Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances
|
|
|
- Lesley Myron Chapman
- 8 years ago
- Views:
Transcription
1 Sleep Medicine Reviews (2004) 8, CLINICAL REVIEW Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances Peter A. Cistulli a, *,1, Helen Gotsopoulos a, Marie Marklund b, Alan A. Lowe c a Department of Respiratory and Sleep Medicine, St George Hospital, University of New South Wales, Kogarah, Sydney, NSW 2217, Australia b Department of Orthodontics, Umea University, Umea, Sweden c Division of Orthodontics, Department of Oral Health Sciences, Faculty of Dentistry, University of British Columbia, Vancouver, BC, Canada KEYWORDS Snoring; Obstructive sleep apnea; Oral appliance; Mandibular advancement Summary Snoring and obstructive sleep apnea form part of a spectrum of sleep disordered breathing affecting a significant proportion of the general population and particularly the middle aged. The consequences can be severe and even life threatening for both the individual directly affected and those more remotely involved. Adverse sequelae can manifest themselves acutely or in the longer term as a result of obstructive breathing induced hypersomnolence, neurocognitive deficits and cardiovascular abnormalities. The combination of anatomical and neuromuscular risk factors in the pathogenesis of OSA has resulted in a varied approach to its management. One such treatment option is mandibular repositioning appliances (MRA), which mechanically stabilize the airway. Whilst the efficacy of this simple intervention has been rigorously proven quite recently in a significant proportion of patients with varying disease severity, individual patient selection in its application remains uncertain. Short-term side-effects are common but usually transient, whilst in the long-term minor permanent adverse developments on the dentition and occlusion have been reported. Considering both the medicolegal implications of snoring and OSA and the increasing popularity of MRA, it is recommended that skilled multidisciplinary respiratory and dental personnel form the primary care team. q 2004 Elsevier Ltd. All rights reserved. Introduction Obstructive sleep apnea (OSA) is a very common disorder, affecting approximately 4% of men and 2% of women in the middle-aged workforce. 1 Snoring, *Corresponding author. address: p.cistulli@unsw.edu.au (P.A. Cistulli). 1 Peter Cistulli has agreed to act as a medical advisor to an Australian start-up company that intends to commercialise an oral appliance for snoring and sleep apnoea. It is anticipated that the company will become operational some time in the second half of Royalties from Kleenway sales are paid directly to the University of British Coloumbia. a precursor to OSA, is even more common affecting 40 60% of adults. 2 These disorders result from sleeprelated narrowing of the upper airway, which is thought to be due to varying combinations of anatomical and neuromuscular factors that culminate in an imbalance of forces acting on the airway. This causes airflow limitation (snoring), partial (hypopnea) or complete (apnea) closure of the upper airway, with consequent adverse effects on sleep quality and gas exchange. Daytime consequences of OSA include a range of symptoms related to excessive sleepiness, neurocognitive impairment, and mood disturbance, which affect quality of life /$ - see front matter q 2004 Elsevier Ltd. All rights reserved. doi: /j.smrv
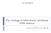
2 444 P.A. Cistulli et al. Nomenclature AHI apnea hypopnea index AI apnea index CPAP continuous positive airway pressure NC neck circumference ODI oxygen desaturation index RCT randomized controlled trial MRA mandibular repositioning appliance MRI MSLT OSA PAS RPAS SN-MP TRD magnetic resonance imaging multiple sleep latency test obstructive sleep apnea posterior airway space retroplatal airway space angle between anterior cranial base and mandibular plane tongue retaining device There is also growing evidence linking OSA to longterm cardiovascular morbidity, including hypertension, myocardial infarction, and stroke, and an increased risk of motor vehicle accidents. It is now recognized that OSA is a serious public health problem. Snoring, either as an accompaniment to OSA or in isolation, also imposes a social burden to patients and their bed partners. In broad terms, the treatment of snoring and OSA is aimed at reducing the vulnerability to upper airway collapse during sleep. In the case of OSA, the most commonly used treatment is Continuous Positive Airway Pressure (CPAP), involving the administration of pressurized air to the upper airway via a nasal or face-mask during sleep. This pneumatically splints the airway, thereby preventing collapse. Prior to CPAP, the only effective treatment was tracheostomy to bypass the upper airway obstruction. Whilst CPAP is a highly efficacious treatment in terms of preventing snoring and obstructive events, as well as producing positive outcomes in terms of sleep quality, daytime function and blood pressure, criticism has been leveled at its expense, obtrusive nature and consequent effects on compliance. 3 This has prompted a search for simpler alternatives. One such alternative that has emerged particularly over the last decade is oral appliance therapy, which relies on repositioning of the tongue and mandible in a way that reduces the tendency of the airway to narrow or collapse during sleep. Two broad appliance classes have emerged, namely mandibular repositioning appliances (MRA) and tongue retaining devices. The former are far more commonly used in clinical practice, and the quantity and quality of scientific literature supporting their use is greater than for tongue retaining devices. Hence, this review will focus on the use of MRA in the treatment of snoring and OSA. preliminary studies suggest that the tongue, soft palate, lateral pharyngeal walls, and mandible interact to control airway size, and that mandibular advancement induces complex changes in these structures, resulting in improved airway stability (see Fig. 1). Specifically, MRA have been shown to increase the lateral dimension of the upper airway, 4 to improve velopharyngeal obstruction, 5 and to enhance the cross-sectional area of the velopharynx, in both the lateral and anteroposterior dimensions. 6 Progressive mandibular advancement produces variable adaptive changes in the velopharyngeal and oropharyngeal regions 7 whilst Rationale for use of MRA in snoring and OSA Whilst details of the mechanism of action of MRA in the treatment of snoring and OSA remain uncertain, Figure 1 Schematic diagram of upper airway anatomy (a) during obstructive sleep apnea without MRA and (b) with MRA.
3 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 445 active mandibular advancement causes an increase in upper airway calibre at most levels, and especially at the oropharynx. 8 A decrease in collapsibility of the upper airway has also been shown to occur with MRA. 9 This has raised the possibility of MRA causing neuromuscular activation of upper airway dilator muscles, although evidence supporting such a hypothesis is weak. The attractiveness of this modality of treatment over other modalities relates to its simplicity, portability, lack of noise and need for a power source, and potentially lower cost. This has prompted a concerted research effort over the last decade to define the clinical role of MRA in the treatment of snoring and OSA. Efficacy and effectiveness of MRA treatment Whilst interest in the use of MRA as a treatment for snoring and OSA has been sparked since its inception in the early days of dentofacial orthopedics, its efficacy in the treatment of sleep-disordered breathing has only been rigorously investigated during the last decade. Randomized controlled trials (RCTs) have been undertaken with MRA comparisons made in the short term against no treatment, both active 12,14,15 14,16 19 and non-active oral appliances, and CPAP. 14,20 25 Outcomes have principally focused on polysomnographic parameters, snoring, daytime sleepiness and other major symptoms, and patient preference. More recently, neuropsychological 23 and cardiovascular 26 endpoints have also been explored. At this time, both the short term benefit of MRA in the treatment of upper airway resistance syndrome (UARS), 27 and its comparison to behavioral and surgical strategies for OSA is uncertain as RCTs on the subject are lacking. Short term efficacy RCTs have proven MRA to be of significant benefit in controlling or significantly reducing the number of obstructive breathing events during nocturnal polysomnography in a significant proportion of patients with mild to severe OSA (Table 1). Additionally, both arterial oxygen saturation levels and arousal frequency during sleep have been shown to significantly improve. Subjectively, in both non-apneic snorers and those with OSA, snoring is reported to be either improved or totally abolished, whilst objectively, the frequency and intensity are reduced. The impact of such treatment on symptomatic daytime sleepiness is less well defined, with some studies reporting a significant improvement with MRA, 18,20,23 whilst others have not, 12,15,19,21,22,24,25 irrespective of the therapeutic interval. Objective findings are even less clear as only one RCT has been carried out showing a small but significant improvement in mean sleep latency on the Multiple Sleep Latency Test with MRA compared with a non-active oral appliance (10.3 ^ 0.5 min vs 9.1 ^ 0.5 min). 18 Patients have reported significant improvements in their quality of sleep with MRA. 18,28 Notably, Engleman et al compared MRA to CPAP and found no difference in cognitive performance between treatments. 23 A more recent development in the assessment of health outcomes with MRA has been the detection of a significant reduction in 24-h diastolic blood pressure compared to an inactive oral appliance during a 4-week treatment interval, similar to that achieved with CPAP. 26 With the exception of one study where considerations of appliance design may be of relevance, 23 MRA therapy has been shown to be preferred by patients in comparison to CPAP. 20,22,24,25 However, it is important to note that its clinical application is limited by a lesser overall objective efficacy compared to CPAP, with the exception of the study by Tan et al. who showed no difference in therapeutic benefit between the two treatments, although there was a high variability in their results with the MRA (Table 1). 25 RCTs using an inactive oral appliance as the control treatment have identified an important placebo effect, and this highlights the need for objective assessment of MRA efficacy, particularly in cases of moderate to severe OSA. 18,19 Forty-one percent of 73 patients treated with an inactive oral appliance by Gotsopoulos et al. expressed satisfactory control of OSA symptoms and 49% indicated a desire to continue with such treatment. 18 Using the same concept, Johnston et al. showed a significant reduction in AHI with their MRA compared to the control appliance, but there was no significant difference in symptomatic scores. 19 Long term effectiveness Long-term studies of MRA in the treatment of snoring and sleep apnea suggest a high success rate, 12,29 31 with follow-up periods of 2 5 years (Table 2). About 80% of patients that are initially successfully treated will experience long-term control of OSA using one-piece appliances according to these studies, which range in sample size from 19 to 39 patients. 12,29 31 A similar or slightly lesser percentage of patients will also be satisfied with the longterm effect on snoring. These long-term 12,29 31 results indicate that there is a slight attenuation
4 Table 1 Efficacy of MRA in OSA. 446 First author (year) Study design Study population Inclusion criteria No. recruited (men) Treatment comparison Treatment interval Study sample Treatment effect Percent patients AHI, 10/hr with MRA (and B/SAHI. 10) AHI pre-mra/ MRA (P-value) AHI pre-comp/ comp (P-value) Between treatments (P-value) O Sullivan (1995) Crossover AHI (20/hr or refused/ unable to use CPAP 57 (52) No treatment Split night 51 Not specified 32.2 ^ 28.5/ 17.5 ^ 22.7 Clark (1996) Crossover AHI $15/hr 23 (23) CPAP 2 weeks ^ 14.30/ ^ (0.0001) Ferguson Crossover AHI 15 50/hr 27 (24) CPAP 4 months ^ 13.8/ (1996) 9.7 ^ 7.3 (,0.005) Ferguson Crossover AHI 15 55/hr 24 (19) CPAP 4 months ^ 15.0/ (1997) 14.2 ^ 14.7 (,0.005) Hans (1997) Parallel ^ 28.4/ group 21.1 ^ 21.4 (#0.05) History of loud snoring; AHI, 30; MSLT,5min Bloch (2000) Crossover AHI $5/hr or snoring and arousal index.20/hr; refused/ unable to use CPAP Mehta (2001) Crossover AHI $10/hr and symptoms Engleman (2002) Gotsopoulos (2002) Crossover AHI $5/hr and symptoms Crossover AHI $10/hr and symptoms 24 (83%) Mandibular repositioning appliance 24 (23) MRA and no treatment 2 weeks MRA ðn ¼ 10Þ; control ðn ¼ 8Þ 1 week Herbst** 75 Monobloc** 88 either appliance** 22.6 ^ 3.1*/ 8.7 ^ 1.5* (Herbst) (,0.05) N/A (,0.01) ^ 14.30/ ^ 3.93 (0.001) 17.6 ^ 13.2/ 3.5 ^ 1.6 (,0.005) 23.5 ^ 16.5/ 4.0 ^ 2.2 (,0.005) 36.5 ^ 43.7/ 46.8 ^ 46.9 (.0.05) 22.6 ^ 3.1*/ 7.9 ^ 1.6* (Monobloc) (,0.05) Not reported (,0.05) (,0.01) (#0.0045) 28 (22) Mandibular repositioning appliance and no treatment 1 week ^ 2/14 ^ 2 (,0.0001) 51 CPAP 8 weeks 48 (36) 47** 31 ^ 26/ 31 ^ 26/8 ^ 6 (0.001) 15 ^ 16 not reported not reported 84 Mandibular 4 weeks 73 (59 men) 55 MRA 12 ^ 2* Control 25 ^ 2* (0.0001) repositioning appliance Johnston (2002) Crossover $4% dip in SaO 2 21 (17) Mandibular 4 6 weeks MRA ^ Control ^ (0.011) repositioning appliance Randerath (2002) Crossover AHI 5 30/hr 20 (16) CPAP 6 weeks 20 30** 17.5 ^ 7.7/ 13.8 ^ 11.1 (.0.05) 17.5 ^ 7.7/ 3.2 ^ 2.9 (,0.01) (,0.01) Rose (2002) Crossover Mild OSA 26 (22) MRA and no treatment 6 8 weeks Silencor ðn ¼ 18Þ Activator ðn ¼ 20Þ Not reported (Pre-Silencorw) 16.0 ^ 4.4/ (Silencorw) 7.4^ 5.3 (S p-value not reported) (Pre-activator) 16.2 ^ 4.6/ (Karwetzky activator) 5.5 ^ 3.3 (,0.01) NS S p-value not reported P.A. Cistulli et al.
5 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 447 Not measured Not measured Not measured Not measured No treatment ðn ¼ 34Þ MRA nights 3, ðn ¼ 18Þ; 7, ðn ¼ 16Þ; 28, ðn ¼ 11Þ 50 No treatment 3, 7, and 28 days Smith (2002) Crossover ESS $10; CPAP use $3 months and (4 hrs per night; (4% dips in SaO 2 NS 22.2 ^ 9.6/ 3.1 ^ 2.8 (,0.001) Tan (2002) Crossover AHI,50/hr 24 (20) CPAP 2 months ^ 9.6/ 8.0 ^ 10.9 (,0.001) Treatment effects are presented as Mean (^SD) or *(^SEM). **Number of patients with AHI,10/hr at baseline not stated. AHI, apnea hypopnea index; B/S, baseline; Comp, comparison treatment; CPAP, continuous positive airway pressure; ESS, Epworth sleepiness scale; hr, hour; MRA, mandibular repositioning appliance; MSLT, multiple sleep latency test; N/A, not applicable NS, not significant; OSA, obstructive sleep apnea; S, significant; SaO 2, oxygen saturation; SD, standard deviation; SEM, standard error of the mean. of the effect of the appliance on upper airway patency over time. However, it is important to note that the studied samples are biased in favor of long term treatment successes since they only constitute between 30 and 77% of all originally treated patients, with the remaining patients discontinuing treatment because of poor outcome or failure to attend follow-up. Consequently, the long-term effectiveness of MRA among initially unselected patients is much lower, perhaps below 50% depending on the patients included. The most efficient way to increase the long-term success rate with the appliance is, therefore, to principally select only patients who are particularly likely to respond to this type of treatment, although this is not currently reliable due to a lack of evidence. It is also important to follow-up patients in the longer term in order to exchange the appliance with a new one when needed and to reassess the effect of treatment in patients who experience weight gain or re-develop symptoms of sleep apnea in order to adjust the appliance or recommend another treatment. The main mechanism of the appliance is to mechanically increase the upper airway and reduce pharyngeal collapsibility. Consequently, causes for an attenuation of the treatment effect of MRA over time will be related to factors that alter the mechanical properties of the pharyngeal airway. Based on limited long-term data, the main reasons appear to be deterioration in the condition of the MRA so that it no longer maintains advancement to the prescribed position, 29 or an increase in body weight with reduced upper airway dimensions. 29,32 Further long-term studies of large samples are required to define the factors determining longterm treatment outcome. Long-term use of MRA for snoring and sleep apnea is associated with widening of the pharynx, 33 shortening and thinning of the soft palate and greater flexion of head posture. This is probably partly related to reduced pharyngeal edema due to less soft tissue vibration from snoring. However, it is unknown whether this long-term change in morphology also produces an amelioration of underlying upper airway pathophysiology. The only study to date that has evaluated the change in underlying OSA severity with long-term MRA use suggests no significant change. 29 MRA as an adjuvant treatment for OSA Whilst the focus of this review has been on the use of MRA as a sole treatment for snoring and OSA, there is also scope to use MRA as an adjuvant to other therapies. For example, the combined use of
6 448 P.A. Cistulli et al. Table 2 Long term effectiveness of MRA in OSA and snoring. First author (year) Time (yrs) Sample ðnþ Criteria AHI means (/hr) Long term success in the long term samples (short term success) Inclusion Long term Short term Long term Sleep apnea Reported snoring Initial Long term AHI, 10 AI, 5 þ AHI, 10 ODI, 5or ODI # 50% AHI, 10 þ AHI # 50% With-out With MRA With-out With MRA 18* 4.2 N/A % (100%) N/A N/A Worsening Rose (2002) # AHI, 30 Initial success, attended follow-up,,5 kg weight gain Fransson (2003) ODI $ 5 Continued treatment 15* N/A N/A 3.1 N/A 82% N/A 87% ODI, 5 1.3* N/A N/A 0.8 N/A 95% N/A Walker-Engström , AI, 25 Continued treatment 11* 1.5 N/A 3.2 N/A N/A 63% (78%) Unchanged (2002) Marklund (2001) AHI $ 5 Initial success (17) continued (2) 24** % (79%) N/A 79% (90%) 84% (90%) 74% (100%) AHI, apnea hypopnea index; AI, apnea index; hr, hour; MRA, mandibular repositioning appliance; N/A, not available or incomparable samples; ODI, oxygen desaturation index; *Registrations prior to treatment start. **Nine patients were evaluated prior to treatment start and 10 patients after treatment start when they had been without their devices for one week. No difference in short term treatment effect between those subgroups. CPAP and MRA has been suggested and this could have application in situations where there is a desire to reduce the CPAP pressure required to control OSA, because of the potentially beneficial effect of MRA on airway caliber. Currently, there is little evidence to support this combined use with CPAP. There is also the potential for combining MRA treatment with conservative measures, for example weight loss and nasal decongestants, to produce a superior effect. Again, at this stage there is no scientific evidence to support such an approach, but this is an area that warrants investigation. Patient selection criteria General indications The prescription of any treatment for OSA, including MRA, follows both subjective and objective appraisal. A clinical history, which preferably includes bed partner input, reveals most frequently the presence of nocturnal habitual snoring, nocturnal witnessed apneas, and excessive daytime sleepiness, which often prompt medical consultation in the first instance. However, these features are not solely relied upon for a definitive diagnosis of OSA, as they lack diagnostic sensitivity and specificity. Overnight polysomnography, usually carried out in the laboratory setting, is required to confirm the presence and severity of the condition. Research and clinical experience with MRA in the treatment of snoring and/or sleep apnea is largely restricted to adults, although one RCT in children (mean age 7.1 years) with malocclusion has reported effective control of snoring and OSA. 34 Mandibular repositioning appliances have been demonstrated to be particularly useful in relieving snoring, at least subjectively, 35 and hence nonapneic snorers represent the largest subgroup for which such treatment should be considered. Practice parameters developed by the American Academy of Sleep Medicine recommend their use in OSA only for those patients with mild severity or those who refuse or cannot tolerate CPAP. 36 However, there is growing evidence supporting an expansion of their use in more severe forms of OSA, provided patients are followed cautiously and objective verification of outcome is monitored. There is also emerging evidence of the benefit of MRA in the treatment of upper airway resistance syndrome, 27 although RCTs are lacking. There is currently no known clinical role for MRA in the treatment of other forms of sleep-disordered breathing, including central sleep apnea and hypoventilation syndromes.
7 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 449 From a dental perspective, the presence of temporomandibular dysfunction may be a contraindication to the use of oral appliances, although this should be assessed on a case-by-case basis by a dentist. Insufficient teeth to support the device or the presence of periodontal disease inducing tooth mobility may preclude treatment. Similarly, a limited capacity for mandibular protrusion (,6 mm) has been suggested to be a contraindication, although studies have reported success with lesser degrees of mandibular advancement. 37 Petit et al recently reported a study of 100 consecutive OSA patients in which 34% were assessed to have the presence of these dental contraindications to oral appliance therapy, the authors implying a limitation of the scope of this form of therapy. Supine-dependent OSA Sleep posture has a significant influence on the dimensions and collapsibility of the upper airway. The tongue and soft palate constitutes a large mass of soft tissue, and hence in the supine position gravitational effects cause reduced airway dimensions. Instead, in the lateral position there are usually smaller amounts of soft tissue that exert obstructive forces on the upper airway. Patients with obstructive sleep apnea who change sleep position from lateral to supine reduce their pharyngeal dimensions and increase pharyngeal collapsibility. In addition, these patients experience a larger downwards and backwards movement of their mandibles during sleep-induced muscle relaxation than do healthy subjects. 38 Moreover, men are probably more susceptible to upper airway obstruction during sleep than women, since they undergo a more marked reduction in airway size during posterior movement of the mandible than women. 39 More than half of patients with OSA have airway obstruction primarily in the supine position, and these patients with supine-dependent OSA tend to have less severe disease with better preserved sleep quality, less obesity, 40 and a more normal pharyngeal morphology compared with patients who have OSA in all positions. Patients who snore only in the supine position have been found to be unlikely to suffer from OSA, in contrast to patients who snore also in the lateral position. 41 Hence, it appears that increased frequencies of breathing abnormalities in the non-supine position reflect greater pharyngeal collapsibility. The earliest manifestation of sleep-disordered breathing is snoring in the supine position. This condition evolves into snoring also in the lateral sleep position and the occurrence of apneas in the supine position. According to this hypothesis, the highest pharyngeal collapsibility exists in patients with snoring and apneas in both lateral and supine positions. Patients with supine-dependent OSA have a higher success rate with MRA compared with patients who have OSA in the lateral position. 42,43 Marklund et al. reported an odds ratio of 30 ðp, 0:01Þ for treatment success in patients with supine-dependent OSA, defined as a supine apnea hypopnea index (AHI) $ 10/h in combination with a lateral AHI, 10/h. 42 Analysis of men and women separately in 188 patients with OSA revealed that supine-dependent OSA predicted treatment success only in men. 32 The significant odds ratio for treatment success in that study was 6 for supinedependent OSA in men, when controlled for mandibular displacement, obesity, weight changes, nasal obstruction, smoking and the year in which treatment started. This figure may be compared with a significant odds ratio of 2.5 for mild sleep apnea, defined as an AHI, 20/h. 32 Among women, milder disease related to successful treatment with an odds ratio of 12, controlled for the same variables as for the men. 32 Another important finding in that study was that women were overall more successful with the appliance than men with an odds ratio of 2.5, when controlled for disease severity, supinedependent OSA, body mass index and age of below 50 years compared with above. 32 Hence MRA is particularly indicated in women, and in men with supine-dependent OSA. This is probably explained by a lower pharyngeal collapsibility in these patients, making it easier to achieve a patent airway with the appliance during sleep. Dental and anthropomorphic predictors of outcome Whilst significant progress has been made in proving the efficacy of MRA for OSA, the ability to predict treatment outcome and hence preselect suitable candidates for this treatment option still remains in its early stages. The pre-treatment AHI has been suggested by some as a possible indicator of treatment effect in OSA patients, with generally more severe levels favoring failure, 10,35 although notable exceptions do exist. 17,44 46 The strength of the pre-treatment AHI in the prediction of treatment success with MRA is probably related to factors such as supine-dependency, obesity and differences in jaw and pharyngeal morphology in the studied samples. Cephalometric parameters alone or in unison with other anthropomorphic and polysomnographic characteristics have been considered to improve the ability to predict post treatment AHI. 17,46,47
8 450 P.A. Cistulli et al. Indicators of a successful outcome have been shown by one study to be a shorter soft palate and a decreased distance between the hyoid bone and the mandibular plane, 46 and by another, the combination of a narrower SNB angle, wider SNA angle, shorter soft palate and narrow oropharynx (PAS). 47 The collective effects of a larger retropalatal airway space (RPAS) and larger angle between anterior cranial base and mandibular plane (SN- MP) as determined by cephalometry, a smaller neck circumference (NC), and lower AHI, were shown by Mehta et al. to favour a reduced AHI with their appliance. 17 Liu et al. found a better treatment response in patients who were younger and had a lower body mass index, longer maxilla, smaller oropharynx, smaller overjet, less erupted maxillary molars, and a larger ratio of vertical airway length to cross-sectional area of the soft palate. 48 Whilst collectively these studies suggest that treatment outcome is chiefly related to anatomical characteristics, such data are too limited to form any general recommendations. More sophisticated technology has been recently introduced by Sanner et al. who were able to show with MRI of the pharynx a lack of significant occlusion on performing the Mueller maneuver with MRA in five of their seven treatment successes. In contrast, all six of the treatment failures showed occlusion despite wearing the MRA. 49 By measuring pharyngeal pressure during sleep, Henke et al. found that whilst oropharyngeal collapse had a very favorable response to MRA, velopharyngeal closure did not prevent a favorable response. 50 Although the development of a valid and reliable predictive tool in the recommendation of MRA is warranted for obvious health, social and economic reasons, this may be a difficult task in view of the multifactorial nature of OSA and heterogeneity of patients. Design features and titration procedures MRA designs A multitude of MRA designs have been reported in the literature and are available commercially. It is not the intention of this review to describe specific MRA, but rather to consider general design principles. Most use traditional dental techniques to attach a one- or two-piece appliance to one or both dental arches and vary in design from relatively simple acrylic moldings to appliances incorporating metallic rod and tube fittings, interarch elastic, metal or plastic connectors, or even magnets. 21,45,51 53 There is general consensus that customized appliances are better tolerated and tend to be more effective than the less commonly used prefabricated appliances, but this is not based on research evidence. This requires dental impressions, a protrusive bite registration and construction by a dental laboratory. Little is known about the influence of appliance design on treatment outcome. The principles of MRA design are thought to include the need for good retention, sufficient protrusion and vertical dimension. MRA that permit jaw movement, laterally 52 or vertically, 17,18 may offer advantages in terms of reducing the risk of temporomandibular joint complications and improving patient acceptance. All MRA produce some downward rotation of the mandible, but there are conflicting data on the effect of the degree of bite opening on treatment outcome. A recent randomized controlled study comparing 4 and 14 mm of bite opening suggests that there is little impact on treatment outcome, although minimal bite opening was better tolerated by patients. 54 Titration procedures The conventional approach to MRA treatment usually involves 4 weeks of adaptation to the appliance followed by 2 3 months of incremental titration, so as to maximize tolerance during this initial phase. Details of such a process, including the initial and target amount of mandibular advancement and the rapidity with which incremental changes are made are highly variable between practitioners. The need for such an acclimatization period is considered a drawback of treatment, particularly in situations where rapid initiation of treatment is warranted. Determination of the amount of mandibular advancement required to prevent OSA in a given patient is a matter of trial and error, as there does not appear to be a correlation between the amount of advancement and therapeutic effect. 17,50 Reliance on symptomatic response alone can be misleading because of the apparent placebo effect associated with MRA. 17,18 A recent study reported the feasibility of single-night MRA titration using a hydraulically controlled appliance. 55 The benefit of such a process for titration is the potential to immediately ascertain the likelihood of treatment success as well as the dose of mandibular advancement required in the individual case. This would avoid the need for an acclimatization period, and potential wastage of resources in patients for whom MRA proves ineffective. However, the potential difficulty of achieving the required mandibular
9 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 451 advancement without inducing discomfort on the first night of use may be a limitation. Adverse effects Side-effects and complications The reported adverse effects associated with MRA 22,56 60 have so far been of limited magnitude. Almost 90% of patients who continue treatment on a regular basis consider that the treatment benefits outweigh any adverse effects. 61 Nevertheless, discomfort from the appliance is the major cause for discontinuation of treatment or poor compliance for about 20 50% of initially treated patients. 32,61,62 This may be exacerbated by using a single position appliance or too rapid titration of the appliance. The usefulness of the appliance will therefore be very much dependent on the patients own experiences or their knowledge about painful or otherwise troublesome side-effects. The introduction of an appliance in the mouth will produce temporary increased salivation and may also induce pain in the teeth or jaws in relation to the magnitude of the forces generated. MRA are derived from functional orthodontic appliances. To prevent airway collapse during sleep, these appliances hold the mandible in a forward and vertically opened position. The MRA is anchored to the dentition, but may also extend over the oral mucosa in order to increase the area of retention. Even so, the teeth are loaded with permanent forces when the appliance is worn at night. The appliance generates reciprocal forces on the teeth and jaws due to its design. The appliance therefore transmits labially directed forces against the lower incisors and palatally directed forces against the upper incisors as the mandible attempts to go back to its normal postural position. Consequently, teeth may change their inclinations and the whole lower jaw may also be displaced during longer term treatment with MRA for snoring and obstructive sleep 12,33,56 59,63,64 apnea. Short term The majority of the patients will experience one or more short-term side-effects such as increased salivation or dryness, discomfort from the teeth or gums, or a perception of an abnormal bite from the appliance. 17,35,58,61 These side-effects are particularly common in patients who discontinue during the first year of treatment. 61,62 Consequently, it is especially important to continuously follow-up new patients and adjust their appliances in order to relieve side-effects. It is also important to maximize the effect of the appliance on snoring and symptoms when indicated, since patients who do not have a sufficient treatment effect are likely to discontinue treatment and experience more dominating side-effects. 62 According to clinical experience, even small adjustments may enhance the tolerability to the appliance and increase the chance of success. The patients should be encouraged to make regular contact with the treating dental practitioner whenever the appliance is inconvenient or does not relieve symptoms. Long term Jaw and teeth discomfort, salivation problems and experiences of an abnormal bite become less prominent with time. 22,61 In contrast, the orthodontic effects on the teeth and jaws are side-effects that become progressively more pronounced during long-term treatment, often 59,63 65 without the patient being aware of them. These adverse events from MRA appear to be quite variable according to the studies reported to date. The predicted orthodontic side-effects with a backward movement of the upper front teeth and a forward movement of the lower front teeth and mandible are more or less obvious in the various studies. Cephalometric X-ray evaluations have revealed that the upper incisors will tip posteriorly with average changes of between and ,64,65 or be unchanged, 33,63 and that the lower incisors will incline anteriorly with average changes of between 1.5 and ,64,65 or be unchanged after about 2 years treatment. 58,63 The mandible may also move forward or downwards during treatment 63,64 or undergo a posterior rotation resulting in a slight backward movement of the mandibular position. 33,58 Robertson found that the mandibular condyle relocates downwards, which in turn produces an increase in the lower face height during treatment. There was no sagittal change in jaw position in that study. 64 In contrast, Bondemark has described increased mandibular prognathism by the appliance, with up to 2 mm anterior movement of the mandible or a mean of 0.48 increase in the SNB-angle, 63 but the significance of this minor change is questionable. The influence of MRA on the upper jaw (SNA) is generally 33,58,63 65 small and clinically insignificant. These cephalometric findings are confirmed in analysis of plaster casts, where average changes are in general minor ,65 A more than 1 mm decrease in overjet has, however, been noticed in between 14 and 26% of longer term treated patients. Some patients may experience extreme changes in their occlusion during long-term treatment with
10 452 P.A. Cistulli et al. MRA. Reductions in overjet up to 3 mm and posterior bite openings as large as 5 mm have been observed in individual patients after 2 years or less. 56,59,64 Moreover, retroclination of the upper incisors with as much as 88 and proclination of the lower front teeth by 138 have been reported. Age, gender, treatment time, dental occlusion or the skeletal dentofacial pattern have so far not explained the differences in morphological changes in studies, involving samples of about 30 patients of between 27 and 80 years of age. 63,65 It has been suggested that the use of a soft elastomeric appliance that extends over the alveolar processes may reduce the mesial shift in occlusion compared with a hard acrylic appliance that is only fixed to the teeth. 59 Marklund et al. found that only half of patients treated with soft elastomeric appliances compared with those treated with hard acrylic appliances were subjected to a decrease in overjet of more than 1 mm. 59 It is likely that a number of factors such as periodontal health, the inclination of front teeth, the jaw morphology, or MRA compliance influence the magnitude of these long-term side-effects. Larger studies are needed to more clearly define the importance of these various factors. Robertson has proposed the potential chronology for various morphological adverse events that can occur during treatment. 64 During the first 6 months, the mandibular condyle may be displaced downwards, which in turn reduces the overbite and overjet and increases the face height. Thereafter, the upper front teeth may undergo a posterior tipping, which progressively decreases the overjet and overbite. After years of treatment proclination of lower incisors with a mean of 4.98 becomes evident, and this produces the greatest reductions in overjet and overbite. 64 Consequently, it is important to continuously monitor the bite among patients treated with MRA, since dental side-effects may develop at various stages of longterm treatment. The appearance of more marked dental side-effects may hinder the continued use of the appliance and, on occasions, an alternative treatment may need to be considered. Clinical experience suggests that the bite changes diminish when MRA is no longer used, although more permanent dental side-effects have been reported. 59,64 Medicolegal issues There is growing evidence of medicolegal activity in some jurisdictions in relation to OSA diagnosis and treatment, including issues related to driver safety and life insurance risk. Many driver licensing authorities across the world recognize that OSA may impair driver safety and have developed guidelines restricting access to driver licenses for patients with untreated OSA. There is good evidence of a higher risk of motor vehicle accidents among OSA patients compared with controls, 67 and CPAP treatment appears to normalize this risk. Similar evidence for MRA do not yet exist, although one would expect that driving risk on treatment would be related to the extent of residual OSA. Given the apparent placebo effect noted with MRA, it is critical to objectively verify treatment outcome when driver safety, particularly in the commercial driver context, is an issue. This may include the use of daytime vigilance tests in appropriate circumstances. Furthermore, given the current requirement for an acclimatization period of some months, MRA are far from ideal in circumstances where rapid initiation of effective treatment is required for a sleepy driver, and hence it is best to use CPAP in such circumstances. With growing experience and awareness of the dental complications of MRA treatment, albeit generally minor, both medical and dental clinicians involved in the care of these patients have an obligation to comply with appropriate informed consent procedures. This is becoming very important in the context of long-term MRA related side-effects, which may encompass permanent orthodontic changes and consequent medicolegal concerns. Treatment compliance The acceptance rate of MRA is moderately high and this appears to be related to the simplicity of the 15,17 22 treatment itself. However, the interpretation of adherence rates is subject to limitation by over-inflated figures reported as a result of a lack of intention to treat analyses and most importantly, unlike CPAP, a lack of objective data for verification. The main reasons for patient refusal to initiate or continue with treatment are a lack of selfperceived efficacy or MRA related side-effects. Whilst reported usage is initially high, 18,19 there is a declining trend over time. Reported compliance figures after 1 year of treatment have varied from 55 to 82%. 30,32,61,68 Clark et al. reported 48% of patients continuing with their MRA after 2 years. 68 Pancer et al. indicated that 76% of their subjects persisted with treatment after an average of 31 ^ 18 months. 69 At 4 years, Walker-Engstrom reported adherence to treatment by 62% of their patients, 30 and at 5 years Marklund et al. reported
11 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 453 Figure 2 Clinical protocol for MRA in OSA (adapted from Lowe ). usage maintenance by 70% of patients. 29 Lowe et al., 52 who used a covert compliance monitor embedded in their MRA, revealed an average nightly usage rate of 6.8 h which is comparable to both diary data from a 4-week trial 18 and self-reported information from observational studies. 30,61,62 Acceptance and compliance rates of MRA in comparison to CPAP for OSA have been found to vary, with no reported difference between treatments 20,23 to superior compliance with MRA. 22,24 Comparison with other treatments The overall benefit of a treatment is related to the product of its effectiveness and the patient s adherence to treatment, the latter being determined to a large extent by the acceptability of the treatment to the patient, and often the bed partner. Whilst CPAP is unquestionably a more effective treatment for OSA, there is now strong evidence from RCTs that patients find MRA a more
12 454 P.A. Cistulli et al. acceptable treatment than CPAP 20 22,24,25 and that for an important subset of patients (30 40%) MRA treatment is as effective as CPAP. 17,18 This gives rise to the question of whether greater adherence to the less effective MRA treatment could have an equivalent cumulative effect as the use of CPAP for less than the entire sleep period. Whilst this comparison may seem unjustified given the lack of evidence on MRA adherence compared to objective data on CPAP usage, this remains an important and unresolved question. Clinical pathways and education Integrative care appears to be central to the successful management of patients with snoring and OSA for whom MRA therapy is indicated. This involves a multidisciplinary approach involving a proficient sleep and dental team. Interdisciplinary communication and treatment planning via a coordinated care pathway would most likely enable an efficient process in the care of these patients. Patient access to and knowledge of such a process is essential in optimizing patient outcomes. Moreover, the development and implementation of evidence based clinical practice guidelines in conjunction with continuing education of the respective disciplines is key in achieving patient focused goals. Whilst to date no formal integrative care pathway has been implemented in the case of MRA for OSA, the Academy of Dental Sleep Medicine has suggested its own clinical protocol (Fig. 2). 70 Such a pathway would require evaluation for its clinical effectiveness and ongoing review for further development. Trends in usage Anecdotal evidence suggests increasing awareness about MRA for snoring and OSA, both among clinicians and patients. This trend appears to apply to North America, Europe, China, Japan, and Australia. In Sweden, the number of prescribed MRA for sleep apnea per annum has increased 3-fold since During this period, medically indicated MRA treatment has become incorporated in the general health care system, resulting in lower fees for the patients and registrations of MRA treatments. In some jurisdictions of North America, up to 50% of patients have some form of insurance that offsets the cost of oral appliances. However, clear evidence about current usage patterns, the expertise of the treating dentists, the clinical pathways being used, the types of appliances, and rigor of follow-up procedures are not available. In 1997, Loube and Strauss reported on a survey of 355 dentists who were members of the American Sleep Disorders Dental Society. 71 The response rate was low (35%), but the data indicated a relatively modest usage of oral appliances among these motivated dentists, with a median of 27 OSA patients per annum. The level of knowledge was mixed, with follow-up polysomnography to objectively evaluate outcome being undertaken infrequently. 71 It would be valuable for further studies of this type to be conducted in order to glean a better picture of current usage of appliances, with the aim of designing interventions to improve clinical practice in this area. There are a multitude of appliances available commercially, but there is little scientific evidence on which to base treatment decisions regarding the particular design to use in the individual patient. Despite a growing momentum in research on MRA in snoring and OSA, only relatively few of the available designs have been subjected to the level of scientific scrutiny upon which sound clinical practice can be based. Unlike CPAP treatment, which Practice points MRA are increasingly being used in clinical practice to treat snoring and OSA. MRA are indicated as first line treatment for snoring. MRA are effective in a substantial proportion of patients with mild to moderate OSA, and lesser proportion of those with severe OSA. Most OSA patients are improved with MRA treatment, with up to 40% achieving a complete response (defined as a return of AHI to,5/h) with some appliances. Supine-dependent OSA in men and female gender appear to be strong predictors of treatment success with MRA. A multidisciplinary approach, involving collaboration between medical (e.g. pulmonologist, sleep physician, family physician) and dental practitioners, to diagnosis and treatment is recommended. Short-term side-effects with MRA are common, but usually minor and transient, and can usually be managed with appropriate dental follow-up. Long-term dental changes with MRA appear to be common, but are generally minor.
13 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 455 Patients must be informed about this prior to commencement of treatment, and the decision to discontinue treatment in the event of such complications should be made in association with the patients, taking into account their desire to change to another treatment. Long-term dental and medical follow-up is essential in order to exchange or adjust the appliance or recommend another treatment in patients who gain weight or experience increased symptoms. Reseach agenda Further studies to determine the impact of MRA on health outcomes. Identify predictors of treatment outcome with MRA. Identify methods to control dental sideeffects with MRA in order to increase its use and the number of successfully treated patients. Determine the influence of design features on treatment outcome and side-effects. Further studies to develop single night titration of MRA for use in clinical practice. Research on the cost-effectiveness of treatment, particularly in comparison to CPAP. Evaluation of clinical pathways for the delivery of oral appliance treatment. can be considered a generic modality, it is possible that MRA effectiveness varies depending on design features, and hence research data cannot be reasonably extrapolated to the modality at large. Acknowledgements Peter Cistulli and Helen Gotsopoulos have received research support from the National Health and Medical Research Council of Australia. Marie Marklund has received research support from The Swedish Association for Heart and Lung Patients and the Swedish Dental Society. Alan Lowe has received research support from various Canadian provincial and federal granting agencies. References 1. Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S. The occurrence of sleep disordered breathing among middleaged adults. N Engl J Med 1993; 328: Ohayon MM, Guilleminault C, Priest RG, Caulet M. Snoring and breathing pauses during sleep: telephone interview survey of a United Kingdom population sample. BMJ 1997; 314: White J, Cates C, Wright J. Continuous positive airways pressure for obstructive sleep apnoea. Cochrane Database Syst Rev 2004;. 4. Schwab RJ et al. Upper airway soft tissue structural changes with a dental appliance in apneics. Am J Respir Crit Care Med 1996; 153: A Ishida M, Inoue Y, Suto Y et al. Mechanisms of action and therapeutic indication of prosthetic mandibular advancement in obstructive sleep apnea syndrome. Psychiatry Clin Neurosci 1998; 52: Ryan CF, Love LL, Peat D, Fleetham JA, Lowe AA. Mandibular advancement oral appliance therapy for obstructive sleep apnoea: effect on awake calibre of the velopharynx. Thorax 1999; 54: L Estrange PR, Battagel JM, Harkness B, Spratley MH, Nolan PJ, Jorgensen GI. A method of studying adaptive changes of the oropharynx to variation in mandibular position in patients with obstructive sleep apnoea. J Oral Rehab 1996; 23: Gao XM, Zeng XL, Fu MK, Huang XZ. Magnetic resonance imaging of the upper airway in obstructive sleep apnea before and after oral appliance therapy. Chin J Dent Res 1999; 2: Ng AT, Gotsopoulos H, Qian J, Cistulli PA. Effect of oral appliance therapy on upper airway collapsibility in obstructive sleep apnea. Am J Respir Crit Care Med 2003; 168: O Sullivan RA, Hillman DR, Mateljan R, Pantin C, Finucane KE. Mandibular advancement splint: an appliance to treat snoring and obstructive sleep apnea. Am J Respir Crit Care Med 1995; 151: Stradling JR, Negus TW, Smith D, Langford B. Mandibular advancement devices for the control of snoring. Eur Respir J 1998; 11: Rose EC, Barthlen GM, Staats R, Jonas IE. Therapeutic efficacy of an oral appliance in the treatment of obstructive sleep apnea: a 2-year follow-up. Am J Orthod Dentofacial Orthop 2002; 121: Smith DM, Stradling JR. Can mandibular advancement devices be a satisfactory substitute for short term use in patients on nasal continuous positive airway pressure? Thorax 2002; 57: Lim J, Lasserson TJ, Fleetham J, Wright J. Oral appliances for obstructive sleep apnoea. Cochrane Database Syst Rev 2004;. 15. Bloch KE, Iseli A, Zhang JN, Xie X, Kaplan V, Stoeckli PW, Russi EW. A randomized, controlled crossover trial of two oral appliances for sleep apnea treatment. Am J Respir Crit Care Med 2000; 162: Hans MG, Nelson S, Luks VG. Comparison of two dental devices for treatment of obstructive sleep apnea syndrome (OSAS). Am J Orthod Dentofacial Orthop 1997; 111: *17. Mehta A, Qian J, Petocz P, Darendeliler MA, Cistulli PA. A randomized, controlled study of a mandibular advancement splint for obstructive sleep apnea. Am J Respir Crit Care Med 2001; 163:
14 456 P.A. Cistulli et al. p The most important references are denoted by an asterisk. *18. Gotsopoulos H, Chen C, Qian J, Cistulli PA. Oral appliance therapy improves symptoms in obstructive sleep apnea: a randomized, controlled trial. Am J Respir Crit Care Med 2002; 166: Johnston CD, Gleadhill IC, Cinnamond MJ, Gabbey J, Burden DJ. Mandibular advancement appliances and obstructive sleep apnoea: a randomized clinical trial. Eur J Orthod 2002; 24: *20. Ferguson KA, Ono T, Lowe AA, Keenan SP, Fleetham JA. A randomized crossover study of an oral appliance vs nasal continuous positive airway pressure in the treatment of mild moderate obstructive sleep apnea. Chest 1996; 109: *21. Clark GT, Blumenfeld I, Yoffe N, Peled E, Lavie P. A crossover study comparing the efficacy of CPAP with anterior mandibular positioning devices on patients with obstructive sleep apnoea. Chest 1996; 109: *22. Ferguson KA, Ono T, Lowe AA, al-majed S, Love LL, Fleetham JA. A short term controlled trial of an adjustable oral appliance for the treatment of mild to moderate obstructive sleep apnoea. Thorax 1997; 52: Engleman HM, McDonald JP, Graham D, Lello GE, Kingshott RN, Coleman EL, Mackay TW, Douglas NJ. Randomized crossover trial of two treatments for sleep apnea/hypopnea syndrome: continuous positive airway pressure and mandibular repositioning splint. Am J Respir Crit Care Med 2002; 166: Randerath WJ, Heise M, Hinz R, Ruehle KH. An individually adjustable oral appliance vs continuous positive airway pressure in mild to moderate obstructive sleep apnea syndrome. Chest 2002; 122: Tan YK, L Estrange PR, Luo YM, Smith C, Grant HR, Simonds AK, Spiro SG, Battagel JM. Mandibular advancement splints and continuous positive airway pressure in patients with obstructive sleep apnoea: a randomized cross-over trial. Eur J Orthod 2002; 24: Gotsopoulos H, Kelly JJ, Cistulli PA. Oral appliance therapy reduces blood pressure in obstructive sleep apnea syndrome: a randomised controlled trial. Sleep 2004;. In press. 27. Yoshida K. Oral device therapy for the upper airway resistance syndrome patient. J Prosthet Dent 2002; 87: Cameron DA, Lyons MF, Fox DL, Banham SW. Pilot study of a semi-flexible intra-oral appliance for the control of snoring. Br Dent J 1998; 185: Marklund M, Sahlin C, Stenlund H, Persson M, Franklin KA. Mandibular advancement device in patients with obstructive sleep apnea: long-term effects on apnea and sleep. Chest 2001; 120: Walker-Engström M-L, Tegelberg Å, Wilhelmsson B. 4-year follow-up of treatment with dental appliance or uvulopalatopharyngoplasty in patients with obstructive sleep apnea. A randomized study. Chest 2002; 121: *31. Fransson AMC, Tegelberg Å, Leissner L. Effects of a mandibular protruding device on the sleep of patients with obstructive sleep apnea and snoring problems: a 2-year follow-up. Sleep Breath 2003; 7: *32. Marklund M, Stenlund H, Franklin KA. Mandibular advancement devices in 630 men and women with obstructive sleep apnea and snoring-tolerability and predictors of treatment success. Chest 2004; 125: Fransson AM, Tegelberg A, Svenson BA, Lennartsson B, Isacsson G. Influence of mandibular protruding device on airway passages and dentofacial characteristics in obstructive sleep apnea and snoring. Am J Orthod Dentofacial Orthop 2002; 122: Villa MP, Bernkopf E, Pagani J, Broia V, Montesano M, Ronchetti R. Randomized controlled study of an oral jaw-positioning appliance for the treatment of obstructive sleep apnea in children with malocclusion. Am J Respir Crit Care Med 2002; 165: *35. Schmidt-Nowara W, Lowe A, Wiegand L, Cartwright R, Perez- Guerra F, Menn S. Oral appliances for the treatment of snoring and obstructive sleep apnea: a review. Sleep 1995; 18: American Sleep Disorders Association, Practice parameters for the treatment of snoring and obstructive sleep apnea with oral appliances. Sleep 1995; 18: Petit F, Pepin J, Bettega G, Sadek H, Raphael B, Levy P. Mandibular advancement devices: rate of contraindications in 100 consecutive obstructive sleep apnea patients. Am J Respir Crit Care Med 2002; 166: Miyamoto K, Özbek MM, Lowe AA. Mandibular posture during sleep in patients with obstructive sleep apnoea. Arch Oral Biol 1999; 44: Mohsenin V. Effects of gender on upper airway collapsibility and severity of obstructive sleep apnea. Sleep Medicine 2003; 4: Oksenberg A, Silverberg DS, Arons E, Radwan H. Positional vs nonpositional obstructive sleep apnea patients. Antromorphic, noctrurnal polysomnographic, and multiple sleep latency test data. Chest 1997; 112: Nakano H, Ikeda T, Hayashi M, Ohshima E, Onizuka A. Effects of body position on snoring in apneic and nonapneic snorers. Sleep 2003; 26: *42. Marklund M, Persson M, Franklin KA. Treatment success with a mandibular advancement device is related to supinedependent sleep apnea. Chest 1998; 114: Yoshida K. Influence of sleep posture on response to oral appliance therapy for sleep apnea syndrome. Sleep 2001; 24: Lowe A, Fleetham J, Ryan F. Effects of a mandibular repositioning appliance used in the treatment of obstructive sleep apnea on tongue muscle activity. Prog Clin Biol Res 1990; 345: Clark GT, Arand D, Chung E, Tong D. Effect of anterior mandibular positioning on obstructive sleep apnoea. Am Rev Respir Dis 1993; 147: Eveloff SE, Rosenberg CL, Carlisle CC, Millman RP. Efficacy of a Herbst mandibular advancement device in obstructive sleep apnea. Am J Respir Crit Care Med 1994; 149: Mayer G, Meier-Ewert K. Cephalometric predictors for orthopaedic mandibular advancement in obstructive sleep apnoea. Eur J Orthod 1995; 17: Liu Y, Lowe AA, Fleetham JA, Park Y-C. Cephalometric and physiological predictors of the efficacy of an adjustable oral appliance for treating obstructive sleep apnea. Am J Orthod Dentofacial Orthop 2001; 120: Sanner BM, Heise M, Knoben B. MRI of the pharynx and treatment efficacy of a mandibular advancement device in obstructive sleep apnoea syndrome. Eur Respir J 2002; 20: Henke KG, Frantz DE, Kuna ST. An oral elastic mandibular advancement device for obstructive sleep apnea. Am J Respir Crit Care Med 2000; 161: Nakazawa Y, Sakamoto T, Yasutake R, Yamaga K, Kotorii T, Miyahara Y, Ariyoshi Y, Kameyama T. Treatment of sleep apnea with prosthetic mandibular advancement (PMA). Sleep 1992; 15: *52. Lowe AA, Sjoholm TT, Ryan CF, Fleetham JA, Ferguson KA,
15 Treatment of snoring and obstructive sleep apnea with mandibular repositioning appliances 457 Remmers JE. Treatment, airway and compliance effects of a titratable oral appliance. Sleep 2000; 23: Gavish A, Vardimon AD, Rachima H, Bloom M, Gazit E. Cephalometric and polysomnographic analyses of functional magnetic system therapy in patients with obstructive sleep apnea. Am J Orthod Dentofacial Orthop 2001; 120: Pitsis A, Darendeliler MA, Gotsopoulos H, Petocz P, Cistulli PA. Effect of vertical dimension on efficacy of mandibular advancement splint therapy in obstructive sleep apnea. Am J Respir Crit Care Med 2002; 166: Petelle B, Vincent G, Gagnadoux F, Rakotonanahary D, Meyer B, Fleury B. One-night mandibular advancement titration for obstructive sleep apnea syndrome: a pilot study. Am J Respir Crit Care Med 2002; 165: Pantin CC, Hillman DR, Tennant M. Dental side effects of an oral device to treat snoring and obstructive sleep apnea. Sleep 1999; 22: Bondemark L, Lindman R. Craniomandibular status and function in patients with habitual snoring and obstructive sleep apnoea after nocturnal treatment with a mandibular advancement splint: a 2-year follow-up. Eur J Orthod 2000; 22: Fritsch KM, Iseli A, Russi EW. Side-effects of mandibular advancement devices for sleep apnea treatment. Am J Respir Crit Care Med 2001; 164: Marklund M, Franklin KA, Persson M. Orthodontic side-effects of mandibular advancement devices during treatment of snoring and sleep apnoea. Eur J Orthod 2001; 23: Rose E, Staats R, Virchow C, Jonas IE. comparative study of two mandibular advancement appliances for the treatment of obstructive sleep apnoea. Eur J Orthod 2002; 24: Shadaba A, Battagel JM, Owa A. Evaluation of the Herbst mandibular advancement splint in the management of patients with sleep-related breathing disorders. Clin Otolaryngol 2000; 25: McGown AD, Makker HK, Battagel JM, L Estrange PR, Grant HR, Spiro SG. Long-term use of mandibular advancement splints for snoring and obstructive sleep apnoea: a questionnaire survey. Eur Respir J 2001; 17: Bondemark L. Does 2 years noctrurnal treatment with a mandibular advancement splint in adult patients with snoring and OSAS cause a change in the posture of the mandible? Am J Orthod Dentofacial Orthop 1999; 116: Robertson CJ. Dental and skeletal changes associated with long term mandibular advancement. Sleep 2001; 24: Rose EC, Staats R, Virchow CJ. Occlusal and skeletal effects of an oral appliance in the treatment of obstructive sleep apnea. Chest 2002; 122: Teran-Santos J, Jimenez-Gomez A, Cordero-Gueva J. The association between sleep apnea and the risk of traffic accidents. N Engl J Med 1999; 340: Clark GT, Sohn JW, Hong CN. Treating obstructive sleep apnea and snoring: assessment of an anterior mandibular positioning device. J Am Dent Assoc 2000; 131: Pancer J, Al-Faifi S, Al-Faifi M. Evaluation of variable mandibular advancement appliance for treatment of snoring and sleep apnea. Chest 1999; 116: Lowe AA. Oral appliances for sleep breathing disorders. In: MH Kryger, T Roth, WC Dement (eds.) Principles and practice of sleep medicine, 3rd ed. Philadelphia, PA: Saunders 2000; Loube DI, Strauss AM. Survey of oral appliance practice among dentists treating obstructive sleep apnoea patients. Chest 1997; 111:
ROLE OF ORAL APPLIANCES TO TREAT OBSTRUCTIVE SLEEP APNEA
 1 ROLE OF ORAL APPLIANCES TO TREAT OBSTRUCTIVE SLEEP APNEA There are three documented ways to treat obstructive sleep apnea: 1. CPAP device 2. Oral Appliances 3. Surgical correction of nasal and oral obstructions
1 ROLE OF ORAL APPLIANCES TO TREAT OBSTRUCTIVE SLEEP APNEA There are three documented ways to treat obstructive sleep apnea: 1. CPAP device 2. Oral Appliances 3. Surgical correction of nasal and oral obstructions
Arlington Dental Associates Ira Stier DDS PC 876 Dutchess Tpk 2 Lafayette Ct. Poughkeepsie, NY 12603 Fishkill, NY 12524 845-454-7023 845-896-4977
 Home Sleep Test Liability Form Study Equipment Due: @ I, accept responsibility for the sleep monitoring device while it is in rny possession. I understand that if I fail to return the device or I return
Home Sleep Test Liability Form Study Equipment Due: @ I, accept responsibility for the sleep monitoring device while it is in rny possession. I understand that if I fail to return the device or I return
Underwriting Sleep Apnea
 Underwriting Sleep Apnea Joel Weiner, MD, FLMI April 29, 2014 WAHLU The Northwestern Mutual Life Insurance Company Milwaukee, WI A Brief Survey Before We Get Started The Weiner Sleepiness Scale How likely
Underwriting Sleep Apnea Joel Weiner, MD, FLMI April 29, 2014 WAHLU The Northwestern Mutual Life Insurance Company Milwaukee, WI A Brief Survey Before We Get Started The Weiner Sleepiness Scale How likely
Diagnosis and Treatment
 Sleep Apnea: Diagnosis and Treatment Sleep Apnea Sleep Apnea is Common Dangerous Easily recognized Treatable Types of Sleep Disordered Breathing Apnea Cessation of airflow > 10 seconds Hypopnea Decreased
Sleep Apnea: Diagnosis and Treatment Sleep Apnea Sleep Apnea is Common Dangerous Easily recognized Treatable Types of Sleep Disordered Breathing Apnea Cessation of airflow > 10 seconds Hypopnea Decreased
Changes in the Evaluation and Treatment of Sleep Apnea
 Changes in the Evaluation and Treatment of Sleep Apnea Joseph DellaValla, MD FACP Medical Director Center for Sleep Medicine At Androscoggin Valley Hospital Sleep Related Breathing Problems Obstructive
Changes in the Evaluation and Treatment of Sleep Apnea Joseph DellaValla, MD FACP Medical Director Center for Sleep Medicine At Androscoggin Valley Hospital Sleep Related Breathing Problems Obstructive
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: DIAGNOSIS OF SLEEP APNEA IN ADULTS DATE: 5/9/2013 HERC COVERAGE GUIDANCE The following diagnostic tests for Obstructive Sleep Apnea (OSA) should
Snoring and Obstructive Sleep Apnea (updated 09/06)
 Snoring and Obstructive Sleep Apnea (updated 09/06) 1. Define: apnea, hypopnea, RDI, obstructive sleep apnea, central sleep apnea and upper airway resistance syndrome. BG 2. What are the criteria for mild,
Snoring and Obstructive Sleep Apnea (updated 09/06) 1. Define: apnea, hypopnea, RDI, obstructive sleep apnea, central sleep apnea and upper airway resistance syndrome. BG 2. What are the criteria for mild,
MODULE. POSITIVE AIRWAY PRESSURE (PAP) Titrations
 MODULE POSITIVE AIRWAY PRESSURE (PAP) Titrations POSITIVE AIRWAY PRESSURE (PAP) TITRATIONS OBJECTIVES At the end of this module the student must be able to: Identify the standards of practice for administering
MODULE POSITIVE AIRWAY PRESSURE (PAP) Titrations POSITIVE AIRWAY PRESSURE (PAP) TITRATIONS OBJECTIVES At the end of this module the student must be able to: Identify the standards of practice for administering
Removable appliances II. Functional jaw orthopedics
 Removable appliances II. Functional jaw orthopedics Melinda Madléna DMD, PhD Associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification
Removable appliances II. Functional jaw orthopedics Melinda Madléna DMD, PhD Associate professor Department of Pedodontics and Orthodontics Faculty of Dentistry Semmelweis University Budapest Classification
Oral Appliances for Snoring and Obstructive Sleep Apnea: A Review
 REVIEW Oral Appliances for Snoring and Obstructive Sleep Apnea: A Review Kathleen A. Ferguson, MD 1 ; Rosalind Cartwright, PhD 2 ; Robert Rogers, DMD 3 ; Wolfgang Schmidt-Nowara, MD 4 1 Division of Respirology,
REVIEW Oral Appliances for Snoring and Obstructive Sleep Apnea: A Review Kathleen A. Ferguson, MD 1 ; Rosalind Cartwright, PhD 2 ; Robert Rogers, DMD 3 ; Wolfgang Schmidt-Nowara, MD 4 1 Division of Respirology,
Raising Sleep Apnea Awareness:
 Raising Sleep Apnea Awareness: Among People with Diabetes in North Carolina, 2012 People with diabetes have more sleep problems than people without diabetes in the same age, sex, and race/ethnicity group.
Raising Sleep Apnea Awareness: Among People with Diabetes in North Carolina, 2012 People with diabetes have more sleep problems than people without diabetes in the same age, sex, and race/ethnicity group.
Treatment of Obstructive Sleep Apnea (OSA)
 MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
Clinical Practice Guideline For Orthodontics
 Clinical Practice Guideline For Orthodontics MOH- Oral Health CSN -Orthodontics -2010 Page 1 of 15 Orthodontic Management Guidelines 1. Definitions: Orthodontics is the branch of dentistry concerned with
Clinical Practice Guideline For Orthodontics MOH- Oral Health CSN -Orthodontics -2010 Page 1 of 15 Orthodontic Management Guidelines 1. Definitions: Orthodontics is the branch of dentistry concerned with
About Sleep Apnea ABOUT SLEEP APNEA
 ABOUT SLEEP APNEA About Sleep Apnea What is Sleep Apnea? Sleep Apnea (from Greek, meaning "without breath") is one of the most common sleep disorders in which breathing stops and then restarts again recurrently
ABOUT SLEEP APNEA About Sleep Apnea What is Sleep Apnea? Sleep Apnea (from Greek, meaning "without breath") is one of the most common sleep disorders in which breathing stops and then restarts again recurrently
Executive Summary. An American Academy of Sleep Medicine and American Academy of Dental Sleep Medicine Clinical Practice Guideline
 Executive Summary Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2015 An American Academy of Sleep Medicine and American
Executive Summary Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2015 An American Academy of Sleep Medicine and American
DENTAL SLEEP PRACTICE
 DENTAL SLEEP PRACTICE You ve decided to add sleep dentistry as a segment of your practice services - here are the basics to ensure success in treating obstructive sleep apnea (OSA) patients. CONTENT 1
DENTAL SLEEP PRACTICE You ve decided to add sleep dentistry as a segment of your practice services - here are the basics to ensure success in treating obstructive sleep apnea (OSA) patients. CONTENT 1
Acknowledgements. Dental Management of Obstructive Sleep Apnea in a Maxillofacial Prosthodontic Practice. Transfer of Information
 Dental Management of Obstructive Sleep Apnea in a Maxillofacial Prosthodontic Practice Alvin G. Wee, BDS, MS, MPH Associate Professor and Director Division of Oral Facial Prosthetics / Dental Oncology
Dental Management of Obstructive Sleep Apnea in a Maxillofacial Prosthodontic Practice Alvin G. Wee, BDS, MS, MPH Associate Professor and Director Division of Oral Facial Prosthetics / Dental Oncology
Polysomnography in Patients with Obstructive Sleep Apnea. OHTAC Recommendation. Polysomnography in Patients with Obstructive Sleep Apnea
 OHTAC Recommendation Polysomnography in Patients with Obstructive Sleep Apnea June 16, 2006 1 The Ontario Health Technology Advisory Committee (OHTAC) met on June 16, 2006 and reviewed a health technology
OHTAC Recommendation Polysomnography in Patients with Obstructive Sleep Apnea June 16, 2006 1 The Ontario Health Technology Advisory Committee (OHTAC) met on June 16, 2006 and reviewed a health technology
Does Depression affect compliance with CPAP therapy in patients with Obstructive Sleep Apnea? Ramesh Metta, MBBS M Jeffery Mador, MD
 Does Depression affect compliance with CPAP therapy in patients with Obstructive Sleep Apnea? Ramesh Metta, MBBS M Jeffery Mador, MD Background Obstructive Sleep Apnea(OSA) Obstructive sleep apnea (OSA)
Does Depression affect compliance with CPAP therapy in patients with Obstructive Sleep Apnea? Ramesh Metta, MBBS M Jeffery Mador, MD Background Obstructive Sleep Apnea(OSA) Obstructive sleep apnea (OSA)
SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656
 SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656 ORTHODONTIC CLASSIFICATION / DIAGNOSIS Goal of diagnosis: An orderly reduction of the data base to a useful list of the patient s problems Useful??
SYSTEMATIC APPROACH TO ORTHODONTIC DIAGNOSIS DENT 656 ORTHODONTIC CLASSIFICATION / DIAGNOSIS Goal of diagnosis: An orderly reduction of the data base to a useful list of the patient s problems Useful??
Classification of Malocclusion
 Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
Classification of Malocclusion What s going on here? How would you describe this? Dr. Robert Gallois REFERENCE: Where Do We Begin? ESSENTIALS FOR ORTHODONTIC PRACTICE By Riolo and Avery Chapter 6 pages
CRANIOFACIAL ABNORMALITIES
 CRANIOFACIAL ABNORMALITIES It is well documented that mouth-breathing children grow longer faces. A paper by Tourne entitled The long face syndrome and impairment of the nasopharyngeal airway, recognised
CRANIOFACIAL ABNORMALITIES It is well documented that mouth-breathing children grow longer faces. A paper by Tourne entitled The long face syndrome and impairment of the nasopharyngeal airway, recognised
Dental Practitioner Guide. Narval CC CAD/CAM Mandibular Repositioning Device
 Dental Practitioner Guide Narval CC CAD/CAM Mandibular Repositioning Device Join global leaders in sleep and respiratory medicine ResMed is a global leader in the development, manufacturing and distribution
Dental Practitioner Guide Narval CC CAD/CAM Mandibular Repositioning Device Join global leaders in sleep and respiratory medicine ResMed is a global leader in the development, manufacturing and distribution
Intraoral Snoring Therapy - Diagnostics - Indications - IST Appliances
 Intraoral Snoring Therapy - Diagnostics - Indications - IST Appliances 2010, www.dr-hinz-dental.de Snoring does not only disturb the partner but also the snorer s health Intraoral appliances are used to
Intraoral Snoring Therapy - Diagnostics - Indications - IST Appliances 2010, www.dr-hinz-dental.de Snoring does not only disturb the partner but also the snorer s health Intraoral appliances are used to
Treatment for Snoring and Obstructive Sleep Apnea. Ri 林 鴻 錡 /AsP 譚 慶 鼎
 Treatment for Snoring and Obstructive Sleep Apnea Ri 林 鴻 錡 /AsP 譚 慶 鼎 Nonsurgical treatment Weight loss Avoidance of alcohol,sedatives,tobacco Positional devices Oral or nasal appliances Nasal continuous
Treatment for Snoring and Obstructive Sleep Apnea Ri 林 鴻 錡 /AsP 譚 慶 鼎 Nonsurgical treatment Weight loss Avoidance of alcohol,sedatives,tobacco Positional devices Oral or nasal appliances Nasal continuous
Treating Sleep Apnea A Review of the Research for Adults
 Treating Sleep Apnea A Review of the Research for Adults Is This Information Right for Me? Yes, if: A doctor said you have mild, moderate, or severe obstructive sleep apnea, or OSA. People with OSA may
Treating Sleep Apnea A Review of the Research for Adults Is This Information Right for Me? Yes, if: A doctor said you have mild, moderate, or severe obstructive sleep apnea, or OSA. People with OSA may
Sleep Difficulties. Insomnia. By Thomas Freedom, MD and Johan Samanta, MD
 Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
Sleep Difficulties By Thomas Freedom, MD and Johan Samanta, MD For most people, night is a time of rest and renewal; however, for many people with Parkinson s disease nighttime is a struggle to get the
ORTHODONTIC TREATMENT
 ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
Headgear Appliances. Dentofacial Orthopedics and Orthodontics. A Common Misconception. What is Headgear? Ideal Orthodontic Treatment Sequence
 Ideal Orthodontic Treatment Sequence Headgear Appliances Natalie A. Capan, D.M.D. 580 Sylvan Avenue, Suite 1M Englewood Cliffs, New Jersey 07632 (201)569-9055 www.capanorthodontics.com CapanOrtho@nj.rr.com
Ideal Orthodontic Treatment Sequence Headgear Appliances Natalie A. Capan, D.M.D. 580 Sylvan Avenue, Suite 1M Englewood Cliffs, New Jersey 07632 (201)569-9055 www.capanorthodontics.com CapanOrtho@nj.rr.com
The etiology of orthodontic problems Fifth session
 بنام خداوند جان و خرد The etiology of orthodontic problems Fifth session دکتر مھتاب نوری دانشيار گروه ارتدنسی Course Outline( 5 sessions) Specific causes of malocclusion Genetic Influences Environmental
بنام خداوند جان و خرد The etiology of orthodontic problems Fifth session دکتر مھتاب نوری دانشيار گروه ارتدنسی Course Outline( 5 sessions) Specific causes of malocclusion Genetic Influences Environmental
Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2015
 Special Articles pii: jc-00186-15 http://dx.doi.org/10.5664/jcsm.4858 Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2015
Special Articles pii: jc-00186-15 http://dx.doi.org/10.5664/jcsm.4858 Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2015
Rapid Resolution of Intense Suicidal Ideation after Treatment of Severe. From the Department of Psychiatry and Psychology (L.E.K.
 Category [Case Report] Rapid Resolution of Intense Suicidal Ideation after Treatment of Severe Obstructive Sleep Apnea Lois E. Krahn, MD Bernard W. Miller, RPSGT Larry R. Bergstrom, MD From the Department
Category [Case Report] Rapid Resolution of Intense Suicidal Ideation after Treatment of Severe Obstructive Sleep Apnea Lois E. Krahn, MD Bernard W. Miller, RPSGT Larry R. Bergstrom, MD From the Department
elf-awareness Toolkit
 S Snoring & Sleep Apnea elf-awareness Toolkit Snoring: Your Dentist Can Test So You Can Rest 2009 Snoring Isn t Sexy, LLC S Snoring & Sleep Apnea elf-awareness Toolkit Snoring: Your Dentist Can Test So
S Snoring & Sleep Apnea elf-awareness Toolkit Snoring: Your Dentist Can Test So You Can Rest 2009 Snoring Isn t Sexy, LLC S Snoring & Sleep Apnea elf-awareness Toolkit Snoring: Your Dentist Can Test So
What is Obstructive Sleep Apnoea?
 Patient Information Leaflet: Obstructive Sleep Apnoea Greenlane Respiratory Services, Auckland City Hospital & Greenlane Clinical Centre Auckland District Health Board What is Obstructive Sleep Apnoea?
Patient Information Leaflet: Obstructive Sleep Apnoea Greenlane Respiratory Services, Auckland City Hospital & Greenlane Clinical Centre Auckland District Health Board What is Obstructive Sleep Apnoea?
Obstructive sleep apnea and type 2 diabetes Obstructive Sleep Apnea (OSA) may contribute to or exacerbate type 2 diabetes for some of your patients.
 Obstructive sleep apnea and type 2 diabetes Obstructive Sleep Apnea (OSA) may contribute to or exacerbate type 2 diabetes for some of your patients. Prevalence of OSA and diabetes Prevalence of OSA Five
Obstructive sleep apnea and type 2 diabetes Obstructive Sleep Apnea (OSA) may contribute to or exacerbate type 2 diabetes for some of your patients. Prevalence of OSA and diabetes Prevalence of OSA Five
Diseases and Health Conditions that can Lead to Daytime Sleepiness
 October 21, 2014 Diseases and Health Conditions that can Lead to Daytime Sleepiness Indira Gurubhagavatula, MD, MPH Associate Professor Director, Occupational Sleep Medicine University of Pennsylvania,
October 21, 2014 Diseases and Health Conditions that can Lead to Daytime Sleepiness Indira Gurubhagavatula, MD, MPH Associate Professor Director, Occupational Sleep Medicine University of Pennsylvania,
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Sleep Position Trainer. The best treatment for Positional OSAS
 Sleep Position Trainer The best treatment for Positional OSAS Innovation distinguishes between a leader and a follower. - Steve Jobs Positional Therapy for (P)OSAS Positional Obstructive Sleep Apnea Syndrome
Sleep Position Trainer The best treatment for Positional OSAS Innovation distinguishes between a leader and a follower. - Steve Jobs Positional Therapy for (P)OSAS Positional Obstructive Sleep Apnea Syndrome
Comparing the Performance and Efficacy of the 3B/BMC RESmart. Auto-CPAP with the ResMed S9 AutoSet
 3B MEDICAL, INC., 21301 US HIGHWAY 27, LAKE WALES, FL. 33859 Comparing the Performance and Efficacy of the 3B/BMC RESmart Auto-CPAP with the ResMed S9 AutoSet Zhi Zhuang, PhD, Research and Development,
3B MEDICAL, INC., 21301 US HIGHWAY 27, LAKE WALES, FL. 33859 Comparing the Performance and Efficacy of the 3B/BMC RESmart Auto-CPAP with the ResMed S9 AutoSet Zhi Zhuang, PhD, Research and Development,
Maharashtra University of Health Sciences, Nashik. Syllabus. Fellowship Course in Sleep Medicine
 Maharashtra University of Health Sciences, Nashik Syllabus Fellowship Course in Sleep Medicine Appendix A a) Title of the Fellowship Course: Fellowship Course in Sleep Medicine b) Duration of Course: 1
Maharashtra University of Health Sciences, Nashik Syllabus Fellowship Course in Sleep Medicine Appendix A a) Title of the Fellowship Course: Fellowship Course in Sleep Medicine b) Duration of Course: 1
CPAP titration: PSG technologist or at Home
 CPAP titration: PSG technologist or at Home Carolyn D Ambrosio, MD, MS Associate Professor of Medicine Director, The Center for Sleep Medicine Tufts Medical Center Conflict of Interest No financial interest
CPAP titration: PSG technologist or at Home Carolyn D Ambrosio, MD, MS Associate Professor of Medicine Director, The Center for Sleep Medicine Tufts Medical Center Conflict of Interest No financial interest
U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria
 U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria Alcune pubblicazioni della Scuola: Impacted maxillary incisors: diagnosis and predictive measurements. Pavoni C, Mucedero M, Laganà G, Paoloni
U.O.C. Ortognatodonzia Area Funzionale Omogena di Odontoiatria Alcune pubblicazioni della Scuola: Impacted maxillary incisors: diagnosis and predictive measurements. Pavoni C, Mucedero M, Laganà G, Paoloni
Department of Pulmonology, Critical Care and Sleep Medicine, Bolan Medical College, Pakistan
 Cronicon OPEN ACCESS PULMONOLOGY AND RESPIRATORY MEDICINE Review Article Sleep Apnea Sanaullah Tareen Department of Pulmonology, Critical Care and Sleep Medicine, Bolan Medical College, Pakistan *Corresponding
Cronicon OPEN ACCESS PULMONOLOGY AND RESPIRATORY MEDICINE Review Article Sleep Apnea Sanaullah Tareen Department of Pulmonology, Critical Care and Sleep Medicine, Bolan Medical College, Pakistan *Corresponding
Fiberoptic bronchoscopy (FOB) is a procedure that pulmonologists
 Original Article Diagnosing Obstructive Sleep Apnea by Performing Fiberoptic Bronchoscopy and PEEP Titration of Mask Continuous Positive Airway Pressure Saenghirunvattana S, MD Sawang Saenghirunvattana,
Original Article Diagnosing Obstructive Sleep Apnea by Performing Fiberoptic Bronchoscopy and PEEP Titration of Mask Continuous Positive Airway Pressure Saenghirunvattana S, MD Sawang Saenghirunvattana,
DIAGNOSIS AND MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA. Venigalla Naga Venu Madhav 1 *
 DIAGNOSIS AND MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA 1 * 1. Dr. M.D.S. Reader, Department of Prosthodontics, Bharati Vidyapeeth Dental College and Hospital, Pune. Abstract Collapsibility of the upper airway
DIAGNOSIS AND MANAGEMENT OF OBSTRUCTIVE SLEEP APNEA 1 * 1. Dr. M.D.S. Reader, Department of Prosthodontics, Bharati Vidyapeeth Dental College and Hospital, Pune. Abstract Collapsibility of the upper airway
Guidelines for Referrals for Orthodontic Treatment
 Advice for General Dental Practitioners, PCTs and LHBs Guidelines for Referrals for Orthodontic Treatment This document has been produced by the British Orthodontic Society Guidelines for Referrals for
Advice for General Dental Practitioners, PCTs and LHBs Guidelines for Referrals for Orthodontic Treatment This document has been produced by the British Orthodontic Society Guidelines for Referrals for
Obstructive Sleep Apnoea
 Obstructive Sleep Apnoea What is obstructive sleep apnoea? People who suffer from Obstructive Sleep Apnoea (OSA) reduce or stop their breathing for short periods while sleeping. This can happen many times
Obstructive Sleep Apnoea What is obstructive sleep apnoea? People who suffer from Obstructive Sleep Apnoea (OSA) reduce or stop their breathing for short periods while sleeping. This can happen many times
EXPECTATIONS OF PHYSICIANS INTENDING TO PRACTISE SLEEP MEDICINE CHANGING SCOPE OF PRACTICE PROCESS BACKGROUND
 EXPECTATIONS OF PHYSICIANS INTENDING TO PRACTISE SLEEP MEDICINE CHANGING SCOPE OF PRACTICE PROCESS BACKGROUND The College is gradually moving toward a system of performance measurement by focusing on a
EXPECTATIONS OF PHYSICIANS INTENDING TO PRACTISE SLEEP MEDICINE CHANGING SCOPE OF PRACTICE PROCESS BACKGROUND The College is gradually moving toward a system of performance measurement by focusing on a
Oral Appliance Therapy and Sleep Apnea
 research reports Clinical A. Hoekema 1 *, B. Stegenga 1, P.J. Wijkstra 2, J.H. van der Hoeven 3, A.F. Meinesz 2, and L.G.M. de Bont 1 Obstructive Sleep Apnea Therapy 1 Department of Oral and Maxillofacial
research reports Clinical A. Hoekema 1 *, B. Stegenga 1, P.J. Wijkstra 2, J.H. van der Hoeven 3, A.F. Meinesz 2, and L.G.M. de Bont 1 Obstructive Sleep Apnea Therapy 1 Department of Oral and Maxillofacial
Efficiency of Three Mandibular Anchorage Forms in Herbst Treatment: A Cephalometric Investigation
 Original Article Efficiency of Three Mandibular Anchorage Forms in Herbst Treatment: A Cephalometric Investigation Dominique Weschler, DDS, Dr Med Dent a ; Hans Pancherz, DDS, Odont Dr, FCDSHK (Hon) b
Original Article Efficiency of Three Mandibular Anchorage Forms in Herbst Treatment: A Cephalometric Investigation Dominique Weschler, DDS, Dr Med Dent a ; Hans Pancherz, DDS, Odont Dr, FCDSHK (Hon) b
2015 Physician Quality Reporting System Data Collection Form: Sleep Apnea (for patients aged 18 and older)
 2015 Physician Quality Reporting System Data Collection Form: Sleep Apnea (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
2015 Physician Quality Reporting System Data Collection Form: Sleep Apnea (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures) is not considered
ABSTRACT INTRODUCTION. Facial Esthetics. Dental Esthetics
 ABSTRACT The FACE philosophy is characterized by clearly defined treatment goals. This increases diagnostic ability and improves the quality and stability of the end result. The objective is to establish
ABSTRACT The FACE philosophy is characterized by clearly defined treatment goals. This increases diagnostic ability and improves the quality and stability of the end result. The objective is to establish
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
pii: jc-00031-15 http://dx.doi.org/10.5664/jcsm.4556
 SPECIAL SECTION pii: jc-00031-15 http://dx.doi.org/10.5664/jcsm.4556 Quality Measures for the Care of Adult Patients with Obstructive Sleep Apnea R. Nisha Aurora, MD 1 ; Nancy A. Collop, MD 2 ; Ofer Jacobowitz,
SPECIAL SECTION pii: jc-00031-15 http://dx.doi.org/10.5664/jcsm.4556 Quality Measures for the Care of Adult Patients with Obstructive Sleep Apnea R. Nisha Aurora, MD 1 ; Nancy A. Collop, MD 2 ; Ofer Jacobowitz,
Understanding Sleep Apnea
 Understanding Sleep Apnea www.sleepmangementsolutions.com What is Obstructive Sleep Apnea (OSA)? OSA afflicts 20 million adult men and women in the U.S. People who have OSA stop breathing repeatedly during
Understanding Sleep Apnea www.sleepmangementsolutions.com What is Obstructive Sleep Apnea (OSA)? OSA afflicts 20 million adult men and women in the U.S. People who have OSA stop breathing repeatedly during
New Mouthpiece Provides Relief for Truckers with Obstructive Sleep Apnea
 For Immediate Release For More Information Contact: Dave Kushin Zebra Communications 805-955-0009 Fax: 805-955-0003 email: dave.kushin@zebracom.net www.zebracom.net New Mouthpiece Provides Relief for Truckers
For Immediate Release For More Information Contact: Dave Kushin Zebra Communications 805-955-0009 Fax: 805-955-0003 email: dave.kushin@zebracom.net www.zebracom.net New Mouthpiece Provides Relief for Truckers
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE
 TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
Obstructive Sleep Apnea and Sleep Disorders in All Age Groups Treatment
 Obstructive Sleep Apnea and Sleep Disorders in All Age Groups Treatment W. McD. Anderson, M.D. Medical Director, Tampa General Hospital Sleep Center Professor of Medicine, USF College of Medicine Program
Obstructive Sleep Apnea and Sleep Disorders in All Age Groups Treatment W. McD. Anderson, M.D. Medical Director, Tampa General Hospital Sleep Center Professor of Medicine, USF College of Medicine Program
Restoring a good night s sleep
 Restoring a good night s sleep Products for diagnosing, treating, and monitoring sleep apnea Sleep apnea solutions A good night s sleep is an essential part of healthy living, but for patients diagnosed
Restoring a good night s sleep Products for diagnosing, treating, and monitoring sleep apnea Sleep apnea solutions A good night s sleep is an essential part of healthy living, but for patients diagnosed
Obstructive Sleep Apnea (Not so) Sweet Dreams
 Obstructive Sleep Apnea (Not so) Sweet Dreams Sleep, riches, and health, to be truly enjoyed, must be interrupted. -- Jean-Paul Richter Presented by: Brad Heltemes, M.D. VP & Chief Medical Director ING
Obstructive Sleep Apnea (Not so) Sweet Dreams Sleep, riches, and health, to be truly enjoyed, must be interrupted. -- Jean-Paul Richter Presented by: Brad Heltemes, M.D. VP & Chief Medical Director ING
X-Plain Temporomandibular Joint Disorders Reference Summary
 X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
X-Plain Temporomandibular Joint Disorders Reference Summary Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can
Control of mandibular incisors with the combined Herbst and completely customized lingual appliance - a pilot study
 Control of mandibular incisors with the combined Herbst and completely customized lingual appliance - a pilot study Dirk Wiechmann 1 *, Rainer Schwestka-Polly 2 *, Hans Pancherz 3 *, Ariane Hohoff 4 *
Control of mandibular incisors with the combined Herbst and completely customized lingual appliance - a pilot study Dirk Wiechmann 1 *, Rainer Schwestka-Polly 2 *, Hans Pancherz 3 *, Ariane Hohoff 4 *
Objectives. Objectives. Objectives. Objectives. Describe Class II div 1
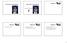 Class II div 1 Malocclusion Class II div 1 Malocclusion Objectives OR What can we do about Goofy? Objectives Describe Class II div 1 Objectives Describe Class II div 1 Describe principles of treatment
Class II div 1 Malocclusion Class II div 1 Malocclusion Objectives OR What can we do about Goofy? Objectives Describe Class II div 1 Objectives Describe Class II div 1 Describe principles of treatment
Sleep Apnea. ACP Oct 26, 2014. Bashir Chaudhary, MD Sleep Institute of Augusta, Augusta GA
 Sleep Apnea ACP Oct 26, 2014 Bashir Chaudhary, MD Sleep Institute of Augusta, Augusta GA Emeritus Professor of Medicine and Assistant Dean of Clinical Affairs, CAHS Medical College of Georgia, Georgia
Sleep Apnea ACP Oct 26, 2014 Bashir Chaudhary, MD Sleep Institute of Augusta, Augusta GA Emeritus Professor of Medicine and Assistant Dean of Clinical Affairs, CAHS Medical College of Georgia, Georgia
Course Curriculum for the Master Degree in Dentistry/Orthodontics
 Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
Jordan University of Science and Technology Faculty of Graduate Studies Course Curriculum for the Master Degree in Dentistry/Orthodontics The Master Degree in Dentistry/ Orthodontics is awarded by the
Chapter 17 Medical Policy
 RAD-1 LCD for Respiratory Assist Devices (L11482) Contractor Information Contractor Name Contractor Number 00635 Contractor Type LCD Information LCD Database ID Number L11482 AdminaStar Federal, Inc. DMERC
RAD-1 LCD for Respiratory Assist Devices (L11482) Contractor Information Contractor Name Contractor Number 00635 Contractor Type LCD Information LCD Database ID Number L11482 AdminaStar Federal, Inc. DMERC
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
You re saving teeth but are you saving lives? An Introduction & Overview of Dental Sleep Medicine Dr. Gy Yatros Diplomates, ABDSM
 You re saving teeth but are you saving lives? An Introduction & Overview of Dental Sleep Medicine Dr. Gy Yatros Diplomates, ABDSM Des Moines, IA May 2, 2015 2 WHO WE ARE Dental Sleep Solutions was founded
You re saving teeth but are you saving lives? An Introduction & Overview of Dental Sleep Medicine Dr. Gy Yatros Diplomates, ABDSM Des Moines, IA May 2, 2015 2 WHO WE ARE Dental Sleep Solutions was founded
Sleep Apnoea and driving the facts. Developed by The OSA Partnership Group and the Driver and Vehicle Licensing Agency (DVLA)
 Sleep Apnoea and driving the facts Developed by The OSA Partnership Group and the Driver and Vehicle Licensing Agency (DVLA) September 2013 Introduction This document has been developed following collaboration
Sleep Apnoea and driving the facts Developed by The OSA Partnership Group and the Driver and Vehicle Licensing Agency (DVLA) September 2013 Introduction This document has been developed following collaboration
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
Three Dimensional Imaging Based Diagnosis for Obstructive Sleep Apnoea: A Conceptual Framework
 Three Dimensional Imaging Based Diagnosis for Obstructive Sleep Apnoea: A Conceptual Framework 1 Syed M. S. Islam, 1 Mithran S. Goonewardene and 2 Paul Sillifant 1 School of Dentistry, The University of
Three Dimensional Imaging Based Diagnosis for Obstructive Sleep Apnoea: A Conceptual Framework 1 Syed M. S. Islam, 1 Mithran S. Goonewardene and 2 Paul Sillifant 1 School of Dentistry, The University of
Compliance Issues in Home CPAP Therapy. Joseph Lewarski, BS, RRT, FAARC
 Compliance Issues in Home CPAP Therapy Joseph Lewarski, BS, RRT, FAARC Obstructive Sleep Apnea Syndrome OSA 1 st recognized over 30 years ago 1981 Sullivan publishes small study in Lancet¹ Late 80s, early
Compliance Issues in Home CPAP Therapy Joseph Lewarski, BS, RRT, FAARC Obstructive Sleep Apnea Syndrome OSA 1 st recognized over 30 years ago 1981 Sullivan publishes small study in Lancet¹ Late 80s, early
GUIDELINES FOR AJODO CASE REPORTS
 GUIDELINES FOR AJODO CASE REPORTS Case reports are published on a regular basis in the AJODO. Not only are these short communications interesting to the clinician in private practice, but they provide
GUIDELINES FOR AJODO CASE REPORTS Case reports are published on a regular basis in the AJODO. Not only are these short communications interesting to the clinician in private practice, but they provide
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS
 RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
General Information about Sleep Studies and What to Expect
 General Information about Sleep Studies and What to Expect Why do I need a sleep study? Your doctor has ordered a sleep study because your doctor is concerned you may have a sleep disorder that is impacting
General Information about Sleep Studies and What to Expect Why do I need a sleep study? Your doctor has ordered a sleep study because your doctor is concerned you may have a sleep disorder that is impacting
Orthodontic mini-implants, or temporary anchorage devices
 Anchors, away by John Marshall Grady, DMD, Dan E. Kastner, DMD, and Matthew C. Gornick, DMD Drs. John Marshall Grady (center), Dan E. Kastner (left), and Matthew C. Gornick (right). Drs. John Marshall
Anchors, away by John Marshall Grady, DMD, Dan E. Kastner, DMD, and Matthew C. Gornick, DMD Drs. John Marshall Grady (center), Dan E. Kastner (left), and Matthew C. Gornick (right). Drs. John Marshall
Respiratory Medicine. Understanding Sleep Apnoea
 Respiratory Medicine Understanding Sleep Apnoea The Respiratory Medicine Service provides inpatient and outpatient care on acute and chronic respiratory diseases. Apart from treating conditions, we also
Respiratory Medicine Understanding Sleep Apnoea The Respiratory Medicine Service provides inpatient and outpatient care on acute and chronic respiratory diseases. Apart from treating conditions, we also
a guide to understanding pierre robin sequence
 a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
33 % of whiplash patients develop. headaches originating from the upper. cervical spine
 33 % of whiplash patients develop headaches originating from the upper cervical spine - Dr Nikolai Bogduk Spine, 1995 1 Physical Treatments for Headache: A Structured Review Headache: The Journal of Head
33 % of whiplash patients develop headaches originating from the upper cervical spine - Dr Nikolai Bogduk Spine, 1995 1 Physical Treatments for Headache: A Structured Review Headache: The Journal of Head
Truck driving is a hazardous occupation,
 324 Validation of Sleep Apnea Screening Criteria Talmage et al Consensus Criteria for Screening Commercial Drivers for Obstructive Sleep Apnea: Evidence of Efficacy James B. Talmage, MD Toney B. Hudson,
324 Validation of Sleep Apnea Screening Criteria Talmage et al Consensus Criteria for Screening Commercial Drivers for Obstructive Sleep Apnea: Evidence of Efficacy James B. Talmage, MD Toney B. Hudson,
20 SLEEP DISORDERS 20.1 RELEVANCE TO DRIVING TASK 20.2 GENERAL MANAGEMENT GUIDELINES
 20 SLEEP DISORDERS 20.1 RELEVANCE TO DRIVING TASK 20.1.1 Fatigue is a major cause of road accidents. Sleepiness and sleep disorders are one important aspect of managing the risks of fatigue (Fatigue Expert
20 SLEEP DISORDERS 20.1 RELEVANCE TO DRIVING TASK 20.1.1 Fatigue is a major cause of road accidents. Sleepiness and sleep disorders are one important aspect of managing the risks of fatigue (Fatigue Expert
Medical Information to Support the Decisions of TUECs INTRINSIC SLEEP DISORDERS
 Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: o Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea syndrome (OSAHS)
Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: o Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea syndrome (OSAHS)
CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea
 CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea Andrew J Westwood, M.D., MRCP(UK) 1, Andrew R Spector, M.D., 2 Sanford H Auerbach, M.D. 3 1 Columbia University College of Physicians
CPAP Treats Muscle Cramps in Patients with Obstructive Sleep Apnea Andrew J Westwood, M.D., MRCP(UK) 1, Andrew R Spector, M.D., 2 Sanford H Auerbach, M.D. 3 1 Columbia University College of Physicians
Scoring (manual, automated, automated with manual review)
 A. Source and Extractor Author, Year Reference test PMID RefID Index test 1 Key Question(s) Index test 2 Extractor B. Study description Sampling population A Recruitment Multicenter? Enrollment method
A. Source and Extractor Author, Year Reference test PMID RefID Index test 1 Key Question(s) Index test 2 Extractor B. Study description Sampling population A Recruitment Multicenter? Enrollment method
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
Oximetry Alone Versus Portable Polygraphy for Sleep Apnea Screening Before Bariatric Surgery
 OBES SURG (2010) 20:326 331 DOI 10.1007/s11695-009-0055-9 CLINICAL RESEARCH Oximetry Alone Versus Portable Polygraphy for Sleep Apnea Screening Before Bariatric Surgery Maude Malbois & Vittorio Giusti
OBES SURG (2010) 20:326 331 DOI 10.1007/s11695-009-0055-9 CLINICAL RESEARCH Oximetry Alone Versus Portable Polygraphy for Sleep Apnea Screening Before Bariatric Surgery Maude Malbois & Vittorio Giusti
U.S. Food and Drug Administration
 U.S. Food and Drug Administration Notice: Archived Document The content in this document is provided on the FDA s website for reference purposes only. It was current when produced, but is no longer maintained
U.S. Food and Drug Administration Notice: Archived Document The content in this document is provided on the FDA s website for reference purposes only. It was current when produced, but is no longer maintained
Sleep Apnea in Stroke. Diagnosis, Consequences & Treatment J.A. Aaronson
 Sleep Apnea in Stroke. Diagnosis, Consequences & Treatment J.A. Aaronson SLEEP APNEA IN STROKE: SUMMARY The overall objective of this thesis was to improve our understanding of the effects of obstructive
Sleep Apnea in Stroke. Diagnosis, Consequences & Treatment J.A. Aaronson SLEEP APNEA IN STROKE: SUMMARY The overall objective of this thesis was to improve our understanding of the effects of obstructive
OUTCOMES OF CPAP TREATMENT IN A SLEEP LABORATORY SPECIALIZED IN NEUROPSYCHIATRY
 JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2004, 55, Suppl 3, 15 22 www.jpp.krakow.pl J. ANTCZAK 1,2, P. GEISLER 2, R. POPP 2 OUTCOMES OF CPAP TREATMENT IN A SLEEP LABORATORY SPECIALIZED IN NEUROPSYCHIATRY
JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2004, 55, Suppl 3, 15 22 www.jpp.krakow.pl J. ANTCZAK 1,2, P. GEISLER 2, R. POPP 2 OUTCOMES OF CPAP TREATMENT IN A SLEEP LABORATORY SPECIALIZED IN NEUROPSYCHIATRY
Perioperative Management of Patients with Obstructive Sleep Apnea. Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine
 Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
Summary of AASM Clinical Guidelines for the Manual Titration of Positive Airway Pressure in Patients with Obstructive Sleep Apnea - Updated July 2012
 Summary of AASM Clinical Guidelines for the Manual Titration of Positive Airway Pressure in Patients with Obstructive Sleep Apnea - Updated July 2012 SUMMARY: Sleep technologists are team members who work
Summary of AASM Clinical Guidelines for the Manual Titration of Positive Airway Pressure in Patients with Obstructive Sleep Apnea - Updated July 2012 SUMMARY: Sleep technologists are team members who work
O bstructive sleep apnoea syndrome (OSAS) is a
 430 SLEEP DISORDERED BREATHING Continuous positive airway pressure reduces daytime sleepiness in mild to moderate obstructive sleep apnoea: a meta-analysis N S Marshall, M Barnes, N Travier, A J Campbell,
430 SLEEP DISORDERED BREATHING Continuous positive airway pressure reduces daytime sleepiness in mild to moderate obstructive sleep apnoea: a meta-analysis N S Marshall, M Barnes, N Travier, A J Campbell,
Implant-retained oral appliances: a novel treatment for edentulous patients with obstructive sleep apnea hypopnea syndrome
 Aarnoud Hoekema Frist de Vries Kees Heydenrijk Boudewijn Stegenga Implant-retained oral appliances: a novel treatment for edentulous patients with obstructive sleep apnea hypopnea syndrome Authors affiliations:
Aarnoud Hoekema Frist de Vries Kees Heydenrijk Boudewijn Stegenga Implant-retained oral appliances: a novel treatment for edentulous patients with obstructive sleep apnea hypopnea syndrome Authors affiliations:
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Children Who Snore Do they have Sleep Apnea? Iman Sami, M.D. Division of Pulmonary and Sleep Medicine, Children s National
 Children Who Snore Do they have Sleep Apnea? Iman Sami, M.D. Division of Pulmonary and Sleep Medicine, Children s National June 3, 2015 No disclosures relevant to this talk No disclosures relevant to this
Children Who Snore Do they have Sleep Apnea? Iman Sami, M.D. Division of Pulmonary and Sleep Medicine, Children s National June 3, 2015 No disclosures relevant to this talk No disclosures relevant to this
Introduction to Dental Anatomy
 Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Condylar position in children with functional posterior crossbites: before and after crossbite correction*
 PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
PEDIATRIC DENTISTRY/Copyright 1980 by The American Academy of Pedodontics/Vol. 2, No. 3 Condylar position in children with functional posterior crossbites: before and after crossbite correction* David
SLEEP AND PARKINSON S DISEASE
 A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
