Effectiveness of foam sclerotherapy for the treatment of varicose veins
|
|
|
- Cornelius Mitchell
- 8 years ago
- Views:
Transcription
1 Effectiveness of foam sclerotherapy for the treatment of varicose veins Vascular Medicine 15(1) The Author(s) 2009 Reprints and permission: sagepub.co.uk/journalspermission.nav DOI: / X Raha Nael and Suman Rathbun Guest Editor: Teresa Carman Abstract Varicose veins (VVs) are associated with lifestyle-limiting symptoms and complications. Patients who fail compression therapy are candidates for more invasive treatments. This study evaluates the efficacy and safety of endovenous foam sclerotherapy (EFS) for the treatment of VVs in a US academic center. We reviewed medical records of a consecutive cohort of patients who underwent EFS over a 2-year period. The primary outcome measure was obliteration of VVs. The secondary outcome measures were symptomatic improvement, ulcer healing, recurrence, and adverse events. A total of 166 patients (217 legs) underwent EFS for pain (81%), pruritis (41%), swelling (17%), ulcerations (17%), thrombophlebitis (14%), and varix rupture (3%). Complete (65%) or near-complete (34%) obliteration was achieved in 215 (99%) legs after one injection. Additional injections achieved complete obliteration in 39 of 53 legs. Ninety-three percent (27/29) of active ulcers healed or were decreasing in size. Five ulcers and 11 VVs recurred. Common adverse events included pain and hyperpigmentation. Thrombosis, hematoma, skin necrosis, and neurologic events were rare. In conclusion, EFS appears to be a safe and effective outpatient therapy for the treatment of symptomatic and complicated VVs. Keywords chronic venous insufficiency; foam sclerotherapy; varicose veins Introduction Chronic venous insufficiency (CVI) is a common and under-recognized problem, affecting greater than 20% of the general population. 1 Varicose veins (VVs), the most common manifestation of CVI, affect up to 25% of women and 15% of men. 1 Additionally, more than 80% of women and men have telangiectasias (spider veins) and reticular veins. 2 It has been estimated that 1% of the general population suffers from venous ulcerations with a United States (US) healthcare cost of three billion dollars per year. 2 The risk of developing VVs is increased in females, with advancing age, family history of venous insufficiency, pregnancy, occupations with prolonged standing, increased body mass index, vascular malformations, and prescription of hormone therapy (oral contraceptives or hormone replacement therapy). 2,3 While VVs have traditionally been regarded as simply a cosmetic problem, more commonly they produce symptoms of heaviness, fatigue, pain, swelling, restlessness, burning, and itching. 2,3 Symptoms often interfere with activities of daily living and result in lost time from work. 3 VVs are associated with a number of complications including spontaneous varix rupture with hemorrhage, superficial thrombophlebitis, deep vein thrombosis (DVT), and venous ulceration. 3 Venous ulcerations are particularly troublesome for the patients since many may take more than 9 months to heal, with 66% lasting more than 5 years. 2 In 2004, the American Venous Forum updated the standardized diagnostic evaluation and classification of patients with CVI, known as the CEAP (Clinical Etiologic Anatomic Pathophysiologic) classification. 4 This classification categorizes the clinical signs of CVI into seven classes and allows objective comparison of disease severity. Despite emphasis on the diagnostic evaluation of patients with CVI, the modern treatment of CVI and complicating VVs has not been rigorously studied. Traditional treatment modalities for VVs include conservative measures using external compression therapy and, if unsuccessful, surgical ligation and stripping of VVs and incompetent deep perforating veins. While surgical treatment of VVs Department of Internal Medicine: Cardiovascular Section, University of Oklahoma Health Sciences Center, Oklahoma City, OK, USA Presented at the Society for Vascular Medicine 18th Annual Meeting, Effectiveness of Endovenous Foam Sclerotherapy for Treatment of Varicose Veins, Baltimore, MD, June 7, Corresponding author: Suman Rathbun University of Oklahoma Health Sciences Center WP 3010, 920 Stanton L. Young Boulevard Oklahoma City, OK USA suman-rathbun@ouhsc.edu
2 28 Vascular Medicine 15(1) has proven effective, it has fallen out of favor due to high cost, time away from work, and procedural complications of wound infection, hematoma, and nerve paresis. 5 More recently, percutaneous interventional therapies including endovenous laser therapy (EVLT), radiofrequency ablation (RFA) followed by microphlebectomy, and chemical sclerotherapy using foam have become available for outpatient treatment of VVs. 3 Despite the availability of endovenous foam sclerotherapy (EFS) for the obliteration of VVs since 1944 and widespread use within the US, there is no commercial foam product available, and the use of this procedure in the US is not FDA-approved. 6 Moreover, few studies in the US have systematically evaluated the efficacy of this procedure in a large series of patients. 7 The purpose of this study is to report the efficacy and safety of EFS for the treatment of symptomatic VVs, venous ulcerations, and venous angiomata in a diverse group of patients at a US academic vascular center. Materials and methods This study reviewed the results of a consecutive cohort of patients who underwent EFS from November 2004 through June 29, 2007 at the University of Oklahoma Vascular Center. The study was approved by the local institutional review board. Patients were initially seen by one of three vascular internists who followed a standardized protocol for management of CVI and VVs, including assessment for failure of conservative management with compression therapy or recurrence of VVs after surgical or other endovenous procedures, foam preparation and delivery techniques, post-procedure observation, and follow-up surveillance. Using Duplex ultrasound examination of the deep and superficial venous systems, all major truncal branches of the venous system were examined for size and evidence of venous incompetence, including the presence of incompetent perforating veins. Patency of the deep venous system was confirmed during the ultrasound examination. Each patient chart was reviewed for demographic characteristics, indication for EFS, previous conservative and/ or surgical treatments for VVs, ultrasound testing evaluation of VVs, procedural characteristics, adverse effects, and long-term follow-up to 1 year using a standardized data collection form in accordance with the published reporting standards for endovenous ablation for the treatment of venous insufficiency. 8 Patients were categorized by severity of venous insufficiency: uncomplicated VVs (CEAP class C2-3: VVs and edema) or severe venous insufficiency (CEAP class C4-6: lipodermatosclerosis, healed ulceration, active ulceration). Patients with venous angiomas and congenital venous malformations, including patients with Klippel-Trenaunay (KT) syndrome, were analyzed in a separate category. The primary outcome measure was the frequency of obliteration (complete, partial, or minimal) of injected varicosities at 1 week post procedure, and on long-term followup. Obliteration of varicosities was characterized using Duplex ultrasound as follows: complete obliteration represented sclerosis of all visualized varicosities and/or tributaries with no evidence of residual patency, partial obliteration referred to greater than 80% sclerosis of the originally visualized VVs with minimal residual patency, and minimal obliteration described less than 80% sclerosis with persistence of the majority of the varicosities and/or its tributaries. The secondary outcome measures were frequency of improvement in venous insufficiency symptoms as reported by the patient, ulcer healing, recurrent ulcers, recurrent VVs, and adverse events following the procedure and on long-term follow-up to 1 year. Description of procedure Immediately prior to the procedure, duplex ultrasound was used to localize the most superficial, accessible segment of the great or small saphenous veins or their tributaries in which the catheter could be easily inserted. Foam was prepared combining sodium tetradecyl sulfate 3% (one part) with room air (three to four parts) using the Tessari method. 9 Foam (average volume 10 ml) was injected under ultrasound guidance with visualization of the foam into the affected vessel followed by manual compression of the saphenofemoral junction for 2 3 minutes while the foam was massaged distally into the venous tributaries to prevent microbubble entry into the deep venous system. Ultrasound examination of the venous systems was performed immediately after procedure to document the presence of foam in the superficial venous tributaries and exclude evidence of DVT. A mmhg thigh-high compression stocking and/or short-stretch bandage were applied to the treated leg. The patient was observed for minutes postprocedure for evidence of immediate adverse events. The patient returned for follow-up at 1 week for ultrasound evaluation of sclerosed VVs and to exclude DVT. Followup ultrasound at 1 week included perforator veins if a DVT was detected. Patients were then seen at weeks 12, 24, and 48 for follow-up. Patients with active ulcerations received optimal wound care with compression therapy before and after the EFS procedure. Results A total of 166 patients (217 legs) underwent EFS. The study population was divided into three categories: uncomplicated VVs (n = 127), severe CVI (n = 86), and venous angiomata (n = 4). Patient demographic information and CEAP classification are given in Table 1. Patients suffered from symptoms of pain with prolonged standing and at rest (81%), pruritis (41%), swelling (17%), recurrent or non-healing ulcerations (17%), superficial thrombophlebitis (14%), and spontaneous varix rupture (3%). Fifty-nine percent of the legs treated were indicated for uncomplicated VVs (CEAP class 2-3), 40% had complicated CVI (CEAP class 4-6), and 2% had venous angiomata. Seventy-seven percent of the patients had
3 Nael R and Rathbun S 29 Table 1. Demographic information No. of patients 166 Male 63 (38%) Female 103 (62%) Mean age (years) 56.7 (18 89) No. of legs 217 Left leg 104 (48%) Right leg 113 (52%) Symptoms Pain 175 (81%) Pruritis 89 (41%) Swelling 36 (17%) Ulcers 36 (17%) Phlebitis 30 (14%) Varix rupture 6 (3%) CEAP class C (59%) C (40%) Congenital 4 (2%) Previous treatments Conservative 167 (77%) Endovascular 10 (5%) Surgical 40 (19%) failed conservative therapy (stockings and compression hose), 5% had undergone endovascular therapy (EVLT, RFA, subfascial endoscopic perforator surgery (SEPS), and previous EFS), and 19% surgical therapy (venous stripping) prior to presenting for EFS. The majority of treated varicosities involved the great saphenous vein (94%) and its tributaries (92%). Eight percent of the treated varicosities included the small saphenous vein and its tributaries (6%). The saphenofemoral junction demonstrated incompetence in 59% of legs. Fiftyfour percent of the legs had incompetent below the knee perforating veins and 12% had incompetent above the knee perforating veins. The mean diameter of the treated varicose veins was 5.83 mm (range: 3 10 mm). Post-sclerotherapy results Patient follow-up is reported for an average of 33 weeks (range weeks; median 24 weeks). Of the 217 legs that underwent EFS, 142 (65%) achieved complete obliteration, 73 (34%) achieved near-complete obliteration, and two (0.9%) had minimal obliteration after the initial injection. The percent obliteration for uncomplicated VVs (CEAP 2 3), complicated CVI (CEAP 4 6), and congenital angiomata is given in Table 2. Thirty-nine of the 53 legs (74%) requiring re-injection (median 1.0) achieved complete obliteration. The remaining 14 legs were not re-injected since these patients had complete relief of their symptoms despite having some residual patency of their VVs. At 1 year, in the 41 legs (19%) that were seen for follow-up, 95% continued to have complete or near complete obliteration of the treated varicose veins (Figure 1A and B). Table 2. Summary of results Obliteration rate Follow-up (weeks) Total: n (%) with f/u 217 (100%) 164 (76%) 122 (56%) Complete obliteration after 1 injection 141 (65%) 109 (66%) 78 (64%) Partial obliteration 74 (34%) 53 (32%) 42 (34%) Minimal obliteration 2 (0.9%) 2 (1%) 2 (2%) Complete after re-injection CEAP 2-3: n (%) with f/u 127 (100%) 90 (71%) 68 (54%) Complete 87 (69%) 65 (72%) 49 (72%) Partial 40 (31%) 25 (28%) 19 (28%) Minimal Complete after re-injection CEAP 4-6: n (%) with f/u 86 (100%) 71 (83%) 52 (60%) Complete 52 (60%) 43 (61%) 28 (54%) Partial 32 (37%) 26 (37%) 22 (42%) Minimal 2 (2%) 2 (3%) 2 (4%) Complete after re-injection Congenital: n (%) with f/u 4 (100%) 3 (75%) 2 (50%) Complete 2 (50%) 1 (33%) 1 (50%) Partial 2 (50%) 2 (67%) 1 (50%) Minimal Complete after re-injection Symptomatic improvement, ulcer healing, recurrence Symptomatic improvement 203/217 (94%) 153/164 (93%) 111/122 (91%) Ulcers healed 23/29 (79%) 21/25 (84%) 17/19 (89%) Ulcers healing 4/29 (14%) 3/25 (12%) 1/19 (5%) Non-healing ulcers 2/29 (7%) 1/25 (4%) 1/19 (5%) Recurrent ulcers 5/29 (17%) 5/25 (20%) 5/19 (26%) Recurrent varicose veins 11/217 (5%) 11/164 (7%) 10/122 (8%)
4 30 Vascular Medicine 15(1) (A) Table 3. Adverse events (n/%) Pain 97 (45%) Hyperpigmentation 51 (23%) Thrombophlebitis 11 (5%) Trapped coagulum 8 (4%) Deep vein thrombosis 5 (2%) Neurologic 2 (0.9%) Skin necrosis 3 (1%) Hematoma 1 (0.4%) Allergic reaction 0 Chest tightness 0 n = 217. (B) incidence of serious adverse events, including hematoma, superficial thrombophlebitis or trapped coagulum, DVT, skin necrosis, and transient neurologic symptoms was low (Table 3). Two patients suffered neurologic side effects: one 62-year-old patient who received an injection of greater than 20 cc of foam when both legs were treated at a single visit as per the patient s request developed visual changes and headache that resolved within 30 minutes. A second 87-year-old patient developed transient confusion and dysarthia that resolved within 2 hours. Both patients were later discovered to have patent foramen ovale (PFO). Discussion Figure 1. (A) Before EFS; (B) 3 months post-efs. Symptomatic improvement and ulcer healing Of the 217 legs treated, 203 (94%) resulted in symptomatic improvement of the patient s initial complaints as reported by the patient at the 1-week follow-up. Twenty-three (79%) of the 29 active ulcers healed and four (14%) were decreasing in size after the procedure. The average time to ulcer healing was 14 weeks (range 1 48 weeks, median 8 weeks). Five legs (17%) developed recurrent ulcerations and 11 legs (5%) developed recurrent VVs (Table 2). Adverse events There were minimal side effects associated with EFS. Ninety-seven (45%) complained of minimal pain, 79 (81%) did not require any pain medications and 18 (19%) required over-the-counter pain medication. Fifty-one (23%) had mild skin hyperpigmentation over the sclerosed VVs. The Our results demonstrate the efficacy of EFS for obliteration of symptomatic VVs in the outpatient setting. Overall, 99% of our patients achieved complete (65%) or near complete (34%) obliteration of their VVs after the initial injection, irrespective of their CEAP classification. Symptomatic improvement was achieved in 93% of the legs injected. Twenty-three of the 29 active ulcers (79%) healed and four (14%) reduced in size at 1 48 weeks (mean 14 weeks) after treatment. Five legs (17%) developed recurrent ulcerations and 11 (5%) had recurrent VVs. These results are comparable to those achieved with surgical or other interventional endovascular procedures. 7,10 19 Our study consisted of a representative number of patients with uncomplicated VVs (59%) and severe venous insufficiency (41%) referred to a vascular outpatient clinic. We have demonstrated that the rate of complete and partial obliteration does not differ between these patients. We observed that few patients with long-term follow-up had recurrent patency of VVs after initial obliteration. There were few adverse effects associated with EFS, the most common being mild post-procedure pain and discomfort that did not require pain medications in most cases, and skin hyperpigmentation, which faded over weeks to months. More serious complications, including hematoma, DVT, superficial thrombophlebitis or trapped coagulum, skin necrosis, and transient neurologic events (headache, visual changes) rarely occurred. Limbs that developed DVT (2%) after the procedure were treated with anticoagulation for 3 months with resolution of their DVT on followup ultrasound examination. One patient with DVT had occlusion of her perforator vein. It is unclear whether this
5 Nael R and Rathbun S 31 represented foam sclerosis of the perforator vein or thrombus since the perforator vein ultimately occluded. There were no suspected cases of pulmonary embolus (PE). There are a number of limitations of our study. This study was not a randomized trial but included a consecutive cohort of patients in a closed practice who underwent EFS at the University of Oklahoma Vascular Center during a defined period of time. No treatment other than EFS for the treatment of VVs was performed during this time, limiting direct comparisons to other therapies. Microphlebectomy was not used. Although the severity of the patients symptoms was not quantified using a standardized questionnaire before or after the procedure, and the severity of symptoms and clinical improvement was determined based on the patients report, all patients were evaluated by one of three trained vascular internists who followed a standardized protocol for management of VVs, EFS procedure, and frequency of follow-up. Follow-up included Duplex ultrasound in all patients to document obliteration of treated VVs. There are a number of unique characteristics in performing EFS. The procedure requires some physician training. Ultrasound guidance is necessary for venous mapping and achieving endovenous access. The foam must be prepared immediately prior to the procedure to limit microbubble coalescence and decay. The procedure is typically performed in Trendelenburg s position to theoretically prevent microbubble entry into the deep venous system and to avoid the potential neurologic sequelae, although this advantage has never been confirmed in clinical studies. Other limitations of EFS include the need for more than one injection in some cases to achieve complete obliteration of the affected VVs and for treatment of recurrent varicosities. However, the procedure is simple with minimal discomfort without the need for anesthesia or hospital admission. Most patients who undergo EFS resume their normal daily activity within 24 hours of the procedure. While no formal analysis has been performed, it is likely to be more cost-effective than other more invasive therapies. Other studies have reported comparable success rates in patients undergoing EFS at similar follow-up intervals after the procedure. 7,10 17 In the only published US study, Bergan et al. demonstrated the efficacy of EFS for the management of CVI in 332 patients (261 uncomplicated VVs, 56 severe CVI, six venous angiomata, and nine KT syndrome), with satisfactory obliteration in all treated veins (average of 2.89 treatments/limb) and a 99% ulcer healing rate at the 6-week follow-up. 7 O Hare et al. achieved 93% obliteration in 165 patients (185 truncal veins) at 2 weeks and 74% complete and 10% partial obliteration at 6 months post-treatment with EFS. Ninety-one percent of these patients had a single treatment session. There was no significant difference in obliteration rate between those with complicated (CEAP C4-6) and uncomplicated (CEAP C1-3) VVs. 10 Myers et al. reported a primary success rate of 52.4% and a secondary success rate of 76.8% by ultrasound surveillance at 36 months in 489 patients (807 saphenous veins) treated with EFS. 11 In a systematic review of foam sclerotherapy for the treatment of VVs, Jia et al. reported an 87% occlusion rate and an 8.1% recurrence rate of the treated veins. 12 Other studies report similar results Two recent systematic reviews and meta-analyses including randomized controlled trials, prospective cohort studies and retrospective case series have evaluated the efficacy of EFS compared with other endovenous ablation and surgical stripping. 18,19 The first review evaluated 10 studies using EFS, most involving less than 100 patients all performed outside the US, and found that it was as effective as surgical stripping for the treatment of VVs, but less effective than EVLT. 18 However, this analysis reported anatomic outcomes only and did not evaluate adverse events or patient satisfaction. A second larger meta-analysis included 22 studies using EFS, with one report from the US, 7 and found complete occlusion of treated veins in 86% with 84% of patients venous ulcers healing. 19 The rate of adverse events was similarly low as with our experience. Although EFS was associated with a slightly lower complete occlusion rate compared to EVLT, it was similar or better than RFA or surgical stripping, and patients undergoing EFS had fewer adverse events, particularly DVT and paresthesia. Despite these favorable reviews, there has been some concern about the occurrence of neurological events after EFS. One recent report described two patients who experienced a transient neurological event. 20 The first was an elderly man who underwent perforator vein treatment with foam and suffered altered consciousness and arm weakness that resolved. The patient was later found to have a small intracardiac shunt. In a second patient, it was unclear whether the foam sclerotherapy procedure caused her presyncopal event since she admitted to intentional altered breathing during the procedure that resulted in her becoming dizzy and striking her head against a side table resulting in loss of consciousness. She also recovered fully after the event. Another case reported a patient who developed right upper extremity weakness, frontal headache, and sweating after injection with 20 ml of polidocanol foam (0.5%). 21 The patient s weakness improved after 10 minutes and completely resolved within 2 weeks. The patient was later found to have a PFO. Most studies report an incidence of transient neurologic events after EFS of less than 1% without long-term sequelae. 7,12 16,22 Currently, the presence of PFO is not considered a contraindication to EFS, although a restricted amount of foam is recommended in patients with symptomatic PFO. 23 Screening for PFO in patients undergoing EFS is considered unnecessary. 24 However, the lack of well-controlled studies has limited the acceptance of EFS as standard treatment for VVs despite being used widely in the US and abroad. While the use of liquid sclerosant with sodium tetradecyl sulphate (STS) has been approved by the FDA for the treatment of VVs, foam preparation and injection has not owing to a lack of randomized trials. However, it has been shown that using foam sclerosant is more effective in achieving obliteration of VVs than the injection of liquid sclerosant. 25,26 Currently, a phase III trial using a commercially prepared microfoam is underway in the US (Varisolve: ClinicalTrials.gov NCT ). If found safe and effective, FDA approval is anticipated. While these phase III studies are in progress, there is an
6 32 Vascular Medicine 15(1) urgent need for US consensus guidelines to clarify the use of EFS for the treatment of patients with VVs. In conclusion, we report the safe and effective use of EFS in a large series of patients for the treatment of symptomatic and complicated VVs in a US academic vascular center. Additional prospective, well-controlled studies are needed in the US to clarify the role of EFS for the treatment of VVs and associated complications of CVI. References 1. Callam MJ. Epidemiology of varicose veins. Br J Surg 1994; 81: Bergan JJ, Schmid-Schonbein GW, Smith PDC, Nicolaides AN, Boisseau MR, Eklof B. Mechanism of disease: chronic venous disease. N Engl J Med 2006; 355: Bartholomew JR, King T, Avisesh S, Vidimos AT. Varicose veins: newer, better treatments available. Cleve Clin J Med 2005; 72: Porter JM, Moneta GL. Reporting standards in venous disease: an update. International Consensus Committee on Chronic Venous Disease. J Vasc Surg 1995; 21: Rigby KA, Palfreyman SJ, Beverley C, Michaels JA. Surgery versus sclerotherapy for the treatment of varicose veins. Cochrane Database Syst Rev 2004; (4): CD Orbach EJ. Sclerotherapy of varicose veins: utilization of an intravenous air block. Am J Surg 1944; 66: Bergan J, Pascarella L, Mekenas L. Venous disorders: treatment with sclerosant foam. J Cardiovasc Surg 2006; 47: Kundu S, Lurie F, Millward SF, et al. Recommended reporting standards for endovenous ablation for the treatment of venous insufficiency: joint statement of The American Venous Forum and The Society of Interventional Radiology. J Vasc Interv Radiol 2007; 18: Tessari L. Nouvelle technique d obtention de la scléromousse. Phlebologie 2000; 53: O Hare JL, Parkin D, Vandenbroeck CP, Earnshaw JJ. Mid term results of ultrasound guided foam sclerotherapy for complicated and uncomplicated varicose veins. Eur J Vasc Endovasc Surg 2008; 36: Myers KA, Jolley D, Clough A, Kirwan J. Outcome of ultrasound-guided sclerotherapy for varicose veins: medium term results assessed by ultrasound surveillance. Eur J Vasc Endovasc Surg 2007; 33: Jia X, Mowatt G, Burr JM, Cassar K, Cook J, Fraser C. Systematic review of foam sclerotherapy for varicose veins. Br J Surg 2007; 94: Darke SG, Baker SJA. Ultrasound-guided foam sclerotherapy for the treatment of varicose veins. Br J Surg 2006; 93: Barrett JM, Allen B, Ockelford A, Goldman MP. Microfoam ultrasound-guided sclerotherapy of varicose veins in 100 legs. Dermatol Surg 2004; 30: Frullini A, Cavezzi A. Sclerosing foam in the treatment of varicose veins and telangiectases: history and analysis of safety and complications. Dermatol Surg 2002; 28: Cavezzi A, Frullini A, Ricci S, Tessari L. Treatment of varicose veins by foam sclerotherapy: two clinical series. Phlebology 2002; 17: Kahle B, Leng K. Efficacy of sclerotherapy in varicose veins - a prospective, blinded, placebo-controlled study. Dermatol Surg 2004; 30: Van den Bos R, Arends L, Kockaert M, Neumann M, Nijsten T. Endovenous therapies of lower extremity varicosities: a meta-analysis. J Vasc Surg 2009; 49: Luebke T, Brunkwall J. Systematic review and meta-analysis of endovenous radiofrequency obliteration, endovenous laser therapy, and foam sclerotherapy for primary varicosis. J Cardiovasc Surg 2008; 49: Bush RG, Derrick M, Manjoney D. Major neurological events following foam sclerotherapy. Phlebology 2008; 23: Forlee MV, Grouden M, Moore DJ, Shanik G. Stroke after varicose vein foam injection sclerotherapy. J Vasc Surg 2006; 43: Guex JJ, Allaert FA, Gillet JL, Chleir F. Immediate and midterm complications of sclerotherapy: report of a prospective multicenter registry of 12,173 sclerotherapy sessions. Dermatol Surg 2005; 31: Breu F, Guggenbichler S. European Consensus Meeting on Foam Sclerotherapy, April 4-6, 2003, Tegernsee, Germany. Dermatol Surg 2004; 30: ; discussion Morrison N, Cavezzi A, Bergan J, Partsch H. Regarding Stroke after varicose vein foam injection sclerotherapy [Letter]. J Vasc Surg 2006; 44: ; author reply Rabe E, Otto J, Schliephake D, Pannier F. Efficacy and safety of great saphenous vein sclerotherapy using standardized polidocanol foam (ESAF): a randomized controlled multicenter clinical trial. Eur J Vasc Endovasc Surg 2008; 35: Hamel-Desnos C, Desmos P, Wollmann JC, Ouvry P, Mako S, Allaert FA. Evaluation of the efficacy of polidocanol in the form of foam compared with liquid form in the sclerotherapy of the greater saphenous vein: initial results. Dermatol Surg 2004; 29:
MEDICAL COVERAGE POLICY. SERVICE: Varicose Veins of the Lower Extremities. PRIOR AUTHORIZATION: Required.
 Page 1 of 5 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your
Page 1 of 5 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your
Effective Date: March 2, 2016
 Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Medical Review Criteria Varicose Vein Procedures Effective Date: March 2, 2016 Treatmetn Subject: Varicose Vein Procedures VeinTreatment of Varicose Policy: Veins HPHC covers specific non-experimental
Surgical Options for Venous Disease. Sandra C Carr MD Vascular Surgery Meriter Wisconsin Heart
 Surgical Options for Venous Disease Sandra C Carr MD Vascular Surgery Meriter Wisconsin Heart Chronic Venous Disease Approximately 23% of adults in the US have varicose veins Estimated 22 million women
Surgical Options for Venous Disease Sandra C Carr MD Vascular Surgery Meriter Wisconsin Heart Chronic Venous Disease Approximately 23% of adults in the US have varicose veins Estimated 22 million women
Non-surgical treatment of severe varicose veins
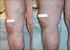 Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Microfoam Ultrasound-Guided Sclerotherapy of Varicose Veins in 100 Legs
 Microfoam Ultrasound-Guided Sclerotherapy of Varicose Veins in 1 Legs JOHN M. BARRETT, FRNZCGP, n BRUCE ALLEN, FRACR, n ANNE OCKELFORD, FRNZCGP, n AND MITCHEL P. GOLDMAN, MD w n Palm Clinic, Auckland,
Microfoam Ultrasound-Guided Sclerotherapy of Varicose Veins in 1 Legs JOHN M. BARRETT, FRNZCGP, n BRUCE ALLEN, FRACR, n ANNE OCKELFORD, FRNZCGP, n AND MITCHEL P. GOLDMAN, MD w n Palm Clinic, Auckland,
Venous Reflux Disease and Current Treatments VN20-87-A 01/06
 Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
PROVIDER POLICIES & PROCEDURES
 PROVIDER POLICIES & PROCEDURES SCLEROTHERAPY TREATMENT OF SUPERFICIAL VARICOSE VEINS OF THE LEGS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance
PROVIDER POLICIES & PROCEDURES SCLEROTHERAPY TREATMENT OF SUPERFICIAL VARICOSE VEINS OF THE LEGS The purpose of this document is to provide guidance to providers enrolled in the Connecticut Medical Assistance
Yes when meets criteria below
 Vein Disease Treatment MP9241 Covered Service: Prior Authorization Required: Additional Information: Medicare Policy: BadgerCare Plus Policy: Yes when meets criteria below Yes None Dean Health Plan covers
Vein Disease Treatment MP9241 Covered Service: Prior Authorization Required: Additional Information: Medicare Policy: BadgerCare Plus Policy: Yes when meets criteria below Yes None Dean Health Plan covers
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Origination Date: June 1, 1993 Review Date: July 20, 2016 Next Review: July, 2018 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins of the
Varicose Vein Treatment Origination Date: June 1, 1993 Review Date: July 20, 2016 Next Review: July, 2018 Medicare C/D Medical Coverage Policy DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins of the
Spotlight Series: Interventional Radiology. Varicose Veins and Venous Insufficiency
 Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Spotlight Series: Interventional Radiology Varicose Veins and Venous Insufficiency What is venous insufficiency? Spectrum of Disease Spider veins and telangiectasias Small reddish and purple veins near
Clinical Medical Policy Varicose Vein Treatment
 Benefit Coverage Covered Benefit for lines of business including: Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Benefit Coverage Covered Benefit for lines of business including: Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
MEDICAL COVERAGE POLICY SERVICE: Varicose Veins of the Lower Extremities. SERVICE: Treatment of Varicose Veins of the Lower Extremities
 Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your particular benefit plan. Each benefit
Important note Even though this policy may indicate that a particular service or supply may be considered covered, this conclusion is not based upon the terms of your particular benefit plan. Each benefit
CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE
 Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
Introduction CHAPTER 15 SCLEROTHERAPY FOR VENOUS DISEASE Original authors: Niren Angle, John J. Bergan, Joshua I. Greenberg, and J. Leonel Villavicencio Abstracted by Teresa L. Carman New technology has
Clinical Review Criteria
 Clinical Review Criteria Treatment of Varicose Veins Radiofrequency Catheter Closure Sclerotherapy Surgical Stripping Trivex System for Outpatient Varicose Vein Surgery VenaSeal Closure System VNUS Closure
Clinical Review Criteria Treatment of Varicose Veins Radiofrequency Catheter Closure Sclerotherapy Surgical Stripping Trivex System for Outpatient Varicose Vein Surgery VenaSeal Closure System VNUS Closure
treatment of varicose and spider veins patient information SAMPLE a publication by advancing vein care
 treatment of varicose and spider veins patient information a publication by advancing vein care Since most veins lie deep to the skin s surface, vein disorders are not always visible to the naked eye.
treatment of varicose and spider veins patient information a publication by advancing vein care Since most veins lie deep to the skin s surface, vein disorders are not always visible to the naked eye.
Medical Coverage Policy Treatment for Varicose Veins-PREAUTH
 Medical Coverage Policy Treatment for Varicose Veins-PREAUTH Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2001 Policy Last Updated: 12/20/2011 Prospective review is recommended/required.
Medical Coverage Policy Treatment for Varicose Veins-PREAUTH Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2001 Policy Last Updated: 12/20/2011 Prospective review is recommended/required.
Suffering from varicose veins? Patient Information. ELVeS Radial Minimally invasive laser therapy of venous insufficiency
 Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Suffering from varicose veins? Patient Information ELVeS Radial Minimally invasive laser therapy of venous insufficiency Do you suffer from heavy legs or visible veins? This makes diseases of the veins
Corporate Medical Policy Treatment of Varicose Veins/Venous Insufficiency. Medical Policy
 Corporate Medical Policy Treatment of Varicose Veins/Venous Insufficiency File name: Treatment of Varicose Veins/ Venous Insufficiency File code: UM.SURG.03 Origination: 9/01/2010 Last Review: 07/15/2010,
Corporate Medical Policy Treatment of Varicose Veins/Venous Insufficiency File name: Treatment of Varicose Veins/ Venous Insufficiency File code: UM.SURG.03 Origination: 9/01/2010 Last Review: 07/15/2010,
Medical Coverage Policy Varicose Vein Treatment sad
 Medical Coverage Policy Varicose Vein Treatment sad EFFECTIVE DATE: 10 28 2001 POLICY LAST UPDATED: 05 07 2013 OVERVIEW Varicose veins are large superficial veins that have become swollen. These veins
Medical Coverage Policy Varicose Vein Treatment sad EFFECTIVE DATE: 10 28 2001 POLICY LAST UPDATED: 05 07 2013 OVERVIEW Varicose veins are large superficial veins that have become swollen. These veins
TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info
 TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info www.heartofthevillages.com TIRED & ACHING LEGS? If you suffer from varicose and spider veins, you are not alone. It is estimated that there are more
TREATMENT OF VARICOSE AND SPIDER VEINS Patient Info www.heartofthevillages.com TIRED & ACHING LEGS? If you suffer from varicose and spider veins, you are not alone. It is estimated that there are more
Modern Management of Varicose Veins
 Modern Management of Varicose Veins GPCME 2008 David Ferrar Vascular and Endovascular Surgeon Vascular Ultrasound Specialist Multimodality treatment Compression stockings Sclerotherapy Ultrasound guided
Modern Management of Varicose Veins GPCME 2008 David Ferrar Vascular and Endovascular Surgeon Vascular Ultrasound Specialist Multimodality treatment Compression stockings Sclerotherapy Ultrasound guided
Varicose veins - 1 -
 Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Varicose veins - 1 - Varicose Veins About 3 in 10 adults develop varicose veins at some time in their life. Most people with varicose veins do not have an underlying disease and they usually occur for
Medical Affairs Policy
 Service: Varicose Vein Treatments PUM 250-0032 Medical Affairs Policy Implemented 04/04/14, 04/01/15, 4/1/16 Reviewed 12/12/14 Revised 12/12/14, 12/11/15 Developed Arise/WPS Policy 12/12/14, 12/11/15 Committee
Service: Varicose Vein Treatments PUM 250-0032 Medical Affairs Policy Implemented 04/04/14, 04/01/15, 4/1/16 Reviewed 12/12/14 Revised 12/12/14, 12/11/15 Developed Arise/WPS Policy 12/12/14, 12/11/15 Committee
Peninsula Commissioning Priorities Group. Commissioning Policy Varicose Vein Referral
 NHS Devon NHS Plymouth Torbay Care Trust Peninsula Commissioning Priorities Group Commissioning Policy Varicose Vein Referral Varicose Vein Referral Guidelines 1. Description of service/treatment Most
NHS Devon NHS Plymouth Torbay Care Trust Peninsula Commissioning Priorities Group Commissioning Policy Varicose Vein Referral Varicose Vein Referral Guidelines 1. Description of service/treatment Most
SEDICO Newsletter Issue 8. Varicose veins
 SEDICO Newsletter Issue 8 Definition: Varicose veins Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere.
SEDICO Newsletter Issue 8 Definition: Varicose veins Varicose veins are veins that have become enlarged and twisted. The term commonly refers to the veins on the leg, although varicose veins occur elsewhere.
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: varicose_veins_treatment_for 12/2000 11/2014 11/2015 11/2014 Description of Procedure or Service A variety
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: varicose_veins_treatment_for 12/2000 11/2014 11/2015 11/2014 Description of Procedure or Service A variety
Local Coverage Determination (LCD): Varicose Veins of the Lower Extremities (L31796)
 Local Coverage Determination (LCD): Varicose Veins of the Lower Extremities (L31796) Contractor Information Contractor Name Palmetto GBA LCD Information Document Information LCD ID L31796 LCD Title Varicose
Local Coverage Determination (LCD): Varicose Veins of the Lower Extremities (L31796) Contractor Information Contractor Name Palmetto GBA LCD Information Document Information LCD ID L31796 LCD Title Varicose
DEBATE ON Management of primary Varicose Veins SURGERY. Adel Husseiny, Kamhawy Vascular Surgery Unit Tanta University
 DEBATE ON Management of primary Varicose Veins SURGERY Adel Husseiny, Kamhawy Vascular Surgery Unit Tanta University Efficacy of treatment alternatives Durability of results Cosmetically acceptable results
DEBATE ON Management of primary Varicose Veins SURGERY Adel Husseiny, Kamhawy Vascular Surgery Unit Tanta University Efficacy of treatment alternatives Durability of results Cosmetically acceptable results
Varicose Vein Therapy: An Introduction to Surgical and Endovascular Treatment
 Varicose Vein Therapy: An Introduction to Surgical and Endovascular Treatment Lower Extremity Venous Anatomy Deep, Superficial, Perforating, Reticular veins Located in two separate compartments (deep and
Varicose Vein Therapy: An Introduction to Surgical and Endovascular Treatment Lower Extremity Venous Anatomy Deep, Superficial, Perforating, Reticular veins Located in two separate compartments (deep and
Varicose veins: Surgery can still be considered as an option in the treatment
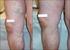 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 12 Ver. I (Dec. 2014), PP 72-77 Varicose veins: Surgery can still be considered as an option
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 12 Ver. I (Dec. 2014), PP 72-77 Varicose veins: Surgery can still be considered as an option
RANDOMIZED CONTROL TRIALS (RCT s) on VARICOSE VEIN ENDOVENOUS TREATMENT
 RANDOMIZED CONTROL TRIALS (RCT s) on VARICOSE VEIN ENDOVENOUS TREATMENT M. PERRIN Lyon - France CONTROVERSIES AND UPDATES IN VASCULAR SURGERY JANUARY 19-21, 2012 Paris B. Eklof Helsingborg, Sweden Thirty
RANDOMIZED CONTROL TRIALS (RCT s) on VARICOSE VEIN ENDOVENOUS TREATMENT M. PERRIN Lyon - France CONTROVERSIES AND UPDATES IN VASCULAR SURGERY JANUARY 19-21, 2012 Paris B. Eklof Helsingborg, Sweden Thirty
Recurrent Varicose Veins. Vineet Mishra, MD Director of Mohs Surgery and Procedural Dermatology University of Texas Health Science Center San Antonio
 Recurrent Varicose Veins Vineet Mishra, MD Director of Mohs Surgery and Procedural Dermatology University of Texas Health Science Center San Antonio Disclosures None Possible Causes of Recurrence DNA:
Recurrent Varicose Veins Vineet Mishra, MD Director of Mohs Surgery and Procedural Dermatology University of Texas Health Science Center San Antonio Disclosures None Possible Causes of Recurrence DNA:
THE VEIN CENTER. State-of-the-Art Treatment for Varicose Veins and Spider Veins
 THE VEIN CENTER State-of-the-Art Treatment for Varicose Veins and Spider Veins Vein Disorders Nearly 50 percent of the adult population suffers from undesirable, sometimes painful vein disease. The most
THE VEIN CENTER State-of-the-Art Treatment for Varicose Veins and Spider Veins Vein Disorders Nearly 50 percent of the adult population suffers from undesirable, sometimes painful vein disease. The most
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE
 CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE Endovenous Laser Ablation is a minimally invasive option for treating great saphenous vein incompetence (leaky valves). The first stage of your surgery
CHINOOK VASCULAR - ENDOVENOUS LASER ABLATION PROCEDURE Endovenous Laser Ablation is a minimally invasive option for treating great saphenous vein incompetence (leaky valves). The first stage of your surgery
TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE?
 TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE? Michel MJP Reijnen Rijnstate Hospital, Arnhem The Netherlands mmpj.reijnen@gmail.com Disclosures
TREATMENT OF VARICOSE VEINS: CAN IT BE IMPROVED BY MECHANOCHEMICAL ABLATION USING THE CLARIVEIN DEVICE? Michel MJP Reijnen Rijnstate Hospital, Arnhem The Netherlands mmpj.reijnen@gmail.com Disclosures
The Treatment of Varicose Veins and Spider Veins
 The Treatment of Varicose Veins and Spider Veins St. Joseph Vein Center Surgical Specialists of St. Joseph, P.C. Glen H. Hastings, M.D., F.A.C.S. 820 Lester Ave., Suite 105 St. Joseph, MI 49085 (269) 983-3368
The Treatment of Varicose Veins and Spider Veins St. Joseph Vein Center Surgical Specialists of St. Joseph, P.C. Glen H. Hastings, M.D., F.A.C.S. 820 Lester Ave., Suite 105 St. Joseph, MI 49085 (269) 983-3368
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Veins. Zapping Varicose. Venous diseases affect many people and represent a major cost to the health-care system.
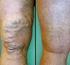 Zapping Varicose Veins Improving the Quality of Life for Sufferers By Jeannette Soriano, MD Venous diseases affect many people and represent a major cost to the health-care system. Hippocrates used compression
Zapping Varicose Veins Improving the Quality of Life for Sufferers By Jeannette Soriano, MD Venous diseases affect many people and represent a major cost to the health-care system. Hippocrates used compression
Varicose Veins: Causes, Symptoms and Management. Andrew C. Stanley MD Section of Vascular Surgery
 Varicose Veins: Causes, Symptoms and Management Andrew C. Stanley MD Section of Vascular Surgery Circulation Heart (Pump)-MI, Sudden Death Arteries (Stroke, Aneurysms, Walking dysfunction, Limb loss) Veins
Varicose Veins: Causes, Symptoms and Management Andrew C. Stanley MD Section of Vascular Surgery Circulation Heart (Pump)-MI, Sudden Death Arteries (Stroke, Aneurysms, Walking dysfunction, Limb loss) Veins
LOWER EXTREMITY VENOUS DUPLEX ULTRASOUND:
 LOWER EXTREMITY VENOUS DUPLEX ULTRASOUND: Chronic Venous Insufficiency Phillip J Bendick, PhD William Beaumont Hospital Royal Oak, Michigan Prevalence: Carotid ASO ~ 3M Peripheral Arterial Dz ~ 5M + CAD
LOWER EXTREMITY VENOUS DUPLEX ULTRASOUND: Chronic Venous Insufficiency Phillip J Bendick, PhD William Beaumont Hospital Royal Oak, Michigan Prevalence: Carotid ASO ~ 3M Peripheral Arterial Dz ~ 5M + CAD
X-Plain Varicose Veins Reference Summary
 X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
Sclerotherapy has been performed for decades to
 Sclerotherapy: Introduction to Solutions and Techniques Charles L. Dietzek, DO, FACOS Perspectives in Vascular Surgery and Endovascular Therapy Volume 19 Number 3 September 2007 317-324 2007 Sage Publications
Sclerotherapy: Introduction to Solutions and Techniques Charles L. Dietzek, DO, FACOS Perspectives in Vascular Surgery and Endovascular Therapy Volume 19 Number 3 September 2007 317-324 2007 Sage Publications
Medical Policy Manual. Date of Origin: October 11, 1999. Topic: Varicose Vein Treatment. Last Reviewed Date: May 2015.
 Medical Policy Manual Topic: Varicose Vein Treatment Section: Surgery Policy No: 104 Date of Origin: October 11, 1999 Last Reviewed Date: May 2015 Effective Date: September 1, 2015 IMPORTANT REMINDER Medical
Medical Policy Manual Topic: Varicose Vein Treatment Section: Surgery Policy No: 104 Date of Origin: October 11, 1999 Last Reviewed Date: May 2015 Effective Date: September 1, 2015 IMPORTANT REMINDER Medical
Information for patients who require Foam Sclerotherapy for Varicose Veins.
 Information for patients who require Foam Sclerotherapy for Varicose Veins. Why do I need this procedure? Everybody has two sets of veins in the legs. These include the superficial and deep veins. Their
Information for patients who require Foam Sclerotherapy for Varicose Veins. Why do I need this procedure? Everybody has two sets of veins in the legs. These include the superficial and deep veins. Their
Venous leg ulcers. Venous Ulcers. Treat the source, not just the symptom
 Venous leg ulcers Venous Ulcers Treat the source, not just the symptom Topics What causes venous ulcers (VU) Treating the source, not just the symptom Diagnosis with venous duplex ultrasound scan Treatment
Venous leg ulcers Venous Ulcers Treat the source, not just the symptom Topics What causes venous ulcers (VU) Treating the source, not just the symptom Diagnosis with venous duplex ultrasound scan Treatment
Health Technology Assessment of Scheduled Surgical Procedures
 HTA of Scheduled Surgical Procedures April 2013 Health Technology Assessment of Scheduled Surgical Procedures Varicose Vein Surgery April 2013 Safer Better Care About the The (HIQA) is the independent
HTA of Scheduled Surgical Procedures April 2013 Health Technology Assessment of Scheduled Surgical Procedures Varicose Vein Surgery April 2013 Safer Better Care About the The (HIQA) is the independent
Varicose veins are generally identified
 Management of Varicose Veins Richard H. Jones, MD, MSPH, Naval Health Clinic, Quantico, Virginia Peter J. Carek, MD, MS, Medical University of South Carolina, Charleston, South Carolina Varicose veins
Management of Varicose Veins Richard H. Jones, MD, MSPH, Naval Health Clinic, Quantico, Virginia Peter J. Carek, MD, MS, Medical University of South Carolina, Charleston, South Carolina Varicose veins
Endovenous Laser Therapy
 Information for patients Endovenous Laser Therapy Northern General Hospital You have been given this leaflet because you will be having Endovenous Laser Therapy (EVLT). This leaflet explains more about
Information for patients Endovenous Laser Therapy Northern General Hospital You have been given this leaflet because you will be having Endovenous Laser Therapy (EVLT). This leaflet explains more about
V03 Varicose Veins Surgery
 V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
Treatment by LASER. Understanding Varicose veins and. Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD)
 Understanding Varicose veins and Treatment by LASER Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD) Orange city Hospital & Research Institute 19, Pandey Lay out, Veer Sawarkar Square, Nagpur 440015
Understanding Varicose veins and Treatment by LASER Dr. Rajesh Mundhada (MD. DNB) Dr. Atul Rewatkar (MD) Orange city Hospital & Research Institute 19, Pandey Lay out, Veer Sawarkar Square, Nagpur 440015
Treatment of Varicose Veins
 Varicose Vein Treatment of Varicose Veins JMAJ 47(3): 146 151, 2004 Osamu SATO Associate Professor, Department of Surgery, Saitama Medical Center Abstract: Varicose vein is a condition that was first described
Varicose Vein Treatment of Varicose Veins JMAJ 47(3): 146 151, 2004 Osamu SATO Associate Professor, Department of Surgery, Saitama Medical Center Abstract: Varicose vein is a condition that was first described
Venous and Lymphatic Disorders
 Venous and Lymphatic Disorders. ก. Venous and Lymphatic Disorders Varicose Veins Deep Vein Thrombosis (DVT) Lymphedema What Is Varicose Veins? Latin: Varicose = Varix = twisted Abnormal venous dilatation
Venous and Lymphatic Disorders. ก. Venous and Lymphatic Disorders Varicose Veins Deep Vein Thrombosis (DVT) Lymphedema What Is Varicose Veins? Latin: Varicose = Varix = twisted Abnormal venous dilatation
VARICOSE VEINS AND VENOUS INSUFFICIENCY
 VARICOSE VEINS AND VENOUS INSUFFICIENCY SURGICAL AND ABLATION TREATMENTS Policy Number: 2014M0064A Effective Date: September 1, 2014 Table of Contents: Page: Cross Reference Policy: POLICY DESCRIPTION
VARICOSE VEINS AND VENOUS INSUFFICIENCY SURGICAL AND ABLATION TREATMENTS Policy Number: 2014M0064A Effective Date: September 1, 2014 Table of Contents: Page: Cross Reference Policy: POLICY DESCRIPTION
Australian Safety and Efficacy Register of New Interventional Procedures Surgical. Rapid review ASERNIP-S REPORT NO. 66
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Rapid review Treatments for varicose veins ASERNIP-S REPORT NO. 66 Australian Safety & Efficacy Register of New
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Rapid review Treatments for varicose veins ASERNIP-S REPORT NO. 66 Australian Safety & Efficacy Register of New
Recurrent Varicose Veins
 Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Information for patients Recurrent Varicose Veins Sheffield Vascular Institute Northern General Hospital You have been diagnosed as having Varicose Veins that have recurred (come back). This leaflet explains
Patient Information Understanding Varicose Veins
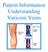 Patient Information Understanding Varicose Veins The Circulatory System Arteries carry oxygenated blood to your legs and the veins carry de-oxygenated blood away from your legs. The blood returns to the
Patient Information Understanding Varicose Veins The Circulatory System Arteries carry oxygenated blood to your legs and the veins carry de-oxygenated blood away from your legs. The blood returns to the
ARTICLE IN PRESS. D.G. Bountouroglou, M. Azzam, S.K. Kakkos, M. Pathmarajah, P. Young and G. Geroulakos*
 Eur J Vasc Endovasc Surg xx, 1 8 (xxxx) doi:10.1016/j.ejvs.2005.08.024, available online at http://www.sciencedirect.com on Ultrasound-guided Foam Sclerotherapy Combined with Sapheno-femoral Ligation Compared
Eur J Vasc Endovasc Surg xx, 1 8 (xxxx) doi:10.1016/j.ejvs.2005.08.024, available online at http://www.sciencedirect.com on Ultrasound-guided Foam Sclerotherapy Combined with Sapheno-femoral Ligation Compared
Prevalence and surgical outcomes of varicose veins at Regional Institute of Medical Sciences, Imphal
 ORIGINAL ARTICLE JIACM 2013; 14(3-4): 209-13 Prevalence and surgical outcomes of varicose veins at Regional Institute of Medical Sciences, Imphal Ksh Kala Singh*, A Surjyalal Sharma**, L Sunil Singh***,
ORIGINAL ARTICLE JIACM 2013; 14(3-4): 209-13 Prevalence and surgical outcomes of varicose veins at Regional Institute of Medical Sciences, Imphal Ksh Kala Singh*, A Surjyalal Sharma**, L Sunil Singh***,
Jose Almeida MD, FACS, RVT Jeff Raines PhD, RVT. Oliver Göckeritz MD Christian Wentzel MD. Tim Richards MD Daniel F. Hoheim, MD.
 Final Results 1 Jose Almeida MD, FACS, RVT Jeff Raines PhD, RVT Miami Vein Center Miami, Florida Oliver Göckeritz MD Christian Wentzel MD Venenzentrum Elserpark Leipzig, Germany John Kaufman MD Dotter
Final Results 1 Jose Almeida MD, FACS, RVT Jeff Raines PhD, RVT Miami Vein Center Miami, Florida Oliver Göckeritz MD Christian Wentzel MD Venenzentrum Elserpark Leipzig, Germany John Kaufman MD Dotter
Do you have any of these varicose vein symptoms?
 Do you have any of these varicose vein symptoms? Heaviness Achiness Swelling Throbbing Itching HASTI Symptoms Ask your doctor if Varithena is right for you Varithena (polidocanol injectable foam) is a
Do you have any of these varicose vein symptoms? Heaviness Achiness Swelling Throbbing Itching HASTI Symptoms Ask your doctor if Varithena is right for you Varithena (polidocanol injectable foam) is a
LONG TERM FOLLOW-UP AFTER ENDOVENOUS LASER ABLATION
 LONG TERM FOLLOW-UP AFTER ENDOVENOUS LASER ABLATION Giorgio Spreafico Centro Multidisciplinare Day Surgery Azienda Ospedaliera Università Padova - Italy Faculty Disclosure I have no financial relationships
LONG TERM FOLLOW-UP AFTER ENDOVENOUS LASER ABLATION Giorgio Spreafico Centro Multidisciplinare Day Surgery Azienda Ospedaliera Università Padova - Italy Faculty Disclosure I have no financial relationships
L. H. Rasmussen, M. Lawaetz, L. Bjoern, B. Vennits, A. Blemings and B. Eklof
 Randomized clinical trial Randomized clinical trial comparing endovenous laser ablation, radiofrequency ablation, foam sclerotherapy and surgical stripping for great saphenous varicose veins L. H. Rasmussen,
Randomized clinical trial Randomized clinical trial comparing endovenous laser ablation, radiofrequency ablation, foam sclerotherapy and surgical stripping for great saphenous varicose veins L. H. Rasmussen,
Treating varicose veins with foam injections using ultrasound guidance
 Issue date February 2013 Information for the public NICE interventional procedures guidance advises the NHS on when and how new procedures can be used in clinical practice. Treating varicose veins with
Issue date February 2013 Information for the public NICE interventional procedures guidance advises the NHS on when and how new procedures can be used in clinical practice. Treating varicose veins with
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endovenous mechanochemical ablation for varicose veins Treating varicose veins
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endovenous mechanochemical ablation for varicose veins Treating varicose veins
PRIMARY VARICOSE VEIN management has undergone a
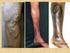 Treatment of Primary Varicose Veins Has Changed with the Introduction of New Techniques Eric Mowatt-Larssen* and Cynthia K. Shortell* New technologies have produced a revolution in primary varicose vein
Treatment of Primary Varicose Veins Has Changed with the Introduction of New Techniques Eric Mowatt-Larssen* and Cynthia K. Shortell* New technologies have produced a revolution in primary varicose vein
Verification of Participation & Certificate Request 28 th Annual Congress Phoenix, Arizona November 6 9, 2014
 Complete this form in its entirety to claim the credits commensurate with your participation at the ACP s 28 th Annual Congress. You can only claim credit for one session if it runs concurrently with others.
Complete this form in its entirety to claim the credits commensurate with your participation at the ACP s 28 th Annual Congress. You can only claim credit for one session if it runs concurrently with others.
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): 7/12/2003 Most Recent Review Date (Revised): 3/29/2016 Effective Date: 8/1/2016 I. POLICY Great or Small Saphenous Veins Treatment of the greater small saphenous veins by
Original Issue Date (Created): 7/12/2003 Most Recent Review Date (Revised): 3/29/2016 Effective Date: 8/1/2016 I. POLICY Great or Small Saphenous Veins Treatment of the greater small saphenous veins by
Treatment of Varicose Veins/Venous Insufficiency
 MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Treatment of Varicose Veins/Venous Insufficiency Number 7.01.519
MEDICAL POLICY POLICY RELATED POLICIES POLICY GUIDELINES DESCRIPTION SCOPE BENEFIT APPLICATION RATIONALE REFERENCES CODING APPENDIX HISTORY Treatment of Varicose Veins/Venous Insufficiency Number 7.01.519
What are spider veins? What is the best treatment for spider veins?
 Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Laser Spider/Leg Vein Q & A What are spider veins? Millions of women and men are bothered by unsightly spider veins on their faces and legs. Spider veins or telangiectasias are those small red, blue and
Emory Healthcare s model for a PA based vein clinic
 Emory Healthcare s model for a PA based vein clinic Stephen Konigsberg PA-C No relationships to disclose Society for Vascular Surgery 2011 Vascular Annual Meeting Chicago, IL June 17, 2011 Division of
Emory Healthcare s model for a PA based vein clinic Stephen Konigsberg PA-C No relationships to disclose Society for Vascular Surgery 2011 Vascular Annual Meeting Chicago, IL June 17, 2011 Division of
EndoVenous Laser Therapy (EVLT) Information Booklet. Dr. Dueck. Varicose Veins
 EndoVenous Laser Therapy (EVLT) Information Booklet Dr. Dueck Varicose Veins Varicose veins are abnormally large veins that protrude from under the skin in the legs. They can be associated with a brown
EndoVenous Laser Therapy (EVLT) Information Booklet Dr. Dueck Varicose Veins Varicose veins are abnormally large veins that protrude from under the skin in the legs. They can be associated with a brown
MEDICAL POLICY SUBJECT: VARICOSITIES, TREATMENT ALTERNATIVES TO VEIN STRIPPING AND LIGATION
 MEDICAL POLICY SUBJECT: VARICOSITIES, TREATMENT PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: VARICOSITIES, TREATMENT PAGE: 1 OF: 10 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
The Treatment of Varicose Veins
 Ann R Coll Surg Engl. 2007 Mar; 89(2): 96 100. doi: 10.1308/003588407X168271 PMCID: PMC1964550 The Treatment of Varicose Veins 1 2 S Subramonia and TA Lees 1 Department of General Surgery, Queen's Medical
Ann R Coll Surg Engl. 2007 Mar; 89(2): 96 100. doi: 10.1308/003588407X168271 PMCID: PMC1964550 The Treatment of Varicose Veins 1 2 S Subramonia and TA Lees 1 Department of General Surgery, Queen's Medical
Australian Safety and Efficacy Register of New Interventional Procedures Surgical. Systematic review ASERNIP-S REPORT NO. 69
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Systematic review Treatments for varicose veins ASERNIP-S REPORT NO. 69 Australian Safety & Efficacy Register
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Systematic review Treatments for varicose veins ASERNIP-S REPORT NO. 69 Australian Safety & Efficacy Register
Varicose Vein Treatment (Endovenous Ablation of Varicose Veins)
 Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
Scan for mobile link. Varicose Vein Treatment (Endovenous Ablation of Varicose Veins) Varicose vein treatment, also known as endovenous ablation, uses radiofrequency or laser energy to cauterize and close
AMERICAN VENOUS FORUM
 Revised Venous Clinical Severity Score AMERICAN VENOUS FORUM Pain : 0 Mild: 1 or other discomfort (ie, aching, heaviness, fatigue, soreness, burning) origin Occasional pain or other discomfort (ie, not
Revised Venous Clinical Severity Score AMERICAN VENOUS FORUM Pain : 0 Mild: 1 or other discomfort (ie, aching, heaviness, fatigue, soreness, burning) origin Occasional pain or other discomfort (ie, not
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
ACUTE DVT MANAGEMENT Richard J. DeMasi, MD April 26, 2014
 ACUTE DVT MANAGEMENT Richard J. DeMasi, MD April 26, 2014 Thromboembolism epidemiology 5 million DVT s 900,000 PE s 290,000 fatalities Heit J. Blood. 2005;106:910. 10 VTE events Since this talk began DVT
ACUTE DVT MANAGEMENT Richard J. DeMasi, MD April 26, 2014 Thromboembolism epidemiology 5 million DVT s 900,000 PE s 290,000 fatalities Heit J. Blood. 2005;106:910. 10 VTE events Since this talk began DVT
Modern Varicose Vein Treatments: What Every Patient Should Know
 The Skin and Vein Center Oneonta Laser Derm & Day Spa Natural Good Looks and Leg Veins Our Specialty Dr Eric Dohner, MD 41-45 Dietz St Oneonta, NY 13820 607/431-2525 www.oneontalaserderm.com Modern Varicose
The Skin and Vein Center Oneonta Laser Derm & Day Spa Natural Good Looks and Leg Veins Our Specialty Dr Eric Dohner, MD 41-45 Dietz St Oneonta, NY 13820 607/431-2525 www.oneontalaserderm.com Modern Varicose
Varicose veins and spider veins
 Varicose veins and spider veins Summary Varicose veins are knobbly, twisted and darkish-blue in appearance, and are most commonly found on people s legs. Varicose veins are caused by faulty valves within
Varicose veins and spider veins Summary Varicose veins are knobbly, twisted and darkish-blue in appearance, and are most commonly found on people s legs. Varicose veins are caused by faulty valves within
Provided by the American Venous Forum: veinforum.org
 CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
CHAPTER 17 SURGICAL THERAPY FOR DEEP VALVE INCOMPETENCE Original author: Seshadri Raju Abstracted by Gary W. Lemmon Introduction Deep vein valvular incompetence happens when the valves in the veins (tubes
Varicose Veins Backgrounder
 What Are Varicose Veins? Varicose veins are a clinical presentation of superficial venous insufficiency a condition in which veins are inefficient in returning blood to the heart due to venous hypertension.
What Are Varicose Veins? Varicose veins are a clinical presentation of superficial venous insufficiency a condition in which veins are inefficient in returning blood to the heart due to venous hypertension.
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis
 Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
VARICOSE VEINS; OUTCOME OF SURGICAL MANAGEMENT AND RECURRENCES
 The Professional Medical Journal www.theprofesional.com ORIGINAL PROF-2328 VARICOSE VEINS; OUTCOME OF SURGICAL MANAGEMENT AND RECURRENCES 1. FCPS Consultant surgeon Department of general surgery Liaquat
The Professional Medical Journal www.theprofesional.com ORIGINAL PROF-2328 VARICOSE VEINS; OUTCOME OF SURGICAL MANAGEMENT AND RECURRENCES 1. FCPS Consultant surgeon Department of general surgery Liaquat
Institute of Health Economics ENDOVENOUS ABLATION INTERVENTIONS FOR SYMPTOMATIC VARICOSE VEINS OF THE LEGS
 Institute of Health Economics ENDOVENOUS ABLATION INTERVENTIONS FOR SYMPTOMATIC VARICOSE VEINS OF THE LEGS September 2014 INSTITUTE OF HEALTH ECONOMICS The Institute of Health Economics (IHE) is an independent,
Institute of Health Economics ENDOVENOUS ABLATION INTERVENTIONS FOR SYMPTOMATIC VARICOSE VEINS OF THE LEGS September 2014 INSTITUTE OF HEALTH ECONOMICS The Institute of Health Economics (IHE) is an independent,
Spider and Varicose Veins
 KRAMES. PATIENT EDUCATION Procedures for Spider and Varicose Veins How Vein Problems Develop Easing Symptoms with Self-Care Minimally Invasive and Surgical Treatment Options , J ;Yf 'i Understanding Problem
KRAMES. PATIENT EDUCATION Procedures for Spider and Varicose Veins How Vein Problems Develop Easing Symptoms with Self-Care Minimally Invasive and Surgical Treatment Options , J ;Yf 'i Understanding Problem
XARELTO (rivaroxaban tablets) in Knee and Hip Replacement Surgery
 XARELTO (rivaroxaban tablets) in Knee and Hip Replacement Surgery Fast Facts: XARELTO is a novel, once-daily, oral anticoagulant recently approved in the United States for the prevention (prophylaxis)
XARELTO (rivaroxaban tablets) in Knee and Hip Replacement Surgery Fast Facts: XARELTO is a novel, once-daily, oral anticoagulant recently approved in the United States for the prevention (prophylaxis)
SURGICAL AND ABLATIVE PROCEDURES FOR VENOUS INSUFFICIENCY AND VARICOSE VEINS
 CLINICAL POLICY SURGICAL AND ABLATIVE PROCEDURES FOR VENOUS INSUFFICIENCY AND VARICOSE VEINS Policy Number: OUTPATIENT 013.24 T2 Effective Date: July 1, 2014 Table of Contents CONDITIONS OF COVERAGE...
CLINICAL POLICY SURGICAL AND ABLATIVE PROCEDURES FOR VENOUS INSUFFICIENCY AND VARICOSE VEINS Policy Number: OUTPATIENT 013.24 T2 Effective Date: July 1, 2014 Table of Contents CONDITIONS OF COVERAGE...
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
A clinical trial designed to discover if the primary treatment of varicose veins should be by Fegan s method or by an operation
 Br. J. Surg. Vol. 62 (1975) 72-76 A clinical trial designed to discover if the primary treatment of varicose veins should be by Fegan s method or by an operation F. S. A. DORAN AND MARY WHITE* SUMMARY
Br. J. Surg. Vol. 62 (1975) 72-76 A clinical trial designed to discover if the primary treatment of varicose veins should be by Fegan s method or by an operation F. S. A. DORAN AND MARY WHITE* SUMMARY
Dr. Linde is an international beauty expert and an acclaimed keynote speaker at conferences all over the world. He is specialized in the treatment of
 VEINS Dr. Linde is an international beauty expert and an acclaimed keynote speaker at conferences all over the world. He is specialized in the treatment of fat pads, wrinkles and transformations of the
VEINS Dr. Linde is an international beauty expert and an acclaimed keynote speaker at conferences all over the world. He is specialized in the treatment of fat pads, wrinkles and transformations of the
The anthropometric characteristics in the two groups were not significantly different.
 Studio prospettico, randomizzato monocentrico per il trattamento sintomatico dell insufficienza venosa cronica degli arti inferiori in pazienti trattati con calze preventive con filato SpikEnergy rispetto
Studio prospettico, randomizzato monocentrico per il trattamento sintomatico dell insufficienza venosa cronica degli arti inferiori in pazienti trattati con calze preventive con filato SpikEnergy rispetto
Day surgery varicose vein treatment using endovenous laser
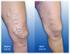 O R I G I N A L A R T I C L E Day surgery varicose vein treatment using endovenous laser P Ho Jensen TC Poon SY Cho Grace Cheung YF Tam WK Yuen Stephen WK Cheng 何 蓓 潘 冬 松 曹 素 賢 張 頌 恩 譚 婉 芳 袁 維 基 鄭 永 強
O R I G I N A L A R T I C L E Day surgery varicose vein treatment using endovenous laser P Ho Jensen TC Poon SY Cho Grace Cheung YF Tam WK Yuen Stephen WK Cheng 何 蓓 潘 冬 松 曹 素 賢 張 頌 恩 譚 婉 芳 袁 維 基 鄭 永 強
Varicose Veins and Spider Veins
 page 1 Varicose Veins and Spider Veins Q: What are varicose veins and spider A: Varicose (VAR-i-kos) veins are enlarged veins that can be blue, red, or fleshcolored. They often look like cords and appear
page 1 Varicose Veins and Spider Veins Q: What are varicose veins and spider A: Varicose (VAR-i-kos) veins are enlarged veins that can be blue, red, or fleshcolored. They often look like cords and appear
Developments in Endovascular and Endoscopic Surgery
 Developments in Endovascular and Endoscopic Surgery Radiofrequency Ablation and Laser Ablation in the Treatment of Varicose Veins Jose I. Almeida, MD, FACS, RVT, 1,2 and Jeffrey K. Raines, PhD, RVT, 1,2
Developments in Endovascular and Endoscopic Surgery Radiofrequency Ablation and Laser Ablation in the Treatment of Varicose Veins Jose I. Almeida, MD, FACS, RVT, 1,2 and Jeffrey K. Raines, PhD, RVT, 1,2
SURGICAL AND ABLATIVE PROCEDURES FOR VENOUS INSUFFICIENCY AND VARICOSE VEINS
 SURGICAL AND ABLATIVE PROCEDURES FOR VENOUS INSUFFICIENCY AND VARICOSE VEINS Protocol: SUR037 Effective Date: 5/1/2015 Table of Contents COMMERCIAL INDICATIONS FOR COVERAGE DEFINITIONS MEDICARE AND MEDICAID
SURGICAL AND ABLATIVE PROCEDURES FOR VENOUS INSUFFICIENCY AND VARICOSE VEINS Protocol: SUR037 Effective Date: 5/1/2015 Table of Contents COMMERCIAL INDICATIONS FOR COVERAGE DEFINITIONS MEDICARE AND MEDICAID
Endovenous Laser: A New Minimally Invasive Method of Treatment for Varicose Veins - Preliminary Observations Using an 810 nm Diode Laser
 Endovenous Laser: A New Minimally Invasive Method of Treatment for Varicose Veins - Preliminary Observations Using an 810 nm Diode Laser Luis NAVARRO, MD,* ROBERT J. MIN, MD, AND CARLOS BONE, MD *Vein
Endovenous Laser: A New Minimally Invasive Method of Treatment for Varicose Veins - Preliminary Observations Using an 810 nm Diode Laser Luis NAVARRO, MD,* ROBERT J. MIN, MD, AND CARLOS BONE, MD *Vein
INFORMATION DOCUMENT. Minimal Invasive Therapy of Leg Veins. Types of Veins. What is the mechanism by which veins develop?
 INFORMATION DOCUMENT Minimal Invasive Therapy of Leg Veins (Injection Microsclerotherapy / Ultrasound Guided Sclerotherapy / Endovenous Laser Therapy-EVLA and Modified Ambulatory Phlebectomy). This document
INFORMATION DOCUMENT Minimal Invasive Therapy of Leg Veins (Injection Microsclerotherapy / Ultrasound Guided Sclerotherapy / Endovenous Laser Therapy-EVLA and Modified Ambulatory Phlebectomy). This document
