Total Knee Replacement
|
|
|
- Leon Blake
- 8 years ago
- Views:
Transcription
1 Total Knee Replacement A Guide for Patients Produced by the British Association for Surgery of the Knee and The British Orthopaedic Association (adapted)
2 KNEE ARTHRITIS If your knee is affected by severe arthritis or injury it may be difficult to perform simple activities such as walking, climbing stairs or sitting comfortably for prolonged periods. You may even feel the pain lying down. In Britain one in five patients over the age of 65 has some form of arthritis and in one in 20 patients the knee is the most severely affected joint. Osteoarthritis can develop for the following reasons: age degenerative rheumatoid arthritis or other inflammatory joint disease trauma which can damage the joint surfaces after some birth defects and growth disorders. Loss of Cartilage Normal Knee
3 HOW THE NORMAL KNEE WORKS The knee is the largest joint in the body and each knee carries half the body weight. It is the articulation between the lower part of the thigh bone (femur) and the upper part of the shin bone (tibia). These are covered by a smooth layer of cartilage called articular cartilage. There is rotation and hinge activity between these two bones. In addition the kneecap or patella is covered by articular cartilage on its under surface and slides in the groove on the front of the femur. There are two large ligaments joining the two bones together, reinforced by strong muscles and tendons at the back and the front of the joint (see appendix). Injury can damage the joint surfaces and the destruction of the cartilage covering the ends of the bone is what we term arthritis. These surfaces become rough and uneven and the joint cannot move smoothly. NON-SURGICAL TREATMENT The initial treatment includes drugs to reduce pain and inflammation, changing activity levels, using walking supports and physiotherapy, and reducing weight. Occasionally keyhole surgery is advised to clean out any damaged areas. However, if these are not successful in curing the symptoms, a total knee replacement may be considered. This operation resurfaces the knee joint removing diseased bone and cartilage from the lower end of the thigh bone, the upper end of the shin bone and the 2
4 back of the kneecap (patella). These surfaces are replaced with metal and plastic implants which allow natural knee motion and function and at the same time relieve pain and correct any deformity, enabling you to resume a greater scope of normal activities. KNEE REPLACEMENT Knee replacement was developed following the success of hip replacement and much of the pioneering work was done in Britain. The early knee replacements in the 1960s and 1970s were fairly basic and the results were mixed. Improvements in surgical materials and techniques have greatly increased the effectiveness so that knee replacement surgery today has a high rate of success in relieving pain and restoring mobility, approximately 95 out of every 100 procedures can be expected to be successful and, even at 10 to 15 years after the operation, will still be giving good service; some knee replacements have lasted 25 years. If the replacement becomes loose, breaks or gets infected another operation is necessary; this is called a revision knee replacement. The replacement will last longer in lighter people and in older people who put less demand on the materials. IS TOTAL KNEE REPLACEMENT RIGHT FOR YOU? Your General Practitioner and Orthopaedic Surgeon may advise knee replacement surgery in the following cases: Severe chronic pain in the knee that limits everyday activities such as walking, going up and down stairs, getting out of a chair, as well as pain at rest, especially at night. The knee may be stiff and swollen and X-ray confirms arthritis. Failure to obtain relief from non-steroidal anti-inflammatory drugs and injections or physiotherapy. Most patients who undergo knee replacement are aged between 60 and 80 but patients younger or older than this may be advised that this is the best treatment for them. THE DECISION TO HAVE TREATMENT This should only be made after discussion with the orthopaedic surgeon whose team is going to carry out the operation. The surgeon will discuss benefits and risks of treatment, and will emphasise that surgery cannot be guaranteed to meet all expectations and that there are risks associated with surgery. There must be a realistic expectation by the patient about what the operation can achieve and, whilst over 90% of patients have dramatic reduction in pain, the operation will not allow a high level of athletic activities and in particular some high impact sports will be excluded from normal activities. In addition, many patients find kneeling and crouching difficult after a knee replacement due to some residual stiffness in the knee. 5
5 WHAT CAN YOU EXPECT FROM YOUR KNEE REPLACEMENT? Two out of three patients can expect good relief of pain and satisfactory function of their knee after a knee replacement. One third of patients experience some degree of pain and a variable level of stiffness in the knee which can affect activities. It is important to understand that the knee heals slowly after a knee replacement and it takes at least three months for the swelling and skin discolouration to settle. The knee will continue to improve as pain lessens and movement recovers, for up to one year after the operation. time spent at these activities, usually starting at about 10 to 12 weeks after your operation. Everybody is different and you should plan your return to a normal lifestyle at your own pace; do not compare yourself with other people! With regard to activities, you will be independent to look after yourself at home when you leave hospital. You will be encouraged to do your exercises regularly and to take a walk at least once a day. Gradually, your walking distance will improve as your knee recovers and you should be able to consider shopping for yourself and returning to non-manual work within two months. The length of time before returning to driving depends on which knee has been replaced. If you have an automatic car and have a LEFT knee replacement, you can consider driving as soon as you can comfortably get into and out of a car and sit comfortably at the wheel. For a RIGHT knee and for all manual gear change cars (whether you have had a right or left knee replacement), it is recommended that you should not return to driving for two months. Finally, for leisure activities such as golf, bowling, swimming, cycling etc, it is recommended that you gradually increase the 6 7
6 THE ORTHOPAEDIC ASSESSMENT This consists of several components: A medical history, when the surgeon gathers information about your general health. Physical examination with assessment of knee movement, stability and strength, followed by an X-ray. Occasionally blood tests and magnetic resonance imaging (MRI) may be required to clarify the diagnosis. The orthopaedic surgeon will assess the results of these and, after discussion, may advise other treatments, leaving total knee replacement as the last resort of a treatment plan. Knee arthroplasty is not usually recommended for patients who are severely overweight, have severe arterial disease in the legs, an infection in the knee, in the lower leg or in the skin, any nerve disorder affecting the knee and severe neurological problems, such as Parkinson's disease. MEDICAL HISTORY You must disclose all health problems and any medication, in particular the following need to be highlighted: allergic reaction to antibiotics, anaesthetics or other drugs prolonged bleeding or excessive bruising previous problems with blood clots in the legs or lungs recent or long-term illnesses gout diabetes psychological or psychiatric illnesses poor healing and scar formation. Drugs such as anti-inflammatory medication, Aspirin, anticoagulants, the contraceptive pill and regular medication. Insulin may be stopped or modified prior to surgery and the surgical team need to know these details. SMOKING Smoking increases surgical and anaesthetic risk and impairs healing. Patients are advised to stop smoking at least two weeks before surgery. PREADMISSION CLINIC You will be seen in a preadmission clinic at the Royal Infirmary of Edinburgh approximately one week before your operation. A pre-operative evaluation will be carried out by with nurses and often the surgeon and anaesthetist will see you on that occasion. This is a good opportunity to ask questions about the operation, risks of surgery and your recovery after a knee replacement. 8 9
7 THE ANAESTHETIC Knee replacement can be performed under a general or spinal anaesthesia, which numbs the lower limbs but you remain awake. Modern anaesthesia is safe but you should discuss this with the anaesthetist. Occasionally there are side effects and a full list of your existing medications and allergies must be given to the anaesthetist. THE OPERATION Most patients are admitted on the day of surgery through the Day of Surgery Admission unit, on level 1 of the Royal Infirmary of Edinburgh. The operation usually takes place with a tourniquet around the thigh to reduce the amount of bleeding and enable the components to be fitted accurately into position. The incision can be anything from 10 to 20cm in length depending on the type of approach and the size of the leg. All the blood vessels, muscles and nerves are protected during surgery and special tools are used to remove the surface of the bone. The components are implanted by shaping the bone to form a tight fit with the prosthesis, which is coated with a special material which allows bone to grow on to the surface and provide fixation (uncemented prosthesis); alternatively bone cement may be used to hold the prosthesis in place (cemented). The wound is closed with internal stitches to keep all the ligaments and muscles securely together, and clips, sutures or special tape on the skin. RECOVERY Following the total knee replacement you will be transferred from the operating theatre into the Recovery Area where there may be several other patients. You will be here for up to two hours while most of the anaesthetic wears off. If you have had a spinal anaesthetic you may not be able to feel your legs when you wake up. You will be given oxygen and pain killing medication, usually through an intravenous line or drip. Very occasionally a special catheter may be introduced into the bladder to drain off the urine if you are unable to feel or pass urine yourself or if you have no feeling due to the spinal anaesthetic. The pain and discomfort might be quite severe in the first few days but the nurses and anaesthetic team will usually be able to administer sufficient pain killers to reduce the pain to acceptable levels. PHYSIOTHERAPY Your physiotherapist will see you the day after your operation. You will be helped to sit out of bed using a walking frame. You will be shown a few exercises to begin moving and strengthening your knee. Once you are confident with the walking frame you will usually then be progressed to sticks and then finally will practise going up and down some stairs. Sticks may be needed for up to six weeks and older patients may have to continue the use of a walking aid for longer periods. Not all patients require out-patient physiotherapy after having 10 11
8 Following total knee replacement patients are encouraged to resume an active lifestyle but are strongly advised against activities that produce high impact such as running and jumping. Sports such as golf, cycling, swimming and walking are encouraged. Other acceptable activities include bowling, croquet, doubles tennis, table tennis and dancing ballroom and line dancing. The following exercises are suitable for most people. It is recommended that you try to do your exercises three times a day. a knee replacement. If you have a good knee bend and good muscle control, out-patient physiotherapy is not necessary. You should, however, continue doing exercises at home for at least three months. During the first few weeks stretching and strengthening the muscles remain goals of treatment. As strength and motion improves you may be instructed on other activities such as distance walking, cycling and swimming. These should restore your feeling of well-being. You may take up to between six and 12 weeks off from work depending on the job and it is useful to discuss this before surgery
9 To maintain or increase range of movement: Lying on your back with a sliding board under your leg and a do-nut under your heel, bend and straighten your knee by sliding your foot up and down. Go as far as you can each way, pushing the back of your knee down into the board as you straighten and stretching the front of your knee at the limit of your bend. Sit on a chair with your foot on a board and do-nut on the floor. Slide your foot backwards and forwards on the board to bend and straighten your knee. As you bend keep your hip down on the chair. It is important to fully straighten the knee. Sometimes people with arthritic knees develop a flexion contracture. This is because the most comfortable position for the painful knee is holding it slightly bent. Over a prolonged period the soft tissues around the back of the knee contract and it becomes impossible to straighten it. Your new knee should be aligned by the surgeon so that it can fully straighten but you may need to stretch the soft tissues to achieve a straight knee. If when doing Exercise No 1 you are unable to straighten the knee fully making the back of the knee touch the board, you should do the following exercises. Rest your ankle on top of a rolled up towel and allow the back of your knee to stretch out. Sitting on a chair, with the leg to be exercised supported on a chair or footstool as shown. Let your leg straighten in this position. You may find this uncomfortable at the back of your knee. Try to gradually increase the length of time you are able to hold this stretch. Build up to 10 minutes if you can. Exercises to Strengthen Muscles: It is very important to strengthen the muscles around the knee so that any movement is well controlled and so the knee is protected from injury. The two main muscle groups to strengthen are: The quadriceps which make up the bulk on the front of your knee. They work to straighten your knee. The hamstrings which make up the back of your thigh and work to bend the knee
10 Quadriceps exercises: Hamstring Exercises: Lying on your back or reclining. Press the back of your knee down onto the bed tensing the muscles at the front of your thigh. At the same time pull your toes up and you should feel the pressure come off your heel. Hold the muscle contraction for about 10 seconds then relax. 7. Position as for Exercise 5. Place a block under the back of your knee - a towel is ideal. Press the back of your knee down into the block until your foot lifts. Bring it up as high as you can without lifting your knee and hold for 10 seconds, before lowering slowly. Sit on an upright chair with your thigh supported to the knee. Straighten your knee and hold for 10 seconds. Lower slowly. Stand upright, holding onto a worktop or chair to help you balance. Stand on the non-operated leg and bend the operated knee bringing your foot up behind you. Hold for 10 seconds, then lower your foot. As your recovery progresses it is good to introduce more functional exercises as these encourage co-ordination of muscle control If you are able to tolerate lying on your tummy, this is useful for working your hamstrings and helping straighten the knee. Lie face down with your feet off the end of the mattress. Slowly bend and straighten your knee
11 Going down: 1) First take your stick down onto the step below. 2) The take a step down with your affected leg. 3) Then take a step down with your healthy leg onto the same step. Sit in a firm chair in front of a wall placing your hands on the wall for balance. Stand up and sit down slowly, keeping your weight evenly between both feet. Stairs: After 6-8 weeks stand in front of a step. Step up and down backwards leading with the un-operated leg. If a handrail is present use it (if no handrail, use both sticks). Going up: 1) First take a step up with your healthy leg. 2) Then take a step up with your affected leg. 3) Then bring your stick up onto the same step. Always go one step at a time. Use of Gym Equipment: Static bike: You may not be able to pedal properly at first but start with the seat high and rock the pedals back and forth. Once you can pedal you may gradually lower the seat and increase resistance as comfort allows. Step machine and leg press: It is safe to use these provided your knee is not forced and resistance is increased gradually as comfort allows. Caution: If you also have a hip replacement the leg press is unsuitable as is any equipment with a very low seat. The stitches or clips are removed after 10 to 14 days. You will be reviewed, either in the nurse/physiotherapy clinic or by the surgeon, and X-rays will be taken in the post-operative period to ensure that everything is progressing well
12 OCCUPATIONAL THERAPY The occupational therapist will see you on the ward prior to going home and discuss your home circumstances with you. If there are problems at home, or connected with your rehabilitation, they will advise you and make arrangements as required. They will also carry out an assessment of your function and make sure that you can manage all every day activities independently. The occupational therapist will offer you practical advice to help you cope at home when you are discharged from hospital. COMPLICATIONS OF KNEE REPLACEMENT SURGERY There are risks following knee replacement surgery despite high standards of practice. Complications can occur that may have permanent effects which is why the operation is only undertaken when all other methods of treatment have failed. Surgeons do not usually outline every single complication but they do point out to you the most serious ones. Serious complications occur in no more than one or two in every 100 patients, but less serious complications can occur more frequently and generally get better. 1. General risks of surgery Possible complications include: Pain around the incision Nausea often from the anaesthetic Heavy bleeding from the surgical site. A blood transfusion may be required if bleeding is particularly heavy. Sometimes systems are used which collect the blood that has leaked into the wound drain and this is then re-transfused Keloid or thickened, raised scars these can be very unpleasant, itchy and unsightly in the early stages but usually will settle down and are not a serious threat to the wound healing Separation of the wound edges sometimes the stitches or clips come adrift and this can cause opening of the wound 20 21
13 Allergies to anaesthetic agents, antiseptic solutions, suture materials or dressings Very rarely there may be any complication of anaesthesia and surgery such as heart attack, heart failure, stroke, kidney failure, and other serious problems. 2. Specific Risks of Knee Replacement Infection Infection around a knee replacement occurs in about one in every 100 patients and is very serious. Infection can develop immediately or many months after the operation. Occasionally, infection can spread in the blood stream from another part of the body and infect the knee. To reduce the risk of infection, antibiotics are given before and after surgery. If you develop an infection after you have had a knee replacement (for example bladder/kidney infection; a skin or dental abscess) you must consult your general practitioner, who will prescribe appropriate treatment to prevent this complication. Occasionally the infection in your knee may be resistant to treatment and a second operation may be needed to remove the components of the knee replacement. Once all the infection has been effectively treated a third operation is performed to insert new components. You may develop other infections after your operation, including chest and urine. Thrombosis and pulmonary embolism Blood clots can form in the deep veins of either leg. This can be life-threatening if they break away from the vein wall and travel in the bloodstream to block the arteries to the lung. Prevention in the form of injections, tablets or special leg pumps is used, depending upon your individual circumstances. If you have ever had a leg thrombosis before it is essential that you tell the medical staff as treatment with Warfarin may be required for three months after the operation. Loosening/breakage The prosthesis may become loose where the metal or cement meets the bone. This can cause pain and eventually another operation may be needed. This is the most common long-term problem affecting knee replacements and requires the worn implant to be removed and a new knee replacement inserted (a revision knee replacement). Scarring, Stiffness and Swelling Heavy scarring after surgery may restrict bending of the knee. To release the scars and improve movement the Surgeon may need to manipulate the knee. If the joint was extremely stiff before surgery, there is likely to be quite a lot of stiffness afterwards. Swelling is common after surgery and may take several months to settle
14 Nerve and Artery Injury A major nerve may be damaged, leading to poor or no leg movements. Most nerve injuries recover well, often completely. Uncommonly, nerve damage may be permanent, leading to permanent numbness and/or weakness of the foot. One of the major arteries near the knee may be injured and require further surgery but this is a very rare complication Skin It is common for the knee to feel hot for many weeks after the operation wound has healed. You may notice this at night time in particular. This hot sensation is a normal part of the healing process and gradually improves, and rarely lasts longer than six months. There will be an area of numbness on the outer side of the wound. This area will become less noticeable with time and will not interfere with the function of your knee. Amputation Rarely, complications due to a severely impaired blood supply, arterial damage or overwhelming infection may lead to amputation of the leg above the knee. The risk is greater for patients who are elderly or in poor general health. The overall risk is one patient in 6,000. RE-OPERATION The prosthesis may become loose requiring revision surgery (as described above) and this can be done in one operation. If the looseness is due to infection, this will usually require two operations with a period of six weeks to six months between them to allow the infection to settle. FINALLY Report to your doctor or the Arthroplasty Nurse Practitioner (telephone number in Appendix) any of the following: Temperatures higher than 38.5 centigrade/102 Fahrenheit, fever, sweating, shivering or chills Severe pain or tenderness Heavy bleeding from the incision Redness around the incision that is spreading Worsening pain or stiffness of the knee Loss of mobility after a fall with increased pain Swelling and pain in the calf of either leg
15 FREQUENTLY ASKED QUESTIONS Why have I still got swelling? Healing tissues are more swollen than normal tissues. This swelling may last for several months. Ankle swelling is due to the fact that each time we take a step the calf muscles contract and help pump blood back to the heart. If you are not putting full weight on the leg, the pump is not as effective and fluid builds up around the ankle. By the end of the day lots of people complain their ankle is more swollen. What can I do about it? When sitting, the ankle pump exercises work the calf muscles and help pump the fluid away. Try to put equal weight through each leg and push off from your toes on each step. Have a rest on the bed after lunch for an hour. You can put one or two pillows lengthways under your leg whilst resting but do not use them at night. Why is my scar warm? Even when the scar has healed there is still healing going on deep inside. This healing process creates heat, which can be felt on the surface. This may continue for up to six months. This is different warmth to that of an infection. Why do I get pain lower down my leg? The tissues take time to settle and referred pain into the shin or behind the knee is quite common. Why do I stiffen up? Most people notice that whilst they are moving around they feel quite mobile. After sitting down, the knee feels stiff when they stand and they need to take three or four steps before it loosens up. This is because those healing tissues are still swollen and are slower to respond than normal tissue. Is it normal to have disturbed nights? Yes, very few people are sleeping through the night at six weeks after the operation. As with sitting, you stiffen up and the discomfort then wakes you up. Also, many people are still sleeping on their backs, which is not their normal sleeping position so sleep patterns are disturbed. You may sleep on your side when you feel comfortable. Most people find it helpful to have a pillow between their legs. I have a numb patch is this okay? Numbness around the incision is due to small superficial nerves being disrupted during surgery. The patch usually gets smaller but there may be a permanent small area of numbness. Why does my joint click? This is normal and it is usually a sign that those swollen tissues are moving over each other differently than before. You should not let this worry you, as again this should improve as healing continues
16 When should I stop using a stick? Stop using a stick when you can walk as well without it as with it. It is better to use a stick you still have a limp so that you do not get into bad habits that are hard to lose. Limping puts extra stain on your other joints, especially your back and other leg. Use the stick in the opposite hand to your operated knee. Many people take a stick out with them for three to four months after the operation as they find they limp more when they get tired. How far should I walk? This varies on your fitness and what your home situation is. You should feel tired, not exhausted when you get home, so gradually build up distance, remembering you have to get back. Will I set off the security scanner alarm at the airport? BAA s advice (May 2005) is that there should be no problem if your joint is made of titanium. Some joints are made of stainless steel and these may set off the alarm. If this happens, have a word with security staff and explain the situation. If you have metal walking sticks or crutches, they will be X-rayed and then can be used on the aircraft. Will I get better? Yes do not despair. It can take up to 12 months to fully recover. You will get there! When can I put my socks on? When you are able to reach your foot. This may take some time. It is different for everyone, so it is when it feels right which is when you are not forcing the bend. Can I go swimming? You can go in a pool with steps as soon as the scar has healed and do gentle exercises. Serious swimming can be started after three months but make sure you are on sure footing (i.e. not in the sea). Breast stroke can be done if it feels comfortable, but start off gently
17 APPENDIX NOTES USEFUL CONTACT TELEPHONE NUMBERS Preadmission Unit: Day of Surgery Unit: Ward 208: Ward 209: Physiotherapy: Occupational Therapy: Appointments: Arthroplasty Advice Line: USEFUL WEBSITES FOR MORE INFORMATION (knee replacement) (information) (knee replacement)
18 This information booklet was produced with support from De Puy UK Ltd
Hip Replacement. Department of Orthopaedic Surgery Tel: 01473 702107
 Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
Information for Patients Hip Replacement Department of Orthopaedic Surgery Tel: 01473 702107 DMI ref: 0134-08.indd(RP) Issue 3: February 2008 The Ipswich Hospital NHS Trust, 2005-2008. All rights reserved.
OPERATION:... Proximal tibial osteotomy Distal femoral osteotomy
 AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
AFFIX PATIENT DETAIL STICKER HERE Forename.. Surname NHS Organisation. Responsible surgeon. Job Title Hospital Number... D.O.B.././ No special requirements OPERATION:..... Proximal tibial osteotomy Distal
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Total Knee Replacement Further Information and Feedback: Tell us how useful
Total knee replacement
 Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Patient Information to be retained by patient What is a total knee replacement? In a total knee replacement the cartilage surfaces of the thigh bone (femur) and leg bone (tibia) are replaced. The cartilage
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
Total hip replacement
 Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Patient Information to be retained by patient What is a total hip replacement? In a total hip replacement both the ball (femoral or thigh bone) side of the hip joint and the socket (acetabular or pelvic
Procedure Information Guide
 Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide Resurfacing hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that
Procedure Information Guide
 Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Procedure Information Guide Total hip replacement Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every effort to ensure that the
Further information You can get more information and share your experience at www.aboutmyhealth.org
 OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
OS01 Total Hip Replacement Further information You can get more information and share your experience at www.aboutmyhealth.org Local information You can get information locally from: Taunton and Somerset
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
KNEE ARTHROSCOPY. Dr C.S. Waller. Orthopaedic Surgeon
 KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
KNEE ARTHROSCOPY Dr C.S. Waller Orthopaedic Surgeon Specializing in surgery of the hip and knee 83826199 What is Arthroscopy? Arthroscopy involves the inspection of the inside of the knee joint with a
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Total knee replacement Uni-compartmental knee replacement
 Your Knee Replacement at the Nuffield Orthopaedic Centre A patient s guide to: Total knee replacement Uni-compartmental knee replacement Welcome to Team Two at the NOC. Together you and your surgeon have
Your Knee Replacement at the Nuffield Orthopaedic Centre A patient s guide to: Total knee replacement Uni-compartmental knee replacement Welcome to Team Two at the NOC. Together you and your surgeon have
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Delivering Excellence. Nuffield Orthopaedic Centre NHS Trust. Information for Patients. Hip and Knee service. Total Knee Replacement NHS
 www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
www.noc.nhs.uk/hipandknee/default.aspx Nuffield Orthopaedic Centre NHS Trust www.noc.nhs.uk NHS Total Knee Replacement Information for Patients Hip and Knee service Delivering Excellence Contents Page
Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865
 Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Write questions or notes here: Level 1, 131-135 Summer Street ORANGE NSW 2800 Ph: 02 63631688 Fax: 02 63631865 Document Title: Revision Total Hip Replacement Further Information and Feedback: Tell us how
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Should I have a knee replacement?
 Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
Introduction Should I have a knee replacement? Knee replacement is an operation to remove the arthritic parts of the knee and replace them with an artificial joint made of metal and plastic. It can either
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary
 X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
X-Plain Hip Replacement Surgery - Preventing Post Op Complications Reference Summary Introduction Severe arthritis in the hip can lead to severe pain and inability to walk. To relieve the pain and improve
Hip arthroscopy Frequently Asked Questions
 Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Hip arthroscopy Frequently Asked Questions What is a hip arthroscopy? Hip arthroscopy is key hole surgery. Usually 2-3 small incisions (about 1 cm long) are made on the side of your hip. Through these
Total Knee Replacement
 Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
Total Knee Replacement Contents Introduction Total Knee Replacement Preparing for surgery Pre-op visit Day of surgery After surgery (In Hospital) After surgery (In Rehab) Exercise Program and Physical
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
TOTAL HIP REPLACEMENT Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a hip replacement? A hip replacement is an operation in which the damaged surfaces of the hip joint are removed
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
HIP JOINT REPLACEMENT
 HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
HIP JOINT REPLACEMENT Information for Patients WHAT IS HIP JOINT REPLACEMENT? The hip joint is a ball-and-socket joint formed by the upper part of the thigh bone (femoral head) and a part of the pelvis
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Premier Orthopaedic Pathway. Physiotherapy after dynamic hip screw (DHS)
 Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Premier Orthopaedic Pathway Physiotherapy after dynamic hip screw (DHS) The surgery After a fractured hip a dynamic hip screw (DHS) is used to hold the bones in place while the fracture heals. It allows
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Y O U R S U R G E O N S. choice of. implants F O R Y O U R S U R G E R Y
 Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Y O U R S U R G E O N S choice of implants F O R Y O U R S U R G E R Y Your Surgeon Has Chosen the C 2 a-taper Acetabular System The
.org. Total Knee Replacement. Anatomy
 Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Total Knee Replacement Page ( 1 ) If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to
Hip Replacement Surgery Understanding the Risks
 Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
Hip Replacement Surgery Understanding the Risks Understanding the Risks of Hip Replacement Surgery Introduction This booklet is designed to help your doctor talk to you about the most common risks you
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme Aim This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, and outline what
Total Knee Replacement Surgery
 Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Total Knee Replacement Surgery On this page: Overview Reasons for Surgery Evaluation Preparing for Surgery Your Surgery Risks Expectations after Surgery Convalescence Also: Partial Knee Replacement Overview
Knee Replacement: Information for Patients and Carers
 Directorate of Surgical Care Department of Orthopaedics Knee Replacement: Information for Patients and Carers This information is for patients who are considering having a knee replacement. What is a Knee
Directorate of Surgical Care Department of Orthopaedics Knee Replacement: Information for Patients and Carers This information is for patients who are considering having a knee replacement. What is a Knee
Total Knee Replacement
 Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Dr C.S. Waller MB BS FRCS(Ed) FRACS FA(Orth)A Specialist Hip and Knee Surgeon Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities
Ankle Stabilisation Procedure
 Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Ankle Stabilisation Procedure Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with an unstable ankle. This leaflet
Total Knee Arthroplasty (Knee Replacement) PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9337 Total Knee Arthroplasty
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9337 Total Knee Arthroplasty
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion
 A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
A Patient s Guide to Arthritis of the Big Toe (Hallux Rigidus) With Discussion on Cheilectomy and Fusion The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
This information is for patients who are considering having a hip replacement.
 Directorate of Surgical Care Department of Orthopaedics Hip Replacement: Information for Patients and Carers This information is for patients who are considering having a hip replacement. What is a hip
Directorate of Surgical Care Department of Orthopaedics Hip Replacement: Information for Patients and Carers This information is for patients who are considering having a hip replacement. What is a hip
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Arthroscopic shoulder stabilisation. Patient Information to be retained by patient
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Shoulder instability The shoulder is the most common joint in the body to dislocate.
Patient Information for Lumbar Spinal Fusion. What is a lumbar spinal fusion? Page 1 of 5
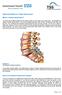 Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
Patient Information for Lumbar Spinal Fusion What is a lumbar spinal fusion? You have been offered surgery to the lumbar region of your spine, your lower back. The operation is called a lumbar spinal fusion.
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
Elbow Joint Replacement A guide for patients
 Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Elbow Joint Replacement A guide for patients GATESHEAD UPPER LIMB UNIT Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 The elbow joint The elbow consists of three bones; the humerus
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
Ankle Arthroscopy and Follow-Up Physiotherapy
 Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Ankle Arthroscopy and Follow-Up Physiotherapy Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have agreed that you might benefit from
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Anterior Hip Replacement
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic health. All decisions about the management of hip replacement and arthritis management must be made in
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle
 A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Lateral Ligament Reconstruction of the Ankle The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Revision Hip Replacement or arthritis management. All decisions
Total Hip Replacement PATIENT INFORMATION
 DEPARTMENT OF ORTHOPAEDICS Total Hip Replacement PATIENT INFORMATION Welcome to Orthopaedic Department at Warwick Hospital TOTAL HIP REPLACEMENT Welcome to the Orthopaedic Department at Warwick Hospital.
DEPARTMENT OF ORTHOPAEDICS Total Hip Replacement PATIENT INFORMATION Welcome to Orthopaedic Department at Warwick Hospital TOTAL HIP REPLACEMENT Welcome to the Orthopaedic Department at Warwick Hospital.
Tired, Aching Legs? Swollen Ankles? Varicose Veins?
 Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
Tired, Aching Legs? Swollen Ankles? Varicose Veins? Healthy Legs 2006 http://healthylegs.com Page 1 Venous disorders are widespread Leg problems are widespread throughout the world, but what most people
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Tibial Intramedullary Nailing
 Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
Tibial Intramedullary Nailing Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2015. Document for issue as handout. Procedure The tibia is the long shin bone in the lower leg. It is a weight
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Rehabilitation After Your Total Knee Replacement
 1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
1809 E. 13 th Street Suite 200 Tulsa, OK 74104-4243 (918) 582-6800 www.toctulsa.com Rehabilitation After Your Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee Replacement or arthritis management. All decisions about
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
V03 Varicose Veins Surgery
 V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
V03 Varicose Veins Surgery What are varicose veins? Varicose veins are enlarged and twisted veins in the leg. They are common and affect up to 3 in 10 people. More women than men ask for treatment, with
Total Knee Replacement
 Manchester Royal Infirmary Total Knee Replacement Department of Orthopaedic Surgery 2 What is a Total Knee Replacement? Total knee replacement is one of the most commonly performed orthopaedic operations
Manchester Royal Infirmary Total Knee Replacement Department of Orthopaedic Surgery 2 What is a Total Knee Replacement? Total knee replacement is one of the most commonly performed orthopaedic operations
Elbow arthroscopy. Key points
 Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
Patient information Elbow arthroscopy This information has been produced to help you gain the maximum benefit and understanding of your operation. It includes the following information: Key points About
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST
 PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
PHYSIOTHERAPY OF HIP AND KNEE AFTER SURGERY AND INJURY BY RACHEL GEVELL PHYSIOTHERAPIST AIMS AND OBJECTIVES To demonstrate the use of physiotherapy assessment and treatment following: Hip Arthroplasty
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY
 HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
HEADER TOTAL HIP REPLACEMENT SURGERY FROM PREPARATION TO RECOVERY ABOUT THE HIP JOINT The hip joint is a ball and socket joint that connects the body to the legs. The leg bone is called the femur. The
Cheltenham Hip Clinic
 Hip surgery At Cheltenham, we treat a wide range of hip conditions. It s important to note that not all hip problems require surgery and we will always look for a non-surgical solution where possible.
Hip surgery At Cheltenham, we treat a wide range of hip conditions. It s important to note that not all hip problems require surgery and we will always look for a non-surgical solution where possible.
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
HIP & KNEE SURGERY PATIENTS
 HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
HIP & KNEE HIP & KNEE SURGERY PATIENTS GET ANSWERS TO FREQUENTLY ASKED QUESTIONS YOU. IMPROVED. 2001 Vail Ave (N. Caswell St. Entrance) Suite 200A Charlotte, NC 28207 orthocarolina.com GENERAL QUESTIONS
Total Hip Arthroplasty (Hip Replacement) PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9336 Facility: Total Hip
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v4.00-04/2011 SW9336 Facility: Total Hip
Total Knee Replacement
 Total Knee Replacement Patient Information Author ID: AW Leaflet Number: Musc 012 Name of Leaflet: Total Knee Replacement Date Produced: April 2014 Review Date: April 2016 Total Knee Replacement Page 1
Total Knee Replacement Patient Information Author ID: AW Leaflet Number: Musc 012 Name of Leaflet: Total Knee Replacement Date Produced: April 2014 Review Date: April 2016 Total Knee Replacement Page 1
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Shoulder stabilisation surgery. Information for patients Orthopaedics
 Shoulder stabilisation surgery Information for patients Orthopaedics page 2 of 20 Introduction The upper limb unit team wants you and your family to understand as much as possible about the operation you
Shoulder stabilisation surgery Information for patients Orthopaedics page 2 of 20 Introduction The upper limb unit team wants you and your family to understand as much as possible about the operation you
Broström Lateral Ligament Reconstruction of Ankle
 Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
Broström Lateral Ligament Reconstruction of Ankle This leaflet aims to answer your questions about having a broström lateral ligament reconstruction of ankle under the care of Mr Sam Singh. It explains
www.noc.nhs.uk ACL Reconstruction Information for Patients Delivering Excellence Hip and Knee service
 www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
www.noc.nhs.uk ACL Reconstruction Information for Patients Hip and Knee service Delivering Excellence Contents Page The classic injury 3 Why does the anterior cruciate ligament fail to heal? 4 Rationale
TOTAL HIP REPLACEMENT
 TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
TOTAL HIP REPLACEMENT 2 Causes of Hip Pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that
No two knees are alike. That s why we personalize your surgery just for you. Zimmer Patient Specific Instruments. For Knee Replacement Surgery
 No two knees are alike. That s why we personalize your surgery just for you. Zimmer Patient Specific Instruments For Knee Replacement Surgery Table of Contents Here s how it works....2 Why does my knee
No two knees are alike. That s why we personalize your surgery just for you. Zimmer Patient Specific Instruments For Knee Replacement Surgery Table of Contents Here s how it works....2 Why does my knee
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
Total elbow joint replacement for rheumatoid arthritis: A Patient s Guide
 www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
www.orthop.washington.edu TABLE OF CONTENTS 1 Overview 2 Review of the condition 3 Considering surgery 5 Preparing for surgery 6 About the procedure 8 Recovering from surgery 9 Convalescence and Rehabilitation
TOTAL KNEE REPLACEMENT
 PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME
 KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
KNEE ARTHROSCOPY POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The arthroscope is a fibre-optic telescope that can be inserted into a joint. A camera is attached to the arthroscope and the
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Arthroscopic Ankle Fusion (Arthrodesis)
 Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
Arthroscopic Ankle Fusion (Arthrodesis) Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed with ankle arthritis and
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Rehabilitation guidelines for patients undergoing knee arthroscopy
 Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Rehabilitation guidelines for patients undergoing knee arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We also want
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Recovering from a broken hip
 Recovering from a broken hip Information for patients, relatives and carers Who will will look look after after me me during during my hospital my hospital stay? stay? A multidisciplinary team of healthcare
Recovering from a broken hip Information for patients, relatives and carers Who will will look look after after me me during during my hospital my hospital stay? stay? A multidisciplinary team of healthcare
