GLOBAL HEADQUARTERS EUROPE r35k0709 BMF
|
|
|
- Barry Gilbert
- 8 years ago
- Views:
Transcription
1 What fascinates you about the body is also what drives us. That s why we re always pushing the boundaries of engineering to make products that help you keep the human form as glorious as it was intended. To learn more about our breadth of products, call or visit us online at biometmicrofixation.com. We d love to join you in a conversation about the future. For more information on Pectus Bar, please contact us at: GLOBAL HEADQUARTERS 1520 Tradeport Drive Jacksonville, FL Tel (904) Toll-Free (800) Fax (904) Order Fax (904) EUROPE Toermalijnring LC Dordrecht The Netherlands Tel Fax europe@biomet.com r35k0709 This brochure is presented to demonstrate the surgical technique, patient selection and post-op protocol utilized by Dr. Donald Nuss. As the manufacturer of this device, Biomet Microfixation does not practice medicine and does not recommend this product or surgical technique for use on a specific patient. The surgeon who performs any implant procedure must determine the appropriate device and surgical procedure for each individual patient. Devices shown in this brochure may not be cleared or licensed for use or sale in your individual country. Please contact your local distributor for information regarding availability of this product. Information contained in this brochure is intended for surgeon or distributor information only and is not intended for patient distribution. All surgeries carry risks. For additional information, please see package insert, or visit our web site at or call BMF
2 Pectus Bar Pectus Excavatum Correction Anticipate. Innovate ṬM
3 An Innovative Technique for the Correction of Pectus Excavatum Anticipation and innovation. These two qualities have made Biomet Microfixation an industry leader. Founded by Walter Lorenz more than thirty years ago, Biomet Microfixation offers instrumentation, plating systems and related products for a wide range of surgical procedures. Using the Nuss Technique, along with the Pectus Bar, surgery to correct Pectus Excavatum is accomplished in less time and with more ease than with other techniques. Dr. Donald Nuss, in cooperation with Biomet Microfixation, has developed a minimally invasive surgical procedure and Pectus Bar implant to remodel the chest wall over a 2 to 3 year period. The Nuss Technique, also known as the Minimally Invasive Repair of Pectus Excavatum (MIRPE), uses principles of minimal-access surgery and thoracoscopy combined with the proper placement of a Pectus Bar to achieve correction of Pectus Excavatum. Pectus Excavatum is a chest disorder occurring in approximately one of every 1,000 children. This congenital deformity is characterized by a concave, funnel shaped chest. The inward facing sternum can apply pressure to the vital organs of the chest resulting in restricted organ growth and shortness of breath. Mildly present at birth, Pectus Excavatum usually becomes more serious throughout childhood, often magnifying considerably during the teenage years. Pectus System Features The Pectus Bar s rounded ends and blunt edges help minimize tissue destruction during implant insertion. The Pectus Bar comes in a variety of lengths ranging from 7 inches (17.8 cm) to 17 inches (43.2 cm) to accommodate most Pectus Excavatum correction procedures. All instruments in the Pectus System are designed to increase simplicity during the Nuss Procedure. The Pectus System Container comes in two sizes and conveniently houses the entire range of Pectus implants and instruments. Specialized titanium bars and stabilizers available for patients with nickel allergies.* Pectus-size bars available for the following: -Special sized bars -Pre-bent bars developed in accordance with patients CT scans* *Titanium and pre-bent bars for pediatric indications only Severe case of Pectus Excavatum. Pre-operative photo. 2 year Post-operative photo at 1 month after bar removal.
4 The Nuss Technique Benefits Minimally Invasive Operation - Use of the MIRPE technique requires neither cartilage incision nor resection for correction of pectus excavatum. There is no need to make an incision in the anterior chest wall, raise pectoralis muscle flaps, resect rib cartilages, nor perform sternal osteotomy. Reduces Operating Time - The procedure requires approximately 40 minutes, as opposed to the 4 to 6 hours required of a chest reconstruction. Minimal Blood Loss - Blood loss is generally 10 to 30ccs, compared to the 300ccs lost with the other products and techniques. 1 Early Return to Regular Activity - The average time for a patient to resume daily activities, once treated with the Pectus Bar, is one month.* * Return time varies depending on each patient. Always consult your physician before resuming any activity. Chest Correction - Using the Pectus Bar the patient can experience ease of breathing, normal chest expansion and elasticity, and proper lung and heart growth. Excellent Long-Term Cosmetic Result - A 10 Year Study of a Minimally Invasive Technique for the Correction of Pectus Excavatum, indicated excellent long-term results. The Journal of Pediatric Surgery, 1998; 33(4). Donald Nuss, M.B., Ch.B.; Robert E. Kelly, Jr., M.D.; Daniel P. Croitoru, M.D.; Michael E. Katz, M.D. Indications and Patient Selection Patients with pectus excavatum are considered for surgical reconstruction between the ages of 4 and 18 years, when the ribs and costal cartilage are neither too malleable nor too rigid. The ideal age is between 8 and 13 years, prior to the adolescent growth period. A complete physical exam and full medical history are completed for all patients to place them into either asymptomatic or symptomatic classifications based on the following criteria: History of progressive worsening of the pectus excavatum. History of the symptoms related but not limited to exercise intolerance, chest pain, and shortness of breath. Clinical evaluation showing severe pectus with the demonstration of cardiac displacement and pulmonary compromise. Asymptomatic patients are given an exercise program to correct their posture and are reevaluated every six months to follow their progress. Patients will be moved into the symptomatic group as indicated by their symptoms. Symptomatic patients are sent for a CT scan, pulmonary-function studies and cardiology examinations. Surgery is supported by the results of the objective criteria obtained from these exams. The criteria includes a CT index (Haller index) of 3.2 or greater, atelectasis, abnormal pulmonary function, cardiac compression, mitral valve prolapse, heart murmurs and A-V conduction delay. These patients may have other abnormalities, such as Marfan s syndrome, Ehlers-Danlos or Poland s syndrome. Prior to the day of surgery, the patient s chest is measured to determine the length of the Pectus Bar. Proper measurement is performed utilizing a measuring tape or a Pectus Bar Template over the deepest portion of the pectus from the right midaxillary to the left midaxillary line. The length of the Pectus Bar required is 1 to 2 cm less than the measured distance because the tape measures the external diameter of the chest and the Pectus Bar traverses the internal diameter. Heart compression and displacement
5 Operative Technique 1. A course of antibiotics is started at the time of surgery to prevent infection and reduce the development of pneumonia. The procedure is performed under general endotracheal anesthesia with muscle relaxation and an epidural block for both operative and postoperative pain control. 1-2 Patient positioned with both arms abducted 2. During the procedure, the patient is positioned with both arms abducted at the shoulders to allow access to the lateral chest-wall. Padding under the arms and proper positioning of the arms will help prevent neurologic injury. 3. The patient is draped, and the chest is marked for surgery with a sterile marking pen. The deepest portion of the pectus is marked. If the deepest point of the pectus is inferior to the sternum, then mark the lower end of the sternum. Using this point, establish a horizontal plane across the pectus region by marking the intercostal spaces at the top of the pectus ridge on both sides. Extend the horizontal plane to the lateral chest wall and mark between the anterior and midaxillary lines for transverse lateral incisions. 3 Patient is draped and marked for surgery Confirming preoperative measurements using a Pectus Bar Template 4 4. The preoperative chest measurement is reconfirmed, and a Pectus Bar is selected for bending into the desired chest-wall curvature. The Pectus Bar Template can be used to visualize the shape necessary to correct the deformity. Special care should be taken in choosing the correct Pectus Bar length to maximize bar stability. 5. Using the Pectus Bender, shape the selected Pectus Bar from the center outward making small gradual bends. Position the cam on the bender at position 0 (minimum radius) then move the cam to position 1, and finally to position 2 (maximum radius). It may be necessary to exaggerate the curvature slightly to allow for the anterior chest-wall pressure and downward force of the sternum. To insure proper union between bar and stabilizer, avoid bending the lateral ends of the Pectus Bar. The selected bar is shaped for each patient Incisions being made at the predetermined marks 5 The selected bar is shaped for each patient
6 6. Bilateral 2.5 cm transverse, thoracic incisions are made at the marks previously drawn in line with the deepest point of the depression in each lateral chest wall between the anterior and midaxillary lines. A skin tunnel is raised anteriorly from both incisions to the top of the pectus ridge at the previously selected intercostal space. The Pectus Bar enters the chest slightly medial to the top of the pectus ridge Advancing the Pectus Bar Introducer to dissect a tunnel for the pectus bar Incisions being made at the predetermined marks 7. A 5mm, 0 or 30 thoracoscope is used during the procedure to visualize the chest organs. Insert the scope on the patient s right side, one to two intercostal spaces below the space which has been chosen for the Pectus Bar. The scope can be used bilaterally using the incision made on the patient s left, or a new stab incision can be made one to two intercostal spaces below the space which has been chosen. The chest is insufflated with CO 2 for adequate visualization. 8. Enter the chest from the patient s right with the proper Pectus Introducer in order to dissect a tunnel for the implant. The small introducer is for younger, smaller patients, ages The long introducer is for older, larger patients, ages Advancing the Pectus Bar Introducer to dissect a tunnel for the pectus bar. 9. The Pectus Introducer is slowly advanced across the mediastinum immediately under the sternum and is gently pushed through the intercostal space on the opposite side. The tip should face anteriorly and stay in contact with the sternum. Advance the device far enough through the opposite incision to allow for elevating the sternum and attaching of the umbilical tape. 9 Introducer is advanced through the chest and the opposite incision 10 Pressure is applied to the sternum to stretch the connective tissues 10. Elevate the sternum by lifting the advanced introducer from both sides of the patient. Apply pressure above and below the sternum to obtain the desired curvature of the sternum. Repeat several times in order to stretch the connective tissues and correct the deformity prior to inserting the bar. Correcting the pectus excavatum by elevating the sternum with the introducer greatly facilitates initial bar rotation and improves bar stability.
7 Operative Technique 11. Two strands of umbilical tape are tied through the hole in the end of the introducer and then pulled through the tunnel by withdrawing the introducer from the patient s right side. One strand is used as a backup, while the other strand of umbilical tape is then attached to the bar and used to guide it through the tunnel. Umbilical tape used to guide the bar The curved Pectus Bar is pulled under the body of the sternum from the patients right side with the convexity facing posteriorly. When the bar is in position, it is flipped with the Pectus Flipper causing the sternum and anterior chest wall to rise into the desired position. 12 Guiding the convex bar through the chest with the convexity facing anteriorly 13 Pectus correction and implant stability are evaluated 13. STABILITY OF THE BAR MUST BE DETERMINED AT THIS TIME. Such assessment will dictate the need for bar stabilization and for placement of a second bar behind the sternum. Typically, patients require one bar. Older, larger and more active patients or patients with a more severe deformity may require an additional bar to achieve proper correction and stability. If needed, a second bar is placed one or two intercostal spaces superiorly or inferiorly to the first bar 14. A subcutaneous pocket is made posteriorly at each incision where the lateral end of the bar will be fitted with a Pectus Bar Stabilizer. One stabilizer is recommended for every bar implanted to limit rotation of the bar. Recommended patient ages for use of the stabilizers are: Patients 4-13 years - use one stabilizer per bar implanted Patients years - use one stabilizer per bar implanted, however one may choose to use two per bar depending on the patient s pectus, muscular development, activity level (ie: sports), and the stability of the bar. 14 Trial fitting a stabilizer ( ) to the implant
8 15. An Elongated Stabilizer is chosen and fitted with the channel facing anteriorly and 1 to 2 cm of the lateral end of the bar exposed through the stabilizer. The stabilizer is then secured to the bar and sutured to the muscle after being properly fitted. The bar and stabilizer(s) should not be too anterior or posterior on the patient as this can lead to pain and tissue erosion. Elongated Stabilizer - Suitable for all patients in the recommended age range. 15 Trial fitting a stabilizer ( ) to the implant 16 Cardiac wire is used to figure 8 suture both the bar and the stabilizer LactoSorb stabilizer 16. The bar and stabilizer are secured to each other and to the chest wall with multiple sutures to anchor the bar and stabilizer to the chest wall and bury the bar and stabilizer with tissue. The size and types of suture presently used are as follows: If using the LactoSorb stabilizer, secure the stabilizer to the bar with a figure-8 suture around the junction of both devices with size O absorbable suture. If using the metal stabilizer, secure the stabilizer to the bar with a figure-8 suture around the junction of both devices with No. 3 cardiac wire or size O non-absorbable suture. Secure the holes in the bar and stabilizer to the chest wall muscles with size O absorbable or non-absorbable suture attached to a UR 6 (right-angle) needle. Secure muscle over the bar with mattress sutures using size O fast or slow absorbable suture attached to a large needle. Close the wound with a small-size, fast-absorbing suture and a dressing. 17. Prior to closing the incisions, place patient in Trendelenburg s position, inflate lungs and apply positive end expiratory pressure (PEEP) of 4 to 6 cm H 2 O to prevent pleural air trapping. 17 Patient Is ready for recovery A chest radiograph should be obtained postoperatively to check for pneumothorax. The radiograph is excellent in showing final bar placement and may be obtained in the operating room or surgery-recovery area, as required. Suture to the chest wall muscles to anchor the device
9 Post-operative Patient Care Patients are kept well sedated for the first 1 to 3 days for postoperative pain management and to prevent bar displacement. Medications and therapies depend on the patient s response to pain and may include the use of an epidural catheter, intravenous morphine for breakthrough pain, patientcontrolled analgesia (PCA) and oral analgesia. Post Operative Patient Handling by the hospital staff is important for avoiding bar displacement. Patients are discharged from the hospital when they are able to walk unassisted. The following protocol is recommended: Recommended postoperative protocol Day 1 Post-Op Out of Bed (OOB) to a chair with assistance OOB ambulation, as tolerated with assistance medical immobilization by nursing staff, as required eggcrate mattress (as indicated) NO chest or waist bending NO twisting NO LOG ROLLING Deep breathing and incentive spirometry every hour while awake Day 2 Post-Op OOB to a chair with assistance OOB ambulation, as tolerated with assistance supine with hip flexion NO chest or waist bending NO twisting NO LOG ROLLING Deep breathing and incentive spirometry every hour while awake Day 3 Post-Op through Discharge Day OOB ambulation with minimal assistance supine with hip flexion NO chest or waist bending NO twisting NO LOG ROLLING Deep breathing and incentive spirometry every hour while awake Once discharged, the patient should maintain good posture and limit activity for the first month, with regular activity permitted after 4 to 6 weeks. The following guidelines have been developed to assist the patient s return to regular activity and reduce the risk of bar displacement: Walking should be done frequently Deep-breathing exercises performed twice a day, every morning and evening Patient can bathe and/or shower after five (5) days No waist bending, twisting or log rolling for first four (4) weeks at home Patient should keep a straight back with no slouching for the first month No heavy lifting for the two (2) months following surgery No sports for the first three (3) months following surgery The implant remains in the patient for a minimum of two years. Should the patient require emergency medical attention during this period, the following recommendations will apply: MedicAlert identification is recommended MRI of the chest or upper abdomen can be performed. Cardiac defibrillation, if necessary, is performed with anterior/posterior paddle placement to deliver electrical charge to the heart The patient should visit the doctor at regular intervals for evaluation of the chest wall. The implant is removed when the chest wall is deemed strong enough to support the sternum. Generally, the bar will remain implanted for a minimum of 2 years, up to a maximum of 3 years following the procedure Bar Removal 1. Surgery for removal of the support bar(s) and stabilizer(s) is performed under general anesthesia as an outpatient procedure. The patient is in the supine position with the arms abducted. Incisions are made in the same locations as during the implantation. 2. The incision will allow access to the lateral tip of the support bar for removal of all stabilizers and any remaining sutures. The support bar is removed by pulling the bar through one incision while rolling the patient to the opposite side. 3. The incisions are closed with absorbable sutures, and a postoperative chest radiograph is recommended.
10 Ordering Information Pectus Bar Implant Size in Inches Size in cm Part # Template Part # Pectus Bar Implant (See chart for details) N/A N/A N/A N/A N/A N/A Standard Container X-Long Container Elongated Pectus Stabilizer LactoSorb Stabilizer Pectus Removal Benders, Pair *Patient specific size bars are available; please contact customer service. Note: Templates are not implantable and should be used for surgical planning only. Pectus Table Top Bender Pectus Introducer Small (18.8 ) Large (20 ) X-large (22.4 ) X Pectus Bender Pectus Bender X-Long Pectus Flipper
11 Warnings and Precautions for Pectus Support Bar System Description The Biomet Microfixation Pectus Support Bar and stabilizers are surgical implants intended to aid treatment of Pectus Excavatum deformity. The Pectus Support Bar provides the surgeon with a means to reposition bony structures (sternum, breastbone) by applying internal force outwardly eliminating the funnel shape deformity. The device should be removed when remodeling is evident. The Pectus Support Bar and stabilizers are made from Stainless Steel, ASTM F 138. Indications Pectus Excavatum and other sternal deformities. Contraindications 1. Patients with mental or neurological conditions who are unwilling or incapable of following instructions. 2. Patients presenting metal sensitivity reactions. 3. Patients with insufficient quantity or quality of bone or fibrous tissue to allow remodeling. 4. Infection Warnings and Precautions The Pectus Support Bar provides the surgeon with a means of treating Pectus Excavatum, funnel chest, a congenital deformity often accompanied by shortness of breath in children. The device is not intended to replace chest wall structures. While the device is intended to expand the chest wall cavity eliminating the features of the deformity, the degree of initial reshaping and permanent remodeling for each case cannot be predetermined. The surgeon is to be thoroughly familiar with the implants and the surgical procedure prior to surgery. The correct selection and placement of the implant is important. Preoperative planning to determine the most appropriate size and final position of the implant is required. The surgeon should avoid sharp bends, reverse bends, or bending the device at a hole. The implant can become dislodged, shift, or flip as a result of improper device selection, improper stabilization, not suturing the device(s), or patient activity too soon after surgery. Even though the implant is mechanically fixed (sutured) in position, care is to be taken to assure that the device is rigidly in apposition to the area of the deformity, as demonstrated by total or partial elimination of the visible deformity. If the deformity is not partially eliminated, a secondary Pectus Support Bar may be required or an alternative method of treatment is to be considered. During the course of the surgical procedure, and during implantation, extreme care is to be taken to avoid contact with the heart and lungs with either the implant or instruments, as contact to these organs can cause death or permanent injury to the patient. When considering removal, the surgeon should weigh the risks verses benefits when deciding when to remove the implant. Where evidence of adequate remolding is present, removal should be performed. Implant removal is to be followed by post operative monitoring to check for reoccurrence of the deformity. Where reoccurrence is encountered, a secondary treatment or alternative treatment maybe necessary. Surgical implants should never be reused. Even though the implant may appear undamaged, it may have imperfections, defects, or internal stress patterns which may lead to breakage or inadequate performance. Patient Warnings Post operative care and monitoring is important. Metallic fixation devices cannot withstand activity levels and loads equal to those placed on a normal healthy chest wall. The implant can loosen, migrate, bend, or break as a result of weight bearing, load bearing, strenuous activity, or traumatic injury. The patient is to be warned by the operating surgeon to limit activities accordingly. Limitation of physical activities may be unique to each patient and the patient should be warned that noncompliance with post operative instructions could lead to complications described above. The patient must be made aware and warned that the deformity or some degree of deformity may be present even after treatment. In addition, the patient is to be warned of general surgical risks and possible adverse effects as listed, prior to surgery.
12 Possible Adverse Effects 1. Metal sensitivity reactions or allergic reaction to the implant material. 2. Pain, discomfort, or abnormal sensation due to the presence of the device. 3. Surgical trauma; permanent or temporary nerve damage, permanent or temporary damage to heart, lungs, and other organs, body structures or tissues. 4. Skin irritation, infection, and pneumothorax. 5. Fracture, breakage, migration, or loosening of the implant. 6. Inadequate or incomplete remodeling of the deformity or return of deformity, prior to or after removal of implant. 7. Permanent injury or death. Sterility Steam sterilize the Pectus Support Bar prior to implantation using steam sterilization equipment which has been properly validated. Following is a recommended minimum cycle for steam sterilization that has been validated by Biomet Microfixation under laboratory conditions. Individual users must validate the cleaning and autoclaving procedures used on-site, including the on-site validation of recommended minimum cycle parameters described below. Pre-vacuumed Steam Sterilization (Hi-VAC) Wrapped: Temperature: Time: Drying Time: 270 Fahrenheit (132º Celsius) Four (4) minutes Thirty (30) minutes MINIMUM Caution: Federal Law (USA) restricts this device to sale by or on the order of a licensed physician. Operating Surgeons and all personnel involved with handling these products are responsible for attaining appropriate education and training within the scope of the activities with which they are involved in the handling and use of this product. Pectus Bar Technique Taken from: 1.Nuss D, Kelly RE, Croitoru D, Katz M. A 10-Year Review of a Minimally Invasive Technique for the Correction of Pectus Excavatum. Journal of Pediatric Surgery, Vol 33, No 4 (April), 1998: pp The Nuss Procedure video, Children s Hospital of the King s Daughters and Eastern Virginia Medical School, Please refer to the product insert for full explanation of warnings and considerations. Strength testing conducted at Biomet Microfixation, Jacksonville, FL. Physicians Address: Donald Nuss, M.B., Ch.B., F.A.C.S., (C), F.A.A.P. 601 Children s Lane, Suite 5B Norfolk, VA Health care personnel bear the ultimate responsibility for ensuring that any packaging method or material, including a reusable rigid container system, is suitable for use in sterilization processing and sterility maintenance in a particular health care facility. Testing should be conducted in the health care facility to assure that conditions essential to sterilization can be achieved. Since Biomet Microfixation is not familiar with individual hospital handling methods, cleaning methods and bioburden, Biomet Microfixation cannot assume responsibility for sterility even though the guideline is followed.
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
(English) NEXUS SPINE SPACER SYSTEM
 (English) NEXUS SPINE SPACER SYSTEM INDICATIONS FOR USE NEXUS Spine Spacer System, a GEO Structure is indicated for use in the thoraco-lumbar spine (i.e., T1 to L5) to replace a diseased vertebral body
(English) NEXUS SPINE SPACER SYSTEM INDICATIONS FOR USE NEXUS Spine Spacer System, a GEO Structure is indicated for use in the thoraco-lumbar spine (i.e., T1 to L5) to replace a diseased vertebral body
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
SPINAL FUSION. North American Spine Society Public Education Series
 SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THYMECTOMY. Thymectomy. Common questions patients ask about thymectomies. www.myasthenia.org
 THYMECTOMY Thymectomy Common questions patients ask about thymectomies. www.myasthenia.org The following are some of the most common questions asked when a thymectomy is being considered for adult and
THYMECTOMY Thymectomy Common questions patients ask about thymectomies. www.myasthenia.org The following are some of the most common questions asked when a thymectomy is being considered for adult and
Blepharoplasty - Eyelid Surgery
 Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
Blepharoplasty - Eyelid Surgery Introduction Eyelid surgery repairs sagging or drooping eyelids. The surgery is also known as blepharoplasty, or an eyelid lift. Sagging or drooping eyelids happen naturally
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Integra. Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE
 Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Instructions for Use
 Pleural Effusion Shunt with External Pump Chamber Catalog No. 42-9005 Instructions for Use Denver Biomedical, Inc. Table of Contents Description 2 Indications 2 Contraindications 2 Warnings 4 Cautions
Pleural Effusion Shunt with External Pump Chamber Catalog No. 42-9005 Instructions for Use Denver Biomedical, Inc. Table of Contents Description 2 Indications 2 Contraindications 2 Warnings 4 Cautions
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Rodding Surgery. 804 W. Diamond Ave., Ste. 210 Gaithersburg, MD 20878 (800) 981-2663 (301) 947-0083
 Rodding Surgery 804 W. Diamond Ave., Ste. 210 Gaithersburg, MD 20878 (800) 981-2663 (301) 947-0083 Fax: (301) 947-0456 Internet: www.oif.org Email: bonelink@oif.org The Osteogenesis Imperfecta Foundation,
Rodding Surgery 804 W. Diamond Ave., Ste. 210 Gaithersburg, MD 20878 (800) 981-2663 (301) 947-0083 Fax: (301) 947-0456 Internet: www.oif.org Email: bonelink@oif.org The Osteogenesis Imperfecta Foundation,
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
BRYAN. Cervical Disc System. Patient Information
 BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
BRYAN Cervical Disc System Patient Information 3 BRYAN Cervical Disc System PATIENT INFORMATION BRYAN Cervical Disc System PATIENT INFORMATION 1 BRYAN Cervical Disc System This patient information brochure
Basic techniques of pulmonary physical therapy (I) 100/04/24
 Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Inferior Vena Cava Filter Placement and Removal
 Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Lentur Cable System. Surgical Technique
 Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
ABDOMINOPLASTY - FREQUENTLY ASKED QUESTIONS (FAQs)
 Executive Level E1, Excen Centre, 119 Willoughby Road, Crows Nest 2065 Tel: 02 9817 7585 www.mycosmeticclinic.net AFFORDABILITY WITH EXCELLENCE Liposuction Breast Augmentation Abdominoplasty Eyelids Surgery
Executive Level E1, Excen Centre, 119 Willoughby Road, Crows Nest 2065 Tel: 02 9817 7585 www.mycosmeticclinic.net AFFORDABILITY WITH EXCELLENCE Liposuction Breast Augmentation Abdominoplasty Eyelids Surgery
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Percutaneous Abscess Drainage
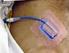 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Titanium Wire with Barb and Needle. For canthal tendon procedures.
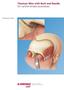 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Breast Reconstruction Frequently Asked Questions
 Breast Reconstruction Frequently Asked Questions GENERAL Do I need to have breast reconstruction? It is never medically necessary to have breast reconstruction. This is considered an elective procedure,
Breast Reconstruction Frequently Asked Questions GENERAL Do I need to have breast reconstruction? It is never medically necessary to have breast reconstruction. This is considered an elective procedure,
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
.org. Distal Radius Fracture (Broken Wrist) Description. Cause
 Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
Distal Radius Fracture (Broken Wrist) Page ( 1 ) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when
A separate consent form for the use of breast implants in conjunction with mastopexy is necessary.
 INFORMED CONSENT BREAST LIFT (MASTOPEXY) INSTRUCTIONS This is an informed consent document that has been prepared to help your plastic surgeon inform you about mastopexy surgery, its risks, and alternative
INFORMED CONSENT BREAST LIFT (MASTOPEXY) INSTRUCTIONS This is an informed consent document that has been prepared to help your plastic surgeon inform you about mastopexy surgery, its risks, and alternative
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Integra. Subtalar MBA Implant
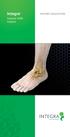 Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
Open Rotator Cuff Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Rotator Cuff Repair is a surgical procedure utilized for a tear in the
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON. Director of surgical department of Lefkos Stavros of Athens
 Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
Laparoscopic hernia repair GEORGIOS SAMPALIS GENERAL SURGEON Director of surgical department of Lefkos Stavros of Athens About 600,000 surgical hernia repair procedures are performed every year... Many
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
Department of Surgery
 Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Patient information for cervical spinal fusion.
 Patient information for cervical spinal fusion. Introduction This booklet has been compiled to help you understand spinal cervical fusion surgery and postoperative rehabilitation. Anatomy The cervical
Patient information for cervical spinal fusion. Introduction This booklet has been compiled to help you understand spinal cervical fusion surgery and postoperative rehabilitation. Anatomy The cervical
The Total Ankle Replacement
 The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-3937 Fax: 314997-3911 Toll Free: 866-869-3937 PEDIACTRIC CATARACT SURGERY A cataract
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
.org. Rotator Cuff Tears: Surgical Treatment Options. When Rotator Cuff Surgery is Recommended. Surgical Repair Options
 Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
Shoulder Replacement Surgery
 In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
In What Activities May I Participate After I Recover? Shoulder Replacement Surgery After undergoing shoulder replacement surgery, it is important to have realistic expectations about the types of activities
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery
 Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
Michael A. Boss, M.D. FMH Plastic, Reconstructive und Aesthetic Surgery Boss Aesthetic Center Schauplatzgasse 23 CH-3011 Bern Switzerland +41 31 311 7691 www.aesthetic-center.com B r e a s t A u g m e
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone:314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 STRABISMUS SURGERY (Post-Op Strabismus
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone:314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 STRABISMUS SURGERY (Post-Op Strabismus
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
The Thorax - Anterior and Lateral Chest Wall
 The Thorax - Anterior and Lateral Chest Wall by Marc Heller,DC When we think of the thorax, most of us think of the thoracic vertebrae and the posterior ribs. When examining for thoracic restrictions,
The Thorax - Anterior and Lateral Chest Wall by Marc Heller,DC When we think of the thorax, most of us think of the thoracic vertebrae and the posterior ribs. When examining for thoracic restrictions,
Elbow Joint Replacement A guide for patients
 Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
Tunneled Central Venous Catheter (CVC) Placement
 PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
Contraindications: Malign or benign strictures in the upper part of esophagus close to the cricopharyngeal muscle.
 Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: volenec@ellacs.cz Instructions for Use FerX-ELLA Esophageal
Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: volenec@ellacs.cz Instructions for Use FerX-ELLA Esophageal
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
CONSTRUCTION WORK and CUMULATIVE TRAUMA DISORDERS
 Connecticut Department of Public Health Environmental and Occupational Health Assessment Program 410 Capitol Avenue MS # 11OSP, PO Box 340308 Hartford, CT 06134-0308 (860) 509-7740 http://www.ct.gov/dph
Connecticut Department of Public Health Environmental and Occupational Health Assessment Program 410 Capitol Avenue MS # 11OSP, PO Box 340308 Hartford, CT 06134-0308 (860) 509-7740 http://www.ct.gov/dph
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
HIP & KNEE SURGERY PATIENTS
 HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System
 *smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
*smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com
 Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Kensington Eye Center 4701 Randolph Road, #G-2 Rockville, MD 20852 (301) 881-5701 www.keceyes.com Natasha L. Herz, MD INFORMED CONSENT FOR DESCEMET S STRIPPING and AUTOMATED ENDOTHELIAL KERATOPLASTY (DSAEK)
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
CHEST TUBES AND CHEST DRAINAGE SYSTEMS
 CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
KnifeLight. Carpal Tunnel Ligament Release. Operative Technique
 KnifeLight Carpal Tunnel Ligament Release Operative Technique Contents Page 1. Features & Benefits 3 Intended Use and Indications 3 Contraindications 3 Features & Benefits 3 2. Operative Technique 4 Antegrade
KnifeLight Carpal Tunnel Ligament Release Operative Technique Contents Page 1. Features & Benefits 3 Intended Use and Indications 3 Contraindications 3 Features & Benefits 3 2. Operative Technique 4 Antegrade
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
SLAP Repair Protocol
 SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
SLAP Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of the scapula
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Lumbar Spine Surgery What to Expect
 Lumbar Spine Surgery What to Expect You have been scheduled for lumbar spine surgery and are probably wondering what to expect with your surgical journey. We will discuss pre- operative tasks, the day
Lumbar Spine Surgery What to Expect You have been scheduled for lumbar spine surgery and are probably wondering what to expect with your surgical journey. We will discuss pre- operative tasks, the day
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
Rotator Cuff Repair Protocol Anatomy and Biomechanics The shoulder is a wonderfully complex joint that is made up of the ball and socket connection between the humerus (ball) and the glenoid portion of
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
INFORMED CONSENT FOR SLEEVE GASTRECTOMY
 INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery.
 Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
