Case Study: Pancreas cancer with Whipple s operation
|
|
|
- Conrad Ferguson
- 8 years ago
- Views:
Transcription
1 Case Study: Pancreas cancer with Whipple s operation Blaauw R, (PhD Nutrition), Associate Professor, Stellenbosch University Correspondence to: Renée Blaauw, rb@sun.ac.za Keywords: pancreas cancer, Whipple procedure, SASPEN case study The following case study was discussed at the SASPEN Workshop held during the Nutrition Congress It is a reflection of the general opinion of the audience, followed by a rationale of the latest literature on the topic. Herewith follows a summarised discussion of the case. SAJCN 2015;28(2):92-96 Introduction A pancreaticoduodenectomy (PD), also known as Whipple s operation, is used for the surgical management of pancreatic head malignancies. It is characterised by removal of the pancreas head, duodenum, distal common bile duct, gallbladder and gastric antrum. 1-3 Variations from the standard procedure are sometimes made which are necessitated by the tumour location and size. The most common variation is the preservation of the pylorus and gastric antrum, known as the pylorus-preserving pancreaticoduodenectomy (PPPD). 1,2 Gastrointestinal continuity is re-established by various anastomoses to the remaining jejunum. Most commonly the remaining part of the stomach is anastomosed to the jejunum (gastrojejunostomy). The rest of the pancreas is anastomosed to the jejunum (pancreaticojejunostomy) and the bile duct to the jejunum (hepaticojejunostomy). 1,2 The nutritional management of patients post surgery is dependent on the preoperative nutritional status, disease involvement and surgical procedure, i.e. resected areas and anastomoses made. Case study A 75-year old male was admitted to hospital on 30 July 2014 with a three-week history of jaundice, pruritus, pale stools and dark urine. He had a history of alcohol abuse, a stable angina and was on medication for hypertension. The differential diagnoses of hepatitis or gallstones or cancer of the pancreas and gallbladder was made. His anthropometric values on admission were: Weight: 53 kg. Height: 170 cm. Usual body weight: 65 kg (i.e. 18% weight loss in less than six months). His biochemical values on day 1 were as follows: A low serum albumin (25 g/l). Raised total bilirubin (206 µmol/l). Raised conjugated bilirubin (173 µmol/l). Raised gamma-glutamyl transferase (1 356 u/l) Raised alkaline phosphatase (1 127 u/l). During hospitalisation (preoperatively), he was placed on a full ward diet. On average, he consumed 60% of his food, and sometimes complained of vomiting after meals. He also presented with blood glucose values ranging from mmol/l. After a computed tomography (CT) of the abdomen, the diagnosis of pancreas head carcinoma with obstructive jaundice was made. Aorta calcifications were also noted. The patient was scheduled for surgery on 17 August and kept nil per mouth from the previous evening. Owing to another medical emergency, he could not go to theatre as planned, and only underwent a PD (standard Whipple s operation) on 18 August Extensive unresectable spreading of the tumour was noted. Postoperatively, he was admitted to the intensive care unit for monitoring. He was placed on free nasogastric (NG) drainage and received sips of water. On 19 August 2014, he was prescribed a diabetic fluid diet, but owing to abdominal distention and episodes of vomiting, this was not given. An insulin sliding scale was started, and he received between 12 and 20 units of short-acting insulin daily to control his blood glucose values. Oral intake was initiated daily, but he was unable to consume more than one third of his fluid diet due to intermittent nausea and vomiting. By 23 August 2014, he was successfully tolerating his diet. It was decided to advance him to a full diabetic diet ;28(2)
2 Question 1: Could you please comment on the nutritional status of the patient on admission, and on any contributing factors? On admission, the patient had a body mass index of 18.3 kg/m 2, indicating undernutrition. Significant weight loss of 18% in less than six months also supports this diagnosis. Contributing factors to the patient s poor nutritional status could have been the presence of pancreas carcinoma, the poor dietary intake (as evidenced by the weight loss,) and a reported history of alcohol abuse. Preoperative nutritional status assessment can assist with early identification of patients with special nutritional needs. It is regarded as an important contributor to postoperative morbidity and mortality. 2,4-6 Certain components warrants special attention. Preoperative serum albumin values are highly regarded as a predictive prognostic variable postoperatively. 2,4,6 A preoperative serum albumin of < 21 g/l is associated with 29% postoperative mortality and 30-day mortality of 65%. 7 Jaundice due to tumour obstruction can indicate the extent of the damage. 2 As always, anorexia and loss of appetite can contribute to weight loss, the extent and duration of which needs to be determined. 2 Cancer cachexia is diagnosed if the weight loss is 10% in six months. 2,4 The combination of anorexia and weight loss 10% is considered a poor prognostic sign. 4 Pancreatic cancer is associated with malnutrition and cachexia. 2,4 Potential contributing mechanisms of cachexia include sustained proinflammatory cytokine response, catabolic effects of sepsis owing to increased energy expenditure, a poor dietary intake and early satiety, as well as gastrointestinal tract side-effects, e.g. vomiting, malabsorption and abdominal pain. 2,4 Upon diagnosis, the majority of patients are already metastatic and the five-year survival rate are less than 5% in the case of extensive metastasis. 1,8 Larger tumours also contribute to poor survival. Surgery or chemotherapy, or a combination thereof, are the most common treatment options for pancreas cancer. 1,3 The former can only be performed in cases of tumours that have not metastasised. Postoperative morbidity can be reduced by decreasing surgical stress, ensuring adequate pain control and early mobilisation, as well as the early introduction of nutrition. 5 Alcohol abuse is also linked to twofold increased morbidity postoperatively. Similarly, daily cigarette smoking (> 2 cigarettes per day for one year) is known to increase postoperative complications. Hence, one month s abstinence preoperatively is strongly recommended in alcohol abusers and smokers. 5 Prolonged operating time, increased preoperative bilirubin, decreased preoperative albumin, advancing age and an advanced stage of cancer, are factors that are linked to increased postoperative mortality. 1,4 Question 2: Do you agree with the preoperative fasting guidelines followed in this case? No. The patient was kept nil per os for longer than 12 hours for the initial scheduled surgery, which had to be extended by another day. This is in contrast to the literature recommendations. Traditionally, overnight fasting is implemented before any surgical procedure. This is performed to decrease gastric content and the risk of pulmonary aspiration. 5,9 However, evidence for the latter effect is slim. 9 The latest recommendations state that the consumption of solids up to six hours, and clear fluids up two hours, before anaesthesia, does not increase gastric residual volume and is recommended before elective surgery. The intake of clear, carbohydrate-rich drinks results in enhanced glucose control postoperatively. Also, the patient is less anxious and presents with less hunger and thirst, and experiences accelerated recovery and a decreased risk of wound dehiscence. 5,9-11 Preoperative carbohydrate-containing drinks should not be given to patients with diabetes mellitus until further information is obtained. However, the guidelines for solids still apply. 5,9 Question 3: Postoperatively, the patient suffered from delayed gastric emptying. Could you speculate on the contributing factors, classify the delayed gastric emptying staging and indicate your treatment strategy? The patient suffered from grade 1 delayed gastric emptying (DGE). The presence of uncontrolled blood glucose (diabetes mellitus), the consequences of Whipple s operation (antral resection) and decreased motilin release (upper small bowel resection) were contributing factors to the DGE in this case. Management include optimal glucose control, promotility drugs and medication to control the acid environment. An oral intake plus supplements should be tried as a first option to achieve optimal intake. Alternatively, enteral nutrition via the nasojejunal route using a semi-elemental or polymeric product should be investigated. The latter is only possible if a feeding tube is inserted during the operation. DGE is regarded as the most common complication post-whipple s operation. It affects from 10-60% of patients, 1,2,3,5 and is the largest contributing factor to postoperative morbidity. 1 Prominent symptoms include nausea, vomiting, bloating, early satiety and abdominal pain. 3 As a result of DGE, oral intake is delayed. This affects the overall quality of life and lengthens hospital stay. 1,2,8 It is recommended that promotility agents are prescribed to these patients. 1,2 The most common causes for the development of DGE include diabetes mellitus; decreased motilin release, owing to small bowel resection; intra-abdominal complications and infections; the use of octreotide, i.e. somatostatin analogue; and surgical techniques, i.e. injury to the vagus nerve or pylorus muscle. 1,2,8 Motilin is secreted by the duodenum and jejunum, and requires an alkaline medium for effective release. The main functions of motilin include controlling gastrointestinal motility by stimulating the gastric contractions and enhancing gastric emptying. 1,2 It is also involved in the release of somatostatin, gall bladder contraction and ;28(2)
3 Table I: The grading of delayed gastric emptying 1,2 Nasogastric tube required Unable to tolerate solid oral intake by postoperative day Grade A Grade B Grade C 4-7 days or reinserted > postoperative day days or reinserted > postoperative day 7 > 14 days or re-inserted > postoperative day Vomiting or gastric distention No/yes Yes Yes Use of nutrition support No Required for first 3 weeks postoperatively Required for more than 3 weeks the stimulation of endogenous release of the endocrine pancreas. Erythromycin and related antibiotics act as non-peptide motilin agonists, and are therefore sometimes used for their ability to stimulate gastrointestinal motility. 1 Somatostatin slows down digestion, the muscle contractions of the gastrointestinal tract, blood flow to the intestines, and hence gastric emptying. Thus, the use of octreotide, a somatostatin analogue, could contribute to the development of DGE. 1 According to a recent systematic review, the risk factors most consistently and significantly associated with DGE were postoperative complications [odds ratio (OR) of 4.71], pancreatic fistula (OR of 2.66) and preoperative diabetes (49% increased risk). 8 The grading of DGE, as recommended by the International Study Group for Pancreatic Surgery, can be seen in Table I. The diagnosis and grading take into account the duration of NG tube placements, as well as the need for tube reinsertion, the duration of insufficient oral intake and presence of gastrointestinal side-effects. It is important to always eliminate the presence of any obstruction or stenosis. 2 Treatment options include: Prokinetic agents: Examples are erythromycin (a motilin receptor agonist) 1,2 and metoclopramide 2 (stimulates smooth muscle and increases gastric emptying). The antrum still needs to be present for optimal function with metoclopramide. Proton-pump inhibitors: Proton-pump inhibitors (PPIs) decrease gastric secretions and result in a more alkaline environment. 1 Insulin therapy for optimal glucose control. 1 Question 4: Please could you comment on the need for an insulin sliding scale to control blood glucose variations? The extent of pancreatic damage due to cancer of the pancreas before surgery, linked to the partial pancreas resection, could result in diabetes mellitus owing to loss of endocrine function. Between 20% and 50% such patients develop diabetes mellitus after pancreatic resection. Blood glucose levels are raised immediately postoperatively due to stress and the use of certain medications. 2,3 This should resolve in many cases. 1,2 However, up to 80% of individuals with pancreatic cancer have diabetes mellitus preceding the diagnosis. This is probably caused by long-term destruction of the pancreatic island tissue by the tumour. 2 Treatment includes insulin therapy, preferably via constant infusion to manage blood glucose levels. Owing to reduced glucagon levels post surgery, patients are also prone to episodes of hypoglycaemia, and this should be managed by regular blood glucose monitoring. 4,5 Question 5: Would you expect this patient to suffer from malabsorption postoperatively? If yes, how would you manage it? Yes. The extent of the pancreatic damage due to the cancer of the pancreas before surgery, linked to the partial pancreas resection, could also result in malabsorption due to loss of exocrine function. Management includes a low-fat intake (the amount is determined by the patient s tolerance), small frequent meals, oral nutrition supplements to ensure optimal intake, and pancreatic enzymes replacement, i.e the amount determined by fat malabsorption. The majority (68-92%) of patients with cancer of the pancreas suffer from exocrine pancreatic insufficiency (EPI). 1,2 This may continue postoperatively. 1 A decreased secretion of bicarbonate by the ailing pancreas results in an acidic environment which denatures the available digestive enzymes. This contributes to insufficient exocrine function. 1 The consequences of EPI include diarrhoea, steatorrhoea (> 90% resected or long-standing pancreatitis), micronutrient deficiencies and weight loss. 2,6 Cancer of the pancreas is also associated with the highest levels of malnutrition. 2 A 72-hour faecal fat test (100 g fat intake) needs to be performed for a diagnosis of EPI to be made. A positive test is reported if > 7% of the total amount of fat consumed is present in the stool. 1 Treatment options include reduced dietary fat intake, individualised according to tolerance, and the use of pancreatic enzymes. 1-3 Although most pancreatic enzymes are enteric coated (except for Viokase ), it is still recommended that PPIs are also administered to neutralise the environment because an acid environment can inactivate the pancreatic enzymes. 1,2 Pancreatic enzymes can be administered via a jejunal feeding tube provided the capsule is opened and the content is mixed with water and bicarbonate. After leaving the mixture for minutes, it can be flushed down the tube or mixed with the formula. 1 The recommended dosage is units of lipase/gram fat or units per meal to a maximum of units/kg/day ;28(2)
4 Question 6: Could you please comment on the nutritional management of this patient? Oral intake should always be used initially, as was implemented in this case. This can be accompanied by oral nutritional supplements if the intake is insufficient. If the combination approach still does not meet the patient s needs, enteral tube feeding (nasojenunal) should be initiated. The main goal of nutritional management in a patient with cancer of the pancreas is to alleviate the effects of cancer cachexia. 4 An individualised approach should be followed so that any specific complications that may arise post surgery can be taken into consideration. The use of the enteral versus parenteral route has been debated extensively. As always, the principle of if the gut works, use it should be the first approach. Early postoperative enteral feeding should be aimed for, as appropriate. 4 The advantages and disadvantages of early enteral feeding are summarised in Table II. The placement of a feeding tube distal to the anastomoses areas (nasojejunal or jejunostomy tube) is ideal. 4 Cyclic feeding seems to be the recommended administration method because it results in less postoperative gastric stasis. 4 Table II: The consequences of early enteral feeding 4,12,13 Advantages Enhances the immune function Decreases infection rates Maintains gut integrity Promotes wound healing Results in less complications Is associated with decreased costs Is a quicker transition to oral intake (versus parenteral nutrition) Disadvantages Diarrhoea Abdominal cramping Excess gas production Delayed gastric emptying Dislocation or blockage of the tube Intra-abdominal leakage Small bowel necrosis The consequence of DGE owing to early enteral feeding was refuted in a recent systematic review which found no significant effect in the development of DGE between patients receiving early enteral feeding and those who did not (OR of 1.05). 8 The use of immunonutrition for 5-7 days perioperatively, 1,4,5 and seven days postoperatively, 4 should be considered because it may reduce the prevalence of infectious complications in patients undergoing major open abdominal surgery. Oral intake in the form of clear fluids can be initiated as soon as possible in such cases where the NG tube has been removed. 1 However, debate exists about the implementation of a clear fluid diet versus allowing the patient to choose which foods he or she prefers. Provided that patients are informed about the potential of impaired gut function in the early postoperative period and advised on management thereof, the latter option results in improved patient satisfaction and an earlier attainment of nutritional needs. 1,5 Oral nutrition supplements, in combination with oral food intake, are an attractive alternative to the use of enteral nutrition. 4 Ensuring that the nutritional goals are met and individualising the prescription of a given patient should remain the main priority. The routine use of parenteral nutrition (PN) as a sole source of nutrition is not recommended, and this option should only be applied when the oral and enteral routes have been unsuccessful. 4 The combination of early enteral nutrition with PN is thought to be superior to PN alone, as found in a recent study which showed decreased infectious complications, a shorter hospital stay, improved nutritional status and improved glucose control in the group receiving the combination therapy. 12 A recent systematic review assessed the outcomes of the different feeding strategies post PD. No major differences in outcome were found between the oral, enteral and parenteral feeding routes. Since the oral route was not inferior to, and in some cases resulted in better outcomes, than the enteral or parenteral route, oral feeding should be considered as the preferred route after PD. 14 Summarising the section on nutritional management According to the Enhanced Recovery after Surgery Society practice guidelines for PD, the routine use of preoperative artificial nutrition is not warranted, but significantly malnourished patients should be optimised with oral supplements or enteral nutrition preoperatively. Postoperatively, patients should be permitted a normal diet after surgery without restrictions. They should be cautioned to begin carefully and to increase intake according to tolerance over 3-4 days. Enteral tube feeding should be given only according to specific indications, and parenteral nutrition should not be employed routinely. 5 Discussion DGE, a pancreatic fistula, diabetes mellitus or glucose intolerance, malabsorption and vitamin and mineral deficiencies are the most common complications encountered post Whipple s operation. 1-3 The patient discussed in this case study suffered from three of these complications. For the sake of completeness, the other two complications will be discussed briefly. Pancreatic fistula Pancreatic fistulas develop in 12-38% of patients postoperatively. 1,2 Well-known risk factors for this complication include being of an age > 65 years, being male, a BMI > 23 kg/m 2, a short main pancreatic duct (< 3 mm), the presence of other co-morbidities, raised preoperative C-reactive protein values, malnutrition and delayed enteral feeding postoperatively. 1 The diagnosis of a fistula, as defined by the International Study Group for Pancreatic Fistulas (ISGFP) is made in the presence of an output via a drain of any fluid on or after postoperative day 3, and when the amylase content of the fluid is greater than three times the upper normal serum value. 1,2 The ISGFP has defined a grading classification for pancreatic fistulas (Table III) ;28(2)
5 Table III: The grading of pancreatic fistulas 1 Grade A Grade B Grade C Sign of infection No Yes Yes Sepsis No No Yes Evidenced by a CT scan or ultrasound No Possibly Yes Reoperation required No No Possibly Nutritional intervention None specific Possibly NPO with EN/PN CT: computed tomography, NPO: nil per os, EN: enteral nutrition, PN: parenteral nutrition Definitely NPO with EN/PN The treatment includes octreotide, a somatostatin analogue, which inhibits pancreatic secretions, 1,2 enteral access distal to the pancreas or PN in the case of a high-output fistula. The use of somatostatin analogues are not recommended as the primary treatment option by the European Society for Clinical Nutrition and Metabolism 5 since they do not produce consistent benefits on outcome. A general description of the management of fistulas was provided in a recent case study discussion. 15 Vitamin and mineral deficiencies The duodenum and proximal jejunum are important sites for the absorption of iron, folate, fatty acid, protein and trace elements. Surgical resections which result these parts of the small bowel being bypassed could result in impaired absorption of iron, calcium, zinc, copper, selenium and fat-soluble vitamins. 1-3 In addition, the occurrence of small intestine bacterial overgrowth, as a result of gastric stasis and the decreased release of gastric acid, is found in up to 40% of patients with pancreas insufficiency. Deficiency of vitamin B 12 and folate is common during the presence of small intestine bacterial overgrowth. 1,3 Conclusion Significant factors are associated with the high rate of mortality in patients with pancreatic cancer. These include the advanced stage of the disease by the time of diagnosis, the inherent aggressive biology of pancreatic adenocarcinoma and a poor nutritional status. The surgical procedure dictates the postoperative complications and management to a large extent. An individualised approach in treating complications and in selecting the most appropriate route of nutrition support is advocated. References 1. Berry AJ. Pancreatic surgery: indications, complications and implications for nutrition intervention. Nutr Clin Pract. 2013;28(3): Pappas S, McDowell N. Nutrition and pancreaticoduodenectomy. Nutr Clin Pract. 2010;25(3): Marcason W. What is the Whipple procedure and what is the appropriate nutrition therapy for it? J Acad Nutr Diet. 2015;115(1): Karagianni VT, Papalois AE, Triantafillidis JK. Nutritional status and nutritional support before and after pancreatectomy for pancreatic cancer and chronic pancreatitis. Indian J Surg Oncol. 2012;3(4): Lassen K, Coolsen MME, Slim K, et al. Guidelines for perioperative care for pancreaticoduodenectomy: Enhanced Recovery after Surgery (ERAS) Society recommendations. Clin Nutr. 2012;31(6): Sanford DE, Sanford AM, Fields RC, et al. Severe nutritional risk predicts decreased long-term survival in geriatric patients undergoing pancreaticoduodenectomy for benign disease. J Am Coll Surg. 2014;219(6): Gibbs J, Cull W, Henderson W, et al. Preoperative serum albumin level as a predictor of operative mortality and morbidity: results from the National VA Surgical Risk Study. Arch Surg. 1999;134(1): Qu H, Sun GR, Zhou SQ, et al. Clinical risk factors of delayed gastric emptying in patients after pancreaticoduodenectomy: a systematic review and meta-analysis. Eur J Surg Oncol. 2013;39(3): Brady MC, Kinn S, Stuart P, et al. Preoperative fasting for adults to prevent perioperative complications (review). [Cochrane review]. In: The Cochrane Library, Issue 4, Oxford: Update Software. 10. Gustafsson UO, Scott MJ, Schwenk W, et al. Guidelines for perioperative care in elective colonic surgery: Enhanced Recovery After Surgery (ERAS) Society recommendations. World J Surg. 2013;37(2): Nygren J, Thorell A, Ljunqgvist O. Are there any benefits from minimizing fasting and optimization of nutrition and fluid management for patients undergoing day surgery. Curr Opin Anaesthesiol. 2007;20(6): Zhu XH, Wu YD, Qiu YD, et al. Effects of early enteral combined with parenteral nutrition in patients undergoing pancreaticoduodenectomy. World J Gastroenterol. 2013;19(35): Osland E, Yunus RM, Khan S, et al. Early versus traditional postoperative feeding in patients undergoing resectional gastrointestinal surgery: a meta-analysis. JPEN Parenter Enteral Nutr. 2011;35(4): Gerritsen A, Besselink MGH, Gouma DJ et al. Systematic review of five feeding routes after pancreaticoduodenectomy. Br J Surg. 2013;100(5): Du Toit AL. Nutritional management of a complicated surgical patient by means of fistuloclysis ;27(4): ;28(2)
Oxford University Hospitals
 Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Oxford University Hospitals NHS Trust Department of Hepatobiliary and Pancreatic Surgery About Pancreatic Surgery A guide for patients and relatives Introduction This booklet has been written to provide
Liver, Gallbladder, Exocrine Pancreas KNH 406
 Liver, Gallbladder, Exocrine Pancreas KNH 406 2007 Thomson - Wadsworth LIVER Anatomy - functions With disease blood flow becomes obstructed Bile All bile drains into common hepatic duct Liver Bile complex
Liver, Gallbladder, Exocrine Pancreas KNH 406 2007 Thomson - Wadsworth LIVER Anatomy - functions With disease blood flow becomes obstructed Bile All bile drains into common hepatic duct Liver Bile complex
Diet and Pancreatic Enzyme Replacement Therapy. Anna Burton Specialist Pancreatic Dietitian Leeds Teaching Hospital NHS Trust
 Diet and Pancreatic Enzyme Replacement Therapy Anna Burton Specialist Pancreatic Dietitian Leeds Teaching Hospital NHS Trust Pancreatic cancer Symptoms which affect nutritional status Patient and carers
Diet and Pancreatic Enzyme Replacement Therapy Anna Burton Specialist Pancreatic Dietitian Leeds Teaching Hospital NHS Trust Pancreatic cancer Symptoms which affect nutritional status Patient and carers
Surgery and cancer of the pancreas
 Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
Surgery and cancer of the pancreas This information is an extract from the booklet Understanding cancer of the pancreas. You may find the full booklet helpful. We can send you a free copy see page 8. Introduction
restricted to certain centers and certain patients, preferably in some sort of experimental trial format.
 Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
Managing Pancreatic Cancer, Part 4: Pancreatic Cancer Surgery, Complications, & the Importance of Surgical Volume Dr. Matthew Katz, Surgeon, MD Anderson Cancer Center, Houston, TX I m going to talk a little
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
The Whipple Procedure. Sally Hodges, Ph.D.(c) Given the length and difficulty of the procedure, regardless of the diagnosis, certain
 The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
The Whipple Procedure Sally Hodges, Ph.D.(c) Preoperative procedures Given the length and difficulty of the procedure, regardless of the diagnosis, certain assurances must occur prior to offering a patient
Bile Duct Diseases and Problems
 Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Bile Duct Diseases and Problems Introduction A bile duct is a tube that carries bile between the liver and gallbladder and the intestine. Bile is a substance made by the liver that helps with digestion.
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders. By: Jalal Hejazi PhD, MSc.
 Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Medical Nutrition Therapy for Upper Gastrointestinal Tract Disorders By: Jalal Hejazi PhD, MSc. Digestive Disorders Common problem; more than 50 million outpatient visits per year Dietary habits and nutrition
Understanding. Pancreatic Cancer
 Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
Acute Pancreatitis. Questionnaire. if yes: amount (cigarettes/day): since when (year): Drug consumption: yes / no if yes: type of drug:. amount:.
 The physical examination has to be done AT ADMISSION! The blood for laboratory parameters has to be drawn AT ADMISSION! This form has to be filled AT ADMISSION! Questionnaire Country: 1. Patient personal
The physical examination has to be done AT ADMISSION! The blood for laboratory parameters has to be drawn AT ADMISSION! This form has to be filled AT ADMISSION! Questionnaire Country: 1. Patient personal
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
LIVER CANCER AND TUMOURS
 LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
LIVER CANCER AND TUMOURS LIVER CANCER AND TUMOURS Healthy Liver Cirrhotic Liver Tumour What causes liver cancer? Many factors may play a role in the development of cancer. Because the liver filters blood
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Bariatric Surgery. Overview of Procedural Options
 Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Cancer Treatment Centers of America Treating the Whole Patient. Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012
 Cancer Treatment Centers of America Treating the Whole Patient Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012 What is Cancer Two types of tumors Liquid tumor Leukemia Lymphoma Aplastic
Cancer Treatment Centers of America Treating the Whole Patient Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012 What is Cancer Two types of tumors Liquid tumor Leukemia Lymphoma Aplastic
What is the Sleeve Gastrectomy?
 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Chapter 6 Gastrointestinal Impairment
 Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Pancreatic Cancer Understanding your diagnosis
 Pancreatic Cancer Understanding your diagnosis Let s Make Cancer History 1 888 939-3333 cancer.ca Pancreatic Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone
Pancreatic Cancer Understanding your diagnosis Let s Make Cancer History 1 888 939-3333 cancer.ca Pancreatic Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Procedure Information Guide
 Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
Procedure Information Guide Surgery to remove the pancreas (whipple's procedure) Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made
GP Guidance: Management of nutrition following bariatric surgery
 GP Guidance: Management of nutrition following bariatric surgery Introduction Patients who are morbidly obese will have struggled with their weight for many years before going forward for bariatric surgery.
GP Guidance: Management of nutrition following bariatric surgery Introduction Patients who are morbidly obese will have struggled with their weight for many years before going forward for bariatric surgery.
Nutritional Management in Esophageal Cancer. Kurt Boeykens Nutrition Nurse Specialist
 Nutritional Management in Esophageal Cancer Kurt Boeykens Nutrition Nurse Specialist 1 Are these patients nutritionally at risk? If surgery: Major surgery Preoperative treatment Chemotherapy and radiation
Nutritional Management in Esophageal Cancer Kurt Boeykens Nutrition Nurse Specialist 1 Are these patients nutritionally at risk? If surgery: Major surgery Preoperative treatment Chemotherapy and radiation
The Whipple s procedure. Information for patients, families and carers
 The Whipple s procedure Information for patients, families and carers Contents Introduction 3 Centralisation 4 What is the pancreas? 5 What is the Whipple s operation? 6 When is it done? 8 Benefits of
The Whipple s procedure Information for patients, families and carers Contents Introduction 3 Centralisation 4 What is the pancreas? 5 What is the Whipple s operation? 6 When is it done? 8 Benefits of
Gallbladder Diseases and Problems
 Gallbladder Diseases and Problems Introduction Your gallbladder is a pear-shaped organ under your liver. It stores bile, a fluid made by your liver to digest fat. There are many diseases and problems that
Gallbladder Diseases and Problems Introduction Your gallbladder is a pear-shaped organ under your liver. It stores bile, a fluid made by your liver to digest fat. There are many diseases and problems that
SINPE trial, Ann Surg 2009. Overall morbidity. Minor Major. Infectious Non infectious. Post-hoc analysis WL < %5 (n=379) WL between 5-10% (n=49)
 Chinese International Symposium on Nutritional Oncology Changchun, June 20-21 2014 IMMUNONUTRITION IN CANCER PATIENTS IMMUNONUTRITION IN SURGERY OBJECTIVE To get the patient undergoing major surgery for
Chinese International Symposium on Nutritional Oncology Changchun, June 20-21 2014 IMMUNONUTRITION IN CANCER PATIENTS IMMUNONUTRITION IN SURGERY OBJECTIVE To get the patient undergoing major surgery for
Nutritional Challenges After Surgery
 Nutritional Challenges After Surgery L I N D A P A T A K I M S R D C S O L D C N S C M D A N D E R S O N C A N C E R C E N T E R H O U S T O N, T E X A S Objectives Identify the reasons that GIST and its
Nutritional Challenges After Surgery L I N D A P A T A K I M S R D C S O L D C N S C M D A N D E R S O N C A N C E R C E N T E R H O U S T O N, T E X A S Objectives Identify the reasons that GIST and its
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Aims of Nutritional Support in Oncology (Parenteral) Part 2
 Aims of Nutritional Support in Oncology (Parenteral) Part 2 Rachel Barrett MSc, BSc (Hons) RD Principal Haematology-Oncology Dietitian Hong Kong Hospital Authority Commissioned Training November 20 th
Aims of Nutritional Support in Oncology (Parenteral) Part 2 Rachel Barrett MSc, BSc (Hons) RD Principal Haematology-Oncology Dietitian Hong Kong Hospital Authority Commissioned Training November 20 th
Omega-3 fatty acids improve the diagnosis-related clinical outcome. Critical Care Medicine April 2006;34(4):972-9
 Omega-3 fatty acids improve the diagnosis-related clinical outcome 1 Critical Care Medicine April 2006;34(4):972-9 Volume 34(4), April 2006, pp 972-979 Heller, Axel R. MD, PhD; Rössler, Susann; Litz, Rainer
Omega-3 fatty acids improve the diagnosis-related clinical outcome 1 Critical Care Medicine April 2006;34(4):972-9 Volume 34(4), April 2006, pp 972-979 Heller, Axel R. MD, PhD; Rössler, Susann; Litz, Rainer
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Learning Objectives. Introduction to Medical Careers. Vocabulary: Chapter 16 FACTS. Functions. Organs. Digestive System Chapter 16
 Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Learning Objectives Introduction to Medical Careers Digestive System Chapter 16 Define at least 10 terms relating to the digestive Describe the four functions of the digestive Identify different structures
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Pancreatic Cancer Information for patients and their families
 Pancreatic Cancer Information for patients and their families This handout answers common questions that are often asked by our patients and families. The information in this booklet is what we talked
Pancreatic Cancer Information for patients and their families This handout answers common questions that are often asked by our patients and families. The information in this booklet is what we talked
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
TPN/ Enteral nutrition. Salsabil HADIRE Dietitian in Oncology Hematology Center of University Hospital Mohammed VI Marrakech-
 TPN/ Enteral nutrition Salsabil HADIRE Dietitian in Oncology Hematology Center of University Hospital Mohammed VI Marrakech- Work plan Part 1: Total Parenteral Nutrition (TPN) Part 2: Enteral Nutrition
TPN/ Enteral nutrition Salsabil HADIRE Dietitian in Oncology Hematology Center of University Hospital Mohammed VI Marrakech- Work plan Part 1: Total Parenteral Nutrition (TPN) Part 2: Enteral Nutrition
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Nutritional support for cancer patients
 Nutritional support for cancer patients Patients who are receiving adequate nutrition have a better prognosis, respond better to chemotherapy and can tolerate higher doses of anticancer treatments. It
Nutritional support for cancer patients Patients who are receiving adequate nutrition have a better prognosis, respond better to chemotherapy and can tolerate higher doses of anticancer treatments. It
Whipple Procedure: A guide for patients and families UHN
 Whipple Procedure: A guide for patients and families UHN Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2014 University Health Network. All rights
Whipple Procedure: A guide for patients and families UHN Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca 2014 University Health Network. All rights
Management of high output stomas (HOS) Marian Martyn Clinical Nurse Specialist
 Management of high output stomas (HOS) Marian Martyn Clinical Nurse Specialist Case History Mr C 50 year old male diagnosed with rectal cancer. He presented to GP with 5 month history of altered bowel
Management of high output stomas (HOS) Marian Martyn Clinical Nurse Specialist Case History Mr C 50 year old male diagnosed with rectal cancer. He presented to GP with 5 month history of altered bowel
Surgery for operable pancreatic cancer
 Surgery for operable pancreatic cancer This fact sheet is for people diagnosed with pancreatic cancer who will be having surgery to remove the cancer. It describes the different surgical procedures that
Surgery for operable pancreatic cancer This fact sheet is for people diagnosed with pancreatic cancer who will be having surgery to remove the cancer. It describes the different surgical procedures that
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Crohn's disease and ulcerative colitis
 Crohn's disease and ulcerative colitis Summary Crohn s disease and ulcerative colitis are collectively known as inflammatory bowel disease (IBD). Crohn s disease can appear in any part of a person s digestive
Crohn's disease and ulcerative colitis Summary Crohn s disease and ulcerative colitis are collectively known as inflammatory bowel disease (IBD). Crohn s disease can appear in any part of a person s digestive
Nutrition Assessment. Miranda Kramer, RN, MS Nurse Practitioner/Clinical Nurse Specialist
 Nutrition Assessment Miranda Kramer, RN, MS Nurse Practitioner/Clinical Nurse Specialist General Considerations Overall caloric intake is it enough, too little or too much? What s in our calories fats,
Nutrition Assessment Miranda Kramer, RN, MS Nurse Practitioner/Clinical Nurse Specialist General Considerations Overall caloric intake is it enough, too little or too much? What s in our calories fats,
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Bariatric Patients, Nutritional Intervention for
 SKILL COMPETENCY CHECKLIST Bariatric Patients, Nutritional Intervention for Link to Dietitian Practice and Skill Standard Met/Initials Prerequisite Skills Competency Areas Knowledge of how to conduct a
SKILL COMPETENCY CHECKLIST Bariatric Patients, Nutritional Intervention for Link to Dietitian Practice and Skill Standard Met/Initials Prerequisite Skills Competency Areas Knowledge of how to conduct a
Surgery for Pancreatic cancer
 Surgery for Pancreatic cancer Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Surgery for Pancreatic cancer Patient Information Booklet Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Over 50% of hospitalized patients are malnourished. Coding for Malnutrition in the Adult Patient: What the Physician Needs to Know
 Carol Rees Parrish, M.S., R.D., Series Editor Coding for Malnutrition in the Adult Patient: What the Physician Needs to Know Wendy Phillips At least half of all hospitalized patients are malnourished,
Carol Rees Parrish, M.S., R.D., Series Editor Coding for Malnutrition in the Adult Patient: What the Physician Needs to Know Wendy Phillips At least half of all hospitalized patients are malnourished,
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Surgery and other procedures to control symptoms
 Surgery and other procedures to control symptoms This fact sheet is for people diagnosed with inoperable pancreatic cancer who will be having surgery or another interventional procedure to relieve symptoms
Surgery and other procedures to control symptoms This fact sheet is for people diagnosed with inoperable pancreatic cancer who will be having surgery or another interventional procedure to relieve symptoms
THE DIGESTIVE SYSTEM
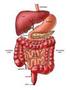 THE DIGESTIVE SYSTEM What is digestion? Digestion is the process of breaking down food so that it's small enough to be absorbed and used by the body for energy or in other bodily functions. Digestion involves
THE DIGESTIVE SYSTEM What is digestion? Digestion is the process of breaking down food so that it's small enough to be absorbed and used by the body for energy or in other bodily functions. Digestion involves
Nutritional Challenges Unique to Pancreatic Cancer
 Nutritional Challenges Unique to Pancreatic Cancer Dena McDowell, MS, RD, CD Registered Dietitian Pancreatic Cancer Program Froedtert & Medical College of Wisconsin Pancreas Endocrine Function Exocrine
Nutritional Challenges Unique to Pancreatic Cancer Dena McDowell, MS, RD, CD Registered Dietitian Pancreatic Cancer Program Froedtert & Medical College of Wisconsin Pancreas Endocrine Function Exocrine
Frequently Asked Questions: Gastric Bypass Surgery at CMC
 Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Frequently Asked Questions: Gastric Bypass Surgery at CMC Please feel free to talk with any member of the Obesity Treatment Center team at Catholic Medical Center regarding any questions, concerns or comments
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
CEU Update. Pancreatic Cancer
 CEU Update A semi-annual publication of the National Association for Health Professionals June 2015 Issue #0615 Pancreatic Cancer The Pancreatic Cancer Action Network, Inc. (PanCAN), established in 1999,
CEU Update A semi-annual publication of the National Association for Health Professionals June 2015 Issue #0615 Pancreatic Cancer The Pancreatic Cancer Action Network, Inc. (PanCAN), established in 1999,
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS
 Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
Adams Memorial Hospital Decatur, Indiana EXPLANATION OF LABORATORY TESTS Your health is important to us! The test descriptions listed below are for educational purposes only. Laboratory test interpretation
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
Nutrition Management After Bariatric Surgery
 Nutrition Management After Bariatric Surgery Federal Bureau of Prisons Clinical Practice Guidelines October 2013 Clinical guidelines are made available to the public for informational purposes only. The
Nutrition Management After Bariatric Surgery Federal Bureau of Prisons Clinical Practice Guidelines October 2013 Clinical guidelines are made available to the public for informational purposes only. The
Laboratory Monitoring of Adult Hospital Patients Receiving Parenteral Nutrition
 Laboratory Monitoring of Adult Hospital Patients Receiving Parenteral Nutrition Copy 1 Location of copies Web based only The following guideline is for use by medical staff caring for the patient and members
Laboratory Monitoring of Adult Hospital Patients Receiving Parenteral Nutrition Copy 1 Location of copies Web based only The following guideline is for use by medical staff caring for the patient and members
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES.
 PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
PATIENT INFORMATION ABOUT ADJUVANT THERAPY AFTER THE WHIPPLE OPERATION FOR ADENOCARCINOMA ( CANCER ) OF THE PANCREAS AND RELATED SITES. Radiation Oncology Sidney Kimmel Cancer Center at Johns Hopkins Last
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Applying the 2016 ASPEN/ SCCM Critical Care Guidelines to Your Practice. Susan Brantley, MS, RD, LDN
 Applying the 2016 ASPEN/ SCCM Critical Care Guidelines to Your Practice Susan Brantley, MS, RD, LDN Objectives: Upon completion of this presentation, participants should be able to: 1. Distinguish the
Applying the 2016 ASPEN/ SCCM Critical Care Guidelines to Your Practice Susan Brantley, MS, RD, LDN Objectives: Upon completion of this presentation, participants should be able to: 1. Distinguish the
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
A Patient s Guide to. Pancreatic Cysts. University of Michigan Comprehensive Cancer Center
 A Patient s Guide to Pancreatic Cysts University of Michigan Comprehensive Cancer Center Staff of the Comprehensive Cancer Center s Multidisciplinary Pancreatic Cancer Program provided information for
A Patient s Guide to Pancreatic Cysts University of Michigan Comprehensive Cancer Center Staff of the Comprehensive Cancer Center s Multidisciplinary Pancreatic Cancer Program provided information for
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Liver Function Tests. Dr Stephen Butler Paediatric Advance Trainee TDHB
 Liver Function Tests Dr Stephen Butler Paediatric Advance Trainee TDHB Introduction Case presentation What is the liver? Overview of tests used to measure liver function RJ 10 month old European girl
Liver Function Tests Dr Stephen Butler Paediatric Advance Trainee TDHB Introduction Case presentation What is the liver? Overview of tests used to measure liver function RJ 10 month old European girl
Nutr 341: Medical Nutrition Therapy: A Case Study Approach 3 rd ed. Case 32 Esophageal Cancer Treated with Surgery and Radiation
 Nutr 341: Medical Nutrition Therapy: A Case Study Approach 3 rd ed. Case 32 Esophageal Cancer Treated with Surgery and Radiation Name: Julianne Edwards Instructions: This is not a group case study; it
Nutr 341: Medical Nutrition Therapy: A Case Study Approach 3 rd ed. Case 32 Esophageal Cancer Treated with Surgery and Radiation Name: Julianne Edwards Instructions: This is not a group case study; it
Gastrointestinal problems in children with Down's syndrome
 Gastrointestinal problems in children with Down's syndrome by Dr Liz Marder This article was written for parents for the Down s Syndrome Association newsletter and is reproduced here with the permission
Gastrointestinal problems in children with Down's syndrome by Dr Liz Marder This article was written for parents for the Down s Syndrome Association newsletter and is reproduced here with the permission
Overview. Nutritional Aspects of Primary Biliary Cirrhosis. How does the liver affect nutritional status?
 Overview Nutritional Aspects of Primary Biliary Cirrhosis Tracy Burch, RD, CNSD Kovler Organ Transplant Center Northwestern Memorial Hospital Importance of nutrition therapy in PBC Incidence and pertinence
Overview Nutritional Aspects of Primary Biliary Cirrhosis Tracy Burch, RD, CNSD Kovler Organ Transplant Center Northwestern Memorial Hospital Importance of nutrition therapy in PBC Incidence and pertinence
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Dietary treatment of cachexia challenges of nutritional research in cancer patients
 Dietary treatment of cachexia challenges of nutritional research in cancer patients Trude R. Balstad 4th International Seminar of the PRC and EAPC RN, Amsterdam 2014 Outline Cancer cachexia Dietary treatment
Dietary treatment of cachexia challenges of nutritional research in cancer patients Trude R. Balstad 4th International Seminar of the PRC and EAPC RN, Amsterdam 2014 Outline Cancer cachexia Dietary treatment
Catholic Medical Center & Androscoggin Valley Hospital. Surgical Weight Loss Options For a Healthier Tomorrow
 Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
CME Test for AMDA Clinical Practice Guideline. Diabetes Mellitus
 CME Test for AMDA Clinical Practice Guideline Diabetes Mellitus Part I: 1. Which one of the following statements about type 2 diabetes is not accurate? a. Diabetics are at increased risk of experiencing
CME Test for AMDA Clinical Practice Guideline Diabetes Mellitus Part I: 1. Which one of the following statements about type 2 diabetes is not accurate? a. Diabetics are at increased risk of experiencing
NUTRITION IN LIVER DISEASES
 NUTRITION IN LIVER DISEASES 1. HEPATITIS: Definition: - Viral inflammation of liver cells. Types: a. HAV& HEV, transmitted by fecal-oral route. b. HBV & HCV, transmitted by blood and body fluids. c. HDV
NUTRITION IN LIVER DISEASES 1. HEPATITIS: Definition: - Viral inflammation of liver cells. Types: a. HAV& HEV, transmitted by fecal-oral route. b. HBV & HCV, transmitted by blood and body fluids. c. HDV
Module 9: Diseases of the Endocrine System and Nutritional Disorders Exercises
 Module 9: Diseases of the Endocrine System and Nutritional Disorders Exercises 1. An 86 year old male with brittle Type I DM is admitted for orthopedic surgery. The physician documents in the operative
Module 9: Diseases of the Endocrine System and Nutritional Disorders Exercises 1. An 86 year old male with brittle Type I DM is admitted for orthopedic surgery. The physician documents in the operative
Diabetes? Does Metabolic Surgery. Experts disagree about how surgery treats diabetes but agree more research needs to be done.
 Does Metabolic Surgery The combination of type 2 diabetes and being significantly overweight is a huge burden. Doctors tell you to lose weight, in essence, to save your life. Weight loss, in addition to
Does Metabolic Surgery The combination of type 2 diabetes and being significantly overweight is a huge burden. Doctors tell you to lose weight, in essence, to save your life. Weight loss, in addition to
7 Reasons You Can t Eat the Foods You Love!
 Dr. Susan Plank s Report: 7 Reasons You Can t Eat the Foods You Love! Betsy Coltrain sat feeling miserable on the couch. She had just finished eating dinner and began to feel the uncomfortable fullness,
Dr. Susan Plank s Report: 7 Reasons You Can t Eat the Foods You Love! Betsy Coltrain sat feeling miserable on the couch. She had just finished eating dinner and began to feel the uncomfortable fullness,
Amylase and Lipase Tests
 Amylase and Lipase Tests Also known as: Amy Formal name: Amylase Related tests: Lipase The Test The blood amylase test is ordered, often along with a lipase test, to help diagnose and monitor acute or
Amylase and Lipase Tests Also known as: Amy Formal name: Amylase Related tests: Lipase The Test The blood amylase test is ordered, often along with a lipase test, to help diagnose and monitor acute or
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Chemoembolization for Patients with Pancreatic Neuroendocrine Tumours
 Chemoembolization for Patients with Pancreatic Neuroendocrine Tumours What is this cancer? Pancreatic Endocrine Tumours are also called Pancreatic Neuroendocrine Tumours. This cancer is rare and it starts
Chemoembolization for Patients with Pancreatic Neuroendocrine Tumours What is this cancer? Pancreatic Endocrine Tumours are also called Pancreatic Neuroendocrine Tumours. This cancer is rare and it starts
Weight Loss Surgery and Bariatric Nutrition. Jeanine Giordano, MS, RD, CDN
 Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Treatment Guide Pancreatic Disease CHOOSING YOUR CARE
 Treatment Guide Pancreatic Disease The pancreas is one of the body s great multi-taskers this dual-purpose organ is also a gland. Some people may not give much thought to the pancreas, especially those
Treatment Guide Pancreatic Disease The pancreas is one of the body s great multi-taskers this dual-purpose organ is also a gland. Some people may not give much thought to the pancreas, especially those
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY. 12a. FOCUS ON Your Risk for Diabetes. Copyright 2011 Pearson Education, Inc.
 PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
PowerPoint Lecture Outlines prepared by Dr. Lana Zinger, QCC CUNY 12a FOCUS ON Your Risk for Diabetes Your Risk for Diabetes! Since 1980,Diabetes has increased by 50 %. Diabetes has increased by 70 percent
How To Treat A Diabetic Coma With Tpn
 GUIDELINES FOR TOTAL PARENTERAL NUTRITION (TPN) IN ADULT BONE MARROW TRANSPLANT PATIENTS TPN Indications TPN is indicated for any patient who is not expected to eat sufficiently for 3-5 days in severe
GUIDELINES FOR TOTAL PARENTERAL NUTRITION (TPN) IN ADULT BONE MARROW TRANSPLANT PATIENTS TPN Indications TPN is indicated for any patient who is not expected to eat sufficiently for 3-5 days in severe
European Dietitians in Oncology: The Future
 European Dietitians in Oncology: The Future Carolina Bento Clare Shaw Julia Lobenwein 1 2 Oncology Workshop Introduction to the committee Clare Shaw (United Kingdom) Carolina Bento (Portugal) Julia Lobenwein
European Dietitians in Oncology: The Future Carolina Bento Clare Shaw Julia Lobenwein 1 2 Oncology Workshop Introduction to the committee Clare Shaw (United Kingdom) Carolina Bento (Portugal) Julia Lobenwein
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
Introduction to obesity surgery
 Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 info@awls.co.nz www.aucklandweightlosssurgery.co.nz
Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 info@awls.co.nz www.aucklandweightlosssurgery.co.nz
Pancreatoduodenectomy (Whipple s Procedure)
 Pancreatoduodenectomy (Whipple s Procedure) Your doctor has arranged to surgically remove part of your pancreas or Whipple s procedure. We have written this pamphlet to help you learn about your surgery
Pancreatoduodenectomy (Whipple s Procedure) Your doctor has arranged to surgically remove part of your pancreas or Whipple s procedure. We have written this pamphlet to help you learn about your surgery
Frequently Asked Questions: Ai-Detox
 What is Ai-Detox? Frequently Asked Questions: Ai-Detox Ai-Detox is a Chinese herbal medicinal formula, produced using state of the art biotechnology, which ensures the utmost standards in quality and safety.
What is Ai-Detox? Frequently Asked Questions: Ai-Detox Ai-Detox is a Chinese herbal medicinal formula, produced using state of the art biotechnology, which ensures the utmost standards in quality and safety.
