Utah State Hospital Nursing Policy and Procedure Manual
|
|
|
- Lillian Gibbs
- 8 years ago
- Views:
Transcription
1 Nursing Policy and Procedure Manual Page 1 Utah State Hospital Nursing Policy and Procedure Manual Table of Contents Chapter 1: Patient Assessment Section 1: Patient Admissions Section 2: Nursing Process Section 3: Nursing Assessment Section 4: Monthly Patient Vital Signs and Weights Section 5: Patient Care Assignments Section 6: Role of Nursing in Patient and Family Education Section 7: Rehabilitative Nursing Care Section 8: Patient Falls Chapter 2: Patient Management Section 1: Caffeine Consumption Section 2 Central Line Management and Protocol (CVAD) Section 3: Care of Enteral Feeding Bags Section 4: Gift Exchanges between Patients and Employees Section 5: Diabetic Guidelines Protocol Section 6: Use of Glucometer Section 7: Directions on Use of the Accu-Chek Inform Glucometer: Section 8: Performing the Control Tests on Accu-Chek Inform Glucometer: Section 9: Glucometer Testing Section 10: Home Visits Section 11: Post-Serious Incident Debriefing Section 12: ARJO Maxilift Protocol Section 13: Return of a Patient Following Medical Separation Section 14: Off Unit Activities Section 15: Notification of On-Call Personnel Section 16: Pass Structure Section 17: Disposition of Patients Personal Property Section 18: Post-Operative Patient Care Protocol Section 19: Oxygen Administration Section 20: Oxygen Saturation Monitor Protocol Section 21: Oxygen Concentrator Protocol Section 22: Oxygen Tank Protocol Section 23: Patient & Patient Living Area Search Section 24: Smoking Section 25: Sore Throat Section 26: Braun Thermoscan Thermometer Protocol Section 27: Care of Urinary Drainage Bags Protocol Section 28: Videotaping and Recording of Patients Section 29: Visitors Section 30: Weights Protocol Section 31: Skin Integrity
2 Nursing Policy and Procedure Manual Page 2 Chapter 3: Medication Section 1: Medications on Day Trips and Camp Trips Section 2: After-Hours Drug Cabinet Section 3: Controlled Substances Section 4: Care of Hep Lock (Saline Caps) IV's Section 5: IV Therapy Certification Section 6: Intravenous Therapy Section 7: Administration of Medications Section 8: Ordering Medications from the Pharmacy Section 9: Reordering Medications from the Pharmacy Section 10: Medication Storage on the Unit Section 11: Transcription of Medication Orders Section 12: Mixing Medications in IV Solutions Section 13: Multi-Dose Vials Section 14: Crash Carts Section 15: Medication for RN Administration Only Section 16: Self-Medication Section 17: Psychotropic Medications & Physical Illness Section 18: Medications for Home Visits, Court Visits or Discharge Section 19: Transcription of Treatment Orders Chapter 4: Emergency Services Section 1: Suspected Rape & Physical Abuse Section 2: Anaphylaxis Protocol Section 3: Human Bite Protocol Section 4: Treatment of Hemorrhage Section 5: Emergency Burn Care Section 6: Code 10 Emergencies Section 7: Code Blue Emergencies Section 8: Orange Emergency Bag Section 9: Emergency Supplies Section 10: Cardiopulmonary Resuscitation Section 11: Use of Automated External Defibrillator ( Aed ) Section 12: Withholding Resuscitative Services Section 13: Treatment of Electrical Shock Section 14: Hanging Incidents Protocol Section 15: Calling Paramedics Directly Section 16: Poison Control: Treatment of Poison Ingestion and Overdose Section 17: Seizure Protocol Section 18: Use of Oronasopharyngeal Suctioning Section 19: Re-Feeding Protocol Chapter 5: Infection Control & Isolation Techniques (See Infection Control Manual) Chapter 6: Personnel Management & Nursing Administration Section 1: Internal Bidding Procedures Section 2: Collaboration with Nursing Schools Section 3: Nursing Personnel Files Section 4: Continuing Education Section 5: Role of Nursing as a Part of Executive Staff Section 6: Family Members at Work Section 7: Fiscal Management Section 8: Grooming and Dress Standards Section 9: Licensure Requirements
3 Nursing Policy and Procedure Manual Page 3 Section 10: New Employee Orientation Section 11: Use of Overtime Protocol Section 12: Official Communication Section 13: Patient Acuity Section 14: Retention and Recruitment of RN s & LPN s Section 15: Vehicle Use Section 16: RN Duties Section 17: Psychiatric Technician Job Description Section 18: Psychiatric Technician/Environmentalist Job Description Section 19: Psychiatric Technician Mentor Job Description Section 20: Licensed Practical Nurse Job Description Section 21: Director of Nursing Job Description Section 22: Nurse Executive Job Description Section 23: Assistant Director of Nursing Job Description Section 24: Clinical Nurse Specialist Job Description Section 25: Infection Control Coordinator Job Description Section 26: Staff Registered Nurse Job Description Section 27: Staffing Coordinator Job Description Section 28: Unit Nursing Director Job Description Section 29: Shift Supervising Registered Nurse Job Description Section 30: Unit Clerk Job Description Section 31: Scheduling Protocol Section 32: Scheduling and Shift Differential Section 33: Requesting Vacation and Time Off Section 34: Sexual Misconduct between Patient and Staff Section 35: Staffing Section 36: Staffing Patterns Chapter 7: Safety Section 1: Section 2: Section 3: Section 4: Section 5: Section 6: Section 7: Section 8: Section 9: Section 10: Section 11: Section 12: Elopement Body Mechanics Employee Medications Fire Evacuation Plan Refrigerator Checklist Keys Medication/Treatment Room Checklist Census Verification/Patient Roll Patient, Employee, and Visitor Safety Violence Prevention Employee Theft or Financial Impropriety Tarasoff Warning Chapter 8: Documentation Section 1: Legal Aspects of Charting Section 2: Confidentiality Section 3: Role of the Nurse in Discharge Planning Section 4: Physician s Orders Section 5: Nursing Care Plans Section 6: Nursing Orders Section 7: Patient Progress Notes
4 Nursing Policy and Procedure Manual Page 4 Chapter 9: Special Treatment Procedures Section 1: Medication of Adult Patients Section 2: Less Restrictive Alternatives to Restraint and Seclusion Section 3: Restraint and Seclusion Section 4: Use of Medical Protective Devices Section 5: Use of Medical Protective Device Protocol Section 6: Restrictions and Limitations of Patient Rights Section 7: Levels of Suicide Precautions Chapter 10: Co-Ordination of Care Section 1: Ekg Protocol Section 2: Lab Work Protocol Section 3: Sending Lab Requests to IHC Laboratory Protocol Section 4: Clozaril Protocol Section 5: Atypical Antipsychotic Medications Protocol Section 6: Coumadin Protocol Section 7: Depakote Protocol Section 8: Dilantin Protocol Section 9: Lithium Protocol Section 10: Tegretol Protocol Section 11: Prolactin Levels Section 12: Quickvue One-Step Strep A Test Section 13: Audiology Clinic Section 14: Dental Clinic--Admission Dental Exams Section 15: Dental Clinic--Radiologic Exposures & Safety Section 16: Dental Clinic--Dental Surgery Post-Operative Instructions Section 17: Dental Appointments Protocol Section 18: Dietary Services--Obtaining Dietary Services Section 19: Dietary Services--Drug/Food Interaction Counseling for Patients Section 20: Dietary Services--Guest Trays Section 21: Dietary Services--Provision of Punch and Other Supplies Used for Administering Medication Section 22: Dietary Services--NPO Orders Section 23: Neurology & EEG Clinics Section 24: Physical Therapy Section 25: Podiatry and Optometry Clinics Section 26: Purchasing Dentures, Orthotics, or Other Appliances Section 27: Purchasing Eyeglasses Section 28: Care of Contact Lenses Section 29: Radiology Section 30: Patient Condition Report Section 31: Patient Preps for Procedures at UVRMC - Colon (Barium Enema) or Colon with Air Section 32: Patient Preps for Procedures at UVRMC - Renal, Visceral, or Pelvic Angiogram Section 33: Patient Preps for Procedures at UVRMC - Upper GI Preparation Section 34: Patient Preps for Procedures at UVRMC - I.V.P. (Adult) Section 35: Patient Preps for Procedures at UVRMC Section 36: Speech and Language Assessments Section 37: Access to Warehouse Supplies Section 38: Accessing Medical Supplies and Pumps Section 39: Volunteers Section 40: Retention and Destruction of Nursing Services Documentation
5 Nursing Policy and Procedure Manual Page 5 Section 41: Facility Planning and Administration Section 42: Ethical Concerns Section 43: Utah State Hospital Statement of Patient Rights Section 44: Common Definitions Chapter 11: Plan for Services Section 1: Philosophy and Framework
6 Nursing Policy and Procedure Manual Page 6 Chapter 1: Patient Assessment Section 1: Patient Admissions Policy The Nurse Executive or designee participates in the hospital admissions system to coordinate patient requirements for nursing care with available nursing resources. Procedure 1. Patients with exceptional medical problems requiring nursing care beyond the reasonable capability of Utah State Hospital are not eligible for admission (see USHOPP - Admissions Section 1 subsection 3.2). 1.1 The Director of Medical Services and the Hospital Clinical Director in collaboration with Nursing Administration determine when this situation exists by conducting an individualized review of each referred case. The review includes Current psychiatric condition of the patient Current medical and nursing needs of the patient Determination of the best treatment facility for the patient using guidelines, policies, information, and personnel from Utah State Hospital, the Utah State Division of Substance Abuse and Mental Health, and other appropriate involved agencies. 2. Admissions to the Children's and Adolescent Units are done through collaborative conferences between the Unit Clinical Director, Service Administrative Director, the Unit Supervising RN and other treatment staff. 3. When a specific unit's nursing staff is unable to assess and meet the patient's nursing care needs due to inadequate nursing resources, Nursing Administration conveys this information to the Hospital Clinical Director and Superintendent who then discuss with the Hospital Admissions Officer the need to limit admissions to the specific unit. 1/91; 9/93, 1/94; 4/98; 8/01; 1/05; 2/07 admiss.pol
7 Nursing Policy and Procedure Manual Page 7 Chapter 1: Patient Assessment Section 2: Nursing Process Policy The nursing process is utilized to aid in determining the patient needs and plan of care for all patients at Utah State Hospital. Registered Nurses at Utah State Hospital prescribe, delegate and coordinate nursing care for patients based upon individual need. Procedure 1. Patient needs are identified and the plan of care is determined through the nursing process. 1.1 Assessment of patient needs 1.2 Diagnosis/problem identification through analysis and synthesis of data 1.3 Development of plan of care including priorities, goals, strategies and nursing orders 1.4 Implementation of plan of care 1.5 Evaluation of patient outcome 2. A Registered Nurse prescribes, delegates and coordinates nursing care for each patient based upon: 2.1 Assessment data and other relevant information 2.2 Identified needs 2.3 Standards of care 2.4 Appropriate nursing interventions 2.5 Establishing policies and procedures 2.6 The nurse's professional judgment 2.7 The patient's response to specific nursing interventions 3. The nursing process is part of a dynamic cycle: evaluation of patient care is followed up by a re-assessment of patient needs to determine whether or not the plan of care requires modification. 3.1 This process is completed whenever the patient s condition changes significantly. 3.2 The process is a part of the re-assessment of the patient s individualized treatment plan every 30 days.
8 Nursing Policy and Procedure Manual Page 8 4. Nursing care is a part of the individual comprehensive treatment plan which is developed by the multidisciplinary team. 01/88; 1/91; 9/93; 1/94; 4/98; 5/01; 2/05; 2/07 nsgproc.pol
9 Nursing Policy and Procedure Manual Page 9 Chapter 1: Patient Assessment Section 3: Nursing Assessment Policy A nursing assessment is completed on all patients admitted to the Utah State Hospital. The nursing process, (assessment, planning, intervention, evaluation), is used to help determine the patient's needs and plan of care. Procedure 1. All patients admitted to the hospital have a nursing assessment completed within the shift on which they are admitted, (no later than eight hours after admission). 1.1 The Nursing Assessment includes: Health Assessment and History Falls Risk Assessment Medical History Allergies/Adverse Drug Reactions Special Care Needs Environmental Safety Nutrition/Dietary Screen Infectious Disease Screen OT/Voc Rehab Screen Dental Screen Educational Needs/Learning Preferences Educational Barriers/Strategies to Address Needs/Barriers Spiritual Needs Admission Note Unit Orientation Other Issues
10 Nursing Policy and Procedure Manual Page Upon admission, the RN interviews the patient and significant others (when available) and fills out the nursing portion of the Integrated Assessment form as completely as possible If the patient or significant others are unable to give information, the reason is stated on the form The RN may gather information on the patient from the source of referral and/or from collaborating discipline members The RN may assign the LPN to collect the data for the nursing assessment form (i.e. vital signs, weight, height, medications being used) The RN may assign the psych tech to collect data for the nursing assessment form (vital signs and weight and height) The RN must confirm the data and information collected by other nursing staff members. 10/87, 11/90, 1/91, 9/93; 4/98; 10/00; 1/05; 2/07 nursassess.pol
11 Nursing Policy and Procedure Manual Page 11 Chapter 1: Section 4: Patient Assessment Monthly Patient Vital Signs and Weights Policy Monthly vital signs and weights are completed and documented on every patient. Procedure 1. A monthly assessment of vital signs and weight is completed on every patient, unless otherwise there is a reason to complete the vitals signs and/or weights more frequently. 1.1 Vital signs include blood pressure, pulse, respirations, and temperature. 2. The vital signs and weight are recorded in E-chart. 3. A monthly assessment of the patient s vital signs and weight is included in the corresponding nursing monthly assessment note. 4. The RN assesses the patients vital signs and refers significant problems to the MD/NP for follow-up, evaluation, and treatment if needed. 1/88; 9/93; 4/98; 10/00; 1/05; 2/07 ptasses.pol
12 Nursing Policy and Procedure Manual Page 12 Chapter 1: Patient Assessment Section 5: Patient Care Assignments Policy The unit staff RN assigns nursing personnel to care for specific patients or groups of patients based on the employees' education, training, experience and licensure and the patients' acuity, problems/needs and level of intervention required. Procedure 1. Information regarding individual patients or groups of patients is obtained through the patient acuity system, reports of other staff members, family members or friends, and all other pertinent data sources. 2. The assignment of nursing personnel is the responsibility of the Staff Registered Nurse and is consistent with the capabilities of the staff and patient. 2.1 The Psychiatric Technician functions under the license and supervision of the staff Registered Nurse. He/she is accountable to the staff Registered Nurse for job assignments. (See Personnel Management Section, Job Description-Psychiatric Technician). 2.2 The Licensed Practical Nurse functions under the supervision of the staff Registered Nurse and abides by the Licensed Practical Nurse's scope of practice statement from the Utah State Board of Nursing, (See Personal Management Section; Job Description - Licensed Practical Nurse and the Nurse Practice Act of the State of Utah). 2.3 The Registered Nurse functions under the supervision of the Unit Nursing Director and the guidelines and scope of practice statement from the Utah State Board of Nursing. (See Personnel Management Section, Job Description - Registered Nurse, and the Nurse Practice Act of the State of Utah). 3. Patient care assignments are made daily on each shift and are based upon the patient's status and the staff member's competence, including: 3.1 the complexity of the patient's condition and required nursing care 3.2 the dynamics of the patient's status 3.3 the complexity of the assessment required by the patient 3.4 the degree of supervision required by each member of the nursing staff 3.5 the availability of supervision 3.6 the relevant infection control and safety issues. 4. When a staff member is given a specific patient care assignment, the staff member is responsible for the following during the assigned shift:
13 Nursing Policy and Procedure Manual Page observing and reporting any change in the patient s condition psychiatrically and medically. 4.2 assisting the patient work toward his/her treatment goals. 4.3 documenting patient status including behaviors and staff interventions. 1/88,11/90; 9/93; 1/94; 4/98; 8/01; 1/05; 2/07 ptassign.pol
14 Nursing Policy and Procedure Manual Page 14 Chapter 1: Patient Assessment Section 6: Role of Nursing in Patient and Family Education Policy Procedure The staff nurse is responsible for teaching significant aspects of care in collaboration with the patient, family, and treatment team. The level of teaching is based upon the understanding of the patient and/or family members. 1. The patient completes a permission to contact family form on admission. 2. The staff nurse collaborates with the patient, family members, and treatment team to assess the need for information. 3. The staff nurse teaches the patient about the importance of medications, compliance in administration, and adverse side effects as indicated by the individual patient's need. 4. The staff nurse and other nursing personnel teach components of activities of daily living to the patient. 5. The staff nurse and other nursing personnel teach other significant components of life skills to the patient. 6. The Clinical Nurse Specialists teach patients about their illness and methods of dealing with their illness when the treatment team refers the patient for this learning experience. 7. When a new treatment or structure is instituted for an individual patient, the treatment team decides on the approach to the patient concerning the changes. 7.1 When agreed upon and delegated by the treatment team, the nurse explains the change in treatment and assesses the patient's level of understanding. 8. The patient's understanding of their treatment plan or structure is evaluated on an ongoing basis during the patient's stay at the hospital. 8.1 The need for reinforcement of patient or family teaching is based upon the level of understanding. 9. The nurse includes the patient and/or family teaching on the patient's treatment plan and documents in the group notes as well as the weekly progress notes that teaching has been done. 10. The staff nurse assesses need for learning in all areas of self-care preparatory for discharge The needs for self-care are included in discharge planning.
15 Nursing Policy and Procedure Manual Page When a patient's family is involved in the patient's treatment and discharge planning, the nurse assesses the family's level of understanding of the patient's required care The family is taught methods of caring for the patient and the level of understanding is evaluated This is completed on a progressive basis throughout the patient's stay at the hospital. 3/88; 9/93; 4/98; 8/01; 1/05; 2/07 pteduc.pol
16 Nursing Policy and Procedure Manual Page 16 Chapter 1: Patient Assessment Section 7: Rehabilitative Nursing Care Policy The philosophy of nursing services and the Utah State Hospital includes returning the patient to his/her optimal health. This encompasses prevention of complications of physical disability, restoration to optimal function, and adaption to an altered life-style. Nursing services focuses on the rehabilitation of the patient through the nursing process. Procedure 1. When a patient is admitted, the nurse completes a nursing assessment that identifies problems, and initiates a nursing care plan with interim objectives that focus on the identified problems. 1.1 Areas of immediate need are identified through the nursing assessment screening process and the necessary contact with other disciplines is made to provide optimal coordination of care for the patient i.e. dietary, infection control, religious advisors, protective services, and education personnel The contact with the needed services is made via Physical disabilities are identified on admission through the nursing assessment, and by the Medical Doctor s/nurse Practitioner's admission history and physical examination. 3. Consultations with physical therapy, occupational therapy, and other rehabilitative resources are made through physician's orders. 4. The Registered Nurse assists physical therapy, occupational therapy, recreational therapy, and other rehabilitative services through programming on the patient care unit in areas such as selfcare skills, interpersonal relationships, sleep patterns, mild to moderate physical exercise, range of motion, use of prosthetic devices, and other rehabilitative treatments. 5. When a treatment procedure on the patient care unit is placed under the jurisdiction of the Registered Nurse, the appropriate service trains the Registered Nurse in the correct procedures for that treatment; i.e., range of motion--- physical therapy; use of splints--physical therapy. 6. Nursing rehabilitative services at the Utah State Hospital are limited. When comprehensive rehabilitative nursing services are required for a specific patient, the physicians refer the patient to a comprehensive rehabilitative service. 7. Patients who have a physical disability that requires rehabilitation, receive instruction in the areas of adaptive living skills, coping mechanisms, and health maintenance. 8. Discharge planning focuses on specific needs. Alternative living arrangements may be made based on the treatment teams recommendations. 9. The rehabilitative treatment of the patient remains a multidisciplinary team approach. 2/88; 9/93;1/94; 4/98; 8/01; 1/05; 2/07 rehab.pol
17 Nursing Policy and Procedure Manual Page 17 Chapter 1: Patient Assessment Section 8: Patient Falls Policy Procedure If an adult patient falls, the RN assesses the patient for injuries. 1. If a patient is witnessed falling to the floor or is found on the floor and does not get up independently, the RN assesses the patient for injuries. 1.1 All staff who witness a patient fall or find a patient on the floor are instructed not to get the patient up until the RN can make an injury assessment. 2. The Physical Assessment module of Nursing Education includes signs and symptoms of pelvic/hip injuries and methods for assessment of such injuries. 3. When a patient falls or is found on the floor, the RN completes the assessment and then notifies the MD/NP of the results of the assessment. 4. The staff member who witnesses the fall or finds the patient on the floor and the RN who completes the injury assessment document the incident and findings in e-chart. 6/01; 1/05; 2/07 pt.falls
18 Nursing Policy and Procedure Manual Page 18 Chapter 2: Patient Management Section 1: Caffeine Consumption Policy Caffeine consumption by patients may interfere with their psychiatric treatment, particularly as it reduces the effectiveness of medications. (See USH:OPP Patient Management Chapter Section 19) Procedure 1. Caffeinated coffee is not available to patients in hospital food services areas. 2. Individual patients' caffeine consumption from other sources may be limited. Taken from USH:OPP 6/98; 8/01; 07/02; 2/05; 2/07 caffeine.pol
19 Nursing Policy and Procedure Manual Page 19 Chapter 2: Section 2: Patient Management Central Line Management and Protocol (CVAD) Purpose To outline the nursing management of a patient with a CVAD. General Information A Central Venous Access Device (CVAD) provides a system for the intravenous administration of medications, and fluids; it increases patient comfort by avoiding multiple venipunctures associated with peripheral venous access; and it provides a means for obtaining blood samples. When a patient requires IV therapy through a Central Venous Access Device, the patient is taken to the IV Clinic at Utah Valley Regional Medical Center for placement of the device. Cvad General Guidelines Management of the CVAD is performed by a qualified RN. 1. The RN adheres to Standard Precautions and sterile technique during all dressing, tubing, filter, cap, and site changes. 2. The RN is alert to possible complication(s) or dislodgement of the catheter. Notify MD/NP immediately if the patient develops s/s infection (pain, fever, chills, increased WBCs, glucose intolerance); air embolus (hypotension, tachycardia, cyanosis, loss of consciousness); pneumothorax (diminished or absent breath sounds); infiltration (swelling at site, pain); phlebitis (redness, edema, pain, drainage.) 3. A 10cc or larger syringe is used for accessing a CVAD line for administration of IV push medications, blood draws, and heparin flushes. 4. If unable to flush a line, DO NOT force solution. Consult with physician regarding line. 5. Before accessing or disconnecting any hub/port connections, clean the hub and IV tubing (while the connection is closed) with providone/iodine swab, wait thirty seconds, then cleanse with one alcohol swab. 6. When CVAD line is discontinued, inspect the catheter for intactness. If a culture of the catheter tip is ordered, use sterile scissors/forceps to remove tip of catheter. Place tip in sterile collection container and send to lab for culture sensitivity test. 7. Measure the length of the external portion of the catheter and record it on appropriate document. Do not rely solely on this measurement as a guarantee of cannula position, but use it as a comparison if the line has been pulled or dislodgement is suspected.
20 Nursing Policy and Procedure Manual Page If patient is restless or pulling on tubes, obtain order for use of safety device to prevent discontinuation of line. Implement appropriate protocols to manage patient if safety devices are warranted/applied. Procedure: PICC Line 1. Hep-locked: 1.1 Heparin Flush: Flush Q day with 3cc of (100u/ml) Heparin using positive pressure technique. 1.2 Blood Draw: Flush line with 5cc saline. Before removing syringe from access port, draw back 3-4cc blood and discard syringe. Draw appropriate amount of blood for sample. Flush line with 10cc saline using start/stop action to gently agitate and create turbulence against lumen walls. Finish with Heparin flush of 3cc of (100u/ml) Heparin using positive pressure technique. (Note: If blood draw is for blood cultures, do not flush line with saline prior to blood draw.) 1.3 Dressing Change: Q week and prn. Stabilize catheter while removing old dressing. Clean site with 3 alcohol wipes followed by 3 betadine wipes, cleansing in a clean to dirty fashion beginning at catheter site to approximately 3 inches beyond the site. Allow site to dry between each application. Do not remove Betadine. (If patient is allergic to Betadine, clean site with Hibiclens, wipe off with 2x2, and follow with Alcohol. Allow to dry between each step of cleaning.) Place a sterile 2x2 under and over the hub site to promote an occlusive dressing and to act as a moisture wick. Complete occlusive dressing by covering 2x2 with a transparent dressing. If patient is sensitive to transparent dressing, cover site with gauze and waterproof tape (making sure tape completely covers the gauze.) 1.4 Assess and document site each time catheter is flushed. 1.5 Flush with 5cc saline prior to and after administration of medications. 2. Continuous Infusion: 2.1 Obtain IV infusion pump. 2.2 Confirm prescribed flow/rate/type of solution for infusion. 2.3 Refer to pump guidelines for correct setting/use of pump. 2.4 Inspect tubing and connections Q 4 hours and prn to ensure it is secure and free of kinks or tension. Observe for any break or disconnection which could lead to bleeding or air embolism. 2.5 Leur-lock or tape each connection to ensure closed system. 2.6 Assess and document site Q 4 hours and prn. 2.7 Flush with 5cc saline prior to and after administration of medications if medication(s) incompatible with IV solution.
21 Nursing Policy and Procedure Manual Page 21 Procedure: Port -A-Cath 1. Patients with newly inserted port-a-caths are monitored closely for signs of infection, but nurses at USH do not access port-a-caths. 2. Port-a-caths are flushed and managed by Utah Valley Regional Medical Center or by the facility designated by the surgeon. Procedure: Heparin Locks (IV Adaptors) 1. Flush each unused port Q 8 hours with 3cc saline using positive pressure technique. 2. Hep-caps are changed Q 48 and prn. 2.1 Cleanse connection site with betadine and alcohol. 2.2 Fill new hep-cap with appropriate solution. 2.3 Clamp catheter with attached plastic clamp. 2.4 Remove previous cap and discard. 2.5 Apply new cap. 2.6 Remove clamp and flush according to protocol. Procedure: Discontinuing Cvad 1. Obtain sterile gloves and suture removal kit (if applicable.) 2. Secure CVAD line while removing dressing. 3. Clip any sutures securing CVAD in place. 4. Remove catheter by firmly, gently, and steadily pulling on the catheter. Inspect tip for breakage. 5. Immediately place gauze dressing on site, apply pressure to prevent any bleeding. An elastictype tape covering may be indicated to assist with maintaining light pressure at site. Documentation: 1. RN documents all teaching and procedures, with findings and patient response. Trouble-Shooting: 1. If lumen flushes easily but unable to aspirate: 1.1 Reposition patient - such as elevate head of bed, turn patient to right or left side, lay patient flat, or raise the patient s arm on the same side as the CVAD above the head. 1.2 Attempt to aspirate, slowly. 1.3 Notify MD of possible fibrin sheath development.
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Medications or therapeutic solutions may be injected directly into the bloodstream
 Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
Intravenous Therapy Medications or therapeutic solutions may be injected directly into the bloodstream for immediate circulation and use by the body. State practice acts designate which health care professionals
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Inform II. Quick Reference Guide. for Healthcare Professionals BLOOD GLUCOSE MONITORING SYSTEM
 Inform II BLOOD GLUCOSE MONITORING SYSTEM Quick Reference Guide for Healthcare Professionals 2 Table of Contents Important... 4 General Information... 6 ACCU-CHEK Inform II Meter...10 How to Perform Patient
Inform II BLOOD GLUCOSE MONITORING SYSTEM Quick Reference Guide for Healthcare Professionals 2 Table of Contents Important... 4 General Information... 6 ACCU-CHEK Inform II Meter...10 How to Perform Patient
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to:
 Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Objectives At the completion of this module, unlicensed assistive personnel (UAP) should be able to: 1. administer medications by subcutaneous injections. 2. document medication administration in the client
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
NORTH CAROLINA BOARD OF NURSING NURSE AIDE II TRAINING MODULE
 PART A: PREPARING FOR ADMINISTRATION OF IV FLUIDS All four parts of this module, including skills checklists must be successfully completed in order to complete this training module. This activity is a
PART A: PREPARING FOR ADMINISTRATION OF IV FLUIDS All four parts of this module, including skills checklists must be successfully completed in order to complete this training module. This activity is a
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS
 SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
SUBCUTANEOUS THERAPY A. ADMINISTERING SUBCUTANEOUS MEDICATIONS INTERMITTENTLY/CONTINUOUSLY B. (SUBCUTANEOUS INFUSION) HYDRODERMOCLYSIS PARTS I. Purposes II. General Information III. Responsibilities IV.
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
Procedure for Inotrope Administration in the home
 Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
Procedure for Inotrope Administration in the home Purpose This purpose of this procedure is to define the care used when administering inotropic agents intravenously in the home This includes: A. Practice
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
RULES OF THE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES OFFICE OF LICENSURE
 RULES OF THE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES OFFICE OF LICENSURE CHAPTER 0940-5-46 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG RESIDENTIAL TREATMENT FACILITIES FOR CHILDREN
RULES OF THE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES OFFICE OF LICENSURE CHAPTER 0940-5-46 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG RESIDENTIAL TREATMENT FACILITIES FOR CHILDREN
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
State of Hawaii. Licensed Practical Nurse - Mental Health
 Entry Level Work HE-6 6.734 Full Performance Work HE-8 6.735 Function and Location This position works in a hospital or clinic which provides care and treatment to patients who are mentally ill. The primary
Entry Level Work HE-6 6.734 Full Performance Work HE-8 6.735 Function and Location This position works in a hospital or clinic which provides care and treatment to patients who are mentally ill. The primary
To maintain a port of entry to venous flow when all available peripheral ports have failed.
 I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
I. Purpose: To maintain a port of entry to venous flow when all available peripheral ports have failed. II. General Comments: Since its development, these catheters have been used with increasing frequency
Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery.
 JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
ARTICLE 10. OUTPATIENT TREATMENT CENTERS
 Section R9-10-1001. R9-10-1002. R9-10-1003. R9-10-1004. R9-10-1005. R9-10-1006. R9-10-1007. R9-10-1008. R9-10-1009. R9-10-1010. R9-10-1011. R9-10-1012. R9-10-1013. R9-10-1014. R9-10-1015. R9-10-1016. R9-10-1017.
Section R9-10-1001. R9-10-1002. R9-10-1003. R9-10-1004. R9-10-1005. R9-10-1006. R9-10-1007. R9-10-1008. R9-10-1009. R9-10-1010. R9-10-1011. R9-10-1012. R9-10-1013. R9-10-1014. R9-10-1015. R9-10-1016. R9-10-1017.
Information for patients and nurses
 Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
Information for patients and nurses Rocket IPC Pleural Catheter Indwelling Catheter Rocket Indwelling Pleural Catheter (IPC) Contents Contact Information...03 What s in the Rocket Dressing Pack and Bottle
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Administration of Medications & Fluids via a Peripheral Intravenous Cannula
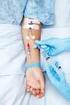 Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Administration of Medications & Fluids via a Peripheral Intravenous Cannula Clinical S.O.P. No.: 22.0 Compiled by: Approved by: Review date: November 2016 Administration of Medications & Fluids via S.O.P.
Title: Fingerstick Glucose by Accu-Chek Inform
 Title: Fingerstick Glucose by Accu-Chek Inform Target Audience: This module is available to aid in assessing competency for all clinical staff who perform fingerstick glucose testing. Contents Instructions...
Title: Fingerstick Glucose by Accu-Chek Inform Target Audience: This module is available to aid in assessing competency for all clinical staff who perform fingerstick glucose testing. Contents Instructions...
Managing Your Non-Tunneled (Percutaneous) Catheter: PICC, SICC, and JCC. What is a PICC catheter?
 Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Policy and Procedure Manual
 Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 RA-13 Admission. History, Physicals and Routine Health Care
Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 RA-13 Admission. History, Physicals and Routine Health Care
Care of a Foley Catheter
 Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Percutaneous Nephrostomy. Care of your Nephrostomy. Department of Urology
 Percutaneous Nephrostomy Care of your Nephrostomy Department of Urology You may encounter some problems at home but these are usually easily overcome. Listed below are some questions patients commonly
Percutaneous Nephrostomy Care of your Nephrostomy Department of Urology You may encounter some problems at home but these are usually easily overcome. Listed below are some questions patients commonly
RN CONSULTATION. KEY TERMS: Assessment Basic tasks Consultation Home health services PRN Written parameters OBJECTIVES:
 RN CONSULTATION The purpose of this section is to assist the learner in understanding the role of a registered nurse (RN) consultant and when to seek RN consultation. KEY TERMS: Assessment Basic tasks
RN CONSULTATION The purpose of this section is to assist the learner in understanding the role of a registered nurse (RN) consultant and when to seek RN consultation. KEY TERMS: Assessment Basic tasks
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
INTRODUCTION TO CLINICAL PRACTICE AND CLINICAL SKILLS 2nd Year MEDICAL YEAR 2009/2010
 INTRODUCTION TO CLINICAL PRACTICE AND CLINICAL SKILLS 2nd Year MEDICAL YEAR 2009/2010 POINT OF CARE TESTING This session is designed to teach you the principals of point of care testing. This is common
INTRODUCTION TO CLINICAL PRACTICE AND CLINICAL SKILLS 2nd Year MEDICAL YEAR 2009/2010 POINT OF CARE TESTING This session is designed to teach you the principals of point of care testing. This is common
Central Venous Catheter Care For Haemodialysis
 Central Venous Catheter Care For Haemodialysis Information For Parents and Carers Haemodialysis Unit 01 878 4757 Main Hospital Number 01 878 4200 Central Venous Catheters We hope this booklet will help
Central Venous Catheter Care For Haemodialysis Information For Parents and Carers Haemodialysis Unit 01 878 4757 Main Hospital Number 01 878 4200 Central Venous Catheters We hope this booklet will help
RULES OF DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES OFFICE OF LICENSURE
 RULES OF DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES OFFICE OF LICENSURE CHAPTER 0940-5-37 MENTAL HEALTH RESIDENTIAL TREATMENT FACILITY TABLE OF CONTENTS 0940-5-37-.01 Definition 0940-5-37-.08
RULES OF DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES OFFICE OF LICENSURE CHAPTER 0940-5-37 MENTAL HEALTH RESIDENTIAL TREATMENT FACILITY TABLE OF CONTENTS 0940-5-37-.01 Definition 0940-5-37-.08
Illinois Department of Public Health STATEMENT OF DEFICIENCIES AND PLAN OF CORRECTION C 04/26/2015. Statement of Licensure Violations:
 (X1) PROVER/SUPPLIER/LIA ENTIFIATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) REGULATORY OR LS ENTIFYING INFORMATION) Final Observations Statement of Licensure Violations: 300.610a) 300.1210b)
(X1) PROVER/SUPPLIER/LIA ENTIFIATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) REGULATORY OR LS ENTIFYING INFORMATION) Final Observations Statement of Licensure Violations: 300.610a) 300.1210b)
MANITOBA PATIENT SERVICE CENTRE STANDARDS
 MANITOBA PATIENT SERVICE CENTRE STANDARDS February 2015 INTRODUCTION These Standards are derived from Z316.7-12 and are approved by the Council of the College of Physicians and Surgeons of Manitoba. These
MANITOBA PATIENT SERVICE CENTRE STANDARDS February 2015 INTRODUCTION These Standards are derived from Z316.7-12 and are approved by the Council of the College of Physicians and Surgeons of Manitoba. These
LICENSED PRACTICAL NURSE (LPN) JOB SUMMARY AND PERFORMANCE CRITERIA (See full job description for physical demands)
 LICENSED PRACTICAL NURSE (LPN) JOB SUMMARY AND PERFORMANCE CRITERIA (See full job description for physical demands) Department Assigned: Nursing Supervisor Title: Registered Nurse Purpose of Your Job Position
LICENSED PRACTICAL NURSE (LPN) JOB SUMMARY AND PERFORMANCE CRITERIA (See full job description for physical demands) Department Assigned: Nursing Supervisor Title: Registered Nurse Purpose of Your Job Position
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Urinary Indwelling Catheter. The Urinary System
 Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Policy and Procedure Manual
 Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 Physical Health Services Dental Services Initial Nursing Summary
Policy and Procedure Manual Resident Assessment (RA) Table of Contents RA-01 RA-02 RA-03 RA-04 RA-05 RA-06 RA-07 RA-08 RA-09 RA-10 RA-11 RA-12 Physical Health Services Dental Services Initial Nursing Summary
Policies & Procedures. I.D. Number: 1073
 Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
Policies & Procedures Title:: CENTRAL VENOUS CATHETERS INSERTION ASSISTING I.D. Number: 1073 Authorization [] Pharmacy Nursing Committee [] MAC Motion #: [x] SHR Nursing Practice Committee Source: Nursing
Catheter Care How to Care for a Urinary Catheter
 Catheter Care How to Care for a Urinary Catheter Ensure patient/client is provided with any available product specific instructions along with this booklet. About Your Catheter Your urinary catheter allows
Catheter Care How to Care for a Urinary Catheter Ensure patient/client is provided with any available product specific instructions along with this booklet. About Your Catheter Your urinary catheter allows
Cytotoxic and Biotherapies Credentialing Programme Module 6
 Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
Cytotoxic and Biotherapies Credentialing Programme Module 6 1. Safe Handling and Administration of Cytotoxic and Biotherapies 2. Waste and Spill Management At the completion of this module the RN will
105 CMR: DEPARTMENT OF PUBLIC HEALTH 105 CMR 210.000: THE ADMINISTRATION OF PRESCRIPTION MEDICATIONS IN PUBLIC AND PRIVATE SCHOOLS
 105 CMR 210.000: THE ADMINISTRATION OF PRESCRIPTION MEDICATIONS IN PUBLIC AND PRIVATE SCHOOLS Section 210.001: Purpose 210.002: Definitions 210.003: Policies Governing the Administration of Prescription
105 CMR 210.000: THE ADMINISTRATION OF PRESCRIPTION MEDICATIONS IN PUBLIC AND PRIVATE SCHOOLS Section 210.001: Purpose 210.002: Definitions 210.003: Policies Governing the Administration of Prescription
Correctional Treatment CenterF
 0BCHAPTER 15 F 1BI. POLICY The California Department of Corrections and Rehabilitation (CDCR) shall maintain s (CTC) to house inmate-patients who do not require general acute care level of services but
0BCHAPTER 15 F 1BI. POLICY The California Department of Corrections and Rehabilitation (CDCR) shall maintain s (CTC) to house inmate-patients who do not require general acute care level of services but
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]
![SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D]](/thumbs/27/9667060.jpg) SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
SUBSTANCE USE DISORDER SOCIAL DETOXIFICATION SERVICES [ASAM LEVEL III.2-D] I. Definitions: Detoxification is the process of interrupting the momentum of compulsive drug and/or alcohol use in an individual
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
STANDARDIZED PROCEDURE BONE MARROW ASPIRATION
 I. Definition: This protocol covers the task of bone marrow aspiration by an Allied Health Professional. The purpose of this standardized procedure is to allow the Allied Health Professional to safely
I. Definition: This protocol covers the task of bone marrow aspiration by an Allied Health Professional. The purpose of this standardized procedure is to allow the Allied Health Professional to safely
PROCEDURE NO. POC.514.01 LBH. Printed copies are for reference only. Please refer to the electronic copy for the latest version.
 Department Of Pathology POC.514.01- Blood Glucose Monitoring Accu-Chek Inform II Procedure-LBH Version# 1 Department PROCEDURE NO. PAGE NO. Point-of-Care Testing POC.514.01 LBH 1 OF 7 Printed copies are
Department Of Pathology POC.514.01- Blood Glucose Monitoring Accu-Chek Inform II Procedure-LBH Version# 1 Department PROCEDURE NO. PAGE NO. Point-of-Care Testing POC.514.01 LBH 1 OF 7 Printed copies are
RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES
 RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-5-41 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG HALFWAY HOUSE TREATMENT FACILITIES TABLE OF CONTENTS
RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-5-41 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG HALFWAY HOUSE TREATMENT FACILITIES TABLE OF CONTENTS
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
OKLAHOMA. Downloaded January 2011
 OKLAHOMA Downloaded January 2011 310:675 7 9.1. Written administrative policies and procedures (f) Emergency care shall be provided to residents in case of sudden illness or accident, including persons
OKLAHOMA Downloaded January 2011 310:675 7 9.1. Written administrative policies and procedures (f) Emergency care shall be provided to residents in case of sudden illness or accident, including persons
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Wound Drain
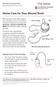 PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
MEDICAL AND HEALTH EMERGENCIES
 IX.041 MEDICAL AND HEALTH EMERGENCIES POLICY The Board shall provide medically appropriate, immediate, quality emergency care in the event of an accident or illness that may compromise the well-being of
IX.041 MEDICAL AND HEALTH EMERGENCIES POLICY The Board shall provide medically appropriate, immediate, quality emergency care in the event of an accident or illness that may compromise the well-being of
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
ARTICLE 3. BEHAVIORAL HEALTH INPATIENT FACILITIES
 Section R9-10-301. R9-10-302. R9-10-303. R9-10-304. R9-10-305. R9-10-306. R9-10-307. R9-10-308. R9-10-309. R9-10-310. R9-10-311. R9-10-312. R9-10-313. R9-10-314. R9-10-315. R9-10-316. R9-10-317. R9-10-318.
Section R9-10-301. R9-10-302. R9-10-303. R9-10-304. R9-10-305. R9-10-306. R9-10-307. R9-10-308. R9-10-309. R9-10-310. R9-10-311. R9-10-312. R9-10-313. R9-10-314. R9-10-315. R9-10-316. R9-10-317. R9-10-318.
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER
 URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
INJECTION TECHNIQUE. IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole
 IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
IVF NURSING OFFICE: (301) 400-2151 Darshana (301) 400-2146 Nicole PLEASE NOTE: If you do not have medications for the next day s dose, you MUST go to the clinic that morning at 6:30 AM for more medications.
Competencies Expected. of the Beginning. Practitioner of. Psychiatric Nursing
 Competencies Expected of the Beginning Practitioner of Psychiatric Nursing Revised March 25, 1995 College of Registered Psychiatric Nurses of British Columbia ******* College of Psychiatric Nurses of British
Competencies Expected of the Beginning Practitioner of Psychiatric Nursing Revised March 25, 1995 College of Registered Psychiatric Nurses of British Columbia ******* College of Psychiatric Nurses of British
RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES
 RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-5-45 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG RESIDENTIAL REHABILITATION TREATMENT FACILITIES TABLE
RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-5-45 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG RESIDENTIAL REHABILITATION TREATMENT FACILITIES TABLE
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home
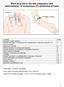 Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
Ward 29 guide to the safe preparation and administration of intravenous (IV) antibiotics at home Contents Page Important contact numbers 1 General information on preparing and administering IV antibiotics
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES
 RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-05-44 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG RESIDENTIAL DETOXIFICATION TREATMENT FACILITIES TABLE
RULES OF THE TENNESSEE DEPARTMENT OF MENTAL HEALTH AND DEVELOPMENTAL DISABILITIES CHAPTER 0940-05-44 MINIMUM PROGRAM REQUIREMENTS FOR ALCOHOL AND DRUG RESIDENTIAL DETOXIFICATION TREATMENT FACILITIES TABLE
Section 6: Your Hemodialysis Catheter
 Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
How to Change a Foley Catheter Step-by-step instructions for the caregiver
 Patient Education How to Change a Foley Catheter Step-by-step instructions for the caregiver This handout gives stepby-step instructions for changing a Foley catheter, a tube in the bladder to drain urine.
Patient Education How to Change a Foley Catheter Step-by-step instructions for the caregiver This handout gives stepby-step instructions for changing a Foley catheter, a tube in the bladder to drain urine.
I-140 Venipuncture for Blood Specimen Collection
 I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
I-140 Venipuncture for Blood Specimen Collection Purpose Obtain a blood specimen by venipuncture for laboratory analysis using aseptic technique. Applies To Registered Nurses Licensed Practical/Vocational
Certified Nursing Assistant Essential curriculum- Maryland Board of Nursing
 Certified Nursing Assistant Essential curriculum- Maryland Board of Nursing Module I Orientation/Introduction A. Identify general information pertaining to the nursing assistant course B. List requirements
Certified Nursing Assistant Essential curriculum- Maryland Board of Nursing Module I Orientation/Introduction A. Identify general information pertaining to the nursing assistant course B. List requirements
Changing Your Central Line Catheter Cap
 Changing Your Central Line Catheter Cap The catheter cap on each lumen of your central line needs to be changed once a week. A lumen is a small tube within your catheter. These same steps can be used for
Changing Your Central Line Catheter Cap The catheter cap on each lumen of your central line needs to be changed once a week. A lumen is a small tube within your catheter. These same steps can be used for
call 811 to get advice from a nurse, or have someone drive the patient to a hospital Emergency Department. Patients should NOT drive themselves.
 Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
 XXX DAYTONA XXX _OCEANSIDE HEALTH CARE PARTNERS Department: Page 1 of 5 POLICY & PROCEDURE Policy Number NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
XXX DAYTONA XXX _OCEANSIDE HEALTH CARE PARTNERS Department: Page 1 of 5 POLICY & PROCEDURE Policy Number NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES. Model Policy for the Management of Students Requiring a Private Duty Nurse in Schools
 Department of Health and Mental Hygiene Maryland State Department of Education Maryland State School Health Council MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES Model Policy for the Management of Students
Department of Health and Mental Hygiene Maryland State Department of Education Maryland State School Health Council MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES Model Policy for the Management of Students
Peripherally Inserted Central Catheter (PICC)
 Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Use of Continuous Subcutaneous Insulin Infusion (CSII) Pumps in Hospitalized Patients Policy and Procedure
 Purpose: To ensure safe and accurate administration of insulin for patients using their own external continuous subcutaneous insulin infusion pump during hospitalization. Definitions: Insulin pump: An
Purpose: To ensure safe and accurate administration of insulin for patients using their own external continuous subcutaneous insulin infusion pump during hospitalization. Definitions: Insulin pump: An
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Foley Catheter Placement
 Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
MINNESOTA. Downloaded January 2011
 4658.00 (GENERAL) MINNESOTA Downloaded January 2011 4658.0015 COMPLIANCE WITH REGULATIONS AND STANDARDS. A nursing home must operate and provide services in compliance with all applicable federal, state,
4658.00 (GENERAL) MINNESOTA Downloaded January 2011 4658.0015 COMPLIANCE WITH REGULATIONS AND STANDARDS. A nursing home must operate and provide services in compliance with all applicable federal, state,
COMMUNITY HOSPITAL REGISTERED NURSE PRINTED NAME:
 COMMUNITY HOSPITAL REGISTERED NURSE EMPLOYEE: PRINTED NAME: REPORTS TO: DEPARTMENT: FMLA STATUS: Date: Director of Med-Surg Nursing Non-exempt PURPOSE: The Registered Nurse is responsible for the ongoing
COMMUNITY HOSPITAL REGISTERED NURSE EMPLOYEE: PRINTED NAME: REPORTS TO: DEPARTMENT: FMLA STATUS: Date: Director of Med-Surg Nursing Non-exempt PURPOSE: The Registered Nurse is responsible for the ongoing
ATI Skills Modules Checklist for Urinary Catheter Care
 For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Urinary Catheter Care Student s name Date Verify order Patient record Assess for procedure need Identify, gather, and prepare
For faculty use only Educator s name Score Date ATI Skills Modules Checklist for Urinary Catheter Care Student s name Date Verify order Patient record Assess for procedure need Identify, gather, and prepare
UW School of Dentistry Comprehensive Medication Policy
 UNIVERSITY OF WASHINGTON SCHOOL OF DENTISTRY Subject: UW School of Dentistry Comprehensive Medication Policy Policy Number: Effective Date: December 2014 Revision Dates: June 2015 PURPOSE This policy provides
UNIVERSITY OF WASHINGTON SCHOOL OF DENTISTRY Subject: UW School of Dentistry Comprehensive Medication Policy Policy Number: Effective Date: December 2014 Revision Dates: June 2015 PURPOSE This policy provides
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
Notice of Rulemaking Hearing. Department of Mental Health and Developmental Disabilities Office of Licensure
 Notice of Rulemaking Hearing Department of Mental Health and Developmental Disabilities Office of Licensure There will be a hearing before the Tennessee Department of Mental Health and Developmental Disabilities,
Notice of Rulemaking Hearing Department of Mental Health and Developmental Disabilities Office of Licensure There will be a hearing before the Tennessee Department of Mental Health and Developmental Disabilities,
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
MISSISSIPPI BOARD OF NURSING IV THERAPY COURSE FOR THE EXPANDED ROLE LICENSED PRACTICAL NURSE COURSE OUTLINE
 THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed
 Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
OCCUPATIONAL GROUP: Health Services. CLASS FAMILY: Allied Health CLASS FAMILY DESCRIPTION:
 OCCUPATIONAL GROUP: Health Services CLASS FAMILY: Allied Health CLASS FAMILY DESCRIPTION: This family of positions is comprised of health care practitioners with formal education and clinical training
OCCUPATIONAL GROUP: Health Services CLASS FAMILY: Allied Health CLASS FAMILY DESCRIPTION: This family of positions is comprised of health care practitioners with formal education and clinical training
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
