes
Holistic Music Therapy and Rehabilitation
 Holistic Music Therapy and Rehabilitation Jennifer Townsend NMT, MT-BC Neurologic Music Therapist Music Therapist-Board Certified The National Flute Association August 15, 2009 From Social Science to Neuroscience
Holistic Music Therapy and Rehabilitation Jennifer Townsend NMT, MT-BC Neurologic Music Therapist Music Therapist-Board Certified The National Flute Association August 15, 2009 From Social Science to Neuroscience
Cerebral Palsy. In order to function, the brain needs a continuous supply of oxygen.
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
8/17/11 IMPROVING RESPIRATORY SUPPORT: NONSPEECH TASKS. DYSARTHRIA TREATMENT: PRACTICE GUIDELINES AND OPTIONS PART 1 KSHA September 2011
 NONSPEECH TASKS DYSARTHRIA TREATMENT: PRACTICE GUIDELINES AND OPTIONS PART 1 KSHA September 2011 Use these strategies if speaker can t generate enough subglottic air pressure to support phonation These
NONSPEECH TASKS DYSARTHRIA TREATMENT: PRACTICE GUIDELINES AND OPTIONS PART 1 KSHA September 2011 Use these strategies if speaker can t generate enough subglottic air pressure to support phonation These
Understanding Impaired Speech. Kobi Calev, Morris Alper January 2016 Voiceitt
 Understanding Impaired Speech Kobi Calev, Morris Alper January 2016 Voiceitt Our Problem Domain We deal with phonological disorders They may be either - resonance or phonation - physiological or neural
Understanding Impaired Speech Kobi Calev, Morris Alper January 2016 Voiceitt Our Problem Domain We deal with phonological disorders They may be either - resonance or phonation - physiological or neural
Technology in Music Therapy and Special Education. What is Special Education?
 Technology in Music Therapy and Special Education What is Special Education? Disabilities are categorized into the following areas: o Autism, visual impairment, hearing impairment, deaf- blindness, multiple
Technology in Music Therapy and Special Education What is Special Education? Disabilities are categorized into the following areas: o Autism, visual impairment, hearing impairment, deaf- blindness, multiple
Every Voice Deserves To Be Heard. Christina Santos MS CCC-SLP INTEGRIS Jim Thorpe Outpatient Rehabilitation Christina.Santos@integrisok.
 Every Voice Deserves To Be Heard Christina Santos MS CCC-SLP INTEGRIS Jim Thorpe Outpatient Rehabilitation Christina.Santos@integrisok.com Course Objectives O Participants will be able to: 1) Identify
Every Voice Deserves To Be Heard Christina Santos MS CCC-SLP INTEGRIS Jim Thorpe Outpatient Rehabilitation Christina.Santos@integrisok.com Course Objectives O Participants will be able to: 1) Identify
MEDICAL POLICY SUBJECT: SPEECH PATHOLOGY AND THERAPY. POLICY NUMBER: 8.01.13 CATEGORY: Therapy/Rehabilitation
 MEDICAL POLICY SUBJECT: SPEECH PATHOLOGY AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
MEDICAL POLICY SUBJECT: SPEECH PATHOLOGY AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
Dysarthria. Dysarthria Review. Review of the Dysarthria Types. Dysarthria Review (con t) Speech Characteristics Flaccid
 Dysarthria Differential diagnosis and treatment of dysarthria in children Presented by K. Farinella, Ph.D., CCC-SLP April 12, 2013 1:30 3pm General diagnostic term for a group of speech disorders resulting
Dysarthria Differential diagnosis and treatment of dysarthria in children Presented by K. Farinella, Ph.D., CCC-SLP April 12, 2013 1:30 3pm General diagnostic term for a group of speech disorders resulting
Contact your Doctor or Nurse for more information.
 A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
TMJ. Problems. Certain headaches and pain in. the ear, jaw, neck, tooth, and. sinus can be the result of a. temporomandibular joint (TMJ)
 DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
Cerebral palsy can be classified according to the type of abnormal muscle tone or movement, and the distribution of these motor impairments.
 The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
Cranial Nerve/Oral Mech Exam: What Every SLP Needs to Know
 Cranial Nerve/Oral Mech Exam: What Every SLP Needs to Know Kelly Dailey Hall, Ph.D. CCC/SLP Pediatric Speech & Language Services, Inc. University of North Carolina Greensboro kdhall2@uncg.edu What s in
Cranial Nerve/Oral Mech Exam: What Every SLP Needs to Know Kelly Dailey Hall, Ph.D. CCC/SLP Pediatric Speech & Language Services, Inc. University of North Carolina Greensboro kdhall2@uncg.edu What s in
What is Obstructive Sleep Apnoea?
 Patient Information Leaflet: Obstructive Sleep Apnoea Greenlane Respiratory Services, Auckland City Hospital & Greenlane Clinical Centre Auckland District Health Board What is Obstructive Sleep Apnoea?
Patient Information Leaflet: Obstructive Sleep Apnoea Greenlane Respiratory Services, Auckland City Hospital & Greenlane Clinical Centre Auckland District Health Board What is Obstructive Sleep Apnoea?
Practical Personal Voice Experience in Speech and Language Therapy Training
 Shewell C. (2000). The voice of experience. Royal College of Speech and Language Therapists Bulletin. November 2000, 7-8. Practical Personal Voice Experience in Speech and Language Therapy Training Christina
Shewell C. (2000). The voice of experience. Royal College of Speech and Language Therapists Bulletin. November 2000, 7-8. Practical Personal Voice Experience in Speech and Language Therapy Training Christina
Speech and Voice Disorders in Parkinson s Disease
 Speech and Voice Disorders in Parkinson s Disease Matt McKeon M.S. CCC-SLP Lead Speech-Language-Pathologist Parkinson care team lead The Virginian CCRC and outpatient clinic March 28, 2015 Numbers for
Speech and Voice Disorders in Parkinson s Disease Matt McKeon M.S. CCC-SLP Lead Speech-Language-Pathologist Parkinson care team lead The Virginian CCRC and outpatient clinic March 28, 2015 Numbers for
Cerebral Palsy: Intervention Methods for Young Children. Emma Zercher. San Francisco State University
 RUNNING HEAD: Cerebral Palsy & Intervention Methods Cerebral Palsy & Intervention Methods, 1 Cerebral Palsy: Intervention Methods for Young Children Emma Zercher San Francisco State University May 21,
RUNNING HEAD: Cerebral Palsy & Intervention Methods Cerebral Palsy & Intervention Methods, 1 Cerebral Palsy: Intervention Methods for Young Children Emma Zercher San Francisco State University May 21,
SPEECH OR LANGUAGE IMPAIRMENT
 I. DEFINITION "Speech or Language Impairment" means a communication disorder, such as stuttering, impaired articulation, a language impairment, or a voice impairment, that adversely affects a child's educational
I. DEFINITION "Speech or Language Impairment" means a communication disorder, such as stuttering, impaired articulation, a language impairment, or a voice impairment, that adversely affects a child's educational
What to Expect When You re Not Expecting Aphasia
 An aphasia diagnosis is unplanned, unexpected, and frustrating, but it s not hopeless. It s a journey. What to Expect When You re Not Expecting Aphasia An ebook from There are 2 million people living with
An aphasia diagnosis is unplanned, unexpected, and frustrating, but it s not hopeless. It s a journey. What to Expect When You re Not Expecting Aphasia An ebook from There are 2 million people living with
THESE ARE A FEW OF MY FAVORITE THINGS DIRECT INTERVENTION WITH PRESCHOOL CHILDREN: ALTERING THE CHILD S TALKING BEHAVIORS
 THESE ARE A FEW OF MY FAVORITE THINGS DIRECT INTERVENTION WITH PRESCHOOL CHILDREN: ALTERING THE CHILD S TALKING BEHAVIORS Guidelines for Modifying Talking There are many young children regardless of age
THESE ARE A FEW OF MY FAVORITE THINGS DIRECT INTERVENTION WITH PRESCHOOL CHILDREN: ALTERING THE CHILD S TALKING BEHAVIORS Guidelines for Modifying Talking There are many young children regardless of age
Treating Sleep Apnea A Review of the Research for Adults
 Treating Sleep Apnea A Review of the Research for Adults Is This Information Right for Me? Yes, if: A doctor said you have mild, moderate, or severe obstructive sleep apnea, or OSA. People with OSA may
Treating Sleep Apnea A Review of the Research for Adults Is This Information Right for Me? Yes, if: A doctor said you have mild, moderate, or severe obstructive sleep apnea, or OSA. People with OSA may
Cerebral Palsy. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com nr200105 Last reviewed: 06/17/2014 1
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Who are these patients? Neck Pain in Voice Disorders. Etiologies of Cervicalgia. Role of Physical Therapy in Treatment of Voice Disorders
 Role of Physical Therapy in Treatment of Voice Disorders DAVID O. FRANCIS, MD MS VANDERBILT VOICE CENTER NOVEMBER 5, 2011 Singers Who are these patients? Performers Athletes Exercise with weights Heavy
Role of Physical Therapy in Treatment of Voice Disorders DAVID O. FRANCIS, MD MS VANDERBILT VOICE CENTER NOVEMBER 5, 2011 Singers Who are these patients? Performers Athletes Exercise with weights Heavy
THOSE WHO USE THEIR VOICE PROFESSIONALLY for singing,
 Robert T. Sataloff, MD, DMA, Associate Editor CARE OF THE PROFESSIONAL VOICE How Do I Maintain Longevity of My Voice? Yolanda D. Heman-Ackah, MD, Robert T. Sataloff, MD, DMA, Mary J. Hawkshaw, BSN, RN,
Robert T. Sataloff, MD, DMA, Associate Editor CARE OF THE PROFESSIONAL VOICE How Do I Maintain Longevity of My Voice? Yolanda D. Heman-Ackah, MD, Robert T. Sataloff, MD, DMA, Mary J. Hawkshaw, BSN, RN,
Laryngeal Cancer. Understanding your diagnosis
 Laryngeal Cancer Understanding your diagnosis Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large
Laryngeal Cancer Understanding your diagnosis Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large
Providing Professional Care in Rehabilitation Services
 For more information about Inspira Rehab Care or for a patient evaluation, please contact any one of our facilities: Inspira Rehab Care Bridgeton Health Center 333 Irving Avenue Bridgeton, NJ 08302 (856)
For more information about Inspira Rehab Care or for a patient evaluation, please contact any one of our facilities: Inspira Rehab Care Bridgeton Health Center 333 Irving Avenue Bridgeton, NJ 08302 (856)
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
THE SPEAKING ABILITY IMPROVEMENT ON THE PRESCHOOLERS WITH CEREBRAL PALSY THROUGH SPEECH THERAPY
 International Journal of Education and Research Vol. 3 No. 9 September 2015 THE SPEAKING ABILITY IMPROVEMENT ON THE PRESCHOOLERS WITH CEREBRAL PALSY THROUGH SPEECH THERAPY Ni Luh Putri Faculty of Education
International Journal of Education and Research Vol. 3 No. 9 September 2015 THE SPEAKING ABILITY IMPROVEMENT ON THE PRESCHOOLERS WITH CEREBRAL PALSY THROUGH SPEECH THERAPY Ni Luh Putri Faculty of Education
Developmental Verbal Dyspraxia
 Developmental Verbal Dyspraxia Pam Williams Dip. CST; M Sc; MRCSLT Pam Williams is Principal Speech and Language Therapist, Nuffield Hearing and Speech Centre, Royal National Throat, Nose and Ear Hospital,
Developmental Verbal Dyspraxia Pam Williams Dip. CST; M Sc; MRCSLT Pam Williams is Principal Speech and Language Therapist, Nuffield Hearing and Speech Centre, Royal National Throat, Nose and Ear Hospital,
Parkinson s Disease Speech and Swallowing
 Parkinson s Disease Speech and Swallowing By Marjorie L. Johnson, MA/CCC-SLP Table of Contents Introduction Chapter 1 Chapter 2 Chapter 3 Chapter 4 Speech and Swallowing Changes in Parkinson s Disease...4
Parkinson s Disease Speech and Swallowing By Marjorie L. Johnson, MA/CCC-SLP Table of Contents Introduction Chapter 1 Chapter 2 Chapter 3 Chapter 4 Speech and Swallowing Changes in Parkinson s Disease...4
Diuretics: You may get diuretic medicine to help decrease swelling in your brain. This may help your brain get better blood flow.
 Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
Hemorrhagic Stroke GENERAL INFORMATION: What is a hemorrhagic stroke? A hemorrhagic stroke happens when a blood vessel in the brain bursts. This may happen if the blood vessel wall is weak, or sometimes
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Many thanks to my sponsor:
 Oral Care for the Medically Complex Patient: From Intensive Care to Long-term Care Michigan Dental Association Lansing MI April 25, 2015 Cindy Kleiman RDH, BS Oral Care Consultant and Speaker Many thanks
Oral Care for the Medically Complex Patient: From Intensive Care to Long-term Care Michigan Dental Association Lansing MI April 25, 2015 Cindy Kleiman RDH, BS Oral Care Consultant and Speaker Many thanks
Cerebral Palsy. www.teachinngei.org p. 1
 Cerebral Palsy What is cerebral palsy? Cerebral palsy (CP) is a motor disability caused by a static, non-progressive lesion (encephalopathy) in the brain that occurs in early childhood, usually before
Cerebral Palsy What is cerebral palsy? Cerebral palsy (CP) is a motor disability caused by a static, non-progressive lesion (encephalopathy) in the brain that occurs in early childhood, usually before
Treatment of Dysarthria in Patients with Multiple Sclerosis. Barbara Bryant Jane Vyce
 Treatment of Dysarthria in Patients with Multiple Sclerosis Barbara Bryant Jane Vyce What is MS? An autoimmune disease Destruction of myelin Destruction of axons What is MS? Etiology/Pathophysiology Cause
Treatment of Dysarthria in Patients with Multiple Sclerosis Barbara Bryant Jane Vyce What is MS? An autoimmune disease Destruction of myelin Destruction of axons What is MS? Etiology/Pathophysiology Cause
Resource Guide to Oral Motor Skill Difficulties in Children with Down Syndrome
 Resource Guide to Oral Motor Skill Difficulties in Children with Down Syndrome By Libby Kumin, Ph.D., CCC-SLP Loyola College, Columbia, MD Why does my child have difficulty with feeding, drinking and speech?
Resource Guide to Oral Motor Skill Difficulties in Children with Down Syndrome By Libby Kumin, Ph.D., CCC-SLP Loyola College, Columbia, MD Why does my child have difficulty with feeding, drinking and speech?
Position Classification Standard for Speech Pathology and Audiology Series, GS-0665
 Position Classification Standard for Speech Pathology and Audiology Series, GS-0665 Table of Contents SERIES DEFINITION... 2 EXCLUSIONS... 2 COVERAGE OF THE SERIES... 3 COVERAGE OF THE STANDARD... 4 OCCUPATIONAL
Position Classification Standard for Speech Pathology and Audiology Series, GS-0665 Table of Contents SERIES DEFINITION... 2 EXCLUSIONS... 2 COVERAGE OF THE SERIES... 3 COVERAGE OF THE STANDARD... 4 OCCUPATIONAL
WHAT IS CEREBRAL PALSY?
 WHAT IS CEREBRAL PALSY? Cerebral Palsy is a dysfunction in movement resulting from injury to or poor development of the brain prior to birth or in early childhood. Generally speaking, any injury or disease
WHAT IS CEREBRAL PALSY? Cerebral Palsy is a dysfunction in movement resulting from injury to or poor development of the brain prior to birth or in early childhood. Generally speaking, any injury or disease
Parkinson s Disease (PD)
 Parkinson s Disease (PD) Parkinson s disease (PD) is a movement disorder that worsens over time. About 1 in 100 people older than 60 has Parkinson s. The exact cause of PD is still not known, but research
Parkinson s Disease (PD) Parkinson s disease (PD) is a movement disorder that worsens over time. About 1 in 100 people older than 60 has Parkinson s. The exact cause of PD is still not known, but research
Rehabilitation Programme of Stroke Patients in RC Kladruby
 Rehabilitation Programme of Stroke Patients in RC Kladruby Bc. Zdeněk Váňa Content About rehabilitation centre Rehabilitation team members roles Stroke patients rehabilitation programme Basic Information
Rehabilitation Programme of Stroke Patients in RC Kladruby Bc. Zdeněk Váňa Content About rehabilitation centre Rehabilitation team members roles Stroke patients rehabilitation programme Basic Information
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136. Days and Hours: Monday Friday 8:30a.m. 6:00p.m. (305) 355 9028 (JMH, Downtown)
 UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider. www.umke.org
 Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
How To Manage A Catastrophic Injury
 Report #14 CATASTROPHIC INJURIES: Paralysis, Amputation, Burns Overview: A catastrophic injury or illness usually occurs suddenly and without warning. Injuries may be considered catastrophic when they
Report #14 CATASTROPHIC INJURIES: Paralysis, Amputation, Burns Overview: A catastrophic injury or illness usually occurs suddenly and without warning. Injuries may be considered catastrophic when they
REHABILITATION SERVICES
 REHABILITATION SERVICES S O U T H A M P T O N H O S P I T A L C o m m i t t e d to E xc e l l e n c e, to C o m m u n i t y, a n d to Yo u. A c ute C a r e R e h a b i l itati o n C a r d i o p u l m o
REHABILITATION SERVICES S O U T H A M P T O N H O S P I T A L C o m m i t t e d to E xc e l l e n c e, to C o m m u n i t y, a n d to Yo u. A c ute C a r e R e h a b i l itati o n C a r d i o p u l m o
St. Luke s MS Center New Patient Questionnaire. Name: Date: Birth date: Right or Left handed? Who is your Primary Doctor?
 St. Luke s MS Center New Patient Questionnaire Name: Date: Birth date: Right or Left handed? Who is your Primary Doctor? Who referred you to the MS Center? List any other doctors you see: Reason you have
St. Luke s MS Center New Patient Questionnaire Name: Date: Birth date: Right or Left handed? Who is your Primary Doctor? Who referred you to the MS Center? List any other doctors you see: Reason you have
Whiplash Associated Disorder
 Whiplash Associated Disorder Bourassa & Associates Rehabilitation Centre What is Whiplash? Whiplash is a non-medical term used to describe neck pain following hyperflexion or hyperextension of the tissues
Whiplash Associated Disorder Bourassa & Associates Rehabilitation Centre What is Whiplash? Whiplash is a non-medical term used to describe neck pain following hyperflexion or hyperextension of the tissues
Dysphagia: What Your Speech Language Pathologist Wants You to Know
 Online Continuing Education for Nurses Linking Learning to Performance I NSIDE T HIS C OURSE: Course Outline... 2 A&P of the Normal Swallow... 3 Symptoms of... 4 Speech-Language Pathologist... 5 Role of
Online Continuing Education for Nurses Linking Learning to Performance I NSIDE T HIS C OURSE: Course Outline... 2 A&P of the Normal Swallow... 3 Symptoms of... 4 Speech-Language Pathologist... 5 Role of
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
6/26/2014 MUSCLE TENSION DYSPHONIA: TREATMENT WHAT IS MTD?
 MUSCLE TENSION DYSPHONIA: TREATMENT Lisa Valasek, MS CCC-SLP WHAT IS MTD? Hypercontraction of the extrinsic muscles of the larynx Incoordination of muscle activity controlling adduction, abduction, and
MUSCLE TENSION DYSPHONIA: TREATMENT Lisa Valasek, MS CCC-SLP WHAT IS MTD? Hypercontraction of the extrinsic muscles of the larynx Incoordination of muscle activity controlling adduction, abduction, and
Jellow. for the Cerebral Palsy. Antara Hazarika, Kumar Anchal, Priti Thankar, Samraat Sardesai. a study by
 Jellow for the Cerebral Palsy a study by Antara Hazarika, Kumar Anchal, Priti Thankar, Samraat Sardesai Index Understanding the world of CP Modes of communication The need for the product ( product rational)
Jellow for the Cerebral Palsy a study by Antara Hazarika, Kumar Anchal, Priti Thankar, Samraat Sardesai Index Understanding the world of CP Modes of communication The need for the product ( product rational)
Normal bladder function requires a coordinated effort between the brain, spinal cord, and the bladder.
 .. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
.. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
Learning about Mouth Cancer
 Learning about Mouth Cancer Creation of this material was made possible in part by a pioneering grant from CBCC-USA. Distributed by India Cancer Initiative What is mouth cancer? Our bodies are made up
Learning about Mouth Cancer Creation of this material was made possible in part by a pioneering grant from CBCC-USA. Distributed by India Cancer Initiative What is mouth cancer? Our bodies are made up
Children who stammer. Also known as stuttering or dysfluency General information
 Children who stammer Also known as stuttering or dysfluency General information Stammering varies with the individual child, but some common features are: Repetition of whole words, for example, When,
Children who stammer Also known as stuttering or dysfluency General information Stammering varies with the individual child, but some common features are: Repetition of whole words, for example, When,
Sleep Difficulties. Insomnia. By Thomas Freedom, MD and Johan Samanta, MD
 Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
 PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS De Anna Looper, RN CHPN Corporate Clinical Consultant / Legal Nurse Consultant Carrefour Associates L.L.C. PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS De Anna Looper, RN CHPN Corporate Clinical Consultant / Legal Nurse Consultant Carrefour Associates L.L.C. PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
Webinar title: Know Your Options for Treating Severe Spasticity
 Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
How To Become A Physio And Rehabilitation Medicine Specialist
 EUROPEAN BOARD OF PHYSICAL AND REHABILITATION MEDICINE LOGBOOK EUROPEAN UNION OF MEDICAL SPECIALISTS UEMS IDENTIFICATION... 2 INSTRUCTIONS FOR USE... 3 THE TRAINING COURSE... 3 TRAINING PROGRAMME... 4
EUROPEAN BOARD OF PHYSICAL AND REHABILITATION MEDICINE LOGBOOK EUROPEAN UNION OF MEDICAL SPECIALISTS UEMS IDENTIFICATION... 2 INSTRUCTIONS FOR USE... 3 THE TRAINING COURSE... 3 TRAINING PROGRAMME... 4
Lateral pterygoid muscle Medial pterygoid muscle
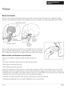 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
Importance of Integrating Stroke Rehabilitation Across the Continuum of Care
 Importance of Integrating Stroke Rehabilitation Across the Continuum of Care Dori Tooke, MHA, PT, CSCS Manager-Inpatient Rehab Program St. Luke s Medical Center Milwaukee, WI Disclosure Nothing to disclose
Importance of Integrating Stroke Rehabilitation Across the Continuum of Care Dori Tooke, MHA, PT, CSCS Manager-Inpatient Rehab Program St. Luke s Medical Center Milwaukee, WI Disclosure Nothing to disclose
Communication problems after stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Communication problems after stroke Many people have communication problems after a stroke. About a third of stroke survivors have some difficulty
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Communication problems after stroke Many people have communication problems after a stroke. About a third of stroke survivors have some difficulty
Personal Training Health Screening Questionnaire
 Personal Training Health Screening Questionnaire Personal Information Today s date: Title: Dr. Mr. Mrs. Ms. Name: / Birth date: Last name First name Age: Address: Phone: (home) City: Phone: (work) Province:
Personal Training Health Screening Questionnaire Personal Information Today s date: Title: Dr. Mr. Mrs. Ms. Name: / Birth date: Last name First name Age: Address: Phone: (home) City: Phone: (work) Province:
Living and Aging with Cerebral Palsy. By Maureen Arcand
 Living and Aging with Cerebral Palsy By Maureen Arcand Living and Aging with Cerebral Palsy Presented to Adults with Cerebral Palsy, their Families & Service Providers By Maureen Arcand November 2002 This
Living and Aging with Cerebral Palsy By Maureen Arcand Living and Aging with Cerebral Palsy Presented to Adults with Cerebral Palsy, their Families & Service Providers By Maureen Arcand November 2002 This
Speech and communication in cerebral palsy
 Speech and communication in cerebral palsy Lindsay Pennington Institute of Health and Society, Newcastle University, England, UK Abstract. Children communicate using speech, vocalisation, facial expression,
Speech and communication in cerebral palsy Lindsay Pennington Institute of Health and Society, Newcastle University, England, UK Abstract. Children communicate using speech, vocalisation, facial expression,
Management in the pre-hospital setting
 Management in the pre-hospital setting Inflammation of the joints Two main types: Osteoarthritis - cartilage loss from wear and tear Rheumatoid arthritis - autoimmune disorder Affects all age groups,
Management in the pre-hospital setting Inflammation of the joints Two main types: Osteoarthritis - cartilage loss from wear and tear Rheumatoid arthritis - autoimmune disorder Affects all age groups,
Maria Tosoni & Lindsey Gannon
 Maria Tosoni & Lindsey Gannon Thoracic Muscles Muscles of Inspiration External Intercostal Muscles & Intercartilaginous Intercostal Muscles Muscles of Expiration Interosseus Intercostal Muscles Abdominal
Maria Tosoni & Lindsey Gannon Thoracic Muscles Muscles of Inspiration External Intercostal Muscles & Intercartilaginous Intercostal Muscles Muscles of Expiration Interosseus Intercostal Muscles Abdominal
