Advanced EKG Interpretation
|
|
|
- Godfrey Stevenson
- 8 years ago
- Views:
Transcription
1 Advanced EKG Interpretation
2 JUNCTIONAL RHYTHMS AND NURSING INTERVENTIONS
3 Objectives Identify specific cardiac dysrhythmias Describe appropriate nursing interventions for specific dysrhythmias
4 Junctional Rhythms Junctional rhythms are named such because their impulse originates from the AV node (AV junction) instead of the SA node. The SA node may be impaired secondary to drug toxicity or underlying cardiac disease. When the AV node does not sense an impulse coming down from the SA node, it will become the pacemaker of the heart.
5 Characteristics of all Junctional Rhythms Inverted (negative) or absent P waves are seen before each QRS complex OR P wave can be hidden in the QRS complex OR P wave may follow the QRS complex PR interval of <0.12 seconds (remember normal is ) QRS complex within normal measurements
6 Most Common Variations Junctional (escape) rhythm: bpm Accelerated junctional rhythm: bpm Junctional tachycardia: >100 bpm Premature junctional complexes (PJCs)
7 Junctional Rhythm Junctional (escape) rhythms originate at or around the AV node and the Bundle of His. The impulse travels up the atria and down to the ventricles resulting in inverted P waves that can occur prior to, during or after the QRS. P waves can also be absent if the impulse does not travel up into the atria. Inverted P wave
8 5 Steps to Identify Junctional Rhythm 1. What is the rate? bpm 2. What is the rhythm? Regular 3. Is there a P wave before each QRS? Are P waves upright and uniform? Usually inverted or absent, may be before, during or after QRS complex 4. What is the length of the PR interval? Will be shortened, if occurs before QRS complex, otherwise not measurable 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Less than 0.12 seconds (3 small squares)
9 Causes and S/S of Junctional Rhythm Causes SA node disease Sick sinus syndrome Inferior wall MI Digitalis toxicity Vagal stimulation Signs and symptoms May be asymptomatic Chest pain Dyspnea Hypotension Altered level of consciousness Blurred vision
10 Risk and Medical Tx of Junctional Rhythm Risk Reduced cardiac output Medical Treatment None if asymptomatic Treat the underlying cause Atropine Temporary or permanent pacemaker
11 Accelerated Junctional Rhythm Accelerated junctional rhythms originate in the bundle of His and fire at a rate of bpm Note: no P waves
12 5 Steps to Identify Accelerated Junctional Rhythm 1. What is the rate? bpm 2. What is the rhythm? Regular 3. Is there a P wave before each QRS? Are P waves upright and uniform? Usually inverted or absent, may be before, during or after QRS complex 4. What is the length of the PR interval? Will be shortened, if occurs before QRS complex, otherwise not measurable 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Less than 0.12 seconds (3 small squares)
13 Causes and S/S of Accelerated Junctional Rhythm Causes SA node disease Digitalis toxicity Hypoxia Increased vagal tone Beta blockers and calcium channel blockers Hypokalemia Inferior or posterior wall MI Signs and symptoms May be asymptomatic Chest pain Dyspnea Hypotension Altered level of consciousness Weak peripheral pulses
14 Risk and Medical Tx of Accelerated Junctional Rhythm Risk Reduced cardiac output Medical Treatment None if asymptomatic Treat the underlying cause Atropine Temporary or permanent pacemaker
15 Junctional Tachycardia Junctional tachycardia is a junctional rhythm with a rate between bpm Note: inverted P waves
16 5 Steps to Identify Junctional Tachycardia 1. What is the rate? bpm 2. What is the rhythm? Regular 3. Is there a P wave before each QRS? Are P waves upright and uniform? Usually inverted or absent, may be before, during or after QRS complex 4. What is the length of the PR interval? Will be shortened, if occurs before QRS complex, otherwise not measurable 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Less than 0.12 seconds (3 small squares)
17 Causes and S/S of Junctional Tachycardia Causes Cardiac ischemia Hypoxia Increased vagal tone CHF Cardiogenic shock Signs and symptoms May be asymptomatic Chest pain Dyspnea Hypotension Altered level of consciousness
18 Risk and Medical Tx of Junctional Tachycardia Risk Reduced cardiac output Medical Treatment None if asymptomatic Treat the underlying cause Rate control Vagal maneuvers Verapamil Cardioversion
19 Premature Junctional Contraction (PJC) A Premature Junctional Contraction is an early beat that occurs prior to the next sinus beat. Similar to a PAC EXCEPT P wave is inverted on the PJC!!
20 5 Steps to Identify Premature Junctional Contraction (PJC) 1. What is the rate? Depends on underlying rhythm 2. What is the rhythm? Irregular noted during the PJC 3. Is there a P wave before each QRS? Are P waves upright and uniform? Usually inverted or absent, may be before, during or after QRS complex 4. What is the length of the PR interval? Will be shortened, if occurs before QRS complex, otherwise not measurable 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Less than 0.12 seconds (3 small squares)
21 Causes and S/S of Premature Junctional Contractions Causes May occur in healthy hearts Digitalis toxicity Cardiac ischemia MI Increased vagal tone CHF Cardiogenic shock Excessive caffeine Signs and symptoms Usually asymptomatic Based on underlying rhythm
22 Risk and Medical Tx of Premature Junctional Contraction Risk If PJCs occur frequently, junctional tachycardia may result Medical Treatment No treatment required unless the PJCs become more frequent
23 HEART BLOCK RHYTHMS AND NURSING INTERVENTIONS
24 Objectives Identify specific cardiac dysrhythmias Describe appropriate nursing interventions for secific dysrhythmias
25 The Heart Block Rhythms Heart blocks are arrhythmias caused by an interruption in the conduction of impulses between the atria and the ventricles. The AV block can be total or partial or it may simply delay conduction.
26 The Heart Block Rhythms First Degree AV Block Second Degree AV Block Type I (Wenckebach) Type II Third Degree AV Block
27 First Degree AV Block First Degree AV Block Is the most common form of heart block Looks similar to sinus rhythm Impulse conduction between the atria and the Bundle of His is delayed at the level of the AV node The PR interval will be prolonged (> 0.20)
28 5 Steps to Identify First Degree AV Block 1. What is the rate? Based on rate of underlying rhythm 2. What is the rhythm? Usually regular 3. Is there a P wave before each QRS? Are P waves upright and uniform? Yes Yes 4. What is the length of the PR interval? >0.20 seconds 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Less than 0.12 seconds (3 small squares)
29 Causes and S/S of First Degree AV Block Causes Can occur in healthy hearts May be temporary Signs and Symptoms Most patients are asymptomatic Dizziness/syncope Myocardial infarction or ischemia Medications digitalis, calcium channel blockers, beta blockers Myocarditis Degenerative changes in the heart
30 Risk and Medical Tx of First Degree AV Block Risk Reduced cardiac output, although this is rare Treatment No treatment is usually necessary if the patient is asymptomatic Treat the underlying cause Monitor closely to detect progression to a more serious form of block
31 2 nd Degree AV Block Mobitz Type I (Wenckeback) The delay of the electrical impulse at the AV node produces a progressive increase in the length of the PR interval (> 0.20 seconds) The PR interval continues to increase in length until the impulse is not conducted or the QRS complex is dropped Lengthening PR intervals Dropped QRS!
32 5 Steps to Identify 2 nd Degree AV Block Mobitz Type I (Wenckebach) 1. What is the rate? Atrial: unaffected Ventricular: usually slower than atrial 2. What is the rhythm? Atrial: regular Ventricular: irregular 3. Is there a P wave before each QRS? Are P waves upright and uniform? Yes Yes, for conducted beats 4. What is the length of the PR interval? Progressively prolongs until a QRS is not conducted 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Less than 0.12 seconds (3 small squares)
33 Causes and S/S of 2 nd Degree AV Block Mobitz Type I (Wenckebach) Causes May occur normally in an otherwise healthy person Coronary artery disease Inferior wall MI Rheumatic fever Medications propanolol, digitalis, verapamil Increased vagal stimulation Signs and Symptoms Usually asymptomatic Lightheadedness Hypotension Symptoms may be more pronounced if the ventricular rate is slow
34 Risk and Medical Tx of 2 nd Degree AV Block Mobitz Type I (Wenckebach) Risk Reduced cardiac output, although this is uncommon Progression to 3 rd degree block! Treatment No treatment is usually necessary if the patient is asymptomatic Treat the underlying cause Monitor closely to detect progression to a more serious form of block, especially if the block occurs during an MI If symptomatic Atropine may improve AV node conduction Temporary pacemaker may help with symptom relief until the rhythm resolves itself
35 2 nd Degree AV Block Mobitz Type II Occurs when there is intermittent interruption of conduction Less common that a 2 nd Degree Type 1 block, but more dangerous PR intervals are regular for conducted beats The atrial rhythm is regular The ventricular rhythm is irregular due to dropped or nonconducted (blocked) beats Will have constant PR intervals with randomly dropped QRS s
36 5 Steps to Identify 2 nd Degree AV Block Mobitz Type II 1. What is the rate? Atrial: unaffected Ventricular: usually slower than atrial, bradycardic 2. What is the rhythm? Atrial: regular Ventricular: irregular 3. Is there a P wave before each QRS? Are P waves upright and uniform? Yes, some not followed by a QRS Yes, for conducted beats 4. What is the length of the PR interval? Constant for conducted beats 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes, intermittently absent Less than or greater than 0.12 seconds
37 Causes and S/S of 2 nd Degree AV Block Mobitz Type II Causes Anterior wall MI Degenerative changes in the conduction system Severe coronary artery disease Signs and Symptoms May be asymptomatic as long as cardiac output is maintained Palpitations Fatigue Dyspnea Chest pain Lightheadedness Hypotension
38 Risk and Medical Tx of 2 nd Degree AV Block Mobitz Type II Risk Reduced cardiac output Progression to 3 rd degree AV block (complete) Treatment May choose to just observe an asymptomatic patient Bedrest to reduce myocardial oxygen demands Oxygen therapy Focus on raising the heart rate to improve cardiac output Isopreterenol Permanent pacemaker
39 3 rd Degree AV Block Complete heart block, AV dissociation Is the most serious type of heart block May progress to asystole, because ventricular rate is usually very slow and ineffective Impulses from the atria are completely blocked at the AV node and can t be conducted to the ventricles P waves are usually march consistently through.no correlation between P s & QRS s
40 5 Steps to Identify 3 rd Degree AV Block 1. What is the rate? Atrial: usually Ventricular: based on site of pacemaker site 2. What is the rhythm? Regular 3. Is there a P wave before each QRS? Are P waves upright and uniform? No relationship to QRS complexes Yes 4. What is the length of the PR interval? Totally variable, no pattern 5. Do all QRS complexes look alike? What is the length of the QRS complexes? Yes Based on site of pacemaker
41 Causes and S/S of 3 rd Degree AV Block Causes Congenital condition Coronary artery disease Anterior or inferior wall MI Degenerative changes in the heart Digitalis toxicity Surgical injury Signs and Symptoms Severe fatigue Dyspnea Chest pain Lightheadedness Changes in mental status Loss of consciousness Hypotension Pallor Diaphoresis
42 Risk and Medical Tx of 3 rd Degree AV Block Risk Reduced cardiac output the patient loses his atrial kick which provides 30% of the blood flow pushes to the ventricles Cardiac standstill Treatment Aim to improve the ventricular rate Atropine Isopreterenol Permanent pacemaker
43 Click on the link! Let s look at what the impulses through the heart look like during a heart block.
44 Bundle Branch Blocks The bundle branches split off from the Bundle of His, one branch for each ventricle Left Bundle Branch Right Bundle Branch Bundle Branch blocks There is an intraventricular conduction delay or block which affects the electrical activity of your heart These electrical patterns can also point to whether the block is affecting the right or the left bundle branch
45 Bundle Branch Blocks Causes of left bundle branch block Never occurs normally Heart disease Congestive heart failure Thickened, stiffened or weakened heart muscle (cardiomyopathy) High blood pressure (hypertension) Anterior wall MI usually signals complete heart block
46 Bundle Branch Blocks Criteria for LBBB QRS duration 0.12 seconds Broad R wave in I and V 6 Prominent QS wave in V 1 Absence of q waves (including physiologic q waves) in I and V 6
47 Bundle Branch Blocks LBBB notice the broad, notched R wave in V1 and V6 and absent Q wave in lead V6 Notched R wave
48 Bundle Branch Blocks Causes of right bundle branch block A heart abnormality that's present at birth (congenital) such as atrial septal defect, a hole in the wall separating the upper chambers of the heart A heart attack (myocardial infarction) A viral or bacterial infection of the heart muscle (myocarditis) High blood pressure (hypertension) Scar tissue that develops after heart surgery A blood clot in the lungs (pulmonary embolism)
49 Bundle Branch Blocks Criteria for RBBB QRS duration 0.12 seconds rsr pattern or notched R wave in V 1 Wide S wave in I and V 6
50 Bundle Branch Blocks RBBB notice the notched R wave of V1 and the broad S wave in I and V6 Notched R wave
51 Bundle Branch Blocks: Treatment Treat the underlying heart disease Reasons for implanting a pacemaker When disease in both the right and left bundle branches appears after an acute heart attack (complete heart block) When bundle branch block is associated with syncope (loss of consciousness) When BBB is associated with heart failure and a reduced left ventricular ejection fraction
52 TEMPORARY PACEMAKERS
53 Temporary Pacemakers Objectives Explain the situations when temporary pacemakers are indicated. Describe the principles of pacing. Illustrate normal and abnormal pacemaker behavior. Discuss the steps to be taken in troubleshooting a temporary pacemaker.
54 What is a Pacemaker? A pacemaker is a small device that's placed in the chest (or on rare occasion, the abdomen) to help control abnormal heart rhythms or arrhythmias. This device uses electrical pulses to prompt the heart to beat at a normal rate.
55 Reasons for Pacemaker Insertion Pacemakers are used to treat arrhythmias. Arrhythmias are problems with the rate or rhythm of the heartbeat. During an arrhythmia, the heart can beat too fast, too slow, or with an irregular rhythm. Severe arrhythmias can damage the body's vital organs and may even cause loss of consciousness or death.
56 Reasons for Pacemaker Insertion During an arrhythmia, the heart may not be able to pump enough blood to the body which may cause symptoms of decreased cardiac output such as fatigue (tiredness), shortness of breath, fainting (syncope), hypotension and decreased LOC. A pacemaker can relieve many arrhythmia symptoms, including fatigue and syncope. A pacemaker also can help a person who has abnormal heart rhythms resume a more active lifestyle. 56
57 Types of a Pacemakers Pacemakers can be temporary or permanent. Temporary pacemakers Used to treat temporary heartbeat problems, such as a slow heartbeat that's caused by a heart attack, heart surgery, or an overdose of medicine. Temporary pacemakers are also used during emergencies until a permanent pacemaker can be implanted or until the temporary condition goes away. If the patient has a temporary pacemaker, they will stay in the hospital as long as the device is in place. Permanent pacemakers are used to control long-term heart rhythm problems. 57
58 Speeds up a slow heart rate. Functions of a Pacemaker Helps control an abnormal rhythm or fast heart rate. Makes sure the ventricles contract normally if the atria are quivering instead of beating with a normal rhythm (as in atrial fibrillation). Coordinates the electrical signaling between the upper and lower chambers of the heart. Coordinates the electrical signaling between the ventricles. Pacemakers that do this are called cardiac resynchronization therapy (CRT) devices. CRT devices are used to treat heart failure. Prevents dangerous arrhythmias caused by a disorder called long Q-T syndrome. 58
59 Who needs a Pacemaker? The most common reasons are bradycardia and heart block. Bradycardia is a slower than normal heartbeat. Those with Heart blocks Is a problem with the heart's electrical system and occurs when an electrical signal is slowed or disrupted as it moves through the heart. Can happen as a result of aging, damage to the heart from a heart attack, or other conditions that interfere with the heart's electrical activity. Certain nerve and muscle disorders also can cause heart block, including muscular dystrophy. 59
60 Who needs a Pacemaker? An Aging Heart or Heart Disease Can damage your sinus node's ability to set the correct pace for your heartbeat. Such damage can cause slower than normal heartbeats or long pauses between heartbeats (sinus arrest). The damage also can cause your heart to alternate between slow and fast rhythms (sick sinus syndrome). 60
61 Who needs a Pacemaker? Having a medical procedure to treat an arrhythmia called atrial fibrillation. A pacemaker can help regulate your heartbeat after the procedure. Taking certain heart medicines, such as beta blockers which may slow your heartbeat too much. 61
62 Who needs a Pacemaker? Fainting (syncope) or having other symptoms of a slow heartbeat. For example, this may happen if the main artery in your neck that supplies your brain with blood is sensitive to pressure. Just quickly turning your neck can cause your heart to beat slower than normal. If that happens, not enough blood may flow to your brain, causing you to feel faint or collapse (syncopal episode). 62
63 Who needs a Pacemaker? Having heart muscle problems that cause electrical signals to travel too slowly through your heart muscle. Having Long Q-T Syndrome, which puts you at risk for dangerous/lethal arrhythmias. Children, adolescents, and people who have certain types of congenital heart disease may get pacemakers. Pacemakers also are sometimes implanted after heart transplants. 63
64 How a Pacemaker Functions A pacemaker system consists of a battery, a computerized generator, and wires with sensors called electrodes on one end. The battery powers the generator, and both are surrounded by a thin metal box. The wires connect the generator to the heart. 64
65 How a Pacemaker Functions A pacemaker monitors and helps control the heartbeat. The electrodes detect the heart's electrical activity and sends data through the wires to the computer in the generator. If the heart rhythm is abnormal, the computer will direct the generator to send electrical pulses to the heart. The pulses then travel through the wires to reach the heart. 65
66 How a Pacemaker Functions Newer pacemakers also can monitor your blood temperature, breathing, and other factors and adjust the heart rate to changes in activity. The pacemaker's computer also records the heart's electrical activity and heart rhythm. The physician will use these recordings to adjust the pacemaker so it works better. The physician can program the pacemaker's computer with an external device. 66
67 How a Pacemaker Functions Pacemakers have one to three wires that are each placed in different chambers of the heart. Single chamber pacemaker The wires in a single-chamber pacemaker usually carry pulses between the right ventricle and the generator. 67
68
69 Principles of Pacing Temporary pacing types Transcutaneous Emergency use with external pacing/defib unit Transvenous Emergency use with external pacemaker Epicardial Wires sutured to right atrium & right ventricle Atrial wires exit on the right of the sternum Ventricular wires exit on the left of the sternum 69
70 Principles of Pacing Wiring systems Unipolar One electrode on the heart (-) Signals return through body fluid and tissue to the pacemaker (+) Bipolar Two electrodes on the heart (- & +) Signals return to the ring electrode (+) above the lead (-) tip 70
71 Principles of Pacing Modes of Pacing Atrial pacing Intact AV conduction system required Ventricular pacing Loss of atrial kick Discordant ventricular contractions Sustains cardiac output Atrial/Ventricular pacing Natural pacing Atrial-ventricular synchrony 71
72 Principles of Pacing 3-letter NBG Pacemaker Code First letter: Chamber Paced V- Ventricle A- Atrium D- Dual (A & V) O- None 72
73 Principles of Pacing 3-letter NBG Pacemaker Code Second letter: Chamber Sensed V- Ventricle A- Atrium D- Dual (A & V) O- None 73
74 Principles of Pacing 3-letter NBG Pacemaker Code Third letter: Sensed Response T- Triggers Pacing I- Inhibits Pacing D- Dual O- None 74
75 Principles of Pacing Commonly used modes: AAI - atrial demand pacing VVI - ventricular demand pacing DDD atrial/ventricular demand pacing, senses & paces both chambers; trigger or inhibit AOO - atrial asynchronous pacing 75
76 Principles of Pacing Atrial and ventricular output Milliamperes (ma) Typical atrial ma 5 Typical ventricular ma 8-10 AV Interval Milliseconds (msec) Time from atrial sense/pace to ventricular pace Synonymous with PR interval Atrial and ventricular sensitivity Millivolts (mv) Typical atrial: 0.4 mv Typical ventricular: 2.0mV 76
77 Temporary Pacemaker Medtronic 5388 Dual Chamber (DDD) 77
78 Pacemaker EKG Strips Assessing Paced EKG Strips Identify intrinsic rhythm and clinical condition Identify pacer spikes Identify activity following pacer spikes Failure to capture Failure to sense EVERY PACER SPIKE SHOULD HAVE A P-WAVE OR QRS COMPLEX FOLLOWING IT. 78
79 Normal Pacing Normal Atrial Pacing Atrial pacing spikes followed by P waves Pacing spikes Followed by a P wave 79
80 Normal Pacing Normal Ventricular pacing Ventricular pacing spikes followed by wide, bizarre QRS complexes QRS will look wide and bizarre b/c impulse is generated in the ventricle does not follow normal pathways from atria Pacing spikes Followed by QRS 80
81 Normal Pacing Normal A-V Pacing Atrial & Ventricular pacing spikes followed by atrial & ventricular complexes 81
82 Normal Pacing DDD mode of pacing Ventricle paced at atrial rate 82
83 Abnormal Pacing Atrial non-capture Atrial pacing spikes are not followed by P waves Impulse is sent from the pacer, but is not captured by the ventricle therefore no QRS following a pacer spike Pacer spike No P wave after spike 83
84 Abnormal Pacing Ventricular non-capture Ventricular pacing spikes are not followed by QRS complexes Impulse is sent from the pacer, but is not captured by the ventricle therefore no QRS following a pacer spike Pacing spike No QRS following QRS complex 84
85 Failure to Capture Causes Insufficient energy delivered by pacer Low pacemaker battery Dislodged, loose, fibrotic, or fractured electrode Electrolyte abnormalities Acidosis Hypoxemia Hypokalemia Danger - poor cardiac output 85
86 Failure to Capture Solutions View rhythm in different leads Change electrodes Check connections Increase pacer output ( ma) Change battery, cables, pacer 86
87 Abnormal Pacing Atrial undersensing Atrial pacing spikes occur irregardless of P waves Pacemaker is not seeing intrinsic activity P wave from pt s intrinsic Pacer sent impulse anyways 87
88 Abnormal Pacing Ventricular undersensing Ventricular pacing spikes occur regardless of QRS complexes Pacemaker is not seeing intrinsic activity Pt s own intrinsic QRS Pacer sends impulse anyways (pacer spike) 88
89 Failure to Sense Causes Pacemaker not sensitive enough to patient s intrinsic electrical activity (mv) Insufficient myocardial voltage Dislodged, loose, fibrotic, or fractured electrode Electrolyte abnormalities Low battery Malfunction of pacemaker or bridging cable 89
90 Failure to Sense Danger is potential for pacer spike to land on T wave Potential (low) Can cause Vfib! Pacer spike on T wave Vfib!!! 90
91 Failure to Sense Solution View rhythm in different leads Change electrodes Check connections Increase pacemaker s sensitivity ( mv) Change cables, battery, pacemaker Check electrolytes 91
92 Assessing Underlying Rhythm Carefully assess underlying rhythm Right way: slowly decrease pacemaker rate until lower than patient s own intrinsic rhythm 92
93 Assessing Underlying Rhythm Assessing Underlying Rhythm Wrong way: pause pacer or unplug cables 93
94 Practice Strip#1 94
95 Mode: AAI Interpretation: Normal atrial pacing
96 Practice Strip #2 96
97 Interpretation: Normal sinus rhythm no pacing May possibly have backup demand rate set if HR falls below certain rate
98 Practice Strip #3 98
99 Mode: DDD (should be pacing atria and ventricles) Interpretation: Ventricular failure to sense Troubleshootin: decrease mv (makes the pacer more sensitive)
100 Practice Strip #4 100
101 Mode: VVI Interpretation: Normal ventricular pacing
102 Practice Strip #5 102
103 Ventricular pacer spike, but no QRS following Atrial pacer spike but no P wave following Mode: DDD Interpretation: Failure to capture atria & ventricles (the P waves seen are the pt s own intrinsic P wave) Troubleshooting: Increase the atrial and ventricular ma
104 Practice Strip #6 104
105 Mode: DDD Interpretation: Normal atrial & ventricular (A-V) pacing
106 Practice Strip #7 106
107 P waves Mode: VVI Interpretation: Normal ventricular pacing w/ normal atrial sensing (note the p wave present without an atrial pacer spike pt is generating on atrial impulse)
108 Practice Strip #8 108
109 Pt generated own P wave, therefore there shouldn t be a pacer spike This pacer spike ok b/c no prior P wave Mode: DDD Interpretation: Atrial failure to sense with normal ventricular pacing Troubleshooting: Decrease mv (making pacer more sensitive)
110 Practice Strip #9 4/07 110
111 No pacer spike for ventricles Mode: VVI Interpretation: Ventricular over-sensing (pacemaker failed to send impulse to generate a ventricular response) Troubleshooting: Increase mv (making pacer less sensitive)
112 ASSESSMENT AND TREATMENT OF THE PATIENT WITH CARDIAC EMERGENCIES
113 Assessment and Treatment of the Patient With Cardiac Emergencies Objectives Discuss the indicators used to differentiate chest pain of cardiac origin from noncardiac origin Describe the pathophysiology of angina pectoris Describe the assessment and management of the patient with angina pectoris Describe the pathophysiology of myocardial infarction
114 Assessment and Treatment of the Patient With Cardiac Emergencies Objectives (continued) Discuss the assessment and management of the patient with acute myocardial infarction Describe the physiology associated with heart failure Discuss the signs and symptoms of left ventricular failure and those of right ventricular failure List the interventions prescribed for the patient in congestive heart failure
115 Assessment and Treatment of the Patient With Cardiac Emergencies Objectives (continued) Define and describe the pathophysiology, assessment, and management of cardiac tamponade Define and describe the pathophysiology, assessment, and management of cardiogenic shock
116 Chest Pain Chest pain is the most common presenting symptom of cardiac disease Patients may express a feeling of impending doom Often patients prefer to believe that they are merely experiencing indigestion and symptoms would be gone by morning
117 Chest Pain Chest pain of cardiac origin is typically described as crushing or squeezing in nature Associated with nausea, vomiting, and diaphoresis May radiate to other areas (jaw, shoulder, arm, etc.)
118 Chest Pain
119 Chest Pain Neuropathy due to destruction of nerve endings can cause inability to perceive pain due to diseases of the nerves Diabetics May present as congestive heart failure as the first symptom of AMI
120 Non-Cardiac Causes of Chest Pain Pleurisy Costrochondritis Pericarditis Myocardial contusion Secondary to trauma Pneumothorax Hemopneumothorax Tension pneumothorax Muscle strain Trauma
121 Angina Pectoris Pain that results from reduction in blood supply to myocardial tissue Pain is typically temporary Commonly caused by atherosclerosis Often predictably associated with exercise Pain is felt when the heart requires more oxygen than the narrowed blood vessels can supply
122 Angina Pectoris
123 Angina Pectoris Stable or predictable angina A particular activity may elicit chest pain Symptoms will usually respond well to appropriate treatment Rest Administration of oxygen Unstable angina Is not elicited by activity Most often occurs at rest Indicates a progression of atherosclerotic heart disease, and is also referred to as preinfarctional angina
124 Angina Pectoris Management Place patient at rest in calm, quiet area Provide reassurance Obtain 12 lead EKG if possible Administer oxygen IV line Administer nitroglycerin
125 Nitroglycerin Causes dilation of blood vessels that reduces the workload of the heart Reduces the need for oxygen because the heart has to pump blood against a lesser pressure Blood remains in dilated vessels and less is returned to the heart
126 Acute Myocardial Infarction Results from a prolonged lack of blood flow to a portion of myocardial tissue and results in a lack of oxygen Myocardial cellular death will follow Electrical properties of cardiac muscle altered or lost Ability of cardiac muscle to function properly is lost
127 Acute Myocardial Infarction Most common cause is thrombus formation Blocks coronary arteries Arteries narrowed by atherosclerotic disease are one of the conditions that increase likelihood of myocardial infarction (MI)
128 Acute Myocardial Infarction
129 Patient Assessment and Management
130 100 percent oxygen Establish an IV line Patient Assessment and Management Measure oxygen saturation level Continuous cardiac monitoring Pain control and management Nitroglycerin, Morphine Sulfate, Demerol Thrombolytic therapy, aspirin
131 ST Elevation ST segment elevation MI (STEMI) is caused by: A complete obstruction of a coronary artery, resulting in damage/necrosis of the full thickness of the heart muscle Diffuse ST segment elevation may be caused by pericarditis Non-ST segment elevation MI (NSTEMI) is caused by: Non-occlusive thrombus Brief occlusion Occlusion with adequate collaterals This results in necrosis involving only partial thickness of the heart muscle
132 ST Elevation ST elevation due to MI usually demonstrates a regional or territorial pattern Anatomic region of the heart and the most likely associated coronary artery: Inferior - Right coronary artery (RCA) Anteroseptal - Left anterior descending (LAD) Anteroapical - Left anterior descending (Distal) Anterolateral - Circumflex Posterior - Right coronary artery (RCA)
133 ST Elevation These regional areas correspond to specific leads on the EKG: V2 through V5 - Anterior MI (LAD) V2 and V3 - Septal MI (LAD) V1, V2, V4, and V5 Anteroseptal MI (LAD) I, AVL Lateral MI (Cx) V4 through V6 Anterolateral MI (Cx) II, III and AVF Inferior MI (RCA) V1 and V2 Posterior MI (RCA)
134 Example of ST Elevation ST Elevation
135 Example of ST Elevation ST Elevation
136 ST Elevation Example of an Inferior MI (Note ST elevation in leads II, III, avf)
137 ST Elevation Example of an Anterior MI (leads V2-V5)
138 Treatment Chest Pain with ST Segment Elevation Notify MD Obtain EKG within 10 minutes of onset of chest pain preferably before giving NTG Give Aspirin (81mg x4, chewable) NTG 0.4mg SL every 5 minutes x3 (hold for SBP <100) Have patent IV prior to giving Draw labs Cardiac enzymes, BMP and CBC
139 Heart Failure Is the inability of the myocardium to meet the cardiac output demands of the body caused by: Coronary disease Valvular disease Myocardial injury Dysrhythmias Hypertension Pulmonary emboli Systemic sepsis Electrolyte disturbances
140 Left Ventricular Failure When a patient s left ventricle ceases to function in an adequate capacity as to sustain sufficient systemic cardiac output Stroke volume decreases Heart rate increases & vasoconstriction occurs to compensate Increased pressure in left ventricle and left atrium Blood pushed back into pulmonary system Can also be pushed back into the right side of the heart if extensive left heart failure Develop pulmonary edema and hypoxia Pink, frothy sputum and significant dyspnea
141
142 Left Ventricular Failure Emergency management Have patient assume position of comfort 100% high-flow oxygen Utilize pulse 90% saturation Monitor LOC for signs of deterioration Establish KVO rate Maintain EKG monitoring Follow protocol for administration of medications Morphine Lasix Nitroglycerine
143 Right Heart Failure When the right ventricle ceases to function properly Causes increase in pressure in right atrium, forcing blood backward into systemic venous system Most common cause is left heart failure Other causes: Valvular heart disease COPD or cor pulmonale Pulmonary embolism Chronic hypertension
144
145 Right Heart Failure Emergency management Have patient assume position of comfort Oxygenation at level to maintain saturation of at least 90% Establish IV at KVO rate Maintain EKG monitoring Consult physician on administration of medications Observe for signs of developing left heart failure
146 Cardiac Tamponade Excess accumulation of fluid in the pericardial sac Causes vary between trauma and medical S/S Muffled heart sounds Distention of jugular veins Narrowing pulse pressures Hypotension Dyspnea Weak, rapid pulse
147 Cardiac Tamponade Beck s triad Muffled heart sounds JVD Narrowed pulse pressure Pulsus paradoxus Systolic blood pressure that drops more than mmhg during inspiration
148 Cardiac Tamponade Emergency management Ensure and maintain patent airway Administer 100% high-flow oxygen Monitor pulse oximetry Establish and maintain IV support Administer pharmacological agents as indicated Pericardiocentesis Invasive aspiration of fluid from the pericardium with a needle
149 Cardiogenic Shock When left ventricular function is so severely compromised that the heart can no longer meet metabolic requirements of the body Often results from extensive myocardial infarction
150 Cardiogenic Shock Most critical form of CHF Ineffective myocardial contractions result in Marked decreased stroke volume Decreased cardiac output Leading to inadequate tissue perfusion Profound hypotension Compensatory tachycardia Tachypnea, often resulting from pulmonary edema Cool, clammy skin caused by massive vasoconstriction Major dysrhythmias Respiratory difficulty Peripheral edema
151 Cardiogenic Shock Aggressive treatment measures Airway management with high flow oxygen Circulatory support, including IV therapy Patient to assume position of comfort Cardiac monitoring Pulse oximetry, maintain O 2 90% Medication therapy Various vasopressors Dopamine Dobutamine Levophed Other medications Morphine Sulfate Nitroglycerin Lasix Digitalis
152 Time for some practice strips!
153 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
154 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 68 bpm/regular 68 bpm/regular 0.28 sec 0.06 sec Sinus rhythm with first-degree AV block, STsegment depression Copyright 2006 by Mosby Inc. All rights reserved.
155 Rhythm Identification This rhythm strip is from a 52-year-old man with substernal chest pain. He has a history of COPD and mitral valve regurgitation. Blood pressure: 140/78. Copyright 2006 by Mosby Inc. All rights reserved.
156 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 75 bpm/regular 75 bpm/regular 0.14 sec 0.06 to 0.08 sec Sinus rhythm with ST-segment depression Copyright 2006 by Mosby Inc. All rights reserved.
157 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
158 Lengthening PR intervals with dropped QRS Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 60 to 98 bpm/irregular 111 bpm/regular Lengthens 0.08 sec Second-degree AV block, type I Copyright 2006 by Mosby Inc. All rights reserved.
159 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
160 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 75 bpm/regular None None 0.08 sec Accelerated junctional rhythm Copyright 2006 by Mosby Inc. All rights reserved.
161 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
162 Pacer spikes Atrial paced activity? No Ventricular paced activity? Yes Paced interval rate 65 Identification 100% ventricular paced rhythm Copyright 2006 by Mosby Inc. All rights reserved.
163 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
164 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 45 bpm/regular 115 bpm/regular No correlation between P & QRS; therefore cannot be measured! 0.16 sec Complete (third-degree) AV block Copyright 2006 by Mosby Inc. All rights reserved.
165 Rhythm Identification This rhythm strip is from a 66-year-old man complaining of chest pain. Blood pressure: 170/96. Copyright 2006 by Mosby Inc. All rights reserved.
166 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 107 bpm/regular 107 bpm/regular 0.24 sec 0.08 sec Sinus tachycardia with first-degree AV block Copyright 2006 by Mosby Inc. All rights reserved.
167 Rhythm Identification This rhythm strip is from a 76-year-old woman complaining of back pain. Her medical history includes a myocardial infarction 2 years ago. Copyright 2006 by Mosby Inc. All rights reserved.
168 Atrial paced activity? No Ventricular paced activity? Yes Paced interval rate 65 Identification 100% ventricular paced rhythm Copyright 2006 by Mosby Inc. All rights reserved.
169 Rhythm Identification This rhythm strip is from an 81-year-old woman with an altered level of responsiveness. blood pressure: 160/70, blood sugar: 114. Copyright 2006 by Mosby Inc. All rights reserved.
170 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 56 bpm/regular 56 bpm/regular 0.24 sec 0.06 sec Sinus bradycardia with first-degree AV block Copyright 2006 by Mosby Inc. All rights reserved.
171 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
172 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 29 bpm/regular 71 bpm/regular Varies 0.16 sec Complete (third-degree) AV block with ST-segment elevation Copyright 2006 by Mosby Inc. All rights reserved.
173 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
174 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 29 bpm/essentially regular None None 0.04 to 0.06 sec Junctional bradycardia with ST-segment depression Copyright 2006 by Mosby Inc. All rights reserved.
175 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
176 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 44 bpm/regular 44 bpm/regular None 0.08 sec Junctional rhythm; ST-segment elevation Copyright 2006 by Mosby Inc. All rights reserved.
177 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
178 Ventricular rate/rhythm Atrial rate/rhythm PR interval QRS duration Identification 60 to 98 bpm/irregular 111 bpm/regular Lengthens 0.08 sec Second-degree AV block type I; ST-segment depression Copyright 2006 by Mosby Inc. All rights reserved.
179 Rhythm Identification Copyright 2006 by Mosby Inc. All rights reserved.
180 Atrial pacing? Yes Ventricular pacing? Yes Paced interval 71 Identification 100% paced rhythm AV pacemaker Copyright 2006 by Mosby Inc. All rights reserved.
181 How about a game??
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
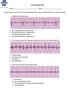 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Equine Cardiovascular Disease
 Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Equine Cardiovascular Disease 3 rd most common cause of poor performance in athletic horses (after musculoskeletal and respiratory) Cardiac abnormalities are rare Clinical Signs: Poor performance/exercise
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Basics of Pacing. Ruth Hickling, RN-BSN Tasha Conley, RN-BSN
 Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Basics of Pacing Ruth Hickling, RN-BSN Tasha Conley, RN-BSN The Cardiac Conduction System Cardiac Conduction System Review Normal Conduction Conduction QRS QRS Complex Complex RR PP ST ST segment segment
Basic Cardiac Rhythms Identification and Response
 Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Interpreting AV (Heart) Blocks: Breaking Down the Mystery
 Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
ACLS Chapter 3 Rhythm Review Instructor Lesson Plan to Accompany ACLS Study Guide 3e
 ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
the basics Perfect Heart Institue, Piyavate Hospital
 ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
Treatments to Restore Normal Rhythm
 Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Living with. Atrial Fibrillation
 Living with Atrial Fibrillation U nderstanding Atrial Fibrillation An estimated 2.7 million Americans are living with atrial fibrillation (AF). That makes it the most common heart rhythm abnormality in
Living with Atrial Fibrillation U nderstanding Atrial Fibrillation An estimated 2.7 million Americans are living with atrial fibrillation (AF). That makes it the most common heart rhythm abnormality in
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Radiofrequency Ablation for Atrial Fibrillation. A Guide for Adults
 Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Systematic Approach to 12 Lead EKG Interpretation
 Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Adult Cardiac Surgery ICD9 to ICD10 Crosswalks
 164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
RAPID INTERPRETATION OF. EKG s
 Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
What to Know About. Atrial Fibrillation
 Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Atrial Fibrillation What to Know About Atrial Fibrillation Understanding Afib Atrial fibrillation, or Afib, is a condition in which the heart beats irregularly speeding up or slowing down, or beating too
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Electrocardiography Review and the Normal EKG Response to Exercise
 Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
What Can I Do about Atrial Fibrillation (AF)?
 Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
Additional Device Information 9529 Reveal XT Insertable Cardiac Monitor The Reveal XT Insertable Cardiac Monitor is an implantable patientactivated and automatically activated monitoring system that records
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Acute Coronary Syndrome. What Every Healthcare Professional Needs To Know
 Acute Coronary Syndrome What Every Healthcare Professional Needs To Know Background of ACS Acute Coronary Syndrome (ACS) is an umbrella term used to cover a spectrum of clinical conditions that are caused
Acute Coronary Syndrome What Every Healthcare Professional Needs To Know Background of ACS Acute Coronary Syndrome (ACS) is an umbrella term used to cover a spectrum of clinical conditions that are caused
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed
 Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
HYPERTROPHIC CARDIOMYOPATHY
 HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
Electrophysiology Daymar College. Lisa H. Young, RN, BSN, MAE 2011
 Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Atrial Fibrillation: The heart of the matter
 Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Atrial Fibrillation: The heart of the matter This booklet has been written especially for people with atrial fibrillation (AF), a heart condition often described as an irregular heartbeat (also known
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Visited 9/14/2011. What is Atrial Fibrillation? What you need to know about Atrial Fibrillation. The Normal Heart Rhythm. 1 of 7 9/14/2011 10:50 AM
 1 of 7 9/14/2011 10:50 AM Current URL: What you need to know about Atrial Fibrillation What is atrial fibrillation? What causes atrial fibrillation? How is atrial fibrillation diagnosed? What are the dangers
1 of 7 9/14/2011 10:50 AM Current URL: What you need to know about Atrial Fibrillation What is atrial fibrillation? What causes atrial fibrillation? How is atrial fibrillation diagnosed? What are the dangers
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona
 Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Christopher M. Wright, MD, MBA Pioneer Cardiovascular Consultants Tempe, Arizona Areas to be covered Historical, current, and future treatments for various cardiovascular disease: Atherosclerosis (Coronary
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
The science of medicine. The compassion to heal.
 A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
A PATIENT S GUIDE TO ELECTROPHYSIOLOGY STUDIES OF THE HEART The science of medicine. The compassion to heal. This teaching booklet is designed to introduce you to electrophysiology studies of the heart.
12 Lead ECGs: Ischemia, Injury & Infarction Part 2
 12 Lead ECGs: Ischemia, Injury & Infarction Part 2 McHenry Western Lake County EMS Localization: Left Coronary Artery Right Coronary Artery Right Ventricle Septal Wall Anterior Descending Artery Left Main
12 Lead ECGs: Ischemia, Injury & Infarction Part 2 McHenry Western Lake County EMS Localization: Left Coronary Artery Right Coronary Artery Right Ventricle Septal Wall Anterior Descending Artery Left Main
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
CBT/OTEP 243 Aspirin Administration for ACS
 Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County 401 5th Avenue, Suite 1200 Seattle, WA 98104 (206) 296-4693 February 2009 CBT/OTEP 243
Seattle-King County EMS Seattle-King County Emergency Medical Services Division Public Health - Seattle/King County 401 5th Avenue, Suite 1200 Seattle, WA 98104 (206) 296-4693 February 2009 CBT/OTEP 243
Atrial Fibrillation (AF) Explained
 James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
VCA Veterinary Specialty Center of Seattle
 An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
An electrocardiogram (ECG) is a graph of the heart`s electrical current, which allows evaluation of heart rate, rhythm and conduction. Identification of conduction problems within the heart begins with
Atrioventricular (AV) node ablation
 Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Atrioventricular (AV) node ablation The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
Banner Staff Service ECG Study Guide
 Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians
 Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99)
 CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99) March 2014 2014 MVP Health Care, Inc. CHAPTER 9 CHAPTER SPECIFIC CATEGORY CODE BLOCKS I00-I02 Acute rheumatic fever I05-I09 Chronic rheumatic heart
CHAPTER 9 DISEASES OF THE CIRCULATORY SYSTEM (I00-I99) March 2014 2014 MVP Health Care, Inc. CHAPTER 9 CHAPTER SPECIFIC CATEGORY CODE BLOCKS I00-I02 Acute rheumatic fever I05-I09 Chronic rheumatic heart
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Electrophysiology study (EPS)
 Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Electrophysiology study (EPS) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Tips and Tricks to Demystify 12 Lead ECG Interpretation
 Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ
 «Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
«Δυσλειτουργία βηματοδότη. Πως μπορούμε να την εκτιμήσουμε στο ιατρείο.» Koσσυβάκης Χάρης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ Diagnostic tools History: symptoms, physical examination 12 leads ECG,
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Atrial Fibrillation. Information for you, and your family, whänau and friends. Published by the New Zealand Guidelines Group
 Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery
 Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
5 MILLION AMERICANS 1. Atrial Fibrillation (AFib) AFib affects an estimated
 A Patient s Guide To with Atrial Fibrillation (AFib) CAUSES RISK FACTORS SYMPTOMS DIAGNOSIS TREATMENTS INSIDE The Healthy Heart... 2 Your Heart In AFib... 4 How Do You Get It?... 6 How Do You Know If You
A Patient s Guide To with Atrial Fibrillation (AFib) CAUSES RISK FACTORS SYMPTOMS DIAGNOSIS TREATMENTS INSIDE The Healthy Heart... 2 Your Heart In AFib... 4 How Do You Get It?... 6 How Do You Know If You
ST Segment Elevation Nothing is ever as hard (or easy) as it looks
 ST Segment Elevation Nothing is ever as hard (or easy) as it looks Cameron Guild, MD Division of Cardiology University of Mississippi Medical Center February 17, 2012 Objectives 1. Describe the electrical
ST Segment Elevation Nothing is ever as hard (or easy) as it looks Cameron Guild, MD Division of Cardiology University of Mississippi Medical Center February 17, 2012 Objectives 1. Describe the electrical
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL
 Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
Marilyn Borkgren-Okonek, APN, CCNS, RN, MS Suburban Lung Associates, S.C. Elk Grove Village, IL www.goldcopd.com GLOBAL INITIATIVE FOR CHRONIC OBSTRUCTIVE LUNG DISEASE GLOBAL STRATEGY FOR DIAGNOSIS, MANAGEMENT
How To Treat Heart Valve Disease
 The Valve Clinic at Baptist Health Madisonville The Valve Clinic at Baptist Health Madisonville Welcome to the Baptist Health Madisonville Valve Clinic at the Jack L. Hamman Heart & Vascular Center. We
The Valve Clinic at Baptist Health Madisonville The Valve Clinic at Baptist Health Madisonville Welcome to the Baptist Health Madisonville Valve Clinic at the Jack L. Hamman Heart & Vascular Center. We
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
Low Blood Pressure. This reference summary explains low blood pressure and how it can be prevented and controlled.
 Low Blood Pressure Introduction Low blood pressure, or hypotension, is when your blood pressure reading is 90/60 or lower. Some people have low blood pressure all of the time. In other people, blood pressure
Low Blood Pressure Introduction Low blood pressure, or hypotension, is when your blood pressure reading is 90/60 or lower. Some people have low blood pressure all of the time. In other people, blood pressure
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
