Official Journal of the Italian College of Phlebology
|
|
|
- Branden York
- 8 years ago
- Views:
Transcription
1 Volume 8 No. 2 August 2007 Official Journal of the Italian College of Phlebology In this issue The eloquence of symbols: Smultronstället Agus G. B. The role of crossectomy in 2007 Allegra C. Focus on an Internet Meeting Passariello F. Late diagnosis of DVT: a persisting problem Arpaia G., Mastrogiacomo O., Carpenedo M., De Gaudenzi E., Milani M., Cimminiello C. Venous thromboembolism in nerosurgical patien: intermittent pneumatic compression as enforced prophylactic method? Apperti M., Goffredi L., Di Lucia A., Luongo M., Moraci A. Carbondioxide Therapy medical system Carbomed The only system certified According to CE Law 93/42 CE0051 class IIB Carboxytherapy: effects on microcirculation and its use in the treatment of severe lymphedema. A. review Varlaro V., Manzo G., Mugnaini F., Bisacci C., Fiorucci P., De Rango P., Bisacci T. Low-Molecular- Weight-Heparins: an update Antignani P. L., Goffredo C., Lassandro Pepe L., Allegra C. Organo Ufficiale del Collegio Italiano di Flebologia
2 Pubblicazione periodica quadimestrale Post Italiane S.p.A. sped. In A.p., 353/2003 (conv. In L 27/02/2004 no. 45)art. 1, comma 1, DCB/CN- Taxe Perçue Carboxytherapy: effects on microcirculation and its use in the treatment of severe lymphedema A review V. VARLARO 1, G. MANZO 1, F. MUGNAINI 1, C. BISACCI 1, P. FIORUCCI 1, P. DE RANGO 2, R. BISACCI 1 Carboxytherapy refers to the administration of CO 2 for therapeutic purposes. It has been shown that, because of the interaction between CO 2 and regulating factors of tissue perfusion, Carboxytherapy acts on the microcirculation at the level of metarterioles, arterioles and precapillary shpincteres by increasing tissue flow velocity and consequently, by improving lymphatic drainage. Analysis of literature data shows a wide range of today applications for this treatment involving either phlebology or nonphlebology fields. Specifically, the positive effect on the increase of lymphatic drainage has more recently made Carboxytherapy useful for treatment of lymphatic stasis. Basic hemodynamic, histologyc and biochemical principles that explain the effects on microcirculation bed and lymphatic drainage are here analyzed to show how Carboxytherapy can be useful in the treatment of diseases such as severe lymphedema. KEY WORDS: Carboxytherapy - Microcirculation - Lymphedema. EDIZIONI MINERVA MEDICA arboxytherapy refers to the administration of CO 2 for therapeutic purposes. 1 Although this treatment originated in France in 1932 and was then introduced in Italy in 1990 by Belotti and De Bernardi, 2 it was only in 1995 that the term Carboxytherapy was coined by Luigi Parassoni during the XVI National Meeting of Esthetical Medicine, promoted at Rome by the Italian Society of Esthetical Medicine Indeed, this therapy was also known as carbon dioxide therapy because of the CO 2 molecular configuration including two oxygen and one hydrogen atoms. Address reprint requests to:.. 1 Interuniversitary Center for the Education and the Research on Phlebology Department of Surgical Sciences University of Perugia, Perugia, Italy 2 Department of Vascular and Endovascular Surgery University of Perugia, Perugia, Italy Hemodynamic essentials The microcirculation The role of cardiovascular system is to provide oxygen, nutrients and hormones to, as well as remove carbon dioxide and wasted from the cells and to ensure body homeostasis by keeping the concentration of dissolved participles, the temperature, the volume and the ph level largely constant. The circulatory system can be subdivided into a pulmonary circulation and a systemic circulation, the last providing to the perfusion for all the tissues except for lungs and also called big circulation or peripheral circulation. 5 Due to dissimilarities concerning development and function, blood vessels are differentiated in arterials, arterioles, metarterioles, capillaries,venules and veins. In the microcirculation arterial tree divides into munerous arterioles which again divide into capillaries and sinusoids. Components of Microcirculation, that refers to the smallest blood vessels in the body, are shown in Figure 1.
3 Arterial vessels supply high pressure blood flow from systems. By the contraction of the heart muscle, the blood is then driven rhythmically (at each systole) and at high pressure through arteries which, due to their elastic properties, represent a pressure chamber. The most important function of large arteries is to reduce the impedance (dynamic resistance to the oscillatory components of pulsatile flow) to left ventricular outflow. This is accomplished directly by arterial expansion during systole and storage of blood for run-off in diastole. The elastic retractions of the arterial walls push and dampen the flow from the large arteries towards the microcirculation. Blood flow is subsequently collected into the low pressure system of the venules and veins. Histology essentials the heart to body tissues. The function of arterioles and metarterioles is to regulate blood flow through capillary bed and to ensure a vis a tergo that allows flow in the microcirculation. The principal function of capillaries is to permit the exchange of substances (water, electrolytes, nutrients, hormones) between tissues and blood. The venules collect blood from capillary bed and finally, the veins transport the blood back to heart and also serve as capacity vessels of large volume. A common characteristic for all the types of circulatory vessels is the distensible property. In the arterial district, distensibility allows vessels to receive high pressure, pulsatile blood flow from the heart pump and to deliver while buffering these pulsatile excessive pressure and flow towards the small peripheral vessels. The highest distensibility is a property of the venous systems. Due to the large expansibility the veins represent a temporary reservoir of large blood volumes which are stored but can be utilized, when necessary, in whichever body district. 5 Elastic retraction is an essential property of arterial vessels in order to ensure a continuous blood flow in the microcirculation. Without this retraction, the blood could reach peripheral bed (microcirculation) exclusively during the systolic phase due to the propulsive heart force. Properties and functions of arterials are explained by the structure of the arterial wall. 5 The wall of arterial vessels is quite thick and strong and is structured in a typical well distinct three-layer configuration that is common for all the arteries: an intimae layer (tunica intima) made up of endothelial cells, a medium layer (tunica media) mainly represented by transverse-oriented smooth muscle fibro cells and an adventitial external layer (tunica adventitia) formed by bundles of fibroblastic cells and collagen fibres mostly oriented with longitudinal direction. An internal elastic membrane is mostly present at the border between tunica intima and media. The external elastic membrane demarcates the border to the tunica adventitia (Figure 2). According to the wall composition two types of arteries, elastic (conductive arteries) and muscular (distributive arteries), can be identified.in elastic arteries, which include the largest arteries of the body, the borders between intima, media and adven-titia are less distinct compared to muscular arteries, due to the presence of numerous fenestrated elastic lamellae in all three layers. In the medium layer up to 70 lamina of elastin with large fenestration can be found. Close to the heart, elasticity of the arteries is of great functional importance: during systole, the aorta and the elastic arteries dilate and then, during diastole, gradually return to their original size due to their elastic properties. By this means, the pulsatile blood flow is turned into a more steady flow, reducing blood pressure requirements. The heart is filled with low pressure blood flow from the venous
4 The most common type of arterial vessels is represented by muscular arteries. In these, the medium layer is composed by variable strata of smooth muscle fibro cells ( myofibroblast ), ranging from 3-4 in the smallest arteries to strata in the largest. Arterioles and metarterioles are small muscular vessels (an endothelium surrounded by one or more layers of smooth muscle cells) and represent a major site for regulating systemic vascular resistance in the micro-circulatory bed. These vessels are named as the heart of the microcirculatory system and provide the vis a tergo for microcirculation flow. Indeed, rhythmical contractions and relaxations in the arterioles walls are the source of the force ( vis a tergo ) that drives and regulates the blood flow into the microcirculation bed. Fluctuations in systemic pressure are almost completely damped out by the arterioles at the level of microcirculatory flow (Figure 3). Finally, in vein vessels the wall is quite thin but contains a muscular layer of smooth myocytes that allows the vessels to expand or to contract and therefore, to collect or release large blood volumes into the circulatory bed. Microcirculation regulation Under normal circumstances, continued adequate perfusion of individual vascular beds is assured by the capacity of blood vessels and heart contraction. Blood vessels are regulated by nervous, hormonal and local stimuli. 5 Neurogenic regulation of blood circulation, provided by the autonomic nervous system, affects general functions such as the distribution of flow to different organs of the body, the strength the heart pump and the rapid regulation of blood pressure. The autonomic regulation of circulatory vessels is mainly due to sympathetic adrenergic fibres, while the parasympathetic nerves mainly act on the heart Sympathetic vasomotor fibres originated in the spinal cord travel with the thoracic nerves and the two upper lumbar nerves to reach the ganglia of sympathetic chain from which they depart using two different ways to innervate the E METARTERIOLE circulatory system: 1. specific sympathetic nerves to supply the heart and the major vessels 2. spinal nerves to regulate peripheral territories. 5 The Sympathetic system provides innervations for all the vascular systems (including arterial and venous systems) with the only exception of capillaries, pre-capillary sphincters and the majority of metarterioles which are mostly regulated by humoral local factors (Figure 4). The vasomotor centre (located in the reticular area of the medulla and in the third inferior of the pons ) repeatedly transmits signals to the sympathetic vasoconstrictive fibres at a rate of per second. This continuous discharge is called as sympathetic vasomotor tone and allows a persistent partial contraction of the vessels wall. Any increase in sympathetic autonomic system output enhances wall vessel contractility (vasomotor effect), peripheral resistance and cardiac filling pressure and decreases vessel capacitance and circulating blood mass. The nervous autonomic system plays a main regulatory function by inducing significant changes in filling and capacity. ARTERIOL VIS A TERGO Figure 3. Microcirculatory arterioles and metarterioles: vis a tergo. Arterioles and metarterioles represent a major site for regulating systemic vascular resistance in the microcirculatory bed. These vessels are the heart of the microcirculatory system and provide the vis a tergo for microcirculation flow. Indeed, rhythmical contractions and relaxations in the arterioles walls are the source of the force ( vis a tergo ) that drives and regulates the blood flow into the microcirculation bed. Fluctuations in systemic pressure are completely damped out by the arterioles at the level of microcirculatory flow. functions and exert only a minor effect on the vessels.
5 However, autonomic system is only just involved in the changes of tissue blood flow, the main regulation of tissue perfusion being driven by local factors (Figure 5). Arteriole ENDOTHELIAL CELLS GROWTH FACTORS, FIBRO-CELLS GROWTH FACTORS, ANGIOGENINE An essential principle of the circulatory function is the ability for each circulatory district to regulate local perfusion according to the specific metabolic necessity. Since in each tissue metabolic requirements vary over the time, local flow accordingly changes. Indeed, local flow needs depend from variable tissue metabolic requirements such as O 2 provision, nutrients supply (glucose, lipid, amino acid.), CO 2 removal, preservation of an appropriate ionic tissue concentration and hormones transportation. Furthermore, there are some tissues with specific functions and requirements. Blood vessels of the skin need to fulfil at least two functions: nourishment and thermoregulation. By regulating skin capillary perfusion, heat loss may significantly vary. At the renal level, local circulation allows the removal of metabolic wasted contributing to the emunctories (depurative) function. As a general rule, the higher the metabolic tissue activity, the higher the local blood flow requirement. At rest, in the muscle tissue there is little metabolic activity and consequently, the basic flow is very low (4 ml/minute/100 g). However, with strong physical activity, muscle metabolic requirements can increase for more than 60 folds and blood flow can increase for more than 20 folds (up to 80 ml/minute per 100 g). 5 CARBON DIOXIDE, ADENOSINE, ADENOSINE DERIVATES, PHOSPHATES, HISTAMINE, Venule PATASSIUMIONS, HYDROGENESIONS- LACTIC ACID Tissue flow is regulated by the release of several local factors (Figure 5). All these local factors contribute to regulate local perfusion in short and long term. Factors regulating short term local perfusion include: CO 2 (carbon dioxide), lactic acid, adenosine derivates, phosphates, histamine, potassium, hydrogen ions. Local factors regulating tissue flow in the long term include endothelial growth factors, fibro cells growth factors and angiogenine. Short term regulation of tissue perfusion (by CO 2 and adenosine) is determined by the enhancement in rhythmic dilations and constrictions of vessel wall at the level of arterioles, metarterioles and precapillary sphincters ( increased vasomotion ) with correspondent flow modifications. These changes of local flow occur within few seconds or minutes with the purpose to maintain perfusion appropriate to local metabolic requirements. Long term regulation of local flow (mediated by growth factors) is managed by the expansion of the microcirculatory bed ( true and false angiogenesis). This vascular bed increase may require few days, weeks or some months. Vasomotion A single metarteriola, a single capillary and the surrounding tissue form a tissue unit. Precapillary sphincters are located at the proximal level of the capillary vessels while several smooth muscle fibrocells surround the metarteriola. Figure 5. Microcirculatory network and regulating factors. Top, left:short term regulating factors. Bottom on the right: long term regulating factors.
6 Experimental models on wing bat under microscopy magnification, have shown that precapillary sphincters may be opened or closed and the metarteriole tone (persistent basal contraction of muscle cells in vessel wall) may change over the time. At a definite time, the number of opened precapillary sphincters corresponds to the tissue requirements for oxygen and nutrients in that time. Furthermore, sphincters and metarterioles can open and close cyclically, several times per minutes. This rhythmic (at regular intervals) opening and closing of metarterioles and precapillary sphincters is named vasomotion. Since smooth muscle cells require oxygen to begin and maintain contraction, the contractile strength of precapillary sphincters increases when oxygen availability rises. Therefore, when oxygen concentration increases above a threshold level, precapillary sphincters and metarterioles close down and tissue flow slows until the excess of oxygen is completely utilized by the tissue cells. On the contrary, any decrease in oxygen concentration causes the release and complete opening of metarterioles and precapillary sphincters with a subsequent enhancement in flow velocity and tissue perfusion. Short term local flow regulation Short term regulation of tissue flow is mainly determined by local factors: CO 2, adenosine, lactic acid, phosphates, histamine, potassium, hydrogen ions. This short term regulation is mediated by vasodilatation at metarterioles and arterioles level due to the relaxation of smooth muscle cells in the vessels wall and the enhanced vasomotion. These adjustments occur within few seconds or minutes to rapidly adapt local flow to tissue requirements. Short term regulation causes abrupt modification of local perfusion due to a very consistent change in the contractile tone of arterioles, metarterioles and precapillary sphincters. Several factors interact for short term regulation, including tissue metabolism, oxygen and nutrients availability. Tissue metabolism: It has been shown that 8 folds increase in tissue metabolism is followed by 4 times increase in the local flow. Consequences of Oxygen and metabolic availability on local flow: at any time local oxygen availability decreases, such as in the altitudes, during pneumonia and in poisoning from carbon monoxide (that reduces haemoglobin ability of carrying oxygen) or cyanides (that reduce oxygen utilization from tissues), as a consequence local blood flow significantly increases. Two different theories are suggested to explain flow changes due to metabolic or oxygen variations: Flow dependent regulation (Vasodilatation hypothesis); Oxygen requirement hypothesis. release of strong vasodilator factors that act by increasing arterioles, metarterioles and pre-capillary sphincters relaxation. This allows substantial vasodilatation and enhanced flow. Several factors have been described as putative mediators of the coupling between oxygen consumption, metabolism increase and vasomotor tone (vasodilatation stimulating factors, released in condition of increased metabolism or decreased oxygen availability) such as adenosine, CO 2, lactic acid, adenosine derivates, phosphates, histamine, potassium and hydrogen ions. 5 Recently, particular attention has been paid to the role of adenosine as one of the most powerful vasodilators acting directly (via the A2 receptors) upon the smooth muscle cells of coronary arteries. The hypothesis that adenosine could represent a major signal coupling the myocardial metabolism and the coronary flow is supported by the observation that its actual concentration in myocardial interstitium is indeed within the range of its vasoactive effect. When coronary flow is reduced, interstitial adenosine levels increase: this is followed by active coronary artery vasodilatation and re-established coronary normal flow. Similarly, in cases of heart hyperactivity and increased metabolites and oxygen consumption, an increase in tissue ATP degradation with increased adenosine production has been observed. It has been hypothesized that the released adenosine, in part, passes outside the muscle cell and stimulates coronary arteries vasodilatation in order to adapt coronary flow to the increased oxygen requirements due to the increased heart activity. 5 Many Authors suppose that the CO 2 promotes vasodilatation at arterioles and metarterioles levels using a mechanism similar to that of adenosine. Increase in interstitial CO 2 tension has indeed been considered a potential signal responsible for the metabolic control of the coronary blood flow. The CO 2 produced during increased myocardial activity directly stimulates coronary vasodilatation in order to increase the coronary flow and to adapt this to the increased cardiac oxygen requirements consequence of the increased activity. THE FLOW DEPENDENT REGULATION OF VASOMOTOR TONE (VASODILATATION HYPOTHESIS) According with the vasodilatation theory, the greater the metabolism or the lower the oxygen availability, the higher the
7 Both, adenosine and CO 2, are physiologic factors used for the autoregulation of local flow, that is the adjustment of local perfusion to metabolic and oxygen tissue requirements. THE OXYGEN REQUIREMENT HYPOTHESIS The flow dependent regulation of vasomotor tone is accepted by many Authors. However, Others support a different mechanism to explain changes in tissue flow: the hypothesis of the oxygen requirement, or better, the nutrients requirement since besides oxygen, many other local nutrients may be probably involved in local flow regulation. 5 Oxygen (such as other nutrients) is needed to maintain the contraction of smooth muscle cells of the arterial wall (vasomotor tone). In situations of scarce availability of oxygen (and other nutrients), arterial vessels tend to relax and dilate. Similarly, during increased metabolic activity, the augmented oxygen consumption could cause a decrease in oxygen availability for vessels smooth muscle fibro cells with consequent local arterial vasodilatation. Long term tissue flow regulation The regulation of tissue flow in the long term is based on the enlargement of the microcirculatory vascular bed. A true Angiogenesis and a false Angiogenesis are involved in obtaining the expansion of microcirculatory bed. 9 True angiogenesis The term angiogenesis refers to the growth, expansion and remodelling of vessels. This process occurs as a consequence of various angiogenic factors that may be released from ischemic tissues, rapid growing tissues or tissues with increased metabolic activity. Today more than 12 angiogenesis factors have been individuated. All of these are small peptides. The three most known factors being: endothelial cell growth factors; fibroblast growth factors; angiogenine. These factors have been isolated from tumoral cells or ischemic tissues. It has been hypothesized that the lack of tissue oxygen is the main cause for the production of angiogenic factors. Each of these factors promotes development of new vessels by the same mechanism of sprouting, growing and remodelling from venules and, more rarely, from capillaries. New arterioles and metarterioles are indeed generated. 5 Hypoxia is a strong stimulus for angiogenesis and therefore, for the regulation of flow in the long term. Indeed, an increase in microcirculatory bed has been found in several animals living in altitudes where atmosphere oxygen concentration is low. Other experimental studies have been performed in chicken embryos incubated in low oxygen atmospheres: development of microcirculatory bed has been doubled with respect to normal animals. Furthermore, in immature neonates who undergo oxygentherapy it has been shown that the increase in oxygen availability causes a rapid interruption in the physiologic process of retinal vessels neoformation, and even the degeneration of some formed capillaries. Subsequently, when the cycle of oxygen-therapy is completed and the newborn returns to a normal oxygen atmosphere concentration, the new condition of relative hypoxia provokes an impulsive fast growth of new vessels. In some circumstances this growth may be excessively chaotic to cause invasion of the vitreous from the neogenerated vessels and consequently blindness (retrolenticular fibroplasias). The Angiogenesis process can be stimulated by decreased availability of oxygen and, consequently by an excess of CO 2. CO 2 may promote the release of local growth factors able to stimulate angiogenesis. The extend of tissue vascularization (angiogenesis) can increase or decrease according with the metabolic activity of the same tissue. If metabolism increases (and therefore the release of CO 2 is high), tissue vascularization expands; vice versa, when metabolic activity decreases (and the CO 2 concentration is low), tissue vascularization concurrently shrinks. In conclusion, in true angiogenesis there is a constant remodeling of microcirculatory vessels according with tissue metabolic requirements. False angiogenesis The theory of false angiogenesis was ideated by Curri. 11 The Author suggested that CO 2 promotes the expansion of microcirculatory bed by the recanalization of virtual capillaries. This false angiogenesis is not directly stimulated by CO 2 but is the consequence of the increased tissue flow. The term false angiogenesis was used because the increase in vascular bed was not due to neoformation of new vessels promoted by growth factors, but for the recanalization of pre-existent virtual capillaries. True and False angiogenesis might cooperate in determining the increase of microcirculatory vascular bed. Indeed this expansion in vascularization may be consequence from the combination of: a true angiogenesis (vessels neoformation) stimulated by endothelial and fibroblast growth factors and angiogenine; 5 a false angiogenesis, that is the recanalization of virtual capillaries stimulated by the notably increased local flow velocity and volume. 9 Carbon DIOXIDE (CO 2 ) metabolism and excretion: biochemical essentials Carbon dioxide (CO 2 ) formed during cellular metabolism moves across the cell wall (from inside to outside) in a gaseous status to be removed. This is because only a very small amount of CO 2 can diffuse as bicarbonate ions that are almost completely impermeable to the cell wall. 7 After entering into the capillary bed, CO 2 undergoes several physical and biochemical reactions that allow its transformation and delivery to tissues. A small fraction (~7%) of the overall plasmatic
8 CO 2 is carried to the lungs as a dissolved gas (in solution). The majority (~70%) of CO 2 reacts with plasmatic water to form carbonic acid : CO 2 +H 2 O H 2 CO 3. This reaction, naturally occurs so slowly (1-3 minutes) in the plasma to loose any relevance. At the opposite, the Erythrocytes contain a specific catalytic enzyme, the carbonic anhydrase, that is able to increase for about 5000 times the reaction speedy. Due to carbonic anhydrase the reaction becomes so fast to reach the steady state in less than 1 second. 7 Therefore, a large fraction of CO 2 is already transformed in car The purpose of Carboxytherapy is to improve or restore microcirculation function when damaged. The final effect is that of a rehabilitation therapy for micro-circulation. The results of CO 2 administration are not only due to the improvement of local parameters of circulation and tissue perfusion but also to the instigation of a partial increase in oxygen tension as a consequence of : a hypercapniainduced rise in capillary blood flow; a drop in cutaneous oxygen consumption; or a right shift of the O 2 dissociation curve (Bohr effect). bonic acid into the red cells before to leave the capillary bed. Within another fraction of a second, carbonic acid dissociates by loosing a proton to become bicarbonate: H 2 CO 3 H + + HCO 3 -. Most of the protons (Hydrogen ions) then combine with haemoglobin in one of the main buffer systems of the red cells. Bicarbonate is rapidly carried outside the red cells with the help of a carrier protein located on the cell wall that allows rapid exchange, in opposite directions, between bicarbonate ions that are expelled and Chloride ions that are carried in ( Chloride ions exchange ). Therefore, chloride ions concentration in the red cells of venous blood is lower that in the red cells of the arterial blood. This reversible binding between CO 2 and water within the erythrocytes is the main carrier used in human body to carry 70% of CO 2 from tissues to lungs. It has been shown in experimental models that by using an inhibitor (e.g., acetazolamide) to block carbonic anhydrase activity in the red cells, the CO 2 removal is significantly lowered and levels of tissue PCO 2 can increase from 45mmHg to 80 mmhg!. Another fraction of CO 2 binds to the ammine radicals (heme sites) of haemoglobin to form carbamylhemoglobin (CO 2 Hb). This is a weak and reversible binding that allows the rapid release of CO 2 in the pulmonary alveoli where PCO 2 is lower than in the capillary bed. Finally, a small fraction of CO 2 combines with plasmatic proteins by the same bindings used with haemoglobin. However, these reactions between CO 2 and plasmatic proteins are significantly slower than that catalyzed in erythrocytes by carbonic anhydrase and can contribute for only 20% of CO 2 transportation. At the capillary level, carbonic acid produced from CO 2 dissociation decreases the ph of the blood. However, the interaction between this acid and plasmatic buffers prevents the excessive increase in blood protons level and therefore, avoids acidosis. The effects of carboxytherapy on the microcirculation
9 The effects of Carboxytherapy in instigating vasodilation are due to interactions between the released CO 2 and factors regulating tissue flow either in short or long term. It has been shown that CO 2 administration can determine: Improvement in local tissue blood flow velocity; Increase in microcirculatory vascular bed (angiogenesis). 1) The increase in tissue blood flow velocity are due to the effects of CO 2 at different levels: CO 2 interferes with the vis a tergo of the microcirculatory system by increasing the elastic retraction in arterioles/metartaerioles and indeed by inducing vasodilatation; 14 CO 2 relaxes smooth muscle fibro cells of pre-capillary sphincters allowing opening of sphincters and therefore an increase in tissue flow velocity; 10, 11 CO 2 enhances erythrocytes deformability. The contraction of smooth muscle cells within the muscular layer of vessel wall requires oxygen. Therefore, oxygen provokes contraction of the metarterioles and precapillary sphincters with a consequent vessel narrowing and a decrease in tissue blood velocity and flow. On the contrary, CO 2 administration determines relaxation of the smooth muscle cells in the metarterioles and precapillary sphincters with a consequent increase in the flow velocity and an overall improvement in the tissue perfusion. This enhanced vasomotion is the critical factor in determining the increase in local tissue perfusion. Indeed, this vasomotion represents the vis a tergo of the microcirculation that drives blood flow towards the capillary bed. 2) The effect of CO 2 as a main regulating factor inducing true and false angiogenesis has been detailed above. lungs. Severe damages of these organs (renal or respiratory failure) may cause excessive accumulation of CO 2. Furthermore, in congestive heart failure, vessel circulations markedly slow down and consequently, the amount of CO 2 removal from tissues is significantly lowered. Chronic congestive heart failure is another pathophysiologic condition causing CO 2 accumulation in which carboxytherapy is questionable. 14 Carboxytherapy should be also avoided in patients under treatment with carbonic anhydrase inhibitors (acetazolamide, diclofenamide, etc..). Indeed, the use of the inhibitor obstacles the main process by which CO 2 can be carried to be excreted trough lungs and kidneys. Therefore, an excessive increase in CO 2 levels during carboxytherapy might occur. Severe anaemia might be another contraindication. This is because the significant reduction in erythrocytes and haemoglobin levels of anaemic conditions translate into a significant deficit of two of the main physiologic systems used for CO 2 elimination: the binding with water at the level of the erythrocytes and the direct interaction with plasmatic haemoglobin. 1. Severe anaemia implies a significant decrease in red cells number, therefore a significant decline in the availability of the main carrier by which CO 2 can be usually transferred to the lungs and kidneys to be eliminated 2. Severe anaemia implies also a decrease in the haemoglobin levels and this reduces also the possibility of CO 2 binding to form carbamylhemoglobin plasmatic, the second most relevant CO 2 carrier from tissues to lungs and kidneys. Therefore, in condition of severe anaemia, CO 2 administration to perform carboxytherapy can further and dangerously increase CO 2 levels and cause severe hypercapnia and acidosis. 14 Carboxytherapy: contraindications and side effects Side effects from Carboxytherapy include minor pain, aches, ecchymoses, and local crackling or burning sensation. Major adverse events are uncommon. Indeed, it has been demonstrated in studies on gynaecologic laparoscopic surgery that even large amounts of CO 2 can be used to expand abdominal cavity (even 2-4 liters of CO 2 ) without any toxic effect. At rest, with normal ventilation (ventilation 6 l/min) the human body consumes 250 ml/min of Oxygen (transported from lungs to tissues) and exhales 200 ml/min of CO 2 (removed from tissues and excreted through pulmonary alveoli). In condition of hyperventilation, Oxygen consumption can increase up to ml /minute and CO 2 can be formed up to ml/minute. (5) During carboxytherapy an average of ml/minute CO 2 are administrated per session: the mild increase in CO 2 levels are easily and therefore promptly resolvable by a mild hyperventilation at the end of treatment without risk of hypercapnia and respiratory acidosis. 10 Nevertheless, in patients with severe respiratory insufficiency, severe renal failure or chronic congestive heart failure Carboxytherapy should be contraindicated. The main excretion of CO 2 and protons (H+) is performed by the kidneys and the
10 A decrease in plasmatic protein levels (and consequently in carbamylhemoglobin and plasmatic proteins) may be caused by chronic liver insufficiency that, indeed, constitutes another contraindication for carboxytherapy. Other contraindication is the presence of gaseous gangrene. This severe infectious disease is caused by anaerobic bacteria entered in the body through skin wounds and is characterized by extensive tissue damages, necrosis, oedema, and severe generalised deteriorated conditions. The infection from anaerobic bacteria (Welchia perfringens, Clostridium septicum, Clostridium novyi, Clostridium sporogenes, Clostridium hystoliticum) may be further enhanced by the increasing in CO 2 level that favours anaerobic environment (because of the concomitant decrease in O 2 concentration). In conclusion, in physiological status any mild hypercapnia is rapidly compensated by an increase in the pulmonary ventilation that increases CO 2 excretion. Therefore, severe hypercapnia and acidosis never occur also after an excessive CO 2 administration. In normal condition (health patients) there is no possibility to cause severe hypercapnia by carboxytherapy. Hypercapnia occurs when the lungs are unable to excrete CO 2 and therefore pco2 significantly increases at the alveoli level. When alveolar PCO 2 reaches mmhg the patient experiences severe dyspnoea. With further increase up to mmHg he becomes drowsy and lethargic (hypercapnic coma). With PCO 2 alveolar levels of mmHg the excessive CO 2 dampens respiratory bulbar center (normally small constant CO 2 levels are necessary to stimulate the centre) and can cause death. 5 gaseous baths CO 2 may be by administered as: true gas spring (carbon dioxide fumarole); carbonated water (carbon dioxide water). Gaseous baths may be generalized or partial. For generalized administration, the patient lies supine or sit down. The entire lower body of the patient is drawn in a hermetically closed plastic bag where CO 2 is insuf flated in order to create a saturated CO 2 atmosphere around the patient legs. These generalized true gas sessions are usually applied for minutes per day and repeated per days. Partial administration technique is applied in cases of localized functional or organic, arterial or lymphatic, disease: a single limb (or part of this) is drawn in the plastic bag that is then hermetically ensured around the limb and insufflated with CO 2. An example of ambulatory gas bath application is the Hydrocarboxytherapy (Figure 6). Carbonated water baths are applied with the full immersion of the patient in carbonated water at a temperature of 34. It can be used natural carbonated water or water artificially enriched with CO 2 jets. Treatment is applied for mean of about minutes per day and repeated for about consecutive days. 11 Gaseous showers are usually applied for the treatment of lower limbs dystrophic ulcers and include: Carboxytherapy: clinical indications in phlebology For all the effects on the microcirculation Carboxytherapy can be used to treat: chronic venous insufficiency (CVI); chronic veno-lymphatic insufficiency (CVLI); venous ulcers. Other indications Localized adiposities (cellulitis); psoriasis; arterial vascular pathologies (Buerger disease, diabetic ulcers, acrocyanosis, atherosclerotic ulcers); aesthetic body disease (skin laxity, skin aging); rheumatism (acute or chronic). Carboxytherapy: administration techniques Two methods for CO 2 administration are employed: percutaneous; subcutaneous injection. Percuteneous administration Includes: gaseous baths and gaseous shower. For
11 Figure 6. Hydrocarboxytherapy (ME.DI.TER). Subcutaneous injections The most common employed method to administrate Carboxytherapy is by subcutaneous injection (hypodermic injection). While CO 2 baths and showers (either gaseous or carbonated water) are applied as thermal therapeutic practice (balneotherapy), CO 2 injection can be administered exclusively in medical settings such as ambulatory practice. Since its first introduction, technology has evolved: in the first times gas bottles and syringes were used. Today, electronic programmable devices are available that allow accurate release of purified and precise CO 2 volumes. A number of filters, located inside the device, separate CO 2 from contaminates such as Clostridium sporogenes spores. Perfectly measured volumes of CO 2 gas are indeed released in a well depurated form to reach the delivery system provided with 30 G (13 mm) terminal needle.once the CO 2 supply starts, few seconds are needed to completely fill the device and to ensure a saturated CO2 atmosphere within the delivery system. Therefore, the needle is introduced into the hypodermic layer and the CO 2 injections causes subcutaneous emphysema. The needle is ensured to the skin with a bandage, while CO 2 continues to spread within the subcutaneous tissue following virtual routes until the achievement of the predefinite volume. CO 2 diffusion and velocity of hypodermic dispersion strictly depends on the laxity of subcutaneous tissues and may vary from patient to patient. Figure 7. Subcutaneous injection: Subtrochanteric site. point gas showers: CO 2 is released throw a small hole at the tip of a pipe. This technique is used for treatment of isolated small ulcers; loco-regional gas showers: CO 2 jets are provided from a multi holes spring ramp where the limb is located after being draped and closed in a plastic bag. Gas showers are applied for a mean of minutes per day in cycles of days. Dosage From few ml up to 2000 ml of CO 2 are administrated in each carboxytherapy session. Usually the medium CO 2 flow is of ml/minute. But, in the first 2-3 minutes lower flows can be used (10-20 ml/min) in order to reduce the itchiness or pain sensation that could be evocated when CO 2 starts to push the way through the subcutaneous layer. After this first phase (about 2-5 minutes) CO 2 flow can be safely increased to ml/minutes. 9 Sites of injection In condition of lower limbs severe lymphatic stasis, subcutaneous injections are applied at subtrochanteres levels: anteriorly and posteriorly, at the medium, medial and lateral thirds of the thigh (Figure 7). Needles are ensured to the skin and the CO 2 is realeased to reach the established dosage. Literature data and personal experience Recent studies have confirmed the vasomotor effects of CO 2, in addition to the absence of relevant sideeffects and toxicity. Curri et al., 1, 4 by using Doppler and Laser Doppler and Albergati and Parassoni et al. 1 by using optic video capillaroscopy (VCSO) verified the increased vasodilatation in the arterioles and metarterioles and the increased vasomotion. An increase in femoral blood flow of te lower limbs, as well as an improvement in treadmill test perimeters were observed by Hartmann and Savin who 6, 12 proposed this treatment for obliterating arteriopathies. Brandi et al. 3 found that the effect of Carboxytherapy on microcirculation was a positive tool in the physiological oxidative lipolytic process and therefore suggested this gas for the treatment of localized adiposities. Indeed local adiposities are commonly associated with alterations in blood and lymphatic drainage. They reported significant
12 variations in the maximum circumference of lower limbs, in the microcirculation studied by oxygen tension (tcpo 2 ) and Laser Doppler, and in the histological analysis of adipose and connective tissues, after this treatment. 3 Figure 8. Lymphoscintigraphy: basal radionuclide scan. Top, left: legs, anterior view. Top, right: legs by posterior view. Bottom, left: thighs ante-rior view. Bottom, right: thighs, posterior view. Figure 9. Lymphoscintigraphy: radionuclide scan after walking (30 min-utes). Top, left : legs, anterior view. Top, right: legs by posterior view. Bottom, left: thighs, anterior view. Bottom, right: thighs, posterior view. More recently, studies have focused on the effect of Carboxytherapy on lymphatic drainage. Indeed, the positive effect of Carboxytherapy in improving microcirculatory flow was found to translate into a similar benefit in increasing the lymphatic drainage. In 2006, Manzo, Villeggia and Verlaro showed by lymphoscintigraphy the improvement in local parameters of circulation and tissue perfusion caused by Carboxytherapy in patients with severe lymphatic stasis. 8 A significant decrease of lymphatic stasis and a docu-mented reestablishment of the physiological lymphatic drainage was found in the treated cases. Furthermore, there was a clinical improvement due to a significant limb volume and circumference reduction. The Authors experience is detailed here following. Figure 10. Carbomed CDT Evolution (Carboxytherapy Italian device).
13 Figure 11. Lymphoscintigraphy: radionuclide scan after 10 sessions of subcutaneous Carboxytherapy (1000 ml CO2 by side). Top, left : legs, ante-rior view. Top, right: legs by posterior view. Bottom, left: thighs anterior view. Bottom, right: thighs, posterior view. Figure 12. Lymphoscintigraphy: final radionuclide scan after walking (30 minutes) + 10 sessions of subcutaneous Carboxytherapy (1000 ml CO2 by side). Top, left : legs, anterior view. Top, right: legs by posterior view. Bottom, left: thighs, anterior view. Bottom, right: thighs, posterior view. In a two years period ( ) a total of 15 female patients affected by severe limphedema were treated by Carboxytherapy: the effects on the lymphatic flow were analysed. Before treatment, all the patients were evaluated by clinical examination, echo-color Doppler and lymphoscintigraphy. Lymphoscintigraphy was performed using computerised gamma camera with double rectangular head (GE Xeleris) by administrating 0.1 ml 99m Tc-Albumin monocolloid through the 1 st interdigital dorsal space of the foot (Figures 8, 9). For each patient 10 weekly sessions of subcutaneous Carboxytherapy using a program mable CO 2 apparatus (Carbomed CDT Evolution by Laboratory Electronics Designer, CE0051-ISO 9001 csq-csq med-iqnet; Figure 10) were applied. The total quantity of CO 2 administrated by week was of 1000ml per side. In all the patients elastic compression was also applied before treatment and maintained for all the period of the study and thereafter. After a week from the last Carboxytherapy session patients underwent a new lymphoscintigraphy examination. According with the final radionuclide scan imaging in all the patients the physiologic lymphatic flow was restored in lower limbs. This result was associated with a decrease in limb volume and lymphedema reduction. Posttreatment radionuclide results are shown in Figures 11, 12. Conclusions Due to the vasomotor effects of CO 2 and the absence of relevant major side-effects and toxicity, Carboxhytherapy has become increasingly diffused for the treatment of a variety of microcirculatory diseases. Specifically, the positive effect on lymphatic drainage in microcirculation let to use Carboxytherapy as an effective therapy for patients with lymphatic stasis. Riassunto Carbossiterapia: effetti sulla microcircolazione e suo uso nel trattamento dell edema linfatico grave. Una review Per carbossiterapia si intende l utilizzo dell anidride carbonica allo stato gassoso a scopo terapeutico. La carbossiterapia esplica i suoi effetti interferendo con i fattori che regolano a breve e a lungo termine il flusso ematico tessutale locale. La carbossiterapia esplica i suoi effetti a livello di microcircolazione: a livello delle metarteriole, delle arteriole, degli sfinteri precapillari determinando un aumento della velocità del flusso ematico tessutale locale e quindi un aumento del flus-so linfatico. Una revisione della letteratura mostra come oggi la Carbossiterapia rappresenti un campo in continua espansione per il trattamento di patologie sia flebologiche che non flebologiche. Vengono qui riportati i principi fondamentali di emodinamica, istologia e biochimica che spiegano l effetto della Carbossiterapia sul microcircolo e sul drenaggio linfatico. In particolare l effetto positivo della Carbossiterapia sull incremento del drenaggio linfatico tissutale (a livello del microcircolo) ha portato ad una sua rivalutazione nel trattamento dell edema linfatico degli arti inferiori. Parole chiave: Carbossiterapia - Microcircolo - Linfedema.
14 References 1 Albergati F, Parassoni L, Lattarulo P, Varlaro V, Curri SB. Carbossiterapia e vasomotion: comparazione tra immagini videocapillaroscopiche e referti doppler laser flow dopo somministrazione di anidride carbonica. Riv. La Medicina Estetica, anno 21, n.1, gennaio-marzo Editrice Salus Internazionale, Roma. 2 Belotti E, De Bernardi M. Utilizzazione della CO 2 termale nella PEFS. Riv. La Medicina Estetica, anno 16, n.1-2 gennaio-giugno Editrice Salus Internazionale, Roma. 3 Brandic C, D Aniello C, Grimaldi L, Bosi B, Dei I, Lattarulo P, Alessandrini C. Carbon dioxide therapy in the treatment of localized adiposities: clinical study and histopathological correlations. Aesth Plast Surg 2001;25: Curri SB, Bombardelli E. Local lipodystrophy and districtual micro-circulation: proposed etiology and therapeutic management. Cosmet Toilet 1994;109:51. 5 Guyton AC, Hall JE. Fisiologia medica, EdiSES, Napoli. 6 Hartmann BR, Bassenge E, Hartmann M. Effects of serial percutaneous application of carbon dioxide in intermittent claudication: results of a controlled trial. Angiology 1997;48:957 7 Lehninger AL. Principi di biochimica, Zanichelli Editore, Bologna. 8. Manzo G, Villeggia P, Varlaro V. La carbossiterapia utilizzata in situazioni cliniche di linfostasi a carico degli arti inferiori: valutazione degli effetti mendiante linfoscintigrafia Abstract Book- XXVII Congresso Nazionale della Società Italiana di Medicina Estetica Riv. La Medicina Estetica, anno 30, n. 1, gennaio-marzo Editrice Salus Internazionale, Roma. 9. Parassoni L, Varlaro V. la carbossiterapia: una metodica in evoluzione. Riv La Medicina Estetica, anno 21, n.1, gennaio-marzo Editrice Salus Internazionale, Roma. 10. Parassoni L, Albergati F, Varlaro V, Curri SB. La carbossiterapia in tema di meccanismi d azione. Riv. La Medicina Estetica, anni 21, n.1, gennaio-marzo Editrice Salus Internazionale, Roma. 11. Parassoni L, Lattarulo P, Albergati F, Varlaro V, Guidi F. Carbossiterapia. Da Bartoletti C.A: Medicina Estetica, Editrice Salus Internazionale, Roma. 12. Savi E, Bailliart O, Bonnin P, Bedu M, Cheynel J, Coudert J, Martine JP. Vasomotor effects f transcutaneous CO 2 stage II peripheral occlusive arterial disease. Angiology, 1995;46: Varlaro V, Parassoni L, Bartoletti CA. La carbossiterapia nella PEFS e nell adiposità localizzata. Riv. La Medicina Estetica, anno 19, n.1, gennaio-marzo Editrice Salus Internazionale, Roma. 14. Varlaro V, Bartoletti CA. La carbossiterapia. Riv. La Medicina Estetica, anno 29, n.3, luglio-settembre Editrice Salus Internazionale, Roma. Pagg
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back
 Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Functions of Blood System. Blood Cells
 Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
Functions of Blood System Transport: to and from tissue cells Nutrients to cells: amino acids, glucose, vitamins, minerals, lipids (as lipoproteins). Oxygen: by red blood corpuscles (oxyhaemoglobin - 4
3. Tunica adventitia is the outermost layer; it is composed of loosely woven connective tissue infiltrated by nerves, blood vessels and lymphatics
 Blood vessels and blood pressure I. Introduction - distribution of CO at rest II. General structure of blood vessel walls - walls are composed of three distinct layers: 1. Tunica intima is the innermost
Blood vessels and blood pressure I. Introduction - distribution of CO at rest II. General structure of blood vessel walls - walls are composed of three distinct layers: 1. Tunica intima is the innermost
Page 1. Introduction The blood vessels of the body form a closed delivery system that begins and ends at the heart.
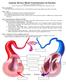 Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Anatomy Review: Blood Vessel Structure & Function Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction The blood vessels
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Blood Vessels and Circulation
 13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
13 Blood Vessels and Circulation FOCUS: Blood flows from the heart through the arterial blood vessels to capillaries, and from capillaries back to the heart through veins. The pulmonary circulation transports
Cardiovascular Physiology
 Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
12.1: The Function of Circulation page 478
 12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
12.1: The Function of Circulation page 478 Key Terms: Circulatory system, heart, blood vessel, blood, open circulatory system, closed circulatory system, pulmonary artery, pulmonary vein, aorta, atrioventricular
Milwaukee School of Engineering Gerrits@msoe.edu. Case Study: Factors that Affect Blood Pressure Instructor Version
 Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Case Study: Factors that Affect Blood Pressure Instructor Version Goal This activity (case study and its associated questions) is designed to be a student-centered learning activity relating to the factors
Human Anatomy and Physiology II Laboratory
 Human Anatomy and Physiology II Laboratory The Circulation (Two Weeks) 1 This lab involves two weeks work studying the vasculature of the human body. Both weeks involve the exercise in the lab manual entitled
Human Anatomy and Physiology II Laboratory The Circulation (Two Weeks) 1 This lab involves two weeks work studying the vasculature of the human body. Both weeks involve the exercise in the lab manual entitled
Circulatory System Review
 Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
2161-1 - Page 1. Name: 1) Choose the disease that is most closely related to the given phrase. Questions 10 and 11 refer to the following:
 Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Name: 2161-1 - Page 1 1) Choose the disease that is most closely related to the given phrase. a disease of the bone marrow characterized by uncontrolled production of white blood cells A) meningitis B)
Cerebral blood flow (CBF) is dependent on a number of factors that can broadly be divided into:
 Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. The
Cerebral Blood Flow and Intracranial Pressure Dr Lisa Hill, SpR Anaesthesia, Royal Oldham Hospital, UK. Email lambpie10@hotmail.com Dr Carl Gwinnutt, Consultant Neuroanaesthetist, Hope Hospital, UK. The
Essentials of Human Anatomy & Physiology. Chapter 15. The Urinary System. Slides 15.1 15.20. Lecture Slides in PowerPoint by Jerry L.
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 15 The Urinary System Slides 15.1 15.20 Lecture Slides in PowerPoint by Jerry L. Cook Functions of the Urinary System Elimination
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 15 The Urinary System Slides 15.1 15.20 Lecture Slides in PowerPoint by Jerry L. Cook Functions of the Urinary System Elimination
Questions on The Nervous System and Gas Exchange
 Name: Questions on The Nervous System and Gas Exchange Directions: The following questions are taken from previous IB Final Papers on Topics 6.4 (Gas Exchange) and 6.5 (Nerves, hormones and homeostasis).
Name: Questions on The Nervous System and Gas Exchange Directions: The following questions are taken from previous IB Final Papers on Topics 6.4 (Gas Exchange) and 6.5 (Nerves, hormones and homeostasis).
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
Tired, Aching Legs? Swollen Ankles? Varicose Veins? An informative guide for patients Are You at Risk? Leg problems are widespread throughout the world, but what most people don t know is that approximately
UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM
 BIOLOGY - 2201 UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM What happens to your body as you run? Breathing, heart rate, temperature, muscle pain, thirsty... Homeotasis Homeostasis is the process of maintaining
BIOLOGY - 2201 UNIT 3 : MAINTAINING DYNAMIC EQUILIBRIUM What happens to your body as you run? Breathing, heart rate, temperature, muscle pain, thirsty... Homeotasis Homeostasis is the process of maintaining
Renal Blood Flow GFR. Glomerulus Fluid Flow and Forces. Renal Blood Flow (cont d)
 GFR Glomerular filtration rate: about 120 ml /minute (180 L a day) Decreases with age (about 10 ml/min for each decade over 40) GFR = Sum of the filtration of two million glomeruli Each glomerulus probably
GFR Glomerular filtration rate: about 120 ml /minute (180 L a day) Decreases with age (about 10 ml/min for each decade over 40) GFR = Sum of the filtration of two million glomeruli Each glomerulus probably
The digestive system eliminated waste from the digestive tract. But we also need a way to eliminate waste from the rest of the body.
 Outline Urinary System Urinary System and Excretion Bio105 Lecture 20 Chapter 16 I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system 1
Outline Urinary System Urinary System and Excretion Bio105 Lecture 20 Chapter 16 I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system 1
Keystone Review Practice Test Module A Cells and Cell Processes. 1. Which characteristic is shared by all prokaryotes and eukaryotes?
 Keystone Review Practice Test Module A Cells and Cell Processes 1. Which characteristic is shared by all prokaryotes and eukaryotes? a. Ability to store hereditary information b. Use of organelles to control
Keystone Review Practice Test Module A Cells and Cell Processes 1. Which characteristic is shared by all prokaryotes and eukaryotes? a. Ability to store hereditary information b. Use of organelles to control
Provided by the American Venous Forum: veinforum.org
 CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
CHAPTER 1 NORMAL VENOUS CIRCULATION Original author: Frank Padberg Abstracted by Teresa L.Carman Introduction The circulatory system is responsible for circulating (moving) blood throughout the body. The
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Ischemia and Infarction
 Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Badizadegan Ischemia and Infarction HST.035 Spring 2003 In the US: ~50% of deaths are due to
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Paramedic Program Anatomy and Physiology Study Guide
 Paramedic Program Anatomy and Physiology Study Guide Define the terms anatomy and physiology. List and discuss in order of increasing complexity, the body from the cell to the whole organism. Define the
Paramedic Program Anatomy and Physiology Study Guide Define the terms anatomy and physiology. List and discuss in order of increasing complexity, the body from the cell to the whole organism. Define the
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Select the one that is the best answer:
 MQ Kidney 1 Select the one that is the best answer: 1) n increase in the concentration of plasma potassium causes increase in: a) release of renin b) secretion of aldosterone c) secretion of H d) release
MQ Kidney 1 Select the one that is the best answer: 1) n increase in the concentration of plasma potassium causes increase in: a) release of renin b) secretion of aldosterone c) secretion of H d) release
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY Human beings are arguably the most complex organisms on this planet. Imagine billions of microscopic parts, each with its own identity,
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY Human beings are arguably the most complex organisms on this planet. Imagine billions of microscopic parts, each with its own identity,
The Circulatory System. Chapter 17 Lesson 1
 The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
The Circulatory System Chapter 17 Lesson 1 Functions of the Circulatory System Your circulatory system maintains an internal environment in which all the cells in your body are nourished. As your heart
Circulatory System and Blood
 Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Circulatory System and Blood 1. Identify the arteries in the diagram and give one function for each. Y: Common carotid artery: sends oxygenated blood to the brain, provide nutrients. X: Subclavian artery:
Gas Exchange Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.awl.
 Gas Exchange Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.awl.com/bc) Page 1. Introduction Oxygen and carbon dioxide diffuse between
Gas Exchange Graphics are used with permission of: adam.com (http://www.adam.com/) Benjamin Cummings Publishing Co (http://www.awl.com/bc) Page 1. Introduction Oxygen and carbon dioxide diffuse between
chemicals > transported from outside to in > waste products created > they need to be removed
 1 Transport systems chemicals > transported from outside to in > waste products created > they need to be removed Simple organisms Diffusion the free movement of particles in a liquid or a gas down a concentration
1 Transport systems chemicals > transported from outside to in > waste products created > they need to be removed Simple organisms Diffusion the free movement of particles in a liquid or a gas down a concentration
BIO 137: CHAPTER 1 OBJECTIVES
 BIO 137: CHAPTER 1 OBJECTIVES 1. Define the terms anatomy and physiology, and explain their relationship using an example of a human structure with its corresponding function. A. ANATOMY = the study of
BIO 137: CHAPTER 1 OBJECTIVES 1. Define the terms anatomy and physiology, and explain their relationship using an example of a human structure with its corresponding function. A. ANATOMY = the study of
LECTURE 1 RENAL FUNCTION
 LECTURE 1 RENAL FUNCTION Components of the Urinary System 2 Kidneys 2 Ureters Bladder Urethra Refer to Renal System Vocabulary in your notes Figure 2-1,page10 Kidney Composition Cortex Outer region Contains
LECTURE 1 RENAL FUNCTION Components of the Urinary System 2 Kidneys 2 Ureters Bladder Urethra Refer to Renal System Vocabulary in your notes Figure 2-1,page10 Kidney Composition Cortex Outer region Contains
CHAPTER 9 BODY ORGANIZATION
 CHAPTER 9 BODY ORGANIZATION Objectives Identify the meaning of 10 or more terms relating to the organization of the body Describe the properties of life Describe the function for the structures of the
CHAPTER 9 BODY ORGANIZATION Objectives Identify the meaning of 10 or more terms relating to the organization of the body Describe the properties of life Describe the function for the structures of the
Heart Rate and Physical Fitness
 Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Heart Rate and Physical Fitness The circulatory system is responsible for the internal transport of many vital substances in humans, including oxygen, carbon dioxide, and nutrients. The components of the
Biology 224 Human Anatomy and Physiology II Week 8; Lecture 1; Monday Dr. Stuart S. Sumida. Excretory Physiology
 Biology 224 Human Anatomy and Physiology II Week 8; Lecture 1; Monday Dr. Stuart S. Sumida Excretory Physiology The following ELEVEN slides are review. They will not be covered in lecture, but will be
Biology 224 Human Anatomy and Physiology II Week 8; Lecture 1; Monday Dr. Stuart S. Sumida Excretory Physiology The following ELEVEN slides are review. They will not be covered in lecture, but will be
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Version 1 2015. Module guide. Preliminary document. International Master Program Cardiovascular Science University of Göttingen
 Version 1 2015 Module guide International Master Program Cardiovascular Science University of Göttingen Part 1 Theoretical modules Synopsis The Master program Cardiovascular Science contains four theoretical
Version 1 2015 Module guide International Master Program Cardiovascular Science University of Göttingen Part 1 Theoretical modules Synopsis The Master program Cardiovascular Science contains four theoretical
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Respiration occurs in the mitochondria in cells.
 B3 Question Which process occurs in the mitochondria in cells? Why do the liver and muscle cells have large number of mitochondria? What is the function of the ribosomes? Answer Respiration occurs in the
B3 Question Which process occurs in the mitochondria in cells? Why do the liver and muscle cells have large number of mitochondria? What is the function of the ribosomes? Answer Respiration occurs in the
PULMONARY PHYSIOLOGY
 I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
Chetek-Weyerhaeuser High School
 Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Introduction to Animal Systems
 Human Body Systems Introduction to Animal Systems Recurring Themes in Biology 1. Correlation between structure and function( seen at many levels) 2. Life is organized at many levels from Smallest ----
Human Body Systems Introduction to Animal Systems Recurring Themes in Biology 1. Correlation between structure and function( seen at many levels) 2. Life is organized at many levels from Smallest ----
D.U.C. Assist. Lec. Faculty of Dentistry General Physiology Ihsan Dhari. The Autonomic Nervous System
 The Autonomic Nervous System The portion of the nervous system that controls most visceral functions of the body is called the autonomic nervous system. This system helps to control arterial pressure,
The Autonomic Nervous System The portion of the nervous system that controls most visceral functions of the body is called the autonomic nervous system. This system helps to control arterial pressure,
1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood?
 1 1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood? 2 The plan shows the blood system of a mammal. What does the part labelled X represent? A heart
1 1 The diagram shows blood as seen under a microscope. Which identifies parts P, Q, R and S of the blood? 2 The plan shows the blood system of a mammal. What does the part labelled X represent? A heart
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Chapter 15. Autonomic Nervous System (ANS) and Visceral Reflexes. general properties Anatomy. Autonomic effects on target organs
 Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
Chapter 15 Autonomic Nervous System (ANS) and Visceral Reflexes general properties Anatomy Autonomic effects on target organs Central control of autonomic function 15-1 Copyright (c) The McGraw-Hill Companies,
TRANSPORT OF BLOOD GASES From The Lungs To The Tissues & Back
 TRANSPORT OF BLOOD GASES From The Lungs To The Tissues & Back Dr. Sally Osborne Department of Cellular & Physiological Sciences University of British Columbia Room 3602, D.H Copp Building 604 822-3421
TRANSPORT OF BLOOD GASES From The Lungs To The Tissues & Back Dr. Sally Osborne Department of Cellular & Physiological Sciences University of British Columbia Room 3602, D.H Copp Building 604 822-3421
Overview of the Cardiovascular System
 Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Overview of the Cardiovascular System 2 vascular (blood vessel) loops: Pulmonary circulation: from heart to lungs and back) Systemic circulation: from heart to other organs and back Flow through systemic
Norepinephrine Effects On the System
 Norepinephrine Effects On the System NE Conversion to Epinephrine in the Circulation Under stress, the increased norepinephrine produced is transmitted throughout the system. This increased level represents
Norepinephrine Effects On the System NE Conversion to Epinephrine in the Circulation Under stress, the increased norepinephrine produced is transmitted throughout the system. This increased level represents
7 Answers to end-of-chapter questions
 7 Answers to end-of-chapter questions Multiple choice questions 1 B 2 B 3 A 4 B 5 A 6 D 7 C 8 C 9 B 10 B Structured questions 11 a i Maintenance of a constant internal environment within set limits i Concentration
7 Answers to end-of-chapter questions Multiple choice questions 1 B 2 B 3 A 4 B 5 A 6 D 7 C 8 C 9 B 10 B Structured questions 11 a i Maintenance of a constant internal environment within set limits i Concentration
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
Human Anatomy & Physiology General
 Human Anatomy & Physiology General Biology is the study of life but, what exactly is life? how are living things different from nonliving things eg. a human from a rock eg. a a human from a robot eg. a
Human Anatomy & Physiology General Biology is the study of life but, what exactly is life? how are living things different from nonliving things eg. a human from a rock eg. a a human from a robot eg. a
6 Easy Steps to ABG Analysis
 6 Easy Steps to ABG Analysis E-Booklet David W. Woodruff, MSN, RN- BC, CNS, CMSRN, CEN 571 Ledge Road, Macedonia, OH 44056 Telephone (800) 990-2629 Fax (800) 990-2585 1997-2012 Ed4Nurses, Inc. All rights
6 Easy Steps to ABG Analysis E-Booklet David W. Woodruff, MSN, RN- BC, CNS, CMSRN, CEN 571 Ledge Road, Macedonia, OH 44056 Telephone (800) 990-2629 Fax (800) 990-2585 1997-2012 Ed4Nurses, Inc. All rights
Acid/Base Homeostasis (Part 4)
 Acid/Base Homeostasis (Part 4) Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) 5. The newly formed bicarbonate moves into the plasma.
Acid/Base Homeostasis (Part 4) Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) 5. The newly formed bicarbonate moves into the plasma.
CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT
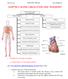 CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT BLOOD CIRCULATION AND TRANSPORT HUMAN BEING PLANTS Function of heart Wilting Structure of heart Blood vessels: characteristics and functions Transpiration: function
CHAPTER 2: BLOOD CIRCULATION AND TRANSPORT BLOOD CIRCULATION AND TRANSPORT HUMAN BEING PLANTS Function of heart Wilting Structure of heart Blood vessels: characteristics and functions Transpiration: function
Determinants of Blood Oxygen Content Instructor s Guide
 Determinants of Blood Oxygen Content Instructor s Guide Time to Complete This activity will take approximately 75 minutes, but can be shortened depending on how much time the instructor takes to review
Determinants of Blood Oxygen Content Instructor s Guide Time to Complete This activity will take approximately 75 minutes, but can be shortened depending on how much time the instructor takes to review
North Bergen School District Benchmarks
 Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Understanding Varicose Veins
 Understanding Varicose Veins Professor Bruce Campbell Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT NOTICE This book is intended not as a
Understanding Varicose Veins Professor Bruce Campbell Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT NOTICE This book is intended not as a
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Hyperbaric Oxygen Therapy WWW.RN.ORG
 Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
Chapter 1 An Introduction to Anatomy and Physiology Lecture Outline
 Chapter 1 An Introduction to Anatomy and Physiology Lecture Outline Introduction Characteristics of Living Things 1. Organization 2. Responsiveness 3. Growth & Differentiation 4. Reproduction 5. Movement
Chapter 1 An Introduction to Anatomy and Physiology Lecture Outline Introduction Characteristics of Living Things 1. Organization 2. Responsiveness 3. Growth & Differentiation 4. Reproduction 5. Movement
Blood vessels. transport blood throughout the body
 Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
Circulatory System Parts and Organs Blood vessels transport blood throughout the body Arteries blood vessels that carry blood AWAY from the heart Pulmonary arteries carry the deoxygenated blood from heart
ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM Section 1 Part B Reading Assignment: Des Jardins - Chapter 1, pp. THE LOWER AIRWAY I.
 ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM Section 1 Part B Reading Assignment: Des Jardins - Chapter 1, pp. THE LOWER AIRWAY I. Cartilaginous Airways A. Trachea 1. extends from the cricoid cartilage
ANATOMY AND PHYSIOLOGY OF THE PULMONARY SYSTEM Section 1 Part B Reading Assignment: Des Jardins - Chapter 1, pp. THE LOWER AIRWAY I. Cartilaginous Airways A. Trachea 1. extends from the cricoid cartilage
Anatomy and Physiology Warm up questions Fall 2013
 Anatomy and Physiology Warm up questions Fall 2013 QUESTION POSSIBLE ANSWERS : Chapter 1 Introduction and Regions Chapter 2 Chemistry I can name systems of the I can identify regions of the I can describe
Anatomy and Physiology Warm up questions Fall 2013 QUESTION POSSIBLE ANSWERS : Chapter 1 Introduction and Regions Chapter 2 Chemistry I can name systems of the I can identify regions of the I can describe
Chapter 16: Circulation
 Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Section 1 (The Body s Transport System) Chapter 16: Circulation 7 th Grade Cardiovascular system (the circulatory system) includes the heart, blood vessels, and blood carries needed substances to the cells
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
4 Week Body Contour / Lipo Light Program
 Natural Health Solutions 14698 Galaxie Ave. Apple Valley, MN 55124 (952) 891-22225 4 Week Body Contour / Lipo Light Program Welcome and Congratulations! This is an important decision towards improving
Natural Health Solutions 14698 Galaxie Ave. Apple Valley, MN 55124 (952) 891-22225 4 Week Body Contour / Lipo Light Program Welcome and Congratulations! This is an important decision towards improving
Acid-Base Balance and the Anion Gap
 Acid-Base Balance and the Anion Gap 1. The body strives for electrical neutrality. a. Cations = Anions b. One of the cations is very special, H +, and its concentration is monitored and regulated very
Acid-Base Balance and the Anion Gap 1. The body strives for electrical neutrality. a. Cations = Anions b. One of the cations is very special, H +, and its concentration is monitored and regulated very
UNIT TERMINAL OBJECTIVE
 UNIT TERMINAL OBJECTIVE 4-2 At the completion of this unit, the EMT-Intermediate student will be able to utilize the assessment findings to formulate a field impression and implement the treatment plan
UNIT TERMINAL OBJECTIVE 4-2 At the completion of this unit, the EMT-Intermediate student will be able to utilize the assessment findings to formulate a field impression and implement the treatment plan
Regulating the Internal Environment Water Balance & Nitrogenous Waste Removal
 Regulating the Internal Environment Water Balance & Nitrogenous Waste Removal 2006-2007 Animal systems evolved to support multicellular life CH CHO O 2 O 2 NH 3 CH CHO O 2 CO 2 NH NH 3 O 2 3 NH 3 intracellular
Regulating the Internal Environment Water Balance & Nitrogenous Waste Removal 2006-2007 Animal systems evolved to support multicellular life CH CHO O 2 O 2 NH 3 CH CHO O 2 CO 2 NH NH 3 O 2 3 NH 3 intracellular
Oxygen Dissociation Curve
 122 Visit http://www.anaesthesiamcq.com for details Chapter 4 Dissociation Curve Can you draw the oxygen dissociation curve of normal adult haemoglobin? How many points on the curve can you indicate with
122 Visit http://www.anaesthesiamcq.com for details Chapter 4 Dissociation Curve Can you draw the oxygen dissociation curve of normal adult haemoglobin? How many points on the curve can you indicate with
HUMAN ANATOMY & PHYSIOLOGY MAINTENANCE 30
 Curriculum Development In the Fairfield Public Schools FAIRFIELD PUBLIC SCHOOLS FAIRFIELD, CONNECTICUT HUMAN ANATOMY & PHYSIOLOGY MAINTENANCE 30 Board of Education Approved 05/22/2007 HUMAN ANATOMY & PHYSIOLOGY
Curriculum Development In the Fairfield Public Schools FAIRFIELD PUBLIC SCHOOLS FAIRFIELD, CONNECTICUT HUMAN ANATOMY & PHYSIOLOGY MAINTENANCE 30 Board of Education Approved 05/22/2007 HUMAN ANATOMY & PHYSIOLOGY
Fundamentals of Anatomy & Physiology Course Outline, Objectives and Accreditation Information
 201 Webster Building 3411 Silverside Road Wilmington, DE 19810 Phone: 1-888-658-6641 Fax: 1-302-477-9744 learn@corexcel.com www.corexcel.com Course Outline, Objectives and Accreditation Information Chapter
201 Webster Building 3411 Silverside Road Wilmington, DE 19810 Phone: 1-888-658-6641 Fax: 1-302-477-9744 learn@corexcel.com www.corexcel.com Course Outline, Objectives and Accreditation Information Chapter
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when
 Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Chapter 48. Nutrients in Food. Carbohydrates, Proteins, and Lipids. Carbohydrates, Proteins, and Lipids, continued
 Carbohydrates, Proteins, and Lipids The three nutrients needed by the body in the greatest amounts are carbohydrates, proteins, and lipids. Nutrients in Food All of these nutrients are called organic compounds,
Carbohydrates, Proteins, and Lipids The three nutrients needed by the body in the greatest amounts are carbohydrates, proteins, and lipids. Nutrients in Food All of these nutrients are called organic compounds,
Blood Pressure Regulation
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Acid-Base Balance and Renal Acid Excretion
 AcidBase Balance and Renal Acid Excretion Objectives By the end of this chapter, you should be able to: 1. Cite the basic principles of acidbase physiology. 2. Understand the bicarbonatecarbon dioxide
AcidBase Balance and Renal Acid Excretion Objectives By the end of this chapter, you should be able to: 1. Cite the basic principles of acidbase physiology. 2. Understand the bicarbonatecarbon dioxide
MOCK Level 3 Anatomy and Physiology for Exercise and Health
 MULTIPLE CHOICE QUESTION PAPER Paper number APEH 3.0 Please insert this reference number in the appropriate boxes on your candidate answer sheet Title Time allocation 50 minutes MOCK Level 3 Anatomy and
MULTIPLE CHOICE QUESTION PAPER Paper number APEH 3.0 Please insert this reference number in the appropriate boxes on your candidate answer sheet Title Time allocation 50 minutes MOCK Level 3 Anatomy and
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Gas Exchange. Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com)
 Gas Exchange Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Oxygen and carbon dioxide diffuse between the alveoli
Gas Exchange Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Oxygen and carbon dioxide diffuse between the alveoli
2.2.1 Pressure and flow rate along a pipe: a few fundamental concepts
 1.1 INTRODUCTION Single-cell organisms live in direct contact with the environment from where they derive nutrients and into where they dispose of their waste. For living systems containing multiple cells,
1.1 INTRODUCTION Single-cell organisms live in direct contact with the environment from where they derive nutrients and into where they dispose of their waste. For living systems containing multiple cells,
Altitude. Thermoregulation & Extreme Environments. The Stress of Altitude. Reduced PO 2. O 2 Transport Cascade. Oxygen loading at altitude:
 Altitude Thermoregulation & Extreme Environments Reduced PO 2 The Stress of Altitude O 2 Transport Cascade Progressive change in environments oxygen pressure & various body areas Oxygen loading at altitude:
Altitude Thermoregulation & Extreme Environments Reduced PO 2 The Stress of Altitude O 2 Transport Cascade Progressive change in environments oxygen pressure & various body areas Oxygen loading at altitude:
Anatomy and Physiology (ANPY) CTY Course Syllabus
 Anatomy and Physiology (ANPY) CTY Course Syllabus When Key Points / Objectives Content Day 1 INTRODUCTION HOMEOSTASIS LEVELS OF ORGANIZATION Day 2 CELLULAR AND MOLECULAR BIOLOGY GENETICS Day 3 INTEGUMENTARY
Anatomy and Physiology (ANPY) CTY Course Syllabus When Key Points / Objectives Content Day 1 INTRODUCTION HOMEOSTASIS LEVELS OF ORGANIZATION Day 2 CELLULAR AND MOLECULAR BIOLOGY GENETICS Day 3 INTEGUMENTARY
Section 7-3 Cell Boundaries
 Note: For the past several years, I ve been puzzling how to integrate new discoveries on the nature of water movement through cell membranes into Chapter 7. The Section below is a draft of my first efforts
Note: For the past several years, I ve been puzzling how to integrate new discoveries on the nature of water movement through cell membranes into Chapter 7. The Section below is a draft of my first efforts
Smooth Muscle. Learning Objectives.
 Smooth Muscle. Learning Objectives. At the end of this course, you should be able to : 1. describe the structure of smooth muscle 2. describe where smooth muscle occurs within the body 3. discuss the structural
Smooth Muscle. Learning Objectives. At the end of this course, you should be able to : 1. describe the structure of smooth muscle 2. describe where smooth muscle occurs within the body 3. discuss the structural
Cells, tissues and organs
 Chapter 8: Cells, tissues and organs Cells: building blocks of life Living things are made of cells. Many of the chemical reactions that keep organisms alive (metabolic functions) take place in cells.
Chapter 8: Cells, tissues and organs Cells: building blocks of life Living things are made of cells. Many of the chemical reactions that keep organisms alive (metabolic functions) take place in cells.
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS
 Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Inotropes/Vasoactive Agents Hina N. Patel, Pharm.D., BCPS Cathy Lawson, Pharm.D., BCPS 1. Definition -an agent that affects the contractility of the heart -may be positive (increases contractility) or
Acid/Base Homeostasis (Part 3)
 Acid/Base Homeostasis (Part 3) Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) 27. Effect of Hypoventilation Now let's look at how the
Acid/Base Homeostasis (Part 3) Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) 27. Effect of Hypoventilation Now let's look at how the
The Body s Transport System
 Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
Circulation Name Date Class The Body s Transport System This section describes how the heart, blood vessels, and blood work together to carry materials throughout the body. Use Target Reading Skills As
the Cardiovascular System
 5 Chapter Anatomy Jones and & Physiology Bartlett Learning, LLC of the Cardiovascular System OUTLINE Introduction The Heart Structures of the Heart Conduction System Functions of the Heart The Blood Vessels
5 Chapter Anatomy Jones and & Physiology Bartlett Learning, LLC of the Cardiovascular System OUTLINE Introduction The Heart Structures of the Heart Conduction System Functions of the Heart The Blood Vessels
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
