Total Hip Replacement
|
|
|
- Noel Young
- 8 years ago
- Views:
Transcription
1 Total Hip Replacement 1. What are the surgical options for the arthritic hip? When non-operative treatments for hip pain due to arthritis fail to work, surgery may be indicated. The surgical options include hip arthroscopy, osteotomy, resurfacing and total hip replacement. a. Role of arthroscopy. Hip arthroscopy is usually an outpatient procedure to repair torn cartilage (aka the labrum) and to remove extra bone that occurs in the very earliest stages of arthritis using small stab incisions around the hip to allow for insertion of the arthroscope (tiny camera). It is rarely indicated for patients over 50 years of age. b. Role of osteotomy. Femoral and acetabular osteotomy surgery involves cutting the bone to reorient the hip joint for conditions with structural abnormalities. It is extensive surgery that requires the insertion of plates and screws to fix the bone while it heals. It requires inpatient hospitalization for several days and recovery usually takes 6-12 weeks. Osteotomy is also rarely performed beyond the age of 40. c. Role of resurfacing. Hip resurfacing is a type of hip replacement that is usually reserved for young active males. It is a metal-on-metal device where the hip ball is capped. It usually requires inpatient hospitalization for several days and recovery usually takes 6-12 weeks. This procedure has recently fallen out of favor and now has few indications. d. Role of Total Hip Replacement. Total hip replacement is the gold standard for disabling hip pain. It can be indicated in all ages, sexes, and activity levels, although generally speaking it is best to do after the age of 60 because of the risk of reoperation after 15 to 20 years due to mechanical failure. It can be performed through various approaches (front, back, side) with various implant designs. Currently the most common designs are made out of titanium with metal heads against the newest plastics. Other materials may be used for the head/ball and liner (e.g., ceramics) in selected cases. It is extensive surgery that requires inpatient hospitalization for 1-3 days, and recovery usually takes 6-8 weeks. 2. Total Hip Replacement a. When do I decide to have it done? The preliminary step in this evaluation is to meet with your surgeon to see if you are a candidate for total hip replacement. This will commonly involve a history, physical examination, and X-rays of the involved hip and pelvis. Even if the pain is significant and the X-rays show advanced arthritis of the joint, the first line of treatment is nearly always non-operative, to include weight loss if appropriate, an exercise regimen, medications, injections, or using a cane. If the symptoms persist despite these measures, then a patient would consider total hip replacement. The decision to move forward with surgery is not always straight forward, and usually involves a thoughtful conversation with yourself, your loved ones, and ultimately your surgeon. The final decision rests with the patient, and is based on the pain and disability from the arthritis influencing the patient s quality of life and activities of daily living. Patients who decide to proceed forward with surgery commonly report that the symptoms from the hip keep them from participating in activities important to them (i.e. walking, work, sleep, putting on socks and shoes, sitting for long periods of time, etc.), AND have been non-responsive to the non-operative measures. -1-
2 b. How long do they last? It is often quoted that total joint replacements last years. This is not the ideal way to interpret the longevity of total joint replacements. The more accurate way to think about longevity is via the annual failure rates. Most current data suggests that both hip and knee replacements have an annual failure rate between %. This means that if you have your total joint today, you have a 90-95% chance that your joint will last 10 years, and 80-85% that it will last 20 yrs. With improvements in technology, these numbers may improve. c. What is minimally invasive surgery, and how big is my scar? Minimally invasive surgery is a term that today describes a combination of reducing incision length and lessening tissue disruption beneath the incision. This includes cutting less muscle and detaching less tendon from bone. Combined with these techniques are the advanced techniques of anesthesia and pain management that take place around surgery. All of this combines to allow patients to feel better, have less pain, and regain function faster than in the recent past. The size of the incision is variable, and depends on several factors that include the size of the patient, the complexity of the surgery, and surgeon preference. Most studies have shown that smaller incisions offer no improvement in pain or recovery and may actually worsen the surgeons ability to adequately do the procedure. d. When will my scar disappear? The scar will heal within a few weeks, but then will remodel and change appearance over the course of 1-2 years. The color often fades and smooths over time to blend into surrounding skin, but will likely never fully disappear. There will be significant variability on the final appearance of any individual scar based on the specific surgery and patient variables. e. Do I have to have general anesthesia? No. While general anesthesia is a safe option, both hip and knee replacements can be performed under regional anesthesia. Choices for regional anesthesia include spinal anesthesia, epidural anesthesia, or one of a variety of peripheral nerve blocks. Many surgeons and anesthesiologists prefer regional anesthesia because of data showing it can reduce complications and improve the patient experience (less pain, less nausea, less narcotic medicine required, etc.). f. Is there a difference between different types of approaches? When a hip is replaced the way a surgeon gains access to the hip is referred to as an approach. There are various types of approaches named according to the direction that the surgery is performed. The most common approach today is referred to as the posterior approach and this is done from the back of the hip. Some more recent improvements to this approach (small incision and less tissue trauma) have been called mini posterior approach. Another currently popular approach is known as the anterior approach, because it is preformed from the front of the hip. The lateral approach is less popular. There are pros and cons of each approach and little science to endorse one over the other. A conversation with your surgeon should help decide which approach in the best for each patient. -2-
3 g. Are there different types of hip replacements? Most implants today have become more similar than different as surgeons and manufacturers have determined which designs work best. One variable that still remains is the bearing surface. The bearing surface is ball and liner that attach to the stem and cup that fix to the bone. The ball can be composed of either metal (cobalt chromium alloy) or ceramic, and the liner can be made of plastic (polyethylene), metal, or ceramic. The ball and liner can then be used in different combinations and are named for the respective ball liner combination (metal on poly, ceramic on poly, ceramic on ceramic, etc.). In 2013, a vast majority of bearings utilize a polyethylene liner with either a metal or ceramic head, with other combinations used with lesser frequency. Having this discussion with your surgeon is best to detail the differences. h. Is there a role for a computer, custom cutting guides, or a robot for my surgery? This question is the subject of many studies that are attempting to evaluate these emerging technologies and their influence of the success of surgeries. In general these technologies have been more popular in total knee replacement than total hip replacement. To date, there appears to be no clear advantage of these technologies, but more research is required to determine what advantage, if any, these may offer. The best approach is to discuss this topic with your surgeon. i. How long do I stay in the hospital? Most patients will stay in the hospital for 1 3 days depending on rehabilitation protocols used and how fast they progress with physical therapy. This is highly dependent upon preoperative conditioning, age, and other medical problems that may hinder a patient s ability to rehab. You should begin planning for your discharge from the hospital before your surgery. There are basically two options for you to consider and plan for your discharge from the hospital. Discharge to Home: If you go directly home from the hospital, any needed equipment and in home physical therapy will be arranged for you by the staff of the Integrated Care Management Department (ICM) of UMSJMC or your discharge planner. Discharge to Inpatient Rehab: If you go to an inpatient rehabilitation facility, those arrangements are made by the staff of the ICM Department. Factors such as your progress in physical therapy, insurance benefit coverage and bed availability determine which facility you are eligible to go to. Your transportation to the rehab facility is provided by family or designee or wheelchair van, which is a personal expense if not covered by your insurance. You are encouraged to take the opportunity now, before you surgery, to investigate and visit rehabilitation facilities. It is best to have at least 2 or 3 alternative facilities of your choice. Your discharge planner will facilitate the process while you are in the hospital. Contact your insurance to verity a benefit/coverage for inpatient rehabilitation. Your length of stay in an inpatient rehabilitation facility, should you go there, is based upon your progress in physical therapy and your insurance benefit coverage. -3-
4 j. Is THR very painful? Pain management following total hip replacement has come a long way over the last years with increased use of regional nerve blocks, spinal blocks, and various other modalities used for pain control. Early range of motion and rapid rehab protocols are also designed to reduce early stiffness and pain, making the procedure in general much less painful than in years past. However, patients handle and perceive pain differently and as such; some patients may have relatively mild pain following the procedure while others may have a more difficult time. Some form of pain medication is usually necessary for several weeks post op. Take pain medication as directed. We recommend you take pain medicine 1 hour before any physical therapy/exercise session. Always take pain medication with food in your stomach to prevent nausea. You should avoid alcohol intake if you are taking narcotics. Alcohol interacts with these medications. You may switch to Tylenol/ acetaminophen as desired. *For Pain medication refills, have your pharmacy call your surgeons office at Plan ahead for your weekend supply. Prescriptions cannot be refilled on the weekends. k. How long does it take to recover? Most hip replacement patients are able to participate in a majority of daily activities by 6 weeks. Overall by 2 months most patients have regained much the endurance and strength lost around the time of surgery and are able to participate in daily activities without restriction. l. Do I need Physical Therapy, and if so, how long? Initially most patients will receive some physical therapy while in the hospital and depending on preoperative conditioning and support, may or may not need additional therapy as an outpatient. Much of the therapy after hip replacement is walking with general stretching and thigh muscle strengthening which many patients can do on their own, without the assistance of a physical therapist. If you go directly home from the hospital, you will have in-home physical therapy about 3 times a week, for 2 weeks. It is advisable to continue physical therapy on an outpatient basis after you are discharged from in-home physical therapy. You should call the outpatient physical therapy facility soon after arriving home, to schedule your first appointment (for the third week after surgery). This is to prevent a lag in your progress. You can call Towson Sports Medicine in Towson at , in Bel Air at , or a facility of your choice that is within your insurance network to make appointment. It is your responsibility to schedule your appointments. We recommend a physical therapy facility that has a pool. Towson Sports medicine has a pool on site. While pool therapy is helpful, it is not mandatory. Your insurance company can tell you which facilities are covered under your plan. If you go to an inpatient rehab facility or transitional care unit from the hospital, you should contact the Out Patient Physical Therapy Facility as soon as you arrive home to set up appointment to continue your physical therapy. You will also be taught a series of exercises that you can perform on your own without supervision. For the first 6-12 weeks after surgery you should spend some time each day working on both flexion and extension of your hip. It is a good idea to change positions every minutes. Avoid a pillow or roll under your knee. A roll under the ankle helps improve extension, prevent a contracture, and relieve pressure on the heel. Aquatic exercising, swimming, and exercise bike are good exercise options, and can be continued indefinitely and independently. -4-
5 You are allowed to climb stairs as desired. You will lead with your non-operated leg going up stairs, and lead with your operated leg when coming down. Gradually, as muscles get stronger and your motion improves, you will be able to perform stairs normally. m. When can I walk after surgery? Utilization of progressive rehab protocols which emphasize increasing mobility and activity, aids a quicker recovery. You will be out of bed, sitting in a chair and walking beginning the day of, or the day after the surgery. You will attend physical therapy sessions two times a day starting the morning after your surgery. You will use a walker at first and, depending on your progress, and may practice walking with a cane before you are discharged. There are exercises to achieve mobility and strengthen the muscles around the hip replacement, but initially these are relatively easy. You will wean to a cane or no assistive device by 2-3 weeks postoperatively. n. When can I shower? Most surgeons do not like the wound to be exposed to water for 5-7 days. However, becoming more popular with surgeons are waterproof dressings that allow patients to shower the day after surgery. Patients then remove the dressing at 7-10 days after surgery. Once dressings are removed you still shouldn t soak the wound for 3-4 weeks until the incision is completely healed. o. When can I drive? If you had surgery on your LEFT hip, you may return to driving as you feel comfortable, if you have an automatic transmission. If surgery was on your RIGHT hip, you should not drive for 1 month, 4 weeks after surgery. However, do not allow their patients to drive until after they have been seen in the office at 4-6 weeks after surgery. Check with your surgeon for more specific direction. p. When can I return to work? Returning to work is highly dependent on the patient s general health, activity level and demands of the job. Depending on the type of job, you may resume work whenever you feel able. More demanding jobs requiring more lifting, walking, or travel may need up to 3 months for full recovery. Always discuss your plan with your surgeon to obtain the proper clearance to resume work. q. What are the major complications following THR? Total hip replacement is an excellent pain relieving procedure and most patients receive approximately 95% pain relief. Although complications are relatively rare (1-5% of patients), patients may experience a complication in the postoperative period. These include very serious and possibly life threatening complications such as heart attack, stroke, pulmonary embolism a blood clot to lungs and kidney failure. Infection is one of the most debilitating complications and often may require prolonged antibiotics with additional surgeries to rid the infection. A blood clot in the leg is also a relatively uncommon complication requiring some type of blood thinner following surgery to reduce the incidence. Another complication specific to hip replacement is dislocation of the joint (1%) that may require additional surgery if dislocation becomes recurring. Leg length differences following surgery are also a possibility and may be difficult to avoid sometimes in order to insure a stable hip. Often this leg length discrepancy is mild and rarely needs treatment. -5-
6 More Information on Blood Clot Prevention A combination of treatments is used to help prevent this complication. They include; early mobilization, compression stockings, and medication. If you do not take Coumadin/Warfarin on a permanent basis before surgery, then you should take Ecotrin, 1 tablet (regular strength, 325mg tablets coated aspirin), twice a day (1 tablet in the morning and 1 tablet in the evening) for 6 weeks after surgery. If prescribed Coumadin, Xarelto pills or Fragmin injections for blood clot prevention, you should continue this until the prescription is finished. If you are taking Coumadin/Warfarin, Fragmin or Xarelto, DO NOT take Ecotrin. Be sure to have INR time levels checked, while taking Coumadin/Warfarin. T.E.D Stockings (white elastic stockings) Put on first thing in the morning and remove 25 when going to bed in the AFTER evening. SURGERY These are important to control swelling. Wear for 6 RECOMMENDED weeks after surgery. POSITIONS AND PRECAUTIONS You should avoid alcohol intake if you are taking Coumadin/Warfarin, or Fragmin, or Xarelto as a blood thinner. Alcohol interacts with these medications. KNEE PATIENTS r. What can I do/not do after hip replacement surgery? Depending on how your surgeon performs uld spend some time each your day surgery, working you may on both have flexion slight differences and extension in your of rehabilitation your knee. It instructions is a good idea including to change s every minutes. restrictions. Avoid a pillow In general or roll most under surgeons your prefer knee. that A roll you under avoid certain the ankle positions helps improve of the hip extenevent a contracture, and increase relief pressure your risk of on dislocation the heel. of the hip for about 6 weeks following surgery. After 6 weeks the that can soft tissues involved in the surgery have healed and restrictions are often lifted allowing more PRECAUTIONS: vigorous activity. Many surgeons suggest that patients avoid any repetitive impact activities that not prop pillow under can knee increase for support. the wear on the implant such as long distance running, basketball, or mogul skiing. ce pillow under calf and Otherwise ankle to limitations elevate leg. following hip replacement surgery are few. HIP PATIENTS Hip precautions mpliance/adherence to the hip Avoid dislocation pivoting your precautions leg for six weeks that are taught and reinforced in your l therapy program is essential Sleep to proper on your healing back of or tissues operated around side only the for joint. 6 weeks Relaxation after surgery of these or as restrictions directed by is your d between 6-12 weeks after surgery surgeon or as directed by your surgeon. ECAUTIONS: Don t cross Don t sit Don t bend your legs. in low/soft over. id pivoting your leg. chairs. ep on back or on operated side only 6-12 weeks after surgery or as directed by your surgeon. s. Early Post-Operative Recovery Period (Your First 4-6 weeks) ong Term Recovery Range of Motion Don t turn your foot in. Operative Site Care: KNEE PATIENTS Staples are removed days post-op, as long as there is no discharge at the incision site. ople require 70 degrees of This flexion will be to done walk by normally a visiting on nurse level or ground, physical 90 therapist degrees if to at home ascend or stairs, by the 100 rehabilitation degrees nd stairs, and 105 degrees staff to get if in out a rehabilitation of a low chair. facility. To walk and stand efficiently, your knee should also come n 10 degrees of being fully Your straight. Total Joint Dr. Dalury Replacment encourages can be totally ROM immersed to be at 0 (for degrees bath or or swimming completely for instance) flat when raight to 120 degrees of flexion. two weeks after surgery, as long as the wound is completely healed, and staples have been removed for 3-4 days. OF MOTION AT SIX WEEKS AND ONE YEAR f motion varies and depends on many individual factors. Your potential will be determined at surgery. -6- eeks: The average is equal to 90 degrees of flexion or more. Year: The average is greater than or equal to 120 degrees of flexion. Some patients achieve less and others
7 Bruising is common after surgery. It may be quite dark in appearance. This is normal. The bruising may extend up the thigh, into the groin and buttock, or down into the ankle and foot before it is completely gone is several weeks. You may have a small area of numbness to the outside of the scar, following a hip replacement. This may last up to one year or more. The dressing will be changed prior to discharge from the hospital. It should be left on for 7-10 days. The dressing is waterproof and will protect the incision while you shower. After the 7-10 days, remove the dressing and leave the incision open to air until the staples are removed. While open to air, DO NOT, get the incision wet until 24 hours after the staples have been removed. You may notice some drainage from the incision upon discharge from the hospital as you increase your mobility/activity at home. This drainage may last hours. If drainage persists beyond this time, contact the office for further instructions. Swelling: Activity related swelling in the operative site that extends down into the same side lower leg, ankle, and foot is normal. Initially after discharge from the hospital, postoperative swelling may increase due to increased activity, mobility, and physical therapy. The more active you are, the more swelling you may note. ICE. Applying Ice to the operative site for 20 minutes per hour will help reduce swelling. It is recommended to do ice application a minimum of four times a day and as often as every hour. The swelling should recede after ice and elevation or early in the morning prior to your being active and mobile. The swelling will become more pronounced gradually throughout the day toward evening time. Postoperative swelling can take up to one year after surgery to resolve. Constipation: Constipation is common due to a number of factors, including narcotic pain medications. If taking these medications over-the-counter, non-prescription stool softeners and laxatives, including suppositories and enemas are recommended. Drinking lots of fluids, especially water and fruit juices, is also helpful. Fever: It is normal to note a low grade fever for 2 weeks after surgery. This is caused by blood in the skin and muscle layers around the surgical site. Blood is an irritant and the body s response is for a slight fever to occur. A fever or 101⁰F/35.5⁰C or more should be reported to the office for further direction. Insomnia: Insomnia is a common complaint following your hip replacement. It can last about 6 to 8 weeks. Non-prescriptive remedies such as diphenhydramine (BENADRYL) may be an effective sleep aid. If insomnia continues, prescription medication may be necessary. Depression: Depression is not an uncommon feeling after joint replacement or any major surgery. Limited mobility, discomfort, increased dependency on others, and medication side effects can be factors that contribute to this feeling. These feelings will typically fade as you begin to return to regular activities. If your feelings of depression persist, consult your family doctor. -7-
8 3. Long term total joint replacement resource information a. How long do I have to follow up? It is important to follow up with your surgeon after your joint replacement. In most cases, joint replacements last for many years. You need to meet with your treating doctor after surgery to insure that your replacement is continuing to function well. In some cases, the replaced parts can start to wear out or loosen. The frequency of required follow up visits is dependent on many factors including the age of the patient, the demand levels placed on the joint, and the type of replacement. Your physician will consider all these factors and tailor a follow-up schedule to meet your needs. In general seeing your surgeon every 1-2 years is recommended. b. Do I need to take antibiotics for certain procedures and how long? This is a controversial topic. The American Academy of Orthopedic Surgery (AAOS) and American Dental Association (ADA) have generally recommended short term antibiotics prior to dental procedures (1 dose 1 hour prior to dental procedure) for patients with joint replacements. This recommendation continued up to 2 years after the joint replacement. Beyond two years after the replacement, continued use of antibiotics prior to dental procedures has been based on the discretion of the treating surgeon and the patient based many factors including whether or not the patient was at increased risk of infection due to immune suppression (i.e., diabetic, transplant patients, and rheumatoid arthritis). The use of prophylactic antibiotics prior to dental cleanings and other invasive procedures remains controversial. Most orthopaedic surgeons now recommend lifetime suppression. Patients should discuss whether or not they need antibiotic prior to dental or other invasive procedures with their treating orthopedic surgeon. c. Will my implant set off metal detectors at airports and courthouses? Usually patients with joint replacements will set off metal detectors. It is unnecessary for patients to inform individuals performing screening for metallic objects (i.e., the Transportation Safety Administration- TSA) that they have had a joint replacement. However, patients will still require screening and will need to follow the directions of screening agents. It should be noted that there are millions of individuals with joint replacements and screening protocols recognize that patients with joint replacements may set off detectors. No specific documentation is required from patients to prove they have a joint replacement. Metal detector screenings follow universal protocols that allow for individuals with joint replacements to proceed after confirmation that no threat. -8-
Dr. Anseth s Frequently Asked Questions about Hip Replacement
 Dr. Anseth s Frequently Asked Questions about Hip Replacement What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with sciatic and lumbar plexus
Dr. Anseth s Frequently Asked Questions about Hip Replacement What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with sciatic and lumbar plexus
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Total Joint Replacement
 Total Joint Replacement Brinceton M. Phipps MD Animas Orthopedic Associates 575 Rivergate Lane, Suite 105 Durango Colorado 970-259-3020 www.brincetonphippsmd.com www.animasorthopedics.com Frequently Asked
Total Joint Replacement Brinceton M. Phipps MD Animas Orthopedic Associates 575 Rivergate Lane, Suite 105 Durango Colorado 970-259-3020 www.brincetonphippsmd.com www.animasorthopedics.com Frequently Asked
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
HIP & KNEE SURGERY PATIENTS
 HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery
 Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Dr. Anseth s Frequently Asked Questions about Knee Replacement Surgery What hospital do you use? Abbott Northwestern Hospital What type of anesthesia do you use? General anesthesia with an additional nerve
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
 Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Total Hip Replacement Hip replacement surgery, or arthroplasty, uses implants to resurface and replace the bones in the joint, re-creating the smooth gliding surfaces that were once intact. Hip replacement
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Hip Replacement Discharge Instructions
 Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
Congratulations on your new hip! You are going home after a successful total hip replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep
PALM BEACH ORTHOPAEDIC INSTITUTE, P.A. FAQ: OUT-PATIENT SURGERY
 DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
DISCLAIMER This information is a general guideline for most out-patient surgeries. Since every case is unique, your surgeon may give you further or differing instructions. Please follow his or her guidelines.
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
.org. Knee Arthroscopy. Description. Preparing for Surgery. Surgery
 Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Knee Arthroscopy Page ( 1 ) Arthroscopy is a common surgical procedure in which a joint (arthro-) is viewed (-scopy) using a small camera. Arthroscopy gives doctors a clear view of the inside of the knee.
Rehabilitation Protocol: Total Hip Arthroplasty (THA)
 Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Hip Arthroplasty (THA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Orthopaedic Surgery Center of Joint Preservation and Replacement After Total Knee Replacement Discharge Instructions
 Congratulations! You are going home after a successful total knee replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep breath and relax.
Congratulations! You are going home after a successful total knee replacement. Although there is still much work to do, we have already achieved a lot. So, when you get home, take a deep breath and relax.
Lumbar or Thoracic Fusion +/- Decompression
 Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Lumbar or Thoracic Fusion +/- Decompression PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, Naprosyn, Aleve, etc) OR ASPIRIN PRODUCTS
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Before Surgery You will likely be asked to see your family physician or an internal medicine doctor for a thorough medical evaluation.
 Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Hip Replacement - Before and After Surgery Your Hip Evaluation An orthopaedic surgeon specializes in problems affecting bones and joints. The surgeon will ask you many questions about your hip
Anterior Approach. to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Fine jewelry is rarely reactive, but cheaper watches, bracelets, rings, earrings and necklaces often contain nickel.
 BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
BEFORE SURGERY What should I do to prepare for my surgery? Arrange for a family member or friend to accompany you to the hospital on the day of your surgery. Cancel any dental appointments that fall within
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Understanding Total Hip Replacement
 Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Assistant Team Physician Denver Nuggets Western Orthopaedics Denver, Colorado Introduction This is designed
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients
 What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
What to Expect from your Hip Arthroscopy Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://dev.aana.org/portals/0/popups/animatedsurgery.htm http://www.isha.net/ http://
Total Knee Replacement
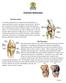 Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
Total Knee Replacement The Knee Joint A total knee replacement, also called total knee arthroplasty, is a surgery performed to remove and replace your knee joint. The knee joint, comprised of the femur
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
HIP JOINT REPLACEMENT
 HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Baker Rehab Group HomeCare Rehab and Nursing LLC
 Baker Rehab Group HomeCare Rehab and Nursing LLC Introduction So it s time for a joint replacement... Are you worried about the surgery? Are you wondering about the pre and post surgical process? Do you
Baker Rehab Group HomeCare Rehab and Nursing LLC Introduction So it s time for a joint replacement... Are you worried about the surgery? Are you wondering about the pre and post surgical process? Do you
Shoulder Dislocation or Instability Surgery: A Guide to Recovery After Surgery
 What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Total Knee Replacement
 Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Cartilage Repair Center
 Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
Cartilage Repair Center Tom Minas, MD, MS 850 Boylston Street, Suite 112 Andreas Gomoll, MD Chestnut Hill, MA 02467 Courtney VanArsdale, PA-C P: 617-732-9967 Lindsey Oneto, PA-C F: 617-732-9272 (Minas)
POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION
 www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
www.southerarizonaspine.com POSTOPERATIVE INSTRUCTION FOR ANTERIOR/POSTERIOR LUMBAR SPINE FUSION This handout will review the care you need to follow once you are home. If you have any questions or concerns,
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM
 ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM The Orthopaedic Surgery Center Welcome Thank you for choosing The Orthopaedic Surgery Center for your medical and surgical needs. It is our goal and privilege
ANTERIOR HIP REPLACEMENT WWW.ORTHOWISCONSIN.COM The Orthopaedic Surgery Center Welcome Thank you for choosing The Orthopaedic Surgery Center for your medical and surgical needs. It is our goal and privilege
Rehabilitation Protocol: Total Knee Arthroplasty (TKA)
 Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Total Knee Arthroplasty (TKA) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
ANTERIOR CERVICAL DECOMPRESSION AND FUSION
 ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
ANTERIOR CERVICAL DECOMPRESSION AND FUSION NOTE: PLEASE DO NOT TAKE ANY NON-STEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs like Advil, Celebrex, Ibuprofen, Motrin, Vioxx, etc) OR ASPIRIN PRODUCTS FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Total Shoulder Arthroplasty
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Total Shoulder Arthroplasty Ms. Ruth Delaney Consultant Orthopaedic Surgeon www.sportssurgeryclinic.com Introduction Arthritis
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program
 Patient Education: Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program Thank you for choosing Johns Hopkins for your hip replacement surgery. We use a team-based approach, and you are
Patient Education: Hip Replacement Surgery Johns Hopkins Hip and Knee Replacement Program Thank you for choosing Johns Hopkins for your hip replacement surgery. We use a team-based approach, and you are
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
KNEE ARTHROSCOPY HANDBOOK
 KNEE ARTHROSCOPY HANDBOOK 1450 Ellis Street Suite 201 Bozeman, Montana 59715 (406) 587-0122 FAX (406) 587-5548 www.bridgerorthopedic.com Your Arthroscopy Handbook Contemplating surgery of any kind leads
KNEE ARTHROSCOPY HANDBOOK 1450 Ellis Street Suite 201 Bozeman, Montana 59715 (406) 587-0122 FAX (406) 587-5548 www.bridgerorthopedic.com Your Arthroscopy Handbook Contemplating surgery of any kind leads
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
[PREPARING FOR TOTAL KNEE REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS]
![[PREPARING FOR TOTAL KNEE REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS] [PREPARING FOR TOTAL KNEE REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS]](/thumbs/26/7449249.jpg) 2012 US CENTER FOR SPORTS MEDICINE DR. COREY G. SOLMAN, JR. [PREPARING FOR TOTAL KNEE REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS] Information regarding the expectations before, during and after surgery
2012 US CENTER FOR SPORTS MEDICINE DR. COREY G. SOLMAN, JR. [PREPARING FOR TOTAL KNEE REPLACEMENT: IMPORTANT INSIGHT FOR PATIENTS] Information regarding the expectations before, during and after surgery
One REVISION TOTAL HIP REPLACEMENT. Ted W. Parcel, DO Scott Sherrill, MD
 One REVISION TOTAL HIP REPLACEMENT Ted W. Parcel, DO Scott Sherrill, MD 84484 RTHR New Cover.indd 1 10/30/13 10:53 AM CMC-Lincoln has earned the Joint Commission s Gold Seal of Approval for Disease-Specific
One REVISION TOTAL HIP REPLACEMENT Ted W. Parcel, DO Scott Sherrill, MD 84484 RTHR New Cover.indd 1 10/30/13 10:53 AM CMC-Lincoln has earned the Joint Commission s Gold Seal of Approval for Disease-Specific
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
One REVISION TOTAL KNEE REPLACEMENT. Ted W. Parcel, DO Larry Martin, MD Scott Sherrill, MD
 One REVISION TOTAL KNEE REPLACEMENT Ted W. Parcel, DO Larry Martin, MD Scott Sherrill, MD 84484 RTKR New Cover.indd 1 10/30/13 10:53 AM CMC-Lincoln has earned the Joint Commission s Gold Seal of Approval
One REVISION TOTAL KNEE REPLACEMENT Ted W. Parcel, DO Larry Martin, MD Scott Sherrill, MD 84484 RTKR New Cover.indd 1 10/30/13 10:53 AM CMC-Lincoln has earned the Joint Commission s Gold Seal of Approval
AFTER SURGERY. What can I do to decrease bruising and/or swelling?
 AFTER SURGERY What should I expect post-operatively? You will have mild bruising and swelling immediately following surgery. Bruising and swelling are normal after surgery and vary from one individual
AFTER SURGERY What should I expect post-operatively? You will have mild bruising and swelling immediately following surgery. Bruising and swelling are normal after surgery and vary from one individual
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
My Spinal Surgery: Going Home
 My Spinal Surgery: Going Home The Spinal Surgery Team has prepared this insert containing information to help prepare you and your family for going home after your spinal surgery. Please visit the UHN
My Spinal Surgery: Going Home The Spinal Surgery Team has prepared this insert containing information to help prepare you and your family for going home after your spinal surgery. Please visit the UHN
Should I have a knee replacement?
 Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
X-Plain Preparing For Surgery Reference Summary
 X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
X-Plain Preparing For Surgery Reference Summary Introduction More than 25 million surgical procedures are performed each year in the US. This reference summary will help you prepare for surgery. By understanding
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Total Hip Replacement. University Hospital Ahuja Medical Center
 Total Hip Replacement University Hospital Ahuja Medical Center Total Hip Replacement Whether you have just begun exploring treatment options or have already decided to undergo hip replacement surgery,
Total Hip Replacement University Hospital Ahuja Medical Center Total Hip Replacement Whether you have just begun exploring treatment options or have already decided to undergo hip replacement surgery,
The Total Ankle Replacement
 The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
The Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please consult your physician
Shared Decision Making
 Deciding what to do about osteoarthritis of the knee This short decision aid is to help you decide what to do about your knee osteoarthritis. You can use it on your own, or with your doctor, to help you
Deciding what to do about osteoarthritis of the knee This short decision aid is to help you decide what to do about your knee osteoarthritis. You can use it on your own, or with your doctor, to help you
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you.
 Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
Neck Surgery (Cervical spine surgery) Remember to bring this handout to the hospital with you. 1 Neck Surgery (cervical spine surgery) Table of contents Page Why do I need neck surgery?... 2 What kinds
TOTAL HIP REPLACEMENT Doug Thompson, MD
 PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. In
PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. In
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Procedure Information Guide
 Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
.org. Total Knee Replacement. Anatomy
 Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Breast Reduction Post-Operative Instructions
 Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
Total Knee Replacement
 Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
Total Knee Replacement Welcome to the Joint Replacement Center at DMOS. With over forty years of total joint experience, DMOS was the first group of surgeons in Iowa to perform the total joint procedures.
