Placement of Dental Implants in Irradiated Bone: The Case for Using Hyperbaric Oxygen
|
|
|
- Cornelius Grant
- 8 years ago
- Views:
Transcription
1 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 64: , 2006 Placement of Dental Implants in Irradiated Bone: The Case for Using Hyperbaric Oxygen Gösta Granström, DDS, MD, PhD* Radiation therapy was originally considered a contraindication for installation of dental implants. 1 Nevertheless, the need to optimally rehabilitate cancer patients has challenged this position. To answer whether the irradiated cancer patient who is scheduled for rehabilitation with osseointegrated implants (OI) would need hyperbaric oxygen therapy (HBO) before surgery, one fundamental question must be asked: Will the patient be subjected to any risk related to OI surgery in relation to having been treated with radiation therapy, or will the implant procedure be performed smoothly without side effects? If the clinician can predict, based on best evidence that there will be no anticipated problems, then HBO is not necessary. The following discussion, however, relates to those patients for whom the experienced OI clinician can anticipate problems in the course of the rehabilitation process of a patient exposed to radiation therapy. The accurate prediction of problems that would challenge OI intervention is of primary importance in the management of the irradiated patient. A series of important questions that the clinician should ask before planning rehabilitation are therefore discussed below, and the author makes an attempt to answer them in a scientifically valid way, based on today s existing knowledge. The reader will then be aware of the pitfalls that might reduce the benefits of OI in the irradiated patient and how some potential challenges and complications can be prevented with HBO. *Professor and Chairman, Department of Otolaryngology, Head and Neck Surgery, Göteborg University, Gothenburg, Sweden. Address correspondence and reprint requests to Dr Granström: ENT-clinic, Sahlgrenska University Hospital, SE Gothenburg, Sweden; gosta.granstrom@orlss.gu.se 2006 American Association of Oral and Maxillofacial Surgeons /06/ $32.00/0 doi: /j.joms Is There a Reason to Use the OI Concept in the Irradiated Patient? The answer is definitely yes. Several publications addressing this question have been published during the last 2 decades. 2-9 The reported benefits the patient can anticipate are related to better masticatory ability from an implant-supported prosthesis, and less damage to the oral mucosa from a denture, particularly if xerostomia is present. Factors such as facilitated swallowing and speech function are also improved. Some cancer patients suffer combined defects from surgery in adjacent tissues such as cheeks, maxillary sinuses, nose, and orbits. These defects usually require cosmetic and functional coverage so that the patient can speak and be a fully social person. A better quality of life is thus expected in patients who have received OI for the treatment of cancer and have persistent side effects from their tumor treatment. However, based on our knowledge of the problems that can arise during the OI procedure, it is the author s strong recommendation that the rehabilitation of irradiated patients should be performed at clinics and institutions that are experienced in treating cancer patients. It should not be part of the general dentist s practice. Are There Any General Drawbacks From Rehabilitating Cancer Patients According to the OI Concept? RECURRENCE When rehabilitating a cancer patient, the risk for tumor recurrence or distant metastases exists. Therefore, many clinicians wait a certain time after cancer treatment to detect possible recurrences. The appropriate surveillance time interval between resection and placement of implants is still controversial. In our clinical material, representing more than 100 cancer patients followed since 1979, a high number of 812
2 GÖSTA GRANSTRÖM 813 cancer patients have survived their disease and are alive and successfully rehabilitated with the OI concept. 10 Mean survival time for those cancer patients still alive today is 16 years, compared with 10 years mean survival time for those who have died. Because of the long expected survival of cancer patients, we are therefore committed to rehabilitating them according to the OI concept. On the other hand, we must plan for a rehabilitation that will last for at least 10 to 20 years. Therefore, implant survival is of great importance in this respect. TUMOR TYPE AND TUMOR SURGERY A vast variety of cancers can occur in the head and neck region. The size and location of tumor might differ, so each patient would need quite different rehabilitation procedures including bone grafts, bone containing flaps and soft tissue flaps in conjunction with OI surgery. The rehabilitation must therefore be individualized for the specific patient. The management of these patients is complex and should occur within a team setting. In our implant unit at the Department of Otolaryngology, Head and Neck Surgery (Göteborg University, Gothenburg, Sweden), we have been working very closely in a team consisting of an oral radiologist, oral surgeon, prosthodontist, maxillofacial surgeon, ear nose and throat surgeon, plastic surgeon, and anaplastologist to plan and perform the variety of required procedures. When needed, other specialists such as speech therapists, dieticians, and physiotherapists have been consulted before treatment. In our files of patients treated during the last 25 years, we have found no factor related to specific drawbacks for the OI-concept regarding tumor type, size, stage, local nodes, or metastasis. Likewise, no specific tumor surgery factor, such as local resections or neck dissection, was related to specific problems encountered with the OI concept. 10 When the implant team and cancer team work closely together, optimal planning for the rehabilitation is achieved. For example, questions such as: can bone necessary for OI implants in the tumor cavity be saved, and can implants be installed at the time of tumor surgery, can be answered before surgery. One must also be aware that there are specific cancer patients with such complicated defects, with such poor tissue quality and other negative contributing factors, that using osseointegration might be impossible. Other solutions must be sought for those patients. GENDER, AGE We have found no evidence in our files that implant survival or complications differ between female and male cancer patients. This holds true even in those cases where osteoporosis may exist. 10 Likewise, we have found that advanced age is not a contraindication. In our active patient files we have 2 irradiated patients who are both 100 years old and are still satisfied implant wearers after more than 20 years. SMOKING, ALCOHOL Several studies have shown that implant failures are higher among smokers. 11 Because a high percentage of patients with cancers of the head and neck region are heavy smokers and alcohol abusers, restriction of these drugs in the planning procedure is recommended. Whether this statement is also valid for irradiated patients is unclear at present. 10 What Factors From Radiotherapy Might Affect OI? RADIOTHERAPY BEFORE/AFTER TUMOR SURGERY There are different cancer therapy approaches throughout the world. In Sweden there is a long tradition of irradiating most cancer patients before tumor surgery. However, from the surgical point of view, it is advantageous to perform tumor surgery before irradiation. Healing of the surgical wound then proceeds more rapidly with fewer complications such as reduced soft tissue healing time, denuded bone, fistula formation, and infections. 12 If osseointegration is taking place at the same time as tumor surgery, the benefit of installing OI implants in nonirradiated bone is then achieved. RADIOTHERAPY BEFORE/AFTER OI SURGERY As a consequence of the practice standards in Sweden, the majority of our cancer patients have been irradiated before osseointegration surgery. Most of the discussion in this article is therefore related to our experience in the irradiated patient. The reverse situation (irradiation with implants already placed in the radiation field), however, may be encountered clinically. There are relatively few studies addressing outcomes of irradiating already-placed implants, but from our previous studies it appears that implant failures during a short-term follow-up were not particularly high. 13 However, according to newer data, implant failures have increased during a longer follow-up. 10 This phenomenon, that implant failures in irradiated bone increase with longer follow-up time, makes it important to define the follow-up time of each study when discussing benefits and drawbacks from OI in irradiated bone. Reporting success with only 2 to 3 years follow-up may give a false impression that OI surgery in irradiated bone is simple and straightforward.
3 814 PLACEMENT OF DENTAL IMPLANTS IN IRRADIATED BONE IRRADIATION DOSE From the available literature, it seems some authors have recommended that OI surgery is safe in patients who have been irradiated at doses below 50 to 55 Gy By defining this selection criterium, no protective measures were found necessary. On the other hand, patients irradiated above 55 Gy would not be rehabilitated with OI implants. That would exclude the majority of cancer patients at our institution from rehabilitation. From an ethical standpoint, it is questionable to leave such a large portion of cancer patients without rehabilitation. We have therefore set out to rehabilitate all patients despite the dose of radiotherapy. Consequently, some patients have been rehabilitated at extremely high doses ( 120 Gy). Implant survival at this high dosage has been very low, and the risk for osteoradionecrosis (ORN) is high. Nevertheless, it is important to define the limitations for the OI concept. The dose Gy (previously termed rad) is furthermore misleading because this denomination does not account for the number of fractions given. If the term cumulative radiation effect is applied and calculated as (Total time of treatment/number of treatments) 0.11 Dose per treatment Number of treatments , a more reliable estimation of irradiation dose can be obtained. Data then show that below a cumulative radiation effect of 18 to 20, relatively few implants will fail (corresponding to 48 to 65 Gy given as standard fractionation radiotherapy), whereas implant failures increase at higher doses. In our experience, at doses above cumulative radiation effect 40 (120 Gy, standard fractionation), all implants have failed. 3,10,18,19 Implants in the same jaw might have been exposed to different irradiation doses. For example, a patient treated for a tonsillar carcinoma will have a higher irradiation dose in the posterior mandible than in the anterior portion. It is therefore necessary to calculate irradiation dose at each implant site before surgery to determine the optimum installation site for implants. Newer forms of focused radiation (such as intensity modulated radiation therapy) produce reverse planned non-homogenous 3-dimensional treatment volumes that delivered increased dose. The consequence is that implants installed in the same region might fall into highly differing radiation dose gradients. Patients that have received irradiation to other parts of the body, not including the craniofacial region, would have an expected implant survival in the craniofacial region comparable to nonirradiated patients. No specific precautions would be needed in these patients. TYPE OF IRRADIATION SOURCE: FRACTIONATION Most studies published on osseointegration in irradiated tissues have used 60 Co as the source for radiotherapy since it is still the most commonly used type of radiation. Thus, the data discussed in this section are mainly related to the effects from 60 Co therapy. Other radiation sources are available, and have been used, the effects of which remain uncertain at present. Other fractionation schemes, such as twice per day treatment, have been used and calculated as cumulative radiation effect. 10 With the development of higher energy radiotherapy protocols and superfractionation, it is likely that in time other effects on osseointegration will be identified. Brachytherapy is also a part of modern oncologic treatment, and its effect on bone tissues is different than external beam radiotherapy. Again, too little is known about the effect on osseointegration today. Further studies will have to be performed addressing these questions. TIME FROM RADIOTHERAPY TO OI SURGERY This factor has been shown to affect osseointegration. 3,12,18 Contrary to what one would believe, irradiation from decades ago seems to have a more negative effect on implant survival than recently administered radiotherapy. This may be attributed to earlier forms of radiation therapy being of lower energy; whereas today, higher energy forms of radiation are typically delivered. A further explanation could be the progressive endarteritis taking place in the irradiated bone, which is known to increase with time. 20 Patients and their dentists seem to forget about irradiation a long time ago. Sometimes it is argued that no specific precautions need to be undertaken just because radiotherapy took place such a long time ago. Contrary to this, these patients need to be handled with the utmost care. In relation to the discussion in this article, these patients should be handled at institutions/clinics in the practice of treating cancer patients. Thorough planning, careful surgery, and HBO are required. ADJUVANT CHEMOTHERAPY Many oncologic treatments use chemotherapy as part of cancer treatment, which is most commonly a combination of radiation therapy and chemotherapy. Whether chemotherapy (in most cases a combination of 5-fluorouracil/cisplatin/methotrexate/bleomycine/ vincristine) affects osseointegration is less well documented. In a retrospective investigation, it was shown that chemotherapy given near the time of OI surgery had a negative effect on implant survival. 21 Implant survival was affected less when chemotherapy was administered some time before or within 1 month after OI surgery. In later studies that included a higher
4 GÖSTA GRANSTRÖM 815 number of implants, and followed patients for a longer period of time, it seemed as if chemotherapy in longer-term perspective has a negative effect on osseointegration, comparable to irradiation. 10 BONE BED, GRAFTED BONE The quality of the bone bed appears to be of utmost importance for a successful result of OI surgery. If the bone has a reduced capacity for healing after irradiation it is expected that it will integrate the implants less effectively. Grafted bone that will replace bone in an irradiation field will act more like the nonirradiated bone. 16,22-24 Therefore, the discussion in this article is restricted to bone that has been irradiated and not replaced by grafts. Implant Factors LENGTH Several reports have shown a higher incidence of implant failures when using short implants. 25 Failure rates for short implants are increased when they are placed into irradiated bone. 10,18,26 Very short (3 to 7 mm) implants were particularly prone to failure. 10 One would thus recommend using the longest possible implants to optimize bicortical anchorage. IMPLANT DESIGN AND SURFACE The author s experience is limited to screw-shaped implants with machined surfaces that have been used consecutively and consequently where chosen for our studies. It is difficult to judge from the literature if other implant designs would perform better in the irradiated tissue. There is recent data showing that a relatively rougher surface might improve osseointegration. 25 Whether this is also a benefit for the irradiated patient is not known. ABUTMENTS Loading in the long axis of implants has been shown to distribute forces optimally. In tumor cavities, however, this has not always been possible to obtain. So-called console abutments are used in areas of limited space for facial prosthetics. Their distribution of load often leads to cantilever effects that might be negative for long-term survival of the implants (see below). PROSTHESIS Cancer patients may have defects from tumor surgery that extend well beyond loss of teeth. The implant-supported prosthesis must therefore be planned, designed, and constructed for each patient. At our institution, in several cases, parts of the jawbone and soft tissues needed to be replaced by alloplastic material. In these situations, defects of the lips, cheeks, or maxilla are replaced as part of the treatment. Such combined intraoral and extraoral cases are not common at our institution. RETENTION Implant survival in irradiated bone has been shown to depend on retention of the prosthesis to a high degree. 10,12,18 The highest implant survival was noted for fixed-retention prostheses. The lowest implant survival was seen for facial prostheses anchored on the combination of clips and magnets on cantilever extensions. 18 In the oral cavity, overdentures have been shown to be associated with higher implant failures. 26,27 SOFT TISSUE Eckert et al 28 noted that significant problems in patients with irradiated implants were related to the soft tissues. Gingivitis was more common in these patients than normally observed. Cover-screw mucosal perforations were observed over the areas of 17% of implants during the healing period between stage-1 and stage-2 surgery. 29 August et al, 30 using the fixed mandibular implant system in 18 patients irradiated before or after implant installation, reported increased problems with the soft tissues. Early soft tissue complications included soft tissue overgrowth, tongue ulceration, and intraoral wound dehiscence. Late complications included fistula formation. Watzinger et al 31 reported an increased degree of the gingivitis in irradiated patients. This was mainly related to poor oral hygiene. Necrosis of soft tissues in the floor of the mouth was observed in 5.2% of patients. 2 RISK FOR ORN IN RELATION TO IMPLANT SURGERY It appears that the risk of ORN is the primary reason that implant therapy is not commonly pursued in previously irradiated patients. The incidence of this severe complication may be underreported in the international literature. Some authors refuse to use implant placement, considering the risk for ORN as overshadowing the possible benefit of providing prosthetic restoration. 32 Several groups report incidental cases developing ORN. 2,3,31,33 In their report from 1998, Wagner et al 33 described 1 (1.6%) case of ORN with related failure of 5 implants. The authors were of the opinion that this rate of incidence is below an estimated risk of 5% reported in other studies. Esser and Wagner 2 reported 2 cases (3.4%) of ORN development related to implant surgery. In our material, ORN has appeared in those patients irradiated with extremely high doses after combined pre- and postoperative radiotherapy. 10 Minimum surgical trauma to the mandible is known to cause ORN in the time
5 816 PLACEMENT OF DENTAL IMPLANTS IN IRRADIATED BONE period close to radiotherapy. 20 Such trauma may typically be associated with extraction or surgery for an OI. So, Why Use HBO? Based on the discussion above, in 1988, we made the choice to use HBO as part of the treatment protocol for irradiated implant patients. The reason for choosing this modality was that it was at that time the only known treatment available that could be used clinically and that was known to counteract the negative effects of irradiation. As we were beginning to treat patients at higher risk, such as those who had been exposed to high-dose radiation therapy, our main goal was to reduce implant failure rates that were considered by our group to be unacceptably high. Our choice was based on the scientific knowledge of HBO s effects on irradiated tissues. The exact mechanism that oxygen exerts at the subcellular level remains to be explored. Recent data shows that oxygen under hyperbaric conditions acts synergistically with several growth factors, which stimulate bone growth and turnover, and other studies show that oxygen can act as a growth factor by itself. 34 For a detailed description of the mechanisms and performance of HBO, the reader is referred to a review article by Kindwall et al. 35 A detailed discussion of HBO effects in relation to osseointegration has also been published. 36,37 Principally, HBO has been shown to improve angiogenesis, 38,39 and bone metabolism and bone turnover. 40,41 In relation to radiotherapy, HBO can thus counteract some of the negative effects from irradiation and actually act as a stimulator of osseointegration. 40 EXPERIMENTAL STUDIES Several studies have been performed to analyze the effects from radiotherapy in the bone surrounding OI implants, and the effects from HBO. For a detailed description of the experimental data and discussion, the reader is referred to references 34, 40, and 42. Principally, irradiation will have an effect on the boneforming cells (osteoblasts and osteocytes) that will reduce their capacity for new bone synthesis. The principal resorptive cells in bone, the osteoclasts, can migrate into the bone after radiotherapy and continue bone resorption. With time, there might be an imbalance where resorption exceeds formation. Radiotherapy will also reduce the number of capillaries in the bone because of a progressive endarteritis. With increasing time, a hypovascular bone bed might occur that is less well adapted to host OI implants. In the above-cited studies, HBO has been shown to increase formation of new formed bone, increase the bone turnover, and increase the vascular supply to the irradiated bone. Further, the force necessary to unscrew the implants (removal torque) has been shown to be reduced by irradiation, but increased with HBO. 43 Interestingly, the recorded effects are measurable not only in experimental animals but also clinically in patients. 42 Thus, there is comprehensive experimental evidence that supports the use of HBO to reduce irradiation-induced effects and to increase osseointegration. CLINICAL STUDIES Today, there are more than 100 scientific publications dealing with OIs in irradiated tissues. In an attempt to summarize the results on implant survival, an analysis of the data available in 2001 was performed. 42 The material comprised reports from 4,392 OIs. Implant survival was calculated from the different studies and plotted as a Kaplan-Meier function. Different regions of insertion were separated from each other, as was material from irradiated, nonirradiated, and HBO-treated patients. 42 With increasing follow-up time, all regions showed an increasing implant failure after irradiation that was higher when compared with nonirradiated patients. HBO improved implant survival in all regions that were subjected to radiation therapy. It should also be appreciated that because of its compact structure, the mandible is a relatively radioresistant bone. In the irradiated mandible, implant survival will remain high for many years, but with longer follow-up times, implant failures appear and after 10 years, failures are high (more than 50%). Compared to the mandible, the maxilla is less radioresistant and failures appear after 5 years. By 10 years, as in the mandible, implant failures are high. 42 A multivariate analysis was performed on 107 irradiated patients who altogether had 631 OI implants installed in different regions. Irradiation increased the failure of implants in all regions compared with nonirradiated controls. HBO improved implant survival in all regions (except temporal-parietal) with significance at the P.001 level, using the Wilcoxon-Rank test. 10 Implants in the oral maxilla performed better than the average implant site. The implant sites that performed poorest were the frontal bone, zygoma, mandible, and nasal maxilla. 10 Advocates against the use of adjunctive HBO for irradiated implant patients usually argue that there are no double-blind, controlled clinical studies proving its efficacy. 44 If one considers such a study to be level 1B evidence according to the American Heart Association (AHA), similar to the National Cancer Institute s (NCI) level 1ii, 45 as the ideal study, then that is true. However, today there is 1 AHA level 1C study discussed above. 42 Furthermore, there are 4 AHA level 3 NCI 2 studies conducted on the topic. 3,18,29,46 Addi-
6 GÖSTA GRANSTRÖM 817 tionally, there are 38 clinical studies published at levels AHA 5 and NCI 3ii that show an increased risk for implant failure in irradiated patients compared with nonirradiated controls. There are also 9 clinical studies evaluating the possibility that HBO prevents implant failure at AHA levels 3 to 5 and NCI levels 2 to 3ii. These show a lower risk for implant failure after adjuvant HBO, equal to nonirradiated tissues. If one correlates these studies to each other, the risk for implant failure without HBO prevention would be 734 implants out of 3,431 (21.4%; variance 0 to 100%); and with HBO prevention 147 out of 1,085 implants (13.5%; variance 0 to 16.8%). However, encouraging results are already reported in the scientific literature; the present author strongly supports randomized, controlled studies. Currently, there is a single-blinded, controlled multicenter study being conducted and the goal of the study is to evaluate OI implant failures in irradiated bone. The study further aims to evaluate the effects of HBO on implant survival. Colleagues with an interest in the study are hereby invited to participate. Information and enrollment can be obtained at ProtocolsIndex.htm. In 2 articles published in 1997 by Larsen 47 (as protagonist) and Keller 48 (as antagonist) in the Journal of Oral and Maxillofacial Surgery, these authors debated the use of HBO for OI implants in irradiated mandibles. At that time, there were only 19 publications available addressing this question. Despite the authors referring to essentially the same publications, they came to different conclusions regarding the actual failure rate in irradiated mandibles. The same problem can also be revealed in the above-cited studies that report failures of implants from 0% to 100%. These differences in reported treatment outcomes may be attributed mainly to the difference in the number of implants installed and length of time the implants had been followed. The higher the number of implants included in a study and the longer time they are followed, the more valid the statistics will be. COST FOR PROCEDURE - WHO PAYS? Another argument for not using HBO is the high cost of the procedure. If the patient has to pay for the whole procedure without support from the health care system, this will of course be of substantial importance in the decision. The cost for HBO in relation to the OI procedure varies greatly in different countries. In Sweden, the cost for HBO would be approximately 10% of a complete fixed implant-supported prosthesis in the upper and lower jaw. The cost for HBO and for the OI procedure is fully covered by the Swedish health care system when rehabilitation involves cancer patients. In nonirradiated non-cancer cases, patients pay most of the OI procedure (no HBO necessary). The cost for HBO must also be placed in relation to avoidance of complications. For example, the cost for 30 HBO treatments (implant protocol) is equivalent to just 1 day at an intensive care unit at the Sahlgrenska University Hospital (Gothenberg, Sweden). The cost for the treatment of just 1 patient with ORN is equivalent to the treatment of the HBO protocol for 40 implant patients at the same hospital. SAFETY AND SIDE EFFECTS HBO is regulated by strict standards in each country. Side effects from HBO are mostly related to difficulties in equalizing the pressure in the middle ears. This can be overcome by transmyringeal grommets. Transitional myopia is described by 30% of patients on long-term treatment. Vision invariably returns to normal within weeks after completion of therapy. In centers where HBO is practiced, long-term evaluations show the procedure to be safe and comfortable for the patients with very few side effects. There are hyperbaric chambers available in all countries where OI surgery is performed. A list of chamber availability can be obtained from (in the US) and (Europe). In conclusion, there is sufficient scientific evidence to show a higher failure rate of OI implants in irradiated patients. This high failure rate can be reduced by adjunctive HBO. Important aspects to consider when comparing outcomes with or without HBO are: region of installation, irradiation dose and timing, adjuvant chemotherapy, quality of the bone bed, implant surgery, implant length and design, prosthetic retention, soft tissue, and risk for ORN. It is important that irradiated cancer patients who require OI implants be treated at institutions/clinics that have experience in the treatment of such patients. 7 References 1. NIH Consensus Development Program: Dental Implants. National Institutes of Health Consensus Development Conference Statement, Available at: DentalImplants069html.htm. Accessed February 9, Esser E, Wagner W: Dental implants following radical oral cancer surgery and adjuvant radiotherapy. Int J Oral Maxillofac Implants 12:552, Granström G, Tjellström A, Brånemark P-I, et al: Bone-anchored reconstruction of the irradiated head and neck cancer patient. Otolaryngol Head Neck Surg 108:334, Marker P, Siemssen SJ, Bastholt L: Osseointegrated implants for prosthetic rehabilitation after treatment of cancer of the oral cavity. Acta Oncol 36:37, Marx RE, Morales MJ: The use of implants in the reconstruction of oral cancer patients. Dent Clin North Am 42:177, McGhee MA, Stern SJ, Callan D, et al: Osseointegrated implants in the head and neck cancer patient. Head Neck 19:659, Parel SM, Tjellström A: The United States and Swedish experience with osseointegration and facial prostheses. Int J Oral Maxillofac Implants 6:75, 1991
7 818 PLACEMENT OF DENTAL IMPLANTS IN IRRADIATED BONE 8. Tolman DE, Taylor PF: Bone-anchored craniofacial prosthesis study: Irradiated patients. Int J Oral Maxillofac Implants 11:612, Wolfaardt JF, Wilkes GH, Parel SM, et al: Craniofacial osseointegration: The Canadian experience. Int J Oral Maxillofac Implants 8:197, Granström G: Osseointegration in irradiated tissues. Experience from our first 100 treated patients. J Oral Maxillofac Surg 2006 (in press) 11. Quirynen M, De Soete M, van Steenberghe D: Infectious risks for oral implants: A review of the literature. Clin Oral Implant Res 13:1, Granström G: Osseointegration in the irradiated patient, in Tolman D, Brånemark P-I (eds): Osseointegration in Craniofacial Reconstruction. Chicago, Quintessence, 1998, pp Granström G, Tjellström A, Albrektsson T: Postimplantation irradiation for head and neck cancer treatment. Int J Oral Maxillofac Implants 8:495, Esposito M, Hirsch J-M, Lekholm U, et al: Biological factors contributing to failures of osseointegrated oral implants. II: Etiopathogenesis. Eur J Oral Sci 106:721, Keller EE: Placement of dental implants in the irradiated mandible: A protocol without adjunctive hyperbaric oxygen. J Oral Maxillofac Surg 55:972, Keller EE, Tolman DE, Zuck SL, et al: Mandibular endosseous implants and autogenous bone grafting in irradiated tissue: A 10-year retrospective study. Int J Oral Maxillofac Implants 12: 800, Kirk I, Gray WH, Watson ER: Cumulative radiation effect. Clin Radiol 22:145, Granström G, Bergström K, Tjellström A, et al: A detailed analysis of titanium implants lost in irradiated tissues. Int J Oral Maxillofac Implants 9:653, Granström G, Tjellström A: Effects of irradiation on osseointegration before and after implant placement. A report of three cases. Int J Oral Maxillofac Implants 12:547, Marx R, Johnson RP: Studies on the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg Oral Med Oral Pathol 64:379, Wolfaardt J, Granström G, Friberg B, et al: A retrospective study of the effects of chemotherapy on osseointegration. J Fac Somat Prosth 2:99, Barber HD, Seckinger RJ, Hayden RE, et al: Evaluation of osseointegration of endosseous implants in radiated vascularised fibula flaps to the mandible. J Oral Maxillofac Surg 53:640, Schliephake H, Neukam F, Schmelzeisen R, et al: Long-term results of endosteal implants used for resaturation of oral function after oncologic surgery. Int J Oral Maxillofac Surg 28:260, Sclaroff A, Haughey B, Gay WD, et al: Immediate mandibular reconstruction and placement of dental implants at the time of ablative surgery. Oral Surg Oral Med Oral Pathol 78:711, Sennerby L, Roos J: Surgical determinants of clinical success of osseointegrated oral implants: A review of the literature. Int J Prosthodont 11:408, Niimi A, Fujimoto T, Nosaka Y, et al: A Japanese multicenter study of osseointegrated implants placed in irradiated tissues: A preliminary report. Int J Oral Maxillofac Implants 12:259, Weischer T, Schettler D, Mohe C: Concept of surgical and implant supported prostheses in rehabilitation of patients with oral cancer. Int J Oral Maxillofac Implants 11:775, Eckert SE, Desjardins RP, Keller EE, et al: Endosseous implants in an irradiated tissue bed. J Prosthet Dent 76:45, Jisander S, Grenthe B, Alberius P: Dental implant survival in the irradiated jaw: A preliminary report. Int J Oral Maxillofac Implants 12:643, August M, Bast B, Jackson M, et al: Use of the fixed mandibular implant in oral cancer patients. A retrospective study. J Oral Maxillofac Surg 56:297, Watzinger F, Ewers R, Henninger A, et al: Endosteal implants in the irradiated lower jaw. J Craniomaxillofac Surg 24:237, Fischer-Brandies E: Das Risiko enossaler Implantationen nach Radiatio. Quintessence 5:873, Wagner W, Esser E, Ostkamp K: Osseointegration of dental implants in patients with and without radiotherapy. Acta Oncol 37:693, Granström G: Pathophysiological basis for HBO in the treatment of healing disorders in radio-injured normal tissues, in Proceedings of the 5th ECHM Consensus Conference, Lisbon, 2001, pp Kindwall E, Gottlieb L, Larsson D: Hyperbaric oxygen therapy in plastic surgery. A review article. Plast Reconstr Surg 88:898, Granström G: The use of hyperbaric oxygen to prevent implant fixture loss in the irradiated patient, in Worthington P, Brånemark P-I (eds): Advanced Osseointegration Surgery. Chicago, Quintessence, 1992, pp Johnsson ÅA. On implant integration in irradiated bone. An experimental study of the effects of hyperbaric oxygenation and delayed implant placement. Thesis, University of Gothenburg, Sweden, Marx R, Ehler W, Tayapongsak P, et al: Relationship of oxygen dose to angiogenesis induction in irradiated tissue. Am J Surg 160:519, Støore G, Granström G: Osteoradionecrosis of the mandible. A microradiographic study of cortical bone. Scand J Plast Reconstr Hand Surg 33:307, Granström G: Hyperbaric oxygen as a stimulator of osseointegration. Adv Otorhinolaryngol 54:33, Johnsson Å A, Sawaii T, Jacobsson M, et al: A histomorphometric study of bone reactions to titanium implants in irradiated bone and the effect of hyperbaric oxygen treatment. Int J Oral Maxillofac Implants 14:699, Granström G: Radiotherapy, osseointegration and hyperbaric oxygen therapy. Periodontology :145, Johnsson K, Hansson Å, Granström G, et al: The effects of hyperbaric oxygenation on bone to titanium implant interface strength with or without prior irradiation. Int J Oral Maxillofac Implant 8:415, Coulthard P, Esposito M, Worthington HV, et al: Therapeutic use of hyperbaric oxygen for irradiated dental implant patients: A systematic review. J Dent Educ 67:64, Feldmeier JJ, Hampson NB: A systematic review of the literature reporting the application of hyperbaric oxygen prevention and treatment of delayed radiation injuries: An evidence based approach. Undersea Hyperb Med 29:4, Granström G, Tjellström A, Brånemark P-I: Osseointegrated implants in irradiated bone: A case-controlled study using adjunctive hyperbaric oxygen therapy. J Oral Maxillofac Surg 57:493, Larsen PE: Placement of dental implants in the irradiated mandible: A protocol involving adjunctive hyperbaric oxygen. J Oral Maxillofac Surg 55:967, Keller EE: Placement of dental implants in the irradiated mandible: A protocol without adjunctive hyperbaric oxygen. J Oral Maxillofac Surg 55:972, 1997
Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros.
 I M P L A N T S in IRRADIATED TISSUES Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros. Adj Associate Professor, National University of Singapore Chair,
I M P L A N T S in IRRADIATED TISSUES Dr Ansgar C Cheng BDS, MS, FRCDC, FRACDS, FAM(S), FCDSS, MRACDS, Cert. Pros., Cert. MaxFac. Pros. Adj Associate Professor, National University of Singapore Chair,
Australian Dental Journal
 Australian Dental Journal The official journal of the Australian Dental Association SCIENTIFIC ARTICLE Australian Dental Journal 2011; 56: 160 165 doi: 10.1111/j.1834-7819.2011.01318.x Oral rehabilitation
Australian Dental Journal The official journal of the Australian Dental Association SCIENTIFIC ARTICLE Australian Dental Journal 2011; 56: 160 165 doi: 10.1111/j.1834-7819.2011.01318.x Oral rehabilitation
Porous surface of extraoral implants: report of two cases rehabilitated with a new Brazilian extraoral implant
 Braz J Oral Sci. October/December 2004 - Vol. 3 - Number 11 Luciano Lauria Dib 1 Joaquim Augusto Piras de Oliveira 2 Renata Lazari Sandoval 3 Ulf Nannmark 4 1 Professor of Stomatology at UNIP, São Paulo,
Braz J Oral Sci. October/December 2004 - Vol. 3 - Number 11 Luciano Lauria Dib 1 Joaquim Augusto Piras de Oliveira 2 Renata Lazari Sandoval 3 Ulf Nannmark 4 1 Professor of Stomatology at UNIP, São Paulo,
Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants
 CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
CLINICAL CONTROVERSIES IN ORAL AND MAXILLOFACIAL SURGERY: PART ONE J Oral Maxillofac Surg 62:1418-1422, 2004 Restoration of the Edentulous Maxilla: The Case for the Zygomatic Implants Eric D. Ferrara,
Osseointegrated craniofacial implants in the rehabilitation of orbital defects: An update of a retrospective experience in the United States
 Osseointegrated craniofacial implants in the rehabilitation of orbital defects: An update of a retrospective experience in the United States Joseph A. Toljanic, DDS, a Steven E. Eckert, DDS, MS, b Eleni
Osseointegrated craniofacial implants in the rehabilitation of orbital defects: An update of a retrospective experience in the United States Joseph A. Toljanic, DDS, a Steven E. Eckert, DDS, MS, b Eleni
Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan
 Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
Journal of Data Science 6(2008), 591-599 Life Table Analysis for Evaluating Curative-effect of One-stage Non-submerged Dental Implant in Taiwan Miin-Jye Wen 1, Chuen-Chyi Tseng 2 and Cheng K. Lee 3 1 National
The Impact of Dental Implants on Maxillofacial Patient s Quality of Life
 46 The Open Pathology Journal, 2011, 5, 46-51 Open Access The Impact of Dental Implants on Maxillofacial Patient s Quality of Life Jorge Gonzalez * Center for Maxillofacial Prosthodontics, Baylor College
46 The Open Pathology Journal, 2011, 5, 46-51 Open Access The Impact of Dental Implants on Maxillofacial Patient s Quality of Life Jorge Gonzalez * Center for Maxillofacial Prosthodontics, Baylor College
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
Dental Implants in Edentulism
 Academy of Medicine, Singapore Dental Implants in Edentulism AMS-MOH Clinical Practice Guidelines 1/2012 Aug 2012 Levels of evidence and grades of recommendation Levels of evidence Level Type of Evidence
Academy of Medicine, Singapore Dental Implants in Edentulism AMS-MOH Clinical Practice Guidelines 1/2012 Aug 2012 Levels of evidence and grades of recommendation Levels of evidence Level Type of Evidence
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS?
 IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
IMPLANT CONSENT FORM WHAT ARE DENTAL IMPLANTS? Dental implants are a very successful and accepted treatment option to replace lost or missing teeth. A dental implant is essentially an artificial tooth
Ridge Reconstruction for Implant Placement
 Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Volume 1, No. 5 July/August 2009 The Journal of Implant & Advanced Clinical Dentistry Ridge Reconstruction for Implant Placement 2 Hours of CE Credit Oral Implications of Cancer Chemotherapy Immediate
Supervisors: Dr. Farhan Raza Khan
 1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
1 Presenter: Dr. Sana Ehsen Supervisors: Dr. Farhan Raza Khan 2 A dental implant (also known as an endosseous implant or fixture) is a surgical component that interfaces with the bone of the jaw to support
Osseo-integrated Dental Implant Policy and Guidelines
 Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
Osseo-integrated Dental Implant Policy and Guidelines 1. PURPOSE The purpose of this document is to outline the Department of Veterans Affairs (DVA) policy regarding the provision of dental implant treatment
ANGEL DENTAL CARE Implant Consent
 This information is to help you make an informed decision about having implant treatment. You should take as much time as you wish to make the decision in relation to signing the following consent form.
This information is to help you make an informed decision about having implant treatment. You should take as much time as you wish to make the decision in relation to signing the following consent form.
DENT IMPLANT restoring qualit S: of LIfE
 DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
DENTAL IMPLANTS: restoring quality of life Dental Implants: A Better Treatment Option. What are dental implants? Dental implants are a safe, esthetic alternative to traditional crowns, bridgework, and
UNMH Oral and Maxillofacial Surgery Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments
 Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
Clinical and Laboratory Procedures for Fixed Margin Implant Abutments Dr. Carl Drago DDS, MS, American Board of Prosthodontics Director, Dental Research BIOMET 3i, Adjunct Faculty Department of Prosthodontics,
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS
 LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
LATERAL BONE EXPANSION FOR IMMEDIATE PLACEMENT OF ENDOSSEOUS DENTAL IMPLANTS Department of Oral Maxillofacial Surgery, Chisinau Abstract: The study included 10 using the split control expansion technique
Prosthetic anchorage for the restoration of patients
 Remote implant anchorage for the rehabilitation of maxillary defects Stephen M. Parel, S, a Per-Ingvar rånemark, M, Ph, b Lars-Olof Ohrnell, S, c and arbro Svensson d aylor ollege of entistry, The Texas
Remote implant anchorage for the rehabilitation of maxillary defects Stephen M. Parel, S, a Per-Ingvar rånemark, M, Ph, b Lars-Olof Ohrnell, S, c and arbro Svensson d aylor ollege of entistry, The Texas
Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation
 2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
2009 New York University College Of Dentistry Linhart Continuing Dental Education Program Presents Current Concepts in American Dentistry: Advances in Implantology and Oral Rehabilitation International
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
A Comprehensive Explanation
 Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
Dental Implants A Comprehensive Explanation Overview Since the 1980s, dental implants have become more popular among dentists and patients. 1 In some clinical situations, implants may be the best treatment
Updated Clinical Considerations for Dental Implant Therapy in Irradiated Head and Neck Cancer Patients
 Updated Clinical Considerations for Dental Implant Therapy in Irradiated Head and Neck Cancer Patients Takako Imai Tanaka, DDS, FDS RCSEd, 1,2 Hsun-Liang Chan, DDS, MS, 2 David Ira Tindle, DDS, MS, 2 Mark
Updated Clinical Considerations for Dental Implant Therapy in Irradiated Head and Neck Cancer Patients Takako Imai Tanaka, DDS, FDS RCSEd, 1,2 Hsun-Liang Chan, DDS, MS, 2 David Ira Tindle, DDS, MS, 2 Mark
The Impact of Oral Implants Past and Future, 1966 2042. Tomas Albrektsson, MD, PhD, ODhc Ann Wennerberg, DDS, PhD
 P R O F E S S I O N A L I S S U E S The Impact of Oral Implants Past and Future, 1966 202 Tomas Albrektsson, MD, PhD, ODhc Ann Wennerberg, DDS, PhD A b s t r a c t This paper traces the history of oral
P R O F E S S I O N A L I S S U E S The Impact of Oral Implants Past and Future, 1966 202 Tomas Albrektsson, MD, PhD, ODhc Ann Wennerberg, DDS, PhD A b s t r a c t This paper traces the history of oral
Prosthetic treatment planning on the basis of scientific evidence.
 Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Prosthetic treatment planning on the basis of scientific evidence. Pjetursson BE, Lang NP. J Oral Rehabil. 2008 Jan;35 Suppl 1:72-9. Faculty of Odontology, University of Iceland, Reykjavik, Iceland, and
Tuition and Fees Dentists - Full time (per annum): 20,000
 Diploma of Oral Surgery Residency Training Program in preparation for the Fachzahnarzt in Oral Surgery Specialty Examination in the Republic of Germany Degree awarded: - Diploma of Oral Surgery - Fachzahnarzt
Diploma of Oral Surgery Residency Training Program in preparation for the Fachzahnarzt in Oral Surgery Specialty Examination in the Republic of Germany Degree awarded: - Diploma of Oral Surgery - Fachzahnarzt
A Study of 25 Zygomatic Dental Implants with 11 to 49 Months Follow-up After Loading
 A Study of 25 Zygomatic Dental Implants with 11 to 49 Months Follow-up After Loading Fredrik Ahlgren, DDS, MSc 1 / Kjell Størksen, DDS 2 /Knut Tornes, DDS, PhD 3 Purpose: The purpose of this study was
A Study of 25 Zygomatic Dental Implants with 11 to 49 Months Follow-up After Loading Fredrik Ahlgren, DDS, MSc 1 / Kjell Størksen, DDS 2 /Knut Tornes, DDS, PhD 3 Purpose: The purpose of this study was
Don t Let Life Pass You By Because Of Oral Bone Loss
 Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Don t Let Life Pass You By Because Of Oral Bone Loss Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader
Outcomes of Placing Short Dental Implants in the Posterior Mandible: A Retrospective Study of 124 Cases
 DENTAL IMPLANTS J Oral Maxillofac Surg 67:713-717, 2009 Outcomes of Placing Short Dental in the Posterior Mandible: A Retrospective Study of 124 Cases Bao-Thy N. Grant, DDS,* Franklin X. Pancko, DDS, and
DENTAL IMPLANTS J Oral Maxillofac Surg 67:713-717, 2009 Outcomes of Placing Short Dental in the Posterior Mandible: A Retrospective Study of 124 Cases Bao-Thy N. Grant, DDS,* Franklin X. Pancko, DDS, and
Don t Let Life Pass You By Because Of Missing Teeth
 Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
Don t Let Life Pass You By Because Of Missing Teeth Ask For Dental Implant Solutions From BIOMET 3i Scan With Your Smartphone! In order to scan QR codes, your mobile device must have a QR code reader installed.
 BISPHOSPHONATE RELATED OSTEONECROSIS OF THE JAW (BRONJ) BISPHOSPHONATES AND WHAT HAPPENS TO BONE VINCENT E. DIFABIO, DDS, MS MEMBER OF THE COMMITTEE ON HEALTHCARE AND ADVOCACY FROM THE AMERICAN ASSOCIATION
BISPHOSPHONATE RELATED OSTEONECROSIS OF THE JAW (BRONJ) BISPHOSPHONATES AND WHAT HAPPENS TO BONE VINCENT E. DIFABIO, DDS, MS MEMBER OF THE COMMITTEE ON HEALTHCARE AND ADVOCACY FROM THE AMERICAN ASSOCIATION
Case Report Mandibular Rehabilitation with Dental Implants: A case report
 Mandibular Rehabilitation with Dental Implants: A case report Yueh-Ling Chao, DDS School of Dentistry, National Taiwan University, Taipei, Taiwan Graduate student, Graduate Institute of Clinical Dentistry,
Mandibular Rehabilitation with Dental Implants: A case report Yueh-Ling Chao, DDS School of Dentistry, National Taiwan University, Taipei, Taiwan Graduate student, Graduate Institute of Clinical Dentistry,
Leslie Laing Gibbard, BSc, BEd, MSc, PhD, DDS George Zarb, BChD, DDS, MS, MS, FRCD(C)
 A P P L I E D R E S E A R C H A 5-Year Prospective Study of Implant-Supported Single-Tooth Replacements Leslie Laing Gibbard, BSc, BEd, MSc, PhD, DDS George Zarb, BChD, DDS, MS, MS, FRCD(C) A b s t r a
A P P L I E D R E S E A R C H A 5-Year Prospective Study of Implant-Supported Single-Tooth Replacements Leslie Laing Gibbard, BSc, BEd, MSc, PhD, DDS George Zarb, BChD, DDS, MS, MS, FRCD(C) A b s t r a
Straumann Bone Level Tapered Implant Peer-to-peer communication
 Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Straumann Bone Level Tapered Implant Peer-to-peer communication Clinical cases April, 2015 Clinical Cases Case No. Site 1 Single unit; Anterior Maxilla 2 Multi-unit; Anterior Maxilla Implant placement
Understanding Dental Implants
 Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
Understanding Dental Implants Comfort and Confidence Again A new smile It s no fun when you re missing teeth. You may not feel comfortable eating or speaking. You might even avoid smiling in public. Fortunately,
TRI Product NewsFlash. December 2015
 TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
TRI Product NewsFlash December 2015 Study Overview 2015 Dear Partners Year in, year out, we are screening all major scientific journals to ensure that our TRI Performance Concept still reflects the latest
What is a dental implant?
 What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
What is a dental implant? Today, the preferred method of tooth replacement is a dental implant. They replace missing tooth roots and form a stable foundation for replacement teeth that look, feel and function
The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review
 IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
IMPLANTS The Immediate Placement of Dental Implants Into Extraction Sites With Periapical Lesions: A Retrospective Chart Review Christopher Lincoln Bell,* David Diehl, Brian Michael Bell, and Robert E.
Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial.
 Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial. Karaky AE, Sawair FA, Al-Karadsheh OA, Eimar HA, Algarugly SA, Baqain ZH. Eur J Oral Implantol. 2011 Spring;4(1):31-8.
Antibiotic prophylaxis and early dental implant failure: a quasi-random controlled clinical trial. Karaky AE, Sawair FA, Al-Karadsheh OA, Eimar HA, Algarugly SA, Baqain ZH. Eur J Oral Implantol. 2011 Spring;4(1):31-8.
Updated: February 2014. 1986-1990 Highland General Hospital, Certificate of Completion Oral & Maxillofacial Surgery Residency
 Edmond Bedrossian DDS, FACD, FACOMS, FAO Diplomate, American Board of Oral & Maxillofacial Surgery Director, Implant Surgery, Alameda Medical Center & UOP School of Dentistry Professor, Department of Oral
Edmond Bedrossian DDS, FACD, FACOMS, FAO Diplomate, American Board of Oral & Maxillofacial Surgery Director, Implant Surgery, Alameda Medical Center & UOP School of Dentistry Professor, Department of Oral
What Dental Implants Can Do For You!
 What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
What Dental Implants Can Do For You! Putting Smiles into Motion About Implants 01. What if a Tooth is Lost and the Area is Left Untreated? 02. Do You Want to Restore Confidence in Your Appearance? 03.
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures
 Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
Improving Esthetics with Sequential Treatment Planning and Implant-Retained Dentures by Timothy F. Kosinski, DDS, MAGD While oral function is the primary concern for most patients, the importance of esthetics
SCD Case Study. Treatment Considerations for Implant Rehabilitation
 SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
SCD Case Study Treatment Considerations for Implant Rehabilitation Multiple surgical and restorative factors play a role in the treatment planning of implant restorations for the edentulous patient (Ali
Retrospective study on the survival rate of IBS implant
 Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
Retrospective study on the survival rate of IBS implant Date : 30. 05. 2013 Written by : Dr. Je Won Wang, Director of research Approved by : Prof. Min Seung Ki - Contents - 1. Purpose Of Study 2. Materials
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION
 MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
MINI IMPLANTS FOR LOWER DENTURE STABLIZATION From the Office of Dr. Michael J. Guy 511A Lakeshore Drive, North Bay ON, P1A 2E3 Mini dental implants (MDI) have become increasingly popular in the past decade
Learning about Mouth Cancer
 Learning about Mouth Cancer Creation of this material was made possible in part by a pioneering grant from CBCC-USA. Distributed by India Cancer Initiative What is mouth cancer? Our bodies are made up
Learning about Mouth Cancer Creation of this material was made possible in part by a pioneering grant from CBCC-USA. Distributed by India Cancer Initiative What is mouth cancer? Our bodies are made up
An adequate amount of bone, in
 CASE REPORT Immediate Loading of Dental Implant After Sinus Floor Elevation With Osteotome Technique: A Clinical Report and Preliminary Radiographic Results Mario Santagata, MD* Luigi Guariniello, MD,
CASE REPORT Immediate Loading of Dental Implant After Sinus Floor Elevation With Osteotome Technique: A Clinical Report and Preliminary Radiographic Results Mario Santagata, MD* Luigi Guariniello, MD,
Modern Tooth Replacement Strategies & Digital Workflow
 Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Modern Tooth Replacement Strategies & Digital Workflow Case Studies by Dr Maurice Salama, DMD AS PUBLISHED BY Dentistry Today, June 2014 Complete Implant Restoration System FACTS: Implant Dentistry Has
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Dental care and treatment for patients with head and neck cancer. Department of Restorative Dentistry Information for patients
 Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Dental care and treatment for patients with head and neck cancer Department of Restorative Dentistry Information for patients i Why have I been referred to the Restorative Dentistry Team? Treatment of
Regions Hospital Delineation of Privileges Oral & Maxillofacial Surgery
 Regions Hospital Delineation of Privileges al & Maxillofacial Surgery Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education
Regions Hospital Delineation of Privileges al & Maxillofacial Surgery Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education
TRAINING STANDARDS IN IMPLANT DENTISTRY
 TRAINING STANDARDS IN IMPLANT DENTISTRY Introduction 2012 1 Dental implants are used to replace one or more missing teeth. Their insertion involves various surgical and restorative dental procedures and
TRAINING STANDARDS IN IMPLANT DENTISTRY Introduction 2012 1 Dental implants are used to replace one or more missing teeth. Their insertion involves various surgical and restorative dental procedures and
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
Tooth Replacement Options
 Dr. Jordan Johnson Johnson Dental Associates http://www.beta.mydentalhub.com/ada/test/ (800) 947-4746 Tooth Replacement Options If you re missing one or more teeth, you may be all too aware of their importance
Dr. Jordan Johnson Johnson Dental Associates http://www.beta.mydentalhub.com/ada/test/ (800) 947-4746 Tooth Replacement Options If you re missing one or more teeth, you may be all too aware of their importance
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012
 PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
PATIENT INFORM CONSENT for IMPLANT RESTORATION Rev 04.2012 Implant placement and restoration involves two major stages: surgical placement of the implant(s) followed by the restoration of the implant after
Dental Bone Grafting Options. A review of bone grafting options for patients needing more bone to place dental implants
 Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Dental Bone Grafting Options A review of bone grafting options for patients needing more bone to place dental implants Dental Bone Grafting Options What is bone grafting? Bone grafting options Bone from
Saudi Fellowship In Dental Implant (SF-DI)
 Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Saudi Fellowship In Dental Implant (SF-DI) Prepared and Updated by Dr. Arwa AL-Sayed Consultant Periodontics and Dental Implants M E M B E R S Dr. Arwa AL-Sayed Dr. Abdulhadi Abanmy Dr. Ali AL-Ghamdi Dr.
Clinical study of a spacer to help prevent osteoradionecrosis resulting from brachytherapy for tongue cancer
 Clinical study of a spacer to help prevent osteoradionecrosis resulting from brachytherapy for tongue cancer Kenichi Obinata, DDS, PhD, a Keiichi Ohmori, DDS, PhD, b Kazuhiko Tuchiya, MD, c Takeshi Nishioka,
Clinical study of a spacer to help prevent osteoradionecrosis resulting from brachytherapy for tongue cancer Kenichi Obinata, DDS, PhD, a Keiichi Ohmori, DDS, PhD, b Kazuhiko Tuchiya, MD, c Takeshi Nishioka,
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
Like natural teeth. Treatment with dental implants is a safe, reliable and well-proven solution for permanently replacing one or more missing teeth.
 Implants for life 2 IMPLANTS FOR LIFE Like natural teeth Treatment with dental implants is a safe, reliable and well-proven solution for permanently replacing one or more missing teeth. Millions of people
Implants for life 2 IMPLANTS FOR LIFE Like natural teeth Treatment with dental implants is a safe, reliable and well-proven solution for permanently replacing one or more missing teeth. Millions of people
Restoring quality to life. Dental implants. A naturally better solution. Patient Education
 Restoring quality to life. Dental implants. A naturally better solution. Patient Education Dental implants: A better treatment option. What are dental implants? Dental implants are a safe, medically proven,
Restoring quality to life. Dental implants. A naturally better solution. Patient Education Dental implants: A better treatment option. What are dental implants? Dental implants are a safe, medically proven,
Eastman Dental Hospital. Dental implants - general information for patients. Department of Restorative Dentistry
 Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
Eastman Dental Hospital Dental implants - general information for patients Department of Restorative Dentistry First published: January 2004 Last review date: March 2014 Next review date: March 2016 Leafl
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have increasingly high
The rate of success of implants in the edentulous
 Clinical evaluation of single-tooth mini-implant restorations: A five-year retrospective study Paolo Vigolo, Dr Odont, MScD, and Andrea Givani, MD, DDS Vicenza, Italy Statement of problem. Placement of
Clinical evaluation of single-tooth mini-implant restorations: A five-year retrospective study Paolo Vigolo, Dr Odont, MScD, and Andrea Givani, MD, DDS Vicenza, Italy Statement of problem. Placement of
Teeth in a Day for the Maxilla and Mandible: Case Report
 Teeth in a Day for the Maxilla and Mandible: Case Report Thomas J. Balshi, DDS, FACP* Glenn J. Wolfinger, DMD, FACP** Abstract Background: A growing body of evidence indicates that successful osseointegration
Teeth in a Day for the Maxilla and Mandible: Case Report Thomas J. Balshi, DDS, FACP* Glenn J. Wolfinger, DMD, FACP** Abstract Background: A growing body of evidence indicates that successful osseointegration
Spedding Dental Clinic. 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk
 DENTAL IMPLANTS Spedding Dental Clinic 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk SPEDDING DENTAL CLINIC Jack Spedding is a partner in Spedding dental clinic. He is a highly
DENTAL IMPLANTS Spedding Dental Clinic 73 Warwick Road Carlisle CA1 1EB T: 01228 521889 www.speddingdental.co.uk SPEDDING DENTAL CLINIC Jack Spedding is a partner in Spedding dental clinic. He is a highly
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Implant therapy using osseointegrated implants has
 Natural Tooth Intrusion Phenomenon With Implants: A Survey Lily T. Garcia, DDS, MS*/Larry J. Oesterle, DDS, MS** A common assumption when planning for treatment for a fixed partial denture potentially
Natural Tooth Intrusion Phenomenon With Implants: A Survey Lily T. Garcia, DDS, MS*/Larry J. Oesterle, DDS, MS** A common assumption when planning for treatment for a fixed partial denture potentially
Dental Implants. Change Your Life & Smile with. Kingston Kitchener Newmarket Oshawa Scarborough Toronto Waterloo
 Change Your Life & Smile with Dental Implants Page 1 Dental Implants 101 3 What To Expect 5 Fees & Financing 6 FAQ Aurora Barrie Brooklin Cambridge Hanover Guelph Kingston Kitchener Newmarket Oshawa Scarborough
Change Your Life & Smile with Dental Implants Page 1 Dental Implants 101 3 What To Expect 5 Fees & Financing 6 FAQ Aurora Barrie Brooklin Cambridge Hanover Guelph Kingston Kitchener Newmarket Oshawa Scarborough
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
DENTAL IMPLANT THERAPY
 DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
DENTAL IMPLANT THERAPY PATIENT WELCOME PACK Dr. Syed Abdullah BDS, MSc (Dental Implants) What are dental implants? In the early 1950s, a Swedish Scientist, Per-Ingvar Branemark observed that titanium metal
Amajor limitation in the use of most
 Volume 75 Number 6 A Targeted Review of Study Outcomes With Short ( 7 mm) Endosseous Dental Implants Placed in Partially Edentulous Patients D. Hagi,* D.A. Deporter,* R.M. Pilliar,* and T. Arenovich Background:
Volume 75 Number 6 A Targeted Review of Study Outcomes With Short ( 7 mm) Endosseous Dental Implants Placed in Partially Edentulous Patients D. Hagi,* D.A. Deporter,* R.M. Pilliar,* and T. Arenovich Background:
INFUSE Bone Graft (rhbmp-2/acs)
 1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic axilla with Cross-Arch ixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic axilla with Cross-Arch ixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Table of Contents. Data Supplement 1: Summary of ASTRO Guideline Statements. Data Supplement 2: Definition of Terms
 Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
Definitive and Adjuvant Radiotherapy in Locally Advanced Non-Small-Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Endorsement of the American Society for Radiation
BICON DENTAL IMPLANTS
 BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
BICON DENTAL IMPLANTS The Bicon Dental Implant System, since 1985, has offered discerning dentists the ability to provide secure implant restorations that look, feel, and function like natural teeth. With
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment
 Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
Replacement of the upper left central incisor with a Straumann Bone Level Implant and a Straumann Customized Ceramic Abutment by Dr. Ronald Jung and Master Dental Technician Xavier Zahno Initial situation
All-on-4 treatment concept with NobelSpeedy Groovy
 All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
All-on-4 treatment concept with NobelSpeedy Groovy Product overview Immediate Function for high patient satisfaction Immediately loaded fixed provisional prosthesis on the day of surgery. Immediate improvement
Appropriate soft tissue closure represents a critical
 Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
Periosteoplasty for Soft Tissue Closure and Augmentation in Preprosthetic Surgery: A Surgical Report Albino Triaca, Dr Med, Dr Med Dent 1 /Roger Minoretti, Dr Med, Dr Med Dent 1 / Mauro Merli, DMD 2 /Beat
A New Beginning with Dental Implants. A Guide to Understanding Your Treatment Options
 A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
A New Beginning with Dental Implants A Guide to Understanding Your Treatment Options Why Should I Replace My Missing Teeth? Usually, when you lose a tooth, it is best for your oral health to have it replaced.
Adramatic increase in the number of dental practitioners
 Risk Management Aspects of Implant Dentistry Navot Givol, DMD 1 /Shlomo Taicher, DMD 2 /Talia Halamish-Shani, LLB 3 /Gavriel Chaushu, DMD, MSc 4 Purpose: To categorize and review complications related
Risk Management Aspects of Implant Dentistry Navot Givol, DMD 1 /Shlomo Taicher, DMD 2 /Talia Halamish-Shani, LLB 3 /Gavriel Chaushu, DMD, MSc 4 Purpose: To categorize and review complications related
2016 Buy Up Dental Care Plan Procedure List
 * This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
* This is in addition to the embedded Preventive Plan (see procedure list at deltadentalco.com/kp_preventive. BASIC SERVICES Minor Restorative Services D2140 Amalgam 1 surface, primary or permanent D2150
Sharjah University in collaboration with
 Sharjah University in collaboration with And Alexandria Oral Implantology Association AOIA Is delighted to invite you to the Comprehensive dental implantology course It is an academic implantology course
Sharjah University in collaboration with And Alexandria Oral Implantology Association AOIA Is delighted to invite you to the Comprehensive dental implantology course It is an academic implantology course
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS
 RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
RESIDENT TRAINING GOALS AND OBJECTIVES STATEMENTS Evaluation and treatment of dental emergencies Recognize, anticipate and manage emergency problems related to the oral cavity. Differentiate between those
Taking the Mystique out of Implant Dentistry. Dr. Michael Weinberg B.Sc., DDS, FICOI
 Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
Taking the Mystique out of Implant Dentistry Dr. Michael Weinberg B.Sc., DDS, FICOI What is Restorative Implant Dentistry? Restorative implant dentistry involves taking a few simple mechanical principles
05 - DENTAL SURGERY. (02) MS (Oral Surgery) Part II Examination
 05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment
 Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Number 3 $1.25 The Most Frequently Asked Questions About Dental Implants... A Consumer s Guide to Understanding Implant Treatment If you are like most people considering dental implants, you probably have
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Your Questions Answered. Regain Your Smile, Change Your Life with DENTAL IMPLANTS! IMPLANT DENTISTRY
 Your Questions Answered Regain Your Smile, Change Your Life with DENTAL IMPLANTS! IMPLANT DENTISTRY PERRY V. GOLDBERG, DDS, MSD WOODHILL MEDICAL PARK 8305 WALNUT HILL LANE, SUITE 125 DALLAS, TEXAS 75231
Your Questions Answered Regain Your Smile, Change Your Life with DENTAL IMPLANTS! IMPLANT DENTISTRY PERRY V. GOLDBERG, DDS, MSD WOODHILL MEDICAL PARK 8305 WALNUT HILL LANE, SUITE 125 DALLAS, TEXAS 75231
Oftentimes, as implant surgeons, we are
 CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
CLINICAL AVOIDING INJURY TO THE INFERIOR ALVEOLAR NERVE BY ROUTINE USE OF INTRAOPERATIVE RADIOGRAPHS DURING IMPLANT PLACEMENT Jeffrey Burstein, DDS, MD; Chris Mastin, DMD; Bach Le, DDS, MD Injury to the
Retention of maxillary implant overdenture bars of different designs
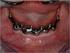 Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
Retention of maxillary implant overdenture bars of different designs Brian H. Williams, DDS, a Kent T. Ochiai, DDS, b Satoru Hojo, DDS, PhD, c Russell Nishimura, DDS, d and Angelo A. Caputo, PhD e School
(970) 663-6878 WWW. REYNOLDSORALFACIAL. COM
 (970) 663-6878 WWW. REYNOLDSORALFACIAL. COM Glossary Anterior-Posterior - Front-back Class I - Normal relationship of teeth Class II - Distal (posterior) relationship of mandibular teeth to maxillary teeth.
(970) 663-6878 WWW. REYNOLDSORALFACIAL. COM Glossary Anterior-Posterior - Front-back Class I - Normal relationship of teeth Class II - Distal (posterior) relationship of mandibular teeth to maxillary teeth.
ORTHODONTIC TREATMENT
 ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
Position Classification Standard for Dental Officer Series, GS-0680
 Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
education Although demographic factors and growing patient awareness of the benefits of dental implants
 education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
education Increasing implant dentistry in undergraduate education using new technology: A pilot project Hugo De Bruyn, MDS, MsC, PhD ± & Stefan Vandeweghe, DDS Although demographic factors and growing
DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI
 Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Good Morning DENTAL IMPLANTS DR JEBIN,MDS.,D.ICOI What is implant? A dental implant is an artificial root that replaces the natural tooth root. Crown Gum Implant Tooth Root Jawbone Parts of implant Cover
Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up
 Article 1 Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up Dr. Gadi Schneider DMD, Specialist in periodontics Dr. Yoram Bruckmayer DMD Long-Term dental Implant Survival
Article 1 Long-Term dental Implant Survival In Fully Endentulous Patients: A 30-66 Month Follow-Up Dr. Gadi Schneider DMD, Specialist in periodontics Dr. Yoram Bruckmayer DMD Long-Term dental Implant Survival
NAPCS Product List for NAICS 62121 (US, Mex): Offices of Dentists
 NAPCS List for NAICS 62121 (US, Mex): Offices of Dentists 62121 1 Services of dentists Providing dental medical attention by means of consultations, preventive services, and surgical and non-surgical interventions.
NAPCS List for NAICS 62121 (US, Mex): Offices of Dentists 62121 1 Services of dentists Providing dental medical attention by means of consultations, preventive services, and surgical and non-surgical interventions.
Dental Implants - the tooth replacement solution
 Dental Implants - the tooth replacement solution Are missing teeth causing you to miss out on life? Missing teeth and loose dentures make too many people sit on the sidelines and let life pass them by.
Dental Implants - the tooth replacement solution Are missing teeth causing you to miss out on life? Missing teeth and loose dentures make too many people sit on the sidelines and let life pass them by.
Ideal treatment of the impaired
 RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
RESEARCH IMPLANTS AS ANCHORAGE IN ORTHODONTICS: ACLINICAL CASE REPORT Dale B. Herrero, DDS KEY WORDS External anchorage Pneumatized Often, in dental reconstruction, orthodontics is required for either
