EGFR-Targeted Therapy for Non-Small Cell Lung Cancer: Focus on EGFR Oncogenic Mutation
|
|
|
- Estella Preston
- 8 years ago
- Views:
Transcription
1 320 Review Ivyspring International Publisher International Journal of Medical Sciences 2013; 10(3): doi: /ijms.4609 EGFR-Targeted Therapy for Non-Small Cell Lung Cancer: Focus on EGFR Oncogenic Mutation Alberto Antonicelli 1,5, Stefano Cafarotti 2, Alice Indini 3, Alessio Galli 4, Andrea Russo 6, Alfredo Cesario 7, Filippo Maria Lococo 8, Patrizia Russo 9, Alberto Franco Mainini 5, Luca Giuseppe Bonifati 5, Mario Nosotti 1, Luigi Santambrogio 1, Stefano Margaritora 8,10, Pierluigi Maria Granone 8 and Andre Emanuel Dutly 2 1. Thoracic Surgery and Lung Transplantation Unit, Foundation IRCCS (Scientific Institute for Research Hospitalization and Health Care) Ca Granda General Hospital, University of Milan, Milan, Italy. 2. Thoracic Surgery EOC Unit San Giovanni Hospital, Bellinzona, Switzerland. 3. Pediatric Oncology Unit, Foundation IRCCS National Cancer Institute (NCI), Milan, Italy. 4. Department of Preclinical Science LITA Vialba, Luigi Sacco Hospital, University of Milan, Milan, Italy. 5. General Thoracic Surgery Unit, Saronno Regional Hospital, Saronno, Italy. 6. Institute of Anestesiology and Intensive Care Medicine, Catholic University of Sacred Heart, Rome, Italy. 7. Deputy Scientific Director, IRCCS San Raffaele Group, Rome, Italy. 8. Division of Thoracic Surgery, Catholic University of Sacred Heart, Rome, Italy. 9. Laboratory of Systems Approaches and Non Communicable Diseases, IRCCS San Raffaele Pisana, Rome, Italy. 10. CFO Florence Cancer Center, Sesto Fiorentino, Italy. Corresponding author: Cafarotti Stefano, MD. Thoracic Surgery EOC Unit San Giovanni Hospital, Bellinzona, Switzerland. cafarottistefano@gmail.com. Tel / 0041 (0) Fax Ivyspring International Publisher. This is an open-access article distributed under the terms of the Creative Commons License ( licenses/by-nc-nd/3.0/). Reproduction is permitted for personal, noncommercial use, provided that the article is in whole, unmodified, and properly cited. Received: ; Accepted: ; Published: Abstract The two essential requirements for pathologic specimens in the era of personalized therapies for non-small cell lung carcinoma (NSCLC) are accurate subtyping as adenocarcinoma (ADC) versus squamous cell carcinoma (SqCC) and suitability for EGFR molecular testing, as well as for testing of other oncogenes such as EML4-ALK and KRAS. Actually, the value of EGFR expressed in patients with NSCLC in predicting a benefit in terms of survival from treatment with an epidermal growth factor receptor targeted therapy is still in debate, while there is a convincing evidence on the predictive role of the EGFR mutational status with regard to the response to tyrosine kinase inhibitors (TKIs). This is a literature overview on the state-of-the-art of EGFR oncogenic mutation in NSCLC. It is designed to highlight the preclinical rationale driving the molecular footprint assessment, the progressive development of a specific pharmacological treatment and the best method to identify those NSCLC who would most likely benefit from treatment with EGFR-targeted therapy. This is supported by the belief that a rationale for the prioritization of specific regimens based on patient-tailored therapy could be closer than commonly expected. Key words: EGFR targeted therapy, NSCLC, advanced, mutation, TKIs, resistance. Introduction Alterations in receptor tyrosine kinases (RTKs) including over expression, amplification or mutation have shown to play a key role in the pathogenesis of lung cancer 1. In recent years, attention has been paid to the role that driver mutations have in tumorigenesis, in order to use them as potential targets for therapy. Such driver mutations include those of the epidermal growth factor receptor (EGFR) and of the anaplastic lymphoma kinase (ALK) 2,3. The EGFR family of TKs, referred to as the HER or ErbB family, consists of four members EGFR (HER1/ErbB1), HER2 (ErbB2), HER3 (ErbB3) and
2 321 HER4 (ErbB4). These members regulate many physiological processes and are involved in the modulation of cell proliferation, apoptosis, cell motility and neovascularisation, thus being able to induce important mechanisms related to cancerogenesis 4,5. The EGFR tyrosine kinase works through the auto-activation of the receptor via its homo/heterodimerization and autophosphorylation on tyrosine-rich cytosolic domains after the binding of the ligand. This leads to the beginning of two main downstream intermediate pathways: the PIK3CA/AKT1/MTOR pathway and the RAS/RAF1/MAP2K1/MAPK1 kinases 6. There is evidence that the activated EGFR can also mediate signals through the STAT transcription factors 7,8. Improper activation and over-expression of EGFR-TK results in increased cell proliferation, survival, invasion and metastasis. This has been implicated in the pathogenesis and progression of many malignancies as well as in the poor prognosis of patients 7,9-10. In malignant cells, including NSCLC cells, the activity of the receptor may become dysregulated and no longer under the control of inherent inhibitory mechanisms 11. Spontaneous EGFR mutations often are oncogenic; that is, they activate the EGFR-signalling pathway in the absence of ligand and promote cell proliferation, survival and anti-apoptotic signals. These signalling networks make EGFR-mutated cells dependent on a functional EGFR for their survival, rendering them addicted to the receptor. Inhibition of EGFR leads to up-regulation of pro-apoptotic molecules and finally results in cell death through the activation of the intrinsic mitochondrial apoptotic pathway 12,13. There are several described mutations in the EGFR gene. The two most common are: 1) short in-frame deletions around the LREA motif of exon 19 (~45-50% of mutations); and 2) a point mutation (CTG to CGG) in exon 21 that results in substitution of leucine by arginine at codon 858, L858R (~45-50% of mutations) 14,15. These mutations are more frequently found in NSCLC with an adenocarcinoma histology, tumors in women, East Asians and never smokers EGFR mutations in lung cancers constitute one of the major subsets among those molecular aberrations occurring in lung cancers. The incidence of EGFR mutations in tumors with non-small-cell histology ranges from ~15% in Caucasians to ~50% in East Asians 17 ; 95% of such mutations have been found in adenocarcinomas 18. Patients bearing EGFR mutations have shown favourable clinical outcomes even with conventional chemotherapy suggesting that EGFR may serve as a predictive factor as well as a prognostic factor 19. Over 50% of patients diagnosed with NSCLC present with stage IIIB or IV disease is not amenable to curative treatment 20 and the only pathologic material guiding systemic therapy may be small biopsy and cytology specimens. Until the recent use of TKIs, the standard first-line treatment for most patients with unresectable NSCLC and good performance status has involved the use of a combination of chemotherapy regimens (usually cisplatin-based), which from the 1970s and 1980s were shown to reproducibly achieve objective response in 20% to 30% of advanced NSCLC patients. The most common combination regimens in use at present are gemcitabine with either cisplatin or carboplatin, followed by paclitaxel-carboplatin, vinorelbine-platinum and docetaxel-platinum combinations 21,22. The addition of the recombinant humanized monoclonal antibody bevacizumab that binds to vascular endothelial growth factor (VEGF) to carboplatin and paclitaxel for the treatment of non-squamous advanced NSCLC has demonstrated to increase RR, PFS and OS when compared to chemotherapy alone 23. Disease progression affects almost all patients after initial treatment and requires additional therapy. The agents approved for second-line therapy in advanced NSCLC are docetaxel 24, pemetrexed 25 and erlotinib 26. When tested in randomized trials 24-26, these agents have demonstrated a PFS below 2-3 months with a median overall survival no longer than 9 months in very few unselected patients. Despite recent advances with approval of more active chemotherapeutic and anti-angiogenesis agents for stage IV NSCLC, standard therapy can provide only modest clinical benefits with significant toxicities when used in unselected patients. In 2004, the identification of somatic mutations in the EGFR gene provided the first glimpse of a possible target for a treatment 27,28 which could maximize clinical outcome in those patients who could benefit from a personalized therapy 29. This implies the identification of certain characteristic molecular lesions meant to be causally responsible for maintenance of the malignant phenotype and also distinctive of the cancer cells. Therapies targeted to these molecular lesions offer the prospect for tumor control and selectivity with less toxicity than traditional chemotherapy. This review is designed to shed light on the rationale supporting the preclinical molecular footprint assessment, on the progressive development of specific pharmacological treatments and on the best method to identify those NSCLCs which would most likely benefit from treatment with EGFR-targeted therapy.
3 322 Rationale of EGFR assessment in Non Small Cell Lung Cancer Somatic mutations in the EGFR gene which account for oncogenesis in NSCLCs are activating mutations that work through a gain of function mechanism (i.e. the ligand-independency of the tyrosine kinase s signalling activity). These types of mutations can be found in 10 to 20% of patients with a NSCLC at an advanced stage and in more than 50% of adenocarcinomas and tumours from East Asians, never smokers and women 30. The described mutations generally interest the exons of the EGFR gene between the 19 th and the 21 th, which correspond to the portion of the receptor with kinase activity, nearby the binding site of ATP (that is fundamental to the activation of the receptor by autophosphorylation). As a result, the receptor is blocked into a state of constitutive activation, signalling to the cell to proliferate and to resist apoptosis. The two most frequent genic mutations responsible for this anomaly in cell cycle are the substitution of arginine for leucine at codon 858 (L858R), exon 21, and in-frame deletions at exon 19 (del E746_A750 is the most common). L858R accounts for 45-50% of mutations while deletions at exon 19 account for another 45-50%. Other rarer mutations (5%) associated with EGFR constitutive activation are insertions in exon 20 and substitutions at the glycine residue at codon 719 in exon 18 (as the G719S mutation). Molecular studies on the receptors harbouring a known L858R mutation demonstrated a decreased affinity of the tyrosine kinase for ATP and an increase in the affinity for the tyrosine kinase inhibitors (TKI). These are drugs studied to specifically target the pathways of oncogenesis mediated by the EGFR hyper-activation and causing little harm to non-tumoral cells 30. There is evidence supporting a different sensitivity of NSCLCs to the TKI gefitinib depending on the presence of an exon 21 mutation or an exon 19 deletion, having deletions at exon 19 been associated with a better response 31. Furthermore, in about 30-75% of samples from NSCLCs, an EGFR over-expression 30 due to epigenetic causes (transcriptional hyper-activation), gene amplification or oncogenic viruses can be detected 7. EGFR over-expression and the consequent augmentation of cell survival and proliferation has also been observed in premalignant lesions, showing the importance of this membrane-associated receptor in tumor growth 7. NSCLCs that over-express both EGFR and HER2 (another member of the HER family) demonstrated an aggressive tumor cell growth. In effect, EGFR/HER2 heterodimers display a greater activity than EGFR homodimers 7. Some studies demonstrated that the EGFR gene amplification, and thus over-expression directly correlates with a better response to tyrosine kinase inhibitors, and NSCLCs that over-express both EGFR and HER2 are more sensitive to this class of drugs than a tumor with an increased expression of EGFR alone. In this perspective, pre-treatment assessment of EGFR and HER2 gene copy number may have a prognostic and a predictive value of response to TKIs in NSCLCs 7,32, but there are no univocal opinions with regard to this topic. However, data from the recent phase 3 FLEX study on patients with advanced NSCLC underpin pre-treatment assessment of EGFR expression by IHC, for EGFR over-expression on the surface of tumoral cells proved to be predictive of better overall survival with a combined treatment of first-line chemotherapy (comprising cisplatin and vinorelbine) plus cetuximab (an anti-egfr monoclonal antibody) relative to chemotherapy alone. Among patients with a high EGFR expression, those who were in the combined treatment group had a median OS of 12 months versus the 9.6 months of patients allocated to the chemotherapy alone arm 33. Which strategy is better in the management of advanced NSCLCs, if the inhibition of mutated EGFR with TKIs or a combined approach with cetuximab plus first-line chemotherapy, is yet to be determined. The combination of cetuximab and a tyrosine kinase inhibitor in the treatment of those tumors which are resistant to TKIs alone is intriguing 34,35, but to date clinical data are still lacking. EGFR expression seen in advanced lung cancers made this an attractive target for molecular intervention in this disease. Several studies (Table 1) have by now demonstrated dramatic improvement in response rates, quality of life, symptoms, and median progression-free-survival (by 2-5 months) with first-line EGFR-TKI therapy compared with standard platinum-doublet chemotherapy in patients with EGFR mutation-positive NSCLC 36,37. Gefitinib and erlotinib were the first two agents to target the tyrosine kinase domain of the EGFR. Both these agents showed encouraging activity in patients with NSCLC who had been previously treated with chemotherapy in the phase I series and then in phase II trials 36,37. This has led to their approval of the treatment in advanced NSCLC. The first two large phase III trials comparing EGFR TKIs in patients previously treated with a different first line therapy were BR and INTEREST 39 trials. BR21 was an international phase III randomized trial comparing erlotinib with placebo in patients who had failed at least one line of cytotoxic chemotherapy. With the survival benefit shown in this trial, erlotinib has been approved for use as second or third-line therapy in NSCLC after failure with a cytotoxic
4 323 chemotherapy regimen by American and European regulatory agencies 38. A randomised, open-label phase III trial (INTEREST) 39 of gefitinib versus docetaxel in previously treated patients established non-inferior survival in patients treated with TKIs compared with chemotherapy, thus suggesting that gefitinib is a valid treatment for pre-treated patients with non-small-cell lung cancer 39. In contrast to the significant clinical and radiological responses seen in patients harbouring EGFR activating mutations, gefitinib and erlotinib have shown only limited activity in non-egfr genotyped, or unselected, NSCLCs when given as first, second or subsequent lines of therapy. 37,40. This has been reported by several prospective trials of gefitinib and erlotinib in EGFR-mutated NSCLC, which showed RRs exceeding 70% in tumors with exon 19 deletions or the L858R mutation, with PFS intervals of 6-14 months and OS times beyond months During the last three years, the predictive value of EGFR mutations for use of gefitinib has been strengthened by the results of three randomized phase III trials that specifically compared TKIs used as first-line therapy with traditional platinum-based chemotherapy in patients with advanced NSCLC. In 2009 the results of IRESSA Pan-Asia Study 36,44 were presented. This trial included 1217 patients of Asian ethnicity who were never smokers or former light smokers yet had histologic diagnosis of adenocarcinoma. The trial demonstrated an improvement in PFS and RR (with no statistical difference in OS) with the use of gefitinib in EGFR-mutated tumors and, in contrast, better RR and PFS with standard chemotherapy in patients without mutations. The first phase III trial of gefitinib versus chemotherapy as initial treatment of recurrent or advanced NSCLC, based on selection of patients with known activating EGFR mutations was the WJTOG3405 trial, reported in This trial documented important achievements in terms of RR and PFS with the use of TKIs. During the same year, such results were confirmed by another similar Japanese phase III trial, NEJ002 37, with RR and PFS definitely favouring the use of gefitinib in the first-line setting of metastatic EGFR-mutated NSCLC. Table 1. Summary of first-line efficacy data of TKIs in patients with EGFR-mutated advanced NSCLC (results from randomized phase III trials of gefitinib/erlotinib versus standard chemotherapy). Trial patient selection treatment/number of patients ORR (%) PFS (months) OS (months) IPASS Asia Carboplatin-Paclitaxel (Mok et al. 2009) never- or light (n=608 total; n=129 EGFR M+) ex-smoker Gefitinib adenocarcinoma (n=609 total; n=132 EGFR M+) p < HR 0.48; p<0.001 HR 1.00; p 0.99 WJTOG 3405 Asia Cisplatin-Docetaxel not reached (Mitsudomi et al. 2010) EGFR mutation (n=86 EGFR M+) Gefitinib (n=86 EGFR M+) p< HR 0.49; p< HR 1.64; p NEJ 002 Asia Carboplatin-Paclitaxel (Maemondo et al. 2010) EGFR mutation (n=100 EGFR M+) Gefitinib (n=98 EGFR M+) p< HR 0.30; p<0.001 HR NR; p 0.31 OPTIMAL Asia Carboplatin-Gemcitabine NA (Zhou et al. 2011) EGFR mutation (n=72 EGFR M+) Erlotinib NA (n=83 EGFR M+) p< HR 0.16; p< NA EURTAC Europe Platinum-Gemcitabine/Docetaxel (Rossell et al. 2012) EGFR mutation (n=87 EGFR M+) Erlotinib (n=86 EGFR M+) OR 7.5; p< HR 0.37; p< HR 1.047; p 0.87 EGFR: epidermal growth factor receptor; ORR: objective response rate; PFS: progression-free survival; OS: overall survival; HR: hazard ratio; OR: odds ratio; NA: not available, NR: not reported. Numerous small studies (mainly conducted in East-Asia) on EGFR-TKI monotherapy with gefitinib rapidly confirmed high objective response rate with this agent used in first-line setting in patients with cancers harbouring a mutation 42,43, Based on the results of the IPASS study, gefitinib was approved for use in Europe for the initial treatment of patients with NSCLC exhibiting EGFR mutations. Confirmatory randomized phase III trials of erlotinib versus standard chemotherapy have recently been concluded in Asia (OPTIMAL trial, NCT ) and Europe (EURTAC trial, NCT ). The positive results
5 324 of these studies suggested that responsiveness in mutation-positive patients was not a function of ethnicity. Furthermore, Caucasian patients demonstrated a spectrum of EGFR mutational subtypes similar to those seen in East Asian patients. Gefitinib and erlotinib have shown a similar spectrum of activity, with little differences in pharmacokinetics determining a major bioavailability for erlotinib 52. This is the only TKI which has been approved by FDA for the management of treatment-naive patients with advanced NSCLC showing EGFR activating mutations 53. EGFR-TKIs as a class are generally well tolerated. The two most common toxicities include dermatologic and GI effects; both of which are mild to moderate, easily managed and reversible 36,37,54. In order to determine whether an EGFR TKI or chemotherapy is the appropriate first-line therapy, the latest guidelines 55 recommend mutation testing for all patients with advanced NSCLC tumor. All EGFR-mutated patients treated with gefitinib or erlotinib invariably develop acquired resistance to this kind of therapy 56,57 (Figure 1). The most common and first identified mutation is the threonine-790 to methionine (T790M) point mutation in exon 20 which represents approximately 50% of all acquired resistance in NSCLC 58. The development of such genetic alteration restores the EGFR TK affinity to ATP, rendering first-generation TKIs inactive 59,60. Other secondary resistance mutations within the same gene have been reported infrequently (L747S, D761Y, T854A) 12, All these mutations, together with T790M, have also been identified in pre-treatment tumors and, similarly, are responsible for both a lesser sensitivity and duration of response to the first generation TKIs 61, Other mechanisms of acquired resistance include MET gene amplification (also accounting for up to 20% of pre-treatment tumoral resistances) 66, increased signalling through parallel pathways such as the ones of VEGF 67 and IGF1R 68, mutations and activation of PIK3CA 69,70 and transformation into a small-cell lung cancer phenotype 71. Concerns have been raised about resistance to TKIs due to mutations in the KRAS gene (which encodes for a protein downstream to the EGFR in the pathway initiated by the activation of the tyrosine kinase) or due to mutations that occur in other proteins of the same cascade (e.g. BRAF 72 ). Even if some studies have underlined that KRAS mutations are negative predictors of sensitivity to TKIs in NSCLCs 73, more recent research demonstrates that they are not necessarily associated with a poor response to this receptor-targeted therapy; this is contrary to the absence of EGFR mutations, which accounts for the lack of effectiveness of treatment with tyrosine kinase inhibitors 74,75. Management of EGFR tumor resistance has become the next challenge in order to lengthen these patients' overall survival; identification of the molecular resistance mechanisms will allow for the treatment of TKI-resistant tumors. A new class of drugs, the so-called second-generation TKIs, may be able to overcome the T790M mutation resistant cell. Compared to first-generation TKIs, these molecules show higher affinity for the ATP-binding domain, form an irreversible covalent bond to the ATP-binding site and are able to stimulate other receptors (e.g. HER2). Neratinib (HKI-272), one of the three agents investigated, hasn't shown good RR when tested on patients with known T790M mutation 76, therefore further development of this drug in lung cancer has been halted. Afatinib (BIBW2992) is being investigated as part of the LUX-Lung program which aims to evaluate the use of TKI in second- or third-line treatment in patients who have acquired resistance to gefitinib or erlotinib (LUX-Lung 1, 4 and 5) as well as the use of TKIs as a first-line treatment in patients with EGFR-activating mutations (LUX-Lung 2, 3 and 6). Therapy with afatinib has demonstrated to improve the disease control rate and to prolong PFS in both LUX-Lung 1 and 2 77,78. The G719S mutation renders the tumor less sensitive to gefitinib, while erlotinib and the second-generation TKI afatinib have proven to be effective in tumors characterized by this substitution 30. Dacomitinib (PF ) is another irreversible TKI able to target the activity of all HER TKs and has shown activity in NSCLC cell lines harbouring the T790M mutation7 9. This molecule has been evaluated in two phase II trials: the first one was after failure of one or two chemotherapy regimens and failure on erlotinib 80 ; the second one compared it with erlotinib in the second- and third-line in patients with advanced NSCLC 81. The results of these studies seem promising and further studies will evaluate dacomitinib in upfront therapy over first-generation TKIs and in resistant EGFR-mutated tumors 82. Pre-treatment EGFR - genotypic assessment As the EGFR mutational profile of NSCLCs is a strong predictor of response to therapy with the highly effective TKIs 36,37, the most recent algorithms for the management of advanced NSCLCs underline the importance of EGFR molecular testing prior to the initiation of therapy 30,83, adopting either a traditional Sanger s sequencing-based analysis 30,84 or PCR assays 30. Recent advances in genome analysis technologies lead to the use of high-throughput next generation sequencing platforms, which may become more
6 325 available in routine clinical practice in a near future 85,86. In particular, EGFR mutations should be sought in those NSCLCs in which they occur most frequently: adenocarcinomas, NSCLCs in people who have never smoked, Asians and women 30. A first-line treatment with TKIs should be initiated in those patients who have a positive result for EGFR mutations, otherwise a standard chemotherapy should be considered 30,83. EGFR mutation-positive NSCLCs which also test positive for mutations associated with primary or, most frequently, secondary resistance to first-generation TKIs (first of all the T790M substitution) may respond better to newer agents like afatinib, and dacomitinib, which have demonstrated a greater effectiveness in these clinical situations, but more clinical data are required 30,56, Figure 1. Ways to leave your EGFR inhibitor: Biochemical pathways leading to resistance to small molecule EGFR drugs such as gefitinib and erlotinib. (A) Structures of two approved EGFR TKIs, gefitinib and erlotinib, used in the treatment of NSCLC. (B) Ribbon diagram of wild-type human EGFR (PDB code 2ITY), illustrating binding of gefitinib to the active site of the kinase. The magenta ball-stick (located just above the gefitinib molecule in the active site) indicates the gatekeeper residue (threonine790) that is commonly mutated to methionine (T790M), resulting in reduced inhibitor binding and drug resistance. (C) Simplified pathway diagram of EGFR signaling through RAS/MEK/ERK and PI3K/PDK1/AKT indicating the points of mutation/amplification in EGFR TKI resistance as reported by Sequist and colleagues. The resistance mechanisms include the EGFR T790M gatekeeper mutation, amplification of EGFR T790M, MET amplification, and PI3KCA mutation (note that additional epithelial to mesenchymal transition changes and transformation from the NSCLC to the SCLC phenotype also lead to resistance but are not covered by this illustration). The illustration also shows the FAS/NF-kB signaling arm downstream of the FAS death receptor that was shown to be important in TKI resistance by Bivona and colleagues. Reprinted from Cancer Cell, 19, Paul Workman and Paul A. Clarke, Resisting Targeted Therapy: Fifty Ways to Leave Your EGFR, , 2011, with permission from Elsevier.
7 326 Furthermore, some studies have supported the validity of pre-treatment measurement of EGFR gene copy number by FISH in predicting response to TKIs 7, NSCLCs which over-express both EGFR and HER2 (over-expression directly correlates with FISH measurement of gene copy number) seem to be more sensitive to TKIs, providing another criterion that can help the clinician in therapeutic decision making 7,32. In any case, these findings on the role of tyrosine kinase receptors over-expression as a positive predictor of response to molecular-targeted drugs are controversial because of the conflicting evidence of different trials 55, It is worth noting that the conflicting evidence may also be due to methodological differences among laboratories performing the FISH assay or to different interpretations of FISH results 90. Accordingly, the only strong evidence on the effectiveness of predictors of success in the treatment of advanced NSCLCs with TKIs is in favor of EGFR mutation assessment 55, In future, when other classes of now developmental targeted drugs are available in clinical practice, the assessment of mutations or overexpression of genes other than EGFR in EGFR negative NSCLCs (KRAS, HER2, ALK/EML4-ALK, PIK3CA, BRAF, FGFR1) may become routine 30,83. Although genotypic assessment may be useful in determining which patients are likely to respond to EGFR TKI therapy, problems are associated with obtaining suitable DNA for pre-treatment analysis. The quality of the samples and the extracted DNA and the quantity of DNA available using current methods may limit the routine use of genotypic assessment. As described above, cancer cells from various sources have been used for genotyping. These include archived surgically resected tissue from patients who subsequently develop recurrent or progressive disease, formaline-fixed paraffine-embedded biopsy tissue, frozen sections, cytology specimens from lavage, pleural effusion, FNA (CTCs), tumor DNA in serum and tumor DNA in plasma or blood. The mutation status of EGFR can be also determined in tumor specimens obtained during curative surgery or at biopsy. Surgery offers the best chance of high-quality and high-volume tumor tissue samples, however only 20-25% of lung cancers are suitable for curative surgery and EGFR TKI therapy is only licensed for use in patients with advanced disease. Generally, there is only a small amount of tumor in routine diagnostic biopsy samples from patients with advanced disease; that is why specimens should be optimized and handled properly so that the most accurate pathologic characterization is achieved by individualizing among NSCLC, especially in adenocarcinoma, those histotypes that are more frequently driven by EGFR mutation. Especially for poorly differentiated neoplasms, a significant amount of specimen is often needed for diagnostic purposes and consumed for special immunohistochemical stains, as P63, P40 (markers of squamous differentiation), TTF-1 (positive in most of primitive lung adenocarcinoma), cromogranine and synaptophysine (marker of neuroendocrine differentiation), therefore reducing the material available for molecular testing. Lim and colleagues were able to obtain sufficient genomic DNA for genotypic assessment from more than 80% of their 24 low-volume samples (needle or forceps biopsy or fine-needle aspiration) 93. Of the 139 patients studied by Shih and colleagues 94 only two had insufficient DNA for analysis, whereas Savic and colleagues 95 successfully sequenced the DNA from 93% of their 84 cytological NSCLC specimens. Nakajima and colleagues 96 determined EGFR mutation status in all 43 patients in their study, and Yoshida and colleagues 97 determined EGFR mutation status in all 35 fine-needle aspiration/biopsy samples in their study. What is of crucial importance is that any tested sample is checked for adequacy in terms of the number and percentage of tumor cells. Two recently published studies reporting successful EGFR mutation detection from FNA cytology samples found EGFR mutation rates significantly lower than those reported from the same laboratories using tissue biopsies 98,99, while a recent review reported a sensitivity between 92% and 100% for EGFR mutation detection in tissue samples, varying with different techniques, and comparable results with cytology samples 100. Follow-up biopsy to determine the T790M mutation status may be unnecessary if further research supports the initial finding that DNA sufficient for genotypic assessment can be isolated from blood samples A study reported a 92% sensitivity for detection of EGFR mutations in patients with metastatic NSCLC with this method (11 of 12 patients) 83. There seems to be homogeneity of EGFR mutational state within the same tumoral lesion, even if histologically heterogeneous, and this provides a rationale for a sample-driven therapy 104. However, it remains to be further elucidated if there are practical consequences in relation to the finding that NSCLCs metastases in extrapulmonary organs or multiple intrapulmonary nodules can either differ from the primary lesion or from each other in regards to the EGFR mutational state and expression 107 as detected by the laboratory. It is in this context if multiple biopsies are necessary to correctly evaluate the EGFR profile. Moreover, the response of some EGFR mutation positive patients to TKIs treatment has proven to be
8 327 "mixed" 105 : this means that clinical responses which are not completely consistent with those expected from the EGFR mutation analysis, could be explained by the aforementioned differences in the EGFR mutational state and expression among different tumoral sites. Furthermore, it seems that chemotherapy is able to modify the EGFR expression in NSCLCs 107 by increasing or decresing it. This should be taken into consideration when anti-egfr monoclonal antibody cetuximab is used to treat patients whose tumoral EGFR expression was assessed before chemotherapy: in this case, EGFR expression should be reassessed after having performed chemotherapy. Conclusions It is reasonable to suggest that personalized therapy for NSCLC patients should include a genetic assessment of the EGFR mutational status for individual patients. In this scenario, our overview aims to focus on the necessity of standardizing and improving pre-diagnostic and diagnostic tools and of optimizing the accuracy and sensitivity of EGFR mutational testing so that it might be introduced into routine clinical practice. The appropriate role of an EGFR mutation routine analysis in the treatment of patients with NSCLC continues to evolve; this on the basis of new prospective clinical studies providing new standards of care such as adequate documentation of the EGFR mutational status in the preclinical setting, during the treatment and in related follow-up. There is reasonable basis to believe in the use of instrumental molecular reassessment of neoplastic biological characteristics for patients with advanced NSCLC throughout the clinical course in order to finely tune the treatment, particularly in the case of disease progression. In this way, TK inhibitors could be used for the best outcome in the patient, and the drug resistance that supervenes during treatment can thus be promptly identified. In addition, close cooperation between clinicians, surgeons, molecular biologists and pathologists is crucial for a continuous improvement in the field of NSCLC target therapy. Abbreviations NSCLC: non small cell lung cancer; ADC: adenocarcinoma; SqCC: squamous cell carcinoma; RTKs: receptor tyrosine kinases; TKIs: tyrosine kinase inhibitors; ALK: anaplastic lymphoma kinase; HER: human epidermal growth factor receptor; ErbB: erythroblastic leukemia viral oncogene homolog; PIK3CA: phosphatidylinositol 3 -kinase; AKT: protein kinase B (PKB); mtor: mammalian target of rapamycin; RAS: rat sarcoma; RAF: rapidly accelerated fibrosarcoma; MAP: mitogen-activated protein; STAT: signal transducers and activators of transcription; VEGF: vascular endothelial growth factor; RR: response rate; ATP: adenosine-5'-triphosphate; IPASS: Iressa pan-asia study; EURTAC: European Tarceva Versus Chemotherapy; FDA: food and drug administration; GI: gastrointestinal; MET: MNNG HOS Transforming gene; IGF1R: insulin-like growth factor 1 receptor; KRAS: v-ki-ras2 Kirsten rat sarcoma viral oncogene homolog; BRAF: v-raf murine sarcoma viral oncogene homolog B1; PCR: polymerase chain reaction; IHC: immunohistochemistry; FISH: fluorescence in situ hybridization; FGFR1: fibroblast growth factor receptor 1; DNA: deoxyribonucleic acid; FNA: fine-needle aspiration; CTCs: circulating tumor cells; SCLC: small cell lung cancer. Acknowledgement The authors gratefully thank Dr. Andrea Vingiani, resident in Anatomic and Clinical Pathology at the University of Milan, for his sincere cooperation. We would like to dedicate the efforts of all our work to Professor Laura Vizzotto. Competing Interests The authors have declared that no competing interest exists. References 1. Arteaga C. Targeting HER1/EGFR: a molecular approach to cancer therapy. Semin Oncol. 2003; 30: Paez JG, Janne PA, Lee JC, et al. EGFR mutations in lung cancer: correlation with clinical response to gefitinib therapy. Science. 2002; 304: Lynch TJ, Bell DW, Sordella R, et al. Activating mutations in the epidermal growth factor receptor underlying responsiveness of non-small-cell lung cancer to gefitinib therapy. N Engl J Med. 2004; 350: Cheng L, Zhang S, Alexander R, et al. The landscape of EGFR pathways and personalized management of non-small-cell lung cancer. Future Oncol. 2011; 7: Normanno N, De Luca A, Bianco C, et al. Epidermal growth factor receptor (EGFR) signaling in cancer. Gene. 2006; 366: Hynes NE, Lane HA. ERBB receptors and cancer: the complexity of targeted inhibitors. Nat Rev Cancer. 2005; 5: HirschFR, Varella-Garcia M, Capuzzo. Predictive value of EGFR and HER2 overexpression in advanced non-small-cell lung cancer. Oncogene. 2009; 28: S32-S Quesnelle KM, Boehm AL, Grandis JR. STAT-mediated EGFR signaling in cancer. J Cell Biochem. 2007; 102(2): Wang X, Zhang S, MacLennan GT, et al. Epidermal growth factor receptor protein expression and gene amplification in the chemorefractory metastatic embryonal carcinoma. Mod Pathol. 2008; 22: Wang X, Zhang S, MacLennan GT, et al. Epidermal growth factor receptor protein expression and gene amplification in small cell carcinoma of the urinary bladder. Clin Cancer Res. 2007; 13: Herbst RS, Heymach JV, Lippman SM. Lung cancer. N Engl J Med. 2008; 359: Costa DB, Halmos B, Kumar A, et al. BIM mediates EGFR tyrosine kinase inhibitor-induced apoptosis in lung cancers with oncogenic EGFR mutations. PLoS Med. 2007; 4: Sharma SV, Haber DA, Settleman J. Epidermal growth factor receptor mutations in lung cancer. Nat Rev Cancer. 2007; 7:
9 Sequist LV, Bell DW, Lynch TJ, et al. Molecular predictor of response to epidermal growth factor receptor antagonists in non-small-cell lung cancer. J ClinOncol. 2007; 25: Ladanyi M, Pao W. Lung adenocarcinoma: guiding EGFR-targeted therapy and beyond. Mod Pathol. 2008; 21 (Suppl 2): S16-S Shigematsu H, Lin L, Takahashi T, et al. Clinical and biological features associated with epidermal growth factor receptor gene mutations in lung cancer. J Natl Cancer Inst. 2005; 97: Pao W, Girard N. New driver mutations in non-small-cell lung cancer. The Lancet Oncology. 2011; 12: Yamamoto H, Toyooka S, Mitsudomi T. Impact of EGFR mutation analysis in non-small-cell lung cancer. Lung Cancer. 2009; 63: Eberhard DA, Johnson BE, Amler LC, et al. Mutations in the epidermal growth factor receptor and in KRAS are predictive and prognostic indicators in patients with non-small-cell lung cancer treated with chemotherapy alone and in combination with erlotinib. J ClinOncol. 2005; 23: Schrump DS, Altorki NK, Henschke CL, et al. Non-small cell lung cancer. In: DeVita VT, ed. Cancer: Principles and Practices of Oncology. Philadelphia: Lippincott Williams & Wilkins; 2005: Azzoli CG, Baker Jr S, Temin S, et al. American Society of Clinical Oncology Clinical Practice Guideline update on chemotherapy for stage IV non-small-cell lung cancer. J Clin Oncol. 2009; 27: Fossella F, Pereira JR, von Pawel J, et al. Randomized, multinational phase III study of docetaxel plus platinum combinations versus vinorelbine plus cisplatin for advanced non-small-cell lung cancer: the TAX 326 study group. J ClinOncol. 2003; 21: Sandler A, Gray R, Perry MC, et al. Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med. 2006; 355: Shepherd FA, Dancey J, Ramlau R, et al. Prospective randomized trial of docetaxel versus best supportive care in patients with non-small-cell lung cancer previously treated with platinum-based chemotherapy. J Clin Oncol. 2000; 18: Hanna N, Shepherd FA, Fossella FV, et al. Randomized phase III trial of pemetrexed versus docetaxel in patients with non-small-cell lung cancer previously treated with chemotherapy. J ClinOncol. 2004; 22: Shepherd FA, Rodrigues PJ, Ciuleanu T, et al. Erlotinib in previously treated non-small-cell lung cancer. NEngl J Med. 2005; 353: Lynch TJ, Bell DW, Sordella R, et al. Activating mutations in the epidermal growth factor receptor underlying responsiveness of non-small-cell lung cancer to gefitinib. N Engl J Med. 2004; 350: Paez JG, Janne PA, Lee JC, et al. EGFR mutations in lung cancer: correlation with clinical response to gefitinib therapy. Science. 2004; 304: Fujita S, Katakami N, Masago K, et al. Customized chemotherapy based on epidermal growth factor receptor mutation status for elderly patients with advanced non-small-cell lung cancer: a phase II trial. BMC Cancer. 2012; 12: Soria JC, Mok TS, Cappuzzo F, Pasi AJ. EGFR-mutated oncogene-addicted non-small cell lung cancer: Current trends and future prospects. Cancer treatment reviews. 2012; 38: Zhu J, Zhong W, Zhang G. Better survival with EGFR exon 19 than exon 21 mutations in gefitinib-treated non-small cell lung cancer patients is due to differential inhibition of downstream signals. Cancer Lett. 2008; 265(2): Cappuzzo F, Varella-Garcia M, Shigematsu H, et al. Increased HER2 gene copy number is associated with response to gefitinib therapy in epidermal growth factor receptor-positive non-small-cell lung cancer patients. Journal of Clinical Oncology. 2005; 23: Pirker R, Pereira JR, von Pawel J. EGFR expression as a predictor of survival for first-line chemotherapy plus cetuximab in patients with advanced non-small-cell lung cancer: analysis of data from the phase 3 FLEX study. Lancet Oncol. 2012; 13: Wang M, Zhao J, Zhang LM. Combined Erlotinib and Cetuximab overcome the acquired resistance to epidermal growth factor receptors tyrosine kinase inhibitor in non-small-cell lung cancer. J Cancer Res Clin Oncol. 2012;138(12): Kim HP, Han SW, Kim SH. Combined lapatinib and cetuximab enhance cytotoxicity against gefitinib-resistant lung cancer cells. Mol Cancer Ther (3): Mok TS, Wu YL, Thongprasert S, et al. Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma. N Engl J Med. 2009; 361: Maemondo M, Inoue A, Kobayashi K, et al. Gefitinib or chemotherapy for non-small-cell lung cancer with mutated EGFR. N Engl J Med. 2010; 362: Zhu CQ, da Cunha Santos G, Ding K, et al. Role of KRAS and EGFR as biomarkers of response to erlotinib in National Cancer Institute of Canada Clinical Trials Group Study BR.21. J ClinOncol. 2008; 26: Kim ES, Hirsh V, Mok T, et al. Gefitinib versus docetaxel in previously treated non-small-cell lung cancer (INTEREST): a randomised phase III trial. Lancet. 2008; 372: Costa DB, Kobayashi S, Tenen DG, et al. Pooled analysis of the prospective trials of gefitinib monotherapy for EGFR-mutant non-small-cell lung cancer. Lung Cancer. 2007; 58: Rosell R, Moran T, Queralt C, et al. Screening for epidermal growth factor mutations in lung cancer. N Engl J Med. 2009; 361: Sequist LV, Martins RG, Spigel D, et al. First-line gefitinib in patients with advanced non-small-cell lung cancer harboring somatic EGFR mutations. J Clin Oncol. 2008; 26: Tamura K, Okamoto I, Kashii T, et al. Multicentre prospective phase II trial of gefitinib for advanced non-small-cell lung cancer with epidermal growth factor receptor mutations: results of the West Japan Thoracic Oncology Group trial (WJTOG0403). Br J Cancer. 2008; 98: Mok T, Wu YC, Thongprasert S, et al. Phase III, randomised, open-label, first-line study gefitinib (G) vs carboplatin/paclitaxel (C/P) in clinically selected patients (PTS) with advanced non-small-cell lung cancer (NSCLC) (IPASS). Ann Oncol. 2008; 19: AbstractLBA Mitsudomi T, Morita S, Yatabe Y, et al. Gefitinib versus cisplatin plus docetaxel in patients with non-small-cell lung cancer harbouring mutations of the epidermal growth factor receptor (WJTOG3405): an open label, randomised phase 3 trial. Lancet Oncol. 2010; 11: Inoue A, Suzuki T, Fukuhara T, et al. Prospective phase II study of gefitinib for chemotherapy-naive patients with advanced non-small cell lung cancer with epidermal growth factor mutations. J ClinOncol. 2006; 24: Asahina H, Yamazaki K, Kinoshita I, et al. A phase II trial of gefitinib as first-line therapy for advanced non-small cell lung cancer with epidermal growth factor receptor. Br J Cancer. 2006; 95: Yoshida K, Yatabe Y, Park JY, et al. Prospective validation for prediction of gefitinib sensitivity by epidermal growth factor receptor gene mutation in patients with non-small cell lung cancer. J Thorac Oncol. 2007; 2: Sugio K, Uramoto H, Onitsuka T, et al. Prospective phase II study of gefitinib in non-small cell lung cancer with epidermal growth factor receptor gene mutations. Lung Cancer. 2009; 64: Zhou C, Wu Y-L, Chen G, et al. Erlotinib versus chemotherapy as first-line treatment for patients with advanced EGFR mutation-positive non-small-cell lung cancer (OPTIMAL, CTONG-0802): a multicentre, open-label, randomised, phase 3 study. Lancet Oncol. 2011; 12: Rosell R, Carcereny E, Gervais R, et al. Erlotinib versus standard chemotherapy as first-line treatment for European patients with advanced EGFR mutation-positive non-small-cell lung cancer (EURTAC): a multicentre, open-label, randomised phase 3 trial. Lancet Oncol. 2012; 13: Scheffler M, Di Gion P, Doroshyenko O, et al. Clinical pharmacokinetics of tyrosine kinase inhibitors: focus on 4-anilinoquinazolines. ClinPharmacokinet. 2011; 50(6): Ettinger DS, Akerley W, Bepler G, et al. Non-small-cell lung cancer. J NatlComprCancNetw. 2010; 8: Thongprasert S, Duffield E, Saijo N et al. Health-related quality-of-life in a randomized fase III first-line study of Gefitinib versus Carboplatin/Paclitaxel in clinically selected patients from Asia with advanced NSCLC (IPASS). J ThoracOncol. 2011; 6: Keedy VL, Temin S, Somerfield MR, et al. American Society of Clinical Oncology Provisional Clinical Opinion: Epidermal Growth Factor Receptor (EGFR) mutation testing for patients with advanced non-small-cell lung cancer considering first-line EGFR Tyrosine kinase inhibitor therapy. J ClinOncol. 2011; 29: Nguyen KS, Kobayashi S, Costa DB. Acquired resistance to epidermal growth factor receptor tyrosine kinase inhibitors in non-small-cell lung cancers dependent on the epidermal growth factor receptor pathway. Clin Lung Cancer. 2009; 10: Jackman D, Pao W, Riely GJ, et al. Clinical definition of acquired resistance to epidermal growth factor receptor tyrosine kinase inhibitors in non-small-cell lung cancer. J Clin Oncol. 2010; 28: Suda K, Onozato R, Yatabe Y, et al. EGFR T790M mutation: a double role in lung cancer survival? J Thorac Oncol. 2009; 4: Pao W, Miller VA, Politi KA, et al. Acquired resistance of lung adenocarcinomas to gefitinib or erlotinib is associated with a second mutation in the EGFR kinase domain. PLoS Med. 2005; 2: e73.
10 Yun CH, Mengwasser KE, Toms AV, et al. The T790M mutation in EGFR kinase causes drug resistance by increasing the affinity for ATP. Proc- NatlAcadSci USA. 2008; 105: Bean J, Riely GJ, Balak M, et al. Acquired resistance to epidermal growth factor receptor kinase inhibitors associated with a novel T854A mutation in a patient with EGFR-mutant lung adenocarcinoma. Clin Cancer Res. 2008; 14: Balak MN, Kwak EL, Shaw AT, et al. Novel D761Y and common secondary T790M mutations in epidermal growth factor receptor-mutant lung adenocarcinomas with acquired resistance to kinase inhibitors. Clin Cancer Res. 2006; 12: Maheswaran S, Sequist LV, Nagrath S, et al. Detection of mutations in EGFR in circulating lung cancer cells. N Engl J Med. 2008; 359: Ayoola A, Barochia A, Belani K, Belani C. Primary and acquired resistance to epidermal growth factor receptor tyrosine kinase inhibitors in non-small cell lung cancer: an update. Cancer Invest. 2012; 30 (5): Su KY, Chen HY, Li KC, et al. Pretreatment epidermal growth factor receptor (EGFR) T790M mutation predicts shorter EGFR tyrosine kinase inhibitor response duration in patients with non-small cell lung cancer. J Clin Oncol. 2012; 30 (4): Chen HJ, Mok TS, Chen ZH, et al. Clinicopathologic and molecular features of epidermal growth factor receptor T790M mutation and c-met amplification in tyrosine kinase inhibitor-resistant Chinese non small cell lung cancer. PatholOncol Res. 2009; 15: Viloria-Petit A, Crombet T, Jothy S, et al. Acquired resistance to the antitumor effect of epidermal growth factor receptor-blocking antibodies in vivo: a role for altered tumor angiogenesis. Cancer Res. 2001; 61: Guix M, Faber AC, Wang SE, et al. Acquired resistance to EGFR tyrosine kinase inhibitors in cancer cells is mediated by loss of IGF-binding proteins. J Clin Invest. 2008; 118: Okudela K, Suzuki M, Kageyama S, et al. PIK3CA mutation and amplification in human lung cancer. PatholInt. 2007; 57: Yamamoto H, Shigematsu H, Nomura M, et al. PIK3CA mutations and copy number gains in human lung cancers. Cancer Res. 2008; 68: Sequist LV, Waltman BA, Dias-Santagata D, et al. Genotypic and histological evolution of lung cancers acquiring resistance to EGFR inhibitors. SciTransl Med. 2011; 3: 75ra Ohashi K, Sequist LV, Arcila ME, et al. Lung cancers with acquired resistance to EGFR inhibitors occasionally harbor BRAF gene mutations but lack mutations in KRAS, NRAS, or MEK1. ProcNatlAcadSci U S A. 2012; 109(31): E Linardou H, Dahabreh IJ, Kanaloupiti D, et al. Assessment of somatic k-ras mutations as a mechanism associated with resistance to EGFR-targeted agents: a systematic review and meta-analysis of studies in advanced non-small-cell lung cancer and metastatic colorectal cancer. Lancet Oncol. 2008; 9(10): Pesek M, Benesova L, Belsanova B, et al. Dominance of EGFR and insignificant KRAS mutations in prediction of tyrosine-kinase therapy for NSCLC patients stratified by tumor subtype and smoking status. Anticancer Res. 2009; 29(7): Roberts PJ, Stinchcombe TE, Der CJ, Socinski MA. Personalized medicine in non-small-cell lung cancer: is KRAS a useful marker in selecting patients for epidermal growth factor receptor- targeted therapy? J Clin Oncol. 2010; 28(31): Sequist LV, Besse B, Lynch TJ, et al. Neratinib, an irreversible pan-erbb receptor tyrosine kinase inhibitor: results of phase II trial in patients with advanced non small-cell lung cancer. J Clin Oncol. 2010; 28: Miller VA, Hirsch V, Cadranel J, et al. Afatinib versus placebo for patients with advanced, metastatic non-small-cell lung cancer after failure of erlotinib, gefitinib, or both, and one or two lines of chemotherapy (LUX-Lung 1): a phase 2b/3 randomised trial. Lancet Oncol. 2012; 13: Yang C, Shih J, Su W, et al. Afatinib for patients with lung adenocarcinoma and epidermal growth factor receptor mutations (LUX-Lung 2): a phase 2 trial. Lancet Oncol. 2012; 13: Engelman JA, Zejnullahu K, Gale CM, et al. PF , an irreversible pan-erbb inhibitor, is effective in lung cancers models with EGFR and ERBB2 mutations that are resistant to gefitinib. Cancer Res. 2007; 67: Boyer MJ, Blackhall FH, Park K, et al. Efficacy and safety of PF versus erlotinib: a global, randomised phase 2 trial in patients with advanced non small cell lung cancer after failure of chemotherapy. In: Proceedings of 46th Annual Meeting of the American Society of Clinical Oncology. J Clin Oncol. 2010; 28 (15 Suppl): abstractlba Takahashi T, Boku N, Murakami H, et al. Phase I and pharmacokinetic study of dacomitinib (PF ), an oral irreversible, small molecule inhibitor of human epidermal growth factor receptor-1, -2, and -4 tyrosine kinases, in Japanese patients with advanced solid tumors. Invest New Drugs 2012; Epub ahead of print. 82. Ramalingam SS, Blackhall F, Krzakowski M, et al. Randomized Phase II Study of Dacomitinib (PF ), an Irreversible Pan-Human Epidermal Growth Factor Receptor Inhibitor, Versus Erlotinib in Patients With Advanced Non-Small-Cell Lung Cancer. J ClinOncol. 2012; 30(27): Tanner NT, Pastis NJ, Sherman C, et al. The role of molecular analyses in the era of personalized therapy for advanced NSCLC. Lung Cancer. 2012; 76: Warth A, Penzel R, Brandt R, et al. Optimized algorithm for Sanger sequencing-based EGFR mutation analyses in NSCLC biopsies. Virchows Arch. 2012; 460(4): Pareek C, Smoczynski R, Tretyn A. Sequencing technologies and genome sequencing. J Appl Genet. 2011; 52(4): Su Z, Ning B, Fang H. Next-generation sequencing and its applications in molecular diagnostics. Expert Rev Mol Diagn. 2011; 11(3): Giaccone G, Wang Y. Strategies for overcoming resistance to EGFR family tyrosine kinase inhibitors. Cancer Treat Rev. 2011; 37(6): Luping Lin, Trever G. Bivona. Mechanisms of resistance to epidermal growth factor receptor inhibitors and novel therapeutic strategies to overcome resistance in NSCLC patients. Chemother Res Pract 2012; Epub ahead of print. 89. Gazdar AF. Activating and resistance mutations of EGFR in non-small-cell lung cancer: role in clinical response to EGFR tyrosine kinase inhibitors. Oncogene. 2009; 28 (Suppl 1): S24-S Varella-Garcia M, Diebold J, Eberhard DA, et al. EGFR fluorescence in situ hybridisation assay: guidelines for application to non-small-cell lung cancer. J Clin Pathol. 2009; 62(11): Pallis AG, Fennell DA, Szutowicz E, et al. Biomarkers of clinical benefit for anti-epidermal growth factor receptor agents in patients with non-small-cell lung cancer. Br J Cancer. 2011; 105(1): Zhang X, Chang A. Molecular predictors of EGFR-TKI sensitivity in advanced non-small cell lung cancer. Int J Med Sci. 2008; 5(4): Lim EH, Zhang SL, Yu K, et al. An alternative approach to determining therapeutic choices in advanced non-small cell lung carcinoma (NSCLC): maximizing the diagnostic procedure and the use of low-volume lung biopsies. J ThoracOnco. 2007; 2: Shih JY, Gow CH, Yu CJ, et al. Epidermal growth factor receptor mutations in needle biopsy/aspiration samples predict response to gefitinib therapy and survival of patients with advanced non small cell lung cancer. Int J Cancer. 2006; 118: Sunaga N, Tomizawa Y, Yanagitani N, et al. Phase II prospective study of the efficacy of gefitinib for the treatment of stage III/IV non-small cell lung cancer with EGFR mutations, irrespective of previous chemotherapy. Lung Cancer. 2007; 56: Nakajima T, Yasufuku K, Sufuku M, et al. Assessment of epidermal growth factor receptor mutation by endobronchial ultrasound-guided transbronchial needle aspiration. Chest. 2007; 132: Yoshida K, Yatabe Y, Park JY, et al. Prospective validation for prediction of gefitinib sensitivity by epidermal growth factor receptor gene mutation in patients with non-small cell lung cancer. J Thorac Oncol. 2007; 2: Garcia-Olivè I, Monsò E, Andreo F, et al. Endobronchial ultrasound-guidedtransbronchial needle aspiration for identifying EGFR mutations. Eur Respir J. 2010; 35: Fassina A, Gazziero A, Zardo D, et al. Detection of EGFR and KRAS mutations ontrans-thoracic needle aspiration of lung nodules by high resolution melting analysis. J ClinPathol. 2009; 62: Ellison G, Zhu G, Moulis A et al. EGFR mutation testing in lung cancer: a review of available methods and their use for analysis of tumour tissue and cytology samples. J Clin Pathol. 2012; 0: Kimura H, Kasahara K, Shibata K, et al. EGFR mutation of tumor and serum ingefitinib-treated patients with chemotherapy-naive non-small cell lung cancer. J ThoracOncol. 2006; 1: Kim KS, Jeong JY, Kim YC, et al. Predictors of the response to gefitinib in refractorynon-small cell lung cancer. Clin Cancer Res. 2005; 11: Mack PC, Holland WS, Burich RA, et al. EGFR mutations detected in plasma areassociated with patient outcomes in erlotinib plus docetaxel-treated non-small celllung cancer. J ThoracOncol. 2009; 4: Mattsson JS, Imgenberg-Kreuz J, Edlund K, et al. Consistent mutation status within histologically heterogeneous lung cancer lesions. Histopathology. 2012; 61(4):
11 Chen ZY, Zhong WZ, Zhang XC, et al. EGFR mutation heterogeneity and the mixed response to EGFR tyrosine kinase inhibitors of lung adenocarcinomas. Oncologist. 2012; 17(7): Sun L, Zhang Q, Luan H, et al. Comparison of KRAS and EGFR gene status between primary non-small cell lung cancer and local lymph node metastases: implications for clinical practice. J ExpClin Cancer Res. 2011; 30(1): Jakobsen JN, Sorensen JB. Intratumor heterogeneity and chemotherapy-induced changes in EGFR status in non-small cell lung cancer. Cancer ChemotherPharmacol. 2012; 69(2):
Successes and Limitations of Targeted Cancer Therapy in Lung Cancer
 Successes and Limitations of Targeted Cancer Therapy in Lung Cancer Kenichi Suda a, b Tetsuya Mitsudomi a a Division of Thoracic Surgery, Department of Surgery, Kinki University Faculty of Medicine, Osaka-Sayama,
Successes and Limitations of Targeted Cancer Therapy in Lung Cancer Kenichi Suda a, b Tetsuya Mitsudomi a a Division of Thoracic Surgery, Department of Surgery, Kinki University Faculty of Medicine, Osaka-Sayama,
Corporate Medical Policy
 Corporate Medical Policy Molecular Analysis for Targeted Therapy for Non-Small Cell Lung File Name: Origination: Last CAP Review: Next CAP Review: Last Review: molecular_analysis_for_targeted_therapy_for_non_small_cell_lung_cancer
Corporate Medical Policy Molecular Analysis for Targeted Therapy for Non-Small Cell Lung File Name: Origination: Last CAP Review: Next CAP Review: Last Review: molecular_analysis_for_targeted_therapy_for_non_small_cell_lung_cancer
Non-Small Cell Lung Cancer
 Non-Small Cell Lung Cancer in East tasia Chia-Chi (Josh) Lin, MD, PhD 林 家 齊 Director of Phase I Center, e Department of Oncology, National Taiwan University Hospital Clinical Associate Professor, Department
Non-Small Cell Lung Cancer in East tasia Chia-Chi (Josh) Lin, MD, PhD 林 家 齊 Director of Phase I Center, e Department of Oncology, National Taiwan University Hospital Clinical Associate Professor, Department
Pharmacogenomic markers in EGFR-targeted therapy of lung cancer
 Pharmacogenomic markers in EGFR-targeted therapy of lung cancer Rafal Dziadziuszko, MD, PhD University of Colorado Cancer Center, Aurora, CO, USA Medical University of Gdansk, Poland EMEA Workshop on Biomarkers,
Pharmacogenomic markers in EGFR-targeted therapy of lung cancer Rafal Dziadziuszko, MD, PhD University of Colorado Cancer Center, Aurora, CO, USA Medical University of Gdansk, Poland EMEA Workshop on Biomarkers,
Maintenance therapy in in Metastatic NSCLC. Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai
 Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
Maintenance therapy in in Metastatic NSCLC Dr Amit Joshi Associate Professor Dept. Of Medical Oncology Tata Memorial Centre Mumbai Definition of Maintenance therapy The U.S. National Cancer Institute s
KRAS Mutation Analysis in Non-Small Cell Lung Cancer (NSCLC) Original Policy Date
 MP 2.04.43 KRAS Mutation Analysis in Non-Small Cell Lung Cancer (NSCLC) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013
MP 2.04.43 KRAS Mutation Analysis in Non-Small Cell Lung Cancer (NSCLC) Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013
NCCN Non-Small Cell Lung Cancer V.1.2011 Update Meeting 07/09/10
 Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Guideline Page and Request NSCL-3 Stage IA, margins positive delete the recommendation for chemoradiation. Stage IB, IIA, margins positive delete the recommendation for chemoradiation + Stage IIA, Stage
Advancing Personalized Therapy for Advanced Non-Small Cell Lung Cancer
 GUIDING THE WAY White Paper Advancing Personalized Therapy for Advanced Non-Small Cell Lung Cancer is a serum proteomic test for patients with advanced non-small cell lung cancer that helps healthcare
GUIDING THE WAY White Paper Advancing Personalized Therapy for Advanced Non-Small Cell Lung Cancer is a serum proteomic test for patients with advanced non-small cell lung cancer that helps healthcare
Published Ahead of Print on April 11, 2011 as 10.1200/JCO.2010.31.8923. J Clin Oncol 29. 2011 by American Society of Clinical Oncology
 Published Ahead of Print on April 11, 2011 as 10.1200/JCO.2010.31.8923 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2010.31.8923 JOURNAL OF CLINICAL ONCOLOGY A S C O S P E C I A
Published Ahead of Print on April 11, 2011 as 10.1200/JCO.2010.31.8923 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2010.31.8923 JOURNAL OF CLINICAL ONCOLOGY A S C O S P E C I A
( targeted therapy ) ( oncogenesis ) ( epidermal. growth factor receptor tyrosine kinase inhibitor EGFR-TKI ) ( epidermal growth
 2008 19 8-13 growth factor receptor tyrosine kinase inhibitor EGFR-TKI ) ( targeted therapy ) ( oncogenesis ) ( epidermal factor receptor monoclonal antibody EGFR-moAb ) growth factor monoclonal antibody
2008 19 8-13 growth factor receptor tyrosine kinase inhibitor EGFR-TKI ) ( targeted therapy ) ( oncogenesis ) ( epidermal factor receptor monoclonal antibody EGFR-moAb ) growth factor monoclonal antibody
Non Small Cell Lung Cancer: Scientific Discoveries and the Pursuit of Progress
 Non Small Cell Lung Cancer: Scientific Discoveries and the Pursuit of Progress Lung Cancer Accounts for 14% of All New Cancer Diagnoses in the United States 1 Lung cancer is the second most common malignancy
Non Small Cell Lung Cancer: Scientific Discoveries and the Pursuit of Progress Lung Cancer Accounts for 14% of All New Cancer Diagnoses in the United States 1 Lung cancer is the second most common malignancy
EGFR gene mutations Ex 19 Ex 21 Paez et al, Science 2004
 Evolution of knowledge in NSCLC Pao and Girard, Lancet Oncology 2011 Fattori da considerare nella scelta terapeutica del NSCLC nel 2012 Stadio di malattia PS Età Comorbidità Compliance e desiderio del
Evolution of knowledge in NSCLC Pao and Girard, Lancet Oncology 2011 Fattori da considerare nella scelta terapeutica del NSCLC nel 2012 Stadio di malattia PS Età Comorbidità Compliance e desiderio del
Targeted Therapy What the Surgeon Needs to Know
 Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Targeted Therapy What the Surgeon Needs to Know AATS Focus in Thoracic Surgery 2014 David R. Jones, M.D. Professor & Chief, Thoracic Surgery Memorial Sloan Kettering Cancer Center I have no disclosures
Name of Policy: Molecular Analysis for Targeted Therapy of Non-Small-Cell Lung Cancer (NSCLC)
 Name of Policy: Molecular Analysis for Targeted Therapy of Non-Small-Cell Lung Cancer (NSCLC) Policy #: 468 Latest Review Date: October 2015 Category: Laboratory Policy Grade: B Background/Definitions:
Name of Policy: Molecular Analysis for Targeted Therapy of Non-Small-Cell Lung Cancer (NSCLC) Policy #: 468 Latest Review Date: October 2015 Category: Laboratory Policy Grade: B Background/Definitions:
The EGFR mutation and precision therapy for lung cancer
 for lung cancer Outcomes in advanced lung cancer have seen meaningful improvement in the past decade thanks to new precision drug therapies. Because tumors usually develop resistance to the drugs, scientists
for lung cancer Outcomes in advanced lung cancer have seen meaningful improvement in the past decade thanks to new precision drug therapies. Because tumors usually develop resistance to the drugs, scientists
ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials)
 ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials) 3 Integrated Trials Testing Targeted Therapy in Early Stage Lung Cancer Part of NCI s Precision Medicine Effort in
ALCHEMIST (Adjuvant Lung Cancer Enrichment Marker Identification and Sequencing Trials) 3 Integrated Trials Testing Targeted Therapy in Early Stage Lung Cancer Part of NCI s Precision Medicine Effort in
MEDICAL POLICY EFFECTIVE DATE: 12/20/07 REVISED DATE: 12/18/08, 12/17/09, 02/17/11, 12/15/11, 12/20/12, 12/19/13, 02/19/15
 MEDICAL POLICY SUBJECT: GENOTYPING - EPIDERMAL GROWTH PAGE: 1 OF: 6 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: GENOTYPING - EPIDERMAL GROWTH PAGE: 1 OF: 6 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Lung cancer is the leading cause of cancer-related death in the United
 Evolving Treatment Paradigms in Non-Small Cell Lung Cancer MARGARET E. M. VAN METER, MD Medical Oncology Fellow Division of Cancer Medicine The University of Texas M.D. Anderson Cancer Center Houston,
Evolving Treatment Paradigms in Non-Small Cell Lung Cancer MARGARET E. M. VAN METER, MD Medical Oncology Fellow Division of Cancer Medicine The University of Texas M.D. Anderson Cancer Center Houston,
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): 9/1/2011 Most Recent Review Date (Revised): 1/27/2015 Effective Date: 11/2/2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS
Original Issue Date (Created): 9/1/2011 Most Recent Review Date (Revised): 1/27/2015 Effective Date: 11/2/2015 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS
Shifting the Paradigm for Maintenance Therapy for Non small-cell Lung Cancer
 J Hong Kong Col Radiol. 2010;13(Suppl):S16-21 ORIGINAL ARTICLE Shifting the Paradigm for Maintenance Therapy for Non small-cell Lung Cancer VHF Lee Department of Clinical Oncology, Queen Mary Hospital,
J Hong Kong Col Radiol. 2010;13(Suppl):S16-21 ORIGINAL ARTICLE Shifting the Paradigm for Maintenance Therapy for Non small-cell Lung Cancer VHF Lee Department of Clinical Oncology, Queen Mary Hospital,
Medical Policy Manual. Date of Origin: August 2010. Topic: Molecular Analysis for Targeted Therapy of Non- Small Cell Lung Cancer (NSCLC)
 Medical Policy Manual Topic: Molecular Analysis for Targeted Therapy of Non- Small Cell Lung Cancer (NSCLC) Section: Genetic Testing Policy No: 56 Date of Origin: August 2010 Last Reviewed Date: December
Medical Policy Manual Topic: Molecular Analysis for Targeted Therapy of Non- Small Cell Lung Cancer (NSCLC) Section: Genetic Testing Policy No: 56 Date of Origin: August 2010 Last Reviewed Date: December
Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study
 Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
Turkish Journal of Cancer Volume 34, No.1, 2004 19 Is the third-line chemotherapy feasible for non-small cell lung cancer? A retrospective study MUSTAFA ÖZDO AN, MUSTAFA SAMUR, HAKAN BOZCUK, ERKAN ÇOBAN,
Future Directions in Clinical Research. Karen Kelly, MD Associate Director for Clinical Research UC Davis Cancer Center
 Future Directions in Clinical Research Karen Kelly, MD Associate Director for Clinical Research UC Davis Cancer Center Outline 1. Status of Cancer Treatment 2. Overview of Clinical Research at UCDCC 3.
Future Directions in Clinical Research Karen Kelly, MD Associate Director for Clinical Research UC Davis Cancer Center Outline 1. Status of Cancer Treatment 2. Overview of Clinical Research at UCDCC 3.
Clinical development of AZD9291 in non-small cell lung cancer
 Clinical development of AZD9291 in non-small cell lung cancer Rachael Lawrance (AstraZeneca) PSI One Day Meeting: The Innovative, Challenging and Diversified World of Respiratory Disease 13 Nov 2015 Overview
Clinical development of AZD9291 in non-small cell lung cancer Rachael Lawrance (AstraZeneca) PSI One Day Meeting: The Innovative, Challenging and Diversified World of Respiratory Disease 13 Nov 2015 Overview
Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART
 Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART Goals Discuss treatment options for stage 4 lung cancer: New and old Discuss new developments in personalized
Harmesh Naik, MD. Hope Cancer Clinic HOW DO I MANAGE STAGE 4 NSCLC IN 2012: STATE OF THE ART Goals Discuss treatment options for stage 4 lung cancer: New and old Discuss new developments in personalized
Emerging Drug List GEFITINIB
 Generic (Trade Name): Manufacturer: Gefitinib (Iressa ) formerly referred to as ZD1839 AstraZeneca NO. 52 JANUARY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence:
Generic (Trade Name): Manufacturer: Gefitinib (Iressa ) formerly referred to as ZD1839 AstraZeneca NO. 52 JANUARY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence:
Evolving Treatment Paradigms in Non-Small Cell Lung Cancer
 PRINTER-FRIENDLY VERSION AT PHARMACYPRACTICE NEWS.COM Evolving Treatment Paradigms in Non-Small Cell Lung Cancer CALEB T. CHU, MD, MPH Postdoctoral Fellow Department of Thoracic/Head and Neck Medical Oncology
PRINTER-FRIENDLY VERSION AT PHARMACYPRACTICE NEWS.COM Evolving Treatment Paradigms in Non-Small Cell Lung Cancer CALEB T. CHU, MD, MPH Postdoctoral Fellow Department of Thoracic/Head and Neck Medical Oncology
Third-line or fourth-line chemotherapy in non-small-cell lung cancer patients with relatively good performance status
 Available online at www.sciencedirect.com Journal of the Chinese Medical Association 74 (2011) 209e214 Original Article Third-line or fourth-line chemotherapy in non-small-cell lung cancer patients with
Available online at www.sciencedirect.com Journal of the Chinese Medical Association 74 (2011) 209e214 Original Article Third-line or fourth-line chemotherapy in non-small-cell lung cancer patients with
Epidermal Growth Factor Receptor Mutations in Patients with Non Small Cell Lung Cancer
 Review Epidermal Growth Factor Receptor Mutations in Patients with Non Small Cell Lung Cancer Bruce E. Johnson and Pasi A. Jänne Lowe Center for Thoracic Oncology, Department of Medical Oncology, Dana-Farber
Review Epidermal Growth Factor Receptor Mutations in Patients with Non Small Cell Lung Cancer Bruce E. Johnson and Pasi A. Jänne Lowe Center for Thoracic Oncology, Department of Medical Oncology, Dana-Farber
Breast and Lung Cancer Biomarker Research at ASCO: Changing Treatment Patterns
 July 2013 Edition Vol. 7, Issue 7 Breast and Lung Cancer Biomarker Research at ASCO: Changing Treatment Patterns By Julie Katz, MPH, MPhil Biomarkers played a prominent role in the research presented in
July 2013 Edition Vol. 7, Issue 7 Breast and Lung Cancer Biomarker Research at ASCO: Changing Treatment Patterns By Julie Katz, MPH, MPhil Biomarkers played a prominent role in the research presented in
Advanced EGFR Mutation-Positive Non Small-Cell Lung Cancer: Case Report, Literature Review, and Treatment Recommendations
 Special Report Advanced EGFR Mutation-Positive Non Small-Cell Lung Cancer: Case Report, Literature Review, and Treatment Recommendations Andrew Kuykendall, MD, and Alberto Chiappori, MD Background: Lung
Special Report Advanced EGFR Mutation-Positive Non Small-Cell Lung Cancer: Case Report, Literature Review, and Treatment Recommendations Andrew Kuykendall, MD, and Alberto Chiappori, MD Background: Lung
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
 Department of Veterans Affairs Health Services Research & Development Service Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
Department of Veterans Affairs Health Services Research & Development Service Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost-Effectiveness
Targeted Therapies in Lung Cancer
 Targeted Therapies in Lung Cancer I Edited by: Simona Carnio Thoracic Oncology Division - St Luigi Hospital Orbassano (TO) - Italy Silvia Novello Department of Oncology - University of Torino - Italy Why
Targeted Therapies in Lung Cancer I Edited by: Simona Carnio Thoracic Oncology Division - St Luigi Hospital Orbassano (TO) - Italy Silvia Novello Department of Oncology - University of Torino - Italy Why
National Horizon Scanning Centre. Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer. December 2007
 Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Vandetanib (Zactima) for advanced or metastatic non-small cell lung cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search.
Cancer Treatment Reviews
 Cancer Treatment Reviews 38 (2012) 416 430 Contents lists available at SciVerse ScienceDirect Cancer Treatment Reviews journal homepage: www.elsevierhealth.com/journals/ctrv Antitumour Treatment EGFR-mutated
Cancer Treatment Reviews 38 (2012) 416 430 Contents lists available at SciVerse ScienceDirect Cancer Treatment Reviews journal homepage: www.elsevierhealth.com/journals/ctrv Antitumour Treatment EGFR-mutated
REPORT PERSPECTIVES IN LUNG CANCER 2010 AMSTERDAM
 REPORT PERSPECTIVES IN LUNG CANCER 2010 AMSTERDAM Valerie Van Damme, Isabelle Wauters, Johan Vansteenkiste Univ. Hospital Leuven and Leuven Lung Cancer Group Introduction Perspectives in Lung Cancer (PILC)
REPORT PERSPECTIVES IN LUNG CANCER 2010 AMSTERDAM Valerie Van Damme, Isabelle Wauters, Johan Vansteenkiste Univ. Hospital Leuven and Leuven Lung Cancer Group Introduction Perspectives in Lung Cancer (PILC)
Lung Cancer: More than meets the eye
 Lung Cancer Education Program November 23, 2013 Lung Cancer: More than meets the eye Shantanu Banerji MD, FRCPC Presenter Disclosure Faculty: Shantanu Banerji Relationships with commercial interests: Grants/Research
Lung Cancer Education Program November 23, 2013 Lung Cancer: More than meets the eye Shantanu Banerji MD, FRCPC Presenter Disclosure Faculty: Shantanu Banerji Relationships with commercial interests: Grants/Research
Targeted agents in lung cancer: EGFR TKI and beyond
 Targeted agents in lung cancer: EGFR TKI and beyond David CL Lam, MBBS, PhD, MD, FCCP, FACP, FRCP, FAPSR Clinical Assistant Professor Department of Medicine University of Hong Kong 13 Nov, 2014 The Changing
Targeted agents in lung cancer: EGFR TKI and beyond David CL Lam, MBBS, PhD, MD, FCCP, FACP, FRCP, FAPSR Clinical Assistant Professor Department of Medicine University of Hong Kong 13 Nov, 2014 The Changing
Cáncer de Pulmón n con Mutación de EGFR: Una Entidad Clínica y Patológica Distinta
 Cáncer de Pulmón n con Mutación de EGFR: Una Entidad Clínica y Patológica Distinta Luis Paz-Ares Hospital Universitario Virgen del Rocio Seville, Spain Advanced NSCLC: chemotherapy has reached a therapeutic
Cáncer de Pulmón n con Mutación de EGFR: Una Entidad Clínica y Patológica Distinta Luis Paz-Ares Hospital Universitario Virgen del Rocio Seville, Spain Advanced NSCLC: chemotherapy has reached a therapeutic
The following information is only meant for people who have been diagnosed with advanced non-small cell
 Important information for people with advanced non-small cell lung cancer The following information is only meant for people who have been diagnosed with advanced non-small cell lung cancer (NSCLC). NSCLC
Important information for people with advanced non-small cell lung cancer The following information is only meant for people who have been diagnosed with advanced non-small cell lung cancer (NSCLC). NSCLC
Treatment Paradigm in NSCLC Treatment
 Treatment Paradigm in NSCLC Treatment Era of Targeted Therapy Aumkhae Sookprasert, MD Medicine Department, KKU Which factors taken to be account in NSCLC treatment? 1. Staging 2. ECOG performance status
Treatment Paradigm in NSCLC Treatment Era of Targeted Therapy Aumkhae Sookprasert, MD Medicine Department, KKU Which factors taken to be account in NSCLC treatment? 1. Staging 2. ECOG performance status
Lung Cancer Genomics and Patient Individualization
 Lung Cancer Genomics and Patient Individualization Ming Sound Tsao, MD, FRCPC Qasim Choksi Chair in Lung Cancer Translational Research University Health Network OCI/PMH Leading Causes of Deaths (WHO) In
Lung Cancer Genomics and Patient Individualization Ming Sound Tsao, MD, FRCPC Qasim Choksi Chair in Lung Cancer Translational Research University Health Network OCI/PMH Leading Causes of Deaths (WHO) In
Nuevas tecnologías basadas en biomarcadores para oncología
 Nuevas tecnologías basadas en biomarcadores para oncología Simposio ASEBIO 14 de marzo 2013, PCB Jose Jimeno, MD, PhD Co-Founder / Vice Chairman Pangaea Biotech SL Barcelona, Spain PANGAEA BIOTECH BUSINESS
Nuevas tecnologías basadas en biomarcadores para oncología Simposio ASEBIO 14 de marzo 2013, PCB Jose Jimeno, MD, PhD Co-Founder / Vice Chairman Pangaea Biotech SL Barcelona, Spain PANGAEA BIOTECH BUSINESS
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness
 Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness Investigators: Paul G. Shekelle, MD, PhD, Director Alicia R. Maher, MD Clinical
Treatment of Metastatic Non-Small Cell Lung Cancer: A Systematic Review of Comparative Effectiveness and Cost Effectiveness Investigators: Paul G. Shekelle, MD, PhD, Director Alicia R. Maher, MD Clinical
Pharmacogenomic Approaches. Luis Paz-Ares Hospital Universitario Virgen del Rocio Seville, Spain
 Pharmacogenomic Approaches Luis Paz-Ares Hospital Universitario Virgen del Rocio Seville, Spain Pharmacogenetics & Pharmacogenomics Medicine tailored to the individual Genetic information, including the
Pharmacogenomic Approaches Luis Paz-Ares Hospital Universitario Virgen del Rocio Seville, Spain Pharmacogenetics & Pharmacogenomics Medicine tailored to the individual Genetic information, including the
targeted therapy a guide for the patient
 targeted therapy FOR LUNG CANCER a guide for the patient TABLE OF CONTENTS lung cancer basics... 2-3 Gene changes... 4-5 Testing... 7-8 Targeted therapy... 9-11 Drugs Targeting EGFR... 12 Drugs Targeting
targeted therapy FOR LUNG CANCER a guide for the patient TABLE OF CONTENTS lung cancer basics... 2-3 Gene changes... 4-5 Testing... 7-8 Targeted therapy... 9-11 Drugs Targeting EGFR... 12 Drugs Targeting
Second-Line Therapy in Non Small-Cell Lung Cancer: The DELTA Between Different Genotypes Widens
 VOLUME 32 NUMBER 18 JUNE 20 2014 JOURNAL OF CLINICAL ONCOLOGY ONCOLOGY GRAND ROUNDS Second-Line Therapy in Non Small-Cell Lung Cancer: The DELTA Between Different Genotypes Widens Alona Zer and Natasha
VOLUME 32 NUMBER 18 JUNE 20 2014 JOURNAL OF CLINICAL ONCOLOGY ONCOLOGY GRAND ROUNDS Second-Line Therapy in Non Small-Cell Lung Cancer: The DELTA Between Different Genotypes Widens Alona Zer and Natasha
Genomic Medicine The Future of Cancer Care. Shayma Master Kazmi, M.D. Medical Oncology/Hematology Cancer Treatment Centers of America
 Genomic Medicine The Future of Cancer Care Shayma Master Kazmi, M.D. Medical Oncology/Hematology Cancer Treatment Centers of America Personalized Medicine Personalized health care is a broad term for interventions
Genomic Medicine The Future of Cancer Care Shayma Master Kazmi, M.D. Medical Oncology/Hematology Cancer Treatment Centers of America Personalized Medicine Personalized health care is a broad term for interventions
Evaluating the Efficiency of Targeted Designs for Randomized Clinical Trials
 Vol. 0, 6759 6763, October 5, 004 Clinical Cancer Research 6759 Perspective Evaluating the Efficiency of Targeted Designs for Randomized Clinical Trials Richard Simon and Aboubakar Maitournam Biometric
Vol. 0, 6759 6763, October 5, 004 Clinical Cancer Research 6759 Perspective Evaluating the Efficiency of Targeted Designs for Randomized Clinical Trials Richard Simon and Aboubakar Maitournam Biometric
The last decade has witnessed the dramatic coming
 Lung Cancer Pathology Changing paradigm and priorities Ming-Sound Tsao, MD, FRCPC Abstract The last decade has witnessed the dramatic coming of age of targeted therapy in lung cancer. Several new targeted
Lung Cancer Pathology Changing paradigm and priorities Ming-Sound Tsao, MD, FRCPC Abstract The last decade has witnessed the dramatic coming of age of targeted therapy in lung cancer. Several new targeted
Stato dell arte e prospettive delle terapie a bersaglio molecolare nel carcinoma polmonare
 Stato dell arte e prospettive delle terapie a bersaglio molecolare nel carcinoma polmonare Giorgio V. Scagliotti Università di Torino Dipartimento di scienze cliniche & biologiche giorgio.scagliotti@unito.it
Stato dell arte e prospettive delle terapie a bersaglio molecolare nel carcinoma polmonare Giorgio V. Scagliotti Università di Torino Dipartimento di scienze cliniche & biologiche giorgio.scagliotti@unito.it
Targeted therapies and brain metastases in lung cancer patients. Benjamin Besse, MD, PhD. Medical Oncologist. 19 septembre 2014
 Targeted therapies and brain metastases in lung cancer patients Benjamin Besse, MD, PhD Medical Oncologist 19 septembre 2014 Targeted therapies and brain mets! Brain mets in NSCLC! Specific targeted therapies!
Targeted therapies and brain metastases in lung cancer patients Benjamin Besse, MD, PhD Medical Oncologist 19 septembre 2014 Targeted therapies and brain mets! Brain mets in NSCLC! Specific targeted therapies!
Developments in Biomarker Identification and Validation for Lung Cancer
 Developments in Biomarker Identification and Validation for Lung Cancer Alexandre Passioukov, MD, PhD Alexandre.Passioukov@eortc.be Contents Introduction Lung cancer pathogenesis NSCLC treatment options
Developments in Biomarker Identification and Validation for Lung Cancer Alexandre Passioukov, MD, PhD Alexandre.Passioukov@eortc.be Contents Introduction Lung cancer pathogenesis NSCLC treatment options
Thorakale Onkologie. ASCO 2013 Aktuelle Studien TZ Berlin Buch 12.6.2013
 Triple negativ Thorakale Onkologie ASCO 2013 Aktuelle Studien TZ Berlin Buch 12.6.2013 Driver Oncogene Mutations in non sq-nsclc Genome Res. 2012 November; 22(11): 2109 2119 8021: Detection of EGFR-activating
Triple negativ Thorakale Onkologie ASCO 2013 Aktuelle Studien TZ Berlin Buch 12.6.2013 Driver Oncogene Mutations in non sq-nsclc Genome Res. 2012 November; 22(11): 2109 2119 8021: Detection of EGFR-activating
Understanding series. new. directions. 1-800-298-2436 LungCancerAlliance.org. A guide for the patient
 Understanding series LUNG CANCER: new treatment directions 1-800-298-2436 LungCancerAlliance.org A guide for the patient TABLE OF CONTENTS What s New in lung cancer? Advancements...4 Changes in genes that
Understanding series LUNG CANCER: new treatment directions 1-800-298-2436 LungCancerAlliance.org A guide for the patient TABLE OF CONTENTS What s New in lung cancer? Advancements...4 Changes in genes that
Prognostic and Predictive Factors in Oncology. Mustafa Benekli, M.D.
 Prognostic and Predictive Factors in Oncology Mustafa Benekli, M.D. NCI Definitions ESMO Course -Essentials of Medical Oncology -Istanbul 2 Prognostic factor: NCI Definition A situation or condition, or
Prognostic and Predictive Factors in Oncology Mustafa Benekli, M.D. NCI Definitions ESMO Course -Essentials of Medical Oncology -Istanbul 2 Prognostic factor: NCI Definition A situation or condition, or
Follow this and additional works at: http://digitalcommons.wustl.edu/open_access_pubs
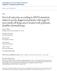 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Survival outcome according to KRAS mutation status in newly diagnosed patients with stage IV non-small cell
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Survival outcome according to KRAS mutation status in newly diagnosed patients with stage IV non-small cell
Mechanisms of primary/secondary resistance to EGFR inhibitors
 UNIVERSITY OF OF TORINO DEPARTMENT OF ONCOLOGY Mechanisms of primary/secondary resistance to EGFR inhibitors Silvia Novello University of Torino Italy Department of Oncology silvia.novello@unito.it www.womengainstlungcancer.eu
UNIVERSITY OF OF TORINO DEPARTMENT OF ONCOLOGY Mechanisms of primary/secondary resistance to EGFR inhibitors Silvia Novello University of Torino Italy Department of Oncology silvia.novello@unito.it www.womengainstlungcancer.eu
Cetuximab (Erbitux) MM.04.005 05/10/2005. HMO; PPO; QUEST Integration 01/01/2015 Section: Prescription Drugs Place(s) of Service: Office: Outpatient
 Cetuximab (Erbitux) Policy Number: Original Effective Date: MM.04.005 05/10/2005 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2015 Section: Prescription Drugs Place(s)
Cetuximab (Erbitux) Policy Number: Original Effective Date: MM.04.005 05/10/2005 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2015 Section: Prescription Drugs Place(s)
Public-Private Partnerships in early phase clinical research: Spurring access to innovative therapeutics
 EPAAC WP8 Research Forum - 2 July, Sofitel Hotel Europe, Brussels Public-Private Partnerships in early phase clinical research: Spurring access to innovative therapeutics JY Blay, Past President EORTC
EPAAC WP8 Research Forum - 2 July, Sofitel Hotel Europe, Brussels Public-Private Partnerships in early phase clinical research: Spurring access to innovative therapeutics JY Blay, Past President EORTC
CLINICAL POLICY Department: Medical Management Document Name: Opdivo Reference Number: CP.PHAR.121 Effective Date: 07/15
 Page: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Page: 1 of 6 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Protocol. Molecular Analysis for Targeted Therapy of Non-Small- Cell Lung Cancer
 Molecular Analysis for Targeted Therapy of Non-Small- Cell Lung (20445) (Formerly Epidermal Growth Factor Receptor [EGFR] Mutation Analysis for Patients with Non-Small Cell Lung [NSCLC] and KRAS Mutation
Molecular Analysis for Targeted Therapy of Non-Small- Cell Lung (20445) (Formerly Epidermal Growth Factor Receptor [EGFR] Mutation Analysis for Patients with Non-Small Cell Lung [NSCLC] and KRAS Mutation
Pulmonary and Critical Care Regional Symposium April 25, 2015
 Pulmonary and Critical Care Regional Symposium April 25, 2015 2015: Molecular Medicine, Resistance Mutations and Immunotherapy. Keeping Up With The Latest in NSCLC Barbara J. Gitlitz MD Associate Professor
Pulmonary and Critical Care Regional Symposium April 25, 2015 2015: Molecular Medicine, Resistance Mutations and Immunotherapy. Keeping Up With The Latest in NSCLC Barbara J. Gitlitz MD Associate Professor
Targeted Treatment and Molecular Biomarkers in Lung Cancer
 Targeted Treatment and Molecular Biomarkers in Lung Cancer Ming Sound Tsao, MD, FRCPC Choksi Chair in Lung Cancer Translational Research Princess Margaret Hospital University of Toronto Uppsula, September
Targeted Treatment and Molecular Biomarkers in Lung Cancer Ming Sound Tsao, MD, FRCPC Choksi Chair in Lung Cancer Translational Research Princess Margaret Hospital University of Toronto Uppsula, September
REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group
 REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group In the 2002 edition of the ASCO meeting, a total of 315 abstracts in the field of respiratory
REPORT ASCO 2002 ORLANDO : LUNG CANCER Johan F. Vansteenkiste, MD, PhD, Univ. Hospital and Leuven Lung Cancer Group In the 2002 edition of the ASCO meeting, a total of 315 abstracts in the field of respiratory
Ovarian Cancer and Modern Immunotherapy: Regulatory Strategies for Drug Development
 Ovarian Cancer and Modern Immunotherapy: Regulatory Strategies for Drug Development Sanjeeve Bala, MD, MPH Ovarian Cancer Endpoints Workshop FDA White Oak September 3, 2015 Overview Immune agents from
Ovarian Cancer and Modern Immunotherapy: Regulatory Strategies for Drug Development Sanjeeve Bala, MD, MPH Ovarian Cancer Endpoints Workshop FDA White Oak September 3, 2015 Overview Immune agents from
Sur les nouveaux médicaments et les perspectives qu ils offrent (traitement à la carte et survie longue)
 Sur les nouveaux médicaments et les perspectives qu ils offrent (traitement à la carte et survie longue) Professeur Jean Trédaniel Unité de cancérologie thoracique Hôpital Saint-Louis Comparison of Four
Sur les nouveaux médicaments et les perspectives qu ils offrent (traitement à la carte et survie longue) Professeur Jean Trédaniel Unité de cancérologie thoracique Hôpital Saint-Louis Comparison of Four
Treatment Paradigms in Advanced Non Small-Cell Lung Cancer
 Treatment Paradigms in Advanced Non Small-Cell Lung Cancer Caroline E. McCoach, MD, PhD, and Karen Kelly, MD Dr McCoach is a clinical research fellow and Dr Kelly is a professor of medicine, an associate
Treatment Paradigms in Advanced Non Small-Cell Lung Cancer Caroline E. McCoach, MD, PhD, and Karen Kelly, MD Dr McCoach is a clinical research fellow and Dr Kelly is a professor of medicine, an associate
REFERENCE CODE GDHC212DFR PUBLICAT ION DATE JUNE 2013 GSK1572932A (NON-SMALL CELL LUNG CANCER) FORECAST AND MARKET ANALYSIS TO 2022
 REFERENCE CODE GDHC212DFR PUBLICAT ION DATE JUNE 2013 GSK1572932A (NON-SMALL CELL LUNG CANCER) GSK1572932A (NON-SMALL CELL LUNG CANCER) - Executive Summary GSK1572932A (MAGE-A3): Key Metrics in NSCLC Markets
REFERENCE CODE GDHC212DFR PUBLICAT ION DATE JUNE 2013 GSK1572932A (NON-SMALL CELL LUNG CANCER) GSK1572932A (NON-SMALL CELL LUNG CANCER) - Executive Summary GSK1572932A (MAGE-A3): Key Metrics in NSCLC Markets
Piano Generale di Emergenza Presidio Ospedaliero di Livorno Viale Alfieri 36
 Aprile 2011 EGFR-TKIs for the treatment of advanced NSCLC with EGFR mutations Piano Generale di Emergenza Presidio Ospedaliero di Livorno Viale Alfieri 36 Federico Cappuzzo Istituto Toscano Tumori Ospedale
Aprile 2011 EGFR-TKIs for the treatment of advanced NSCLC with EGFR mutations Piano Generale di Emergenza Presidio Ospedaliero di Livorno Viale Alfieri 36 Federico Cappuzzo Istituto Toscano Tumori Ospedale
Rapid Review: EGFR gene mutation testing in patients with advanced NSCLC for access to Gefitinib for sector discussion
 Rapid Review: EGFR gene mutation testing in patients with advanced NSCLC for access to Gefitinib for sector discussion June 2012 Key words: NSCLC, EGFR, EGFR-TKIs, New Zealand situation, personalised testing,
Rapid Review: EGFR gene mutation testing in patients with advanced NSCLC for access to Gefitinib for sector discussion June 2012 Key words: NSCLC, EGFR, EGFR-TKIs, New Zealand situation, personalised testing,
Targeting angiogenesis in NSCLC: Clinical trial update Martin Reck Lung Clinic Grosshansdorf Grosshansdorf, Germany
 Targeting angiogenesis in NSCLC: Clinical trial update Martin Reck Lung Clinic Grosshansdorf Grosshansdorf, Germany This presentation was selected by the 15 th World Conference on Lung Cancer Program Committee
Targeting angiogenesis in NSCLC: Clinical trial update Martin Reck Lung Clinic Grosshansdorf Grosshansdorf, Germany This presentation was selected by the 15 th World Conference on Lung Cancer Program Committee
How To Treat Lung Cancer With Gefitinib
 Lung Cancer 71 (2011) 249 257 Contents lists available at ScienceDirect Lung Cancer journal homepage: www.elsevier.com/locate/lungcan Review Gefitinib as first-line treatment for patients with advanced
Lung Cancer 71 (2011) 249 257 Contents lists available at ScienceDirect Lung Cancer journal homepage: www.elsevier.com/locate/lungcan Review Gefitinib as first-line treatment for patients with advanced
SYSTEMIC THERAPY FOR STAGE IV NON-SMALL CELL LUNG CANCER: AMERICAN SOCIETY OF CLINICAL ONCOLOGY CLINICAL PRACTICE GUIDELINE UPDATE
 Which patients with stage IV NSCLC should be treated with chemotherapy? NSCLC with nonsquamous cell carcinoma, negative or unknown EGFR-sensitizing mutation and ALK gene rearrangement status, and PS 0-1
Which patients with stage IV NSCLC should be treated with chemotherapy? NSCLC with nonsquamous cell carcinoma, negative or unknown EGFR-sensitizing mutation and ALK gene rearrangement status, and PS 0-1
Corporate Medical Policy
 Corporate Medical Policy Ado-Trastuzumab Emtansine (Trastuzumab-DM1) for Treatment of File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ado_trastuzumab_emtansine_(trastuzumab-dm1)_for_treatment_of_her-2_positivemalignancies
Corporate Medical Policy Ado-Trastuzumab Emtansine (Trastuzumab-DM1) for Treatment of File Name: Origination: Last CAP Review: Next CAP Review: Last Review: ado_trastuzumab_emtansine_(trastuzumab-dm1)_for_treatment_of_her-2_positivemalignancies
Treatment of Stage IV Non-small Cell Lung Cancer
 CHEST Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER, 3RD ED: ACCP GUIDELINES Treatment of Stage IV Non-small Cell Lung Cancer Diagnosis and Management of Lung Cancer, 3rd ed: American College of Chest
CHEST Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER, 3RD ED: ACCP GUIDELINES Treatment of Stage IV Non-small Cell Lung Cancer Diagnosis and Management of Lung Cancer, 3rd ed: American College of Chest
Update on Targeted Therapies of NSCLC
 Update on Targeted Therapies of NSCLC Tanja Cufer, MD, PhD University Clinic Golnik Medical Faculty Ljubljana, Slovenia Bled 2014 1 Systemic Therapy of Advanced NSCLC: Chemotherapy Range Cht improves survival
Update on Targeted Therapies of NSCLC Tanja Cufer, MD, PhD University Clinic Golnik Medical Faculty Ljubljana, Slovenia Bled 2014 1 Systemic Therapy of Advanced NSCLC: Chemotherapy Range Cht improves survival
Lung Cancer Research: From Prevention to Cure!
 Lung Cancer Research: From Prevention to Cure! Ravi Salgia, M.D, Ph.D Associate Professor of Medicine Director, Thoracic Oncology Research Program Department of Medicine Section of Hematology/Oncology
Lung Cancer Research: From Prevention to Cure! Ravi Salgia, M.D, Ph.D Associate Professor of Medicine Director, Thoracic Oncology Research Program Department of Medicine Section of Hematology/Oncology
To Treat or Not to Treat: When Is Adjuvant EGFR TKI Therapy Appropriate?
 To Treat or Not to Treat: When Is Adjuvant EGFR TKI Therapy Appropriate? Ramsey Asmar, MD, and Balazs Halmos, MD Abstract The use of epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor (TKI)
To Treat or Not to Treat: When Is Adjuvant EGFR TKI Therapy Appropriate? Ramsey Asmar, MD, and Balazs Halmos, MD Abstract The use of epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor (TKI)
Managing Acquired Resistance in EGFR- Mutated Non Small Cell Lung Cancer
 Managing Acquired Resistance in EGFR- Mutated Non Small Cell Lung Cancer Patrick M. Forde, MD, and David S. Ettinger, MD The authors are affiliated with the Johns Hopkins Sidney Kimmel Comprehensive Cancer
Managing Acquired Resistance in EGFR- Mutated Non Small Cell Lung Cancer Patrick M. Forde, MD, and David S. Ettinger, MD The authors are affiliated with the Johns Hopkins Sidney Kimmel Comprehensive Cancer
REPORT ASCO 2011 CHICAG0 : RESPIRATORY ONCOLOGY Johan Vansteenkiste / Christophe Dooms, Univ. Hospital Leuven and Leuven Lung Cancer Group
 1 REPORT ASCO 2011 CHICAG0 : RESPIRATORY ONCOLOGY Johan Vansteenkiste / Christophe Dooms, Univ. Hospital Leuven and Leuven Lung Cancer Group 10 MESSAGE HIGHLIGHTS Early stage non-small cell lung cancer
1 REPORT ASCO 2011 CHICAG0 : RESPIRATORY ONCOLOGY Johan Vansteenkiste / Christophe Dooms, Univ. Hospital Leuven and Leuven Lung Cancer Group 10 MESSAGE HIGHLIGHTS Early stage non-small cell lung cancer
SEARCH METHODOLOGY SEARCH STRATEGY #1 (SYSTEMATIC REVIEWS): PubMed 1966-3/16/2012 Cochrane Database of Systematic Reviews All years
 Appendix A. Search Strategy for Systematic Reviews and Cost-Effectiveness Analyses (Search #1) TREATMENT OF METASTATIC NON-SMALL-CELL LUNG CANCER SEARCH METHODOLOGY SEARCH STRATEGY #1 (SYSTEMATIC REVIEWS):
Appendix A. Search Strategy for Systematic Reviews and Cost-Effectiveness Analyses (Search #1) TREATMENT OF METASTATIC NON-SMALL-CELL LUNG CANCER SEARCH METHODOLOGY SEARCH STRATEGY #1 (SYSTEMATIC REVIEWS):
Current Progress for Non-Small Cell Lung Cancer Treatment
 Chemotherapy : Mechanisms of Action Current Progress for Non-Small Cell Lung Cancer Treatment Topo inhibitors Alkylators CHR Tubulin active agents Topo I,II Pt Wen-Pin Su, M.D./ Prof. Wu-Chou Su National
Chemotherapy : Mechanisms of Action Current Progress for Non-Small Cell Lung Cancer Treatment Topo inhibitors Alkylators CHR Tubulin active agents Topo I,II Pt Wen-Pin Su, M.D./ Prof. Wu-Chou Su National
Avastin in breast cancer: Summary of clinical data
 Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Avastin in breast cancer: Summary of clinical data Worldwide, over one million people are diagnosed with breast cancer every year 1. It is the most frequently diagnosed cancer in women 1,2, and the leading
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VI. THERAPY. III. TARGETED THERAPY FOR NON SMALL CELL LUNG CANCER Prof.
 Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VI. THERAPY. III. TARGETED THERAPY FOR NON SMALL CELL LUNG CANCER Prof. Alberto Riccardi Targeted therapies. I. Signaling pathways
Corso Integrato di Clinica Medica ONCOLOGIA MEDICA AA 2010-2011 LUNG CANCER. VI. THERAPY. III. TARGETED THERAPY FOR NON SMALL CELL LUNG CANCER Prof. Alberto Riccardi Targeted therapies. I. Signaling pathways
Summary ID# 13095. Clinical Study Summary: Study H3E-EW-B012
 Page 1 Summary ID# 13095 Clinical Study Summary: Study H3E-EW-B012 First-line Treatment of Non-Small Cell Lung Cancer under Routine Conditions: Observational Study on Overall Survival Date summary electronically
Page 1 Summary ID# 13095 Clinical Study Summary: Study H3E-EW-B012 First-line Treatment of Non-Small Cell Lung Cancer under Routine Conditions: Observational Study on Overall Survival Date summary electronically
National Medical Policy
 National Medical Policy Subject: Policy Number: Molecular Tumor Markers for Non-Small Cell Lung Cancer (NSCLC) NMP206 Effective Date*: November 2010 Update: June 2015 This National Medical Policy is subject
National Medical Policy Subject: Policy Number: Molecular Tumor Markers for Non-Small Cell Lung Cancer (NSCLC) NMP206 Effective Date*: November 2010 Update: June 2015 This National Medical Policy is subject
Chemotherapy in Advanced Non-Small Cell Lung Cancer: Optimal Treatment Approach for Elderly and Patients With Poor Performance Status
 Chemotherapy in Advanced Non-Small Cell Lung Cancer: Optimal Treatment Approach for Elderly and Patients With Poor Performance Status Tracey L. Evans, MD Abstract In spite of advances in molecular profiling
Chemotherapy in Advanced Non-Small Cell Lung Cancer: Optimal Treatment Approach for Elderly and Patients With Poor Performance Status Tracey L. Evans, MD Abstract In spite of advances in molecular profiling
Zeroing in on Non-Small Cell Lung Cancer: Integrating Targeted Therapies into Practice
 Lung Cancer: Integrating Targeted Therapies into Practice Table of Contents Program Information... 2 Faculty Biographies... 3 Genomic Profiling of NSCLC for EGFR Inhibitors... 4 Fred R. Hirsch, MD, PhD
Lung Cancer: Integrating Targeted Therapies into Practice Table of Contents Program Information... 2 Faculty Biographies... 3 Genomic Profiling of NSCLC for EGFR Inhibitors... 4 Fred R. Hirsch, MD, PhD
Miquel Àngel Seguí Palmer
 Miquel Àngel Seguí Palmer HER2+ Breast Cancer is characterized by overexpression of HER2 receptors HER2+ Breast Cancer is characterized by overexpression of HER2 receptors HER2+ status is associated with
Miquel Àngel Seguí Palmer HER2+ Breast Cancer is characterized by overexpression of HER2 receptors HER2+ Breast Cancer is characterized by overexpression of HER2 receptors HER2+ status is associated with
Biomarker Trends in Breast Cancer Research
 WHITE PAPER Biomarker Trends in Breast Cancer Research Jason Hill, PhD, Associate Director, External Science Affairs, Quintiles Quintiles examines the novel drug combinations and mechanisms of action that
WHITE PAPER Biomarker Trends in Breast Cancer Research Jason Hill, PhD, Associate Director, External Science Affairs, Quintiles Quintiles examines the novel drug combinations and mechanisms of action that
Systemic Therapy for Stage IV Non-Small Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Update
 Systemic Therapy for Stage IV Non-Small Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Update Introduction The purpose of this guideline update is to revise the 2011
Systemic Therapy for Stage IV Non-Small Cell Lung Cancer: American Society of Clinical Oncology Clinical Practice Guideline Update Introduction The purpose of this guideline update is to revise the 2011
HER2 Status: What is the Difference Between Breast and Gastric Cancer?
 Ask the Experts HER2 Status: What is the Difference Between Breast and Gastric Cancer? Bharat Jasani MBChB, PhD, FRCPath Marco Novelli MBChB, PhD, FRCPath Josef Rüschoff, MD Robert Y. Osamura, MD, FIAC
Ask the Experts HER2 Status: What is the Difference Between Breast and Gastric Cancer? Bharat Jasani MBChB, PhD, FRCPath Marco Novelli MBChB, PhD, FRCPath Josef Rüschoff, MD Robert Y. Osamura, MD, FIAC
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER
 GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
GUIDELINES FOR THE MANAGEMENT OF LUNG CANCER BY Ali Shamseddine, MD (Coordinator); as04@aub.edu.lb Fady Geara, MD Bassem Shabb, MD Ghassan Jamaleddine, MD CLINICAL PRACTICE GUIDELINES FOR THE TREATMENT
Lung cancer remains the leading cause of cancer-related death in the. Evolving Treatment Paradigms in Non-Small Cell Lung Cancer
 PRINTER-FRIENDLY VERSION AT CLINICALONCOLOGY.COM Evolving Treatment Paradigms in Non-Small Cell Lung Cancer KATHRYN F. MILEHAM, MD Staff Oncologist HEATHER D. BROOKS, MD Staff Oncologist EDWARD S. KIM,
PRINTER-FRIENDLY VERSION AT CLINICALONCOLOGY.COM Evolving Treatment Paradigms in Non-Small Cell Lung Cancer KATHRYN F. MILEHAM, MD Staff Oncologist HEATHER D. BROOKS, MD Staff Oncologist EDWARD S. KIM,
Cancer Treatments Subcommittee of PTAC Meeting held 2 March 2012. (minutes for web publishing)
 Cancer Treatments Subcommittee of PTAC Meeting held 2 March 2012 (minutes for web publishing) Cancer Treatments Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Cancer Treatments Subcommittee of PTAC Meeting held 2 March 2012 (minutes for web publishing) Cancer Treatments Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Activity of pemetrexed in thoracic malignancies
 Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
Activity of pemetrexed in thoracic malignancies Results of phase III clinical studies of pemetrexed in malignant pleural mesothelioma and non-small cell lung cancer show benefit P emetrexed (Alimta) is
EGFR MUTATIONS IN NON-SMALL CELL LUNG CANCER: LOCAL EPIDEMIOLOGY AND CLINICAL IMPORTANCE
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2015 vol. 119, no. 4 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS EGFR MUTATIONS IN NON-SMALL CELL LUNG CANCER: LOCAL EPIDEMIOLOGY AND CLINICAL IMPORTANCE F. Rusu-Cordunean
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2015 vol. 119, no. 4 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS EGFR MUTATIONS IN NON-SMALL CELL LUNG CANCER: LOCAL EPIDEMIOLOGY AND CLINICAL IMPORTANCE F. Rusu-Cordunean
non-small-cell lung cancer Quimioterapia adjuvante para câncer de pulmão não pequenas
 Adjuvant chemotherapy for non-small-cell lung cancer Quimioterapia adjuvante para câncer de pulmão não pequenas células Daniel B. Costa, MD, PhD, MMSc Division i i of Hematology/Oncology l Beth Israel
Adjuvant chemotherapy for non-small-cell lung cancer Quimioterapia adjuvante para câncer de pulmão não pequenas células Daniel B. Costa, MD, PhD, MMSc Division i i of Hematology/Oncology l Beth Israel
Management of stage III A-B of NSCLC. Hamed ALHusaini Medical Oncologist
 Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
Management of stage III A-B of NSCLC Hamed ALHusaini Medical Oncologist Global incidence, CA cancer J Clin 2011;61:69-90 Stage III NSCLC Includes heterogeneous group of patients with differences in the
