NEURO-OTOLOGIC TEST CENTER EVALUATION IN MILD TRAUMATIC BRAIN INJURY
|
|
|
- Primrose Singleton
- 8 years ago
- Views:
Transcription
1 A Case Study NEURO-OTOLOGIC TEST CENTER EVALUATION IN MILD TRAUMATIC BRAIN INJURY Brian J. McKinnon, MD, MBA Assistant Professor, Otology/Neurotology Department of Otolaryngology-Head & Neck Surgery Medical College of Georgia th Street Augusta, GA Alex Kiderman, PhD Chief Technology Officer Neuro Kinetics, Inc. 128 Gamma Drive Pittsburgh, PA Terri E. Ives, ScD, AuD, F-AAA, CCC-A Clinical Director - Audiology Neuro Kinetics, Inc. 128 Gamma Drive Pittsburgh, PA
2 Abstract: Introduction: Opportunities to evaluate neuro-otologic test data on a subject prior to and following a mild traumatic brain injury (mtbi) are rare. An exception is if there is data collected on a pre m-tbi subject as part of a normative data collection program and or product development testing. This case report involves just such a unique mix of circumstances where data had been collected on a normal test subject who later suffered an mtbi. Methods and Materials: Prior to the subject s mtbi, Optokinetic (OKN), Spontaneous, Saccade, Horizontal and Vertical Gaze, Subjective Visual Vertical (SVV) and Subjective Visual Horizontal (SVH), Head Thrust Test (HTT), and Sinusoidal Harmonic Acceleration (SHA) data was collected during product development testing. These tests were repeated numerous times during the six months following the injury. Results: All results prior to the accident were within normal parameters. Following the mtbi, all results were abnormal, suggesting both peripheral and central vestibular dysfunction. At six months following the mtbi event, the subject s results for HTT, and SHA tests remained abnormal. Conclusions: The findings in this report underscore the potential benefits of a more aggressive neuro-otologic evaluation of patients with mtbi for both clinical investigation, and clinical management. 2
3 BACKGROUND Of the estimated 1.5 million traumatic brain injuries occurring annually (1), approximately 75-90% are mild traumatic brain injury (mtbi) (1, 2). Mild traumatic brain injury has been defined (1, 3) as a blunt trauma induced physiological disruption of brain function, as manifested by a least one of the following: any period of loss of consciousness lasting thirty minutes or less; any loss of memory for events immediately before or after the accident; any alteration in mental state at the time of the accident (eg, feeling dazed, disoriented, or confused); and/or focal neurological deficit(s) that may or may not be transient. The definition of mtbi does not include posttraumatic amnesia of greater than 24 hours, an initial Glasgow Coma Scale (GCS) of less than 12 within thirty minutes following injury and/ or loss of consciousness of greater than thirty minutes. Symptoms such as headache, dizziness, irritability, fatigue, or poor concentration, when identified soon after injury, can support the diagnosis of mtbi, but cannot be used to make the diagnosis in the absence of loss of consciousness or altered consciousness (3). The mtbi patient commonly complains of somatic, cognitive and behavioral problems following injury (4-11), symptoms that can persist for several months (12). As summarized in the National Center for Injury Prevention and Control s Report to Congress on Mild Traumatic Brain Injury in the United States: Steps to Prevent a Serious Public Health Problem (1), lost time from work can be substantial, and rates of unemployment in those that have suffered mild traumatic brain injury is markedly higher than the general population. The economic burden from mild traumatic brain injury is reportedly $16.7 billion per year (1). 3
4 Neuro Kinetics, Inc (NKI) manufactures the I-Portal NOTC (Neuro-Otologic Test Center). The I-Portal NOTC has the capacity to execute a full battery of ocular motor and motion stimulus tests while measuring the response of the eyes at over 100 hz. The I-Portal NOTC technology executes the same battery of tests traditionally used in the diagnosis of vestibular and neurological disorders. Most of the NKI employees and a number of outside test subjects have been tested in the I-Portal NOTC as part of NKI s product development process allowing for the collection of a sizable set of normal subject data. The following case report is based on one of those product development test subjects who later suffered an mtbi. CASE REPORT A 47-year-old male NKI employee was in a bicycle accident that resulted in a mild closed head injury on April 7, At the time of the injury, he was physically very active and in general good health. The accident occurred while traveling at approximately 20 miles per hour when the front wheel of his bicycle locked as a result of a flat tire, catapulting him over the handle bars resulting in an impact to his head and left shoulder. The subject was wearing a Bell Avalanche bicycle helmet, purchased in the late 90 s and meeting the safety standard of the time (13). The helmet incurred a midline break from the incident. The patient experienced no loss of consciousness, but did have an altered mental state immediately after the accident that he described as seeing stars and having his bell rung. 4
5 The patient immediately sought care at a local hospital and was evaluated in the emergency room. He presented with chief complaints of cephalgia and neck pain. A head CAT scan without contrast did not reveal any insult. The treating physician diagnosed the patient with a mild head injury without concussion. Post discharge from the emergency room, the patient experienced symptoms of diplopia and excessive fatigue which gradually improved during the following six months, but did not fully resolve. The subject, tested at NKI prior to the mtbi on several occasions for the purposes of product development, had no history of prior head or vestibular injury before this incident and all previous I-Portal NOTC test data collected was within normal limits. Post mtbi, the subject was tested regularly with I-Portal NOTC evaluation. METHODS AND MATERIALS All tests were performed utilizing the I-Portal NOTC and in the manner stated by the User Manual (14) with the exception of the Head Thrust Test (HTT). The HTT is a well defined standard neuro-otological test being adapted to a passive head-on-body (spine-in-alignment) test using the I-Portal NOTC. This subject was run using 385 ft lb servo direct torque motor at an acceleration of 750 deg/sec². Each HTT set included 10 clockwise (CW; rightward referenced to patient) and 10 counterclockwise (CCW; leftward referenced to patient) randomized trials. During testing, both horizontal and vertical eye data compared to chair velocity were collected. Each trial was analyzed separately; cycle(s) contaminated by artifacts (blinks, head slippage, unexpected saccades) were removed. Latencies were removed for all cycles. All accepted cycles in the CW direction were averaged and all accepted cycles in the CCW direction were averaged for individual CW and CCW gain calculations. 5
6 The patient had undergone Optokinetic (OKN), Spontaneous, Horizontal and Vertical Gaze, Saccade, Subjective Visual Vertical (SVV) and Subjective Visual Horizontal (SVH), Head Thrust Test (HTT), and Sinusoidal Harmonic Acceleration (SHA) testing prior to the mtbi injury as part of the product development process. After the injury occurred, these tests were repeated for six months following injury, at the intervals shown in Table 1. The subject continued to be tested post mtbi as part of product development testing. The subject was tested randomly multiple times using standard vestibular testing protocols with the I-Portal NOTC platform. Not all tests were run in all sessions due to subject discomfort resulting from diplopia and a false sense of target motion. RESULTS Throughout the testing there was a consistent pattern showing an initial diminution in vestibular response, with gradual improvement over the several months. Optokinetics Optokinetics (OKN) testing was performed at 20 deg/sec, 40 deg/sec and 60 deg/sec CW and CCW. The results are detailed in figures 1-3. OKN gains and symmetry pre-injury were within normal limits. OKN gain post mtbi was depressed for all conditions with the CCW direction having greater reduction than CW. Twenty degrees per second OKN recovered the most quickly for CW to pre-injury levels at a one week post injury but relapsed until two months post injury. Counter-clockwise results at 20 deg/sec followed a waxing and waning pattern until one month post injury when eye velocity gain continued to improve until pre-injury levels were attained at 2.5 months. Optokinetic testing at 40 and 60 deg/sec rotation followed a pattern similar pattern of 6
7 recovery. Nearly all gain results improved on repeat testing over time. Significant asymmetry was noted at 20 deg/sec for the first 3 weeks and at 40 deg/sec at 4 days post injury and at 60 deg/sec slightly over one month post injury. Spontaneous nystagmus, Horizontal and Vertical Gaze No spontaneous, or gaze nystagmus was present in pre-injury testing. Post mtbi, center gaze position spontaneous nystagmus (vision denied) of deg/sec left beating was noted. Spontaneous nystagmus was left beating in gaze left and right and right beating in gaze up and gaze down, with gaze up being the most prominent (2.67 deg/sec). There was no nystagmus with vision present. By three weeks post injury the spontaneous nystagmus had resolved (figure 4). Subjective Visual Vertical (SVV) and Subjective Visual Horizontal (SVH) Subjective Visual Vertical (0.4 deg) and SVH (0.3 deg) pre-injury were within normal limits. Post mtbi both SVV and SVH rotated toward the patient s right side at 4.45 and 3.6 degrees respectively. The degree of rotation decreased steadily until 8 weeks post injury where SVV and SVH returned to normal (figure 5). Results returned to near initial test results at 2.5 months post injury. Head Thrust Test (HTT) NKI is developing a new Head Thrust test (HTT) using the high torque rotary motor incorporated in its I-Portal NOTC-C system to run a test at accelerations of up to 2000 degrees per second squared with the spine in alignment, head-on-body rotation. As part of the product and test development, the subject was tested at750 deg/sec 2. Each HTT set included 10 clockwise (CW; rightward referenced to patient) and 10 counterclockwise (CCW; leftward referenced to patient) randomized trials. 7
8 Before the accident, left and right gains were approximately one (1). While a normative data base has yet to be collected for this new test, a gain of one (1) is the value logically expected for a normal subject. Gains decreased to 0.81 for CW HTT and 0.51 for CCW HTT at initial testing. At three months post injury gains were still lower CCW than before the accident (figure 6). Saccades During saccade testing, peak eye velocity (deg/sec), percent accuracy (main saccade only), percent overall accuracy, (sum of main and additional corrective saccades), and latency (sec), were measured separately for left (figure 7) and right eye (figure 8) moving to the left or right. It was observed that latency, accuracy and overall accuracy did not change significantly before and after accident but peak eye velocity became abnormally low bilaterally and bi-directionally. Sinusoidal Harmonic Acceleration The subject underwent sinusoidal harmonic acceleration chair rotation testing seven times over a six month period. Testing frequencies were 0.01Hz, 0.02Hz, 0.04Hz, 0.08Hz, 0.16Hz, 0.32Hz, 0.64Hz, 1.28Hz and sometimes 1.5Hz at a velocity of 60 deg/sec. Analyses were based on the multivariate statistics model put forth by Dimitri et al (15). Out of 7 series of tests, 5 showed abnormal overall low gain (4/25/2008, 6/4/2008, 6/23/2008, 7/10/2008, and 10/8/2008) but only one showed overall abnormal asymmetry (4/15/2008). 8
9 DISCUSSION Mild Traumatic Brain Injury is viewed as a major health concern in children and young adults (1) and for our soldiers returning from Iraq and Afghanistan. The definition of what is considered an mtbi is evolving, and as stated earlier, the impact on the individual and the wider society as a whole is significant. The mechanism of dysfunction is thought related to diffuse axonal injury that occurs from the sustained acceleration and deceleration inertial forces associated with mtbi (16), and rarely are findings noted on computed tomography or magnetic resonance imaging. Microscopic findings reveal the Wallerian-type axonal degeneration. Data from motor vehicles collisions indicate that the threshold average velocity for severe diffuse axonal injury is 15 miles/hr (17), a speed that can easily be reproduced in sports or other activities such as bicycling, as in this case study. Reports of vestibular testing following mild traumatic brain injury are intriguing, but variations in the definition of mtbi and in the vestibular testing performed makes interpretation challenging. Gottshall (18) used active Dynamic Visual Acuity Testing (DVAT) in combination with the Dizziness Handicap Index (DHI) as an outcome measure in mtbi subjects, and concluded that the combination was useful in assisting providers with recommendations for activities such as returning to work. However, further work from the same author suggests that acute vestibular dysfunction as measured with active DVAT and Computerized Dynamic Posturography (CDP) was not an independent predictor of work status at twelve months (19). Others (20) have raised concerns that the results of active DVAT can give false negative findings, as active head movements can generate both compensatory and anticipatory saccades. 9
10 Marzo (21) found that of 12 mtbi patients tested, five had abnormalities noted on CDP, typically condition 5 and 6, three had caloric weakness and two had central findings on electronystagmography. Of the six who underwent rotary chair testing, none were abnormal. Hoffer (22) also performed post mtbi vestibular testing, and used it to help define three posttraumatic classifications: positional vertigo which did not have abnormality on vestibular testing; migraine associated dizziness (PTMAD) which had vestibulo-ocular reflex (VOR) gain, phase, or symmetry abnormalities, high frequency VOR gain abnormalities, and normal CDP; spatial disorientation which had VOR gain, phase, or symmetry abnormalities, high frequency VOR gain abnormalities, and abnormal CDP, and central findings on visual vestibulo-ocular reflex or visual fixation abnormalities or videonystagmography (VNG) testing. Both the PTMAD and the spatial disorientation mtbi groups had a mid frequency (0.32 and 0.64 Hz) phase shift on SHA, with several in both groups showing an abnormally low gain in the mid frequency range. After 6 to 8 weeks of vestibular therapy, 84% of those with PTMAD had improvement in VOR, only 27% in the spatial disorientation mtbi group. At 6 months post injury, the subject had continued complaints of fatigue and diplopia, which are well documented chronic complaints typical in mtbi(1). Initially, the subject had significant changes in OKN, Saccades, Spontaneous, HTT, SHA, and SVV/SVH testing, suggestive of both central and peripheral injuries. Over time, CW OKN returned to baseline and the spontaneous nystagmus resolved. However, SVV and SVH, tests of otolith function OKN, HTT, and SHA at six months had not returned to baseline, supporting the possibility of persistent peripheral and central deficits. While a case report, 10
11 the findings with this subject support a more aggressive vestibular evaluation of patients with mtbi for both the purpose of clinical investigation, and clinical management. 11
12 References 1. National Center for Injury Prevention and Control. Report to Congress on Mild Traumatic Brain Injury in the United States: Steps to Prevent a Serious Public Health Problem. Atlanta, GA: Centers for Disease Control and Prevention; Kraus JF, Fife D, Cox P, et al. Incidence, severity and external causes of pediatric brain injury. Am J Dis Child 1986;140: American Congress of Rehabilitation Medicine. Definition of mild traumatic brain injury. Head Trauma Rehabil 1993;8: Binder LM. A review of mild head trauma. II. Clinical implications. J Clin Exp Neuropsychol 1997;19:3: Levin H, Mattis S, Ruff RM. Neurobehavioral outcome following minor head injury: a three-center study. J Neurosurg 1987;66: Gronwall D, Wrightson P. Cumulative effects of concussion. Lancet 1975;2: Alves WM, Colohan AR, O Leary TJ, et al. Understanding post-traumatic symptoms after minor head injury. J Head Trauma Rehabil 1986;1: Cicerone KD, Kalmar K. Does premorbid depression influence post-concussive symptoms and neuropsychological functioning? Brain Injury 1997;11: , 9. Whitney SL, Rossi MM. Efficacy of vestibular rehabilitation. Otolaryngol Clin North Am 2000;33:3; Alves WM, Colohan AR, O Leary TJ, et al. Understanding post-traumatic symptoms after minor head injury. J Head Trauma Rehabil 1986;1: Wright SC. Case report: post concussion syndrome after minor head injury. Aviat Space Environ Med 1998;69:
13 12. Evans RW. The post concussion syndrome and the sequelae of mild head injury. Neurol Clin 1992;10: U.S. Consumer Product Safety Commission, Office of Compliance, Requirements for Bicycle Helmets, 16 C.F.R. Parts Neuro Kinetics, Inc, Neuro-Otologic Test Center, User Manual, Section 2 Operations, Dimitri PS, Wall C 3rd, Oas JG. Classification of human rotation test results using parametric modeling and multivariate statistics. Acta Otolaryngol 1996;116: Meythaler JM, Peduzzi JD, Eleftheriou E, Novack TA. Current concepts: diffuse axonal injury-associated traumatic brain injury. Arch Phys Med Rehabil 2001;82: Lorenzo L, Mirdamadi M, Fennesy-Ketola K, Barbat SD, Jeong H-Y, Prasad P, et al. Improving head impact protection. Automot Eng 1996:104: Gottshall K, Drake A, Gray N, McDonald E, Hoffer ME. Objective vestibular tests as outcome measures in head injury patients. Laryngoscope 2003;113: Gottshall KR, Gray NL, Drake AI, Tejidor R, Hoffer ME, McDonald EC. To investigate the influence of acute vestibular impairment following mild traumatic brain injury on subsequent ability to remain on activity duty 12 months later. Mil Med 2007;172: Black RA, Halmagyi GM, Thurtell MJ, Todd MJ, Curthoys IS. The active headimpulse test in unilateral peripheral vestibulopathy. Arch Neurol 2005;62:
14 21. Marzo SJ, Leonetti JP, Raffin MJ, Letarte P. Diagnosis and management of posttraumatic vertigo. Laryngoscope 2004;114: Hoffer ME, Gottshall KR, Moore R, Balough BJ, Wester D. Characterizing and treating dizziness after mild head trauma. Otol Neurotol 2004;25:
15 Figure 1. OKN (20 deg/sec) Velocity Gain Four days after the accident the subject s OKN gain diminished for CCW rotation from 0.94 before injury to 0.3 and from 1 to 0.74 for CW rotation with asymmetry increased from 3% to 48%. Approximately 2 weeks after injury gain on CCW increased and CW decreased until asymmetry became less than 20%. Gain on both sides then started to increase with CW continuing to lead CCW. Eight weeks after accident OKN gain became close to pre-accident level (0.96 vs. 1.0 CW, 4% below pre-accident testing, and 0.77 vs CCW, 18% below pre-accident testing). 15
16 Figure 2. OKN (40 deg/sec) Velocity Gain The subject s OKN gain diminished on CW rotation from 0.75 before injury to 0.34 (4 days after accident) and from 0.73 to 0.15 on CCW rotation. Asymmetry 4 days after accident was 41%. The trend shows that after approximately 4 weeks gain on CCW started to increase and follow CW. Eleven weeks after accident gain normalized (0.75 versus 0.75 on CW and 0.62 versus 0.73 on CCW, 15% below pre-injury testing). 16
17 Figure 3. OKN (60 deg/sec) Velocity Gain Four days after accident subject s OKN gain diminished on CW rotation from 0.54 before injury to 0.4 and there was no response from CCW. The first response from CCW was noted after 2 weeks and was 0.23 versus 0.53 before accident. At that time the CW gain decreased to 0.2. Both directions continued to increase, with the CW direction leading the CCW. 17
18 Figure 4. Spontaneous Nystagmus, Horizontal and Vertical Gaze Four days after accident it was recorded that subject had spontaneous left beating nystagmus in primary position and gaze right/left (vision denied) and right beating nystagmus in gaze up/down. Maximum average slow phase velocity of 2.27 deg/sec during gaze up. No beats of spontaneous nystagmus had been observed before accident. By three weeks after accident, the spontaneous nystagmus resolved. 18
19 Figure 5. Subjective Visual Vertical (SVV) and Subjective Visual Horizontal (SVH) Four days after accident it was recorded that result of SVV and SVH testing became abnormal: SVV increased from -0.4 deg before accident to deg and SVH increased from -0.3 deg before accident to +3.6 deg. By eight weeks after accident SVV and SVH returned to normal. 19
20 Figure 6. Head Thrust Test Head Thrust Test at approximately 2 weeks after accident showed reduced gain for CCW (referenced to patient) thrusts (0.51) and CW (0.81) with asymmetry of Before the accident CCW and CW gain was near 1.0. Four weeks after accident, asymmetry remained with CCW gain reduced compared to CW gain. Overall gains at six months were still lower than before accident. 20
21 Figure 7. Percentage of Peak Velocity for Right Eye Horizontal Saccades At 8 weeks after accident, percentage of peak eye velocity below the normal range was increased from 0% before accident to 66% for right eye moving right and from 22% to 81% for right eye moving left. 21
22 Figure 8. Percentage of Peak Velocity for Left Eye Horizontal Saccades At 8 weeks after accident, percentage of peak eye velocity below the normal range was increased from 16% to 68% for left eye moving left and from 22% to 70% for left eye moving right. 22
23 Table 1. Date, Time and Tests Completed Date Time OKN SN,GHV SVV,SVH HTT L S R S SHA 4/11/ * * * 4/15/ * * * * * 4/21/ * * * * 4/24/ * * 4/25/ * * * * 4/28/ * * * * * * 5/01/ * * * * 5/13/ * * * * * 5/16/ * * * * * * * 6/3/ * * 6/4/ * * * * * 6/23/ * * * * * 7/10/ * * * * Time recorded in 24 hour format at start of test session. OKN=optokinetics; SN, GHV= spontaneous nystagmus, horizontal and vertical gaze (vision denied); SVV, SVH= subjective visual vertical and subjective visual horizontal testing; HTT= head thrust test, L S= left eye saccade testing; R S= right eye saccade testing; SHA= sinusoidal harmonic acceleration testing. 23
Attention & Memory Deficits in TBI Patients. An Overview
 Attention & Memory Deficits in TBI Patients An Overview References Chan, R., et.al.. (2003). Are there sub-types of attentional deficits in patients with persisting post- concussive symptoms? A cluster
Attention & Memory Deficits in TBI Patients An Overview References Chan, R., et.al.. (2003). Are there sub-types of attentional deficits in patients with persisting post- concussive symptoms? A cluster
TBI TRAUMATIC BRAIN INJURY WITHIN THE MILITARY/VETERAN POPULATION
 TBI TRAUMATIC BRAIN INJURY WITHIN THE MILITARY/VETERAN POPULATION What is TBI? An external force that disrupts the normal function of the brain. Not all blows or jolts to the head result in a TBI. The
TBI TRAUMATIC BRAIN INJURY WITHIN THE MILITARY/VETERAN POPULATION What is TBI? An external force that disrupts the normal function of the brain. Not all blows or jolts to the head result in a TBI. The
Handicap after acute whiplash injury A 1-year prospective study of risk factors
 1 Handicap after acute whiplash injury A 1-year prospective study of risk factors Neurology 2001;56:1637-1643 (June 26, 2001) Helge Kasch, MD, PhD; Flemming W Bach, MD, PhD; Troels S Jensen, MD, PhD From
1 Handicap after acute whiplash injury A 1-year prospective study of risk factors Neurology 2001;56:1637-1643 (June 26, 2001) Helge Kasch, MD, PhD; Flemming W Bach, MD, PhD; Troels S Jensen, MD, PhD From
SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY
 J Rehabil Med 2005; 37: 137 141 SPECIAL REPORT SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Lena Holm, 1,2 J. David Cassidy, 3 Linda J. Carroll 4 and
J Rehabil Med 2005; 37: 137 141 SPECIAL REPORT SUMMARY OF THE WHO COLLABORATING CENTRE FOR NEUROTRAUMA TASK FORCE ON MILD TRAUMATIC BRAIN INJURY Lena Holm, 1,2 J. David Cassidy, 3 Linda J. Carroll 4 and
Concussion/MTBI Certification Series. Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University
 Concussion/MTBI Certification Series Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University Please note that spaces are limited for this specialty certification program.
Concussion/MTBI Certification Series Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University Please note that spaces are limited for this specialty certification program.
What is a concussion? What are the symptoms of a concussion? What happens to the brain during a concussion?
 What is a concussion? The working definition used today for concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces (developed by the consensus
What is a concussion? The working definition used today for concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces (developed by the consensus
Traumatic brain injury (TBI), caused either by blunt force or acceleration/
 Traumatic Brain Injury (TBI) Carol A. Waldmann, MD Traumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons
Traumatic Brain Injury (TBI) Carol A. Waldmann, MD Traumatic brain injury (TBI), caused either by blunt force or acceleration/ deceleration forces, is common in the general population. Homeless persons
BINSA Information on Mild Traumatic Brain Injury
 Mild traumatic brain injuries (MTBI) occur through sporting, car and workplace accidents. Mild brain injury is not easily diagnosed. This fact sheet explains how it may be recognised and assessed, and
Mild traumatic brain injuries (MTBI) occur through sporting, car and workplace accidents. Mild brain injury is not easily diagnosed. This fact sheet explains how it may be recognised and assessed, and
Skate Australia Concussion Guidelines
 Skate Australia Concussion Guidelines Introduction Forces strong enough to cause concussion are common in all roller sports. Even though helmets are worn in most disciplines, the risk of concussion is
Skate Australia Concussion Guidelines Introduction Forces strong enough to cause concussion are common in all roller sports. Even though helmets are worn in most disciplines, the risk of concussion is
Concussion Management Program for Red Bank Catholic High School Athletic Department
 Concussion Management Program for Red Bank Catholic High School Athletic Department *This document should be used as a framework for a successful concussion management program but is not intended to replace
Concussion Management Program for Red Bank Catholic High School Athletic Department *This document should be used as a framework for a successful concussion management program but is not intended to replace
A PEEK INSIDE A CLOSED HEAD INJURY CLAIM... 1
 A PEEK INSIDE A CLOSED HEAD INJURY CLAIM By: Douglas Fletcher Fernando Fred Arias Dr. Jim Hom April 11, 2014 CONTENTS A PEEK INSIDE A CLOSED HEAD INJURY CLAIM... 1 SYMPTOMATOLOGY... 2 CRITICAL INFORMATION...
A PEEK INSIDE A CLOSED HEAD INJURY CLAIM By: Douglas Fletcher Fernando Fred Arias Dr. Jim Hom April 11, 2014 CONTENTS A PEEK INSIDE A CLOSED HEAD INJURY CLAIM... 1 SYMPTOMATOLOGY... 2 CRITICAL INFORMATION...
Concussions and Mild Head Injury. Post Concussion Syndrome. Whiplash Injuries
 Concussions and Mild Head Injury Post Concussion Syndrome Whiplash Injuries Treat the cause, not just the symptoms NeuroSensory Center of Eastern Pennsylvania 250 Pierce Street, Suite 317 Kingston, PA
Concussions and Mild Head Injury Post Concussion Syndrome Whiplash Injuries Treat the cause, not just the symptoms NeuroSensory Center of Eastern Pennsylvania 250 Pierce Street, Suite 317 Kingston, PA
Traumatic Brain Injury and Incarceration. Objectives. Traumatic Brain Injury. Which came first, the injury or the behavior?
 Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Traumatic Brain Injury and Incarceration Which came first, the injury or the behavior? Barbara Burchell Curtis RN, MSN Objectives Upon completion of discussion, participants should be able to Describe
Early Response Concussion Recovery
 Early Response Concussion Recovery KRISTA MAILEY, BSW RSW, CONCUSSION RECOVERY CONSULTANT CAREY MINTZ, PH.D., C. PSYCH., PRACTICE IN CLINICAL NEUROPSYCHOLOGY FOR REFERRAL: Contact Krista Mailey at (204)
Early Response Concussion Recovery KRISTA MAILEY, BSW RSW, CONCUSSION RECOVERY CONSULTANT CAREY MINTZ, PH.D., C. PSYCH., PRACTICE IN CLINICAL NEUROPSYCHOLOGY FOR REFERRAL: Contact Krista Mailey at (204)
Recovering from a Mild Traumatic Brain Injury (MTBI)
 Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Brain Injury Litigation Today
 MILD TRAUMATIC BRAIN INJURY PAPER 3.1 Brain Injury Litigation Today These materials were prepared by Joseph E. Murphy, QC, of Murphy Battista LLP, Vancouver, BC, for the Continuing Legal Education Society
MILD TRAUMATIC BRAIN INJURY PAPER 3.1 Brain Injury Litigation Today These materials were prepared by Joseph E. Murphy, QC, of Murphy Battista LLP, Vancouver, BC, for the Continuing Legal Education Society
Introduction to Dizziness and the Vestibular System
 Introduction to Dizziness and the Vestibular System David R Friedland, MD, PhD Professor and Vice-Chairman Chief, Division of Otology and Neuro-otologic Skull Base Surgery Chief, Division of Research Department
Introduction to Dizziness and the Vestibular System David R Friedland, MD, PhD Professor and Vice-Chairman Chief, Division of Otology and Neuro-otologic Skull Base Surgery Chief, Division of Research Department
Primary Motor Pathway
 Understanding Eye Movements Abdullah Moh. El-Menaisy, MD, FRCS Chief, Neuro-ophthalmology ophthalmology & Investigation Units, Dhahran Eye Specialist Hospital, Dhahran, Saudi Arabia Primary Motor Pathway
Understanding Eye Movements Abdullah Moh. El-Menaisy, MD, FRCS Chief, Neuro-ophthalmology ophthalmology & Investigation Units, Dhahran Eye Specialist Hospital, Dhahran, Saudi Arabia Primary Motor Pathway
A Parent s Guide to Choosing a Sports Concussion Specialist Brain Injury Alliance of New Jersey Concussion in Youth Sports Committee
 A Parent s Guide to Choosing a Sports Concussion Specialist Brain Injury Alliance of New Jersey Concussion in Youth Sports Committee The following is a guideline for parents to use when choosing a sports
A Parent s Guide to Choosing a Sports Concussion Specialist Brain Injury Alliance of New Jersey Concussion in Youth Sports Committee The following is a guideline for parents to use when choosing a sports
NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion
 NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion Introduction Concussion is an important injury for the professional football player, and the diagnosis, prevention,
NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion Introduction Concussion is an important injury for the professional football player, and the diagnosis, prevention,
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY
 NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
Neuropsychological Assessment in Sports-Related Concussion: Part of a Complex Puzzle
 Neuropsychological Assessment in Sports-Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
Neuropsychological Assessment in Sports-Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
The Indiana Trial Lawyer Association s Lifetime Achievement Seminar. Honoring Peter L. Obremsky. May 23-24, 2005
 The Indiana Trial Lawyer Association s Lifetime Achievement Seminar Honoring Peter L. Obremsky May 23-24, 2005 The Use of Medical Literature in the Brain Injury Case Thomas C. Doehrman Doehrman-Chamberlain
The Indiana Trial Lawyer Association s Lifetime Achievement Seminar Honoring Peter L. Obremsky May 23-24, 2005 The Use of Medical Literature in the Brain Injury Case Thomas C. Doehrman Doehrman-Chamberlain
Brain Injury Litigation. Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com
 Brain Injury Litigation Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com Some General Facts About Traumatic Brain Injury TBIs contribute to a substantial number of deaths and
Brain Injury Litigation Peter W. Burg Burg Simpson Eldredge Hersh & Jardine, P.C. www.burgsimpson.com Some General Facts About Traumatic Brain Injury TBIs contribute to a substantial number of deaths and
A comparison of complaints by mild brain injury claimants and other claimants describing subjective experiences immediately following their injury
 Archives of Clinical Neuropsychology 16 (2001) 689 695 A comparison of complaints by mild brain injury claimants and other claimants describing subjective experiences immediately following their injury
Archives of Clinical Neuropsychology 16 (2001) 689 695 A comparison of complaints by mild brain injury claimants and other claimants describing subjective experiences immediately following their injury
Department of Defense INSTRUCTION. DoD Policy Guidance for Management of Mild Traumatic Brain Injury/Concussion in the Deployed Setting
 Department of Defense INSTRUCTION NUMBER 6490.11 September 18, 2012 USD(P&R) SUBJECT: DoD Policy Guidance for Management of Mild Traumatic Brain Injury/Concussion in the Deployed Setting References: See
Department of Defense INSTRUCTION NUMBER 6490.11 September 18, 2012 USD(P&R) SUBJECT: DoD Policy Guidance for Management of Mild Traumatic Brain Injury/Concussion in the Deployed Setting References: See
Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi.
 Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi. Suresh Kumar, M.D. AUTHOR Director of: Neurology & Headaches Center Inc. Neurocognitve &TBI Rehabilitation Center
Montreal Cognitive Assessment (MoCA) as Screening tool for cognitive impairment in mtbi. Suresh Kumar, M.D. AUTHOR Director of: Neurology & Headaches Center Inc. Neurocognitve &TBI Rehabilitation Center
Post-Concussion Syndrome
 Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Defined as a complex process affecting the brain, induced by traumatic biomechanical forces.
 Concussion Protocol Defined as a complex process affecting the brain, induced by traumatic biomechanical forces. May be caused by a direct blow to the head, face, neck or elsewhere on the body with force
Concussion Protocol Defined as a complex process affecting the brain, induced by traumatic biomechanical forces. May be caused by a direct blow to the head, face, neck or elsewhere on the body with force
TYPE OF INJURY and CURRENT SABS Paraplegia/ Tetraplegia
 Paraplegia/ Tetraplegia (a) paraplegia or quadriplegia; (a) paraplegia or tetraplegia that meets the following criteria i and ii, and either iii or iv: i. ii. iii i. The Insured Person is currently participating
Paraplegia/ Tetraplegia (a) paraplegia or quadriplegia; (a) paraplegia or tetraplegia that meets the following criteria i and ii, and either iii or iv: i. ii. iii i. The Insured Person is currently participating
Integrated Neuropsychological Assessment
 Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Traumatic Brain Injury in Young Athletes. Andrea Halliday, M.D. Oregon Neurosurgery Specialists
 Traumatic Brain Injury in Young Athletes Andrea Halliday, M.D. Oregon Neurosurgery Specialists Variability in defining concussion Lack of reliable biomarkers for concussions Reliance on subjective system
Traumatic Brain Injury in Young Athletes Andrea Halliday, M.D. Oregon Neurosurgery Specialists Variability in defining concussion Lack of reliable biomarkers for concussions Reliance on subjective system
Neuropsychological Assessment in Sports- Related Concussion: Part of a Complex Puzzle
 Neuropsychological Assessment in Sports- Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
Neuropsychological Assessment in Sports- Related Concussion: Part of a Complex Puzzle Jillian Schuh, PhD 1, 2, John Oestreicher, PhD 1, & Linda Steffen, PsyD 1 1 Catalpa Health 2 Department of Neurology,
The Petrylaw Lawsuits Settlements and Injury Settlement Report
 The Petrylaw Lawsuits Settlements and Injury Settlement Report TRAUMATIC BRAIN INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Brain Injury Cases The Petrylaw Lawsuits Settlements
The Petrylaw Lawsuits Settlements and Injury Settlement Report TRAUMATIC BRAIN INJURIES How Minnesota Juries Decide the Value of Pain and Suffering in Brain Injury Cases The Petrylaw Lawsuits Settlements
Traumatic brain injury (TBI)
 Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
Traumatic brain injury (TBI) A topic in the Alzheimer s Association series on understanding dementia. About dementia Dementia is a condition in which a person has significant difficulty with daily functioning
A patient guide to mild traumatic brain injury
 A patient guide to mild traumatic brain injury Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
A patient guide to mild traumatic brain injury Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Mild head injury: How mild is it?
 Mild head injury: How mild is it? Carly Dutton; Gemma Foster & Stephen Spoors Sunderland and Gateshead Community Acquired Brain Injury Service (CABIS), Northumberland, Tyne and Wear NHS Foundation Trust
Mild head injury: How mild is it? Carly Dutton; Gemma Foster & Stephen Spoors Sunderland and Gateshead Community Acquired Brain Injury Service (CABIS), Northumberland, Tyne and Wear NHS Foundation Trust
Internuclear ophthalmoplegia: recovery and plasticity
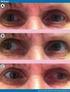 Internuclear ophthalmoplegia: recovery and plasticity M. J. Doslak, L. B. Kline, L. F. Dell'Osso, and R. B. Daroff We studied refixational eye movements of a patient during the gradual resolution of an
Internuclear ophthalmoplegia: recovery and plasticity M. J. Doslak, L. B. Kline, L. F. Dell'Osso, and R. B. Daroff We studied refixational eye movements of a patient during the gradual resolution of an
CONCUSSION AND HEAD INJURY AWARENESS POLICY TRAINING C I T Y O F S O U T H J O R D A N 9 / 2 0 1 1
 CONCUSSION AND HEAD INJURY AWARENESS POLICY TRAINING C I T Y O F S O U T H J O R D A N 9 / 2 0 1 1 UTAH STATE LEGISLATION 2011 General Legislative Session House Bill 204: Enacts the Protection of Athletes
CONCUSSION AND HEAD INJURY AWARENESS POLICY TRAINING C I T Y O F S O U T H J O R D A N 9 / 2 0 1 1 UTAH STATE LEGISLATION 2011 General Legislative Session House Bill 204: Enacts the Protection of Athletes
Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury. Canadian Family Physician
 Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury 1 Canadian Family Physician Volume 32, September 1986 Arthur Ameis, MD Dr. Ames practices physical medicine and rehabilitation,
Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury 1 Canadian Family Physician Volume 32, September 1986 Arthur Ameis, MD Dr. Ames practices physical medicine and rehabilitation,
Objectives. Definition. Epidemiology. The journey of an athlete
 Sport Concussion Chantel Debert MD MSc FRCPC CSCN Physical Medicine and Rehabilitation Department of Clinical Neurosciences Hotchkiss Brain Institute, University of Calgary Objectives Definition Epidemiology
Sport Concussion Chantel Debert MD MSc FRCPC CSCN Physical Medicine and Rehabilitation Department of Clinical Neurosciences Hotchkiss Brain Institute, University of Calgary Objectives Definition Epidemiology
General Disclaimer (learned from Dr. Melhorn)
 Mild Traumatic Brain Injury: Postconcussion Syndrome, Persistent Posttraumatic Headache, etc. Robert J. Barth, Ph.D. Chattanooga, TN and Birmingham, AL General Disclaimer (learned from Dr. Melhorn) All
Mild Traumatic Brain Injury: Postconcussion Syndrome, Persistent Posttraumatic Headache, etc. Robert J. Barth, Ph.D. Chattanooga, TN and Birmingham, AL General Disclaimer (learned from Dr. Melhorn) All
Traumatic Brain Injury Lawsuit
 Traumatic Brain Injury Lawsuit D Legal Guide Simple Step-By-Step Guide to Your Brain & Traumatic Brain Injury (TBI) [Type text] Distributed By: www.downtownlalw.com A Simple Step-by-Step Guide to your
Traumatic Brain Injury Lawsuit D Legal Guide Simple Step-By-Step Guide to Your Brain & Traumatic Brain Injury (TBI) [Type text] Distributed By: www.downtownlalw.com A Simple Step-by-Step Guide to your
Advanced Clinical Solutions. Serial Assessment Case Studies
 Advanced Clinical Solutions Serial Assessment Case Studies Advanced Clinical Solutions Serial Assessment Case Studies Case Study 1 Client C is a 62-year-old White male who was referred by his family physician
Advanced Clinical Solutions Serial Assessment Case Studies Advanced Clinical Solutions Serial Assessment Case Studies Case Study 1 Client C is a 62-year-old White male who was referred by his family physician
Concussion Guidance for the General Public
 CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
Ronald G. Riechers, II, M.D. Medical Director, Polytrauma Team Cleveland VAMC Assistant Professor Department of Neurology Case Western Reserve
 Ronald G. Riechers, II, M.D. Medical Director, Polytrauma Team Cleveland VAMC Assistant Professor Department of Neurology Case Western Reserve University The opinions or assertions contained herein are
Ronald G. Riechers, II, M.D. Medical Director, Polytrauma Team Cleveland VAMC Assistant Professor Department of Neurology Case Western Reserve University The opinions or assertions contained herein are
Concussion Management Return to Play Protocol
 Concussion Management Return to Play Protocol Returning to play following a concussion involves a stepwise progression once the individual is symptom free. There are many risks to premature return to play
Concussion Management Return to Play Protocol Returning to play following a concussion involves a stepwise progression once the individual is symptom free. There are many risks to premature return to play
Cognitive Rehabilitation of Blast Traumatic Brain Injury
 Cognitive Rehabilitation of Blast Traumatic Brain Injury Yelena Bogdanova, PhD VA Boston Healthcare System Rehabilitation Research & Development Boston University School of Medicine IOM Committee on Cognitive
Cognitive Rehabilitation of Blast Traumatic Brain Injury Yelena Bogdanova, PhD VA Boston Healthcare System Rehabilitation Research & Development Boston University School of Medicine IOM Committee on Cognitive
INTERNATIONAL RUGBY BOARD Putting players first
 Summary Principles Concussion must be taken extremely seriously to safeguard the long term welfare of Players. Players suspected of having concussion must be removed from play and must not resume play
Summary Principles Concussion must be taken extremely seriously to safeguard the long term welfare of Players. Players suspected of having concussion must be removed from play and must not resume play
V OCATIONAL E CONOMICS, I NC.
 V OCATIONAL E CONOMICS, I NC. This document was downloaded from Vocational Economics Inc. (www.vocecon.com). For more information on this document, visit: www.vocecon.com/articles/arttbi.htm DEFINING VOCATIONAL
V OCATIONAL E CONOMICS, I NC. This document was downloaded from Vocational Economics Inc. (www.vocecon.com). For more information on this document, visit: www.vocecon.com/articles/arttbi.htm DEFINING VOCATIONAL
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Test Request Tip Sheet
 With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136. Days and Hours: Monday Friday 8:30a.m. 6:00p.m. (305) 355 9028 (JMH, Downtown)
 UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
UNIVERSITY OF MIAMI, LEONARD M. MILLER SCHOOL OF MEDICINE CLINICAL NEUROPSYCHOLOGY UHEALTH PSYCHIATRY AT MENTAL HEALTH HOSPITAL CENTER 1695 N.W. 9th Avenue, Suite 3302H Miami, FL. 33136 Days and Hours:
NEW TRENDS AND ISSUES IN NEUROPSYCHOLOGY: Mild Traumatic Brain Injury and Postconcussive Syndrome Cases
 NEW TRENDS AND ISSUES IN NEUROPSYCHOLOGY: Mild Traumatic Brain Injury and Postconcussive Syndrome Cases Carl F. Mariano Barry H. Uhrman Introduction to Neuropsychology As many of you are aware, clinical
NEW TRENDS AND ISSUES IN NEUROPSYCHOLOGY: Mild Traumatic Brain Injury and Postconcussive Syndrome Cases Carl F. Mariano Barry H. Uhrman Introduction to Neuropsychology As many of you are aware, clinical
DECISION NO. 1708/10
 B. Kalvin WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1708/10 BEFORE: B. Kalvin : Vice-Chair HEARING: September 9, 2010 at Toronto Oral DATE OF DECISION: September 15, 2010 NEUTRAL CITATION:
B. Kalvin WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 1708/10 BEFORE: B. Kalvin : Vice-Chair HEARING: September 9, 2010 at Toronto Oral DATE OF DECISION: September 15, 2010 NEUTRAL CITATION:
The Role of Physical Therapy in Post Concussion Management. Non Disclosure
 The Role of Physical Therapy in Post Concussion Management. Cook Children s Sports Medicine Symposium Ryan Blankenship, PT, SCS Non Disclosure No conflicts of interest. 1 Course Objectives Participants
The Role of Physical Therapy in Post Concussion Management. Cook Children s Sports Medicine Symposium Ryan Blankenship, PT, SCS Non Disclosure No conflicts of interest. 1 Course Objectives Participants
Head Injury. Dr Sally McCarthy Medical Director ECI
 Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
Head Injury Dr Sally McCarthy Medical Director ECI Head injury in the emergency department A common presentation 80% Mild Head Injury = GCS 14 15 10% Moderate Head Injury = GCS 9 13 10% Severe Head Injury
IF IN DOUBT, SIT THEM OUT.
 IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: Grassroots sport and general public Modified from World Rugby s Guidelines on Concussion Management for the General Public Introduction The
IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: Grassroots sport and general public Modified from World Rugby s Guidelines on Concussion Management for the General Public Introduction The
Michael J. Sileo, MD. Orthopedic Associates of Long Island (OALI)
 Michael J. Sileo, MD Orthopedic Associates of Long Island (OALI) ! Jeremy Thode, AD! Center Moriches BOE ! Safety of our student-athletes is our Number 1 concern! NYS is now forcing our hand " Referees
Michael J. Sileo, MD Orthopedic Associates of Long Island (OALI) ! Jeremy Thode, AD! Center Moriches BOE ! Safety of our student-athletes is our Number 1 concern! NYS is now forcing our hand " Referees
LAW: THE PAEDIATRIC PERSPECTIVE
 LAW: THE PAEDIATRIC PERSPECTIVE More than one million Canadian and American children sustain traumatic brain injuries (TBI) each year. Many of these injuries occur in traumatic events e.g., motor vehicle,
LAW: THE PAEDIATRIC PERSPECTIVE More than one million Canadian and American children sustain traumatic brain injuries (TBI) each year. Many of these injuries occur in traumatic events e.g., motor vehicle,
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic
 Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Overview of evidence: Prognostic factors following whiplash injury
 Overview of evidence: Prognostic factors following whiplash injury Confidence in conclusions (that an association exists) are presented in both text and graphical format, using the following legend: =
Overview of evidence: Prognostic factors following whiplash injury Confidence in conclusions (that an association exists) are presented in both text and graphical format, using the following legend: =
HANDLING NON-CATASTROPHIC BRAIN INJURY CASES
 HANDLING NON-CATASTROPHIC BRAIN INJURY CASES WE VE LEARNED THAT THE BRAIN IS MORE PLASTIC THAN WE ONCE THOUGHT AND THAT DAMAGE CAN COM FROM ITS MOVEMENT WITHIN THE SKULL AFTER A BLOW TO THE HEAD OR TO
HANDLING NON-CATASTROPHIC BRAIN INJURY CASES WE VE LEARNED THAT THE BRAIN IS MORE PLASTIC THAN WE ONCE THOUGHT AND THAT DAMAGE CAN COM FROM ITS MOVEMENT WITHIN THE SKULL AFTER A BLOW TO THE HEAD OR TO
AR159 February 9, 2015
 AR159 February 9, 2015 1.0 PURPOSE AR CONCUSSION PROTOCOL The purpose of this protocol is to provide information regarding the prevention, identification and management of concussions. Everyone has a role
AR159 February 9, 2015 1.0 PURPOSE AR CONCUSSION PROTOCOL The purpose of this protocol is to provide information regarding the prevention, identification and management of concussions. Everyone has a role
Symptoms following mild head injury:
 200 20ournal of Neurology, Neurosurgery, and Psychiatry 1992;55:200-204 Symptoms following mild head injury: expectation as aetiology Wiley Mittenberg, Diane V DiGiulio, Sean Perrin, Anthony E Bass Nova
200 20ournal of Neurology, Neurosurgery, and Psychiatry 1992;55:200-204 Symptoms following mild head injury: expectation as aetiology Wiley Mittenberg, Diane V DiGiulio, Sean Perrin, Anthony E Bass Nova
3. Overview: The next 8 pages contain the concussion management algorithms guiding garrison medical care at the time of injury to 7 days.
 ATTACHMENT 2 (CONCUSSION MANAGEMENT IN THE GARRISON SETTING ALGORITHMS) TO HQDA EXORD DA GUIDANCE FOR MANAGEMENT OF CONCUSSION/MILD TRAUMATIC BRAIN INJURY IN THE GARRISON SETTING 1. General: Implementation
ATTACHMENT 2 (CONCUSSION MANAGEMENT IN THE GARRISON SETTING ALGORITHMS) TO HQDA EXORD DA GUIDANCE FOR MANAGEMENT OF CONCUSSION/MILD TRAUMATIC BRAIN INJURY IN THE GARRISON SETTING 1. General: Implementation
Cognitive Assessment and Rehabilitation in mtbi Patients. Shannon E. Auxier, MS CCC-SLP Judy M. Mikola, PhD CCC-SLP
 Cognitive Assessment and Rehabilitation in mtbi Patients Shannon E. Auxier, MS CCC-SLP Judy M. Mikola, PhD CCC-SLP Disclaimer The views expressed in this presentation are those of the presenters and do
Cognitive Assessment and Rehabilitation in mtbi Patients Shannon E. Auxier, MS CCC-SLP Judy M. Mikola, PhD CCC-SLP Disclaimer The views expressed in this presentation are those of the presenters and do
Whiplash injuries can be visible by functional magnetic resonance imaging. Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp.
 Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY
 Traumatic brain injury EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY Traumatic brain injury (TBI) is a common neurological condition that can have significant emotional and cognitive consequences.
Traumatic brain injury EMOTIONAL AND BEHAVIOURAL CONSEQUENCES OF HEAD INJURY Traumatic brain injury (TBI) is a common neurological condition that can have significant emotional and cognitive consequences.
mtbi Concussion, Post Concussion Syndrome and mtbi
 mtbi Concussion, Post Concussion Syndrome and mtbi Barry Willer PhD bswiller@buffalo.edu Immediate Symptoms Secondary Symptoms Cognitive Issues Ideally with Baseline Understanding Persistent Symptoms
mtbi Concussion, Post Concussion Syndrome and mtbi Barry Willer PhD bswiller@buffalo.edu Immediate Symptoms Secondary Symptoms Cognitive Issues Ideally with Baseline Understanding Persistent Symptoms
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
Sport Concussion in New Zealand ACC National Guidelines
 Sport Concussion in New Zealand ACC National Guidelines This guideline document has been produced to inform National Sports Organisations (NSOs), and recreation, education and health sectors in their development
Sport Concussion in New Zealand ACC National Guidelines This guideline document has been produced to inform National Sports Organisations (NSOs), and recreation, education and health sectors in their development
Pediatric Vestibular Assessment for Children Who Are Deaf or Hard of Hearing
 Kristen Janky, Au.D., Ph.D., CCC-A Vestibular Audiologist Vestibular Services, Clinical Coordinator Pediatric Vestibular Assessment for Children Who Are Deaf or Hard of Hearing Kristen Janky Au.D., Ph.D.,
Kristen Janky, Au.D., Ph.D., CCC-A Vestibular Audiologist Vestibular Services, Clinical Coordinator Pediatric Vestibular Assessment for Children Who Are Deaf or Hard of Hearing Kristen Janky Au.D., Ph.D.,
THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL
 THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL AFL Research board AFL MEDICAL OFFICERS' ASSOCIATION THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL This document has been published by the AFL
THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL AFL Research board AFL MEDICAL OFFICERS' ASSOCIATION THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL This document has been published by the AFL
TBI Global Synapse Town Hall: Your TBI Information Connection
 Today s webinar is: TBI Global Synapse Town Hall: Your TBI Information Connection Nov. 20, 2013, 2:30-4 p.m. (EST) Moderator: Alison Cernich, Ph.D., ABPP Deputy Director Defense Centers of Excellence for
Today s webinar is: TBI Global Synapse Town Hall: Your TBI Information Connection Nov. 20, 2013, 2:30-4 p.m. (EST) Moderator: Alison Cernich, Ph.D., ABPP Deputy Director Defense Centers of Excellence for
United States Department of Labor Employees Compensation Appeals Board DECISION AND ORDER
 United States Department of Labor C.B., Appellant and DEPARTMENT OF VETERANS AFFAIRS, VETERANS HEALTH ADMINISTRATION, Lexington, KY, Employer Appearances: Joshua S. Harp, Esq., for the appellant Office
United States Department of Labor C.B., Appellant and DEPARTMENT OF VETERANS AFFAIRS, VETERANS HEALTH ADMINISTRATION, Lexington, KY, Employer Appearances: Joshua S. Harp, Esq., for the appellant Office
Concussion: Sideline Assessment
 Concussion: Sideline Assessment Damion A. Martins, MD Director, Orthopedics & Sports Medicine Program Director, Sports Medicine Fellowship - Atlantic Health System Director of Internal Medicine - New York
Concussion: Sideline Assessment Damion A. Martins, MD Director, Orthopedics & Sports Medicine Program Director, Sports Medicine Fellowship - Atlantic Health System Director of Internal Medicine - New York
B U R T & D A V I E S PERSONAL INJURY LAWYERS
 TRANSPORT ACCIDENT LAW - TRAUMATIC BRAIN INJURY Traumatic Brain Injury ( TBI ) is a common injury in transport accidents. TBI s are probably the most commonly undiagnosed injuries in a hospital setting.
TRANSPORT ACCIDENT LAW - TRAUMATIC BRAIN INJURY Traumatic Brain Injury ( TBI ) is a common injury in transport accidents. TBI s are probably the most commonly undiagnosed injuries in a hospital setting.
GAZE STABILIZATION SYSTEMS Vestibular Ocular Reflex (VOR) Purpose of VOR Chief function is to stabilize gaze during locomotion. Acuity declines if
 GAZE STABILIZATION SYSTEMS Vestibular Ocular Reflex (VOR) Purpose of VOR Chief function is to stabilize gaze during locomotion. Acuity declines if slip exceeds 3-5 deg/sec. Ex: Head bobbing and heel strike
GAZE STABILIZATION SYSTEMS Vestibular Ocular Reflex (VOR) Purpose of VOR Chief function is to stabilize gaze during locomotion. Acuity declines if slip exceeds 3-5 deg/sec. Ex: Head bobbing and heel strike
Recovery From Mild Concussion in High School Athletes Journal of Neurosurgery 2003;98:295-301
 Lovell MR, Collins MW, Iverson G, Field M, Maroon JC, Cantu R, Podell K, Powell JW, Belza M, Fu FH. Recovery from mild concussion in high school athletes. Journal of Neurosurgery 2003;98295-301;2003. Recovery
Lovell MR, Collins MW, Iverson G, Field M, Maroon JC, Cantu R, Podell K, Powell JW, Belza M, Fu FH. Recovery from mild concussion in high school athletes. Journal of Neurosurgery 2003;98295-301;2003. Recovery
A GUIDE TO IN RUGBY UNION
 A GUIDE TO The aim of this brochure is to provide information on concussion to those involved in rugby union in Ireland. Concussion MUST be taken extremely seriously. Any player with a suspected concussion
A GUIDE TO The aim of this brochure is to provide information on concussion to those involved in rugby union in Ireland. Concussion MUST be taken extremely seriously. Any player with a suspected concussion
Diagnostic Tests for Vestibular Problems By the Vestibular Disorders Association
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Diagnostic Tests for Vestibular Problems By the Vestibular Disorders Association The inner ear
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG WWW.VESTIBULAR.ORG Diagnostic Tests for Vestibular Problems By the Vestibular Disorders Association The inner ear
EARLY RECOVERY FOR persons with significant TBI is
 ORIGINAL ARTICLE Patterns of Recovery of Posttraumatic Confusional State in Neurorehabilitation Admissions After Traumatic Brain Injury Mark Sherer, PhD, Stuart A. Yablon, MD, Risa Nakase-Richardson, PhD
ORIGINAL ARTICLE Patterns of Recovery of Posttraumatic Confusional State in Neurorehabilitation Admissions After Traumatic Brain Injury Mark Sherer, PhD, Stuart A. Yablon, MD, Risa Nakase-Richardson, PhD
Concussion Rates per Sport
 PSE4U UNIT 1: SPORTS-RELATED HEAD INJURIES DUE DATE: LATE PENALTY (-5% PER WEEK): K/U T/I C A FINAL MARK 10 10 10 32 62 PART A: BRAINSTORMING [T/I /10] [C /10] 1.) Construct a mind-map: research the amount
PSE4U UNIT 1: SPORTS-RELATED HEAD INJURIES DUE DATE: LATE PENALTY (-5% PER WEEK): K/U T/I C A FINAL MARK 10 10 10 32 62 PART A: BRAINSTORMING [T/I /10] [C /10] 1.) Construct a mind-map: research the amount
Cognitive Functioning in TBI Patients: A Review of Literature
 Middle-East Journal of Scientific Research 3 (3): 120-125, 2008 ISSN 1990-9233 IDOSI Publications, 2008 Cognitive Functioning in TBI Patients: A Review of Literature Divya Upadhyay Research fellow, Centre
Middle-East Journal of Scientific Research 3 (3): 120-125, 2008 ISSN 1990-9233 IDOSI Publications, 2008 Cognitive Functioning in TBI Patients: A Review of Literature Divya Upadhyay Research fellow, Centre
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL
 BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy. Spine Volume 21(16) August 15, 1996, pp 1877-1883
 Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
Nonoperative Management of Herniated Cervical Intervertebral Disc With Radiculopathy 1 Spine Volume 21(16) August 15, 1996, pp 1877-1883 Saal, Joel S. MD; Saal, Jeffrey A. MD; Yurth, Elizabeth F. MD FROM
EYE-TRAC Advance. A research study funded by the Department of Defense
 EYE-TRAC Advance A research study funded by the Department of Defense BROCHURE CONTENTS About BTF..................................................... 1 Eye-Trac Advance Overview....................................1
EYE-TRAC Advance A research study funded by the Department of Defense BROCHURE CONTENTS About BTF..................................................... 1 Eye-Trac Advance Overview....................................1
63rd Legislature AN ACT CREATING THE DYLAN STEIGERS PROTECTION OF YOUTH ATHLETES ACT; PROMOTING
 63rd Legislature SB0112 AN ACT CREATING THE DYLAN STEIGERS PROTECTION OF YOUTH ATHLETES ACT; PROMOTING SAFETY FOR YOUTH ATHLETES; PROVIDING DEFINITIONS; REQUIRING EACH SCHOOL DISTRICT TO ADOPT A POLICY
63rd Legislature SB0112 AN ACT CREATING THE DYLAN STEIGERS PROTECTION OF YOUTH ATHLETES ACT; PROMOTING SAFETY FOR YOUTH ATHLETES; PROVIDING DEFINITIONS; REQUIRING EACH SCHOOL DISTRICT TO ADOPT A POLICY
Head Injury in Children
 Head Injury in Children The worst fear of every parent is to receive news that your child has been injured in an accident. Unfortunately, in our society, accidental injuries have become the leading threat
Head Injury in Children The worst fear of every parent is to receive news that your child has been injured in an accident. Unfortunately, in our society, accidental injuries have become the leading threat
Vestibular Assessment
 Oculomotor Examination A. Tests performed in room light Vestibular Assessment 1. Spontaneous nystagmus 2. Gaze holding nystagmus 3. Skew deviation 4. Vergence 5. Decreased vestibular ocular reflex i. Head
Oculomotor Examination A. Tests performed in room light Vestibular Assessment 1. Spontaneous nystagmus 2. Gaze holding nystagmus 3. Skew deviation 4. Vergence 5. Decreased vestibular ocular reflex i. Head
8 th Annual W/C Spine Summit. Ted A. Lennard, MD Feb. 12, 2015
 8 th Annual W/C Spine Summit Ted A. Lennard, MD Feb. 12, 2015 Case Study 45 y.o. male Truck Accident on 1/15/12 Slid on ice and crossed median. Case Study Taken by ambulance to ER in Texas +Loss of consciousness
8 th Annual W/C Spine Summit Ted A. Lennard, MD Feb. 12, 2015 Case Study 45 y.o. male Truck Accident on 1/15/12 Slid on ice and crossed median. Case Study Taken by ambulance to ER in Texas +Loss of consciousness
RECOVERY IN THE FIRST YEAR AFTER MILD HEAD INJURY: DIVERGENCE OF SYMPTOM STATUS AND SELF-PERCEIVED QUALITY OF LIFE
 J Rehabil Med 2007 Preview ORIGINAL REPORT RECOVERY IN THE FIRST YEAR AFTER MILD HEAD INJURY: DIVERGENCE OF SYMPTOM STATUS AND SELF-PERCEIVED QUALITY OF LIFE Marcus H. Heitger 1,2, Richard D. Jones 1,2,
J Rehabil Med 2007 Preview ORIGINAL REPORT RECOVERY IN THE FIRST YEAR AFTER MILD HEAD INJURY: DIVERGENCE OF SYMPTOM STATUS AND SELF-PERCEIVED QUALITY OF LIFE Marcus H. Heitger 1,2, Richard D. Jones 1,2,
Assessment and Treatment of Cognitive Impairment after Acquired Brain Injury
 Assessment and Treatment of Cognitive Impairment after Acquired Brain Injury Dr Brian O Neill, D.Clin.Psy. Brain Injury Rehabilitation Trust, Glasgow Honorary Research Fellow, University of Stirling Brain
Assessment and Treatment of Cognitive Impairment after Acquired Brain Injury Dr Brian O Neill, D.Clin.Psy. Brain Injury Rehabilitation Trust, Glasgow Honorary Research Fellow, University of Stirling Brain
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Assessment and Management of Visual Dysfunction Associated with Mild Traumatic Brain Injury. Clinical Recommendation Overview
 Assessment and Management of Visual Dysfunction Associated with Mild Traumatic Brain Injury Clinical Recommendation Overview Learning Objectives Describe an overview of visual dysfunction associated with
Assessment and Management of Visual Dysfunction Associated with Mild Traumatic Brain Injury Clinical Recommendation Overview Learning Objectives Describe an overview of visual dysfunction associated with
Functions of the Brain
 Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
