Ramesh Rengan MD PhD Department of Radiation Oncology University of Washington ASTRO Spring Refresher Course March 8, 2014
|
|
|
- Ashley Bennett
- 8 years ago
- Views:
Transcription
1 The Management of Lung Cancer Ramesh Rengan MD PhD Department of Radiation Oncology University of Washington ASTRO Spring Refresher Course March 8, 2014
2 Overview Introduction Screening and Workup Early Stage NSCLC Operable Medically Inoperable Locally Advanced NSCLC Surgery-based options for IIIA Disease Inoperable Small Cell Lung Cancer Conclusions
3 Introduction: The Scope of the Problem 213,380 patients are diagnosed yearly with lung cancer in the US with approximately 160,390 deaths
4 Introduction: The Scope of the Problem Stage at Diagnosis 5-year Survival Localized Regional Distant Adapted from Jemal et al. CA Cancer J. Clin 57: (2007)
5 The Challenge of Treating NSCLC Lung cancer is aggressive Normal lung is very radiosensitive The lung is a vital organ The uninvolved lung doesn t work
6 Improving Clinical Outcome local control toxicity PROBABILITY Treatment Intensification DOSE OF RADIATION
7 Improving Clinical Outcome Disease Control toxicity PROBABILITY Treatment Intensification (more RT; more chemo; surgery) Treatment Intensity
8 Screening and Diagnostic Workup
9 Screening Early lung cancer detection cure CT is effective in detecting early lung cancer However: Prior studies of CXR: No mortality advantage Studies demonstrating increased survival subject to lead time and over diagnosis bias etc Impact of false positive studies?
10 Screening NLST Protocol Schema Annual Interim Analyses : 4/2006-4/2010 Final: October 2010
11 Kaplan-Meier curves for lung cancer mortality Probability of survival: ALL participants Years from randomization CT arm CXR arm
12 Lung cancer case survival Kaplan Meier curve Probability of survival: Participants with lung cancer Years from randomization CT arm CXR arm
13 Kaplan-Meier curves for all-cause mortality Probability of survival: ALL participants Years from randomization CT arm CXR arm
14 Diagnostic Workup: Patient Selection Stage IIIA/IIIB NSCLC N=153 PET - PET+ Hicks et al JNM 2001
15 Diagnostic Workup: Impact of mediastinal nodal involvement 5yr OS Stage IA 75% Stage IB 55% Stage IIA 50% Stage IIB 40% Stage IIIA 10-35% Stage IIIB 5-8% Stage IV <5%
16 Invasive staging of mediastinum: cervical mediastinocopy Gold standard is surgical staging with cervical mediastinoscopy Sensitivity is 44-92% with 100% specificity Invasive procedure Risk of complications (rare) Requires skilled thoracic surgeon (operator dependent) Often omitted in inoperable patients
17 Diagnostic Workup: Methods for staging mediastinum Mediastinal LN Biopsy Lymph Node Levels EBUS-FNA EUS-FNA Mediastinoscopy: Cervical Mediastinoscopy: Chamberlain
18 Diagnostic Workup: Mediastinoscopy vs EBUS ASTER Trial Rx 241 NSCLC pts Resectable No PET+ LNs Mediastinoscopy EBUS Rx Mediastinoscopy Rx Thoracotomy Combination of EBUS + Mediastinoscopy had higher sensitivity (94%) than Mediastinoscopy alone (79%) or EBUS alone (85%) (p=0.02) EBUS alone vs mediastinoscopy alone: no difference in lymph node sensitivity 18% vs 7% futile thoracotomy rate in the mediastinoscopy vs EBUS group (p=0.02) Annema et al JAMA 2010
19 Diagnostic Workup: Impact of mediastinal nodal involvement Is PET alone adequate for staging the mediastinum? INVASIVE SEN SPEC SEN SPEC CT PET/CT PET/CT with LAD (22%FDGavid; but neg) MED EBUS- TBNA Kim et al JTO S2:S Kramer et al Ann. Surg. 238: PET/CT without LAD 75 (25% not FDG avid) 93 Gould et al AIM 139:
20 Diagnostic Staging and Workup: Summary points Staging workup should include PET/CT for all lung cancer patients For all non-metastatic patients invasive staging of the mediastinum should be performed when possible Including all medically inoperable patients UW approach All patients undergo PET/CT All patients undergo invasive staging Operable patients undergo additional mediastinoscopy Subset of inoperable patients undergo EBUS-TBNA alone
21 Early Stage Disease Stage IA/IB
22 Early Stage Operable Disease 276 patients, intraoperatively T1N0 Lobectomy vs limited resection registered 771 patients (clinical T1N0), but excluded 495 due to benign disease, tumor location, size or nodal status. LCSG showed trend towards increased likelihood of death with limited resection LCSG showed three-fold increase in local failure with wedge resection vs. lobectomy
23 Early Stage Operable Disease: High Risk Patients
24 Early Stage Operable Disease: High Risk Patients Is there a lumpectomy for the lung?
25 Early Stage Operable Disease: High Risk Patients
26 Source: ACOSOG Website
27 Studies of Brachytherapy Author Number of patients Local Recurrence Santos (Surg 2003;134:691-6) 102 2% Lee (Ann Thorac Surg 2003;75:237-42) %
28 Z4032 A Randomized Phase III Study of Sublobar Resection (SR) vs Sublobar Resection plus Brachytherapy (SRB) in High-risk patients with NSCLC, 3cm or smaller
29 Z4032: A Randomized Phase III Study of Sublobar Resection (SR) vs Sublobar Resection plus Brachytherapy (SRB) in High-risk patients with NSCLC, 3cm or smaller There was no significant difference between the arms in time to local recurrence (HR = 0.87; 5% CI: 0.41, 1.86, p=0.72). There was no difference in the rate of local recurrence between SR and SRB arms (12.8% versus 12.5%, p=0.94). There was no difference in the location of local recurrence between SR and SRB arms: At the staple line (6.4% versus 4.8%, p=0.94); away from the staple line (3.7% versus 3.8%, p=1.00); nodal (1.8% versus 3.8%, p=0.44). SRB did not reduce the rate of local recurrence in patients with a compromised surgical margin (margin < 1cm; margin:tumor ratio <1; positive staple line cytology). There was no significant difference in overall survival between SR (71%) and SRB (72%) (p=0.81) at 3 years. Brachytherapy does not improve clinical outcome over SR alone in this patient population ASCO 2013
30 Surgery - Medically Inoperable Cor pulmonale Severe coronary artery disease Renal failure Poor pulmonary function DLCO <50% FEV1/FVC ratio < 50 75% of predicted Impaired nutritional status
31 Medically Inoperable Early Stage: Role of RT Study n Dose 5-yr Author (Gy) survival Dosoretz % 5-yr CSS 5-yr local Krol % 31% 25% Kaskowitz % 13% 0% Sibley % Rosenzweig % 39% 43%
32 Medically Inoperable Early Stage: Stereotactic Body Radiotherapy Nyman et al Lung Cancer 2006
33 SBRT: Indiana University Phase II Trial 70 patients ct1/t2 NO Medically Inoperable NSCLC 35 patients ct1n0 20Gy x 3 35 patients ct2n0 22Gy x 3 Safety Preliminary Efficacy Safety Preliminary Efficacy
34 Early Stage NSCLC, Medically Inoperable: Is SBRT Effective? Indiana U., Phase II (Timmerman, et al.): efficacy Local Control 95% at 2yrs 88% at 3 yrs Overall Survival 55% at 2yrs 43% at 3 yrs JCO, 2006
35 Medically Inoperable Early Stage: Hypofractionated Stereotactic Radiation Author # of Patients Overall Survival Onishi et al % (3-yr) Timmerman 70 55% (2-yr) Nyman 45 71% (2-yr) Xia 43 78% (3-yr) Nagata 31 79% (2-yr) Uematsu 50 66% (3-yr) Fukumoto 25 47% (2-yr) Wulf 20 32% (2-yr)
36 Grade 3-5 Toxicity: Location p = 0.003
37 SBRT: Central Lesion Toxicity
38 Medically Inoperable Early Stage: Hypofractionated Stereotactic Radiation Correspondence Central-Airway Necrosis after Stereotactic Body-Radiation Therapy N Engl J Med 2012; 366:
39 Median follow-up of 35 months No grade IV/V toxicities Central lesion SBRT
40 SBRT Dose and IGRT
41 SBRT Dose and IGRT JTO patients receiving SBRT for early stage NSCLC All patients underwent daily OBI with CBCT LR was 4% for BED 105 or greater 12Gy x 4 (BED=105.6 Gy); 20Gy x 3 (BED=180Gy); 10Gy x 5 (BED=100Gy) BED 10 = nd(1 + d/10) α/β=10
42 SBRT Dose and IGRT Radiation Therapy Oncology Group (RTOG) Protocol 0915: A Randomized Phase II Study Comparing 2 Stereotactic Body Radiation Therapy (SBRT) Schedules for Medically Inoperable Patients with Stage I Peripheral Non-Small Cell Lung Cancer Videtic ASTRO Gy x 1 (Arm 1) vs 12Gy x 4 (Arm 2) 86 evaluable patients (41 in arm 1, 45 in arm 2) Median follow up was 20.6 months OS at 1 year was 85.4% (95% CI: %) for arm 1 patients and 91.1% (95% CI: %) for arm 2 PFS at 1 year was 78.0% (95% CI: %) for arm 1 and 84.4% (95% CI: %) for arm 2 The PC rates at 1 year were 97.1% (95% CI: %) for arm 1 and 97.6% (95% CI: %) for arm 2 Both regimens are safe and effective 34Gy x 1 will be experimental arm in next RTOG phase III trial
43 SBRT and IGRT Grills et al IJROBP patients treated with SBRT with CBCT Compared setup with tattoo alone vs CBCT CBCT reduced margin requirements from 9-13mm to 1-2mm
44 SBRT and IGRT 87 patients receiving SBRT for medically inoperable stage I NSCLC Determine need for CBCT over KV-KV matching along IGRT procedure: position with KV-KV; then perform CBCT ~20% of patients required shift of 3mm or greater after KV-KV Conclusion: CBCT is critical to avoid marginal misses in SBRT Corradetti et al PRO 2012
45 SBRT For Operable Disease
46 SBRT for Operable Disease Grills et al JCO 2010 Similar local control, locoregional control and CSS to wedge
47 SBRT for Operable Disease RTOG 0618:Stereotactic body radiation therapy (SBRT) to treat operable early-stage lung cancer patients (ASCO 2013) 18Gy x 3 33 patients enrolled, 26 evaluable 2-year local failure 7.7%; OS 84% One patient required surgical salvage with lobectomy for recurrence RTOG 1021: SBRT vs sublobar resection- closed due to poor accrual ROSEL: SBRT vs surgical resection (lobectomy or sublobar)- closed due to poor accrual
48 SBRT: Practical Considerations Dose and fractionation Peripheral lesions 12Gy x4 to 20Gy x 3 all reasonable (BED > 105Gy) Simulation 4DCT is essential to account for tumor motion Margins IGTV PTV usually 3-5mm margin IGRT Volumetric IGRT is essential given small # of fractions and small margins Grills et all (IJROBP); Corradetti et al (PRO 2012)
49 My approach 12.5Gy x 4 for peripheral lesions 10Gy x 5 for apical or chest wall proximate lesions Chest wall invasion treated with standard fractionation 7.5Gy x 5 for central lesions on registry protocol RTOG SBRT: Practical Considerations Proton trial in development for central lesions (Simone PI) Gy x 4 vs 30Gy x 1 showed equivalent control results ~97% LC in both arms; similar toxicity (ASTRO 2013) 0813 pending 10Gy x 5 for centrally located lesions Grade 5 toxicities have been observed 0618 pending for operable early stage
50 Early Stage NSCLC IA/IB: Good pulmonary function: lobectomy Marginal function: sublobar resection Inoperable: High-dose radiation alone IIA/B: Surgery or RT with either neoadjuvant or adjuvant chemotherapy
51 LOCALLY ADVANCED NSCLC
52 Locally Advanced NSCLC T 3 N1 Positive ipsilateral hilar/ peribronchial nodes (N1) T 1-2-3, N2 Positive ipsilateral mediastinal/ subcarinal nodes (N2) T4, N0-3, M0 Locally invasive Pleural/ pericardial effusion Satellite nodules in primary-tumor lobe T1-4, N3, M0 Contralateral mediastinal/ hilar nodes Any scalene or supraclavicular nodes
53 Treatment of IIIA: Surgery Based Options Surgery Chemo +/-RT -Chemo (IALT/ANITA) - RT (PORT/ANITA) Chemo Surgery -Roth, Rosell, -Depierre Chemorads surgery - Albain, Rusch
54 Adjuvant Chemotherapy N=1867 I(.36)-II(.25)-III(.39) NSCLC R0 resections Observation ( 935) cddp based ( 922) +/- RTx < 60 Gy Le Chevalier, NEJM 2004
55 Adjuvant Chemotherapy IALT n= countries, initial accrual goal was /20 M/F Mean age 59 Squamous 47%, ACAs 40% Chemo to start < 60 days after surgery Median f/up is 56 months Le Chevalier, NEJM 2004
56 Adjuvant Chemotherapy IALT N= chemo Control Median Survival (months) Median DFS (months) OS 5 years (%) Le Chevalier, NEJM 2004
57 Surgery Chemotherapy Cisplatin-based CT for completely resected disease IALT pts with resected stage I-III: Post-op cis-based CT vs observation, ~25% received post op XRT 5 year OS improved at 45% versus 40% (p = 0.03) ANITA pts with resected stage Ib-III: Post-op cis/ VLB x4 vs observation 5 year OS improved at 42% vs 26% for stage IIIA patients Arriagada R et al. N Engl J Med Jan 22;350(4): Douillard JY, Lancet Oncol Sep;7(9):
58 Surgery XRT Adjuvant XRT in IIIA Disease Lung Cancer Study Group pts with stage II or III squamous cell lung cancer Randomized post-op to XRT (50Gy) vs observation local recurrence, but no improved OS PORT Meta-analysis 1998 updated in trials that compared adjuvant XRT to observation Accrual , stage I-III pts, XRT 30-60Gy 18% increased risk of death in XRT group Subset analysis: No OS difference in stage III N Engl J Med Nov 27;315(22): Lancet Jul 25;352(9124):
59 PORT Meta-Analysis
60 PORT Meta-Analysis: Impact 65% 51% 37% 19% 8% 4% Bekelman et al IJROBP 2006
61 PORT Meta-Analysis: A Closer Look Radiation Treatment Details PORT Meta-Analysis 3D-CRT
62 PORT Meta-Analysis Is this Is this result really at all surprising? RELEVANT?
63 PORT: Who can benefit? Not detrimental in N2 disease
64 PORT: Who can benefit? N2 Patients 1987 patients PORT p= OBS Lally et al JCO 2006
65 PORT in the era of chemotherapy: Is there a role? ANITA
66 Surgery XRT Summary Post op chemo for stage III disease: IALT/ANITA Post op chemort for surprise N2 disease: Using modern RT techniques 5040cGy for R0 resection Start RT 4-6 weeks after last cycle of chemo Post op chemort for positive margins 6120cGy Start RT first alone or with concurrent chemotherapy 4-6 weeks after surgery
67 Treatment of IIIA: Surgery Based Options Surgery Chemo +/-RT -Chemo (IALT/ANITA) -RT (PORT/ANITA) Chemo Surgery -Roth, Rosell, -Depierre Chemorads surgery - Albain, Rusch
68 Neoadjuvant Chemotherapy: Rationale Surgical Rationale Initial response may facilitate local therapy Reduced incidence of (+) surgical margins Potential use of less radical surgery and organ preservation Chemotherapy/Systemic Rationale Improved drug delivery through intact vasculature Possible eradication of occult regional and distant micrometastases Useful in vivo assessment of tumor responsiveness: implications for molecular staging and further treatment
69 Induction Chemotherapy + Surgery in Stage III NSCLC: Results of Randomized Trials Investigators RX # Pts. Resect Rate (%) Med Surv (mo) 5-yr Surv (%) Pass et al (1992) Surgery CT+Surgery Roth et al (1994) Surgery CT+Surgery Rosell et al (1994) Surgery CT+Surgery Depierre et al (1999) Surgery CT+Surgery NR Roth JA, J Natl Cancer Inst May 4;86(9): Rosell R, N Engl J Med Jan 20;330(3): Depierre A, J Clin Oncol Jan 1;20(1):
70 Chemo Surgery Summary If operable and goal is to get to surgery for N2 disease: Platin doublet surgery chemo/rt as indicated My Approach regarding post-operative therapy: Deliver PORT after surgery if residual N2 disease is identified If multiple nodes are identified, consider additional adjuvant chemotherapy (switch regimen) Observe patients who obtain clearance of mediastinum (~30%)
71 Treatment of IIIA: Surgery Based Options Surgery Chemo +/-RT - Chemo (IALT/ANITA) - RT (ANITA) Chemo Surgery - Roth, Rosell, - Depierre Chemorads surgery - Albain, Rusch
72
73 INT 0139: Definitive CT/RT vs Induction CT/RT Surgery for Stage IIIA NSCLC Stage IIIA (T1-3, pn2, M0) NSCLC N = 429 (396 eligible) R A N D O M I Z E Cis/VP16 x 2 cycles w/concurrent XRT 45Gy Cis/VP16 x 2 cycles w/concurrent XRT 45Gy Re-evaluate 2 to 4 weeks post RT; if no PD Surgery Continue RT to 61GY Re-evaluate 7 days prior to RT completion; if no PD Cis/VP16 x 2 cycles Cis/VP16 x 2 cycles Albain et al. Lancet
74 Lung Intergroup Trial 0139 Objectives 1. Determine if resection after CT/RT results in improved outcome compared to CT plus full-course RT (arms based on SWOG 8805 and SWOG 9019) 2. Analyze progression-free, overall, and long-term survival; toxicity; and patterns of failure
75 Trimodality therapy: The Results of INT 0139 A CT/RT/S CT/RT B CT/RT/S CT/RT HR= %CL ( ) p=0.017 HR= %CL ( ) p=0.24 Progression-free survival (A) and overall survival (B) of intention-to-treat population CT/RT/S=chemotherapy plus radiotherapy followed by surgery (group 1,n=202). CT/RT=chemotherapy plus radiotherapy (group 2, n=194). median follow-up for all patients was 22 5 months (range ) Albain et al Lancet 2009
76 Trimodality therapy: The Results of INT 0139 Pathological N0 (n=76) Pathological N1 3, unknown (n=88) No surgery (n=38) 38/202= 18% of patients MS= 7.9 Months 5-yr survival= 3% (point estimate) Albain et al Lancet 2009
77 The Risks of Trimodality Therapy Preoperative Chemoradiotherapy 45 to 50Gy 4-6 weeks
78 The Risks of Trimodality Therapy 4-6 weeks 15-20Gy? Surviving Cells After 45-50Gy Minimal chance of cure
79 45% (13/29) of T0N0 pts underwent pneumonectomy Albain et al ASCO 2005
80 INT 0139 Exploratory Survival Analysis All but 1 postoperative death followed a pneumonectomy Hypothesized survival advantage for CT/RT/S if lobectomy performed and for CT/RT if pneumonectomy Patients on CT/RT/S were matched with those on CT/RT arm on 4 prestudy factors (KPS, age, sex, T stage); match feasible for 90/98 lobectomies and 51/54 pneumonectomies
81 INT 0139 Overall Survival of Pneumonectomy Subset versus Matched CT/RT Subset % Alive MS 3 yr OS 5 yr OS / / / CT/RT/S 19 mos. CT/RT 29 mos. 36% 45% 22% 24% Months from Randomization logrank p = NS / / / / Dead/Total CT/RT/S 38/51 CT/RT 42/51 / / / Albain, et al. Lancet 2009
82 INT0139 Overall Survival of the Lobectomy Subset versus Matched CT/RT Subset 100 Dead/Total 75 CT/RT/S 57/90 CT/RT 74/90 % Alive 50 // Logrank p = / / / / / / / / / / 25 / / / / CT/RT/S CT/RT / / / / / 0 MS 34 mos. 22 mos. 5 yr OS 36% 18% Months from Randomization
83 INT0139 Overall Survival Matched CT/RT Subset CT/RT (Pneumonectomy) % Alive 50 CT/RT (Lobectomy) 25 0 MS 5 yr OS CT/RT (Pneumonectomy) 29 mos. 24% CT/RT (Lobectomy) 22 mos. 18% Months from Randomization
84 Issues with this exploratory analysis Unplanned and retrospective Matching criteria are not necessarily valid Cannot reliably predict a priori who will require lobectomy vs pneumonectomy 45% of pt0n0 patients in trimodality arm underwent a pneumonectomy
85 ChemoXRT Surgery Summary Trimodality therapy is stressful! Coordination with surgeon and medonc from day 1 Trimodality therapy should not be used to convert a marginally resectable patient to resectable This approach only applies to resectable patients Surgery has to be planned from the start Absolute contraindication if patient requires a right pneumonectomy Lobectomy candidates may benefit from this approach Needs to be confirmed in a prospective trial Albain KS, Lancet, 2009
86 ChemoXRT Surgery (Superior Sulcus) SWOG 9416/Intergroup 0160 (Rusch) 111 pts superior sulcus T3-4N0-1, (-) MEAD 2 cycles of Cis/etop + 45 Gy concurrent RT Responder underwent resection 3-5 weeks later followed by 2 additional cycles of adjuvant chemotherapy 95/83 had a thoracotomy and 76 (92%) had a complete resection 54 (65%) showed pcr or microscopic residual disease 2 yr OS 55% for all patients and 70% for those with complete resection Rusch VW et al. J Thorac Cardiovasc Surg Mar;121(3):
87 Operable Stage IIIA Disease Chemotherapy/Surgery vs Chemoradiotherapy?
88 Operable Stage IIIA Disease EORTC 08941: STUDY DESIGN SURGERY IIIA NSCLC 579 pts unresectable N2 disease CDDP chemo 3 cycles Response assessment 332 responders RADIATION 60 Gy 6 weeks JNCI 2007
89 Operable Stage IIIA Disease SURGERY 16.4 MONTHS RADIATION 17.5 MONTHS NO DIFFERENCE
90 Definitive Chemoradiotherapy for Stage III
91 Treatment of IIIA/B: ChemoXRT Sequential Chemoradiotherapy Chemotherapy Radiotherapy vs RT alone Dillman, Sause Concurrent Chemoradiotherapy Concurrent chemoradiotherapy vs RT alone Schaake-Koning, Jeremic Sequential vs Concurrent Chemoradiotherapy Sequential vs Concurrent chemoradiotherapy RTOG 9410, Furuse, Fournel, Auperin meta-analysis Augmentation Strategies Chemotherapy Concurrent Chemoradiotherapy vs Concurrent Chemoradiotherapy CALGB Vokes Concurrent Chemoradiotherapy Chemotherapy vs Concurrent Chemoradiotherapy HOG/LUN Hanna Targeted Agent addition SWOG 0023 Local Augmentation RTOG 0617
92 Chemotherapy XRT CALGB 8433 Dillman RTOG Sause CEBI 138 LeChevalier N 77/ / 151/ / 176 Arms I XRT alone II Cis/VBL XRT I QD XRT II BID XRT III Cis/ VBL XRT I XRT alone II Chemo XRT Chemo* XRT 60 Gy 60 Gy (69.6 in BID) 65 Gy (2.5 Gy fx) MST (mo) 9.7/ 13.8 (SS) 11.4/ 12.0/ 13.2 (SS) 9/ 12 OS (% 2 yr) 13 / 26 (SS) 19/ 24/ 32 (SS) 14/ 21 (SS) OS (% 5 yr) 6/ 17 (SS) 5/ 6/ 8 (NS) 3/ 5 (NS) % LF Not analyzed 41/ 45/ 41 (NS) Not analyzed % DM Not analyzed 35/ 37/ 24 (p=0.045,ff) 40/ 27 (3yr) p<0.001 * sandwich regimen of induction chemotherapy with videstine/ lomustine/ cisplatin/ cyclophosphamide
93 Chemo XRT Relative to XRT alone: Significantly fewer distant mets demonstrated in RTOG and CEBI 138 No local control improvement with chemo Survival advantage likely due to delayed distant metastases 5 year OS still disappointing
94 Concurrent ChemoRT EORTC 8844 Shaake- Koning Jeremic, 1995 Jeremic, 1996 N 108/ 102/ 96 61/ 52/ 56 66/ 65 Arms I XRT alone II Cis qwk + XRT III Cis qday + XRT I XRT alone II Carbo/ VP16 q3wk + XRT III Carbo/ VP16 qwk + XRT I XRT alone II Carbo/VP16 qday + XRT XRT 55 Gy split BID to 64.8 Gy BID to 69.6 Gy MST (mo) 10.5/ 11/ 12.5 (p=0.009) 8/ 13/ 18 (p<0.05) 14/ 22 (p<0.05) OS (% 2yr) 13/ 19/ 26 (p=0.009) Not reported 24/ 43 (p<0.05) OS (% 3yr) 2/ 13/ 16 (p=0.009) 6.6/ 16/ 23 (p<0.05) 9/ 23 (4 year) (p<0.05) LRFS (%2y) 19/ 30/ 31 (p=0.003) 35/ 30/ 42 (p=0.76) 19/ 42 (4y,p=0.015) DMFS(%2y) 8/ 9/ 13 (p=0.16) 42/ 52/ 52 (p=0.54) 33/ 39 (4y,p=0.33)
95 Concurrent chemoradiotherapy Relative to XRT alone: Significantly improved LOCAL CONTROL demonstrated in EORTC and Jeremic No reduction in distant mets with chemo Survival advantage likely due to improved local control 5 year OS still disappointing
96 Sequential vs Concurrent Speaks directly to the question of the value of local control in locally advanced disease Concerns about increased toxicity with concurrent regimens
97 Sequential vs Concurrent RTOG 94-10: Curran et al pts, Stage II-III Cisplatin/vinblastine 60Gy vs cisplatin/vinblastine and concurrent 60Gy vs cisplatin/oral VP-16 with concurrent BID 69.6Gy Furuse et al NPC 95-01: Fournel et al 2005 Auperin meta-analysis Curran WJ et al. JNCI 2011 Furuse K et al. J Clin Oncol Sep;17(9): Fournel P et al. J Clin Oncol Sep 1;23(25): Auperin A, J Clin Oncol 2010 May 1;28(13):
98 Sequential vs Concurrent Furuse et. al. RTOG 9410 Curran NPC Fournel N 156/ total 103/ 102 Arms I cis/vind/mm XRT II cis/vind/mm + XRT I cis/vbl XRT II cis/ VBL + XRT III cis/vp16 + BID XRT I cis/vinor XRT II cis/vp16 + XRT cis/vinor X 2 XRT 56 Gy (split in arm II) 60 Gy (BID to 69.6) 66 Gy MST (mo) 13.3/ 16.5 (p<0.05) 14.6/ 17.0 (SS)/ / 16.3 (NS) OS (% 3yr) 14.7/ 22.3 (p<0.05) 17/ 26/ / 24.8 (p=0.24) OS (% 5yr) 8.8/ 15.8 (p<0.05) 12/ 21 (SS)/ 17 (4 yr) 14/ 20.7 (4 yr) (NS) % LF 39/ 33 (p = 0.27) 65/56/47 70/ 53 (p = 0.17) % DM No significant diff Not available 47/ 58 (p = 0.17)
99 Sequential vs Concurrent: Meta-analysis 1205 patients pooled Median f/u 6 years OS benefit with concurrent chemo RT (HR 0.84, SS); 3- years absolute benefit 5.7% (18% to 24%), 5-years 4.5% (11% to 15%) Auperin A, J Clin Oncol 2010 May 1;28(13):
100 Sequential vs Concurrent: Meta-analysis Decrease in locoregional progression (HR 0.777, SS); absolute decrease of 6% at 5 years (35% to 29%) No difference in PFS (HR 0.9, p=0.07). No difference on distant progression (HR 1.04, NS), with 5-year rate of ~40% Toxicity: Acute Grade 3-4 esophageal toxicity worse (RR 4.9, SS), increase from 4% to 18%; no significant difference in acute pulmonary toxicity
101 Concurrent ChemoXRT Summary OS improved with concurrent chemoxrt (with platinum based chemo) Improvement in local control demonstrated in EORTC and by Jeremic (1996) Toxicity tolerable for selected patients
102 Concurrent Chemoradiotherapy: Augmentation Strategies Systemic Augmentation Cytotoxic chemotherapy Induction chemotherapy Chemoradiotherapy CALGB Concurrent chemoradiotherapy Consolidative chemotherapy HOG/LUN trial Targeted agents Concurrent chemoradiotherapy Gefitinib SWOG 0023 Local Augmentation Surgery Concurrent chemoradiotherapy Surgery INT 0139 (Albain) RT Dose Concurrent chemoradiotherapy 60Gy vs 74Gy RTOG 0617
103 Systemic Augmentation: Induction chemotherapy JCO 2007 Inoperable Stage IIIA/IIIB patients CALGB PS 0 or 1 No weight loss exclusion
104 Systemic Augmentation: Induction chemotherapy No significant differences in survival ITT MS 12 vs 14 months (p=ns) Good PS <5% weight loss MS 16 vs 14 months (p=ns) Toxicity Maximum toxicity reported were higher with induction (40% vs 26% G4) p=0.004
105 Hanna N, et al. JCO Systemic Augmentation: Consolidation chemotherapy HOG LUN 01-24/USO ChemoRT Cisplatin 50 mg/m 2 IV d 1,8,29,36 Etoposide 50 mg/m 2 IV d 1-5 and Concurrent RT 59.4 Gy (1.8 Gy/fr) Stratification variables: PS 0-1 vs 2 IIIA vs IIIB CR vs non-cr R A N D O M I Z E Docetaxel 75 mg/m 2 q3 wk x 3 Observation Study end points Primary: Overall survival accrue 210 to demonstrate an increase in MST from 15 mo 24 mo with > 80% power Secondary: Progression-free survival and toxicity
106 Systemic Augmentation: Consolidation chemotherapy 100% Percent of patients surviving 75% 50% 25% Observation: Median: 24.1 ms ( ) 3 year survival rate: 27.6% Docetaxel: Median: 21.5 ms ( ) 3 year survival rate: 27.2% P-value: % Observation Docetaxel Consolidation Months since registration
107 Systemic Augmentation: Targeted Agents SWOG 0023 R A N D O M I Z E D Definitive TX Consolidation Maintenance CDDP/VP-16 XRT docetaxel PLACEBO PLACEBO GEFITINIB CDDP/VP-16 XRT docetaxel Gefitinib
108 Local Augmentation: More RT Dose INST. No. of Patients Stage III (%) Dose (Gy) ENI Induction (%) Esophagitis Grade 3 (%) Median Survival (months) Duke Yes 27 3 IIIA 13.0 IIIB 10.0 UM No 24 7 III 16.0 RTOG No 14 3 NR Shanghai Yes Carolina Yes CALGB Yes Concurrent MSKCC No
109 Local Augmentation: More RT Dose RTOG 0617 A Randomized Phase III Comparison of Standard Dose (60 Gy) Versus High-Dose (74 Gy) Conformal Radiotherapy with Concurrent and Consolidation Carboplatin/Paclitaxel +/- Cetuximab In Patients with Stage IIIA/IIIB Non-Small Cell Lung Cancer Intergroup Participation: RTOG, NCCTG, CALGB
110 Schema S T R A T I F Y RT Technique 1. 3D-CRT 2. IMRT Zubrod PET Staging 1. No 2. Yes Histology 1. Squamous 2. Non- Squamous R A N D O M I Z E Concurrent Treatment Arm A Concurrent chemotherapy* RT to 60 Gy, 5 x per wk for 6 wks Arm B Concurrent chemotherapy* RT to 74 Gy, 5 x per wk for 7.5 wks Arm C Concurrent chemotherapy* and Cetuximab RT to 60 Gy, 5 x per wk for 6 wks Arm D Concurrent chemotherapy* and Cetuximab RT to 74 Gy, 5 x per wk for 7.5 wks Consolidation Treatment Arm A Consolidation chemotherapy* Arm B Consolidation chemotherapy* Arm C Consolidation chemotherapy* and Cetuximab Arm D Consolidation chemotherapy* and Cetuximab *Carboplatin and paclitaxel
111 Primary Objective To compare the overall survival of patients treated with high-dose versus standard-dose conformal radiation therapy with concurrent chemotherapy. To compare the overall survival of patients treated with cetuximab versus without cetuximab with concurrent chemoradiotherapy.
112 Pretreatment Characteristics 60 Gy 74 Gy (n=213) (n=206) Age (median) Gender Male 125 (58.7%) 120 (58.3%) Female 88 (41.3%) 86 (41.7%) Race Other 26 (12.2%) 29 (14.1%) White 187 (87.8%) 177 (85.9%) RT Technique 3DCRT 115 (53.9%) 109 (52.9%) IMRT 98 (46.1%) 97 (47.1%) PET Staging 91.1% 88.8% Histology Adenocarcinoma 84 (39.4%) 71 (34.5%) Squamous 89 (41.8%) 97 (47.1%) NSCLC NOS 40 (18.7%) 38 (18.4%) AJCC Stage Stage IIIA 143 (67.1%) 131 (63.6%) Stage IIIB 70 (32.9%) 75 (36.4%)
113 Overall Survival Survival Rate (%) Patients at Risk Standard High dose 0 HR=1.56 (1.19, 2.06) p= Months since Randomization Standard (60 Gy) High dose (74 Gy) Dead Total Median Survival Time 28.7 months 19.5 months Month Survival Rate 66.9% 53.9%
114 RTOG 0617: Dosimetric Data Distribution 60 Gy (n=203) Mean (Median) 74 Gy (n=197) Mean (Median) GTV Volume (cc) (92.2) (96.4) Heart V5 (%) 47.4 (45.7) 45.6 (46.1) Heart V50 (%) 7(4.2) 11(5.6) Lung V20 (%) 28.7 (28.8) 30.9 (31.9) Esophagus Dose (Gy) 24.7 (25.1) 29.8 (28.9) Esophagus V60 (%) 15 (13) 25.6 (25.7) Mean Margin CTV to PTV (mm) 7.9 (6.6) 7.7 (6.6)
115 Local Failure 100 Local Progression Rate (%) Standard (60 Gy) High dose (74 Gy) HR=1.37 (0.99, 1.89) Fail Total p= Month Local Progression Rate 34.3% 25.1% 0 Patients at Risk Standard High dose Months since Randomization
116 Multivariate Cox Model Covariate Comparison (RL) HR (95% CI) p-value Radiation dose 60 Gy v 74 Gy 1.51 (1.12, 2.04) Histology Non-squam v Squam 1.31 (0.99, 1.75) Max esophagitis grade <3 vs (1.06, 2.20) Heart Contour Per Protocol vs. Not per protocol 0.67 (0.47, 0.96) GTV Continuous (1.000, 1.002) Heart V50(%) Continuous (1.004, 1.030) Backwards Selection: Exit criteria p>0.10 Two-sided p-values Removed from model: Age (continuous), overall RT review (per protocol vs. not per protocol), and lung V5 (continuous)
117 My interpretation Level 1 evidence against high dose is compelling in unselected stage III NSCLC Prospective trials aimed at adaptive dose escalation are underway Difficult to justify doses of 70Gy and beyond Although improving local control is still important My standard is 6660cGy/180cGy fraction for locally advanced NSCLC
118 HYPOFRACTIONATION
119 HYPOFRACTIONATION 79 patients enrolled all treated with IFRT 57 to 85.5Gy in 25 fractions Involved field only Median f/u 17 months MTD is maximum dose that yielded <20% risk of severe toxicity MTD was (second dose level) Cannon et al JCO 2013 MS was 16 months, 3-year survival 29%
120 Locally Advanced NSCLC: What is the right dose? 4/8/07: New diagnosis of NSCLC. Undergoes bronchoscopy with biopsy and debulking and diagnostic thoracentesis Post-RT 4/18/07 Seen CT in of RadOnc Chest by me. rt Undergoes change PET/CT only- no residual disease 4.5 x 3.8 intensely FDG-avid mediastinal nodal conglomerate RLL primary tumor; small non-fdg avid nodules in RML Date of Scan: 2/26/13 Malignant PE confirmed (small volume) Simulated for RT to encompass mediastinal nodes and RLL tumor 4/22/07 Presents to ED with hemoptysis. Repeat bronch shows complete recurrence of right BI tumor Dose received: 250 x 14 (3500cGy) from 4/23-5/ /23 started RT to mediastinal conglomerate and dominant RLL mass
121 Target Delineation and IGRT
122 Locally Advanced NSCLC: Treatment Volume Rosenzweig et al JCO 2007 Fernandes et al R&O 2010 What is the right volume? IFRT vs ENI Most studies show EN failure rate to be 4-8% IFRT reduces toxicity
123 Target Delineation CT simulation Identification of Occult Tumor FDG-PET scan CT - defined PTV Register Derive GTV - PTV Paraesophageal node seen on PET, but not CT Treatment planning
124 Target Delineation The importance of image registration
125 Target Delineation Concordance Rate Non-registered: 61% Concordance Rate Registered: 70% p<0.05 Fox et al IJROBP 2005
126 Treatment Delivery: IGRT IJROBP 2012 Grade 3: Tumor outside PTV Grade 2: Tumor inside PTV Grade 1: Tumor inside IGTV Grade 0: Tumor inside GTV CBCT with carina match was superior to both CBCT spine and tattoos
127 Locally Advanced NSCLC: Practical Considerations RT Dose Gy in 1.8Gy/ fraction (RTOG 0617) Simulation 4D PET/CT simulation Target Delineation IFRT as defined on PET/CT (Fox et al IJROBP) IGRT Daily CBCT with match to carina (PMH IJROBP) Chemotherapy Platin doublet, given concurrently. No clear role for induction or consolidation
128 Locally advanced NSCLC: Summary local control toxicity PROBABILITY Treatment Intensification DOSE OF RADIATION
129 Locally advanced NSCLC: Summary Disease Control toxicity PROBABILITY We may have reached a therapeutic plateau for treatment intensification in locally advanced disease (More RT- 0617; Induction chemo-calgb 39801; Consolidation chemo- HOG Surgery- 0139) Treatment Intensification (more RT; more chemo; surgery) Treatment Intensity
130 Locally advanced NSCLC: Summary All treatments are equally good/bad Patient KPS, tumor burden, institutional preference all play a role UW approach: Concurrent chemoradiotherapy with cisplatin/etoposide for excellent PS patients Concurrent chemoradiotherapy with carbo/taxol for intermediate PS patients Poor PS patients sequential chemoradiotherapy Until systemic therapy improves local treatments will have diminished importance
131 Small Cell Lung Cancer
132 Background JCO 2006 ~15% lung cancers are small cell Declining in incidence SEER database reports SCLC cases declined from 17% to 13% in the past 30 years Female incidence is increasing Risk factors: SMOKING, uranium exposure, radon exposure
133 Clinical Presentation Symptoms related to central location: SOB, cough, dyspnea, chest pain, PNA, hoarseness, dysphagia, SVC syndrome Hemoptysis less common because of submucosal location Radiographs Usually is a large central lesion Usually with extensive lymphadenopathy 2/3 present with mets at diagnosis: Bone, liver, adrenals, bone marrow, brain
134 LS-SCLC: Malignant Pleural Effusion Veteran s Affairs Lung Study Group Limited SCLC (L-SCLC) 1/3 Confined to one hemithorax Regional nodes that can be encompassed in a reasonable radiation port May include ipsilateral SCV Nodes Extensive SCLC (E-SCLC) 2/3 Including Malignant Pleural Effusion Marburg Definition Included patients with small pleural effusion Defined a separate cohort ED I (Large volume disease, malignant PE); ED2 had distant mets LS and EDI had similar median survival ~12 vs ~11 months ED2 had poorer survival ~6 months
135 Initial Workup CT: Chest, including adrenals MRI Brain (including asymptomatic pts) Positive in ~8% of asymptomatic patients PET/CT (~10% of patients are upstaged from LS to ES and 25% reveal unsuspected nodal mets that could alter RT plan) Survival advantage to PET stage LS-SCLC (Xanthopoulos et al in press) CBC, CMP, LDH Consider bone marrow biopsy if counts are low PFT s
136 Outcomes Untreated: Median survival time of patients with unresectable disease randomized to receive supportive care only L-SCLC: 12 weeks E-SCLC: 5 weeks Stage Complete Response Median Survival 2 yr OS L-SCLC 60-75% months E-SCLC 20-35% 6-12 months 25-50% 1-2% DeVita et al. Principles and Practice of Oncology, 2008
137 Treatment Overview LIMITED STAGE Etoposide + cisplatin or carboplatin (4-6 cycles) Concomitant RT (twice-daily if feasible) COMPLETE RESPONSE PCI Observe for progression Smoking cessation If long term remission, surveillance for 2nd primary PARTIAL RESPONSE Observe for progression Smoking cessation EXTENSIVE STAGE Etoposide + cisplatin or carboplatin (4-6 cycles) PROGRESSION (Performance status 0-2) Topotecan or CAV
138 Surgery STCVS 2006 What about the role of surgery? Historically, surgery had little to no role Recent data suggests good survival in stage I patients Penn approach- surgery not used except if incidental at thoracotomy Chemotherapy is still given postoperatively, followed by PCI
139 Radiotherapy in LS-SCLC
140 Role of Radiation 13 randomized trials, 2140 patients Limited disease only 5% improvement in overall survival at 3 yrs Trend favored benefit for younger patients Meta-Analysis of Thoracic Radiotherapy Pignon, NEJM, 1992
141 Timing: Early vs. Late JCO 2004 Early thoracic radiotherapy is superior Early definied as starting Cycle 1 or Cycle 2; less than 9 weeks after start of chemo Significance diminishes with longer timepoints
142 Treatment Volume: Pre-chemo vs. Post-chemo NCCTG/Mayo retrospective study Most failures in the treatment field, so supported post-chemo volumes SWOG randomized trial No change in recurrence rate Not relevant if giving early RT!
143 Treatment Volume: ENI vs. IFRT JJCO 2012 No PET PET IFRT appears ok in PET-staged patients ENI was utilized in Turrisi trial IFRT being investigated prospectively in Europe and RTOG Penn approach Use ENI when feasible
144 Fractionation Turrisi et al. NEJM 1999 (Intergroup 0096): Twice-daily compared with once-daily thoracic radiotherapy in limited smallcell lung cancer treated concurrently with cisplatin and etoposide. Randomly assigned 417 patients with L-SCLC 45 Gy TRT QD/5 weeks 45 Gy BID/3 weeks Concurrent chemo: cisplatin + etoposide (4 cycles of cisplatin 60 mg/m2 and etoposide 120 mg/m2 (EP) Q3W) TRT begun at cycle 1 of 4 planned TRT: Target volume was gross tumor and bilateral mediastinal and ipsilateral hilar nodes Margin 1-1.5cm Supraclavicular fossa not treated if not involved PCI offered at 12 weeks for CR Turrisi AT, et al. N. Engl. J. Med Jan 28;340(4):265-71
145 Turrisi Trial: Results BID TRT benefit: median survival significantly longer: 23 vs. 19 months 2yr survival: 47% vs. 41% 5yr survival: 26% vs. 16% Local failure QD 52% vs BID 36% (p=0.06) Toxicity: Grade 3 esophagitis QD 11% vs. 27%, no difference in Grade 4 esophagitis Summary: established 45 Gy given twice daily over 3 weeks as standard regimen
146 Dose Escalation Phase II Study CALGB Demonstrated safety of 70 Gy in 2 Gy fractions with concurrent chemotherapy Bogart et al. IJROBP 2004
147 CALGB Phase III ARM Regimen Study BED 2-year OS A 45 Gy (1.5Gy BID/3 weeks) INT % B 70 Gy (2Gy QD/7 weeks) CALGB 84 48% C 61.2 (1.8 Gy Concomitant Boost for final 9 days/5 weeks) RTOG % Concurrent Chemotherapy: Cisplatin/Etoposide Currently Accruing
148 Prophylactic Cranial Irradiation 987 patients in CR from 7 randomized trials between RR of death 0.84 in PCI group compared to control (observation only) 5.4% increase in 3 year survival: 15.3 vs. 20% 25.3% decrease in 3 yr incidence of brain metastases with PCI Unable to assess impact of PCI on cognitive function
149 Dose for PCI Lancet Oncol 2009 PCI 99-01,EORTC , RTOG 0212 and IFCT randomized trial Eligible patients: LS-SCLC CR after thoracic RT and chemotherapy Low Dose (25 Gy/10fxn (std)) vs High Dose (36 Gy/18 fxn or 36 Gy/24 fxn (1.5 Gy bid)) With Median FU=39 mo, no difference in 2 year incidence of brain mets (29%LD vs 23%HD, p=0.18) 2 year OS (42%LD vs 37%HD, p=0.05) Conclusion: PCI at 25 Gy remain the standard of care Péchoux CL et al Lancet Oncology 2009
150 Consequence of higher PCI dose Ann Onc 2011 IJROP 2011 Combined analysis was performed across all 4 trials No significant difference across all QOL and Cognitive parameters over 3 years between LD and HD arm Some critical individual domains (intellectual deficit, etc) were poorer in HD arm Secondary endpoint analysis of phase II randomized trial (RTOG 0212) Neurophychologic tests and QOL assessments prior to PCI, then at 6 mo, 12 mo and annually for 3 years. ND and CNT at 12 mo sig higher in high dose arms 2&3 (p=0.02) My approach: 25 Gy in 10 fractions
151 Extensive stage small cell lung cancer JCO 1999 Role for thoracic radiotherapy in extensive stage Primary site of failure is intrathoracic Improved median survival: 17 vs. 11 months 5 year OS 9.1 vs. 3.7%, P = RTOG 0937: Ongoing Randomized Phase II Trial Comparing PCI Alone to PCI + Consolidative Thoracic RT (QD IFRT: 300cGy x15) for E-SCLC My approach: Excellent PS patients with extrathoracic CR, will consider
152 Extensive stage small cell lung cancer: PCI NEJM 2007 Brain a significant site of failure in extensive stage disease EORTC randomized trial demonstrated a survival benefit to ES-responders Criticism- no brain imaging required. Patients screened clinically for brain mets (HA, N/V, Visual, Cognitive, Seizure, FNS) My approach: Use PCI in ES disease on case-by-case basis
153 Small Cell Lung Cancer: Practical Considerations Treatment approach for LS-SCLC ENI to 45Gy in 1.5BID fractions Alternate options 1.8-2Gy QD to 70Gy (RTOG 9712) IFRT if ENI is not feasible (JJCO 2012) Simulation IGRT Use PET/CT for staging and to inform treatment planning if IFRT is used No clear data, but given the rapid volume change- would use CBCT if available Treatment delivery technique PCI 3D-CRT, all-fields daily (Rengan in submission, presented Chicago lung) 2.5Gy x 10 to 25Gy is standard
154 Summary L-SCLC: Chemo plus XRT (Turissi and Pignon meta-analysis) Early XRT (Murray and Fried Meta-analysis) Performance status should be always be considered 45 Gy twice daily in 1.5 Gy fractions or ~70 Gy daily in 1.8-2Gy fractions (Turrisi or CALGB 39808) E-SCLC Ongoing CALGB Platin doublet Thoracic radiotherapy in excellent PS with extrathoracic CR PCI reasonable option in L-SCLC or E-SCLC Auperin Meta-analysis and Slotman Trial
155 THANK YOU!
Management of stage III A-B of NSCLC. Hamed ALHusaini Medical Oncologist
 Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
Small Cell Lung Cancer
 Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
Small Cell Lung Cancer Types of Lung Cancer Non-small cell carcinoma (NSCC) (87%) Adenocarcinoma (38%) Squamous cell (20%) Large cell (5%) Small cell carcinoma (13%) Small cell lung cancer is virtually
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
SMALL CELL LUNG CANCER
 Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Protocol for Planning and Treatment The process to be followed in the management of: SMALL CELL LUNG CANCER Patient information given at each stage following agreed information pathway 1. DIAGNOSIS New
Lung Cancer Treatment Guidelines
 Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Updated June 2014 Derived and updated by consensus of members of the Providence Thoracic Oncology Program with the aid of evidence-based National Comprehensive Cancer Network (NCCN) national guidelines,
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Lung Cancer and Mesothelioma
 Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Lung Cancer and Mesothelioma Robert Kratzke, M.D. John C. Skoglund Professor of Lung Cancer Research Section of Heme/Onc/Transplant Department of Medicine University of Minnesota Medical School Malignant
Adjuvant Therapy Non Small Cell Lung Cancer. Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015
 Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Adjuvant Therapy Non Small Cell Lung Cancer Sunil Nagpal MD Director, Thoracic Oncology Jan 30, 2015 No Disclosures Number of studies Studies Per Month 12 10 8 6 4 2 0 1 2 3 4 5 6 7 8 9 10 11 12 1 2 3
Radiation Therapy in the Treatment of
 Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Lung Cancer Radiation Therapy in the Treatment of Lung Cancer JMAJ 46(12): 537 541, 2003 Kazushige HAYAKAWA Professor and Chairman, Department of Radiology, Kitasato University School of Medicine Abstract:
Update on Small Cell Lung Cancer
 Welcome to Master Class for Oncologists Session 3: 2:45 PM - 3:30 PM Washington, DC March 28, 2009 Small Cell Lung Cancer: Best Practices & Recent Advances Speaker: Bruce E. Johnson, MD Professor of Medicine,
Welcome to Master Class for Oncologists Session 3: 2:45 PM - 3:30 PM Washington, DC March 28, 2009 Small Cell Lung Cancer: Best Practices & Recent Advances Speaker: Bruce E. Johnson, MD Professor of Medicine,
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians
 Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
Treatment Algorithms for the Management of Lung Cancer in NSW Guide for Clinicians Background The Cancer Institute New South Wales Oncology Group Lung (NSWOG Lung) identified the need for the development
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
REPORT ASCO 1998 LOS ANGELES : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group Educational session Treatment of stage III non-small cell lung cancer (NSCLC) in
A Practical Guide to Advances in Staging and Treatment of NSCLC
 A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
A Practical Guide to Advances in Staging and Treatment of NSCLC Robert J. Korst, M.D. Director, Thoracic Surgery Medical Director, The Blumenthal Cancer Center The Valley Hospital Objectives Revised staging
B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC
 Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Lung Cancer B. Dingle MD, FRCPC, Brian Yaremko MD,FRCPC, R. Ash, MD, FRCPC, P. Truong, MD, FRCPC EPIDEMIOLOGY The estimated incidence of lung cancer in Canada for 2007 is 23,300 with 12,400 occurring in
Stage I, II Non Small Cell Lung Cancer
 Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Stage I, II Non Small Cell Lung Cancer Best Results T1 (less 3 cm) N0 80% 5 year survival No Role Adjuvant Chemotherapy Radiation Therapy Reduces Local Recurrence No Improvement in Survival 1 Staging Mediastinal
Mesothelioma. Malignant Pleural Mesothelioma
 Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Mesothelioma William G. Richards, PhD Brigham and Women s Hospital Malignant Pleural Mesothelioma 2,000-3,000 cases per year (USA) Increasing incidence Asbestos (50-80%, decreasing) 30-40 year latency
Maintenance therapy in in Metastatic NSCLC. Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai
 Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board
 Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board Abstract Introduction Management of stage III non small-cell lung cancer (NSCLC) is complex and requires careful work-up, staging,
Management of Stage III, N2 NSCLC: A Virtual Thoracic Oncology Tumor Board Abstract Introduction Management of stage III non small-cell lung cancer (NSCLC) is complex and requires careful work-up, staging,
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines
 Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
Non-Small Cell Lung Cancer Treatment Comparison to NCCN Guidelines April 2008 (presented at 6/12/08 cancer committee meeting) By Shelly Smits, RHIT, CCS, CTR Conclusions by Dr. Ian Thompson, MD Dr. James
PET/CT in Lung Cancer
 PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
PET/CT in Lung Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria GLOBOCAN 2012 #1 #3 FDG-PET/CT
Epidemiology, Staging and Treatment of Lung Cancer. Mark A. Socinski, MD
 Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Epidemiology, Staging and Treatment of Lung Cancer Mark A. Socinski, MD Associate Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive Cancer Center University of
Radiotherapy for Non-Small Cell Lung Cancer. Standard Treatment Options Radiotherapy Planning
 Radiotherapy for Non-Small Cell Lung Cancer I II Standard Treatment Options Radiotherapy Planning TNM Staging System Disease Staging - Management is based on disease stage - Stage I-II: early stage - Stage
Radiotherapy for Non-Small Cell Lung Cancer I II Standard Treatment Options Radiotherapy Planning TNM Staging System Disease Staging - Management is based on disease stage - Stage I-II: early stage - Stage
Stage IIIB disease includes patients with T4 tumors,
 Guidelines on Treatment of Stage IIIB Non-small Cell Lung Cancer* James R. Jett, MD, FCCP; Walter J. Scott, MD, FCCP; M. Patricia Rivera MD, FCCP; and William T. Sause, MD, FACR Stage IIIB includes patients
Guidelines on Treatment of Stage IIIB Non-small Cell Lung Cancer* James R. Jett, MD, FCCP; Walter J. Scott, MD, FCCP; M. Patricia Rivera MD, FCCP; and William T. Sause, MD, FACR Stage IIIB includes patients
The Need for Accurate Lung Cancer Staging
 The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
The Need for Accurate Lung Cancer Staging Peter Baik, DO Thoracic Surgery Cancer Treatment Centers of America Oklahoma Osteopathic Association 115th Annual Convention Financial Disclosures: None 2 Objectives
Jedi Wisdom for Lung Cancer Radiotherapy: May the Force Be With You
 Jedi Wisdom for Lung Cancer Radiotherapy: May the Force Be With You SHAUN LOEWEN MD PhD FRCPC Assistant Professor, University of Manitoba Radiation Oncologist, CancerCare Manitoba Disclosure Relationship
Jedi Wisdom for Lung Cancer Radiotherapy: May the Force Be With You SHAUN LOEWEN MD PhD FRCPC Assistant Professor, University of Manitoba Radiation Oncologist, CancerCare Manitoba Disclosure Relationship
Pulmonary function. Is patient potentially operable? Yes. tests 3. Yes. Pulmonary function. tests 3, if clinically indicated. Yes
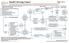 INITIAL EVALUATION Pathology consistent with small cell lung cancer History and physical Chest X-ray Laboratory studies to include: hematological and full chemistry panels CT chest and upper abdomen Pet
INITIAL EVALUATION Pathology consistent with small cell lung cancer History and physical Chest X-ray Laboratory studies to include: hematological and full chemistry panels CT chest and upper abdomen Pet
Moving forward, where are we with Clinical Trials?
 Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
Moving forward, where are we with Clinical Trials? Dennis A. Wigle Division of Thoracic Surgery Mayo Clinic AATS/STS General Thoracic Surgery Symposium Sunday, April 27 th 2014 2012 MFMER slide-1 Where
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015. 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV
 CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
CANCER PULMON: ESTADIOS INICIALES POSTMUNDIAL PULMON DENVER 2015 8-10-2015.Manuel Cobo Dols S. Oncología Médica HU Málaga Regional y VV Meta-analisis LACE: adyuvancia vs no adyuvancia Pignon JP, et al.
SAKK Lung Cancer Group. Current activities and future projects
 SAKK Lung Cancer Group Current activities and future projects SAKK Lung Cancer Group Open group of physicians interested in lung cancer Mostly Medical Oncologists, but also Thoracic Surgeons Radiation
SAKK Lung Cancer Group Current activities and future projects SAKK Lung Cancer Group Open group of physicians interested in lung cancer Mostly Medical Oncologists, but also Thoracic Surgeons Radiation
Small Cell Lung Cancer
 Small Cell Lung Cancer Lung Practice Guideline Dr. Brian Dingle MSc, MD, FRCPC Approval Date: April 2007 Revised: November 2008 This guideline is a statement of consensus of the Thoracic Disease Site Team
Small Cell Lung Cancer Lung Practice Guideline Dr. Brian Dingle MSc, MD, FRCPC Approval Date: April 2007 Revised: November 2008 This guideline is a statement of consensus of the Thoracic Disease Site Team
Non-small Cell Lung Cancer: Locally Advanced
 Non-small Cell Lung Cancer: Locally Advanced Daniel W. Golden MD, PGY-5, Ryan Bair MD, PGY-3, and Matthew Koshy MD, Assistant Professor Pritzker School of Medicine, University of Chicago Chicago Clinical
Non-small Cell Lung Cancer: Locally Advanced Daniel W. Golden MD, PGY-5, Ryan Bair MD, PGY-3, and Matthew Koshy MD, Assistant Professor Pritzker School of Medicine, University of Chicago Chicago Clinical
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VIII. THERAPY. V. SMALL CELL LUNG CANCER Prof. Alberto Riccardi SMALL CELL LUNG CARCINOMA Summary of treatment approach * limited
Malignant Mesothelioma State of the Art
 Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Malignant Mesothelioma State of the Art Paul Baas The Netherlands Cancer Institute August 12, 2011, Carlsbad, CA Summary Diagnosis; epithelial type subdivided Pleiomorphic vs other Staging: IASLC-IMIG
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. IV. THERAPY. I. NON SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. IV. THERAPY. I. NON SMALL CELL LUNG CANCER Prof. Alberto Riccardi TREATMENT OF LUNG CARCINOMA * overall treatment approach to
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. IV. THERAPY. I. NON SMALL CELL LUNG CANCER Prof. Alberto Riccardi TREATMENT OF LUNG CARCINOMA * overall treatment approach to
Particle Therapy for Lung Cancer. Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org
 Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Particle Therapy for Lung Cancer Bradford Hoppe MD, MPH Assistant Professor University of Florida bhoppe@floridaproton.org Content Rationale for Particle Therapy in Lung Cancer Proof of Principle Treatment
Radiotherapy in locally advanced & metastatic NSC lung cancer
 Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
Radiotherapy in locally advanced & metastatic NSC lung cancer Dr Raj Hegde. MD. FRANZCR Consultant Radiation Oncologist. William Buckland Radiotherapy Centre. Latrobe Regional Hospital. Locally advanced
National Clinical Trials Network Groups Update Fall 2014
 National Clinical Trials Network Groups Update Fall 2014 Walter J Curran, Jr, MD An NRG Oncology Group Chair Executive Director Winship Cancer Institute of Emory University Atlanta, GA NCTN Groups Update
National Clinical Trials Network Groups Update Fall 2014 Walter J Curran, Jr, MD An NRG Oncology Group Chair Executive Director Winship Cancer Institute of Emory University Atlanta, GA NCTN Groups Update
Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases
 I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
I Congresso de Oncologia D Or July 5-6, 2013 Integrating Chemotherapy and Liver Surgery for the Management of Colorectal Metastases Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University
Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer. A Single Institution Experience
 ORIGINAL ARTICLE Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer A Single Institution Experience Michael Hsie, MD,* Stefania Morbidini-Gaffney, MD,* Leslie J. Kohman, MD, Elisabeth
ORIGINAL ARTICLE Definitive Treatment of Poor-Risk Patients with Stage I Lung Cancer A Single Institution Experience Michael Hsie, MD,* Stefania Morbidini-Gaffney, MD,* Leslie J. Kohman, MD, Elisabeth
Management of low grade glioma s: update on recent trials
 Management of low grade glioma s: update on recent trials M.J. van den Bent The Brain Tumor Center at Erasmus MC Cancer Center Rotterdam, the Netherlands Low grades Female, born 1976 1 st seizure 2005,
Management of low grade glioma s: update on recent trials M.J. van den Bent The Brain Tumor Center at Erasmus MC Cancer Center Rotterdam, the Netherlands Low grades Female, born 1976 1 st seizure 2005,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma
 Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Accelerated hemithoracic radiation followed by extrapleural pneumonectomy for malignant pleural mesothelioma Marc de Perrot, Ronald Feld, Natasha B Leighl, Andrew Hope, Thomas K Waddell, Shaf Keshavjee,
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro. Joon H. Lee 9/17/2012
 Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Extrapleural Pneumonectomy for Malignant Mesothelioma: Pro Joon H. Lee 9/17/2012 Malignant Pleural Mesothelioma (Epidemiology) Incidence: 7/mil (Japan) to 40/mil (Australia) Attributed secondary to asbestos
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Alternatives to Surgical Resection for Early Stage Lung Cancer
 Alternatives to Surgical Resection for Early Stage Lung Cancer Neil A. Christie MD University of Pittsburgh Medical Center Department of Thoracic Surgery Allied Health Personnel Symposium AATS 2014 Conflicts
Alternatives to Surgical Resection for Early Stage Lung Cancer Neil A. Christie MD University of Pittsburgh Medical Center Department of Thoracic Surgery Allied Health Personnel Symposium AATS 2014 Conflicts
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER
 AFA 08958 From Bench to Bedside From KK DT1 10/27/2015 12:04 PM 01 ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER Hak Choy, MD University of Texas Southwestern Medical Center Dallas, Texas, USA Orchestrating
AFA 08958 From Bench to Bedside From KK DT1 10/27/2015 12:04 PM 01 ROLE OF RADIATION THERAPY FOR RESECTABLE LUNG CANCER Hak Choy, MD University of Texas Southwestern Medical Center Dallas, Texas, USA Orchestrating
Radiotherapy in Lung
 Radiotherapy in Lung CancerAnatomy Oblique fissure in both lungs. Horizontal fissure in Right lung. Trachea bifurcates at the level of T5. Lymph nodes are divided into stations. Intrapulmonary, bronchopulmonary
Radiotherapy in Lung CancerAnatomy Oblique fissure in both lungs. Horizontal fissure in Right lung. Trachea bifurcates at the level of T5. Lymph nodes are divided into stations. Intrapulmonary, bronchopulmonary
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs. Case Study. Surgery. Lumpectomy and Radiation
 Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
Management of Postmenopausal Women with T1 ER+ Tumors: Options and Tradeoffs Michael Alvarado, MD Associate Professor of Surgery University of California San Francisco Case Study 59 yo woman with new palpable
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer
 Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
Protein kinase C alpha expression and resistance to neo-adjuvant gemcitabine-containing chemotherapy in non-small cell lung cancer Dan Vogl Lay Abstract Early stage non-small cell lung cancer can be cured
L Lang-Lazdunski, A Bille, S Marshall, R Lal, D Landau, J Spicer
 Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Pleurectomy/decortication, hyperthermic pleural lavage with povidone-iodine and systemic chemotherapy in malignant pleural mesothelioma. A 10-year experience. L Lang-Lazdunski, A Bille, S Marshall, R Lal,
Outcomes of Patients With Stage III Nonsmall Cell Lung Cancer Treated With Chemotherapy and Radiation With and Without Surgery
 Outcomes of Patients With Stage III Nonsmall Cell Lung Cancer Treated With Chemotherapy and Radiation With and Without Surgery Hale B. Caglar, MD 1 ; Elizabeth H. Baldini, MD, MPH 1 ; Megan Othus, MS 2
Outcomes of Patients With Stage III Nonsmall Cell Lung Cancer Treated With Chemotherapy and Radiation With and Without Surgery Hale B. Caglar, MD 1 ; Elizabeth H. Baldini, MD, MPH 1 ; Megan Othus, MS 2
Controversies in Management of. Inoperable NSCLC. Inoperable NSCLC. Introduction:
 Inoperable NSCLC Controversies in Management of Inoperable NSCLC Introduction: It is difficult to overemphasize the magnitude of lung cancer as Public Health Problem in our society. - In US, Lung cancer
Inoperable NSCLC Controversies in Management of Inoperable NSCLC Introduction: It is difficult to overemphasize the magnitude of lung cancer as Public Health Problem in our society. - In US, Lung cancer
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline
 Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline An ASCO Endorsement of Treatment of Small Cell Lung Cancer:
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline An ASCO Endorsement of Treatment of Small Cell Lung Cancer:
Treatment Paradigm in NSCLC Treatment
 Treatment Paradigm in NSCLC Treatment Era of Targeted Therapy Aumkhae Sookprasert, MD Medicine Department, KKU Which factors taken to be account in NSCLC treatment? 1. Staging 2. ECOG performance status
Treatment Paradigm in NSCLC Treatment Era of Targeted Therapy Aumkhae Sookprasert, MD Medicine Department, KKU Which factors taken to be account in NSCLC treatment? 1. Staging 2. ECOG performance status
Diagnosis and multimodality management of stage III non-small cell lung cancer Review Article
 Cancer Therapy Vol 6, page 81 Cancer Therapy Vol 6, 81-94, 2008 Diagnosis and multimodality management of stage III non-small cell lung cancer Review Article Kevin Sullivan, Zujun Li, John Rescigno, Michael
Cancer Therapy Vol 6, page 81 Cancer Therapy Vol 6, 81-94, 2008 Diagnosis and multimodality management of stage III non-small cell lung cancer Review Article Kevin Sullivan, Zujun Li, John Rescigno, Michael
the standard of care 2009 5/1/2009 Mesothelioma: The standard of care take home messages PILC 2006 Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009
 Mesothelioma: The standard of care Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
Mesothelioma: The standard of care Jan.vanmeerbeeck@ugent.be Brussels, March 7, 2009 take home messages PILC 2006 All patients should receive adequate palliation of dyspnea and pain before starting chemotherapy
New Trends & Current Research in the Treatment of Lung Cancer, Pt. II
 New Trends & Current esearch in the Treatment of Lung Cancer, Pt. II Howard (Jack) West, MD President & CEO, GACE Medical Director, Thoracic Oncology Program Swedish Cancer Institute Seattle, WA Cancer
New Trends & Current esearch in the Treatment of Lung Cancer, Pt. II Howard (Jack) West, MD President & CEO, GACE Medical Director, Thoracic Oncology Program Swedish Cancer Institute Seattle, WA Cancer
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Non-Small Cell Lung Cancer John delcharco, MD (Statistics based on CVMC data 2009-2013) Statistics Lung cancer is the leading cause of cancer deaths in the United States. The American Cancer Society estimates
Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART
 Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART Goals Discuss treatment options for stage 4 lung cancer: New and old Discuss new developments in personalized
Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART Goals Discuss treatment options for stage 4 lung cancer: New and old Discuss new developments in personalized
How To Treat A Cancer With A Radical
 Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Management of mesothelioma Jan.vanmeerbeeck@ugent.be Amsterdam, March 6, 2010 1 management Palliation Symptomatic care Pain Breathlessness Radiotherapy Chemotherapy Surgery Radical (intention to cure)
Principles of Radiation Therapy A Bapsi Chakravarthy, MD Associate e P rofessor Professor Radiation Oncology
 Principles of Radiation Therapy A Bapsi Chakravarthy, MD Associate Professor Radiation Oncology Disclosure Information I have no financial relationships to disclose relevant to the conten of this presentation.
Principles of Radiation Therapy A Bapsi Chakravarthy, MD Associate Professor Radiation Oncology Disclosure Information I have no financial relationships to disclose relevant to the conten of this presentation.
Multidisciplinary Therapy of Stage IIIA Non Small-Cell Lung Cancer: Long-term Outcome of Chemoradiation With or Without Surgery
 Special Report Multidisciplinary Therapy of Stage IIIA Non Small-Cell Lung Cancer: Long-term Outcome of Chemoradiation With or Without Surgery Charu Aggarwal, MD, Linna Li, MD, Hossein Borghaei, DO, Ranee
Special Report Multidisciplinary Therapy of Stage IIIA Non Small-Cell Lung Cancer: Long-term Outcome of Chemoradiation With or Without Surgery Charu Aggarwal, MD, Linna Li, MD, Hossein Borghaei, DO, Ranee
INTRODUCTION. liver neoplasms, adrenal gland neoplasms, non small-cell lung cancer, radionuclide imaging, bisphosphonates,
 VOLUME 22 NUMBER 2 JANUARY 15 2004 JOURNAL OF CLINICAL ONCOLOGY A S C O S P E C I A L A R T I C L E American Society of Clinical Oncology Treatment of Unresectable Non Small-Cell Lung Cancer Guideline:
VOLUME 22 NUMBER 2 JANUARY 15 2004 JOURNAL OF CLINICAL ONCOLOGY A S C O S P E C I A L A R T I C L E American Society of Clinical Oncology Treatment of Unresectable Non Small-Cell Lung Cancer Guideline:
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka
 Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Adiuwantowe i neoadiuwantowe leczenie chorych na zaawansowanego raka żołądka Neoadiuvant and adiuvant therapy for advanced gastric cancer Franco Roviello, IT Neoadjuvant and adjuvant therapy for advanced
Malignant Mesothelioma: an Update
 Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Malignant Mesothelioma: an Update Nico van Zandwijk Asbestos Diseases Research Institute Bernie Banton Centre University of Sydney Australia Physicians Week RACP 19-5-2009 Health Risks of Asbestos Fibers
Malignant Mesothelioma Current Approaches to a Difficult Problem. Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center
 Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Malignant Mesothelioma Current Approaches to a Difficult Problem Raja M Flores, MD Thoracic Surgery Memorial Sloan-Kettering Cancer Center Malignant Pleural Mesothelioma Clinical Presentation Insidious
Cesare Gridelli 1, Francesca Casaluce 2, Assunta Sgambato 2, Fabio Monaco 3, Cesare Guida 4
 Editorial Treatment of limited-stage small cell lung cancer in the elderly, chemotherapy vs. sequential chemoradiotherapy vs. concurrent chemoradiotherapy: that s the question Cesare Gridelli 1, Francesca
Editorial Treatment of limited-stage small cell lung cancer in the elderly, chemotherapy vs. sequential chemoradiotherapy vs. concurrent chemoradiotherapy: that s the question Cesare Gridelli 1, Francesca
3.0 With final Comments for presentation at Sub Group Meeting 24. 24.11.10
 Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
Guideline for the Treatment of Lung Cancer Version History 2.0 Endorsed by the Governance Committee as treatment of lung cancer 27.07.09 with radiotherapy and chemotherapy. 2.1 Re-written to include the
U.S. Food and Drug Administration
 U.S. Food and Drug Administration Notice: Archived Document The content in this document is provided on the FDA s website for reference purposes only. It was current when produced, but is no longer maintained
U.S. Food and Drug Administration Notice: Archived Document The content in this document is provided on the FDA s website for reference purposes only. It was current when produced, but is no longer maintained
The expanding role of systemic treatment in non-small cell lung cancer neo-adjuvant therapy
 17 (Supplement 10): x108 x112, 2006 doi:10.1093/annonc/mdl247 The expanding role of systemic treatment in non-small cell lung cancer neo-adjuvant therapy E. Felip & E. Vilar Oncology Department, Vall d
17 (Supplement 10): x108 x112, 2006 doi:10.1093/annonc/mdl247 The expanding role of systemic treatment in non-small cell lung cancer neo-adjuvant therapy E. Felip & E. Vilar Oncology Department, Vall d
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Mesothelioma. 1. Introduction. 1.1 General Information and Aetiology
 Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Mesothelioma 1. Introduction 1.1 General Information and Aetiology Mesotheliomas are tumours that arise from the mesothelial cells of the pleura, peritoneum, pericardium or tunica vaginalis [1]. Most are
Neoplasms of the LUNG and PLEURA
 Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Neoplasms of the LUNG and PLEURA 2015-2016 FCDS Educational Webcast Series Steven Peace, BS, CTR September 19, 2015 2015 Focus o Anatomy o SSS 2000 o MPH Rules o AJCC TNM 1 Case 1 Case Vignette HISTORY:
Case Number: RT2009-114(M) Potential Audiences: Intent Doctor, Oncology Special Nurse, Resident Doctor
 Extensive-Stage Small Cell Lung Cancer Post Full-Course Chemotherapy with Residual Locoregional Cancer Disease: the Role and Treatment Consideration of Radiotherapy Case Number: RT2009-114(M) Potential
Extensive-Stage Small Cell Lung Cancer Post Full-Course Chemotherapy with Residual Locoregional Cancer Disease: the Role and Treatment Consideration of Radiotherapy Case Number: RT2009-114(M) Potential
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE LUNG CANCER Lung Site Group Lung Cancer Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES LUNG SITE LUNG CANCER Lung Site Group Lung Cancer Authors: Dr. Meredith Giuliani, Dr. Andrea Bezjak 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
 Efficacy Results from the ToGA Trial: A Phase III Study of Trastuzumab Added to Standard Chemotherapy in First-Line HER2- Positive Advanced Gastric Cancer Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
Efficacy Results from the ToGA Trial: A Phase III Study of Trastuzumab Added to Standard Chemotherapy in First-Line HER2- Positive Advanced Gastric Cancer Van Cutsem E et al. Proc ASCO 2009;Abstract LBA4509.
Stomach (Gastric) Cancer. Prof. M K Mahajan ACDT & RC Bathinda
 Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
Stomach (Gastric) Cancer Prof. M K Mahajan ACDT & RC Bathinda Gastric Cancer Role of Radiation Layers of the Stomach Mucosa Submucosa Muscularis Serosa Stomach and Regional Lymph Nodes Stomach and Regional
Lung Cancer. Public Outcomes Report. Submitted by Omar A. Majid, MD
 Public Outcomes Report Lung Cancer Submitted by Omar A. Majid, MD Lung cancer is the most common cancer-related cause of death among men and women. It has been estimated that there will be 226,1 new cases
Public Outcomes Report Lung Cancer Submitted by Omar A. Majid, MD Lung cancer is the most common cancer-related cause of death among men and women. It has been estimated that there will be 226,1 new cases
Survival analysis of 220 patients with completely resected stage II non small cell lung cancer
 窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
窑 Original Article 窑 Chinese Journal of Cancer Survival analysis of 22 patients with completely resected stage II non small cell lung cancer Yun Dai,2,3, Xiao Dong Su,2,3, Hao Long,2,3, Peng Lin,2,3, Jian
5. Non small Cell Lung Cancer
 5. Non small Cell Lung Cancer Introduction The cancer registry in Sweden shows a continuous increase of lung cancer cases from 867 in 1958 when the registry started to 2 846 in 2000. The Swedish cancer
5. Non small Cell Lung Cancer Introduction The cancer registry in Sweden shows a continuous increase of lung cancer cases from 867 in 1958 when the registry started to 2 846 in 2000. The Swedish cancer
Carcinoma of the Cervix. Kathleen M. Schmeler, MD Associate Professor Department of Gynecologic Oncology
 Carcinoma of the Cervix Kathleen M. Schmeler, MD Associate Professor Department of Gynecologic Oncology Cervical Cancer Treatment Treatment Microinvasive (Stage IA1): Simple (extrafascial) hysterectomy/cone
Carcinoma of the Cervix Kathleen M. Schmeler, MD Associate Professor Department of Gynecologic Oncology Cervical Cancer Treatment Treatment Microinvasive (Stage IA1): Simple (extrafascial) hysterectomy/cone
Clinical Indications and Results Following Chest Wall Resection
 Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Clinical Indications and Results Following Chest Wall Resection for Recurrent Malignant Pleural Mesothelioma Ali SO, Burt BM, Groth SS, DaSilva MC, Yeap BY, Richards WG, Baldini EH and Sugarbaker DJ. Division
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology. Endorsement of the American College of Chest Physicians (ACCP) Guideline
 Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline Table of Contents Data Supplement 1: Summary of included
Treatment of Small Cell Lung Cancer: American Society of Clinical Oncology Endorsement of the American College of Chest Physicians (ACCP) Guideline Table of Contents Data Supplement 1: Summary of included
Efficacy of chemotherapy combined hyperfractionated accelerated radiotherapy on limited small cell lung cancer
 [Chinese Journal of Cancer 27:10, 353-357; October 2008]; 2008 Sun Yat-Sen University Cancer Center Clinical Research Paper Efficacy of chemotherapy combined hyperfractionated accelerated radiotherapy
[Chinese Journal of Cancer 27:10, 353-357; October 2008]; 2008 Sun Yat-Sen University Cancer Center Clinical Research Paper Efficacy of chemotherapy combined hyperfractionated accelerated radiotherapy
Should we use Docetaxel in hormone- naïve prostate cancer? Karim Fizazi, MD, PhD Institut Gustave Roussy Villejuif, France
 Should we use Docetaxel in hormone- naïve prostate cancer? Karim Fizazi, MD, PhD Institut Gustave Roussy Villejuif, France Disclosure Participation to advisory boards/honorarium from: Amgen, Astellas,
Should we use Docetaxel in hormone- naïve prostate cancer? Karim Fizazi, MD, PhD Institut Gustave Roussy Villejuif, France Disclosure Participation to advisory boards/honorarium from: Amgen, Astellas,
Treatment of Stage III Non-small Cell Lung Cancer
 CHEST Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER, 3RD ED: ACCP GUIDELINES Treatment of Stage III Non-small Cell Lung Cancer Diagnosis and Management of Lung Cancer, 3rd ed: American College of
CHEST Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER, 3RD ED: ACCP GUIDELINES Treatment of Stage III Non-small Cell Lung Cancer Diagnosis and Management of Lung Cancer, 3rd ed: American College of
Is an evidence-based approach realistic in non-small cell lung cancer (NSCLC)?
 Is an evidence-based approach realistic in non-small cell lung cancer (NSCLC)? Authors Key words P.A. Coucke, N. Barthelemy, L. Bosquee, J.P. van Meerbeeck NSCLC, sequential and concomitant chemo-radiotherapy,
Is an evidence-based approach realistic in non-small cell lung cancer (NSCLC)? Authors Key words P.A. Coucke, N. Barthelemy, L. Bosquee, J.P. van Meerbeeck NSCLC, sequential and concomitant chemo-radiotherapy,
LUNG CANCER INTRODUCTION
 LUNG CANCER INTRODUCTION Lung cancer remains the leading cause of cancer death in the UK. Approximately 50% of those diagnosed present with stage IV disease. Significant advances in the management of lung
LUNG CANCER INTRODUCTION Lung cancer remains the leading cause of cancer death in the UK. Approximately 50% of those diagnosed present with stage IV disease. Significant advances in the management of lung
Post-recurrence survival in completely resected stage I non-small cell lung cancer with local recurrence
 Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
Post- survival in completely resected stage I non-small cell lung cancer with local J-J Hung, 1,2,3 W-H Hsu, 3 C-C Hsieh, 3 B-S Huang, 3 M-H Huang, 3 J-S Liu, 2 Y-C Wu 3 See Editorial, p 185 c A supplementary
CHAPTER 6: TREATMENT FOR SMALL CELL LUNG CANCER
 CHAPTER 6: TREATMENT FOR SMALL CELL LUNG CANCER INTRODUCTION This chapter provides an overview of treatment for small cell lung cancer (SCLC). Treatment options are presented based on the extent of disease.
CHAPTER 6: TREATMENT FOR SMALL CELL LUNG CANCER INTRODUCTION This chapter provides an overview of treatment for small cell lung cancer (SCLC). Treatment options are presented based on the extent of disease.
ORIGINAL ARTICLE THORACIC ONCOLOGY
 Ann Surg Oncol (2013) 20:1934 1940 DOI 10.1245/s10434-012-2800-x ORIGINAL ARTICLE THORACIC ONCOLOGY Predictors for Locoregional Recurrence for Clinical Stage III-N2 Non-small Cell Lung Cancer with Nodal
Ann Surg Oncol (2013) 20:1934 1940 DOI 10.1245/s10434-012-2800-x ORIGINAL ARTICLE THORACIC ONCOLOGY Predictors for Locoregional Recurrence for Clinical Stage III-N2 Non-small Cell Lung Cancer with Nodal
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Radiotherapy in Lung Cancer. Dr. Vassilis Kouloulias. Radiotherapy in lung cancer. Dr. V. Kouloulias
 Radiotherapy in Lung Cancer Dr. Vassilis Kouloulias Assistant Professor of Radiation Oncologist, 2 nd Dpt. Radiology, University of Athens, Greece. Key Words Small cell lung cancer (SCLC), Non-small cell
Radiotherapy in Lung Cancer Dr. Vassilis Kouloulias Assistant Professor of Radiation Oncologist, 2 nd Dpt. Radiology, University of Athens, Greece. Key Words Small cell lung cancer (SCLC), Non-small cell
2.2.5 Target Volumes in Small Cell Lung Cancer
 Target Volumes in Small Cell Lung Cancer 111 2.2.5 Target Volumes in Small Cell Lung Cancer Yolanda I. Garces and James A. Bonner CONTENTS 2.2.5.1 Introduction 111 2.2.5.2 Tumor Volume Definitions 111
Target Volumes in Small Cell Lung Cancer 111 2.2.5 Target Volumes in Small Cell Lung Cancer Yolanda I. Garces and James A. Bonner CONTENTS 2.2.5.1 Introduction 111 2.2.5.2 Tumor Volume Definitions 111
Lungenkrebs. Lungenkrebs Häufigkeit
 Lungenkrebs Prof. Dr. E.W. Russi Pneumologie 1.9.2008 Lungenkrebs Häufigkeit The Principles and Practice of Medicine William Osler New York D. Appleton and Company 1892 Section IV DISEASE OF THE RESPIRATORY
Lungenkrebs Prof. Dr. E.W. Russi Pneumologie 1.9.2008 Lungenkrebs Häufigkeit The Principles and Practice of Medicine William Osler New York D. Appleton and Company 1892 Section IV DISEASE OF THE RESPIRATORY
EVIDENCE TABLE. Study Objective. (Purpose of Study)
 . Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 997; (6):70-77.. Greene FL, Page DL, Fleming ID, et al, eds, for the American Joint Committee on Cancer. AJCC Cancer
. Mountain CF. Revisions in the International System for Staging Lung Cancer. Chest 997; (6):70-77.. Greene FL, Page DL, Fleming ID, et al, eds, for the American Joint Committee on Cancer. AJCC Cancer
Non small-cell lung cancer, mesothelioma, and thymoma
 CHAPTER 7 Non small-cell lung cancer, mesothelioma, and thymoma Robert J. McKenna, Jr., MD, Benjamin Movsas, MD, Dong M. Shin, MD, and Fadlo R. Khuri, MD NSC LUNG In the United States, lung cancer has
CHAPTER 7 Non small-cell lung cancer, mesothelioma, and thymoma Robert J. McKenna, Jr., MD, Benjamin Movsas, MD, Dong M. Shin, MD, and Fadlo R. Khuri, MD NSC LUNG In the United States, lung cancer has
Malignant Pleural Mesothelioma in Singapore
 RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
RESEARCH COMMUNICATION C SP Yip 1, HN Koong 2, CM Loo 3, KW Fong 1* Abstract Aim: To examine the clinical characteristics and outcomes of malignant pleural mesothelioma (MPM) in Singapore. Methods and
