Aesthetic Value of Immediately Loaded Immediate Post-extraction Implants
|
|
|
- Reynard Burns
- 8 years ago
- Views:
Transcription
1 2 EDI A retrospective assessment of the performance of implants in obtaining the essential initial stability Aesthetic Value of Immediately Loaded Immediate Post-extraction Implants Matteo Danza, MD 1, Tania Sinderowsky 2, Francesco Carinci 3 and Professor Stefano Fanali 4 The field of implantology is continually evolving. New indications are established and existing ones updated, new components and systems are constantly being introduced, and on top of all this, patients have rising expectations of ever earlier function. We are increasingly asked to solve aesthetic problems involving the anterior maxilla, where we need to be very careful to balance the possibility of obtaining an excellent result in a shorter time against our responsibility to minimize the risk of unnecessary failure. It is very satisfying to both patient and practitioner to be able to replace an extracted tooth immediately with an implant-supported restoration that reproduces its shape, size and function. The international literature is full of studies which provide the foundations for our everyday clinical practice, and which support us in deciding to load an implant that has just been placed in a fresh extraction socket. This approach disrupts the local anatomical and physical situation by forcing both hard and soft tissues to follow our intentions. 1 Dental School, University of Chieti, Italy 2 Maxillofacial surgeon, free professional in Tel Aviv 3 Maxillofacial Surgery, University of Ferrara, Italy 4 Head of the Department of Odontostoma - tologia II, University of Chieti, Italy For some time now, a team from our institute has been working with implants placed in post-extraction sockets. A team from the G. D Annunzio University Oral Medicine Clinic, Chieti (director: Professor Stefano Fanali), analyzed the clinical and radiological behaviour of implants placed at different times after extraction, i.e. immediate, early delayed and late delayed placement, with bone regeneration where necessary. The most striking conclusion was that the most successful implants were those placed immediately after extraction [1]. The most likely reason is that the surgical procedure probably disturbs the spatial distribution of the forces generated by the dental root that ensure the crucial vascularization of the alveolar ridge, but we do not completely interrupt its function as it is immediately restored, albeit in a different form, when an implant is placed in the extraction site.
2 EDI 3 This article offers a retrospective assessment of the performance of the Spiral and Spiral Flare Bevel (SFB) implants (Alpha-Bio Implant Ltd., Petah Tikva, Israel) in obtaining the essential initial stability that is a minimum and sufficient condition for obtaining osseointegration in immediate post-extraction implants subjected to immediate loading. Post-extraction implants Although the validity, predictability and high success rate of this implant placement method have been recognized in many articles published over the last few years [2], the method has not yet been formally recognized as being equal to other methods used in traditional protocols. Many of our colleagues take a defensive approach, regarding the technique as a dangerous simplification of the traditional method because of the relative difficulty in obtaining initial stability and the large number of cases in which further bone regeneration is required to fill a gap between socket and implant. However, in spite of this the method continues to be used successfully and has been studied in many leading centres all over the world. Recently, the University of Tübingen (Germany) published a very interesting study in the International Journal of Oral and Maxillofacial Implants, the leading journal in the field of osseointegration, presenting six-year follow-up data for 124 Frialit implants inserted in post-extraction sockets. Sixtyeight percent of the implants supported single-tooth restorations. The survival rate was 99% after the first year, dropping to 97% after six years in function [3]. Other studies have compared immediate postextraction implantation with conventional implantation. A team from Tel Aviv University placed 380 implants, 117 (31%) of which were placed using an immediate post-extraction method, while the other 263 were placed in mature bone using a conventional method. Five-year survival rate was 96% for implants in the first group and 89.4% for implants in the second group. The study results showed that in the critical part of the maxilla, the posterior maxilla, the five-year cumulative survival rate (CSR) was 100% for immediate post-extraction implants and 72% for those placed using a traditional protocol [4]. It is now well recognized that immediate postextraction implantation preserves maxillary anatomy and maintains bone morphology; a large number of clinical studies on this subject have reported a high level of success, but none of them has ever included histological analysis of implants placed in post-extraction sockets without filling material or membrane. In November 2001, our university (Chieti) published an interesting study in which 48 patients received at least one post-extraction implant, in symmetrical quadrants, in addition to other implants inserted using a conventional protocol. The study was carried out without the use of filling materials or membranes, just a flap repositioned coronally to obtain primary wound closure. After six months, the implants inserted by the post-extraction method were removed and the sections were examined histologically. In particular, the percentage of boneimplant contact was measured. There were no statistically significant differences in clinical, radiographic or histological parameters between the two groups of implants. It was concluded that although no bone regeneration had been used, there was no difference in the degree of osseointegration between the two groups of implants when the bone-implant gap was less than 2 mm [5]. Immediate loading In edentulous patients, fixed implant-supported restorations can have a very high success rate, if implants are allowed to heal without loading for three to six months. Many published data have shown that this type of restoration can be successful for many years [6, 7]. The disadvantage of the procedure is that the patient has to wear a full provisional denture for several months, as a healing period of three to six months is recommended after the teeth have been extracted and implants placed, before any loading is applied to the implants. The patient cannot wear any kind of denture for at least two weeks after the procedure. A further disadvantage of using a full denture after the extractions is that existing papillae are flattened [8]. In 1977, Schnittman and Tarnow [9, 10] suggested that full dentures could usefully be dispensed with during the implantation process. In patients who have lost all their teeth from periodontal disease and who intend to have an implantsupported fixed restoration, a temporary restoration placed immediately onto post-extraction implants would be an even greater benefit. Many published studies have shown that implants inserted immediately after dental extraction can have a similar success rate to that of implants placed in healed sites [11-19]. For immediate implants, a success rate of more than 95% may be expected. Many studies have now been published confirming that excellent results can be obtained with immediate loading of both edentulous arches [9, 10, 15, 17] and individual teeth [18, 19] although in the latter case the immediate loading was not functional
3 4 EDI loading as the provisional restorations were not functional. True functional immediate loading takes place only in edentulous arches; this concept has been validated over time with bar-retained implantsupported overdentures. Examples of fixed restorations on implants in edentulous mandibles have been widely reported in the literature. In similar cases, Randow and co-workers [20] reported a 100% success rate in 16 patients in whom implants were placed and then immediately subjected to early loading. Five or six implants (minimum length 10 mm) were placed in each of the 16 patients between the mental foramina and then loaded with a fixed superstructure bilaterally extending to include the second premolar. The follow-up for this study lasted 18 months. In Loma Linda University (California), Rungcharassaeng and co-workers [21] confirmed the high success rate of this treatment method and confirmed that it is a valid and predictable option, provided that the prerequisites of careful patient selection and case planning are complied with. Gatti, Helfinger and Chiapasco (2000) assessed immediate loading in mandibular overdentures with ITI implants placed between the mental foramina, obtaining an identical success rate (96%) after three years of follow-up to that for conventional delayed loading [22]. Piattelli and co-workers analyzed bone reaction to early loading (two weeks) around plasma sprayed implants in cynomolgus monkeys. Histological study showed that high percentages of bone-implant contact can be obtained with this implant placement protocol [23]. Testori and co-workers carried out a histological study of two Osseotite (3i) immediately-loaded implants which were sampled four months after loading. Histological and morphometric analysis confirmed a high percentage of bone-implant contact (85%) [24]. Horiuchi and co-workers studied immediate loading with Brånemark implants with a screw-retained provisional metal-reinforced resin prosthesis in 140 implants placed in an 8 to 24 month period [25]. The criterion for loading was a placement torque of 40 Ncm or more; implants with a lower placement torque or implants that required bone grafting were submerged. The success rate was 97.2%. Similar percentages (95%) were obtained by Jaffin, Kumar and Barman with implants that were loaded immediately (within 72 hours) with reinforced resin provisionals. Inclusion criteria were adequate bone volume and density for a minimum of four (10 mm diameter or greater) implants in the mandible, and six in the maxilla. In this study, fewer sandblasted/ acid-etched implants were lost than machined implants [26]. In 2001, Grunder carried out a comprehensive study and reported results for 91 implants, 66 of which were inserted immediately after extraction in the post-extraction sockets and all of which were loaded immediately [8]. No bone grafting or membranes were used in any of the 66 post-extraction sites, despite the fact that in many cases there were gaps between the implant surface and the post-extraction parietal alveolar bone. It is very interesting to review the different treatment strategies used for implants that are not in contact with bone, especially in singlestage surgery. The classic approach is that good bone-implant contact at the height of the first thread is needed for good long-term results. Nir-Hadar and co-workers [27] showed that with the submerged method, when there was a gap between implant and bone, there was a strong tendency for pre-implant defects to fill with bone in both the horizontal and vertical planes, up to the cover screw. These results were based mainly on clinical observations. Akimoto and co-workers [28] showed that when the submerged implant method was used without bone regeneration, the bone-implant gap filled with new bone. As the gap widened, the amount of boneimplant contact decreased. When the initial gap was 1.35 mm, there was a very low amount of boneimplant contact. Brunel and co-workers [29] carried out a careful study of bone regeneration methods combined with post-extraction implant placement in beagle dogs. In the control group, defects between 2.5 and 4.00 mm were left untreated and 50% of the implants failed. In both treatment groups, failure rates were 30% when hydroxyapatite was used to fill the gap and 0% when a collagen membrane was applied, alone or in combination with hydroxyapatite. Implants in the control group that had been successful without any additional treatment had a better level of bone-implant contact. The study concluded that the use of bioabsorbable materials slightly increases osseointegration when used in conjunction with the immediate placement of non-submerged implants. In the Grunder study [8], implant failures did not appear to be related to gaps between the coronal part of the implant and the bone. Gaps were present in all implant sites but all the failures occurred in the posterior region. These failures were therefore related to implant location. Six out of seven implants had been positioned in the posterior maxilla, and five of these were between 8.5 and 10 mm long [30, 31]. In the Grunder study, the main cause of failure was poor bone
4 EDI 5 Fig. 1 Radiographic appearance of the incisor at the first visit. 1 2 Fig. 2 Clinical appearance of 21. Fig. 3 Detail of previous photo. 3 4 Fig. 4 Broken coronal fragment and the extracted root fragment. quality (100% of implant failures were in type IV bone). Other causes of failure were provisional restorations without metal reinforcement in patients with bruxism, and imperfectly seated abutments. In this study, initial stability was achieved in 100% of cases, and for this reason alone, treatment could be considered successful. The global success rate of 92.31% after 24 months may be acceptable. It was not possible to demonstrate that implant surface had any positive effect, as there was no control group. Success rates could certainly have been higher if patients had been selected more carefully, by enrolling patients with good bone quality and volume in the posterior maxilla. The conclusions of the Grunder study were that functional loading with immediate post-extraction implants for fixed restorations of complete arches, without the use of bone substitutes or barrier membrane, could be successful over a two-year period. Immediate loading of post-extraction implants: case histories Case history 1 A 25-year-old patient came to our clinic wanting to solve the aesthetic and functional problems caused by his left upper central incisor. From the history, it emerged that the tooth had suddenly had a traumatic oblique fracture a few years earlier, which was treated endodontically with fracture union obtained using a bonding method (Fig. 1). The patient reported that he had had to reattach the fragment on a number of occasions and now felt it was unstable; the fragment was also slightly extruded and had migrated vestibularly. His major concern was the disfiguring aesthetic result if the tooth was removed. Physical examination showed the crown of tooth 21 with clear discoloration, slight extrusion and slight mobility (Figs. 2 and 3). The treatment plan involved removal of the fragment followed by intraoperative assessment of the treatment options, i.e. fabrication of a post and core for an all-ceramic crown, if the clinical situation would allow this, or alternatively, extraction of the fractured tooth and immediate replacement with an implant-supported crown. The patient signed a standard informed consent form and accepted the treatment plan. At the next visit, the coronal fragment was removed and after examining the fragment and the fracture margins (Fig. 4), we decided on extraction and replacement with an immediate post-extraction implant. The fragment was extracted atraumatically with the usual care required in these situations to preserve the integrity of the alveolar cortex and to encourage predictable bone regeneration around the coronal portion of the implant and long-term survival for the post-extraction implants [32, 33]. The root fragment was therefore carefully luxated; toothextraction forceps were only used after the fragment had been mobilized.
5 6 EDI 5 6 Fig. 5 SFB implant. Fig. 6 Angle of palatal axis. 7a 7b Fig. 7a Prosthetically determined positioning of the implant head... Fig. 7b... with 0 Paraguide system. 7c 7d Fig. 7c... with 15 Paraguide system. Fig. 7d... with 25 Paraguide system. After careful curettage, the socket was washed with saline and the site was prepared for implant placement through the extraction socket, without any incision of the soft tissues. The implant chosen for this type of restoration was a Spiral Flare Bevel (SFB) implant, Alpha-Bio. The implant has special features in the form of a tapered neck and NanoTec surface treatment, which make it possible to obtain a thicker layer of well vascularized, keratinized tissue around the implant neck (Fig. 5). The implant site was prepared using the palatal wall of the socket and native alveolar bone for 3 to 4 mm beyond the apex of the extracted tooth, in order to achieve the crucial initial stability. The osteotomy was started on the palatal wall of the extraction site using a 2-mm round bur, under copious irrigation with saline. Once this initial step had been completed we were able to use the series of rotary instruments specified for the operative procedure, in order, along the palatal preparation axis cut by the first drill (Fig. 6). A 6 x 13 mm SFB implant was inserted in the first part of the prepared socket along the direction set by the rotary instruments, but the first three to four threads were hardly engaged when it had to be redirected vestibularly by a gradual levering action using a manual insertion instrument (surgical screwdriver). Correcting the implant axis during insertion meant that the implant head emerged in a prosthetically ideal position without compromising the vestibular bone wall, resorption of which could have caused dangerous recession of the soft tissues, especially in a thin periodontal biotype (Figs. 7a to d) [34].
6 EDI 7 Figs. 8a and b Straight abutment connected immediately to implant. 8a 8b Fig. 8c Abutment prepared intra orally. 8c Fig. 9 The provisional crown has just been put in place. Note the flapless technique and the absence of sutures Fig. 10 General view in centric occlusion. The implant head was positioned 3 mm apically, at the future gingival margin. The height of the soft tissues determines the dimension available for the emergence profile and for the maintenance of a sufficiently deep peri-implant sulcus to ensure the long-term health of the peri-implant soft tissues. The gap between the implant and the vestibular wall was not filled by bone grafting, as this is not necessary if the width of the gap is less than 2 mm [5]. We used the ParaGuide system which adjusts the parallelism of the implant and is an extremely useful guide when choosing the ideal prosthetic abutment (Figs. 7a to d); we chose a preformed straight abutment which was connected immediately to the implant and modified immediately in position, using special multi-blade diamond burs for titanium (Figs. 8a to c). An acrylic resin temporary crown prepared beforehand was rebased and cemented provisionally to the abutment that had just been placed (Fig. 9). Occlusion was checked very carefully in view of the patient s overbite, and the optimum provisional crown occlusion was obtained, with light centric contact and no contact in the lateral excursions (Fig. 10). The patient was discharged with the usual instructions to continue taking the antibiotic (amoxicillin 1 g twice daily) for a further five days, practice careful oral hygiene, rinse twice a day with 0.12% chlorhexidine mouthwash and avoid biting or tearing at food so as not to overload the new dental implant.
7 8 EDI Fig. 11 Postoperative radiograph a 12b Figs. 12a and b Radiographic and clinical appearance eight days after the procedure. 13a 13b Figs. 13a to d Healing of soft tissues two months after the procedure and follow-up radiograph. 13c 13d Postoperative intraoral radiograph showed that all the factors involved had been addressed and the implant-crown assembly had integrated very well into the patient s actual anatomy (Fig. 11). The postoperative course was uneventful, with no complications. The patient returned for a check-up eight days later and reported that he had not had any problems. At this visit, the appearance of the soft tissues was excellent (Figs. 12a and b). The patient s good oral health continued to improve; at a check-up two months later, the clinical and radiographic appearances were very encouraging, and an alginate impression was taken to make an individual impression tray (Figs. 13a to d). Soft-tissue healing, clinical situation and radio - graphic appearance of the result when the definitive abutment and the all-ceramic crown were tried-in were all excellent, and all the features for which we had chosen the SFB implant were found to be very satisfactory (Figs. 14a to e). They could also be confirmed radiographically (Figs. 15 and 16). The intimate contact between implant and surrounding bone tissue is clearly visible on the radio - graphs. The healthy state of the implant and its osseointegration had a direct effect on the soft tissues overlying the emerging implant structures. The interproximal papillae were perfectly preserved with the colour and stroma resembling those of a natural tooth.
8 EDI 9 Figs. 14a to e Stages in gradual tissue maturation. 14a 14b 14c 14d 14e Fig. 15 Radiograph at time of abutment try-in. Fig. 16 Radiograph at time of try-in of the crown. This vascularization of the peri-implant soft tissues is probably related to the special profile and reverse taper of the SFB implant neck, as these features deliver a larger amount of inter-implant alveolar bone from which the vascular system can support the papillae. The vascularization requirement of the periimplant soft tissues should always be borne in mind when planning implant-supported restorations. To allow adequate organization of the connective tissue and the supracrestal epithelial tissue, the inter-implant space (or the distance between abutments, whether natural or alloplastic) should be at least 3 mm to provide a sufficiently wide base for the shape and the projection of the papilla for harmonious development of the profile and structure [1]. The maintenance of a healthy peri-implant mucosal seal over time depends on both prevention of sepsis and the ability to satisfy the morphological and anatomical requirements for establishing a suitable vascular support for the connective tissue stroma of the inter-implant papillae, to ensure the maximum vitality and reactivity of the tissue itself and the epithelium covering it. Placing implants too close to each other or excessively close to contiguous natural elements reduces the amount of space left for the papilla, leading to the development of narrow and elongated papillae with less vascularization and increased susceptibility
9 10 EDI 17a 17b Figs. 17a and b Laboratory photo: Implant and all-ceramic crown, ready for the try-in. 18a 18b Figs. 18a to e Stages in completion of the procedure. 18c 18d 18e to any microbial insult. This leads to a certain degree of instability in the mucosal seal, with more apical reorganization of all of the tissues that contribute to the biological width (peri-implant bone, supracrestal connective tissue and junctional epithelium). The SFB implant appears to have the characteristics needed to satisfy these requirements. At the next visit a week later we placed the prosthetic abutment obtained by adapting a prefabricated provisional abutment, with the characteristic golden colour of the transmucosal neck obtained by excessive oxidation of titanium (Figs. 17a and b). At the next check-up a few days later, the definitive fabricated crown was placed (Figs. 18a to e).
10 EDI 11 Fig. 1 Initial patient ortho - pantomogram. 1 2 Fig. 2 Baseline clinical situation. Fig. 3 Tissues after root extraction. 3 4 Fig. 4 Small access flap for optimum positioning of the more distal implant. Fig. 5 Post-extraction placement of NT Certain implants inserted immediately at sites 25 and Fig. 6 Healing abutments positioned for suturing. Fig. 7 Repositioning of the flap around the healing abutments using Dr Palacci s interimplant papilla regeneration method. Case history 2 This was a 76-year-old woman who came to our clinic with a fractured bridge in the second quadrant (25-27). The patient s main concern was to avoid having to wear a removable partial denture. Her general dental health was excellent. She was offered a prosthetic implant solution in the form of post-extraction placement of two implants at sites 25 and 26 (Figs. 1 and 2). The patient reviewed the treatment plan and signed a standard informed consent form. On the day scheduled for surgery, the patient took 3 g of amoxicillin one hour before the procedure and rinsed with a 0.2% chlorhexidine solution for two minutes. The two root fragments were extracted in accordance with the protocol for delicate and minimally invasive surgery [32]. First of all, we performed a delicate syndesmotomy, then luxated and elevated the 7 root fragments. Particular care was taken to preserve the vestibular cortical bone, which is thin and delicate and very important for preventing vestibular bone recession (Figs. 3 and 4). At the same visit as the extractions, two Osseotite NT Certain (3i) implants (5 x 13 mm and 5 x 11.5 mm) were inserted after careful modification of the postextraction sockets (Figs. 5 to 7).
11 12 EDI 8 9 Fig. 8 Healing of soft tissues and excellent state of health of the two implants. Fig. 9 Reproduction of the soft tissues in the laboratory Fig. 10 Abutments. Fig. 11 Trying-in the abutments Fig. 12 Lined provisional crown. Fig. 13 Follow-up radiograph. Fig. 14 Radiograph after replacement of the distal implant. After placement, the implants were connected to healing abutments to allow accurate repositioning of the flap and so obtain the aesthetic results that the patient wanted, using Dr Palacci s papilla regeneration technique [35]. The postoperative period was uncomplicated. Healing of the peri-implant soft tissues clearly testified to the excellent state of health of both implants (Fig. 8), and about two months after placement they were fitted with prosthetic abutments and gradually loaded with an acrylic resin provisional crown (Figs. 9 to 12). When we were taking the transfer coping impression, about 40 days after loading, we realized that the most distal implant (26) had lost stability, which was confirmed with radiographs showing transparent haloes around the implant (Fig. 13). The implant was removed and replaced at the same visit with a 6 x 11.5 mm Alfa Bio SFB implant, changing its orientation and recording its position with an intra-operative impression (Fig. 14).
12 EDI 13 Fig. 15 Intraoperative view Fig. 16 Provisional crowns after adjustment. Fig. 17 Follow-up radio graph after crowns have been fitted Fig. 18 Abutments connected to implants. Fig. 19 Definitive ceramic crowns. 19 Figs. 20 to 22 Follow-up radio - graphs taken after fitting of definitive crowns, three months and six months after loading A 25 pre-angled abutment was placed on the implant that had just been inserted, and the provisional resin crown was trimmed to fit (Figs. 15 and 16). A week later, the second definitive abutment was connected and the two ceramic crowns were placed (Figs. 17 to 19). Control radiographs taken after the prosthetic work had been completed and three and six months after loading confirmed the healthy status and excellent osseointegration of the implants (Figs. 20 to 22). Results for the SFB implant inserted using an immediate post-extraction method and subjected to immediate loading were very encouraging at the time of writing. This type of procedure generally needs to be followed-up later.
13 14 EDI 1 2 Fig. 1 Initial clinical appearance. Fig. 2 Initial radiographic appearance. Fig. 3 Implant in position. 3 4 Fig. 4 The preformed abutment has just been adjusted and connected to the implant using gentle torque of 15 Ncm on the fixation screw. 5 6 Fig. 5 The acrylic resin temporary crown manu factured in the laboratory prior to implant insertion, based on a diagnostic wax-up; it has been trimmed and cemented with provisional cement. 7 Case history 3 A 20-year-old woman came to our clinic for extraction of an impacted third molar (48); tooth 46 had been extracted the previous week because of untreatable root caries. The patient, an aspiring actress, said that she had heard that treatment times were very long for implant-supported restoration after a single tooth has been extracted. We suggested surgical extraction of the impacted tooth and immediate placement of a post-extraction implant at position 46 with immediate loading, with a treatment plan giving a much shorter time for solving the problem. The patient accepted our treatment plan and signed a standard informed consent form. Clinical and radiographic examination clearly showed the recent extraction of 46 (Figs. 1 and 2). It was decided to use the distal socket for insertion of a 6 x 13 mm SPI implant (Alpha-Bio), because this was the implant that would give the best emergence profile. We performed an incision distal to site 47 to allow access to the third molar. The incision went around site 47 intracrevicularly and continued along the middle of the crest to the edentulous region in order to open the margins of the residual alveolar wound, which had not yet re-epithelialized, and to expose the post-extraction socket, which was still fresh. Fig. 6 The procedure is concluded by suturing both the third molar extraction region and the implant region. Fig. 7 Follow-up radio - graph shows intimate contact between the implant and the surrounding bone tissue.
14 EDI 15 Fig. 8 Healing of the soft tissues around the immediately placed provisional crown shows the beneficial effect of immediate loading on vascularization. 8 9 Fig. 9 Complete integration of the implant abutment with the tissues has sculpted the gingival contour Figs. 10 and 11 Gingival walls at the emergence site. Fig. 12 Abutment. Fig. 13 Definitive allceramic crown Fig. 14 Enlargement of previous image. The distal socket chosen for implant placement was modified and optimized by the use of increasing diameter drills, as described in the standard Alpha-Bio surgical protocol, so that an SPI implant could be inserted (Fig. 3). The implant was seated in the distal socket, achieving excellent initial stability, which allowed us to continue with immediate provisionalization. The residual lingual and vestibular gaps were small enough not to require grafting with biomaterials. A titanium abutment from the catalogue range was connected at the same visit as the post-extraction implant was inserted, making it possible to load the implant immediately with an acrylic resin provisional crown, to contribute to soft tissue management (Figs. 4 to 7). The rule of light centric occlusion and no contact in the lateral excursions was complied with. About two months later, the soft tissues appeared healthy, and we took an impression of the implant 14 position. Figures 8 to 14 clearly illustrate the excellent results obtained with the SPI implant using the method described (Alpha-Bio). The prosthetic work was completed using a wide platform abutment (see Fig. 12) and an all-ceramic crown (Figs. 15 and 16). All stages from insertion to fitting of the crown were monitored radiographically. The images show the stages described (Figs. 17 to 20).
15 16 EDI Figs. 15 and 16 Laboratory images of the crown Fig. 17 Follow-up radio - graph of inserted implant. Fig. 18 Radiograph after two months of healing Fig. 19 Radiograph to check abutment connection. Fig. 20 Follow-up radio - graph of abutment connection. Conclusions This article discusses a procedure that is becoming increasingly more predictable and that is now routinely performed by a large number of professionals. There are a number of advantages in using this method: single surgical stage; biological tissue sparing; ease of obtaining initial stability; aesthetic solution to edentulousness; good success rate, found to be around 98% in our population; and better integration of both hard and soft tissues. In fact, from our experience it would appear that immediate loading in itself, and even better, immediate loading of a post-extraction implant, has a marked positive effect on the quality of peri-implant soft tissues. In our patients we have consistently found that periimplant tissue was keratinized, stable, fibrous and free of any trace of inflammation. The cases presented here used SFB and SPI implants (Alpha-Bio), which in these specific applications invariably satisfied the demands placed upon them. They can be used electively for immediate implantation after tooth extraction because of their special features of dual taper profile, high performance self-drilling and self-tapping, gradual increase in diameter and variable thread profile in the apicocoronal direction, which deliver excellent primary stability. A list of references can be found on Contact Address Matteo Danza, MD Via Carducci Pescara ITALY Fax: dama.t@fastwebnet.it
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
IMPLANTS IN FOCUS. Endosseous dental implant restorations PLANNING FOR IMPLANT RESTORATIONS
 IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
IMPLANTS IN FOCUS PLANNING FOR IMPLANT RESTORATIONS Replacing a missing maxillary central incisor with a dental implant can be the most demanding restoration in dentistry, so it s important to consider
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
The SATURN implant by Cortex Dental Industries
 The SATURN implant by Cortex Dental Industries By Dr. Zvi Laster DMD W e P r o v e I t E v e r y D a y A case report using a newly designed implant specifically designed for immediate post-extraction loading
The SATURN implant by Cortex Dental Industries By Dr. Zvi Laster DMD W e P r o v e I t E v e r y D a y A case report using a newly designed implant specifically designed for immediate post-extraction loading
Renaissance of One-Piece Implants
 2 EDI Minimally invasive and patient-friendly treatment concepts using one-piece implants Renaissance of One-Piece Implants Hannes Thurm-Meyer, dentist, Bremen, Germany, Thomas Horn, master dental technician,
2 EDI Minimally invasive and patient-friendly treatment concepts using one-piece implants Renaissance of One-Piece Implants Hannes Thurm-Meyer, dentist, Bremen, Germany, Thomas Horn, master dental technician,
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Implants in your Laboratory: Abutment Design
 1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
1/2 point CDT documented scientific credit. See Page 41. Implants in your Laboratory: Abutment Design By Leon Hermanides, CDT A patient s anatomical limitations have the greatest predictive value for successful
Bone augmentation procedure without wound closure
 THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
THE CREATION OF ATTACHED GINGIVA IMMEDIATELY AFTER EXTRACTION Bone augmentation procedure without wound closure One of the characteristics of wound healing after an extraction is that the alveolar process
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
SCD Case Study. Treatment Considerations for Implant Rehabilitation
 SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration
 Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
Implant Replacement of the Maxillary Central Incisor Utilizing a Modified Ceramic Abutment (Thommen SPI ART) and Ceramic Restoration ROBERT SCHNEIDER, DDS, MS* ABSTRACT The prosthetic restoration of a
CHAPTER 10 RESTS AND PREPARATIONS. 4. Serve as a reference point for evaluating the fit of the framework to the teeth.
 CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
CHAPTER 10 RESTS AND DEFINITIONS A REST is any rigid part of an RPD framework which contacts a properly prepared surface of a tooth. A REST PREPARATION or REST SEAT is any portion of a tooth or restoration
Single anterior tooth replacement: clinical approaches
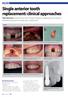 Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
Single anterior tooth replacement: clinical approaches Paul Swanson examines the role of implant design in approaching a range of treatment protocols for replacing a single tooth Case 1 Figure 1: Patient
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
Rehabilitation of a complex case with zirconium dental implants
 Rehabilitation of a complex case with zirconium dental Authors_Dr Andrea Enrico Borgonovo, Dr Marcello Dolci, Dr Rachele Censi, Dr Oscar Arnaboldi, Dr Virna Vavassori & Prof Carlo Maiorana, Italy _Introduction
Rehabilitation of a complex case with zirconium dental Authors_Dr Andrea Enrico Borgonovo, Dr Marcello Dolci, Dr Rachele Censi, Dr Oscar Arnaboldi, Dr Virna Vavassori & Prof Carlo Maiorana, Italy _Introduction
CDT 2015 Code Change Summary New codes effective 1/1/2015
 CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
CDT 2015 Code Change Summary New codes effective 1/1/2015 Code Nomenclature Delta Dental Policy D0171 Re-Evaluation Post Operative Office Visit Not a Covered Benefit D0351 3D Photographic Image Not a Covered
Dental Implant Options in Atrophic Jaws
 Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
Dental Implant Options in Atrophic Jaws Orthopedic Application Jay B. Reznick, D.M.D., M.D. Diplomate, American Board of Oral and Maxillofacial Surgery Tarzana, CA Endopore Dental Implant System Screw-Type
The Mandibular Two-Implant Overdenture First-Choice. Standard of Care for the Edentulous Denture Patient
 The Mandibular Two-Implant Overdenture First-Choice Standard of Care for the Edentulous Denture Patient Joseph R. Carpentieri, DDS Dennis P. Tarnow, DDS ii Preface Preface The prosthetic management of
The Mandibular Two-Implant Overdenture First-Choice Standard of Care for the Edentulous Denture Patient Joseph R. Carpentieri, DDS Dennis P. Tarnow, DDS ii Preface Preface The prosthetic management of
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE
 IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
IMMEDIATE CUSTOM IMPLANT PROVISIONALIZATION: A PROSTHETIC TECHNIQUE Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 5 JUNE Surgical and restorative techniques that can reduce the loss of hard and soft tissues
Prosthodontist s Perspective
 Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Unless otherwise noted, the content of this course material is licensed under a Creative Commons Attribution - Non-Commercial - Share Alike 3.0 License. Copyright 2008, Dr. Jeff Shotwell. The following
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report
 Vol. 34 No. 2, September 2015 Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report Sang-ki Byun, Yung-bin Lee, Woohyun
Vol. 34 No. 2, September 2015 Reconstruction of the anterior maxilla with implants using customized zirconia abutments and all-ceramic crowns: a clinical case report Sang-ki Byun, Yung-bin Lee, Woohyun
Dental Implants and Esthetics
 Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
Dental Implants and Esthetics Charles J. Goodacre, DDS, MSD; Chad J. Anderson, MS, DMD Continuing Education Units: 1 hour Online Course: www.dentalcare.com/en-us/dental-education/continuing-education/ce203/ce203.aspx
2016 Buy Up Dental Care Plan Procedure List
 * This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
* This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
Healing Abutment Selection. Perio Implant Part I. Implant Surface Characteristics. Single Tooth Restorations. Credit and Thanks for Lecture Material
 Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Healing Abutment Selection Perio Implant Part I Credit and Thanks for Lecture Material Implant Surface Characteristics!CAPT Robert Taft!CAPT Greg Waskewicz!Periodontal Residents NPDS and UMN!Machined Titanium!Tiunite!Osseotite
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Ceramics on Implants Fixed Zirconium Dioxide-Based Restorations in the Rehabilitation of the Edentulous upper Jaw
 38 STARGET 1 I 11 ceramic restorations arne F. BOEcklER and MIcHaEl seitz Ceramics on Implants Fixed Zirconium Dioxide-Based Restorations in the Rehabilitation of the Edentulous upper Jaw Introduction
38 STARGET 1 I 11 ceramic restorations arne F. BOEcklER and MIcHaEl seitz Ceramics on Implants Fixed Zirconium Dioxide-Based Restorations in the Rehabilitation of the Edentulous upper Jaw Introduction
Final Result 1 year later. Patient Case 19. Preoperative: Main Complaint:
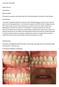 Patient Case 19 Preoperative: Main Complaint: The patient presented to the practice with the 21 that according to her started to move forward. Dental History I have been treating this patient for many
Patient Case 19 Preoperative: Main Complaint: The patient presented to the practice with the 21 that according to her started to move forward. Dental History I have been treating this patient for many
CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT
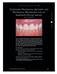 CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
CONTINUING EDUCATION 1 4 CUSTOMIZED PROVISIONAL ABUTMENT AND PROVISIONAL RESTORATION FOR AN IMMEDIATELY-PLACED IMPLANT Gerard J. Lemongello, Jr, DMD* LEMONGELLO 19 7 AUGUST The use of immediate implant
NARROW DIAMETER implant
 ND NARROW DIAMETER implant TABLE OF CONTENTS ND - NARROW DIAMETER implant Implant characteristics page 04 Dental implant page 05 Open Tray Impression Transfer page 06 Titanium Abutments page 07 O-Ball
ND NARROW DIAMETER implant TABLE OF CONTENTS ND - NARROW DIAMETER implant Implant characteristics page 04 Dental implant page 05 Open Tray Impression Transfer page 06 Titanium Abutments page 07 O-Ball
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
Chapter 6 Aesthetical improvement Use of one-piece type implants
 Chapter 6 Aesthetical improvement Use of one-piece type implants 1. Improving esthetics with one-piece implant Director of Kinebuchi Dental Clinic Takao Kinebuchi Aesthetics of two-piece two-stage type
Chapter 6 Aesthetical improvement Use of one-piece type implants 1. Improving esthetics with one-piece implant Director of Kinebuchi Dental Clinic Takao Kinebuchi Aesthetics of two-piece two-stage type
CAD/CAM technology supporting successful implant therapy
 CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
CAD/CAM technology supporting successful implant therapy Suheil M. Boutros, DDS, MS, Manuel Fricke, DT Modern implantology opens up new treatment options for individuals with only minimal or no remaining
B978-0-443-06895-9.00005-8,
 B978-0-443-06895-9.00005-8, 00005 Chapter Restorative management 5 of dental implants 5.1 Basic implant terminology 133 5.2 Planning dental implants 134 5.3 Surgical phases 135 5.4 Provisional and definitive
B978-0-443-06895-9.00005-8, 00005 Chapter Restorative management 5 of dental implants 5.1 Basic implant terminology 133 5.2 Planning dental implants 134 5.3 Surgical phases 135 5.4 Provisional and definitive
Periodontal surgery report for crown lengthening of tooth number 24,25
 411 PDS Periodontal surgery report for crown lengthening of tooth number -Course director : Dr. Nahid Ashri - instructor: Dr.Fatin Awaratani - - Student Name: Hanadi Alyami Computer Number: K S U - D E
411 PDS Periodontal surgery report for crown lengthening of tooth number -Course director : Dr. Nahid Ashri - instructor: Dr.Fatin Awaratani - - Student Name: Hanadi Alyami Computer Number: K S U - D E
Restorative Guidelines
 Restorative Guidelines Contents Restorative Guidelines 4.1 Neoss Implant System 4.2 4.2 Esthetiline Solution 4.3 4.3 Provisional Abutments 4.8 4.4 Impression Techniques Implant Level 4.12 4.5 NeoLink
Restorative Guidelines Contents Restorative Guidelines 4.1 Neoss Implant System 4.2 4.2 Esthetiline Solution 4.3 4.3 Provisional Abutments 4.8 4.4 Impression Techniques Implant Level 4.12 4.5 NeoLink
Treatment planning for the class 0, 1A, 1B dental arches
 Treatment planning for the class 0, 1A, 1B dental arches Dr.. Peter Hermann Dr Reminder: Torquing movement on tooth supported denture : no movement Class 1 movement in one direction (depression) Class
Treatment planning for the class 0, 1A, 1B dental arches Dr.. Peter Hermann Dr Reminder: Torquing movement on tooth supported denture : no movement Class 1 movement in one direction (depression) Class
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Boston College, BS in Biology 1980-1984. University of Southern California, Doctor of Dental Surgery, DDS, 1990.
 CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
CLINICAL CASE REPORT Sinus Augmentation with Immediate Implant insertion Multidisciplinary Approach to Anterior Implant Therapy Immediate Implant after Extraction of Lower Molar Tooth DR. SHERMAN LIN Boston
Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation
 Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
Clinical Histologic comparison of biologic width around teeth versus implants: The effect on bone preservation Kazuto Makigusa 1 Abstract Histological analysis of the biological width surrounding primate
A New Beginning with Dental Implants. A Guide to Understanding Your Treatment Options
 A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
SURGICAL MANUAL. Step By Step Techniques
 SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
SURGICAL MANUAL Step By Step Techniques TABLE OF CONTENTS PRE-SURGICAL 1 8 MEASUREMENT OF BONE.......................... 2 BONE CLASSIFICATION........................... 3 IMPLANT SIZE SELECTION.........................
Replacement of a single front tooth Surgical procedure and three-year results
 Case Report 10 2011 Replacement of a single front tooth Surgical procedure and three-year results Dr Peter Randelzhofer Munich, Germany Prosthetics Dr Peter Randelzhofer studied dentistry in Munich, Germany,
Case Report 10 2011 Replacement of a single front tooth Surgical procedure and three-year results Dr Peter Randelzhofer Munich, Germany Prosthetics Dr Peter Randelzhofer studied dentistry in Munich, Germany,
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation
 Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Replacing Hopeless Retained Deciduous Teeth in Adults Utilizing Dental Implants: Concepts and Case Presentation by Michael Tischler, DDS Published: Dentistry Today November 2005 Photos at end of article
Choosing the right type of abutment
 50 Producing custom implant abutments using CAD/CAM Choosing the right type of abutment S. KHALILOVA 1, F. KISTLER 2, S. ADLER 3, S. WEISS 3, S. KISTLER 2 AND J. NEUGEBAUER 2,4 Rapid developments in the
50 Producing custom implant abutments using CAD/CAM Choosing the right type of abutment S. KHALILOVA 1, F. KISTLER 2, S. ADLER 3, S. WEISS 3, S. KISTLER 2 AND J. NEUGEBAUER 2,4 Rapid developments in the
HEALTH SERVICES POLICY & PROCEDURE MANUAL. SUBJECT: Types of Dental Treatments Provided EFFECTIVE DATE: July 2014 SUPERCEDES DATE: January 2014
 PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
PAGE 1 of 5 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4369, 4-4375 PURPOSE To provide guidelines for determining appropriate levels of care and types
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Standard Internal Hex
 Standard Internal Hex Touareg TM -OS Touareg TM -S Swell TM Touareg -S Touareg -OS Swell About ADIN Adin Dental Implant Systems Ltd., designs, manufactures and markets state of the art, technologically
Standard Internal Hex Touareg TM -OS Touareg TM -S Swell TM Touareg -S Touareg -OS Swell About ADIN Adin Dental Implant Systems Ltd., designs, manufactures and markets state of the art, technologically
DENTAL IMPLANT THERAPY
 DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
Aesthetics meets CAD/CAM in the dental surgery
 62 EDI New state-of-the-art options for implant-supported restorations Aesthetics meets CAD/CAM in the dental surgery Dr Mathias Siegmund, M.Sc., Regensburg, Germany Thanks to the new Sub-Tec CAD/CAM TiBase
62 EDI New state-of-the-art options for implant-supported restorations Aesthetics meets CAD/CAM in the dental surgery Dr Mathias Siegmund, M.Sc., Regensburg, Germany Thanks to the new Sub-Tec CAD/CAM TiBase
Regular C/X Prosthetics. Prosthetics
 Regular C/X Prosthetics /X C/ Prosthetics ANKYLOS C/X Prosthetics For more than 20 years, the ANKYLOS system developed by Prof. Dr. G.-H. Nentwig and Dr. Dipl.-Ing. Walter Moser with its TissueCare Connection
Regular C/X Prosthetics /X C/ Prosthetics ANKYLOS C/X Prosthetics For more than 20 years, the ANKYLOS system developed by Prof. Dr. G.-H. Nentwig and Dr. Dipl.-Ing. Walter Moser with its TissueCare Connection
procedures & products NOBELESTHETICS including Procera
 procedures & products NOBELESTHETICS including Procera First from Nobel Biocare. NOBELPERFECT, (NP, RP, WP), NOBELDIRECT (NP, RP, WP), Brånemark System, NOBELREPLACE and NOBELSPEEDY Implants. A complete
procedures & products NOBELESTHETICS including Procera First from Nobel Biocare. NOBELPERFECT, (NP, RP, WP), NOBELDIRECT (NP, RP, WP), Brånemark System, NOBELREPLACE and NOBELSPEEDY Implants. A complete
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
BICON DENTAL IMPLANTS
 BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
BioHorizons Education Programme 2015
 BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
BioHorizons Education Programme 2015 SPMP14328GB Rev A November 2014 Contents The Role of Implants in Restorative Dentistry An Introduction to Contemporary Implant Prosthodontics Sinus Elevation Socket
DENT IMPLANT restoring qualit S: of LIfE
 DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
Dental Implant Restoration
 Dental Implant Restoration Principles and Procedures Stuart H. Jacobs Brian C. O Connell London, Berlin, Chicago, Tokyo, Barcelona, Beijing, Istanbul, Milan, Moscow, New Delhi, Paris, Prague, São Paulo,
Dental Implant Restoration Principles and Procedures Stuart H. Jacobs Brian C. O Connell London, Berlin, Chicago, Tokyo, Barcelona, Beijing, Istanbul, Milan, Moscow, New Delhi, Paris, Prague, São Paulo,
Clinical Perspectives
 Clinical Perspectives From Richard J. Lazzara, DMD, MScD Inside This Issue: NanoTite Implants: The Next Generation Of Dental Implants Case Presentations By: Roberto Cocchetto, DMD, ITALY Harold S. Baumgarten,
Clinical Perspectives From Richard J. Lazzara, DMD, MScD Inside This Issue: NanoTite Implants: The Next Generation Of Dental Implants Case Presentations By: Roberto Cocchetto, DMD, ITALY Harold S. Baumgarten,
education Although demographic factors and growing patient awareness of the benefits of dental implants
 education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Powertome Assisted Atraumatic Tooth Extraction
 Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
Powertome Assisted Atraumatic Tooth Extraction White et al Jason White, DDS 1 2 3 Abstract Background: While traditional dental extraction techniques encourage minimal trauma, luxated elevation and forceps
ATLANTIS abutments design guide CAD/CAM patient-specific abutments
 ATLANTIS abutments design guide CAD/CAM patient-specific abutments Contents Introduction 4 This manual helps you to explore all the benefits of ATLANTIS CAD/CAM patient-specific abutments. It gives you
ATLANTIS abutments design guide CAD/CAM patient-specific abutments Contents Introduction 4 This manual helps you to explore all the benefits of ATLANTIS CAD/CAM patient-specific abutments. It gives you
FABRICATING CUSTOM ABUTMENTS
 FABRICATING CUSTOM ABUTMENTS LUC AND PATRICK RUTTEN How much should a Dental Technician know about the clinical aspects of implantology? The answer is clear: as much as possible. This is the distinction
FABRICATING CUSTOM ABUTMENTS LUC AND PATRICK RUTTEN How much should a Dental Technician know about the clinical aspects of implantology? The answer is clear: as much as possible. This is the distinction
General Dentist Fees
 General Dentist Fees January 1, 2015 Not all codes are covered benefits. Please check the member s plan for verification and limitations. There are no fee increases for 2015, but new CDT codes have been
General Dentist Fees January 1, 2015 Not all codes are covered benefits. Please check the member s plan for verification and limitations. There are no fee increases for 2015, but new CDT codes have been
Restoration of a screw retained single tooth restoration in the upper jaw with Thommen Titanium base abutment.
 Restoration of a screw retained single tooth restoration in the upper jaw with Thommen Titanium base abutment. Dr. med. dent. David McFadden, Dallas County, USA Initial situation (single X-ray) Tooth 16
Restoration of a screw retained single tooth restoration in the upper jaw with Thommen Titanium base abutment. Dr. med. dent. David McFadden, Dallas County, USA Initial situation (single X-ray) Tooth 16
A promising treatment option
 46 EDI Immediate rehabilitation of the edentulous mandible with four rigidly bar-splinted implants in a patient with rheumatoid arthritis: A case report A promising treatment option Dr Peter Gehrke 1,
46 EDI Immediate rehabilitation of the edentulous mandible with four rigidly bar-splinted implants in a patient with rheumatoid arthritis: A case report A promising treatment option Dr Peter Gehrke 1,
Clinical Indications For Immediate Restoration Of Implants Using PreFormance Provisional Components
 Clinical Indications For Immediate Restoration Of Implants Using PreFormance Provisional Components By Richard J. Lazzara, DMD, MScD Inside This Issue: Clinical Case Presentations Optimizing Anterior Aesthetics
Clinical Indications For Immediate Restoration Of Implants Using PreFormance Provisional Components By Richard J. Lazzara, DMD, MScD Inside This Issue: Clinical Case Presentations Optimizing Anterior Aesthetics
porcelain fused to metal crown
 Lectur.5 Dr.Adel F.Ibraheem porcelain fused to metal crown the most widely used fixed restoration,it is full metal crown having facial surface (or all surfaces) covered by ceramic material. It consist
Lectur.5 Dr.Adel F.Ibraheem porcelain fused to metal crown the most widely used fixed restoration,it is full metal crown having facial surface (or all surfaces) covered by ceramic material. It consist
Anatomic limitations in the maxilla provide challenges
 Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
Osteotome Single-Stage Dental Implant Placement With and Without Sinus Elevation: A Clinical Report Orest G. Komarnyckyj, DDS*/Robert M. London, DDS** Forty-three sites in 16 patients were selected for
NobelActive. procedures and products
 NobelActive procedures and products precautions and warnings Manufacturer: Nobel Biocare AB, Box 5190, SE-402 26 Göteborg, Sweden. Phone: +46 31 81 88 00. Fax: +46 31 16 31 52 www.nobelbiocare.com Important!
NobelActive procedures and products precautions and warnings Manufacturer: Nobel Biocare AB, Box 5190, SE-402 26 Göteborg, Sweden. Phone: +46 31 81 88 00. Fax: +46 31 16 31 52 www.nobelbiocare.com Important!
Rehabilitation of Endondontically Failed Anterior teeth by Immediate Replacement and Loading of an Implant supported Crown: A Case Report.
 RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES Rehabilitation of Endondontically Failed Anterior teeth by Immediate Replacement and Loading of an Implant supported Crown: A Case Report. Lalit Kumar 1
RESEARCH AND REVIEWS: JOURNAL OF DENTAL SCIENCES Rehabilitation of Endondontically Failed Anterior teeth by Immediate Replacement and Loading of an Implant supported Crown: A Case Report. Lalit Kumar 1
Eastman Dental Hospital. Dental implants - general information for patients. Department of Restorative Dentistry
 Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Dental Implant Treatment after Improvement of Oral Environment by Orthodontic Therapy
 Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
Dental implant treatment after impr Title environment by orthodontic therapy. Sekine, H; Miyazaki, H; Takanashi, Author(s) Matsuzaki, F; Taguchi, T; Katada, H Journal Bulletin of Tokyo Dental College,
1 The Single Tooth Implant. The Ultimate Aesthetic Challenge
 1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
1 The Single Tooth Implant The Ultimate Aesthetic Challenge by Daniel G. Pompa, D.D.S. 2 Before starting any Maxillary Anterior Single Implant, or any case in the esthetic zone: TAKE A PHOTO OF YOUR PATIENT
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
Removing fixed prostheses using the ATD automatic crown and bridge remover
 Removing fixed prostheses using the ATD automatic crown and bridge remover By Dr. Ian E. Shuman, Baltimore, MD. Information provided by J. Morita USA When removing cemented provisionals and final fixed
Removing fixed prostheses using the ATD automatic crown and bridge remover By Dr. Ian E. Shuman, Baltimore, MD. Information provided by J. Morita USA When removing cemented provisionals and final fixed
4-1-2005. Dental Clinical Criteria and Documentation Requirements
 4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
prosthetic technique manual
 prosthetic technique manual TABLE OF CONTENTS Introduction 1 Treatment Planning 2-5 Restorative Options Implant-level Cement-retained Restorations Implant-level Screw-retained Restorations Abutment-level
prosthetic technique manual TABLE OF CONTENTS Introduction 1 Treatment Planning 2-5 Restorative Options Implant-level Cement-retained Restorations Implant-level Screw-retained Restorations Abutment-level
platform shifting Nobel Biocare is shifting gingival beauty to the next level
 platform shifting Nobel Biocare is shifting gingival beauty to the next level Nobel Biocare is shifting gingival beauty to the next level Platform Shifting is the latest in Nobel Biocare s offering of
platform shifting Nobel Biocare is shifting gingival beauty to the next level Nobel Biocare is shifting gingival beauty to the next level Platform Shifting is the latest in Nobel Biocare s offering of
Abutment fracture in a bridge supported by natural teeth and implants
 Abutment fracture in a bridge supported by natural teeth and implants Authors_Dr Gregory-George Zafiropoulos, Dr Giorgio Deli & Dr Rainer Valentin, Germany/Italy _Introduction Implant treatment has evolved
Abutment fracture in a bridge supported by natural teeth and implants Authors_Dr Gregory-George Zafiropoulos, Dr Giorgio Deli & Dr Rainer Valentin, Germany/Italy _Introduction Implant treatment has evolved
In 1999, more than 1 million people in
 Clinical SHOWCASE Slip-and-Fall Injuries Causing Dental Trauma Morley S. Rubinoff, DDS, Cert Prosth Clinical Showcase is a series of pictorial essays that focus on the technical art of clinical dentistry.
Clinical SHOWCASE Slip-and-Fall Injuries Causing Dental Trauma Morley S. Rubinoff, DDS, Cert Prosth Clinical Showcase is a series of pictorial essays that focus on the technical art of clinical dentistry.
SOFT TISSUE RECESSION AROUND IMPLANTS: IS IT STILL UNAVOIDABLE?
 CONTINUING EDUCATION X X SOFT TISSUE RECESSION AROUND IMPLANTS: IS IT STILL UNAVOIDABLE? André P. Saadoun, DDS, MS* Bernard Touati, DDS, MS SAADOUN 19 1 JANUARY/FEBRUARY When treatment with dental implants
CONTINUING EDUCATION X X SOFT TISSUE RECESSION AROUND IMPLANTS: IS IT STILL UNAVOIDABLE? André P. Saadoun, DDS, MS* Bernard Touati, DDS, MS SAADOUN 19 1 JANUARY/FEBRUARY When treatment with dental implants
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
ADA Insurance Codes for Laboratory Procedures:
 ADA Insurance Codes for Laboratory Procedures: Inlay/Onlay Restorations D2510 Inlay - metallic - one surface D2520 Inlay - metallic - two surfaces D2530 Inlay - metallic - three or more surfaces D2542
ADA Insurance Codes for Laboratory Procedures: Inlay/Onlay Restorations D2510 Inlay - metallic - one surface D2520 Inlay - metallic - two surfaces D2530 Inlay - metallic - three or more surfaces D2542
Accelerated Patient Rehabilitation
 Accelerated Patient Rehabilitation Providing The Tools Necessary For An Immediate Solution: NanoTite Implants QuickBridge Provisional Components Navigator System For CT Guided Surgery Initial Patient Presentation
Accelerated Patient Rehabilitation Providing The Tools Necessary For An Immediate Solution: NanoTite Implants QuickBridge Provisional Components Navigator System For CT Guided Surgery Initial Patient Presentation
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
deltadentalins.com/usc
 Plan Benefit Highlights for: UNIVERSITY OF SOUTHERN CALIFORNIA STUDENT PLAN Group No: 05008 The Delta Dental PPO table plan provides you great dental benefits at a reasonable cost. With a table of allowance
Plan Benefit Highlights for: UNIVERSITY OF SOUTHERN CALIFORNIA STUDENT PLAN Group No: 05008 The Delta Dental PPO table plan provides you great dental benefits at a reasonable cost. With a table of allowance
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI
 Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Flapless Implant Surgery for Replacement of Posterior Teeth
 Course Number: 108.2 Flapless Implant Surgery for Replacement of Posterior Teeth Authored by J. Steven Cloyd, DDS Upon successful completion of this CE activity 1 CE credit hour may be awarded A Peer-Reviewed
Course Number: 108.2 Flapless Implant Surgery for Replacement of Posterior Teeth Authored by J. Steven Cloyd, DDS Upon successful completion of this CE activity 1 CE credit hour may be awarded A Peer-Reviewed
Contents. Cement retained restoration. Screw retained restoration. Overdenture retained restoration. TS Implant System. 70 ComOcta Gold Abutment
 Contents TS Implant System Cement retained restoration Screw retained restoration 06 Cement-retained bridges with the Solid abutment system (non- 72 Screw retained crown with the ComOcta Gold abutment
Contents TS Implant System Cement retained restoration Screw retained restoration 06 Cement-retained bridges with the Solid abutment system (non- 72 Screw retained crown with the ComOcta Gold abutment
Implanting Brilliancy
 Implanting Brilliancy NEW: ANKYLOS C/X with the option of indexing & more 3 ANKYLOS certainly a brilliant choice The true value of an implant system first becomes apparent when it establishes permanent
Implanting Brilliancy NEW: ANKYLOS C/X with the option of indexing & more 3 ANKYLOS certainly a brilliant choice The true value of an implant system first becomes apparent when it establishes permanent
Another Implant Option for Missing Teeth with Challenging Symmetry Patrick Gannon, DDS and Luke Kahng, CDT
 Another Implant Option for Missing Teeth with Challenging Symmetry Patrick Gannon, DDS and Luke Kahng, CDT Introduction A 58 year old male had been missing teeth #7=12 for approximately 28 years. During
Another Implant Option for Missing Teeth with Challenging Symmetry Patrick Gannon, DDS and Luke Kahng, CDT Introduction A 58 year old male had been missing teeth #7=12 for approximately 28 years. During
