IHCP banner page. Laboratory fee pricing available for CPT code 88112
|
|
|
- Martin Oliver
- 10 years ago
- Views:
Transcription
1 IHCP banner page INDIANA HEALTH COVERAGE PROGRAMS BR JUNE 3, 2014 Laboratory fee pricing available for CPT code Effective July 7, 2014, the Indiana Health Coverage Programs (IHCP) will update the pricing for Current Procedural Terminology (CPT 1 ) code Cytopathology, selective cellular enhancement technique with interpretation (e.g., liquid based slide preparation method), except cervical or vaginal to include lab fee pricing. The pricing update applies retroactively to dates of service (DOS) on or after July 1, MORE IN THIS ISSUE Beginning July 7, 2014, claims for CPT code billed with one of the following revenue codes that previously denied for explanation of benefits (EOB) Laboratory CPT codes linked to 6000 Manual pricing required may be resubmitted for dates of service on or revenue codes 300 and 309 after July 1, HCPCS code A9520 linked to 310 Pathology lab revenue code Pathology/cytology Medical and medical crossover 319 Pathology/other claims denied for edit 6637 Claims beyond the original one-year filing limit must include a copy of this Banner Clarification of FFS timely filing Page as an attachment and must be filed within one year of the publication date. limitation 1 CPT copyright 2012 American Medical Association. All rights reserved. CPT is a registered trademark of the American Medical Association. EHR Incentive Program documentation requirements Page 1 of 5
2 Laboratory CPT codes linked to revenue codes 300 and 309 Effective July 7, 2014, the Indiana Health Coverage Programs (IHCP) will link the Current Procedural Terminology (CPT) codes in Table 1 to one or both of the following revenue codes: 300 Laboratory-General 309 Laboratory-Other Laboratory CPT codes 89049, 99000, and will also have laboratory fee pricing added. Both the revenue code linkages and the laboratory fee pricing apply retroactively to dates of service (DOS) on or after July 1, Table 1 CPT codes linked to revenue codes 300 and 309 for DOS on or after July 1, 2013 Procedure Code Description Revenue Code Linkage Oncoprotein; des-gamma-carboxy-prothrombin (DCP) 300 and Allergen specific IgG quantitative or semiquantitative, each allergen 300 and Caffeine halothane contracture test (CHCT) for malignant hyperthermia susceptibility, including interpretation and report Handling and/or conveyance of specimen for transfer from the office to a laboratory Handling and/or conveyance of specimen for transfer from the patient in other than an office to a laboratory (distance may be indicated) 300 and Beginning July 7, 2014, for reimbursement consideration, providers may bill the procedure codes and revenue codes together, as appropriate, for DOS on or after July 1, Claims for these procedure codes that previously denied for invalid revenue code combinations or no pricing on file may be resubmitted. Claims beyond the original one-year filing limit must include a copy of this Banner Page as an attachment and must be filed within one year of the publication date. HCPCS code A9520 linked to revenue code 343 Effective July 7, 2014, the Indiana Health Coverage Programs (IHCP) will link Healthcare Common Procedure Coding System (HCPCS) code A9520 Technetium tc-99m, tilmanocept, diagnostic, up to 0.5 millicuries to revenue code 343 Nuclear Medicine-Diagnostic Radiopharmaceuticals. This linkage applies retroactively to dates of service (DOS) on or after July 1, Beginning July 7, 2014, for reimbursement consideration, providers may bill HCPCS code A9520 and revenue code 343 together, as appropriate, for DOS on or after July 1, Claims for procedure code A9520 with revenue code 343 that previously denied for explanation of benefits (EOB) 520 Invalid revenue code and procedure code combination may be resubmitted. Claims beyond the original one-year filing limit must include a copy of this Banner Page as an attachment and must be filed within one year of the publication date. Page 2 of 5
3 Medical and medical crossover claims denied for edit 6637 to be reprocessed or adjusted Medical and medical crossover claims billed with the Current Procedural Terminology (CPT) codes in Table 2 erroneously denied for edit 6637 Drug administration not payable on the same date of service as an evaluation and management service. Denials affected claims with dates of service from January 1, 2013, through July 3, Table 2 CPT codes erroneously denied for edit 6637 for DOS from January 1, 2013, through July 3, 2014 CPT Code Description Immunization Administration (includes percutaneous, intradermal, subcutaneous, or intramuscular injections); each additional vaccine (single or combination vaccine/toxoid) (list separately in addition to code for primary procedure) Immunization administration by intranasal or oral route; one vaccine (single or combination vaccine/toxoid) Immunization administration by intranasal or oral route; each additional vaccine (single or combination vaccine/toxoid) (list separately in addition to code for primary procedure) Claims for these procedure codes that denied or claims that paid with a denied detail line for edit 6637 will be mass reprocessed or mass adjusted. Reprocessed or adjusted claims will begin appearing on Remittance Advice (RA) statements dated July 15, 2014, identified by internal control numbers (ICNs) that begin with a region code of 80 (mass reprocessed) or 56 (mass adjusted). Any overpayment will appear as an accounts receivable. The accounts receivable will be recouped at 100% from future claims paid to the respective provider number. Clarification of FFS timely filing limitation on claims due to retroactive coverage and billing changes The Indiana Health Coverage Programs (IHCP) policy imposes a one-year timely filing limit on all fee-for-service (FFS) claims. Current policy requires providers to file a claim within one year from the date of service. If a provider files a claim beyond the one-year limitation, the provider must submit acceptable documentation justifying the extension. Chapter 10 of the IHCP Provider Manual provides additional information regarding timely filing and acceptable documentation required to waive the limit. Providers are reminded that the timely filing policy applies to claims affected by retroactive coverage notices and reimbursement or billing changes issued by the IHCP. If retroactive changes allow for an extension of the original one-year filing limit, any resulting claim submission or resubmission is subject to a one-year filing limit based on the date of the publication in which the retroactive change is announced. Claims filed beyond the original one-year filing limit due to retroactive IHCP changes must include a copy of the related provider publication (IHCP Bulletin or Banner Page) as an attachment. For reimbursement consideration, the claim must be submitted within one year of the date of that publication. Page 3 of 5
4 Indiana EHR Incentive Program documentation requirements updated For Program Year 2014, Indiana requires that all providers participating in the Indiana Electronic Health Records (EHR) Incentive Program submit documentation as outlined in Table 3. Table 3 Required documentation for the Indiana EHR Incentive Program in Program Year 2014 Providers Year 1 Years 2-6 Eligible providers Eligible hospitals 1. Acceptable documentation as proof of relationship between provider and EHR vendor * 2. Documentation from the Office of the National Coordinator for Health IT (ONC) showing proof of certified EHR technology. ** 3. The Indiana EHR pre-payment review team will request documentation supporting the provider s current submission of patient volume for variances greater than 20%, as compared to the Medicaid Management Information System (MMIS). 4. If the provider is attesting to public health 1. Medicare Cost Report spreadsheet 2. Acceptable documentation as proof of relationship between provider and EHR vendor * 3. Documentation from the Office of the National Coordinator for Health IT (ONC) showing proof of certified EHR technology. ** 4. The Indiana EHR pre-payment review team will request documentation supporting the provider s current submission of patient volume for variances greater than 20%, as compared to the Medicaid Management Information System (MMIS). 5. If the provider is attesting to public health 1. Documentation from the Office of the National Coordinator for Health IT (ONC) showing proof of certified EHR technology. ** 2. The Indiana EHR pre-payment review team will request documentation supporting the provider s current submission of patient volume for variances greater than 20%, as compared to the Medicaid Management Information System (MMIS). 3. If the provider is attesting to public health 1. Documentation from the Office of the National Coordinator for Health IT (ONC) showing proof of certified EHR technology. ** 2. The Indiana EHR pre-payment review team will request documentation supporting the provider s current submission of patient volume for variances greater than 20%, as compared to the Medicaid Management Information System (MMIS). 3. If the provider is attesting to public health Notes * Acceptable documentation refers to the certified EHR technology by name and certification number, and includes financial and/or contractual commitment. Examples include the EHR contract, invoice, or receipt that includes provider name and point of contact; vendor name and point of contact; and CEHRT name, version, and ONC-issued CEHRT ID. ** Proof must verify that the current CEHRT version meets program year requirements. A screen shot from the ONC website is acceptable proof. *** Providers that report public health measures will receive confirmation of registration and/or submission from the ISDH, and should scan and upload this confirmation as documentation for the EHR attestation. continued Page 4 of 5
5 If you have questions regarding these documentation requirements or the Indiana EHR attestation process, please contact Indiana Medicaid EHR Customer Service via at or call QUESTIONS? If you have questions about this publication, please contact Customer Assistance at COPIES OF THIS PUBLICATION If you need additional copies of this publication, please download them from indianamedicaid.com. SIGN UP FOR IHCP NOTIFICATIONS To receive notices of IHCP publications, subscribe by clicking the blue subscription envelope here or on the pages of indianamedicaid.com. TO PRINT A printer-friendly version of this publication, in black and white and without graphics, is available for your convenience. Page 5 of 5
Completing Your MPIP Attestation: Supporting Documentation
 Overview This tip sheet provides examples of the types of supporting documentation that may be requested during a pre-payment review in order to verify an eligible professional's (EP) or eligible hospital's
Overview This tip sheet provides examples of the types of supporting documentation that may be requested during a pre-payment review in order to verify an eligible professional's (EP) or eligible hospital's
Home Health, Hospice and Long-Term Care. HP Provider Relations/October 2015
 Home Health, Hospice and Long-Term Care HP Provider Relations/October 2015 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Home Health, Hospice and Long-Term Care HP Provider Relations/October 2015 Agenda Claim inquiry on Web interchange By member number and date of service Understand claim status information, disposition,
Instructions for submitting Claim Reconsideration Requests
 Instructions for submitting Claim Reconsideration Requests A Claim Reconsideration Request is typically the quickest way to address any concern you have with how we processed your claim. With a Claim Reconsideration
Instructions for submitting Claim Reconsideration Requests A Claim Reconsideration Request is typically the quickest way to address any concern you have with how we processed your claim. With a Claim Reconsideration
INSTRUCTIONS FOR REPORTING IMMUNIZATION SERVICES TO THIRD PARTY PAYERS (Billing Guide)
 INSTRUCTIONS FOR REPORTING IMMUNIZATION SERVICES TO THIRD PARTY PAYERS (Billing Guide) NOTE: All italicized words or phrases are defined at the end of this document. Adults (19 years of age and older)
INSTRUCTIONS FOR REPORTING IMMUNIZATION SERVICES TO THIRD PARTY PAYERS (Billing Guide) NOTE: All italicized words or phrases are defined at the end of this document. Adults (19 years of age and older)
Immunization Coding and Billing Basics
 Immunization Billing Project Webinar Session - II Immunization Coding and Billing Basics September 26, 2013 PRESENTED BY CHRIS PERKEY, RN, CMPE SENIOR CONSULTANT CONSULTING AND PRACTICE MANAGEMENT SERVICES
Immunization Billing Project Webinar Session - II Immunization Coding and Billing Basics September 26, 2013 PRESENTED BY CHRIS PERKEY, RN, CMPE SENIOR CONSULTANT CONSULTING AND PRACTICE MANAGEMENT SERVICES
Chapter 10: Claims Processing Procedures
 I N D I A N A H E A L T H C O V E R A G E P R O G R A M S P R O V I D E R M A N U A L Chapter 10: Claims Processing Procedures Library Reference Number: PRPR10004 10-1 Chapter 10: Revision History Version
I N D I A N A H E A L T H C O V E R A G E P R O G R A M S P R O V I D E R M A N U A L Chapter 10: Claims Processing Procedures Library Reference Number: PRPR10004 10-1 Chapter 10: Revision History Version
Molina Healthcare of Washington, Inc. CLAIMS
 CLAIMS As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your reference:
CLAIMS As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your reference:
Qtr 2. 2011 Provider Update Bulletin
 West Virginia Medicaid WEST VIRGINIA Department of Health & Human Resources Qtr 2. 2011 Provider Update Bulletin West Virginia Medicaid Provider Update Bulletin Qtr. 2, 2011 Volume 1 Inside This Issue:
West Virginia Medicaid WEST VIRGINIA Department of Health & Human Resources Qtr 2. 2011 Provider Update Bulletin West Virginia Medicaid Provider Update Bulletin Qtr. 2, 2011 Volume 1 Inside This Issue:
Medical Practitioner Reimbursement
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Medical Practitioner Reimbursement L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 6 P U B L I S H E D : F E B R U A R Y 25,
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Medical Practitioner Reimbursement L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 6 P U B L I S H E D : F E B R U A R Y 25,
CHAPTER 7 (E) DENTAL PROGRAM CLAIMS FILING CHAPTER CONTENTS
 CHAPTER 7 (E) DENTAL PROGRAM CHAPTER CONTENTS 7.0 CLAIMS SUBMISSION AND PROCESSING...1 7.1 ELECTRONIC MEDIA CLAIMS (EMC) FILING...1 7.2 CLAIMS DOCUMENTATION...2 7.3 THIRD PARTY LIABILITY (TPL)...2 7.4
CHAPTER 7 (E) DENTAL PROGRAM CHAPTER CONTENTS 7.0 CLAIMS SUBMISSION AND PROCESSING...1 7.1 ELECTRONIC MEDIA CLAIMS (EMC) FILING...1 7.2 CLAIMS DOCUMENTATION...2 7.3 THIRD PARTY LIABILITY (TPL)...2 7.4
Surgical/ASC Claims Revenue Cycle Management: An Introduction to Our Processes and Protocols
 Surgical/ASC Claims Revenue Cycle Management: An Introduction to Our Processes and Protocols 200 Old Country Road, Suite 470 Mineola, NY 11501 Phone: 516-294-4118 Fax: 516-294-9268 www.businessdynamicslimited.com
Surgical/ASC Claims Revenue Cycle Management: An Introduction to Our Processes and Protocols 200 Old Country Road, Suite 470 Mineola, NY 11501 Phone: 516-294-4118 Fax: 516-294-9268 www.businessdynamicslimited.com
Medicaid. Important Contact Information. In This Issue
 In This Issue Medicare & Medicaid Limitations Page 2 Resubmitting Denied Claims Page 2 Certain DME Under $50 Require PA Page 3 Top Reasons Claims are Returned to Providers Page 4 Medicaid New Medicaid
In This Issue Medicare & Medicaid Limitations Page 2 Resubmitting Denied Claims Page 2 Certain DME Under $50 Require PA Page 3 Top Reasons Claims are Returned to Providers Page 4 Medicaid New Medicaid
Provider Adjustment, Time limit & Medicare Override Job Aid
 Provider Adjustment, Time limit & Medicare Override Job Aid Contents Overview... 1 Medicaid Resolution Inquiry Form... 1 Medicare Overrides... 3 Time Limit Overrides... 3 Adjusting a Claim through the
Provider Adjustment, Time limit & Medicare Override Job Aid Contents Overview... 1 Medicaid Resolution Inquiry Form... 1 Medicare Overrides... 3 Time Limit Overrides... 3 Adjusting a Claim through the
2010 BCBSNC Provider Conference Top 20 Questions Answers
 Questions Answers There is currently no centralized listing of all out-of-state Blue Plan alpha prefixes. There is a listing available for BCBSNC alpha prefixes only; please contact your Provider Relations
Questions Answers There is currently no centralized listing of all out-of-state Blue Plan alpha prefixes. There is a listing available for BCBSNC alpha prefixes only; please contact your Provider Relations
Billing Medicaid as a Secondary Payer. Provider Relations / Second quarter 2015
 Billing Medicaid as a Secondary Payer Provider Relations / Second quarter 2015 Agenda Other Coverage How to Identify Other Coverage and Request Coverage Updates Medicare Crossover Claims Third-Party Liability
Billing Medicaid as a Secondary Payer Provider Relations / Second quarter 2015 Agenda Other Coverage How to Identify Other Coverage and Request Coverage Updates Medicare Crossover Claims Third-Party Liability
Understanding Your Role in Maximizing Revenue in a FQHC
 Understanding Your Role in Maximizing Revenue in a FQHC Cynthia M Patterson President N Charleston SC 29420-1093 [email protected] P: (843) 597-8437 F: (888) 697-8923 Have systems
Understanding Your Role in Maximizing Revenue in a FQHC Cynthia M Patterson President N Charleston SC 29420-1093 [email protected] P: (843) 597-8437 F: (888) 697-8923 Have systems
Competitive Acquisition Program (CAP) for Part B Drugs & Biologicals Training for Supplemental Insurance Companies August 2007
 Competitive Acquisition Program (CAP) for Part B Drugs & Biologicals Training for Supplemental Insurance Companies August 2007 DISCLAIMER This information release is the property of Noridian Administrative
Competitive Acquisition Program (CAP) for Part B Drugs & Biologicals Training for Supplemental Insurance Companies August 2007 DISCLAIMER This information release is the property of Noridian Administrative
Understanding Meaningful Use. Review of Part 1 and Part 2
 Understanding Meaningful Use Review of Part 1 and Part 2 Understanding Meaningful Use Pat Wise RN, MA, MS, FHIMSS COL (USA ret'd) Vice President, Healthcare Information Systems Meaningful Use Financial
Understanding Meaningful Use Review of Part 1 and Part 2 Understanding Meaningful Use Pat Wise RN, MA, MS, FHIMSS COL (USA ret'd) Vice President, Healthcare Information Systems Meaningful Use Financial
Wisconsin Medicaid Electronic Health Record Incentive Program for Eligible Hospitals
 P-00358D Wisconsin Medicaid Electronic Health Record Incentive Program for Eligible Hospitals User Guide i Table of Contents 1 Introduction... 1 2 Before You Begin... 2 2.1 Register with Centers for Medicare
P-00358D Wisconsin Medicaid Electronic Health Record Incentive Program for Eligible Hospitals User Guide i Table of Contents 1 Introduction... 1 2 Before You Begin... 2 2.1 Register with Centers for Medicare
Claims and Billing Process. AHCCCS Provider Identification Number and NPI Number
 Claims and Billing Process AHCCCS Provider Identification Number and NPI Number All United Healthcare Community Plan providers requesting reimbursement for services must be properly registered with AHCCCS
Claims and Billing Process AHCCCS Provider Identification Number and NPI Number All United Healthcare Community Plan providers requesting reimbursement for services must be properly registered with AHCCCS
REV - Disallowance Procedure
 REV - Disallowance Procedure Purpose: conducts disallowance cycles to recover funds from providers where Medicaid paid the provider, but the member has access to Medicare or commercial insurance covering
REV - Disallowance Procedure Purpose: conducts disallowance cycles to recover funds from providers where Medicaid paid the provider, but the member has access to Medicare or commercial insurance covering
HEALTH DEPARTMENT BILLING GUIDELINES
 HEALTH DEPARTMENT BILLING GUIDELINES Acknowledgement: Current Procedural Terminology (CPT ) is copyright 2015 American Medical Association. All Rights Reserved. No fee schedules, basic units, relative
HEALTH DEPARTMENT BILLING GUIDELINES Acknowledgement: Current Procedural Terminology (CPT ) is copyright 2015 American Medical Association. All Rights Reserved. No fee schedules, basic units, relative
The Ins and Outs of Coding Vaccines
 The Ins and Outs of Coding Vaccines When it comes to reporting vaccines provided in an outpatient setting, correct coding is not always a simple process. Patients frequently require more than one vaccine
The Ins and Outs of Coding Vaccines When it comes to reporting vaccines provided in an outpatient setting, correct coding is not always a simple process. Patients frequently require more than one vaccine
SECTION 7: APPEALS TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1
 TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 SECTION 7: APPEALS 7.1 Appeal Methods................................................................. 7-2 7.1.1 Electronic Appeal Submission.......................................................
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 SECTION 7: APPEALS 7.1 Appeal Methods................................................................. 7-2 7.1.1 Electronic Appeal Submission.......................................................
Checklist and Related Guidance for Meaningful Use Audits
 Checklist and Related Guidance for Meaningful Use Audits This checklist was prepared by Jill M. Girardeau, Partner, Womble Carlyle Sandridge & Rice, LLP and Dina Marty, Counsel, Wake Forest Baptist Medical
Checklist and Related Guidance for Meaningful Use Audits This checklist was prepared by Jill M. Girardeau, Partner, Womble Carlyle Sandridge & Rice, LLP and Dina Marty, Counsel, Wake Forest Baptist Medical
Wisconsin Medicaid Electronic Health Record Incentive Program for Eligible Professionals
 P- Wisconsin Medicaid Electronic Health Record Incentive Program for Eligible Professionals June 15,2015 User Guide i Table of Contents 1 Introduction... 1 2 Before You Begin... 2 2.1 Register
P- Wisconsin Medicaid Electronic Health Record Incentive Program for Eligible Professionals June 15,2015 User Guide i Table of Contents 1 Introduction... 1 2 Before You Begin... 2 2.1 Register
interchange Provider Important Message
 Q How do I start to create a new claim? Q How do I select the appropriate claim type within the claim if I ve chosen Institutional claim type? Q How do I learn what each field on the internet claim means?
Q How do I start to create a new claim? Q How do I select the appropriate claim type within the claim if I ve chosen Institutional claim type? Q How do I learn what each field on the internet claim means?
Healthcare Claiming. Help Desk Q&A, Reports and Claiming Tips. Presenter: Stacey Alsdurf. SSIS Fiscal Mentor Meeting Healthcare Claiming 02/11/15
 Healthcare Claiming Help Desk Q&A, Reports and Claiming Tips Presenter: Stacey Alsdurf 1 Presentation Overview Healthcare Claim Proofing Reprocessing Healthcare Claims Using Reports in SSIS Claiming Tips
Healthcare Claiming Help Desk Q&A, Reports and Claiming Tips Presenter: Stacey Alsdurf 1 Presentation Overview Healthcare Claim Proofing Reprocessing Healthcare Claims Using Reports in SSIS Claiming Tips
Online Claim Entry UB-04. Presented by: Xerox State Healthcare, LLC Provider Relations
 Online Claim Entry UB-04 Presented by: Xerox State Healthcare, LLC Provider Relations Resources When online use: Ask Service Representative [email protected] [email protected] Call Center 505-246-0710
Online Claim Entry UB-04 Presented by: Xerox State Healthcare, LLC Provider Relations Resources When online use: Ask Service Representative [email protected] [email protected] Call Center 505-246-0710
How to read the paper remittance advice. How to review claim and adjustment information How to correct overpayments and underpayments
 How to read the paper remittance advice How to review claim and adjustment information How to correct overpayments and underpayments Overview DMAP mails the paper Remittance Advice (RA) weekly. It tells
How to read the paper remittance advice How to review claim and adjustment information How to correct overpayments and underpayments Overview DMAP mails the paper Remittance Advice (RA) weekly. It tells
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201503 JANUARY 27, 2015
 IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201503 JANUARY 27, 2015 FSSA announces the NEW Healthy Indiana Plan! Coverage for qualifying Hoosiers will start effective Feb. 1, 2015 The Indiana Family
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201503 JANUARY 27, 2015 FSSA announces the NEW Healthy Indiana Plan! Coverage for qualifying Hoosiers will start effective Feb. 1, 2015 The Indiana Family
! Claims and Billing Guidelines
 ! Claims and Billing Guidelines Electronic Claims Clearinghouses and Vendors 16.1 Electronic Billing 16.2 Institutional Claims and Billing Guidelines 16.3 Professional Claims and Billing Guidelines 16.4
! Claims and Billing Guidelines Electronic Claims Clearinghouses and Vendors 16.1 Electronic Billing 16.2 Institutional Claims and Billing Guidelines 16.3 Professional Claims and Billing Guidelines 16.4
Chapter 5: Third Party Liability
 I N D I A N A H E A L T H C O V E R A G E P R O G R A M S P R O V I D E R M A N U A L Chapter 5: Third Party Liability Library Reference Number: PRPR10004 5-1 Document Version Number Version 1.0 September,
I N D I A N A H E A L T H C O V E R A G E P R O G R A M S P R O V I D E R M A N U A L Chapter 5: Third Party Liability Library Reference Number: PRPR10004 5-1 Document Version Number Version 1.0 September,
Telehealth Services Billing Overview. Kathy J. Chorba California Telehealth Resource Center [email protected]
 Telehealth Services Billing Overview Kathy J. Chorba California Telehealth Resource Center [email protected] Senate Bill 1665 Telemedicine Development Act of 1996 Mandated all payers develop a
Telehealth Services Billing Overview Kathy J. Chorba California Telehealth Resource Center [email protected] Senate Bill 1665 Telemedicine Development Act of 1996 Mandated all payers develop a
PENNSYLVANIA MEDICAL ASSISTANCE EHR INCENTIVE PROGRAM ELIGIBLE HOSPITAL PROVIDER MANUAL
 Eligible Hospital Provider Manual v.3.1 PENNSYLVANIA MEDICAL ASSISTANCE EHR INCENTIVE PROGRAM ELIGIBLE HOSPITAL PROVIDER MANUAL UPDATED: OCTOBER 19, 2015 1 Eligible Hospital Provider Manual v.3.1 Contents
Eligible Hospital Provider Manual v.3.1 PENNSYLVANIA MEDICAL ASSISTANCE EHR INCENTIVE PROGRAM ELIGIBLE HOSPITAL PROVIDER MANUAL UPDATED: OCTOBER 19, 2015 1 Eligible Hospital Provider Manual v.3.1 Contents
Behavioral Health Provider Training: Substance Abuse Treatment Updates
 Behavioral Health Provider Training: Substance Abuse Treatment Updates Agenda Laboratory Services Behavioral Health Claims Submission Process Targeted Case Management Utilization Management eservices Claims
Behavioral Health Provider Training: Substance Abuse Treatment Updates Agenda Laboratory Services Behavioral Health Claims Submission Process Targeted Case Management Utilization Management eservices Claims
TABLE OF CONTENTS. Claims Processing & Provider Compensation
 TABLE OF CONTENTS Claims Address... 2 Claim Submission... 2 Claim Payment... 2 Claim Payment Adjustments.... 2 Claim Disputes... 2 Recovery of Overpayments... 3 Balance Billing... 3 Annual Health Assessment
TABLE OF CONTENTS Claims Address... 2 Claim Submission... 2 Claim Payment... 2 Claim Payment Adjustments.... 2 Claim Disputes... 2 Recovery of Overpayments... 3 Balance Billing... 3 Annual Health Assessment
Florida Medicaid EHR Incentive Program. Eligible Hospitals
 Florida Medicaid EHR Incentive Program Eligible Hospitals What? Health Information Technology Economic and Clinical Health Act aka ARRA aka Stimulus $2 billion for the creation of state level Health Information
Florida Medicaid EHR Incentive Program Eligible Hospitals What? Health Information Technology Economic and Clinical Health Act aka ARRA aka Stimulus $2 billion for the creation of state level Health Information
To start the pre-approval process, providers must fill out a short online survey, available at: https://www.surveymonkey.com/s/hrszft2.
 Maryland Medicaid EHR Incentive Program Attestation Form for Eligible Providers to Meet Program Requirements Under the Certified Electronic Health Record (CEHRT) Flexibility Rule for Program Year 2014
Maryland Medicaid EHR Incentive Program Attestation Form for Eligible Providers to Meet Program Requirements Under the Certified Electronic Health Record (CEHRT) Flexibility Rule for Program Year 2014
Institutional Claim Billing Reimbursement. HP Provider Relations/October 2013
 Institutional Claim Billing Reimbursement HP Provider Relations/October 2013 Agenda Objectives Institutional Claim Basics Inpatient Claim Payment Outpatient Claim Payment Enhanced Code Auditing Billing
Institutional Claim Billing Reimbursement HP Provider Relations/October 2013 Agenda Objectives Institutional Claim Basics Inpatient Claim Payment Outpatient Claim Payment Enhanced Code Auditing Billing
Electronic Health Record Incentive Program Update May 29, 2015. Florida Health Information Exchange Coordinating Committee
 Electronic Health Record Incentive Program Update May 29, 2015 Florida Health Information Exchange Coordinating Committee Topics Payment Data Participation Years and Payments Meaningful Use Progression
Electronic Health Record Incentive Program Update May 29, 2015 Florida Health Information Exchange Coordinating Committee Topics Payment Data Participation Years and Payments Meaningful Use Progression
Handbook for Providers of Therapy Services
 Handbook for Providers of Therapy Services Chapter J-200 Policy and Procedures For Therapy Services Illinois Department of Healthcare and Family Services CHAPTER J-200 THERAPY SERVICES TABLE OF CONTENTS
Handbook for Providers of Therapy Services Chapter J-200 Policy and Procedures For Therapy Services Illinois Department of Healthcare and Family Services CHAPTER J-200 THERAPY SERVICES TABLE OF CONTENTS
To submit electronic claims, use the HIPAA 837 Institutional transaction
 3.1 Claim Billing 3.1.1 Which Claim Form to Use Claims that do not require attachments may be billed electronically using Provider Electronic Solutions (PES) software (provided by Electronic Data Systems
3.1 Claim Billing 3.1.1 Which Claim Form to Use Claims that do not require attachments may be billed electronically using Provider Electronic Solutions (PES) software (provided by Electronic Data Systems
MEDICAL ASSISTANCE BULLETIN
 ISSUE DATE September 12, 2014 SUBJECT EFFECTIVE DATE September 15, 2014 MEDICAL ASSISTANCE BULLETIN NUMBER 99-14-08 BY Implementation of National Correct Coding Initiative Related Modifiers Vincent D.
ISSUE DATE September 12, 2014 SUBJECT EFFECTIVE DATE September 15, 2014 MEDICAL ASSISTANCE BULLETIN NUMBER 99-14-08 BY Implementation of National Correct Coding Initiative Related Modifiers Vincent D.
Claims Procedures. H.2 At a Glance. H.4 Submission Guidelines. H.9 Claims Documentation. H.17 Codes and Modifiers. H.
 H.2 At a Glance H.4 Submission Guidelines H.9 Claims Documentation H.17 Codes and Modifiers H.22 Reimbursement H.25 Denials and Appeals At a Glance pledges to provide accurate and efficient claims processing.
H.2 At a Glance H.4 Submission Guidelines H.9 Claims Documentation H.17 Codes and Modifiers H.22 Reimbursement H.25 Denials and Appeals At a Glance pledges to provide accurate and efficient claims processing.
Submitting Special Batch Claims and Claim Appeals
 Submitting Special Batch Claims and Claim Appeals Nevada Medicaid and Nevada Check Up August 2013 2012 Hewlett-Packard Development Company, L.P. The information contained herein is subject to change without
Submitting Special Batch Claims and Claim Appeals Nevada Medicaid and Nevada Check Up August 2013 2012 Hewlett-Packard Development Company, L.P. The information contained herein is subject to change without
AAP Meaningful Use: Certified EHR Technology Criteria
 AAP Meaningful Use: Certified EHR Technology Criteria On July 13, 2010, the US Centers for Medicare and Medicaid Services (CMS) released a Final Rule establishing the criteria with which eligible pediatricians,
AAP Meaningful Use: Certified EHR Technology Criteria On July 13, 2010, the US Centers for Medicare and Medicaid Services (CMS) released a Final Rule establishing the criteria with which eligible pediatricians,
Provider Notification
 Provider Notification Date of Notification June 1, 2012 Revision Date N/A Plans Affected All Lines of Business Subject Notice of Change to Billing Requirements for Drugs Administered in Outpatient Clinical
Provider Notification Date of Notification June 1, 2012 Revision Date N/A Plans Affected All Lines of Business Subject Notice of Change to Billing Requirements for Drugs Administered in Outpatient Clinical
Harbor s Payment to Providers Policy and Procedures is available on the Harbor website and will be updated annually or as changes are necessary.
 Original Approval Date: 01/31/2006 Page 1 of 10 I. SCOPE The scope of this policy involves all Harbor Health Plan, Inc. (Harbor) contracted and non-contracted Practitioners/Providers; Harbor s Contract
Original Approval Date: 01/31/2006 Page 1 of 10 I. SCOPE The scope of this policy involves all Harbor Health Plan, Inc. (Harbor) contracted and non-contracted Practitioners/Providers; Harbor s Contract
Access to Health Insurance Invoice Process
 Access to Health Insurance Invoice Process Invoicing Guidelines The Department will send the premium payment reimbursement directly to the Insurance Company. The Insurance Company collects the rest of
Access to Health Insurance Invoice Process Invoicing Guidelines The Department will send the premium payment reimbursement directly to the Insurance Company. The Insurance Company collects the rest of
How to Use the Medicare National Correct Coding Initiative (NCCI) Tools
 DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services R How to Use the Medicare National Correct Coding Initiative (NCCI) Tools Knowing how to look up Medicare NCCI code pair
DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services R How to Use the Medicare National Correct Coding Initiative (NCCI) Tools Knowing how to look up Medicare NCCI code pair
CPT Consumer Friendly Descriptors: Their Use in Engaging Patients in their Health Care
 CPT Consumer Friendly Descriptors: Their Use in Engaging Patients in their Health Care Speakers Nancy Spector, BSN, MSC AMA Electronic Medical Systems Elizabeth Lumakovska, MPA, RHIT, CPEHR AMA Medical
CPT Consumer Friendly Descriptors: Their Use in Engaging Patients in their Health Care Speakers Nancy Spector, BSN, MSC AMA Electronic Medical Systems Elizabeth Lumakovska, MPA, RHIT, CPEHR AMA Medical
Introduction. Table of Contents
 Table of Contents Introduction... 2 Billing Project Background... 2 Immunization Billing Manual Developed... 3 Topics in the Manual... 4 Section 1 - Participating Provider Application Process... 4 Section
Table of Contents Introduction... 2 Billing Project Background... 2 Immunization Billing Manual Developed... 3 Topics in the Manual... 4 Section 1 - Participating Provider Application Process... 4 Section
Third Party Liability
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Third Party Liability L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 7 P U B L I S H E D : F E B R U A R Y 2 5, 2 0 1 6 P
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER REFERENCE M ODULE Third Party Liability L I B R A R Y R E F E R E N C E N U M B E R : P R O M O D 0 0 0 1 7 P U B L I S H E D : F E B R U A R Y 2 5, 2 0 1 6 P
101 CMR: EXECUTIVE OFFICE OF HEALTH AND HUMAN SERVICES 101 CMR 312.00: FAMILY PLANNING SERVICES
 101 CMR 312.00: FAMILY PLANNING SERVICES Section 312.01: General Provisions 312.02: General Definitions 312.03: General Rate Provisions 312.04: Reporting Requirements 312.05: Severability 312.01: General
101 CMR 312.00: FAMILY PLANNING SERVICES Section 312.01: General Provisions 312.02: General Definitions 312.03: General Rate Provisions 312.04: Reporting Requirements 312.05: Severability 312.01: General
Laboratory and Radiology
 Physician Services Laboratory and Radiology Contacting Wisconsin Medicaid Web Site dhfs.wisconsin.gov/ The Web site contains information for providers and recipients about the following: Program requirements.
Physician Services Laboratory and Radiology Contacting Wisconsin Medicaid Web Site dhfs.wisconsin.gov/ The Web site contains information for providers and recipients about the following: Program requirements.
Preview of the Attestation System for the Medicare Electronic Health Record (EHR) Incentive Program
 Preview of the Attestation System for the Medicare Electronic Health Record (EHR) Incentive Program The Medicare EHR Incentive Program provides incentive payments to eligible professionals, eligible hospitals
Preview of the Attestation System for the Medicare Electronic Health Record (EHR) Incentive Program The Medicare EHR Incentive Program provides incentive payments to eligible professionals, eligible hospitals
ARChoices. HPE Fiscal Agent for the Arkansas Division of Medical Services. September 2016
 ARChoices HPE Fiscal Agent for the Arkansas Division of Medical Services September 2016 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and Voids Current CPT Codes
ARChoices HPE Fiscal Agent for the Arkansas Division of Medical Services September 2016 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and Voids Current CPT Codes
Revenue Cycle Management Process
 OVERVIEW It is important for everyone involved in the billing cycle process to be familiar with how each step of the encounter provides opportunities to assure successful and compliant billing. The purpose
OVERVIEW It is important for everyone involved in the billing cycle process to be familiar with how each step of the encounter provides opportunities to assure successful and compliant billing. The purpose
Connecticut Medical Assistance Program Refresher for Home Health Providers. Presented by The Department of Social Services & HP for Billing Providers
 Connecticut Medical Assistance Program Refresher for Home Health Providers Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Home Health Agenda Fee Schedule Update
Connecticut Medical Assistance Program Refresher for Home Health Providers Presented by The Department of Social Services & HP for Billing Providers 1 Training Topics Home Health Agenda Fee Schedule Update
Eligible Professionals User Guide for the Georgia Medicaid EHR Incentive Program
 Introduction Eligible Professionals User Guide for the Georgia Medicaid EHR Incentive Program Version 1.0 September 5, 2011 1 Introduction Table of Contents Introduction... 3 How to apply for the Georgia
Introduction Eligible Professionals User Guide for the Georgia Medicaid EHR Incentive Program Version 1.0 September 5, 2011 1 Introduction Table of Contents Introduction... 3 How to apply for the Georgia
Provider Appeals and Billing Disputes
 Provider Appeals and Billing Disputes UniCare Billing Dispute Internal Review Process A claim appeal is a formal written request from a physician or provider for reconsideration of a claim already processed
Provider Appeals and Billing Disputes UniCare Billing Dispute Internal Review Process A claim appeal is a formal written request from a physician or provider for reconsideration of a claim already processed
Providers must attach a copy of the payer s EOB with the UnitedHealthcare Community Plan dental claim (2012 ADA form).
 UnitedHealthcare Community Plan (formerly APIPA) Medicaid Dental Claims and Billing Process Effective Dates of Service October 01, 2015 or after AHCCCS Provider Identification Number and NPI Number All
UnitedHealthcare Community Plan (formerly APIPA) Medicaid Dental Claims and Billing Process Effective Dates of Service October 01, 2015 or after AHCCCS Provider Identification Number and NPI Number All
MEDICAID BASICS BOOK Third Party Liability
 Healthy Connections Visual MEDICAID BASICS BOOK Third Party Liability An illustrated companion to the interactive courses at: MedicaideLearning.com. This topic includes content from the exclusive Third
Healthy Connections Visual MEDICAID BASICS BOOK Third Party Liability An illustrated companion to the interactive courses at: MedicaideLearning.com. This topic includes content from the exclusive Third
Medicaid Registration/Payment Process
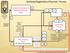 Medicaid Registration/Payment Process Copyright 2011. All Rights Reserved. Pristine Technology Solutions, Inc Pristine Technology Solutions Inc. Register w/cms 1 1 Centers for Medicare & Medicaid Services
Medicaid Registration/Payment Process Copyright 2011. All Rights Reserved. Pristine Technology Solutions, Inc Pristine Technology Solutions Inc. Register w/cms 1 1 Centers for Medicare & Medicaid Services
Ambulatory Surgery Centers Billing Instructions
 Health and Recovery Services Administration (HRSA) Ambulatory Surgery Centers Billing Instructions About this publication This publication supersedes all previous billing instructions for Ambulatory Surgery
Health and Recovery Services Administration (HRSA) Ambulatory Surgery Centers Billing Instructions About this publication This publication supersedes all previous billing instructions for Ambulatory Surgery
An initial course of ABA therapy is subject to PA and is covered when all the following criteria are met:
 IHCP bulletin Note: This bulletin is obsolete. Please see BT201606 for the corrected version of this bulletin. INDIANA HEALTH COVERAGE PROGRAMS BT201605 JANUARY 15, 2016 IHCP adds coverage of applied behavioral
IHCP bulletin Note: This bulletin is obsolete. Please see BT201606 for the corrected version of this bulletin. INDIANA HEALTH COVERAGE PROGRAMS BT201605 JANUARY 15, 2016 IHCP adds coverage of applied behavioral
SECTION 6: CLAIMS FILING TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1
 SECTION 6: CLAIMS FILING TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 OCTOBER 2015 TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 OCTOBER 2015 SECTION 6: CLAIMS FILING Table of Contents 6.1 Claims
SECTION 6: CLAIMS FILING TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 OCTOBER 2015 TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 OCTOBER 2015 SECTION 6: CLAIMS FILING Table of Contents 6.1 Claims
DCS Medicaid Training
 DCS Medicaid Training HP Provider Relations March 2012 1 2010 Hewlett-Packard Development Company, L.P. The information contained herein is subject to change without notice Agenda What is Medicaid Outpatient
DCS Medicaid Training HP Provider Relations March 2012 1 2010 Hewlett-Packard Development Company, L.P. The information contained herein is subject to change without notice Agenda What is Medicaid Outpatient
The benefits of electronic claims submission improve practice efficiencies
 The benefits of electronic claims submission improve practice efficiencies Electronic claims submission vs. manual claims submission An electronic claim is a paperless patient claim form generated by computer
The benefits of electronic claims submission improve practice efficiencies Electronic claims submission vs. manual claims submission An electronic claim is a paperless patient claim form generated by computer
Section 9. Claims Claim Submission Molina Healthcare PO Box 22815 Long Beach, CA 90801
 Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
Section 9. Claims As a contracted provider, it is important to understand how the claims process works to avoid delays in processing your claims. The following items are covered in this section for your
CMS 1500 Training 101
 CMS 1500 Training 101 HP Enterprise Services Learning Objective Welcome, this training presentation will educate you on how to complete a CMS 1500 claim form; this includes a detailed explanation of all
CMS 1500 Training 101 HP Enterprise Services Learning Objective Welcome, this training presentation will educate you on how to complete a CMS 1500 claim form; this includes a detailed explanation of all
Targeted Case Management. March 2016
 Targeted Case Management March 2016 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and Voids Current CPT Codes and Place of Service Codes Timely Filing WebRA ICD-10
Targeted Case Management March 2016 Topics for Today Provider Training Provider Manuals Submitting Claims Claim Adjustments and Voids Current CPT Codes and Place of Service Codes Timely Filing WebRA ICD-10
SECTION 6: CLAIMS FILING
 TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 SECTION 6: CLAIMS FILING 6.1 Claims Information............................................................... 6-5 6.1.1 TMHP Processing Procedures.......................................................
TEXAS MEDICAID PROVIDER PROCEDURES MANUAL: VOL. 1 SECTION 6: CLAIMS FILING 6.1 Claims Information............................................................... 6-5 6.1.1 TMHP Processing Procedures.......................................................
Appendix A Denial Management and Negotiation Hearing Screening
 Appendix A Denial Management and Negotiation Hearing Screening Ideally, hearing screenings should be covered benefits that are separately payable by the health plan. While health plan benefits may include
Appendix A Denial Management and Negotiation Hearing Screening Ideally, hearing screenings should be covered benefits that are separately payable by the health plan. While health plan benefits may include
Welcome to your Premera HSA plan!
 Welcome to your Premera HSA plan! You re enrolled in the HSA plan from Premera Blue Cross. It comes fully assembled and integrated, so you can immediately enjoy the financial advantages of its health savings
Welcome to your Premera HSA plan! You re enrolled in the HSA plan from Premera Blue Cross. It comes fully assembled and integrated, so you can immediately enjoy the financial advantages of its health savings
ARKANSAS MEDICAID PROGRAM
 ARKANSAS MEDICAID PROGRAM CHILDREN S MEDICAL SERVICES (CMS) TARGETED CASE PROVIDER MANUAL DEPARTMENT OF HUMAN SERVICES DIVISION OF MEDICAL SERVICES EDS Arkansas Medicaid Manual: CMS TARGETED CASE Page:
ARKANSAS MEDICAID PROGRAM CHILDREN S MEDICAL SERVICES (CMS) TARGETED CASE PROVIDER MANUAL DEPARTMENT OF HUMAN SERVICES DIVISION OF MEDICAL SERVICES EDS Arkansas Medicaid Manual: CMS TARGETED CASE Page:
Reimbursement for Physician- Administered Drugs:
 Reimbursement for Physician- Purchased and Physician- Administered Drugs: Understanding the Buy and Bill Process 60889-R5-V1 This information is provided d for your background education and is not intended
Reimbursement for Physician- Purchased and Physician- Administered Drugs: Understanding the Buy and Bill Process 60889-R5-V1 This information is provided d for your background education and is not intended
Part B Education Exclusive: Modifier 59 Edit Update Questions
 Cahaba GBA would like to provide some clarification of the use of Modifier 59. The modifier is not limited to National Correct Coding Initiative (NCCI) pairs. We apologize for any confusion our July article
Cahaba GBA would like to provide some clarification of the use of Modifier 59. The modifier is not limited to National Correct Coding Initiative (NCCI) pairs. We apologize for any confusion our July article
CLAIM FORM REQUIREMENTS
 CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
CLAIM FORM REQUIREMENTS When billing for services, please pay attention to the following points: Submit claims on a current CMS 1500 or UB04 form. Please include the following information: 1. Patient s
