GUIDELINE. Effective antibiotic therapy is recommended for cases of peritoneal dialysis catheterrelated
|
|
|
- Harold Roberts
- 8 years ago
- Views:
Transcription
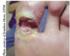
1 Peritoneal dialysis catheter related infection: exit site and tunnel Date written: April 2013 Author: Josephine Chow GUIDELINE No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions are based on Level III and IV evidence) Effective antibiotic therapy is recommended for cases of peritoneal dialysis catheterrelated infection. Either intraperitoneal or oral antibiotics may be considered. IMPLEMENTATION AND AUDIT Primarily, audit should consist of ongoing research to continually improve and validate our ability to predict outcomes based on medical parameters. BACKGROUND Exit site infection (ESI) has been defined as clinically apparent infection at the exit site with or without a positive culture. Included in this definition is catheter tunnel tract infection. Clinical signs of infection include purulent drainage, redness, swelling, warmth and tenderness over or around the exit site. Exit site and tunnel infections are a significant cause of morbidity and are responsible for a significant proportion of patient dropout from peritoneal dialysis. [1] The bacteria that colonise the exit site are the same as those responsible for ESIs, but are different to those that cause peritonitis. [2] There are various stages in the development of an infected exit site, which include serous and purulent drainage, abscess formation and tunnel infection. Early identification and diagnosis of the various infection stages are vital for the initiation of prompt and effective therapy. Ultrasonography of the exit site has been used to diagnose exit site and tunnel infections. A sonolucent zone around the external cuff over 1 mm thick following treatment with a course of antibiotic treatment and also with the involvement of the proximal cuff are associated with poor clinical outcome. [3] With the ultrasonographic studies, a tunnel infection is confirmed when the subcutaneous pathway is clinically occulted. [4] Prevention of infection is considered essential for the successful maintenance of peritoneal dialysis (PD). Strategies to prevent or reduce the risk of infection include rigorous exit site care, catheter care and meticulous attention to the use of a clean no-touch technique for dialysis exchanges. Both antibiotic and antimicrobial agents and dressing technique play important roles in the survival of the PD catheter. The objective of this guideline was to review current evidence in the prevention and management of catheter exit site infection and tunnel infection.
2 SEARCH STRATEGY Databases searched: MeSH terms and text words for peritoneal dialysis were combined with MeSH terms and text words for catheter, peritonitis, exit site infection and tunnel infection. The search was carried out in Medline (1950 September Week 3, 2010). The Cochrane Renal Group Trials Register was also searched for trials not indexed in Medline. Date of searches: 15 October WHAT IS THE EVIDENCE? Evaluation of the exit site/tunnel and diagnosis of infection Twardowski et al performed 565 evaluations of healed exit sites in 56 patients. [5,6] A new classification was developed with six distinct categories of exit site appearance: acute infection, chronic infection, external cuff infection, traumatised exit, etc. The outcomes in each category were correlated with treatment measures in a 5-year longitudinal study. A cross-sectional study was conducted with 45 patients, using loupe and magnifier evaluations. Ninety-one percent (41/45) of the evaluations were in agreement. Vychytil et al investigated indications and outcomes of 738 ultrasound examinations of the PD catheter tunnel. [7] The research team concluded that tunnel ultrasonography is useful to assess whether tunnel infection is present, and the severity of involvement. By using ultrasonography, a therapeutic regimen can be evaluated and reviewed. Therapy for exit site/tunnel infection Flanigan et al reported a randomised, prospective study comparing intraperitoneal vancomycin plus oral rifampin or oral trimethoprim/ sulfamethoxazole for Gram-positive catheter infections. [8] There were 126 recorded catheter infections resulting in a rate of 0.67 episodes per patient year of exposure. The cure rate of Gram-positive catheter infections treated with vancomycin plus rifampin (86% cured) was indistinguishable from that achieved with oral trimethoprim/sulfamethoxazole (89% cured; P = 0.99). Precautions need to be considered to retard the development of vancomycin-resistant enterococcus (VRE), if prolonged use of vancomycin is planned. Plum et al in a prospective randomised study, showed the greater efficacy of the intraperitoneal (IP) application of clindamycin as a first-line antibiotic compared with the oral route for the treatment of tunnel infections. [9] The results showed no significant difference in the pericatheter fluid along the catheter at study entry, with 4 mm (median; range: 2-6 mm) in the oral group and 4 mm (range: 2-4 mm) in the IP group. The IP treatment resulted in a decrease to 0 mm (0-2 mm) after 28 days (P < 0.05), while the diameter was still 2 mm (0-10 mm; ns) in the oral group. The disappearance of ESI also occurred earlier in the IP group (51 vs 15 days; ns). Catheter removal occurred once in the IP group and twice in the oral group within 6 months of study entry. There was no difference in clinical outcomes. Disinfectant Luzar reported a multicentre RCT where adult continuous ambulatory peritoneal dialysis (CAPD) patients were randomised to disinfect the exit site 2 3 times per week with a 20 g/l solution of povidone iodine and then cover the exit site with sterile gauze, or cleanse the exit site daily with non-disinfectant soap on sterile gauze. [10] There was a reduction in the rate of ESIs with the use of povidone-iodine solution compared with the soap and water cleansing (P = 0.07).
3 Wilson randomised 149 adult PD patients and examined the effectiveness of standard dressing changes versus standard dressing changes plus povidone-iodine dry powder spray (2.5%) in the prevention of ESIs and/or peritonitis. [11] Povidone-iodine did not reduce the number of total infections, ESIs or peritonitis compared with the control group over the period of the study. Other considerations Dong et al reported a prospective observational study in Chinese CAPD patients. A total of 130 patients were examined during their PD bag exchange procedure 6 months after dialysis initiation. [12] Various items were observed such as dirty nails, improper hand washing, insufficient ultraviolet radiation, not wearing a face mask, checking for bag expiration or leakage, not flushing before filling and suspected connection contamination. It was concluded from a multivariate Cox regression analysis that not wearing a face mask or cap was significantly associated with a first episode of peritonitis [HR: 7.26, 95% CI: ; P < 0.001]. Keane et al reported a summary of treatment recommendations for ESI from a consensus panel of experts. [13] The treatment recommendations for Gram-positive purulent drainage at the exit site are 2-4 weeks of a cephalosporin or vancomycin combined with oral rifampicin in the case of persistent infection, and ciprofloxacin for the treatment of Gram-negative infections. Ibels et al conducted a survey in 1995 of 35 PD units in Australia. [1] In all units, a swab culture was obtained at the first sign of PD catheter ESI and exit site care procedures were reviewed with patients. Exit site infection rates were monitored, data collated, and procedures evaluated routinely in two-thirds of units. While the antibiotics used varied, most units used vancomycin or oral flucloxacillin. Catheter exit site and tunnel infections accounted for 12% and 6%, respectively, of the principal indications for removal of the peritoneal catheter. No correlations were undertaken between practices and outcomes. Turner et al randomised 66 patients into one of three catheter groups: immobilizer, tape, or nonimmobilized group. [14] The incidence of ESI over 347 patient-months was recorded. The results show no significant difference in infection rate between the three groups. While the findings of the study point to a need for a better quality immobilizer, the short duration of the study precluded any definitive conclusion being drawn. Scalamogna et al reported data on surgical intervention, such as external cuff shaving in tunnel infections. [15,2,16] Shaving the cuff as a rescue treatment was effective for almost 50% of patients with antibiotic-resistant Staphylococcus aureus ESI. The catheters of the remaining patients were removed because of peritonitis associated with tunnel infection.. SUMMARY OF THE EVIDENCE There are no randomised trials comparing the different classification and evaluation systems for ESI. The International Society for Peritoneal Dialysis (ISPD) has developed a simple scoring system for the signs and symptoms of PD exit site. The scoring system is easy to use and provides guidance on timing to treat immediately rather than waiting for a swab result. It also recommends that purulent discharge is an absolute indicator for antibiotic treatment. [4] There are two randomised trials that have compared antibiotic therapy treatment for exit site/tunnel infection. One study compared intraperitoneal vancomycin plus oral rifampin or oral trimethoprim/sulfamethoxazole for Gram-positive catheter infections. There was no difference with either treatment on catheter infection cure rate. The second study showed that there is greater efficacy with the intraperitoneal application of clindamycin as a first-line antibiotic compared with the oral route, for the treatment of tunnel infections.
4 Randomised trials evaluating the effectiveness of povidone-iodine have provided inconclusive results. Povidone-iodine spray powder was not found to be better than standard dressing in relation to ESI, peritonitis or tunnel infection. Therefore, no definitive conclusions regarding the effectiveness of povidone iodine in reducing the rate of ESI or peritonitis in PD patients can be established on present evidence. WHAT DO THE OTHER GUIDELINES SAY? Kidney Disease Outcomes Quality Initiative: No recommendation. UK Renal Association: [17] Topical antibiotic administration should be used to reduce the frequency of S. aureus and Gram negative exit-site infection and peritonitis (1A). Exit site infection is suggested by pain, swelling, crusting, erythema and serous discharge; purulent discharge always indicates infection. Swabs should be taken for culture and initial empiric therapy should be with oral antibiotics that will cover S. aureus and P. aeruginosa (1 B). Canadian Society of Nephrology: No recommendation. European Renal Best Practice Guidelines: Exit site infection should be treated according to the guidelines of the International Society for Peritoneal Dialysis. [18]. Adjustments can be considered depending on the sensitivity patterns of microorganisms in the unit. (Evidence C) Topical treatment may be applied in equivocal cases or as adjuvant therapy. (Evidence C) International Guidelines: ISPD Guidelines/Recommendations (2005). [4] The diagnosis of a catheter exit site infection should be made in the presence of a purulent discharge from the sinus tract, or marked pericatheter swelling, redness, and/or tenderness, with or without a pathogenic organism cultured from the exit site. Infectious symptoms should be rated according to an objective scoring system. Antibiotic treatment of a catheter exit site infection should be started after culture results have been obtained, unless signs of severe infection are present. The antibiotic should be chosen according to the susceptibilities of the cultured organism. Treatment duration should be 2-4 weeks. SUGGESTIONS FOR FUTURE RESEARCH 1. Prospectively gather data to allow better prediction of outcomes after an ESI or tunnel infection. This should include more specific data than is currently collected, including symptoms, history of previous infection, and mode of contamination. 2. Perform a long term randomised trial with sufficient power and blinding to look at the most effective antibiotic treatment for exit site and tunnel infection. 3. Run a diagnosis study such as using ultrasound examinations of the peritoneal catheter tunnel and a classification of ESI system. 4. Conduct studies and publish results on different ESI treatment protocols.
5 REFERENCES 1. Ibels LS, Venus PD, Watts RL, et al. Peritoneal dialysis catheter management and exit site care: an Australian survey of current practices. Nephrology 1997; 3: Scalamogna A, Castelnovo C, De Vecchi A, et al. Exit-site and tunnel infections in continuous ambulatory peritoneal dialysis patients. Am J Kidney Dis 1991; 18: Kwan TH, Tong MK, Siu YP, Leung KT, Luk SH, Cheung YK. Ultrasonography in the management of exit site infections in peritoneal dialysis patients. Nephrology (Carlton) 2004; 9: Piraino B, Bailie GR, Bernardini J, et al. Peritoneal dialysis-related infections recommendations: 2005 update. Perit Dial Int 2005; 25: Twardowski ZJ, Prowant BF. Exit-site study methods and results. Perit Dial Int 1996; 16 (Suppl 3): S6-S Twardowski ZJ, Prowant BF. Current approach to exit-site infections in patients on peritoneal dialysis. Nephrol Dial Transplant 1997; 12: Vychytil A, Lilaj T, Lorenz M, et al. Ultrasonography of the catheter tunnel in peritoneal dialysis patients: what are the indications? Am J Kidney Dis 1999; 33: Flanigan MJ, Hochstetler LA, Langholdt D, et al. Continuous ambulatory peritoneal dialysis catheter infections: diagnosis and management. Perit Dial Int 1994; 14: Plum J, Artik S, Busch T, et al. Oral versus intraperitoneal application of clindamycin in tunnel infections: a prospective, randomized study in CAPD patients. Perit Dial Int 1997; 17: Luzar MA, Brown CB, Balf D, et al. Exit site care and exit-site infection in continuous ambulatory peritoneal dialysis (CAPD): results of a randomized multicenter trial. Perit Dial Int 1990; 10: Wilson AR, Lewis C, O Sullivan H, Shetty N, Neild GH, Mansell M. The use of povidone iodine in exit site care for patients undergoing continuous peritoneal dialysis (CAPD). J Hosp Infect 1997; 35: Dong J, Chen Y. Impact of the bag exchange procedure on the risk of peritonitis. Perit Dial Int 2009; 30: Keane WF, Bailie GR, Boeschoten E, et al. International Society for Peritoneal Dialysis. Adult peritoneal dialysis-related peritonitis treatment recommendations: 2000 update. Perit Dial Int 2000; 20: Turner K, Edgar D, Hair M, et al. Does catheter immobilization reduce exit-site infections in CAPD patients? Adv Perit Dial 1992; 8: Scalamogna A, Castelnovo C, De Vecchi A, et al. Staphylococcus aureus exit-site and tunnel infection in CAPD. Adv Perit Dial 1990; 6: Scalamogna A, De Vecchi A, Maccario M, et al. Cuff-shaving procedure. A rescue treatment for exit-site infection unresponsive to medical therapy. Nephrol Dial Transplant 1995; 10: Woodrow G, Davies S. Peritoneal dialysis in CKD. UK Renal Association; 30 July Gokal R, Alexander S, Ash S, et al. Peritoneal catheters and exit-site practices toward optimum peritoneal access: 1998 update. International Society for Peritoneal Dialysis. Perit Dial Int 1998; 18:
6 Table 1 Characteristics of included studies Study ID (author, year) Flanigan MJ et al 1994 Plum J et al 1997 Luzar MA et al 1990 N Study Design Setting Participants Intervention (experimental group) 93 Randomised 100 Randomised 127 Randomised Single centre America Multi centre Germany Multicentre, Europe PD patients PD patients with catheter tunnel infections PD patients Vancomycin plus Rifampin Oral Clindamycin Povidone iodine Intervention (control group) Trimethoprim / Sulfamethoxazole Intraperitoneal Clindamycin Simple soap Follow up (months) Comments Wilson APR et al Randomised UK PD patients Povidone iodine dry spray Standard protocol (alcohol wipes) 12 Table 2 Quality of randomised trials Study ID (author, year) Flanigan MJ et al 1994 Plum J et al 1997 Luzar MA et al 1990 Wilson APR et al 1997 Method of allocation concealment * Blinding (participants) (investigators) (outcome assessors) Intention-to-treat analysis Alternation Not stated Not stated Not stated Unclear 0% Open label trial No Not stated Not stated Unclear 9% Central Not stated Not stated Not stated Unclear 0% Central No Not stated Not stated Yes 2.7% Loss to follow up (%) * Choose between: central; third party (e.g. pharmacy); sequentially labelled opaque sealed envelopes; alternation; not specified. Choose between: yes; no; unclear.
7 Table 3a Results for dichotomous outcomes Study ID (author, year) Outcomes Intervention group (no. of patients with events/no. of patients exposed) Control group (no. of patients with events/no. of patients exposed) Relative risk (RR) [95% CI] Risk difference (RD) [95% CI] Flanigan MJ et al 1994 Peritonitis rate 22/44 24/ (95% CI: 0.73, 1.68) 0.05 (95% CI: -0.15, 0.25) Luzar MA et al 1990 Peritonitis rate (episode per patient year) 17/ / (95% CI: 0.47, 1.61) (95% CI: -0.19, 0.12) Luzar MA et al 1990 Exit site infection Exit site infection rate (episode per patient year) 15/ / (95% CI: 0.41, 1.45) (95% CI: -0.21, 0.09) Wilson APR et al 1997 Peritonitis rate (patient months per episode) 13/77 1: /72 1: (95% CI: 0.31, 1.15) (95% CI: -0.26, 0.03) Wilson APR et al 1997 Exit site infection (patient months per episode) 14/77 1: /72 1: (95% CI: 0.45, 1.68) (95% CI: -0.15, 0.10)
10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
TREATMENT OF PERITONEAL DIALYSIS (PD) RELATED PERITONITIS. General Principles
 WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
Current Trends in the Use of Peritoneal Dialysis Catheters
 Advances in Peritoneal Dialysis, Vol. 22, 2006 Dana Negoi, Barbara F. Prowant, Zbylut J. Twardowski The Tenckhoff catheter was developed in 1968 and has been widely used since for chronic peritoneal dialysis
Advances in Peritoneal Dialysis, Vol. 22, 2006 Dana Negoi, Barbara F. Prowant, Zbylut J. Twardowski The Tenckhoff catheter was developed in 1968 and has been widely used since for chronic peritoneal dialysis
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Improving outcomes in peritoneal dialysis exit site care Andrea Whittle & Kirsten Black
 Improving outcomes in peritoneal dialysis exit site care Andrea Whittle & Kirsten Black Whittle, A., & Black, K. (2014). Improving outcomes in peritoneal dialysis exit site care. Renal Society of Australasia
Improving outcomes in peritoneal dialysis exit site care Andrea Whittle & Kirsten Black Whittle, A., & Black, K. (2014). Improving outcomes in peritoneal dialysis exit site care. Renal Society of Australasia
A PROSPECTIVE RANDOMIZED STUDY ON THREE DIFFERENT PERITONEAL DIALYSIS CATHETERS
 Proceedings of the First Asian Chapter Meeting ISPD December 13 15, 2002, Hong Kong Peritoneal Dialysis International, Vol. 23 (2003), Supplement 2 0896-8608/03 $3.00 +.00 Copyright 2003 International
Proceedings of the First Asian Chapter Meeting ISPD December 13 15, 2002, Hong Kong Peritoneal Dialysis International, Vol. 23 (2003), Supplement 2 0896-8608/03 $3.00 +.00 Copyright 2003 International
Your Guide to Peritoneal Dialysis Module 3: Doing Peritoneal Dialysis at Home
 Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Your Guide to Peritoneal Dialysis Module 3: 6.0959 in Preparing to do PD One of the most important things about PD is to keep the dialysis area and anything that comes in contact with the PD equipment
Management of Catheters Infectious Diseases Working Party/Nurses Group
 Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Management of Catheters Infectious Diseases Working Party/Nurses Group Arno Mank RN PhD, Amsterdam (NL) www.ebmt.org London 09/04/2012 Content Background Management of CVC Types of CVC Care aspect of CVC
Recurrent and Relapsing Peritonitis: Causative Organisms and Response to Treatment
 Recurrent and Relapsing Peritonitis: Causative Organisms and Response to Treatment Cheuk-Chun Szeto, MD, FRCP, Bonnie Ching-Ha Kwan, MBBS, MCP(UK), Kai-Ming Chow, MBChB, MRCP(UK), Man-Ching Law, BN, RN,
Recurrent and Relapsing Peritonitis: Causative Organisms and Response to Treatment Cheuk-Chun Szeto, MD, FRCP, Bonnie Ching-Ha Kwan, MBBS, MCP(UK), Kai-Ming Chow, MBChB, MRCP(UK), Man-Ching Law, BN, RN,
Patient Training and Staff Education. Judith Bernardini University of Pittsburgh
 Patient Training and Staff Education Judith Bernardini University of Pittsburgh Outline This talk reviews the recommended steps to prepare the nurse to educate patients for home PD. Continuing education
Patient Training and Staff Education Judith Bernardini University of Pittsburgh Outline This talk reviews the recommended steps to prepare the nurse to educate patients for home PD. Continuing education
Are venous catheters safe in terms of blood tream infection? What should I know?
 Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Are venous catheters safe in terms of blood tream infection? What should I know? DIAGNOSIS, PREVENTION AND TREATMENT OF HAEMODIALYSIS CATHETER-RELATED BLOOD STREAM INFECTIONS (CRBSI): A POSITION STATEMENT
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Patient Training and Staff Education. Judith Bernardini University of Pittsburgh
 Patient Training and Staff Education Judith Bernardini University of Pittsburgh Outline This talk reviews the recommended steps to prepare the nurse to educate patients for home PD. Continuing education
Patient Training and Staff Education Judith Bernardini University of Pittsburgh Outline This talk reviews the recommended steps to prepare the nurse to educate patients for home PD. Continuing education
Care of Your Hickman Catheter
 Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
Care of Your Hickman Catheter Johns Hopkins Kimmel Cancer Center, Revised 7/11 Contents What is a Hickman Catheter? Page 3 Does the Catheter Limit My Activities? Page 4 How Do I Care for My Catheter? Page
MRSA. Living with. Acknowledgements. (Methicillin-Resistant Staphylococcus aureus)
 How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
How can I keep myself healthy? Hand washing and use of an alcohol-based hand sanitizer are the primary way to prevent acquiring or transmitting bacteria. If you get a cut or scrape, wash it well with soap
Treatment of dialysis catheter infection
 Treatment of dialysis catheter infection Date written: May 2012 Author: George Chin GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Treatment of dialysis catheter infection Date written: May 2012 Author: George Chin GUIDELINES No recommendations possible based on Level I or II evidence SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Insertion of a Peritoneal Dialysis Catheter under Local Anaesthetic
 Insertion of a Peritoneal Dialysis Catheter under Local Anaesthetic Information for patients about percutaneous placement of a Tenckhoff Catheter in the abdomen Exceptional healthcare, personally delivered
Insertion of a Peritoneal Dialysis Catheter under Local Anaesthetic Information for patients about percutaneous placement of a Tenckhoff Catheter in the abdomen Exceptional healthcare, personally delivered
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care
 Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Long-term urinary catheters: prevention and control of healthcare-associated infections in primary and community care A NICE pathway brings together all NICE guidance, quality standards and materials to
Tunneled Hemodialysis Catheters: Placement and complications
 Tunneled Hemodialysis Catheters: Placement and complications Arif Asif, M.D. Director, Interventional Nephrology Associate Professor of Medicine University of Miami, FL Tunneled Hemodialysis Catheters:
Tunneled Hemodialysis Catheters: Placement and complications Arif Asif, M.D. Director, Interventional Nephrology Associate Professor of Medicine University of Miami, FL Tunneled Hemodialysis Catheters:
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
DEPARTMENT OF RENAL NURSING PROTOCOLS AND PROCEDURES PERITONEAL DIALYSIS
 DEPARTMENT OF RENAL NURSING PROTOCOLS AND PROCEDURES PERITONEAL DIALYSIS Version Number: 3 Date Developed: April 07 Feb 08 Reason for change: Update Developed By: Dr. Neal Morgan, Johanna McWilliams CNM2,
DEPARTMENT OF RENAL NURSING PROTOCOLS AND PROCEDURES PERITONEAL DIALYSIS Version Number: 3 Date Developed: April 07 Feb 08 Reason for change: Update Developed By: Dr. Neal Morgan, Johanna McWilliams CNM2,
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Methicillin resistant staphylococcus aureus (MRSA)
 Methicillin resistant staphylococcus aureus (MRSA) Patient information Service: Infection Control Team Divison: Intergrated Medical and Rehabiltitation Services Infectioncontrol@homerton.nhs.uk Telephone
Methicillin resistant staphylococcus aureus (MRSA) Patient information Service: Infection Control Team Divison: Intergrated Medical and Rehabiltitation Services Infectioncontrol@homerton.nhs.uk Telephone
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Use of Packing for Surgical Wounds. Maggie Benson Clinical Problem Solving II
 Use of Packing for Surgical Wounds Maggie Benson Clinical Problem Solving II Purpose Present patient management s/p Incision and Drainage in an outpatient setting Examine evidence for the use of wound
Use of Packing for Surgical Wounds Maggie Benson Clinical Problem Solving II Purpose Present patient management s/p Incision and Drainage in an outpatient setting Examine evidence for the use of wound
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol
 Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol PURPOSE: To provide guidance for personnel in order to prevent the spread of Antibiotic Resistant Microorganisms
Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol PURPOSE: To provide guidance for personnel in order to prevent the spread of Antibiotic Resistant Microorganisms
Black Hills Healthcare System
 Black Hills Healthcare System Methicillin Resistant Staphylococcal Aureus (MRSA) Patient and Family Information What is MRSA? Staphylococcus Aureus, often referred to simply as staph, is a bacteria commonly
Black Hills Healthcare System Methicillin Resistant Staphylococcal Aureus (MRSA) Patient and Family Information What is MRSA? Staphylococcus Aureus, often referred to simply as staph, is a bacteria commonly
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California
 Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
Tuberculosis (TB) Screening Guidelines for Substance Use Disorder Treatment Programs in California 1 of 7 Table of Contents Preface 2 TB Symptoms and TB History 2 Initial Screening 2 Follow-Up Screening
Intra-abdominal abdominal Infections
 Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
4. Infection control measures
 4. Infection control measures Apart from general hygienic practices and vaccination, staff of institutions should also adopt specific infection control measures against communicable diseases. The measures
4. Infection control measures Apart from general hygienic practices and vaccination, staff of institutions should also adopt specific infection control measures against communicable diseases. The measures
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED
 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
Best Practice for Umbilical Cord Care. Kaitlin Robertson. Radford University School of Nursing
 Best Practice for 1 Running head: BEST PRACTICE FOR UMBILICAL Best Practice for Umbilical Cord Care Kaitlin Robertson Radford University School of Nursing Best Practice for 2 Significance During pregnancy
Best Practice for 1 Running head: BEST PRACTICE FOR UMBILICAL Best Practice for Umbilical Cord Care Kaitlin Robertson Radford University School of Nursing Best Practice for 2 Significance During pregnancy
If several different trials are mentioned in one publication, the data of each should be extracted in a separate data extraction form.
 General Remarks This template of a data extraction form is intended to help you to start developing your own data extraction form, it certainly has to be adapted to your specific question. Delete unnecessary
General Remarks This template of a data extraction form is intended to help you to start developing your own data extraction form, it certainly has to be adapted to your specific question. Delete unnecessary
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM
 ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults. A Systematic Review (Cochrane database August 2013)
 Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
VRE. Living with. Learning how to control the spread of Vancomycin-resistant enterococci (VRE)
 VRE Living with Learning how to control the spread of Vancomycin-resistant enterococci (VRE) CONTENTS IMPORTANT VRE is a serious infection that may become life-threatening if left untreated. If you or
VRE Living with Learning how to control the spread of Vancomycin-resistant enterococci (VRE) CONTENTS IMPORTANT VRE is a serious infection that may become life-threatening if left untreated. If you or
I. Questions for VAD slide program
 I. Questions for VAD slide program 1. The rate of central line associated blood stream infections (CLABSI) in the adult ICUs in Johns Hopkins Hospital is lower than the national average. 2. The mortality
I. Questions for VAD slide program 1. The rate of central line associated blood stream infections (CLABSI) in the adult ICUs in Johns Hopkins Hospital is lower than the national average. 2. The mortality
Addressing the challenge of healthcare associated infections (HCAIs) in Europe
 POSITION PAPER 05 January 2011 Addressing the challenge of healthcare associated infections (HCAIs) in Europe A Call for Action Page 1 of 8 A holistic approach to combating HCAIs in Europe We must rise
POSITION PAPER 05 January 2011 Addressing the challenge of healthcare associated infections (HCAIs) in Europe A Call for Action Page 1 of 8 A holistic approach to combating HCAIs in Europe We must rise
OUTLINE Supportive care management of the advanced CKD patient
 RENAL SUPPORTIVE CARE. NURSING EXPERIENCE AND PERSPECTIVES Renal Supportive Care Symposium 2013 Elizabeth Josland CNC OUTLINE Supportive care management of the advanced CKD patient Recognise patients who
RENAL SUPPORTIVE CARE. NURSING EXPERIENCE AND PERSPECTIVES Renal Supportive Care Symposium 2013 Elizabeth Josland CNC OUTLINE Supportive care management of the advanced CKD patient Recognise patients who
EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY. Methicillin-resistant Staph aureus: Management in the Outpatient Setting
 EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY Methicillin-resistant Staph aureus: Management in the Outpatient Setting Date Originated: Date Reviewed: Date Approved: Page 1 of Approved by: Department
EAST CAROLINA UNIVERSITY INFECTION CONTROL POLICY Methicillin-resistant Staph aureus: Management in the Outpatient Setting Date Originated: Date Reviewed: Date Approved: Page 1 of Approved by: Department
TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management
 TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management WHY IS THIS IMPORTANT? Depression causes fluctuations in mood, low self esteem and loss of interest or pleasure in normally
TECHNICAL/CLINICAL TOOLS BEST PRACTICE 7: Depression Screening and Management WHY IS THIS IMPORTANT? Depression causes fluctuations in mood, low self esteem and loss of interest or pleasure in normally
healthcare associated infection 1.2
 healthcare associated infection A C T I O N G U I D E 1.2 AUSTRALIAN SAFETY AND QUALITY GOALS FOR HEALTH CARE What are the goals? The Australian Safety and Quality Goals for Health Care set out some important
healthcare associated infection A C T I O N G U I D E 1.2 AUSTRALIAN SAFETY AND QUALITY GOALS FOR HEALTH CARE What are the goals? The Australian Safety and Quality Goals for Health Care set out some important
Tunneled Central Venous Catheter (CVC) Placement
 PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
PATIENT EDUCATION patienteducation.osumc.edu Tunneled Central Venous Catheter (CVC) Placement A tunneled Central Venous Catheter (CVC) is a special type of intravenous (IV) line that is placed into a large
INFECTION CONTROL PRECAUTIONS
 INFECTION CONTROL PRECAUTIONS Outline Standard Precautions Droplet Precautions Contact Precautions Airborne Precautions References STANDARD PRECAUTIONS Use Standard Precautions, or the equivalent, for
INFECTION CONTROL PRECAUTIONS Outline Standard Precautions Droplet Precautions Contact Precautions Airborne Precautions References STANDARD PRECAUTIONS Use Standard Precautions, or the equivalent, for
Primary prevention of chronic kidney disease: managing diabetes mellitus to reduce the risk of progression to CKD
 Primary prevention of chronic kidney disease: managing diabetes mellitus to reduce the risk of progression to CKD Date written: July 2012 Author: Kate Wiggins, Graeme Turner, David Johnson GUIDELINES We
Primary prevention of chronic kidney disease: managing diabetes mellitus to reduce the risk of progression to CKD Date written: July 2012 Author: Kate Wiggins, Graeme Turner, David Johnson GUIDELINES We
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
Living healthy with MRSA
 Stamford Health System Having MRSA means what? Living healthy with MRSA Discharge information for patients and families WASHING YOUR HANDS IS THE KEY!!! Staph aureus is a bacteria that lives on your skin
Stamford Health System Having MRSA means what? Living healthy with MRSA Discharge information for patients and families WASHING YOUR HANDS IS THE KEY!!! Staph aureus is a bacteria that lives on your skin
Organization and Structure of a Peritoneal Dialysis Program: an important ingredient for success
 Organization and Structure of a Peritoneal Dialysis Program: an important ingredient for success Fredric O. Finkelstein Hospital of St. Raphael, Yale University New Haven. CT 1 Overview of Presentation
Organization and Structure of a Peritoneal Dialysis Program: an important ingredient for success Fredric O. Finkelstein Hospital of St. Raphael, Yale University New Haven. CT 1 Overview of Presentation
case management controlled
 The effecte ffects s of a nurse-led case management programme on patients undergoing peritoneal dialysis: a randomized controlled trial Susan Chow RN, PhD The HK Polytechnic University Frances Wong RN,
The effecte ffects s of a nurse-led case management programme on patients undergoing peritoneal dialysis: a randomized controlled trial Susan Chow RN, PhD The HK Polytechnic University Frances Wong RN,
PD the Good Catheter
 PD the Good Catheter Joseph J. Naoum, MD., FACS. Assistant Professor, Weill Cornell Medical College The Methodist Hospital, Division of Vascular Surgery Cardiovascular Surgery Associates 6550 Fannin St.,
PD the Good Catheter Joseph J. Naoum, MD., FACS. Assistant Professor, Weill Cornell Medical College The Methodist Hospital, Division of Vascular Surgery Cardiovascular Surgery Associates 6550 Fannin St.,
Components of CVC Care Bundle. selection
 Components of CVC Care Bundle Catheter site selection Site of insertion influences the subsequent risk for CR-BSI and phlebitis The influence of site is related in part to the risk for thrombophlebitis
Components of CVC Care Bundle Catheter site selection Site of insertion influences the subsequent risk for CR-BSI and phlebitis The influence of site is related in part to the risk for thrombophlebitis
Environmental Management of Staph and MRSA in Community Settings July 2008
 Page 1 of 7 Environmental Management of Staph and MRSA in Community Settings July 2008 Questions addressed on this page What are Staph and MRSA? How is Staph and MRSA spread? What is the role of the environment
Page 1 of 7 Environmental Management of Staph and MRSA in Community Settings July 2008 Questions addressed on this page What are Staph and MRSA? How is Staph and MRSA spread? What is the role of the environment
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Tenckhoff Peritoneal Dialysis Catheter Insertion in a Northern Ireland District General Hospital.
 Ulster Med J 2015;84(3):166-170 Paper Tenckhoff Peritoneal Dialysis Catheter Insertion in a Northern Ireland District General Hospital. Donna McCartan 1, Ronan Gray 1,2, John Harty 3, Geoff Blake 1. Accepted:
Ulster Med J 2015;84(3):166-170 Paper Tenckhoff Peritoneal Dialysis Catheter Insertion in a Northern Ireland District General Hospital. Donna McCartan 1, Ronan Gray 1,2, John Harty 3, Geoff Blake 1. Accepted:
Solid Organ Transplantation
 Solid Organ Transplantation Infection Prevention And Control Transplant Atlantic 2011 October 13/2011 Kathy Hart Introduction In the past several years, the drugs that we use, the surgeries themselves,
Solid Organ Transplantation Infection Prevention And Control Transplant Atlantic 2011 October 13/2011 Kathy Hart Introduction In the past several years, the drugs that we use, the surgeries themselves,
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Canine Lymphoma Frequently Asked Questions by Pet Owners
 Canine Lymphoma Frequently Asked Questions by Pet Owners What is lymphoma? The term lymphoma describes a diverse group of cancers in dogs that are derived from white blood cells called lymphocytes. Lymphocytes
Canine Lymphoma Frequently Asked Questions by Pet Owners What is lymphoma? The term lymphoma describes a diverse group of cancers in dogs that are derived from white blood cells called lymphocytes. Lymphocytes
Infection control. Self-study course
 Infection control Self-study course Course objectives By the end of this course you will be able to: 1) Define a germ 2) Define the environment that a germ needs to live and grow 3) Explain the chain of
Infection control Self-study course Course objectives By the end of this course you will be able to: 1) Define a germ 2) Define the environment that a germ needs to live and grow 3) Explain the chain of
High Impact Intervention Central venous catheter care bundle
 High Impact Intervention Central venous catheter care bundle Aim To reduce the incidence of catheter related bloodstream infection (CRBSI). Introduction The aim of the care bundle, as set out in this high
High Impact Intervention Central venous catheter care bundle Aim To reduce the incidence of catheter related bloodstream infection (CRBSI). Introduction The aim of the care bundle, as set out in this high
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015
 Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Maria Dalbey RN. BSN, MA, MBA March 17 th, 2015 2 Objectives Participants will be able to : Understand the Pathogenesis of Tuberculosis (TB) Identify the Goals of Public Health for TB Identify Hierarchy
Surgical Site Infection Prevention
 Surgical Site Infection Prevention 1 Objectives 1. Discuss risk factors for SSI 2. Describe evidence-based best practices for SSI prevention 3. State principles of antibiotic prophylaxis 4. Discuss novel
Surgical Site Infection Prevention 1 Objectives 1. Discuss risk factors for SSI 2. Describe evidence-based best practices for SSI prevention 3. State principles of antibiotic prophylaxis 4. Discuss novel
Advice for those affected by MRSA outside of hospital
 Advice for those affected by MRSA outside of hospital If you have MRSA this leaflet provides information and advice for managing your day-to-day life. 1 About MRSA There are lots of different types or
Advice for those affected by MRSA outside of hospital If you have MRSA this leaflet provides information and advice for managing your day-to-day life. 1 About MRSA There are lots of different types or
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: infusion_therapy_in_the_home 3/1998 2/2016 2/2017 2/2016 Description of Procedure or Service Home infusion
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: infusion_therapy_in_the_home 3/1998 2/2016 2/2017 2/2016 Description of Procedure or Service Home infusion
BestPractice. Evidence Based Practice Information Sheets for Health Professionals. This Practice Information Sheet Covers The Following Concepts:
 Volume 2, Issue 1, 1998 ISSN 1329-1874 BestPractice Evidence Based Practice Information Sheets for Health Professionals Purpose The purpose of this practice information sheet is to provide summarised best
Volume 2, Issue 1, 1998 ISSN 1329-1874 BestPractice Evidence Based Practice Information Sheets for Health Professionals Purpose The purpose of this practice information sheet is to provide summarised best
DECISION AND SUMMARY OF RATIONALE
 DECISION AND SUMMARY OF RATIONALE Indication under consideration Clinical evidence Clofarabine in the treatment of relapsed acute myeloid leukaemia (AML) The application was for clofarabine to remain in
DECISION AND SUMMARY OF RATIONALE Indication under consideration Clinical evidence Clofarabine in the treatment of relapsed acute myeloid leukaemia (AML) The application was for clofarabine to remain in
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
The true cost of wounds. And how to reduce it
 The true cost of wounds And how to reduce it Wounds are a growing challenge Wounds have been called the silent epidemic. In a typical hospital setting today, between 25% and 40% of beds will be occupied
The true cost of wounds And how to reduce it Wounds are a growing challenge Wounds have been called the silent epidemic. In a typical hospital setting today, between 25% and 40% of beds will be occupied
Site Care of Your Central Venous Catheter Sterile
 Site Care of Your Central Venous Catheter Sterile Dressing Change Sterile Technique The skin surrounding your catheter s exit site must be kept clean, and a new sterile dressing should be applied on a
Site Care of Your Central Venous Catheter Sterile Dressing Change Sterile Technique The skin surrounding your catheter s exit site must be kept clean, and a new sterile dressing should be applied on a
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Value of Ultrasound-guided Irrigation and Drainage of
 Value of Ultrasound-guided Irrigation and Drainage of Refractory Pyocysts in ADPKD 1. Daryoush Saedi M.D., Department of Radiology, Hasheminejad Kidney Center, School of Medicine, Iran University of Medical
Value of Ultrasound-guided Irrigation and Drainage of Refractory Pyocysts in ADPKD 1. Daryoush Saedi M.D., Department of Radiology, Hasheminejad Kidney Center, School of Medicine, Iran University of Medical
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Central Venous Catheter (CVC) Sterile Dressing Change - The James
 PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
PATIENT EDUCATION patienteducation.osumc.edu Central Venous Catheter (CVC) Sterile Dressing Change - The James A dressing protects your catheter site and helps reduce the risk of infection. You will need
PG Certificate / PG Diploma / MSc in Clinical Pharmacy
 PG Certificate / PG Diploma / MSc in Clinical Pharmacy Programme Information September 2014 Entry School of Pharmacy Queen s University Belfast Queen s University Belfast - Clinical Pharmacy programme
PG Certificate / PG Diploma / MSc in Clinical Pharmacy Programme Information September 2014 Entry School of Pharmacy Queen s University Belfast Queen s University Belfast - Clinical Pharmacy programme
HICKMAN Catheter Care with a Needleless Connector
 HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
HICKMAN Catheter Care with a Needleless Connector Table of Contents Part 1 Learning about the HICKMAN Catheter... 2 Part 2 Caring for Your Hickman Catheter... 3 A. Preventing Infection... 3 B. Bathing...
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY
 STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
Bloodborne Pathogens (BBPs) Louisiana Delta Community College
 Bloodborne Pathogens (BBPs) Louisiana Delta Community College 1 Bloodborne Pathogens Rules & Regulations Office of Risk Management (ORM) requires development of a bloodborne pathogens plan low risk employees
Bloodborne Pathogens (BBPs) Louisiana Delta Community College 1 Bloodborne Pathogens Rules & Regulations Office of Risk Management (ORM) requires development of a bloodborne pathogens plan low risk employees
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations. J. Stuart Wolf, Jr., M.D.
 Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Wound Care on the Field. Objectives
 Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Wound Care on the Field Brittany Witte, PT, DPT Cook Children s Medical Center Objectives Name 3 different types of wounds commonly seen in sports and how to emergently provide care for them. Name all
Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * COLLECTION OF CASE STUDIES
 COLLECTION OF CASE STUDIES Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * *All patients were treated with systemic antibiotics Post-surgical V.A.C. VeraFlo
COLLECTION OF CASE STUDIES Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * *All patients were treated with systemic antibiotics Post-surgical V.A.C. VeraFlo
Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC
 Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC 1 Clostridium difficile (C.difficile) Antibiotic induced diarrhea Can cause pseudomembranous colitis Most common cause of acute infectious
Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC 1 Clostridium difficile (C.difficile) Antibiotic induced diarrhea Can cause pseudomembranous colitis Most common cause of acute infectious
BLOODBORNE PATHOGENS EXPOSURE CONTROL PROGRAM
 BLOODBORNE PATHOGENS EXPOSURE CONTROL PROGRAM Purpose: The purpose of this program is to eliminate or minimize employee and student exposure to blood and other potentially infectious materials. This exposure
BLOODBORNE PATHOGENS EXPOSURE CONTROL PROGRAM Purpose: The purpose of this program is to eliminate or minimize employee and student exposure to blood and other potentially infectious materials. This exposure
Section 6: Your Hemodialysis Catheter
 Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
41 Assisting with Minor Surgery
 Learning Outcomes 41.1 Define the medical assistant s role in minor surgical procedures. 41-2 CHAPTER 41 Assisting with Minor Surgery 41.2 Describe types of wounds and explain how they heal. 41.3 Describe
Learning Outcomes 41.1 Define the medical assistant s role in minor surgical procedures. 41-2 CHAPTER 41 Assisting with Minor Surgery 41.2 Describe types of wounds and explain how they heal. 41.3 Describe
An Infusion of Quality and Safety STAT!
 Quality is not an act, it is a habit. Aristotle An Infusion of Quality and Safety STAT! Quality is not an act, it is a habit. Mary Kakenmaster MSN, RN, CNE Oakton Community College mkakenma@oakton.edu
Quality is not an act, it is a habit. Aristotle An Infusion of Quality and Safety STAT! Quality is not an act, it is a habit. Mary Kakenmaster MSN, RN, CNE Oakton Community College mkakenma@oakton.edu
Training the PD Patient. Judith Bernardini University of Pittsburgh
 Training the PD Patient Judith Bernardini University of Pittsburgh Nurses as teachers: Most health professionals have little or no formal background in the principles of education The complexity of the
Training the PD Patient Judith Bernardini University of Pittsburgh Nurses as teachers: Most health professionals have little or no formal background in the principles of education The complexity of the
Assuring Data Quality
 Assuring Data Quality Jennie Wilson Programme Leader SSI Surveillance Dept. of Healthcare-Associated Infection & Antimicrobial Resistance, Health Protection Agency SSI cumulative incidence (%) 8.0% 7.0%
Assuring Data Quality Jennie Wilson Programme Leader SSI Surveillance Dept. of Healthcare-Associated Infection & Antimicrobial Resistance, Health Protection Agency SSI cumulative incidence (%) 8.0% 7.0%
Nosocomial Bloodstream infection. Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
 Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Educational Module for Nursing Assistants in Long-term Care Facilities: Antibiotic Use and Antibiotic Resistance
 Educational Module for Nursing Assistants in Long-term Care Facilities: Antibiotic Use and Antibiotic Resistance Antibiotic resistance is an increasing concern for everyone. This module: Defines antibiotic
Educational Module for Nursing Assistants in Long-term Care Facilities: Antibiotic Use and Antibiotic Resistance Antibiotic resistance is an increasing concern for everyone. This module: Defines antibiotic
SECTION 12.1 URINARY CATHETERS
 SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
