Comparison of spinal anesthesia with combined sciatic-femoral nerve block for outpatient knee arthroscopy
|
|
|
- Ilene Sullivan
- 8 years ago
- Views:
Transcription
1 Journal of Clinical Anesthesia (2008) 20, Original contribution Comparison of spinal anesthesia with combined sciatic-femoral nerve block for outpatient knee arthroscopy Felix R. Montes MD (Associate Professor) a,, Eduardo Zarate MD (Assistant Professor) b, Reinaldo Grueso MD (Assistant Instructor) b, Juan C. Giraldo MD (Staff Anesthesiologist) a, Maria P. Venegas MD (Resident) b, Andrea Gomez MD (Resident) b, Jose D. Rincón MD (Assistant Professor) a, Marcela Hernadez MD (Resident) a, Mariana Cabrera MD (Research Assistant) a a Department of Anesthesiology, Fundación Cardio Infantil-Instituto de Cardiología, Universidad del Rosario, Bogotá, Colombia b Department of Anesthesia, Hospital de San Ignacio, Universidad Javeriana, Bogotá, Colombia Received 5 March 2007; revised 13 February 2008; accepted 2 April 2008 Keywords: Ambulatory anesthesia; Knee arthroscopy, outpatient; Spinal anesthesia; Peripheral nerve blocks Abstract Study Objective: To compare spinal anesthesia and combined sciatic-femoral nerve block for outpatient knee arthroscopy. Design: Prospective, randomized, controlled study. Setting: Postoperative recovery area at a university-affiliated medical center. Patients: 50 ASA physical status I and II adult outpatients undergoing arthroscopic knee surgery. Interventions: Study subjects were equally divided (n = 25 each) into spinal and sciatic-femoral groups. Spinal group patients received spinal anesthesia with 7.5 mg of 0.5% hyperbaric bupivacaine. Sciaticfemoral group patients received combined sciatic-femoral nerve blocks using a mixture of 20 ml of lidocaine 2% plus 20 ml of bupivacaine 0.5%. Measurements: Times including that from arrival in the operating room to readiness for surgery, duration of surgery, recovery time, and patient satisfaction were recorded. Analgesia and occurrence of adverse events also were recorded. Main Results: No significant differences between the two groups were found for any of the study measurements of recovery. After discharge, postoperative pain differed significantly between groups only at 6 hours (P b 0.002). Patient satisfaction was high with both techniques. Conclusions: Combined sciatic-femoral nerve block for outpatient arthroscopic knee surgery offers satisfactory anesthesia, with a clinical profile similar to that of low-dose spinal anesthesia. Sciatic-femoral nerve blocks are associated with significantly lower pain scores during the first 6 postoperative hours Elsevier Inc. All rights reserved. This study was supported by departmental funding. Corresponding author. Tranexco 1194tp6co, PO Box , Miami, FL 33102, USA. Tel.: ; fax: address: felix.ramon.montes@gmail.com (F.R. Montes) /$ see front matter 2008 Elsevier Inc. All rights reserved. doi: /j.jclinane
2 416 F.R. Montes et al. 1. Introduction Knee arthroscopy is a commonly performed ambulatory surgical procedure. Both general and diverse types of regional anesthesia have been used successfully for this surgery. Peripheral nerve blocks or spinal anesthesia may have some benefits in the outpatient setting and result in less postoperative resource use, better immediate postoperative analgesia, and better patient satisfaction [1-4]. In recent years, peripheral nerve blocks have become increasingly popular [5], but they are still less common than spinal anesthesia, mainly because of the increased time and expertise required as well as the delayed recovery associated with their use [6]. Few data are currently available in the literature comparing peripheral blocks with small-dose spinal anesthetic techniques [7]. To obtain more information on this topic, we conducted this prospective randomized study to test the hypothesis that using a combined sciatic-femoral nerve block results in shorter time to discharge as compared with spinal anesthesia in patients undergoing a less invasive category of outpatient knee surgery [3]. 2. Materials and methods After approval by the Fundación Cardio Infantil- Instituto de Cardiología, Bogotá, Colombia, institutional ethics committee and obtaining written informed consent from each individual, we enrolled into the study 50 patients undergoing elective outpatient knee arthroscopy. All patients were ASA physical status I or II and aged between 18 and 65 years. Exclusion criteria included anterior cruciate ligament repair, morbid obesity (body mass index N35 kg/m 2 ), medical contraindication to regional anesthesia (eg, allergy, bleeding disorders, localized infection, and neurologic disease), and respiratory or cardiac disease. All patients received intravenous (IV) premedication with 0.03 mg/kg of midazolam and one μg per kg of fentanyl, followed by a 7-mL/kg infusion of lactated Ringer's solution. Using a computer-generated randomization table, we allocated patients to two groups to receive either spinal anesthesia (spinal group, n = 25) or a combined sciaticfemoral nerve block (sciatic-femoral group, n = 25). Spinal anesthesia was performed at the L2-3 or L3-4 interspace with a 25-gauge Whitacre needle (Becton Dickinson Co, Flanklin Lakes, NJ) using the midline approach, with the patient placed in the lateral position with the operative side dependent. After free flow of cerebrospinal fluid, 7.5 mg of hyperbaric 0.5% bupivacaine was injected with the needle aperture directed laterally, toward the dependent side, with the patient turned supine. Combined sciatic-femoral nerve blocks were performed using a mixture of 20 ml of lidocaine 2% plus 20 ml of bupivacaine 0.5%. Nerve blocks were placed with the aid of a nerve stimulator connected to a 21-gauge 100-mm Stimuplex block needle (B. Braun Medical Inc, Melsungen, Germany). Stimulation frequency was set at two Hz, whereas the intensity of the stimulating current was 0.3 to 0.5 ma. With the patient in the lateral decubitus position, we performed the sciatic nerve block according to the Labat approach [8]. After we noted a twitch of either the hamstring or soleus muscles, or the foot or toes, 20 ml of local anesthetic mixture was injected. The patient was immediately turned supine, and the femoral nerve block was performed. The stimulating needle was inserted lateral to the femoral artery at the intersection of the femoral artery and a line connecting the anterior superior iliac spine to the pubic tubercle. On elicitation of a quadriceps (patella twitch) response with a current of 0.3 to 0.5 ma, 20 ml of the anesthetic solution was injected. Standard monitoring was used throughout the study, including continuous electrocardiography (lead II), heart rate, noninvasive arterial blood pressure measured every 5 minutes, and oxygen saturation via continuous pulse oximetry (SpO 2 ). Sensory block was evaluated using the pinprick test (22-gauge hypodermic needle), and it was judged adequate if there was a complete loss of pinprick sensation at T12 in the spinal group, or in the femoral and sciatic nerve distribution in the sciatic-femoral group. Motor block was evaluated using a modified Bromage scale (0 = no motor block; 1 = hip blocked; 2 = hip and knee blocked; and 3 = hip, knee, and ankle blocked). For the purpose of the study, hypotension was defined as systolic blood pressure less than 90 mmhg or a decrease of more than 25% from baseline mean arterial pressure, and it was treated with a bolus of ephedrine 5 to 10 mg IV. In addition to the loading dose of IV fluids, patients received lactated Ringer's solution as deemed necessary by the anesthesiologist. Inadequate anesthesia (patient complaint of pain) was treated with a bolus of fentanyl one μg per kg IV, with a second bolus allowed. If more than two μg/kg of fentanyl was required to maintain patient comfort, the regional anesthesia technique was considered a failure, and general anesthesia was induced. The primary outcome measure was time to home discharge, which was defined as the interval from end of surgery until a patient was discharged home. In addition, anesthesia-controlled time and surgeon-controlled time were recorded [9,10]. Anesthesia-controlled time was defined as the sum of (1) the time from operating room (OR) entry until surgical preparation began (anesthesia preparation time), plus (2) time from the end of the surgical procedure until OR exit (OR emergence time). Surgeon-controlled time was defined as the time from the beginning of skin preparation to the start of surgery (surgical preparation time), plus the time from surgery start to surgery finish (duration of surgery). Because it is of particular importance to our practice, we calculated the total time elapsed between the moment the patient entered the OR until the patients left the OR (ie, total OR time).
3 Spinal vs. nerve blocks for knee arthroscopy Table 1 Demographic characteristics Sciatic-femoral nerve block (n = 24) Spinal anesthesia (n = 25) Age (yrs) 46 ± ± 14 Weight (kg) 67 ± ± 13 Height (cm) 166 ± ± 8 ASA physical status I II 6 9 Women, n (%) 14 (58) 15 (60) Men, n (%) 10 (42) 10 (40) Operating procedure Meniscectomy Synovectomy 8 7 Chondroplasty 5 7 Lateral release 4 4 Plica removal 2 3 Loose body removal 1 2 Data are presented as means ± SD, percentage, or n as indicated. All patients were assessed in the recovery area at 15-minute intervals with the Mayo Modified Discharge Scoring System (Appendix A), an accepted modification of the Aldrete postoperative discharge criteria [11] to asses readiness for primary recovery area discharge. A Mayo Modified Discharge Scoring System of 8 or higher was noted and was taken as a time that could be used as an index of fitness to move from a primary recovery area to a secondary area [2]. In the phase 2 recovery area, patients were assessed every 15 minutes. Once they had achieved a score of 9 points on the postanesthetic discharge scoring system (PADSS), they were deemed fit for discharge [12] (Appendix B). The time taken to obtain a PADSS score of 9 or higher and the time patients were actually discharged were both recorded. Voiding was not required before home readiness, but the time to void was recorded if the patient had not yet left the hospital. There was no minimum length of stay in either the primary or secondary recovery areas. Pain was assessed at rest with a 100-mm visual analog scale (VAS) every 15 minutes until hospital discharge. In the phase 1 recovery area, morphine sulfate 2.5 mg was administered by IV injection every 5 to 10 minutes until the patient was comfortable (VAS score 40 mm). The pain management protocol in phase 2 and at home consisted of 400 mg of oral ibuprofen every 8 hours and rescue analgesia with oral acetaminophen (one g) if the patient asked for more analgesic. When patients were discharged from the hospital, they were asked to rate their pain intensity at rest on the VAS at 6, 12, 18, and 24 hours after surgery and record their analgesic consumption. A standardized telephone questionnaire was conducted by a research assistant 24 hours after surgery. Patients were questioned about postoperative pain, nausea, backache, postdural puncture headache, and transient neurologic symptoms (TNS). Transient neurologic symptoms were defined as pain or dysesthesia in the buttocks, thighs, or calves occurring within 24 hours. Patient satisfaction was assessed by asking patients whether they would receive the same anesthesia in the future. Sample size estimates were based on time to home discharge (in min). It was estimated that a sample size of 23 per group would provide 80% power to detect a clinically meaningful difference of 40 minutes (within-group SD, 49 mins) at α = Student's t test was used to determine the significance of normally distributed parametric values and Wilcoxon rank sum test for nonnormally distributed data. Categorical variables were tested using χ 2 test or, when appropriate, Fisher's exact test. Statistical significance was accepted at P b Results Fifty patients were enrolled in the study, with 25 patients in each group. One patient in the sciaticfemoral group required general anesthesia because of failure of the regional technique; hence, this patient was excluded from the analysis. There were no significant differences between the two groups in demographic characteristics, ASA physical status, or type of surgical procedures performed (Table 1). Total OR time, duration of surgery, and surgical preparation time did not differ significantly between the two groups, although mean anesthesia preparation time was longer (6 min) in patients given combined sciatic-femoral Table 2 Postoperative outcomes Sciatic-femoral nerve block (n = 24) Spinal anesthesia (n = 25) Anesthesia-controlled time Anesthesia preparation 23 ± ± time (min) OR emergence time (min) 6 ± 3 7 ± Surgeon-controlled time Surgical preparation time 24 ± 9 24 ± (min) Duration of surgery (min) 38 ± ± Total OR time (min) 97 ± ± Mayo Modified Discharge 27 ± ± score 8 (min) PADSS ± ± Actual home discharge (min) 219 ± ± Data are presented as means ± SD. Anesthesia preparation time = patient enters operating room (OR) until surgical preparation begins OR; emergence time = from the end of surgery until OR exit; surgical preparation time = from when the skin preparation begins to when surgery starts; PADSS = postanesthetic discharge scoring system. P 417
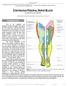
4 418 F.R. Montes et al. Fig. 1 Postoperative visual analog scores for pain. Data are shown as means ± SD. RA = recovery area. *P b 0.05 vs sciaticfemoral group. nerve blocks (Table 2). Patients in both groups achieved in a similar period a Mayo Modified Discharge score of 8, which was the criterion for eligibility for discharge from the primary recovery area. No statistical differences were found between the two groups in the time to achieve a PADSS score of 9 or higher or in the time taken to leave the hospital (Table 2). In the recovery area, no differences were found between the groups in VAS scores. After discharge, pain scores were significantly lower in the sciatic-femoral group (10 ± 24 mm) than in the Spinal group (50 ± 35 mm, P = 0.002). There were no differences in the postoperative VAS pain scores between the groups at 12, 18, or 24 hours (Fig. 1). In the hospital, three patients (12%) of the spinal anesthesia group received analgesics compared with two patients (8.3%) of the sciatic-femoral nerve block group (P = 0.095). After discharge, there was no significant difference between the groups in consumption of oral analgesics. No patient required antiemetic therapy. No cases of postdural puncture headache or other complications were reported at postoperative follow-up. Patient satisfaction was high in both groups, and all patients reported that they would accept the same anesthesia technique again if required for future operations. 4. Discussion The results of this study show that patients undergoing knee arthroscopy achieved home-readiness criteria and time to discharge home equally after both spinal anesthesia with small doses of bupivacaine and combined sciatic-femoral nerve blocks using a multiple-injection technique. Even though performing a sciatic-femoral nerve block took slightly longer than administering the spinal anesthesia, total OR time was similar with both techniques. The increased time required to perform the anesthetic procedure in the sciatic-femoral group is explained by the need for more than one block to successfully accomplish this technique. Even though there was a statistically significant difference in anesthesia preparation time in favor of spinal anesthesia, the clinical relevance of this finding may be limited. Similar findings have been reported in other investigations comparing peripheral nerve blocks with general anesthesia [1,13] or spinal anesthesia [7]. As has been suggested, placing peripheral nerve blocks preoperatively in the holding area rather than in the OR would decrease OR time in this group of patients [10]. However, use of a separate block room has cost implications in itself that may outweigh any benefit from the reduced OR time [14]. Adequate pain management is essential to facilitate rehabilitation after knee arthroscopy. Regional techniques consistently provide superior postoperative analgesia when compared with general anesthesia [1,2,15,16]. The possible difference in postoperative analgesia between diverse regional anesthesia techniques has been investigated only minimally. In the present study, a sciatic-femoral nerve block provided better analgesia than spinal anesthesia only at 6 hours after surgery. Some investigators have postulated that in low invasive knee surgery, such as the type performed during this investigation, a multimodal analgesic approach maintains VAS pain scores less than 30 (100 mm scale) regardless of intraoperative anesthetic technique [15,17]. In our study, this approach to postoperative pain management was not used; however, postoperative analgesia was effectively provided with nonsteroidal anti-inflammatory drugs. Comparable results have already been reported in a similar clinical setting [4,13,18] and suggest that there may be minimal discomfort associated with standard outpatient knee arthroscopy. However, it is important to remember that our study was powered to detect differences for time to home discharge. Although the difference in other outcomes (ie, pain, postoperative nausea and vomiting, and TNS) between the groups was not statistically significant, it should be considered that a type 2 error cannot be excluded, and further sufficiently powered studies are advocated to evaluate these points. In clinical studies such as ours, the choice of a control group becomes difficult. Admittedly, there are numerous alternative anesthetic techniques to use for outpatient knee arthroscopy. We chose the low-dose hyperbaric bupivacaine spinal anesthesia group as our control because this technique is the one that we use routinely when not using peripheral nerve blocks. Low-dose bupivacaine has been used for spinal anesthesia for procedures of short duration in an attempt to avoid the use of local anesthetics such as lidocaine, which is known to cause adverse effects such as TNS. In this study, sciatic-femoral nerve block failed to provide acceptable surgical anesthesia in one patient. This 4% failure rate is comparable with the failure rate found in previous work [19] that used a similar technique (ie, multiple-injection technique) to accomplish this block.
5 Spinal vs. nerve blocks for knee arthroscopy The failure rate after small-dose bupivacaine anesthesia is between 3% and 6% [2,4,20,21]. This finding shows that both techniques provide similar effective anesthesia, rendering them viable options for outpatient knee surgery, with no practical advantage of one over the other in success rate. In the present study, recovery times after 7.5 mg of intrathecal bupivacaine were significantly lower than those recovery times reported in previous investigations with similar doses of bupivacaine [2,7,20,21]. In those studies, achievement of home-readiness criteria ranged from 129 to 241 minutes, with recovery of spontaneous voiding being the most common limiting factor to fulfill home discharge criteria. Mulroy et al [22] supported a relaxation of the requirements for voiding after outpatient spinal anesthesia with short-duration drugs (or small doses of hyperbaric bupivacaine) and in patients undergoing surgical procedures of low risk for urinary retention. This new approach to home discharge after outpatient procedures reduces the time required before the patient is ready to go home, and it is now part of our routine practice. In spite of changing the criteria for home readiness in patients undergoing spinal anesthesia, this approach did not result in a shorter time to hospital discharge when compared with combined sciaticfemoral nerve blocks. In our experience as well as that of other researchers, the overall length of stay in the postanesthesia care unit is often related to multiple administrative or nonmedical issues [23-25]. The most common cause of discharge delays in our unit was attributed to system factors such as paperwork processing handled by administrative personnel (filling out forms, invoicing, and billing clearance). In spite of these nonanesthesia-related factors, discharge time is relevant in an absolute way to patients when planning for assistance on the day of surgery [26]. Physicians are often concerned about discharging patients who were given a long-acting peripheral nerve block of the lower extremity, because of a loss of proprioception and the protective reflex of pain [6]. A large study showed that this practice may be done safely and is associated with a high degree of efficacy and satisfaction [27]. Based on this study, the presence of an insensate lower extremity was not considered a contraindication to home discharge. In addition, peripheral nerve blocks are frequently prolonged into the postoperative period at home so as to optimize pain relief [28]. However, a recent publication reported 4 falls among 233 patients (1.7%) who received a femoral perineural catheter for pain management at home [29]. This finding suggests that this practice may not be free of complications and, in some cases, may create unnecessary risk without apparent benefit. In conclusion, our results show that in patients undergoing outpatient arthroscopy, there are no significant differences in recovery or discharge times after a combined sciatic-femoral nerve block compared with spinal anesthesia (using low-dose bupivacaine). Appendix A. Mayo modified discharge scoring system [2] Variable Score Motor activity Active motion, voluntary or on command 2 Weak motion, voluntary or on command 1 No motion 0 Respiration Coughs on command or cries 2 Maintains airway without support 1 Requires airway maintenance 0 Systolic blood pressure ±20% of preanesthetic level 2 ±20%-50% of preanesthetic level 1 ±50% of preanesthetic level 0 Consciousness Fully awake or easily aroused when called 2 Responds to stimuli and exhibits protective reflexes 1 No response or absence of protective reflexes 0 Oxygen saturation Preoperative reading without 2 supplemental oxygen Preoperative reading with 1 supplemental oxygen bpreoperative reading with or without 0 supplemental oxygen Points are assigned from each variable and added. Appendix B. Postanesthesia discharge scoring system [12] Variable Score Vital signs ±20% of preoperative values 2 ±20%-40% of preoperative values 1 ±40% of preoperative values 0 Ambulation and mental status Oriented 3 and has ability to ambulate (with 2 crutches) Oriented 3 or has ability to ambulate (with 1 crutches) Neither 0 Pain or nausea and vomiting Minimal 2 Moderate 1 Severe 0 Surgical bleeding Minimal 2 Moderate 1 Severe 0 Intake and output Has had oral fluid and has voided 2 Has had oral fluid or has voided 1 Neither 0 Points are assigned from each variable and added. 419
6 420 F.R. Montes et al. References [1] Hadzic A, Karaca PE, Hobeika P, et al. Peripheral nerve blocks result in superior recovery profile compared with general anesthesia in outpatient knee arthroscopy. Anesth Analg 2005;100: [2] Jankowski CJ, Hebl JR, Stuart MJ, et al. A comparison of psoas compartment block and spinal and general anesthesia for outpatient knee arthroscopy. Anesth Analg 2003;97: [3] Williams B, Kentor ML, Vogt MT, et al. Femoral-sciatic nerve blocks for complex outpatient knee surgery are associated with less postoperative pain before same-day discharge: a review of 1,200 consecutive cases from the period Anesthesiology 2003; 98: [4] Korhonen AM, Valanne JV, Jokela RM, Ravaska P, Korttila KT. A comparison of selective spinal anesthesia with hyperbaric bupivacaine and general anesthesia with desflurane for outpatient knee arthroscopy. Anesth Analg 2004;99: [5] Auroy Y, Benhamou D, Bargues L, et al. Major complications of regional anesthesia in France: the SOS Regional Anesthesia Hotline Service. Anesthesiology 2002;97: [6] Klein SM, Pietrobon R, Nielsen KC, Warner DS, Greengrass RA, Steele SM. Peripheral nerve blockade with long-acting local anesthetics: a survey of the Society for Ambulatory Anesthesia. Anesth Analg 2002;94:71-6. [7] Casati A, Cappelleri G, Fanelli G, et al. Regional anaesthesia for outpatient knee arthroscopy: a randomized clinical comparison of two different anaesthetic techniques. Acta Anaesthesiol Scand 2000;44: [8] Enneking FK, Chan V, Greger J, Hadzić A, Lang SA, Horlocker TT. Lower-extremity peripheral nerve blockade: essentials of our current understanding. Reg Anesth Pain Med 2005;30:4-35. [9] Donham RT, Mazzei WJ, Jones RL. Association of anesthesia clinical directors' procedural times glossary: glossary of times used for scheduling and monitoring of diagnostic and therapeutic procedures. Am J Anesthesiol 1996;23(5S):3-12. [10] Williams BA, Kentor ML, Williams JP, et al. Process analysis in outpatient knee surgery: effects of regional and general anesthesia on anesthesia-controlled time. Anesthesiology 2000;93: [11] Aldrete JA. The post-anesthesia recovery score revisited. J Clin Anesth 1995;7: [12] Chung F. Are discharge criteria changing? J Clin Anesth 1993; 5(6 Suppl 1):64S-8S. [13] Casati A, Cappelleri G, Berti M, Fanelli G, Di Benedetto P, Torri G. Randomized comparison of remifentanil-propofol with a sciaticfemoral nerve block for out-patient knee arthroscopy. Eur J Anaesthesiol 2002;19: [14] Armstrong KP, Cherry RA. Brachial plexus anesthesia compared to general anesthesia when a block room is available. Can J Anaesth 2004;51:41-4. [15] Wong J, Marshall S, Chung F, Sinclair D, Song D, Tong D. Spinal anesthesia improves the early recovery profile of patients undergoing ambulatory knee arthroscopy. Can J Anaesth 2001;48: [16] Patel NJ, Flashburg MH, Paskin S, Grossman R. A regional anesthetic technique compared to general anesthesia for outpatient knee arthroscopy. Anesth Analg 1986;65: [17] Jacobson E, Forssblad M, Rosenberg J, Westman L, Weidenhielm L. Can local anesthesia be recommended for routine use in elective knee arthroscopy? A comparison between local, spinal, and general anesthesia. Arthroscopy 2000;16: [18] Marsan A, Kirdemir P, Mamo D, Casati A. Prilocaine or mepivacaine for combined sciatic-femoral nerve block in patients receiving elective knee arthroscopy. Minerva Anestesiol 2004;70: [19] Fanelli G, Casati A, Garancini P, Torri G. Nerve stimulator and multiple injection technique for upper and lower limb blockade: failure rate, patient acceptance, and neurologic complications. Study Group on Regional Anesthesia. Anesth Analg 1999;88: [20] Cappelleri G, Aldegheri G, Danelli G, et al. Spinal anesthesia with hyperbaric levobupivacaine and ropivacaine for outpatient knee arthroscopy: a prospective, randomized, double-blind study. Anesth Analg 2005;101: [21] Valanne JV, Korhonen AM, Jokela RM, Ravaska P, Korttila KK. Selective spinal anesthesia: a comparison of hyperbaric bupivacaine 4 mg versus 6 mg for outpatient knee arthroscopy. Anesth Analg 2001; 93: [22] Mulroy MF, Salinas FV, Larkin KL, Polissar NL. Ambulatory surgery patients may be discharged before voiding after short-acting spinal and epidural anesthesia. Anesthesiology 2000;97: [23] Montes FR, Trillos JE, Rincón IE, et al. Comparison of total intravenous anesthesia and sevoflurane-fentanyl anesthesia for outpatient otorhinolaryngeal surgery. J Clin Anesth 2002;14: [24] Waddle JP, Evers AS, Piccirillo JF. Postanesthesia care unit length of stay: quantifying and assessing dependent factors. Anesth Analg 1998; 87: [25] Bekker AY, Berklayd P, Osborn I, Bloom M, Yarmush J, Turndorf H. The recovery of cognitive function after remifentanil-nitrous oxide anesthesia is faster than after an isoflurane-nitrous oxide-fentanyl combination in elderly patients. Anesth Analg 2000;91: [26] Pavlin DJ, Rapp SE, Polissar NL, Malmgren JA, Koerschgen M, Keyes H. Factors affecting discharge time in adult outpatients. Anesth Analg 1998;87: [27] Klein SM, Nielsen KC, Greengrass RA, Warner DS, Martin A, Steele SM. Ambulatory discharge after long-acting peripheral nerve blockade: 2382 blocks with ropivacaine. Anesth Analg 2002;94: [28] Ilfeld BM, Enneking FK. Continuous peripheral nerve blocks at home: a review. Anesth Analg 2005;100: [29] Williams BA, Kentor ML, Bottegal MT. The incidence of falls at home in patients with perineural femoral catheters: a retrospective summary of a randomized clinical trial. Anesth Analg 2007;104:1002.
DISCHARGE CRITERIA FOR PHASE I & II- POST ANESTHESIA CARE
 REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
Femoral Nerve Block/3-in-1 Nerve Block
 Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
INTERSCALENE BLOCK AND OTHER ARTICLES ON ANESTHESIA FOR ARTHROSCOPIC SURGERY NOT QUALIFYING AS EVIDENCE
 INTERSCALENE BLOCK AND OTHER ARTICLES ON ANESTHESIA FOR ARTHROSCOPIC SURGERY NOT QUALIFYING AS EVIDENCE Hughes MS, Matava MJ, et al. Interscalene Brachial Plexus Block for Arthroscopic Shoulder Surgery.
INTERSCALENE BLOCK AND OTHER ARTICLES ON ANESTHESIA FOR ARTHROSCOPIC SURGERY NOT QUALIFYING AS EVIDENCE Hughes MS, Matava MJ, et al. Interscalene Brachial Plexus Block for Arthroscopic Shoulder Surgery.
The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson
 The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson As a private practice anesthesiologist, I am often asked: What are the potential benefits of regional anesthesia (RA)? My
The Impact of Regional Anesthesia on Perioperative Outcomes By Dr. David Nelson As a private practice anesthesiologist, I am often asked: What are the potential benefits of regional anesthesia (RA)? My
The Efficacy of Continuous Bupivacaine Infiltration Following Anterior Cruciate Ligament Reconstruction
 The Efficacy of Continuous Bupivacaine Infiltration Following Anterior Cruciate Ligament Reconstruction Heinz R. Hoenecke, Jr., M.D., Pamela A. Pulido, R.N., B.S.N., Beverly A. Morris, R.N., C.N.P., and
The Efficacy of Continuous Bupivacaine Infiltration Following Anterior Cruciate Ligament Reconstruction Heinz R. Hoenecke, Jr., M.D., Pamela A. Pulido, R.N., B.S.N., Beverly A. Morris, R.N., C.N.P., and
Bier Block (Intravenous Regional Anesthesia)
 Bier Block (Intravenous Regional Anesthesia) History August Bier introduced this block in 1908. Early methods included the use of two separate tourniquets and procaine was the local anesthetic of choice.
Bier Block (Intravenous Regional Anesthesia) History August Bier introduced this block in 1908. Early methods included the use of two separate tourniquets and procaine was the local anesthetic of choice.
The ASA defines anesthesiology as the practice of medicine dealing with but not limited to:
 1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
1570 Midway Pl. Menasha, WI 54952 920-720-1300 Procedure 1205- Anesthesia Lines of Business: All Purpose: This guideline describes Network Health s reimbursement of anesthesia services. Procedure: Anesthesia
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011
 Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Common Regional Nerve Blocks Quick Guide developed by UWHC Acute Pain Service Jan 2011 A single shot nerve block is the injection of local anesthetic to block a specific nerve distribution. It can be placed
Local Anesthetics Used for Spinal Anesthesia
 Local Anesthetics Used for Spinal Anesthesia Several local anesthetics are used for spinal anesthesia. These include procaine, lidocaine, tetracaine, levobupivacaine, and bupivacaine. Local anesthetics
Local Anesthetics Used for Spinal Anesthesia Several local anesthetics are used for spinal anesthesia. These include procaine, lidocaine, tetracaine, levobupivacaine, and bupivacaine. Local anesthetics
ANESTHESIA. Anesthesia for Ambulatory Surgery
 ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
ANESTHESIA & YOU Anesthesia for Ambulatory Surgery T oday the majority of patients who undergo surgery or diagnostic tests do not need to stay overnight in the hospital. In most cases, you will be well
30. BASIC PEDIATRIC REGIONAL ANESTHESIA
 30. BASIC PEDIATRIC REGIONAL ANESTHESIA INTRODUCTION Military anesthesia providers often encounter pediatric patients while delivering medical care in the field. The application of regional anesthesia
30. BASIC PEDIATRIC REGIONAL ANESTHESIA INTRODUCTION Military anesthesia providers often encounter pediatric patients while delivering medical care in the field. The application of regional anesthesia
To outline nursing management of patients receiving epidural anesthesia during labor (Includes walking epidurals and combined spinal-epidurals).
 HOSPITAL NAME INSTITUTIONAL POLICY AND PROCEDURE (IPP) Department: Manual: Section: TITLE/DESCRIPTION POLICY NUMBER LABOR: EPIDURAL EFFECTIVE DATE REVIEW DUE REPLACES NUMBER NO. OF PAGES APPROVED BY APPLIES
HOSPITAL NAME INSTITUTIONAL POLICY AND PROCEDURE (IPP) Department: Manual: Section: TITLE/DESCRIPTION POLICY NUMBER LABOR: EPIDURAL EFFECTIVE DATE REVIEW DUE REPLACES NUMBER NO. OF PAGES APPROVED BY APPLIES
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Introduction. Alexandria Journal of Anaesthesia and Intensive Care
 44 Femoral Nerve Block versus Spinal Anesthesia for Lower Limb Peripheral Vascular Surgery By Ahmed Mansour, MD Assistant Professor of Anesthesia, Faculty of Medicine, Alexandria University. Abstract Perioperative
44 Femoral Nerve Block versus Spinal Anesthesia for Lower Limb Peripheral Vascular Surgery By Ahmed Mansour, MD Assistant Professor of Anesthesia, Faculty of Medicine, Alexandria University. Abstract Perioperative
2.0 Synopsis. Vicodin CR (ABT-712) M05-765 Clinical Study Report R&D/07/095. (For National Authority Use Only) to Part of Dossier: Volume:
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Vicodin CR Name of Active Ingredient: Hydrocodone/Acetaminophen Extended Release (ABT-712) Individual Study Table Referring to Part of Dossier: Volume:
2.0 Synopsis Abbott Laboratories Name of Study Drug: Vicodin CR Name of Active Ingredient: Hydrocodone/Acetaminophen Extended Release (ABT-712) Individual Study Table Referring to Part of Dossier: Volume:
NIH Public Access Author Manuscript Br J Anaesth. Author manuscript; available in PMC 2007 January 16.
 NIH Public Access Author Manuscript Published in final edited form as: Br J Anaesth. 2005 August ; 95(2): 250 254. The use of a stimulating catheter for total knee replacement surgery - preliminary results
NIH Public Access Author Manuscript Published in final edited form as: Br J Anaesth. 2005 August ; 95(2): 250 254. The use of a stimulating catheter for total knee replacement surgery - preliminary results
ANESTHESIA - Medicare
 ANESTHESIA - Medicare Policy Number: UM14P0008A2 Effective Date: August 19, 2014 Last Reviewed: January 1, 2016 PAYMENT POLICY HISTORY Version DATE ACTION / DESCRIPTION Version 2 January 1, 2016 Under
ANESTHESIA - Medicare Policy Number: UM14P0008A2 Effective Date: August 19, 2014 Last Reviewed: January 1, 2016 PAYMENT POLICY HISTORY Version DATE ACTION / DESCRIPTION Version 2 January 1, 2016 Under
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
With the shift away from costly preoperative
 BRIEF REPORTS Are Patients Comfortable Consenting to Clinical Anesthesia Research Trials on the Day of Surgery? Richard Brull, MD, Colin J. L. McCartney, MBChB, FRCA, FFARCSI, Vincent W. S. Chan, MD, FRCPC,
BRIEF REPORTS Are Patients Comfortable Consenting to Clinical Anesthesia Research Trials on the Day of Surgery? Richard Brull, MD, Colin J. L. McCartney, MBChB, FRCA, FFARCSI, Vincent W. S. Chan, MD, FRCPC,
Comparison of Procedural Times for Ultrasound-Guided Perineural Catheter Insertion in Obese and Nonobese Patients
 ORIGINAL RESEARCH Comparison of Procedural Times for Ultrasound-Guided Perineural Catheter Insertion in Obese and Nonobese Patients Edward R. Mariano, MD, MAS, Jay B. Brodsky, MD Article includes CME test
ORIGINAL RESEARCH Comparison of Procedural Times for Ultrasound-Guided Perineural Catheter Insertion in Obese and Nonobese Patients Edward R. Mariano, MD, MAS, Jay B. Brodsky, MD Article includes CME test
Corporate Medical Policy
 File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
The Outpatient Knee Replacement Program at Orlando Orthopaedic Center. Jeffrey P. Rosen, MD
 The Outpatient Knee Replacement Program at Orlando Orthopaedic Center Jeffrey P. Rosen, MD Anesthesia Pain Management Post-Op / Discharge Protocols The Orlando Orthopaedic Center Joint Replacement Team
The Outpatient Knee Replacement Program at Orlando Orthopaedic Center Jeffrey P. Rosen, MD Anesthesia Pain Management Post-Op / Discharge Protocols The Orlando Orthopaedic Center Joint Replacement Team
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Regional anesthesia for outpatient surgery
 Anesthesiology Clin N Am 21 (2003) 289 303 Regional anesthesia for outpatient surgery Michael F. Mulroy, MD*, Susan B. McDonald, MD Virginia Mason Medical Center, Department of Anesthesia B2-AN, 1100 Ninth
Anesthesiology Clin N Am 21 (2003) 289 303 Regional anesthesia for outpatient surgery Michael F. Mulroy, MD*, Susan B. McDonald, MD Virginia Mason Medical Center, Department of Anesthesia B2-AN, 1100 Ninth
Center for Medicaid and State Operations/Survey and Certification Group
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-12-25 Baltimore, Maryland 21244-1850 Center for Medicaid and State Operations/Survey
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services 7500 Security Boulevard, Mail Stop S2-12-25 Baltimore, Maryland 21244-1850 Center for Medicaid and State Operations/Survey
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Acute Pain Management in the Opioid Dependent Patient. Maripat Welz-Bosna MSN, CRNP-BC
 Acute Pain Management in the Opioid Dependent Patient Maripat Welz-Bosna MSN, CRNP-BC Relieving Pain in America (IOM) More then 116 Million Americans have pain the persists for weeks to years $560-635
Acute Pain Management in the Opioid Dependent Patient Maripat Welz-Bosna MSN, CRNP-BC Relieving Pain in America (IOM) More then 116 Million Americans have pain the persists for weeks to years $560-635
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice
 PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists
 Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Guidelines for Core Clinical Privileges Certified Registered Nurse Anesthetists Copyright 2005 222 South Prospect Park Ridge, IL 60068 www.aana.com Guidelines for Core Clinical Privileges Certified Registered
Updated Guide to Billing for Regional Anesthesia (United States)
 Updated Guide to Billing for Regional Anesthesia (United States) Tae-Wu Edward Kim, MD* w Stanford University School of Medicine, Palo Alto, California Veterans Affairs Palo Alto Health Care System, Palo
Updated Guide to Billing for Regional Anesthesia (United States) Tae-Wu Edward Kim, MD* w Stanford University School of Medicine, Palo Alto, California Veterans Affairs Palo Alto Health Care System, Palo
Comparison of the effects between clonidine and epinephrine added with bupivacine in brachial plexus block.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 11 Ver. I (Nov. 2014), PP 54-58 Comparison of the effects between clonidine and epinephrine
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 11 Ver. I (Nov. 2014), PP 54-58 Comparison of the effects between clonidine and epinephrine
Pain Relief during Labour and Delivery: What Are My Options?
 Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
Pain Relief during Labour and Delivery: What Are My Options? To help you prepare for the birth of your baby, this booklet answers some of the questions you may have about pain relief options. You should
A Patient s Guide to PAIN MANAGEMENT. After Surgery
 A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
A Patient s Guide to PAIN MANAGEMENT After Surgery C o m p a s s i o n a n d C o m m i t m e n t A Patient s Guide to Pain Management After Surgery If you re facing an upcoming surgery, it s natural to
r JOHNS HOPKINS HEALTHCARE Physician Guidelines Subject: Anesthesia Processing Guidelines Lines of Business: EHP, USFHP, Priority Partners
 Revision Date: 11/14/14 Last Reviewed Date: 11/14/14 Page 1 of 7 ACTION New Procedure Amending Procedure Number: Superseding Procedure Number: Repealing Procedure Number: REFERENCES: AMPT Committee ASA
Revision Date: 11/14/14 Last Reviewed Date: 11/14/14 Page 1 of 7 ACTION New Procedure Amending Procedure Number: Superseding Procedure Number: Repealing Procedure Number: REFERENCES: AMPT Committee ASA
MODERATE SEDATION RECORD (formerly termed Conscious Sedation)
 (POLICY #DOC-051) Page 1 of 6 WELLSPAN HEALTH - YORK HOSPITAL NURSING POLICY AND PROCEDURE Dates: Original Issue: September 1998 Annual Review: March 2012 Revised: March 2010 Submitted by: Brenda Artz
(POLICY #DOC-051) Page 1 of 6 WELLSPAN HEALTH - YORK HOSPITAL NURSING POLICY AND PROCEDURE Dates: Original Issue: September 1998 Annual Review: March 2012 Revised: March 2010 Submitted by: Brenda Artz
CODING AND COMPLIANCE NEW APPOINTMENT AND REAPPOINTMENT MODULE FOR ANESTHESIA FACULTY
 CODING AND COMPLIANCE NEW APPOINTMENT AND REAPPOINTMENT MODULE FOR ANESTHESIA FACULTY ANESTHESIA BILLING: MUST BE DOCUMENTED AS: Personally performed: you perform the case without a resident or a CRNA
CODING AND COMPLIANCE NEW APPOINTMENT AND REAPPOINTMENT MODULE FOR ANESTHESIA FACULTY ANESTHESIA BILLING: MUST BE DOCUMENTED AS: Personally performed: you perform the case without a resident or a CRNA
Patient Care Services Policy & Procedure Title: No. 8720-0059
 Page: 1 of 8 I. SCOPE: This policy applies to Saint Francis Hospital, its employees, medical staff, contractors, patients and visitors regardless of service location or category of patient. This policy
Page: 1 of 8 I. SCOPE: This policy applies to Saint Francis Hospital, its employees, medical staff, contractors, patients and visitors regardless of service location or category of patient. This policy
Post anesthesia recovery rate evaluated by using White fast tracking scoring system
 Munevera Hadžimešiæ et al. Journal of Health Sciences 2013;3(3):88-195 http://www.jhsci.ba Journal of Health Sciences RESEARCH ARTICLE Open Access Post anesthesia recovery rate evaluated by using White
Munevera Hadžimešiæ et al. Journal of Health Sciences 2013;3(3):88-195 http://www.jhsci.ba Journal of Health Sciences RESEARCH ARTICLE Open Access Post anesthesia recovery rate evaluated by using White
Medical Coverage Policy Monitored Anesthesia Care (MAC)
 Medical Coverage Policy Monitored Anesthesia Care (MAC) Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2004 Policy Last Updated: 1/8/2013 Prospective review is recommended/required.
Medical Coverage Policy Monitored Anesthesia Care (MAC) Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2004 Policy Last Updated: 1/8/2013 Prospective review is recommended/required.
Program Specification for Master Degree Anesthesia, ICU and Pain Management
 Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
M A T E R N I T Y C A R E. Managing Pain. During Labor & Delivery
 M A T E R N I T Y C A R E Managing Pain During Labor & Delivery Managing Your Pain One of the most common concerns about labor and delivery is pain. How much will it hurt? How will I cope? At MidMichigan
M A T E R N I T Y C A R E Managing Pain During Labor & Delivery Managing Your Pain One of the most common concerns about labor and delivery is pain. How much will it hurt? How will I cope? At MidMichigan
Top-up for Cesarean section. Dr. Moira Baeriswyl, Prof. Christian Kern
 Top-up for Cesarean section Dr. Moira Baeriswyl, Prof. Christian Kern In which situations? 2 What exactly is a Top-up? 3 C-section, NOW!! Emergency C-section requires a rapid onset of sustained analgesia
Top-up for Cesarean section Dr. Moira Baeriswyl, Prof. Christian Kern In which situations? 2 What exactly is a Top-up? 3 C-section, NOW!! Emergency C-section requires a rapid onset of sustained analgesia
VA SAN DIEGO HEALTHCARE SYSTEM MEMORANDUM 118-28 SAN DIEGO, CA
 GUIDELINES FOR PATIENT-CONTROLLED ANALGESIA (PCA) AND PATIENT- CONTROLLED EPIDURAL ANALGESIA (PCEA) FOR ACUTE PAIN MANAGEMENT 1. PURPOSE: To assure the safe and effective use of patient controlled analgesia
GUIDELINES FOR PATIENT-CONTROLLED ANALGESIA (PCA) AND PATIENT- CONTROLLED EPIDURAL ANALGESIA (PCEA) FOR ACUTE PAIN MANAGEMENT 1. PURPOSE: To assure the safe and effective use of patient controlled analgesia
Post-operative Pain Management
 Post-operative Pain Management Total Hip Replacement www.ormc.org A member of the Greater Hudson Valley Health System Post-operative Pain MANAGEMENT Post-operative pain management after total joint replacement
Post-operative Pain Management Total Hip Replacement www.ormc.org A member of the Greater Hudson Valley Health System Post-operative Pain MANAGEMENT Post-operative pain management after total joint replacement
INTRODUCTION BY ANDRÉ P BOEZAART MD, PHD
 BY ANDRÉ P BOEZAART MD, PHD Author Affiliation: Department of Anesthesia, University of Iowa, Iowa City, IA INTRODUCTION Due to the multiplicity and divergence of the nerve supply to the joints of the
BY ANDRÉ P BOEZAART MD, PHD Author Affiliation: Department of Anesthesia, University of Iowa, Iowa City, IA INTRODUCTION Due to the multiplicity and divergence of the nerve supply to the joints of the
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Mississippi Board of Nursing
 Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Epidural Anesthesia. Advantages of Epidural Anesthesia
 Epidural Anesthesia Epidural anesthesia involves the use of local anesthetics injected into the epidural space to produce a reversible loss of sensation and motor function. Epidural anesthesia requires
Epidural Anesthesia Epidural anesthesia involves the use of local anesthetics injected into the epidural space to produce a reversible loss of sensation and motor function. Epidural anesthesia requires
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
PHSW Procedural Sedation Post-Test Answer Key. For the following questions, circle the letter of the correct answer(s) or the word true or false.
 PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
Anesthesia Coding and Compliance. Presented by: Melanie Lafferty June 2015
 Anesthesia Coding and Compliance Presented by: Melanie Lafferty June 2015 Conflict of Interest Disclosure Statement Melanie Lafferty, Vice President of Practice Management Medac, Inc. I have the following
Anesthesia Coding and Compliance Presented by: Melanie Lafferty June 2015 Conflict of Interest Disclosure Statement Melanie Lafferty, Vice President of Practice Management Medac, Inc. I have the following
Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines for the Management of Major Regional Analgesia
 PS03 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Faculty of Pain Medicine Guidelines for the Management of Major Regional Analgesia 1. OVERVIEW This document is intended to apply to
PS03 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Faculty of Pain Medicine Guidelines for the Management of Major Regional Analgesia 1. OVERVIEW This document is intended to apply to
Intraocular Pressure and Quality of Blockade in Peribulbar Anesthesia Using Ropivacaine or Lidocaine with Adrenaline: A Double-Blind Randomized Study
 Tohoku J. Exp. Med., 2004, Ropivacaine 204, 203-208 in Peribulbar Block: a Comparison with Lidocaine 203 Intraocular Pressure and Quality of Blockade in Peribulbar Anesthesia Using Ropivacaine or Lidocaine
Tohoku J. Exp. Med., 2004, Ropivacaine 204, 203-208 in Peribulbar Block: a Comparison with Lidocaine 203 Intraocular Pressure and Quality of Blockade in Peribulbar Anesthesia Using Ropivacaine or Lidocaine
519.2 ANESTHESIA SERVICES. Background... 2. Policy... 2. 519.2.1 Covered Services... 2. 519.2.1.1 Anesthesiologist Directed Services...
 TABLE OF CONTENTS SECTION PAGE NUMBER Background... 2 Policy... 2 519.2.1 Covered Services... 2 519.2.1.1 Anesthesiologist Directed Services... 3 519.2.1.2 Emergency Anesthesia... 4 519.2.1.3 Monitored
TABLE OF CONTENTS SECTION PAGE NUMBER Background... 2 Policy... 2 519.2.1 Covered Services... 2 519.2.1.1 Anesthesiologist Directed Services... 3 519.2.1.2 Emergency Anesthesia... 4 519.2.1.3 Monitored
Fine jewelry is rarely reactive, but cheaper watches, bracelets, rings, earrings and necklaces often contain nickel.
 BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
Recommendations for the Perioperative Care of Patients Selected for Day Care Surgery
 Page 1 of 7 Recommendations for the Perioperative Care of Patients Selected for Day Care Surgery Version Effective Date 1 Feb 1993 (Reviewed Feb 2002) 2 Oct 2012 Document No. HKCA P5 v2 Prepared by College
Page 1 of 7 Recommendations for the Perioperative Care of Patients Selected for Day Care Surgery Version Effective Date 1 Feb 1993 (Reviewed Feb 2002) 2 Oct 2012 Document No. HKCA P5 v2 Prepared by College
devoted physicians. collaborative partners. metrics-driven quality.
 Regional Anesthesia and Multimodal Pain Management Improves Outcomes, Reduces Costs and Boosts Patient Satisfaction devoted physicians. collaborative partners. metrics-driven quality. usap.com jlrmedicalgroup.com
Regional Anesthesia and Multimodal Pain Management Improves Outcomes, Reduces Costs and Boosts Patient Satisfaction devoted physicians. collaborative partners. metrics-driven quality. usap.com jlrmedicalgroup.com
CHAP2-CPTcodes00000-01999_final103115.doc Revision Date: 1/1/2016
 CHAP2-CPTcodes00000-01999_final103115.doc Revision Date: 1/1/2016 CHAPTER II ANESTHESIA SERVICES CPT CODES 00000-09999 FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES Current
CHAP2-CPTcodes00000-01999_final103115.doc Revision Date: 1/1/2016 CHAPTER II ANESTHESIA SERVICES CPT CODES 00000-09999 FOR NATIONAL CORRECT CODING INITIATIVE POLICY MANUAL FOR MEDICARE SERVICES Current
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Your anaesthetist may suggest that you have a spinal or epidural injection. These
 Risks associated with your anaesthetic Section 11: Nerve damage associated with a spinal or epidural injection Your anaesthetist may suggest that you have a spinal or epidural injection. These injections
Risks associated with your anaesthetic Section 11: Nerve damage associated with a spinal or epidural injection Your anaesthetist may suggest that you have a spinal or epidural injection. These injections
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Evaluation of a Morphine Weaning Protocol in Pediatric Intensive Care Patients
 Evaluation of a Morphine Weaning Protocol in Pediatric Intensive Care Patients Jennifer Kuhns, Pharm.D. Pharmacy Practice Resident Children s Hospital of Michigan **The speaker has no actual or potential
Evaluation of a Morphine Weaning Protocol in Pediatric Intensive Care Patients Jennifer Kuhns, Pharm.D. Pharmacy Practice Resident Children s Hospital of Michigan **The speaker has no actual or potential
British Journal of Anaesthesia 101 (2): 250 4 (2008) doi:10.1093/bja/aen132 Advance Access publication May 30, 2008
 British Journal of Anaesthesia 11 (2): 25 4 (28) doi:1.193/bja/aen132 Advance Access publication May 3, 28 REGIONAL ANAESTHESIA International normalized ratio and prothrombin time values before the removal
British Journal of Anaesthesia 11 (2): 25 4 (28) doi:1.193/bja/aen132 Advance Access publication May 3, 28 REGIONAL ANAESTHESIA International normalized ratio and prothrombin time values before the removal
Conscious Sedation Policy
 PURPOSE Provide guidelines to ensure safe and consistent process for patient selection, administration, monitoring and discharge care of patients receiving conscious sedation. Conscious sedation refers
PURPOSE Provide guidelines to ensure safe and consistent process for patient selection, administration, monitoring and discharge care of patients receiving conscious sedation. Conscious sedation refers
Spinal Injections. North American Spine Society Public Education Series
 Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Spinal Injections North American Spine Society Public Education Series What Is a Spinal Injection? Your doctor has suggested that you have a spinal injection to help reduce pain and improve function. This
Liau DW : Injuries and Liability Related to Peripheral Catheters: A Closed Claims Analysis. ASA Newsletter 70(6): 11-13 & 16, 2006.
 Citation Liau DW : Injuries and Liability Related to Peripheral Catheters: A Closed Claims Analysis. ASA Newsletter 70(6): 11-13 & 16, 2006. Full Text An anesthesiologist inserted a 14-gauge peripheral
Citation Liau DW : Injuries and Liability Related to Peripheral Catheters: A Closed Claims Analysis. ASA Newsletter 70(6): 11-13 & 16, 2006. Full Text An anesthesiologist inserted a 14-gauge peripheral
Equine Sedation, Anesthesia and Analgesia
 Equine Sedation, Anesthesia and Analgesia Janyce Seahorn, DACVAA, DACVIM-LA, DACVECC Lexington Equine Surgery and Sports Medicine Equine Veterinary Specialists Georgetown, KY The need for equine field
Equine Sedation, Anesthesia and Analgesia Janyce Seahorn, DACVAA, DACVIM-LA, DACVECC Lexington Equine Surgery and Sports Medicine Equine Veterinary Specialists Georgetown, KY The need for equine field
Title/Subject Procedural Sedation and Analgesia Page 1 of 10
 Policy Procedural Sedation and Analgesia Page 1 of 10 Scope: Providers and nurses (M.D., D.O., D.M.D., D.D.S., A.P.R.N., P.A., R.N.) with appropriate privileges and who have successfully demonstrated adequate
Policy Procedural Sedation and Analgesia Page 1 of 10 Scope: Providers and nurses (M.D., D.O., D.M.D., D.D.S., A.P.R.N., P.A., R.N.) with appropriate privileges and who have successfully demonstrated adequate
Significant nerve damage is uncommonly associated with a general anaesthetic
 Risks associated with your anaesthetic Section 10: Nerve damage associated with an operation under general anaesthetic Section 10: Significant nerve damage is uncommonly associated with a general anaesthetic
Risks associated with your anaesthetic Section 10: Nerve damage associated with an operation under general anaesthetic Section 10: Significant nerve damage is uncommonly associated with a general anaesthetic
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
National Clinical Programme in Surgery (NCPS) Care Pathway for the Management of Day Case Laparoscopic Cholecystectomy
 National Clinical Programme in Surgery (NCPS) Care Pathway for the Management of Day Case Consultant Surgeon DRAFT VERSION 0.5 090415 Table of Contents 1.0 Purpose... 3 2.0 Scope... 3 3.0 Responsibility...
National Clinical Programme in Surgery (NCPS) Care Pathway for the Management of Day Case Consultant Surgeon DRAFT VERSION 0.5 090415 Table of Contents 1.0 Purpose... 3 2.0 Scope... 3 3.0 Responsibility...
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MANAGEMENT OF THE PREGNANT PATIENT WITH EPIDURAL ANESTHESIA POLICY #: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: PAGE: 126.722 (maternal) 10/88
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MANAGEMENT OF THE PREGNANT PATIENT WITH EPIDURAL ANESTHESIA POLICY #: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: PAGE: 126.722 (maternal) 10/88
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Influence of ph Most local anesthetics are weak bases.
 Local anesthetics The agent must depress nerve conduction. The agent must have both lipophilic and hydrophilic properties to be effective by parenteral injection. Structure-activity relationships The typical
Local anesthetics The agent must depress nerve conduction. The agent must have both lipophilic and hydrophilic properties to be effective by parenteral injection. Structure-activity relationships The typical
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]
![SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]](/thumbs/27/9667060.jpg) SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D.
 PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D. A. INDICATIONS: Periocular steroid injection involves placement of steroid around the eye to treat intraocular inflammation or swelling of
PERIOCULAR (SUBTENON) STEROID INJECTION ERIC S. MANN M.D.,Ph.D. A. INDICATIONS: Periocular steroid injection involves placement of steroid around the eye to treat intraocular inflammation or swelling of
Perioperative Management of Patients with Obstructive Sleep Apnea. Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine
 Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
The most important room in the hospital : that s
 ECRI Institute Perspectives Postanesthesia care action plan aims to ensure optimal patient safety The most important room in the hospital : that s what a landmark 1969 case in Canada Laidlaw v. Lions Gate
ECRI Institute Perspectives Postanesthesia care action plan aims to ensure optimal patient safety The most important room in the hospital : that s what a landmark 1969 case in Canada Laidlaw v. Lions Gate
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
Epinephrine and clonidine do not improve intrathecal sufentanil analgesia after total hip replacement ²
 British Journal of Anaesthesia 89 (4): 562±6 (2002) Epinephrine and clonidine do not improve intrathecal sufentanil analgesia after total hip replacement ² R. Fournier*, E. Van Gessel, A. Weber and Z.
British Journal of Anaesthesia 89 (4): 562±6 (2002) Epinephrine and clonidine do not improve intrathecal sufentanil analgesia after total hip replacement ² R. Fournier*, E. Van Gessel, A. Weber and Z.
The Basics of Anesthesia
 The Basics of Anesthesia Billing. Judy A. Wilson, CPC,CPC-H,CPC-P,CPC-I,CANPC,CMBSI,CMRS Disclosures This presentation is intended to provide basic educational information regarding coding/billing for
The Basics of Anesthesia Billing. Judy A. Wilson, CPC,CPC-H,CPC-P,CPC-I,CANPC,CMBSI,CMRS Disclosures This presentation is intended to provide basic educational information regarding coding/billing for
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Acute & Chronic Pain Management (requiring opioid analgesics) in Patients Receiving Pharmacotherapy for Opioid Addiction
 Acute & Chronic Pain Management (requiring opioid analgesics) in Patients Receiving Pharmacotherapy for Opioid Addiction June 9, 2011 Tufts Health Care Institute Program on Opioid Risk Management Daniel
Acute & Chronic Pain Management (requiring opioid analgesics) in Patients Receiving Pharmacotherapy for Opioid Addiction June 9, 2011 Tufts Health Care Institute Program on Opioid Risk Management Daniel
Comparison of Fascia Iliaca Compartment Block and 3-in-1 Block in Adults Undergoing Knee Arthroscopy and Meniscal Repair
 Comparison of Fascia Iliaca Compartment Block and 3-in-1 Block in Adults Undergoing Knee Arthroscopy and Meniscal Repair LT Jerrol B. Wallace, CRNA, MSN, NC, USN LT Joseph A. Andrade, CRNA, MSN, NC, USN
Comparison of Fascia Iliaca Compartment Block and 3-in-1 Block in Adults Undergoing Knee Arthroscopy and Meniscal Repair LT Jerrol B. Wallace, CRNA, MSN, NC, USN LT Joseph A. Andrade, CRNA, MSN, NC, USN
Thoracic Epidural Catheterization Using Ultrasound in Obese Patients for Bariatric Surgery
 IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
General Anesthesia Factors affecting recovery and discharge following ambulatory surgery
 858 858 CANADIAN JOURNAL OF ANESTHESIA General Anesthesia Factors affecting recovery and discharge following ambulatory surgery [Les facteurs influençant la récupération et la sortie après une opération
858 858 CANADIAN JOURNAL OF ANESTHESIA General Anesthesia Factors affecting recovery and discharge following ambulatory surgery [Les facteurs influençant la récupération et la sortie après une opération
Pain Management after Surgery Patient Information Booklet
 Pain Management after Surgery Patient Information Booklet PATS 509-15-05 Your Health Care Be Involved Be involved in your healthcare. Speak up if you have questions or concerns about your care. Tell a
Pain Management after Surgery Patient Information Booklet PATS 509-15-05 Your Health Care Be Involved Be involved in your healthcare. Speak up if you have questions or concerns about your care. Tell a
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Sedation for diagnostic and therapeutic procedures in children and young people 1.1 Short title Sedation in children and young
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Sedation for diagnostic and therapeutic procedures in children and young people 1.1 Short title Sedation in children and young
John J Christoforetti, MD Mark Langhans Jr, BS, JT Redshaw, BS, Michael Allen DPT, Ellen Wilson ATC, Elizabeth Pickle, Ben Kivlan PT
 SAFETY OF OUTPATIENT HIP ARTHROSCOPY AS COMPARED TO INPATIENT ADMISSION: A PROSPECTIVE COHORT STUDY OF THE FIRST 100 OPERATIVE ARTHROSCOPIES FOR A FELLOWSHIP TRAINED HIP ARTHROSOCOPIST John J Christoforetti,
SAFETY OF OUTPATIENT HIP ARTHROSCOPY AS COMPARED TO INPATIENT ADMISSION: A PROSPECTIVE COHORT STUDY OF THE FIRST 100 OPERATIVE ARTHROSCOPIES FOR A FELLOWSHIP TRAINED HIP ARTHROSOCOPIST John J Christoforetti,
SECTION 5 HOSPITAL SERVICES. Free-Standing Ambulatory Surgical Center
 SECTION 5 HOSPITAL SERVICES Table of Contents 1 GENERAL POLICY... 2 1-1 Clients Enrolled in a Managed Care Plan... 3 1-2 Clients NOT Enrolled in a Managed Care Plan (Fee-for-Service Clients)..................
SECTION 5 HOSPITAL SERVICES Table of Contents 1 GENERAL POLICY... 2 1-1 Clients Enrolled in a Managed Care Plan... 3 1-2 Clients NOT Enrolled in a Managed Care Plan (Fee-for-Service Clients)..................
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Comparison of the Duration of Sensory Block and Side Effects of Adding Different Doses of Intrathecal fentanyl to Lidocaine 5% in Spinal Anesthesia
 JOURNAL OF IRANIAN CLINICAL RESEARCH ORIGINAL ARTICLE Comparison of the Duration of Sensory Block and Side Effects of Adding Different Doses of Intrathecal fentanyl to Lidocaine 5% in Spinal Anesthesia
JOURNAL OF IRANIAN CLINICAL RESEARCH ORIGINAL ARTICLE Comparison of the Duration of Sensory Block and Side Effects of Adding Different Doses of Intrathecal fentanyl to Lidocaine 5% in Spinal Anesthesia
Drugs & Everything Else
 Pain Relief, Common Drugs & Everything Else Henrik Jörnvall MD, PhD MKAIC November 11 2011 Lidocaine Noradrenaline Isoflurane Morphine Ropivacaine Platelets l t Pethidine Dobutamine Propofol Normal Saline
Pain Relief, Common Drugs & Everything Else Henrik Jörnvall MD, PhD MKAIC November 11 2011 Lidocaine Noradrenaline Isoflurane Morphine Ropivacaine Platelets l t Pethidine Dobutamine Propofol Normal Saline
Pain Relief Options for Labor. Providing You with Quality Care, Information and Support
 Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Pain Relief Options for Labor Providing You with Quality Care, Information and Support What can I expect during my labor and delivery? As a patient in the Labor and Delivery Suite at Lucile Packard Children
Changes in Practice: Evidence Based Nursing Revealed
 Changes in Practice: Evidence Based Nursing Revealed Gloria Spencer,, RN, MSPHN Sr. Nursing Instructor Nursing Education Department PACU Staff Nurses Yolanda Ayson, MSN, RN Maria Aguda, BSN, CPAN Imelda
Changes in Practice: Evidence Based Nursing Revealed Gloria Spencer,, RN, MSPHN Sr. Nursing Instructor Nursing Education Department PACU Staff Nurses Yolanda Ayson, MSN, RN Maria Aguda, BSN, CPAN Imelda
OB PBLD L117 Labor and Delivery in the Age of Ebola Upper 20B-20C. PI PBLD L120 He's 15, Needs This Operation, and He's DNR!
 ETHICS - Saturday, October 24 OB PBLD L117 Labor and Delivery in the Age of Ebola PI PBLD L120 He's 15, Needs This Operation, and He's DNR! PD PBLD L118 Sex, Drugs, and Rock 'N' Roll: An Anxious Adolescent
ETHICS - Saturday, October 24 OB PBLD L117 Labor and Delivery in the Age of Ebola PI PBLD L120 He's 15, Needs This Operation, and He's DNR! PD PBLD L118 Sex, Drugs, and Rock 'N' Roll: An Anxious Adolescent
