33 Botulinum Toxin Type A in the Management of Oromandibular Dystonia and Bruxism
|
|
|
- Marylou Gibbs
- 8 years ago
- Views:
Transcription
1 Scientific and Therapeutic Aspects of Botulinum Toxin edited by M.F. Brin, J. Jankovic, and M. Hallett Lippincott Williams & Wilkins, Philadelphia, Botulinum Toxin Type A in the Management of Oromandibular Dystonia and Bruxism Ron Tintner and Joseph Jankovic Oromandibular dystonia (OMD) refers to involuntary spasms of masticatory, lingual, and pharyngeal muscles. Phenomenologically, there are seven types of OMD: jaw-closing dystonia (JCD); jaw-opening dystonia (JOD); jaw-deviation dystonia (JDD); lip and perioral dystonia; lingual dystonia; pharyngeal dystonia; and combination OMD (1). OMD may be seen in isolation (focal dystonia), as part of a more widespread segmental cranial dystonia, or as part of a multisegmental or generalized dystonia. In 1910, the French neurologist Henry Meige described a syndrome, sometimes still referred to as Meige s syndrome, that occurred predominantly in middle-aged women and consisted of spasms of the eyelids as well as contractions of the pharyngeal, jaw, and tongue muscles (2). Because Meige was not the first to describe the disorder (Horatio Wood, a Philadelphia neurologist, described facial and oromandibular dystonia in 1887) (3), the syndrome is now more accurately referred to as cranial dystonia. The etiologies of OMD are diverse (Table 33.1). The leading cause is primary (idiopathic) dystonia, which is often associated with other dystonias, particularly cervical and cranial. Some cases of OMD may be manifestations of inherited disorders; however, DYT1 dystonia, caused by a mutation of the torsina gene on chromosome 9q34, the most common form of inherited dystonia, rarely involves the cranial structures (4). A patient with adult-onset OMD and no obvious family history of dystonia has Throughout this chapter n m refers to mean SD, unless indicated otherwise. been reported with a mutation of the gene for GTP cyclohydrolase 1, which causes the syndrome of dopa-responsive dystonia (5). The patient responded well to treatment with L-dopa. In addition to the primary dystonias, other common causes of OMD are drugs (tardive OMD) and peripheral injury, such as dental procedures and jaw trauma (6,7). Until the advent of botulinum toxin (BTX) therapy, systemic pharmacologic agents were the traditional mainstay of treatment for OMD. Anticholinergics (e.g., trihexyphenidyl, benztropine), benzodiazepines (e.g., clonazepam, lorazepam, diazepam), baclofen, and tetrabenazine (which deplete dopamine and block dopamine receptors), were useful in some patients (8). Chronic systemic pharmacotherapy, however, is largely unsatisfactory because of modest improvements and frequent side effects, resulting in a low therapeutic ratio. Dental appliances have occasionally been helpful (9). There are no effective regional denervating surgical procedures, such as those used for cervical dystonia or blepharospasm. Central stereotactic surgery, such as pallidotomy (10) and deep brain stimulation (11) have been used successfully for treatment of generalized and hemidystonias, but there is no information regarding their use for more limited craniofacial dystonias. The remainder of this review focuses on regional procedures, particularly chemodenervation with BTX. The pharmacology of BTX and the mechanisms by which this potent biologic toxin produces local chemodenervation, benefiting patients with involuntary muscular spasms such as 343
2 344 SCIENTIFIC AND THERAPEUTIC ASPECTS OF BOTULINUM TOXIN TABLE Etiology of abnormal jaw and mouth movements Dystonias Primary (idiopathic) dystonia Inherited dystonia syndromes X-linked dystonia parkinsonism (Lubag); locus: DYT3 Dopa-responsive dystonia; locus: DYT5 Adult-onset idiopathic torsion dystonia of mixed type; locus: DYT6 Focal, adult-onset idiopathic torsion dystonia; locus: DYT7 Adult- and juvenile-onset idiopathic torsion dystonia of mixed type and mild severity; locus: DYT13 Secondary dystonias Drug-induced (dopamine receptor-blocking drugs, levodopa, and some serotonin reuptake inhibitors) Anoxic brain damage Peripheral dystonia (posttraumatic after oromandibular or dental injury or surgery) Neurodegenerative disorders with dystonia Parkinson s disease (jaw tremor and levodopa-induced dyskinesias) Multiple system atrophy (especially that caused by levodopa-induced dyskinesias) Progressive supranuclear palsy Huntington s disease Bruxism (idiopathic, diurnal, mental retardation, neurodegenerative disorders) Hemimasticatory spasm Hemifacial spasm Satoyoshi s syndrome those seen in OMD, are discussed elsewhere in this volume and in other reviews (12 14). Although denervation of motor endplates has been proposed as the leading mechanism of action of BTX in dystonia, including OMD (15), there are certain paradoxes about its action that are not fully explained (16). First, the clinical effect of BTX appears to continue beyond the point of inducing weakness. Second, although BTX has been thought to affect muscle spindles, it is effective in the treatment of facial spasms, even though facial muscles are void of muscle spindles (17). Third, BTX treatment decreases sensory symptoms, including premonitory sensations experienced by patients with tics and dystonia (see Chapter 32 regarding the treatment of tics with BTX). Finally, there is controversy as to the role of central effects of BTX in patients with dystonia. Transcranial magnetic stimulation of the motor cortex in patients with limb dystonia has been used to demonstrate that BTX can transiently alter intracortical inhibition (18) and normalize distorted primary motor cortex projections to hand and forearm muscles. Secondary alteration of central sensorimotor physiology and an additional primary effect on muscle spindle function are probably critical in the longterm efficacy of BTX in dystonia (19,20). To test this hypothesis directly, blockade of muscular afferents has been performed. Yoshida et al. (21) treated 13 patients with OMD resistant to pharmacotherapy or dental treatment by injecting diluted lidocaine and alcohol intramuscularly to reduce muscle spindle afferent activity. All patients reportedly showed clinical improvement after this therapy with reduced electromyographic (EMG) activities in the affected muscles. The overall subjective improvement was 57.7% 25.1% (mean SD) on a self-rating scale. There was a 70% mean improvement in JCD, which was significantly higher than the 38% improvement in JOD. This mode of therapy may turn out to be useful when more experience is obtained and should ultimately be compared directly with BTX. MUSCLE SELECTION Ideally, one should be able to determine which muscles are primarily involved in the abnormal movements, and inject these muscles with the appropriate dose of BTX, thus affecting only those actions involved in the production of the abnormal movement or posture. Table 33.2 lists TABLE Muscles affecting jaw and tongue movement Muscle Actions Masseter Temporalis Internal pterygoid Digastric External pterygoid Genioglossus Hyoglossus Geniohyoid Mylohyoid Jaw closing Jaw closing; anterior fibers assist in jaw opening and deviation Jaw closing Jaw opening Jaw opening; jaw deviation to opposite side and protrusion Tongue protrusion Tongue protrusion Jaw opening Elevation of hyoid; jaw opening
3 BOTULINUM TOXIN TYPE A IN OROMANDIBULAR DYSTONIA AND BRUXISM 345 the muscles involved in oromandibular function and their actions. As can be seen, any given movement can be produced by several muscles. The masseters, temporalis or internal (medial) pterygoids represent potential injection targets for JCD, and the submental muscles or external (lateral) pterygoids for JOD. Palpation may be helpful in this approach, but not all muscles are palpable. Another approach might be to monitor muscle activity by EMG and inject those muscles that show increased activity during the particular abnormal movement or posture. This is, however, not always possible because EMG recordings of all involved muscles during action dystonia, such as OMD, are technically difficult. In some forms of focal dystonia, the pattern of muscle involvement may change over time (22). Furthermore, dystonia is a disorder of the CNS and specified at the level of movements, not muscles, adding to the complexity of treatment. These issues remain unresolved and studies directly comparing various modes and dosage of BTX administration remain to be done. Thus, different methods of muscle selection, techniques of injection, and assessment of response account for the observed differences across different studies. RESULTS OF TRIALS OF BTX IN OMD Many anecdotal and small case series detailing response of OMD to BTX have been reported (23 27), including one using a primary qualityof-life measure (28). We restrict our discussion, however, to the two large case series published. These reports also have the advantage of being relatively recent; i.e., after preliminary experience has allowed refinement of techniques and assessments of results. In the experience reported by the group at Columbia University College of Physicians and Surgeons (CPS), muscle selection was made using EMG and a relatively large number of muscles were considered (29). In the other study, conducted at Baylor College of Medicine (BCM), muscle selection was based on clinical observation and examination coupled with extensive, long-term experience (30). Both groups used BOTOX (Allergan Pharmaceuticals) preparation of BTX type A (BTX-A). Brin et al. (29) described their experience with 96 patients with OMD. Onset was generally when the patients ages were in the mid-40s, but the ages at injection and duration of symptoms are not given. More than 70% of patients in all movement groups had idiopathic OMD. Response was rated primarily by a subjective linear scale, in which subjects were asked to assess their percent normal function from 0% to 100%. All muscles involved in jaw motion were considered for injection. EMG was always used to inject the pterygoids and usually to inject the other muscles. In all movement categories, patients function improved from about 30% of normal function to about 74% after BTX-A treatment. JDD patients started from a higher baseline (39%) with the same final functional status, and thus showed less percent change; however, only five patients were treated. Adverse effects were seen in 13 of 96 (14%) patients and at 29 of 481 (6%) visits. Of 14 instances of dysphagia, only one was severe enough to require a change in diet. Most of the cases of dysphagia were seen in patients with JOD and were associated with injection of the digastrics. The details of the demographics and response of individual subgroups and muscles are given in Tables 33.3, 33.4, and The au- TABLE Distribution of types of oromandibular dystonia in case series from Columbia University College of Physicians and Surgeons (CPS) and Baylor College of Medicine (BCM) BCM CPS Distribution Percent (number) Percent (number) Jaw-closing dystonia 52.5% (85) 53.1% (51) Jaw-opening dystonia 21.6 (35) 41.7 (40) Jaw-deviation dystonia 1.9 (3) 5.2 (5) Mixed jaw-movement dystonia 24.0 (39)
4 346 SCIENTIFIC AND THERAPEUTIC ASPECTS OF BOTULINUM TOXIN TABLE BTX-A doses in JCD and JOD in case series from Columbia University College of Physicians and Surgeons (CPS) and Baylor College of Medicine (BCM) Muscle BCM (BOTOX Units) CPS (BOTOX Units) Masseter 54.2 (25 to 100) 24.5 (2 to 100) Temporalis 18.5 (2 to 75) Medial pterygoid 16.3 (5 to 40) Lateral pterygoid 15.9 (2.5 to 60) Anterior digastric 9.8 (3.75 to 30) Submentalis 28.6 (10 to 200) thors do not describe how they verified the placement of the EMG electrode in a particular muscle. For other aspects of the controversy associated with EMG-guided BTX injections, the reader is referred to a recently published review (31). Tan and Jankovic (30) reported their longterm experience with BTX-A for OMD. Of 202 patients seen from 1988 through 1998, diagnosed clinically to have OMD in a movement disorders clinic over a period of 10 years, 162 patients satisfied the study inclusion criteria of being refractory to other treatments, having at least one follow-up visit and having symptoms of sufficient severity to interfere with swallowing, speech or chewing. The mean age was years and the mean follow-up period was years. The masseters and submental muscles were the only two muscle groups injected with BTX-A for JCD and JOD, respectively, in this group of patients. More than half (52.5%) of the patients had JCD. A total of 2,529 BTX-A treatments were administered into the masseter muscles, submental muscles, or both during a total of 1,213 treatment visits. The mean doses of BTX-A (per side) were U for the masseters and U for the submental muscles. The overall mean total duration of response was weeks. The primary efficacy variable was the global effect of BTX-A. To calculate the global effect score, the peak effect (range 0 to 4, where 4 complete abolition of the dystonia and 0 no effect) is decreased by 1 if mild adverse effect occurred and by 2 if more severe adverse effect was experienced. The mean global effect of BTX-A was Of the JCD patients, 80% (68 of 85) responded with a score 3 (i.e., moderate to marked improvement); 40% (14 of 35) of JOD, 33% (1 of 3) of JDD, and 52% (16 of 31) of the mixed patients. Fifty-one (31.5%) patients reported adverse effects with BTX-A in at least one visit. Complications such as dysphagia and dysarthria were reported in 135 (11.1%) of all treatment visits. There was a poorer re- TABLE Therapeutic and adverse effects of BTX-A in JCD and JOD in case series from Columbia University College of Physicians and Surgeons (CPS) and Baylor College of Medicine (BCM)* BCM CPS Jaw-closing dystonia Effect (ultimate % normal function) Duration (weeks; mean SD) Adverse events: % of patients Adverse events: % of visits Jaw-opening dystonia Effect (ultimate % normal function) Duration (weeks; mean SD) Adverse events: % of patients Adverse events: % of visits *A comparison of the two studies is not entirely appropriate because of different methods of patient selection, assessment of results and adverse effects, injection techniques, and other differences.
5 BOTULINUM TOXIN TYPE A IN OROMANDIBULAR DYSTONIA AND BRUXISM 347 sponse and higher complication rate with JOD than with the other types of OMD (Tables ). Because of different methods of patient and muscle selection, different methods of assessing severity, response, and adverse effects, and different injection techniques, it is impossible to compare the two studies; the overall results, however, appear to be similar. Both studies found that, as compared to JCD, JOD is associated with a higher frequency of adverse effects. While the BCM group reported a longer duration of benefit as compared to the CPS group, there was a higher frequency of adverse effects, probably related to higher dose of BTX-A, higher sensitivity of reporting adverse effects, or both. The higher dose may have been necessitated by greater severity of OMD in the BCM patient population. During the past several years we have modified our technique by directing the injection needle and administering the total dosage as a single bolus into the most anterior portion of the submental complex; this has resulted in a marked reduction in dysphagia and other complications. The CPS group preferentially injects the external pterygoids, and if necessary, adds the digastrics and submentals. TONGUE PROTRUSION DYSTONIA Tongue protrusion dystonia (TPD) usually interferes with speech and chewing and is most frequently seen in patients with tardive dystonia and with primary (idiopathic) cranial dystonia, but this form of lingual dystonia is also typically present in patients with neuroacanthocytosis. Treatment of this form of focal dystonia is particularly challenging because medications are universally ineffective (except possibly tetrabenazine in tardive lingual dystonia), and BTX- A injections into the tongue muscles can result in severe dysarthria and dysphagia, which are rarely associated with aspiration requiring intubation for airway protection (32). Gelb et al. reported their experience with 13 patients with TPD (21). They injected an average of 18.3 U (range, 10 to 27) into the genioglossus and hypoglossus muscles, although the exact location of the EMG needle could not be confirmed. The patients function improved from 32% to 76% of normal function and the effect lasted weeks. Adverse events were seen in 38.5% of patients and 13% of visits. Five patients developed dysarthria and dysphagia, requiring a change in diet; one developed aspiration pneumonia. Charles et al. (33) performed a retrospective analysis of clinical findings and results of BTX- A treatment in 9 patients treated at Vanderbilt between 1989 and After unsuccessful treatment with conventional oral medications the patients were injected with BTX-A into their genioglossus muscles at four sites via a submandibular approach. A marked reduction in tongue protrusion was achieved in six patients (67%). Of 35 consecutive injections, 83% were successful at reducing tongue protrusion. Mild dysphagia complicated 14% of the injections. The average dose injected was 34 3 U and the average duration of effect was 15 2 weeks. Because the various muscles involved in tongue protrusion cannot be reliably differentiated clinically or by EMG sampling, we prefer the term submental muscles rather than naming individual muscles layered in the submental area. These muscles are involved in various functions, including tongue protrusion and jaw opening. BRUXISM AND OTHER OROMANDIBULAR SYNDROMES Bruxism is a diurnal or nocturnal activity that consists of clenching, grinding, bracing, and gnashing of the teeth. Its exact prevalence is unknown, but it is probably much more common than thought because the vast majority of patients with bruxism probably never seek medical attention and the disorder is often misdiagnosed as TMJ (temporomandibular joint) syndrome, although TMJ may occur as a secondary complication of bruxism. Some view bruxism as a form of OMD; it was present in 78.5% of 79 patients with cranial-cervical dystonia (34). Besides dystonia, bruxism can also be seen in a variety of other disorders, particularly mental retardation
6 348 SCIENTIFIC AND THERAPEUTIC ASPECTS OF BOTULINUM TOXIN and other forms of CNS damage, as well as neurodegenerative disorders such as Huntington s disease (35). In an open trial, Tan and Jankovic (36) studied 18 subjects with severe bruxism lasting an average of years (range, 3 to 40). A total of 241 injections of BTX-A were administered in the masseter muscles during 123 treatment visits. The mean dose of the BTX-A was U (range, 25 to 100 U) per masseter muscle on one side. The mean total duration of response was weeks (range, 6 to 78), and the mean peak effect on a scale of 0 to 4, in which 4 is equal to total abolishment of grinding, was Only one subject (5.6%) reported having experienced dysphagia. OTHER OROMANDIBULAR CONDITIONS Freund et al. (37) evaluated subjective and objective responses to treatment with BTX-A in an uncontrolled study of a group of 46 patients with various TMJ disorders. Both masseter muscles were injected with 50 U each and both temporalis muscles with 25 U each under EMG guidance. Subjects were assessed at 2-week intervals for 8 weeks. Outcome measures included subjective assessment of pain by visual analog scale (VAS), measurement of mean maximum voluntary contraction (MVC), interincisal oral opening, tenderness to palpation, and a functional index based on multiple VAS. There were significant differences in all median outcome measures between the pretreatment assessment and the four follow-up assessments except for MVC. Although MVC was significantly reduced midway through the study, it had returned to pretreatment values by the final two assessments. All other outcome measures remained significantly different from the pretreatment findings. Paired correlation of variables including age, sex, diagnosis, depression index, and time of onset showed no significant differences. BTX-A injections produced significant improvements in pain, function, mouth opening, and tenderness to palpation. MVC initially diminished and then returned to the initial values. Reduced severity of symptoms and improved functional abilities seemed to have extended beyond the period of the muscle-relaxing effects of BTX-A. A case of recurrent dislocations of the TMJ because of spasticity from multiple sclerosis has been reported (38). This resolved for periods of up to 4 months following chemodenervation of the masseter and pterygoid muscles with injections of BTX-A. Hemimasticatory spasm is a rare disorder of the trigeminal nerve that produces involuntary jaw closure as a result of unilateral contractions of jaw-closing muscles (39). It is sometimes associated with facial hemiatrophy. The masseter inhibitory reflex is absent during periods of spasm. Needle EMG demonstrates irregular bursts of motor unit potentials that are identical to the pattern observed in hemifacial spasm. The electrophysiologic findings suggest ectopic excitation of the trigeminal motor root or its nucleus, an abnormality that is analogous to ectopic excitation of the facial nerve in hemifacial spasm. This ectopic excitation can be caused by peripheral irritation of the trigeminal nerve itself, entrapment of the motor branches in the infratemporal fossa or focal demyelination of motor branches of the trigeminal nerve. Hemimasticatory spasm has been reported to respond to BTX-A in several case reports (30 42). Masticatory muscle spasms caused by Satoyoshi s syndrome have also been successfully treated with BTX-A (43). CONCLUSIONS AND REMAINING QUESTIONS In summary, BTX-A is now considered the treatment of choice for OMD. Injection into the masseter (and possibly temporalis and internal pterygoids) usually results in marked improvement of JCD and associated bruxism. In JOD, injection of BTX-A into the submental muscles and/ or the external pterygoids is usually associated with a robust improvement in jaw opening and dysarthria, although a small percentage of patients may develop transient dysphagia, which can be minimized by directing the injection into the most anterior portion of the submental complex. BTX-A treatment of TPD is also usually
7 BOTULINUM TOXIN TYPE A IN OROMANDIBULAR DYSTONIA AND BRUXISM 349 highly successful, although this procedure carries a risk of dysphagia. There are many unanswered questions that should be addressed by future studies. How do we optimize the therapeutic ratio, especially in JOD and TPD? What is the best method of identifying and selectively injecting the most appropriate muscles? Can additional benefit be obtained by injecting more than one muscle (e.g., injecting temporalis muscles in addition to the masseter muscles in patients with JCD, or injecting pterygoids in addition to submental muscles in patients with JOD)? Because individual muscles in the submental complex are difficult to differentiate by palpation (and even with EMG), what is the role of EMG or ultrasound (44) in locating the muscles responsible for the abnormal jaw movements and postures? What is the role of ethanol and lidocaine (muscle-afferent blockers) (45) in conjunction with BTX-A in the treatment of OMD? Why is dryness of mouth a rarely reported side effect of BTX-A treatment for OMD, even though BTX-A injection into salivary glands, adjacent to the muscles injected in patients with OMD, is increasingly used for the treatment of sialorrhea (46,47)? These and other questions need to be addressed by properly designed trials. It is clear, however, that even without the benefit of all the answers, the use of BTX-A has been accepted as the treatment of choice not only for focal dystonias, such as OMD, but also for a rapidly expanding number of disorders associated with excessive or inappropriate muscle contractions (48). REFERENCES 1. Cardoso F, Jankovic J. Oromandibular dystonia. In: Tsui J, Calne D, eds. Handbook of dystonia. New York: Marcel Dekker; 1995: Meige H. Les convulsions de la face: Une forme clinique de convulsions faciales, bilaterale et mediane. Rev Neurol (Paris) 1910;21: Wood HC. Nervous diseases and their diagnosis. Philadelphia, PA: JB Lippincott, 1887: Bressman SB, de Leon DDR, Ozelius L, et al. Clinicalgenetic spectrum of primary dystonia. Adv Neurol 1998; 78: Steinberger D, Topka H, Fischer D, et al. GCH1 mutation in a patient with adult-onset oromandibular dystonia. Neurology 1999;52: Sankhla C, Lai EC, Jankovic J. Peripherally induced oromandibular dystonia. J Neurol Neurosurg Psychiatry 1998;65: Tan EK, Jankovic J. Tardive and idiopathic oromandibular dystonia: a clinical comparison. J Neurol Neurosurg Psychiatry 2000;68: Jankovic J. Medical therapy and botulinum toxin in dystonia. Adv Neurol 1998;78: Sutcher H, Underwood R, Beatty R, et al. Orofacial dyskinesia: a dental dimension. JAMA 1971;216: Ondo WG, Desaloms JM, Jankovic J, et al. Pallidotomy for generalized dystonia. Mov Disord 1998;13: Coubes P, Roubertie A, Vayssiere N, et al. Treatment of DYT1-generalised dystonia by stimulation of the internal globus pallidus. Lancet 2000;355: Humeau Y, Doussau F, Grant NJ, et al. How botulinum and tetanus neurotoxins block neurotransmitter release. Biochimie 2000;82: Huang W, Foster JA, Rogachefsky AS. Pharmacology of botulinum toxin. J Am Acad Dermatol 2000;43: Schiavo G, Matteoli M, Montecucco C. Neurotoxins affecting neuroexocytosis. Physiol Rev 2000;80: American Academy of Neurology. Assessment: the clinical usefulness of botulinum toxin-a in treating neurologic disorders. Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 1990;40: Giladi N. The mechanism of action of botulinum toxin type A in focal dystonia is most probably through its dual effect on efferent (motor) and afferent pathways at the injected site. J Neurol Sci 1997;152: Filippi GM, Errico P, Santarelli R, et al. Botulinum A toxin effects on rat jaw muscle spindles. Acta Otolaryngol 1993;113: Gilio F, Curra A, Lorenzano C, et al. Effects of botulinum toxin type A on intracortical inhibition in patients with dystonia. Ann Neurol 2000;48: Kaji K. Facts and fancies on writer s cramp. Muscle Nerve 2000;23: Hallett M. How does botulinum toxin work? Ann Neurol 2000;48: Yoshida K, Kaji R, Kubori T, et al. Muscle afferent block for the treatment of oromandibular dystonia. Mov Disord 1998;13: Gelb DJ, Yoshimura DM, Olney RK, et al. Change in pattern of muscle activity following botulinum toxin injections for torticollis. Ann Neurol 1991;29: Van den Bergh P, Francart J, Mourin S, et al. Five-year experience in the treatment of focal movement disorders with low-dose DYSPORT botulinum toxin. Muscle Nerve 1995;18: Heise GJ, Mullen MP. Oromandibular dystonia treated with botulinum toxin: report of case. J Oral Maxillofac Surg 1995;53: Berardelli A, Formica A, Mercuri B, et al. Botulinum toxin treatment in patients with focal dystonia and hemifacial spasm. A multicenter study of the Italian Movement Disorder Group. Ital J Neurol Sci 1993;14: Hermanowicz N, Truong DD. Treatment of oromandibular dystonia with botulinum toxin. Laryngoscope 1991;101:
8 350 SCIENTIFIC AND THERAPEUTIC ASPECTS OF BOTULINUM TOXIN 27. Maurri S, Brogelli S, Alfieri G, et al. Use of botulinum toxin in Meige s disease. Riv Neurol 1988;58: Bhattacharyya N, Tarsy D. Impact on quality of life of botulinum toxin treatments for spasmodic dysphonia and oromandibular dystonia. Arch Otolaryngol Head Neck Surg 2001;127: Brin M, Blitzer A, Herman S, et al. Oromandibular dystonia: treatment of 96 cases with botulinum A. In: Jankovic J, Hallett M, eds. Therapy with botulinum toxin. New York: Marcel Dekker; 1994: Tan EK, Jankovic J. Botulinum toxin A in patients with oromandibular dystonia: long-term follow-up. Neurology 1999;53: Jankovic J. Needle EMG guidance is rarely required. Muscle Nerve 2001;24: Blitzer A, Brin MF, Fahn S. Botulinum toxin injections for lingual dystonia [Letter]. Laryngoscope 1991;101: Charles PD, Davis TL, Shannon KM, Hook MA, Warner JS. Tongue protrusion dystonia: treatment with botulinum toxin. South Med J 1997;90: Watts MW, Tan EK, Jankovic J. Bruxism and cranialcervical dystonia: is there a relationship? Cranio 1999; 17: Tan EK, Jankovic J, Ondo W. Bruxism in Huntington s disease. Mov Disord 2000;15: Tan EK, Jankovic J. Treating severe bruxism with botulinum toxin. J Am Dent Assoc 2000;131: Freund B, Schwartz M, Symington JM. Botulinum toxin: new treatment for temporomandibular disorders. Br J Oral Maxillofac Surg 2000;38: Daelen B, Thorwirth V, Koch A. Treatment of recurrent dislocation of the temporomandibular joint with type A botulinum toxin. Int J Oral Maxillofac Surg 1997;26: Jankovic J. Etiology and differential diagnosis of blepharospasm and oromandibular dystonia. In: Jankovic J, Tolosa E, eds. Facial dyskinesias. New York: Raven Press, 1988: Auger R, Litchy W, Cascino T, et al. Hemimasticatory spasm: clinical and electrophysiologic observations. Neurology 1992;42: Kim HJ, Jeon BS, Lee KW. Hemimasticatory spasm associated with localized scleroderma and facial hemiatrophy. Arch Neurol 2000;57: Ebersbach G, Kabus C, Schelosky L, et al. Hemimasticatory spasm in hemifacial atrophy: diagnostic and therapeutic aspects in two patients. Mov Disord 1995;10: Merello M, Garcia H, Nogues M, et al. Masticatory muscle spasm in a non-japanese patient with Satoyoshi syndrome successfully treated with botulinum toxin. Mov Disord 1994;9: Emshoff R, Bertram S, Strobl H. Ultrasonographic cross-sectional characteristics of muscles of the head and neck. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999;87: Mezaki T, Matsumoto S, Sakamoto T, et al. [Cervical echomyography in cervical dystonia and its application to the monitoring for muscle afferent block (MAB).] Rinsho Shinkeigaku 2000;40: Pal PK, Calne DB, Calne S, et al. Botulinum toxin A as treatment for drooling saliva in PD. Neurology 2000; 54: Porta M, Gamba M, Bertacchi G, et al. Treatment of sialorrhoea with ultrasound guided botulinum toxin type A injection in patients with neurological disorders. J Neurol Neurosurg Psychiatry 2001;70: Thomas M, Jankovic J. Botulinum toxin treatment of tics, myoclonus, stiff-person syndrome, gait freezing and rigidity. In: Moore P, Naumann M, eds. Handbook of botulinum toxin treatment, 2nd ed. London: Blackwell Science, 2002 (in press).
BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required]
![BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required] BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required]](/thumbs/29/13417512.jpg) BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required] Medical Policy: MP-RX-01-11 Original Effective Date: March 24, 2011 Reviewed: Revised: This policy applies to products
BOTOX Injection (Onabotulinumtoxin A) for Migraine Headaches [Preauthorization Required] Medical Policy: MP-RX-01-11 Original Effective Date: March 24, 2011 Reviewed: Revised: This policy applies to products
Webinar title: Know Your Options for Treating Severe Spasticity
 Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
Webinar title: Know Your Options for Treating Severe Spasticity Presented by: Dr. Gerald Bilsky, Physiatrist Medical Director of Outpatient Services and Associate Medical Director of Acquired Brain Injury
Parkinson's s disease - a
 Parkinson's Disease Parkinson's s disease - a progressive disorder of the nervous system that affects movement. The most common perception of Parkinson s is the patient having tremors. Hands shaking, inability
Parkinson's Disease Parkinson's s disease - a progressive disorder of the nervous system that affects movement. The most common perception of Parkinson s is the patient having tremors. Hands shaking, inability
Guidelines for Insurance Approval and the Appeal Process in the Treatment of Spasmodic Dysphonia with Botulinum Toxin Injections
 NATIONAL SPASMODIC DYSPHONIA ASSOCIATION Guidelines for Insurance Approval and the Appeal Process in the Treatment of Spasmodic Dysphonia with Botulinum Toxin Injections Published by National Spasmodic
NATIONAL SPASMODIC DYSPHONIA ASSOCIATION Guidelines for Insurance Approval and the Appeal Process in the Treatment of Spasmodic Dysphonia with Botulinum Toxin Injections Published by National Spasmodic
PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
 PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS De Anna Looper, RN CHPN Corporate Clinical Consultant / Legal Nurse Consultant Carrefour Associates L.L.C. PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS De Anna Looper, RN CHPN Corporate Clinical Consultant / Legal Nurse Consultant Carrefour Associates L.L.C. PARKINSON S DISEASE IN LONG-TERM-CARE SETTINGS
Four Oral Motor Disorders: Bruxism, Dystonia, Dyskinesia and Drug-Induced Dystonic Extrapyramidal Reactions
 Dent Clin N Am 51 (2007) 225 243 Four Oral Motor Disorders: Bruxism, Dystonia, Dyskinesia and Drug-Induced Dystonic Extrapyramidal Reactions Glenn T. Clark, DDS, MS*, Saravanan Ram, BDS, MDS Department
Dent Clin N Am 51 (2007) 225 243 Four Oral Motor Disorders: Bruxism, Dystonia, Dyskinesia and Drug-Induced Dystonic Extrapyramidal Reactions Glenn T. Clark, DDS, MS*, Saravanan Ram, BDS, MDS Department
ABC s of Parkinson s Disease 4/29/15 Karen Parenti, MS, PsyD
 ABC s of Parkinson s Disease 4/29/15 Karen Parenti, MS, PsyD What is Parkinson s Disease? Parkinson's disease is a progressive disorder of the nervous system that affects movement. It develops gradually,
ABC s of Parkinson s Disease 4/29/15 Karen Parenti, MS, PsyD What is Parkinson s Disease? Parkinson's disease is a progressive disorder of the nervous system that affects movement. It develops gradually,
Europass Curriculum Vitae
 Europass Curriculum Vitae Personal information First name(s) / Surname(s) Address(es) Alfredo Berardelli Department of Neurology and Psychiatry Viale dell Università, 30 00185 Rome - Italy Telephone(s)
Europass Curriculum Vitae Personal information First name(s) / Surname(s) Address(es) Alfredo Berardelli Department of Neurology and Psychiatry Viale dell Università, 30 00185 Rome - Italy Telephone(s)
BOTOX Treatment. for Chronic Migraine. Information for patients and their families. Botulinum Toxin Type A
 BOTOX Treatment Botulinum Toxin Type A for Chronic Migraine Information for patients and their families. Is Chronic Migraine the same as Migraine? Chronic Migraine is similar to migraine as sufferers experience
BOTOX Treatment Botulinum Toxin Type A for Chronic Migraine Information for patients and their families. Is Chronic Migraine the same as Migraine? Chronic Migraine is similar to migraine as sufferers experience
Dystonia Neurology Services in the UK. Val Wells Service Development Manager The Dystonia Society
 Dystonia Neurology Services in the UK Val Wells Service Development Manager The Dystonia Society 1 Dystonia? Dystonia is a movement disorder characterised by, patterned, directional and sustained muscle
Dystonia Neurology Services in the UK Val Wells Service Development Manager The Dystonia Society 1 Dystonia? Dystonia is a movement disorder characterised by, patterned, directional and sustained muscle
Anthem Central Region Clinical Claims Edit
 Please compare the claim's date of adjudication to the range of the edit in question. Prior versions, if any, can be found below. Subject: Chemodenervation of Muscles of Different Areas with Chemodenervation
Please compare the claim's date of adjudication to the range of the edit in question. Prior versions, if any, can be found below. Subject: Chemodenervation of Muscles of Different Areas with Chemodenervation
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Intrathecal Baclofen for CNS Spasticity Last Review Date: November 13, 2015 Number: MG.MM.ME.31bC5 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Tone Management in Cerebral Palsy. Jenny Wilson, MD wilsjen@ohsu.edu OHSU and Shriners Hospital for Children October, 2015
 Tone Management in Cerebral Palsy Jenny Wilson, MD wilsjen@ohsu.edu OHSU and Shriners Hospital for Children October, 2015 Disclosures I am involved in a Dysport sponsored research study Goals Describe
Tone Management in Cerebral Palsy Jenny Wilson, MD wilsjen@ohsu.edu OHSU and Shriners Hospital for Children October, 2015 Disclosures I am involved in a Dysport sponsored research study Goals Describe
Understanding Parkinson s Disease
 Understanding Parkinson s Disease Irene Oh, MD Neurologist, Movement Disorders Specialist The Neurology Center of Southern California, Encinitas & Escondido Introduction PD was first described in 1817
Understanding Parkinson s Disease Irene Oh, MD Neurologist, Movement Disorders Specialist The Neurology Center of Southern California, Encinitas & Escondido Introduction PD was first described in 1817
In recent years some doctors have treated spasticity in children with Botox, the musclerelaxing agent used cosmetically for wrinkles.
 The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.christopherreeve.org/site/c.mtkzkgmwkwg/b.4453419/k.3757/spasticity.h tm
The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. http://www.christopherreeve.org/site/c.mtkzkgmwkwg/b.4453419/k.3757/spasticity.h tm
PARKINSON S DISEASE INTRODUCTION. Parkinson s disease is defined as a disease of the nervous system that affects voluntary movement.
 PARKINSON S DISEASE INTRODUCTION Parkinson s disease is a disorder of the brain and the nervous system. It is one of the more common neurological diseases in people over the age of 60, and it is more common
PARKINSON S DISEASE INTRODUCTION Parkinson s disease is a disorder of the brain and the nervous system. It is one of the more common neurological diseases in people over the age of 60, and it is more common
People with Parkinson s often experience pain caused by muscle
 Symptoms and lifestyle Muscle cramps and dystonia People with Parkinson s often experience pain caused by muscle cramps and/or dystonia. This information sheet looks at what muscle cramps and dystonia
Symptoms and lifestyle Muscle cramps and dystonia People with Parkinson s often experience pain caused by muscle cramps and/or dystonia. This information sheet looks at what muscle cramps and dystonia
EMG and the Electrodiagnostic Consultation for the Family Physician
 EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
EMG and the Electrodiagnostic Consultation for the Family Physician Stephanie Kopey, D.O., P.T. 9/27/15 The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) Marketing Committee
Nursing Care of Patients with Movement Disorders. Catholic Health 2 nd Annual Neurorehab Symposium November 1, 2014
 Nursing Care of Patients with Movement Disorders Catholic Health 2 nd Annual Neurorehab Symposium November 1, 2014 Types of Movement Disorders Parkinson s disease Huntington s disease Dystonia Tremors
Nursing Care of Patients with Movement Disorders Catholic Health 2 nd Annual Neurorehab Symposium November 1, 2014 Types of Movement Disorders Parkinson s disease Huntington s disease Dystonia Tremors
GLOSSARY OF TERMS. This glossary explains the terms and words often used in association with Parkinson s.
 Antagonist This glossary explains the terms and words often used in association with Parkinson s. Medications which have a negative effect on particular cells in the body. In Parkinson s dopamine antagonists
Antagonist This glossary explains the terms and words often used in association with Parkinson s. Medications which have a negative effect on particular cells in the body. In Parkinson s dopamine antagonists
Cerebral palsy can be classified according to the type of abnormal muscle tone or movement, and the distribution of these motor impairments.
 The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
Billing and Coding Guidelines
 Billing and Coding Guidelines Contractor Name Wisconsin Physicians Service Insurance Corporation Title INJ- 018 Botulinum Toxin Type A & Type B Revision Effective Date 10/01/2011 AMA CPT/ ADA CDT Copyright
Billing and Coding Guidelines Contractor Name Wisconsin Physicians Service Insurance Corporation Title INJ- 018 Botulinum Toxin Type A & Type B Revision Effective Date 10/01/2011 AMA CPT/ ADA CDT Copyright
ORTHODONTIC TREATMENT
 ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
ORTHODONTIC TREATMENT Informed Consent for the Orthodontic Patient As a general rule, positive orthodontic results can be achieved by informed and cooperative patients. Thus, the following information
What is PD? Dr Catherine Dotchin MD MRCP Consultant Geriatrician
 What is PD? Dr Catherine Dotchin MD MRCP Consultant Geriatrician Overview of presentation Case history Video example pre and post treatment Historical review PD in the UK Epidemiology and aetiology Making
What is PD? Dr Catherine Dotchin MD MRCP Consultant Geriatrician Overview of presentation Case history Video example pre and post treatment Historical review PD in the UK Epidemiology and aetiology Making
1: Motor neurone disease (MND)
 1: Motor neurone disease (MND) This section provides basic facts about motor neurone disease (MND) and its diagnosis. The following information is an extracted section from our full guide Living with motor
1: Motor neurone disease (MND) This section provides basic facts about motor neurone disease (MND) and its diagnosis. The following information is an extracted section from our full guide Living with motor
CONSUMER MEDICINE INFORMATION
 CONSUMER MEDICINE INFORMATION BOTOX (botulinum toxin, type A) purified neurotoxin complex The information in this leaflet is ONLY a summary and is not a complete statement about BOTOX injection. Your doctor
CONSUMER MEDICINE INFORMATION BOTOX (botulinum toxin, type A) purified neurotoxin complex The information in this leaflet is ONLY a summary and is not a complete statement about BOTOX injection. Your doctor
Background. Physiotherapy Management
 Mr. Alex Wong, Senior physiotherapist, QEH Mr. Barry Ma, Physiotherapist, QEH Background Trigeminal neuralgia is a neuropathic pain syndrome that affects the trigeminal or 5 th cranial nerve, one of the
Mr. Alex Wong, Senior physiotherapist, QEH Mr. Barry Ma, Physiotherapist, QEH Background Trigeminal neuralgia is a neuropathic pain syndrome that affects the trigeminal or 5 th cranial nerve, one of the
1st Edition 2015. Quick reference guide for the management of acute whiplash. associated disorders
 1 1st Edition 2015 Quick reference guide for the management of acute whiplash associated disorders 2 Quick reference guide for the management of acute whiplash associated disorders, 2015. This quick reference
1 1st Edition 2015 Quick reference guide for the management of acute whiplash associated disorders 2 Quick reference guide for the management of acute whiplash associated disorders, 2015. This quick reference
National Hospital for Neurology and Neurosurgery. Managing Spasticity. Spasticity Service
 National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
PARKINSON S DISEASE AND PARKINSONISM. Dr Phil Wood Geriatrician, Waitemata DHB Clinical Unit Leader, Waikato DHB
 PARKINSON S DISEASE AND PARKINSONISM Dr Phil Wood Geriatrician, Waitemata DHB Clinical Unit Leader, Waikato DHB OUTLINE Covering:- Why this is an important area of Medical and Psychiatric care The variety
PARKINSON S DISEASE AND PARKINSONISM Dr Phil Wood Geriatrician, Waitemata DHB Clinical Unit Leader, Waikato DHB OUTLINE Covering:- Why this is an important area of Medical and Psychiatric care The variety
Michelle H. Cameron, M.D., P.T., M.C.R. Portland VA MS Center of Excellence- West, and Oregon Health & Science University
 Michelle H. Cameron, M.D., P.T., M.C.R. Portland VA MS Center of Excellence- West, and Oregon Health & Science University Ileana Howard, M.D. VA Puget Sound, Seattle, WA and University of Washington PVA
Michelle H. Cameron, M.D., P.T., M.C.R. Portland VA MS Center of Excellence- West, and Oregon Health & Science University Ileana Howard, M.D. VA Puget Sound, Seattle, WA and University of Washington PVA
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Long-Term Outcome of Trigeminal Nerve Injuries Related to Dental Treatment
 DENTOALVEOLAR SURGERY J Oral Maxillofac Surg 69:2284-2288, 2011 Long-Term Outcome of Trigeminal Nerve Injuries Related to Dental Treatment M. Anthony Pogrel, DDS, MD, FACS, FRCS,* Ryan Jergensen, DDS,
DENTOALVEOLAR SURGERY J Oral Maxillofac Surg 69:2284-2288, 2011 Long-Term Outcome of Trigeminal Nerve Injuries Related to Dental Treatment M. Anthony Pogrel, DDS, MD, FACS, FRCS,* Ryan Jergensen, DDS,
a guide to understanding facial palsy a publication of children s craniofacial association
 a guide to understanding facial palsy a publication of children s craniofacial association a guide to understanding facial palsy this parent s guide to facial palsy is designed to answer questions that
a guide to understanding facial palsy a publication of children s craniofacial association a guide to understanding facial palsy this parent s guide to facial palsy is designed to answer questions that
Chapter 28. Drug Treatment of Parkinson s Disease
 Chapter 28 Drug Treatment of Parkinson s Disease 1. Introduction Parkinsonism Tremors hands and head develop involuntary movements when at rest; pin rolling sign (finger and thumb) Muscle rigidity arthritis
Chapter 28 Drug Treatment of Parkinson s Disease 1. Introduction Parkinsonism Tremors hands and head develop involuntary movements when at rest; pin rolling sign (finger and thumb) Muscle rigidity arthritis
Motor dysfunction 2: Spinal cord injury and subcortical motor disorders ANATOMY REVIEW: Basal Ganglia
 Motor dysfunction 2: Spinal cord injury and subcortical motor disorders ANATOMY REVIEW: Basal Ganglia A group of subcortical nuclei caudate, putamen, globus pallidus Caudate & Putamen = Neostriatum caudate
Motor dysfunction 2: Spinal cord injury and subcortical motor disorders ANATOMY REVIEW: Basal Ganglia A group of subcortical nuclei caudate, putamen, globus pallidus Caudate & Putamen = Neostriatum caudate
Guidelines for Medical Necessity Determination for Speech and Language Therapy
 Guidelines for Medical Necessity Determination for Speech and Language Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Speech and Language Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guideline for the Management of Acute Peripheral Facial nerve palsy. Bells Palsy in Children
 Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Guideline for the Management of Acute Peripheral Facial nerve palsy Definition Bells Palsy in Children Bell palsy is an acute, idiopathic unilateral lower motor neurone facial nerve palsy that is not associated
Oculopharyngeal muscular dystrophy (OPMD)
 Oculopharyngeal muscular dystrophy (OPMD) The term muscular dystrophy is used to cover a wide range of conditions which have in common progressive muscle weakness due to an inherited genetic defect (mutation).
Oculopharyngeal muscular dystrophy (OPMD) The term muscular dystrophy is used to cover a wide range of conditions which have in common progressive muscle weakness due to an inherited genetic defect (mutation).
STROKE CARE NOW NETWORK CONFERENCE MAY 22, 2014
 STROKE CARE NOW NETWORK CONFERENCE MAY 22, 2014 Rehabilitation Innovations in Post- Stroke Recovery Madhav Bhat, MD Fort Wayne Neurological Center DISCLOSURE Paid speaker for TEVA Neuroscience Program.
STROKE CARE NOW NETWORK CONFERENCE MAY 22, 2014 Rehabilitation Innovations in Post- Stroke Recovery Madhav Bhat, MD Fort Wayne Neurological Center DISCLOSURE Paid speaker for TEVA Neuroscience Program.
MD pathophysiology. Phenomenology of movement disorders and gait disturbances. Phenomenology in MD. Hyperkinetic movements.
 MD pathophysiology Phenomenology of movement disorders and gait disturbances Genetic mutation or environmental injury of basal ganglia functioning Pallidum, thalamus, subthalamic nucleus, caudate nucleus,
MD pathophysiology Phenomenology of movement disorders and gait disturbances Genetic mutation or environmental injury of basal ganglia functioning Pallidum, thalamus, subthalamic nucleus, caudate nucleus,
Movement disorders and gait disturbances. Kovács Norbert PTE ÁOK Neurológiai Klinika Pécs
 Movement disorders and gait disturbances Kovács Norbert PTE ÁOK Neurológiai Klinika Pécs 1 MD pathophysiology Genetic mutation or environmental injury of basal ganglia functioning Pallidum, thalamus, subthalamic
Movement disorders and gait disturbances Kovács Norbert PTE ÁOK Neurológiai Klinika Pécs 1 MD pathophysiology Genetic mutation or environmental injury of basal ganglia functioning Pallidum, thalamus, subthalamic
Multifocal Motor Neuropathy. Jonathan Katz, MD Richard Lewis, MD
 Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Multifocal Motor Neuropathy Jonathan Katz, MD Richard Lewis, MD What is Multifocal Motor Neuropathy? Multifocal Motor Neuropathy (MMN) is a rare condition in which multiple motor nerves are attacked by
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies
 Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Cervicogenic Headache: A Review of Diagnostic and Treatment Strategies 1 Journal of the American Osteopathic Association April 2005, Vol. 105, No. 4 supplement, pp. 16-22 David M. Biondi, DO FROM ABSTRACT:
Botulinum toxin A for the treatment of chronic neck pain
 Pain 94 (2001) 255 260 www.elsevier.com/locate/pain Botulinum toxin A for the treatment of chronic neck pain Anthony H. Wheeler a, *, Paula Goolkasian b, Stephanie S. Gretz c a Charlotte Spine Center,
Pain 94 (2001) 255 260 www.elsevier.com/locate/pain Botulinum toxin A for the treatment of chronic neck pain Anthony H. Wheeler a, *, Paula Goolkasian b, Stephanie S. Gretz c a Charlotte Spine Center,
Cerebral Palsy: Intervention Methods for Young Children. Emma Zercher. San Francisco State University
 RUNNING HEAD: Cerebral Palsy & Intervention Methods Cerebral Palsy & Intervention Methods, 1 Cerebral Palsy: Intervention Methods for Young Children Emma Zercher San Francisco State University May 21,
RUNNING HEAD: Cerebral Palsy & Intervention Methods Cerebral Palsy & Intervention Methods, 1 Cerebral Palsy: Intervention Methods for Young Children Emma Zercher San Francisco State University May 21,
a guide to understanding moebius syndrome a publication of children s craniofacial association
 a guide to understanding moebius syndrome a publication of children s craniofacial association a guide to understanding moebius syndrome this parent s guide to Moebius syndrome is designed to answer questions
a guide to understanding moebius syndrome a publication of children s craniofacial association a guide to understanding moebius syndrome this parent s guide to Moebius syndrome is designed to answer questions
Parkinson Disease Levodopa-Induced Dyskinesia. Christopher Kenney, MD Novartis Pharmaceuticals
 Parkinson Disease Levodopa-Induced Dyskinesia Christopher Kenney, MD Novartis Pharmaceuticals Disclosures Dr. Kenney is a full-time employee of Novartis Pharmaceuticals Corporation The opinions expressed
Parkinson Disease Levodopa-Induced Dyskinesia Christopher Kenney, MD Novartis Pharmaceuticals Disclosures Dr. Kenney is a full-time employee of Novartis Pharmaceuticals Corporation The opinions expressed
Cerebral Palsy Information
 Cerebral Palsy Information The following information was extracted from the Mayo Clinic s website Definition: "Cerebral palsy" is a general term for a group of disorders that appear during the first few
Cerebral Palsy Information The following information was extracted from the Mayo Clinic s website Definition: "Cerebral palsy" is a general term for a group of disorders that appear during the first few
F r e q u e n t l y A s k e d Q u e s t i o n s
 Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Myasthenia Gravis Q: What is myasthenia gravis (MG)? A: Myasthenia gravis (meye-uhss- THEEN-ee-uh GRAV uhss) (MG) is an autoimmune disease that weakens the muscles. The name comes from Greek and Latin
Module 1: The Somato-Motor System: Tendon Tap reflex
 Module 1: The Somato-Motor System: Tendon Tap reflex Module Objectives: 1. Describe the anatomic pathway of a tendon tap reflex. 2. Explain how a tendon tap reflex assessment assists in diagnosis of a
Module 1: The Somato-Motor System: Tendon Tap reflex Module Objectives: 1. Describe the anatomic pathway of a tendon tap reflex. 2. Explain how a tendon tap reflex assessment assists in diagnosis of a
Role of Electrodiagnostic Tests in Neuromuscular Disease
 Role of Electrodiagnostic Tests in Neuromuscular Disease Electrodiagnostic tests Electroencephalogram (EEG) Electromyography (NCV, EMG) Cerebral evoked potentials (CEP) Motor evoked potentials (MEP) Electronystagmogram
Role of Electrodiagnostic Tests in Neuromuscular Disease Electrodiagnostic tests Electroencephalogram (EEG) Electromyography (NCV, EMG) Cerebral evoked potentials (CEP) Motor evoked potentials (MEP) Electronystagmogram
TMJ. Problems. Certain headaches and pain in. the ear, jaw, neck, tooth, and. sinus can be the result of a. temporomandibular joint (TMJ)
 DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
DIVISION OF ORAL AND MAXILLOFACIAL SURGERY TMJ Problems Certain headaches and pain in the ear, jaw, neck, tooth, and sinus can be the result of a temporomandibular joint (TMJ) problem. People with TMJ
Cerebral Palsy. In order to function, the brain needs a continuous supply of oxygen.
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Up to 5000 children in the United States are diagnosed with cerebral palsy every year. This reference
The use of botulinum toxin is considered medically necessary for the FDA-labeled indications of:
 COVERAGE: The use of botulinum toxin is considered medically necessary for the FDA-labeled indications of: Strabismus, Blepharospasm, Facial nerve (VII) disorders, or Cervical dystonia. The use of botulinum
COVERAGE: The use of botulinum toxin is considered medically necessary for the FDA-labeled indications of: Strabismus, Blepharospasm, Facial nerve (VII) disorders, or Cervical dystonia. The use of botulinum
ALL ABOUT SPASTICITY. www.almirall.com. Solutions with you in mind
 ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
Cerebral Palsy. 1995-2014, The Patient Education Institute, Inc. www.x-plain.com nr200105 Last reviewed: 06/17/2014 1
 Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Cerebral Palsy Introduction Cerebral palsy, or CP, can cause serious neurological symptoms in children. Thousands of children are diagnosed with cerebral palsy every year. This reference summary explains
Oh, 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8
 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
Advances in MOvEMEnt DIsOrDErs:
 Advances in MOvEMEnt DIsOrDErs: The NYC Movement Disorder CME Symposium sunday, April 7, 2013 Icahn School of Medicine at Mount Sinai the goldwurm AuDItOrIuM New York, NY Course Director Course Co-Director
Advances in MOvEMEnt DIsOrDErs: The NYC Movement Disorder CME Symposium sunday, April 7, 2013 Icahn School of Medicine at Mount Sinai the goldwurm AuDItOrIuM New York, NY Course Director Course Co-Director
Parkinson s Disease (PD)
 Parkinson s Disease (PD) Parkinson s disease (PD) is a movement disorder that worsens over time. About 1 in 100 people older than 60 has Parkinson s. The exact cause of PD is still not known, but research
Parkinson s Disease (PD) Parkinson s disease (PD) is a movement disorder that worsens over time. About 1 in 100 people older than 60 has Parkinson s. The exact cause of PD is still not known, but research
THE TMJ TREATMENT CENTER
 THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
THE TMJ TREATMENT CENTER TEMPOROMANDIBULAR JOINT DISORDERS, CRANIOFACIAL DISORDERS, CERVICOCRANIAL INSTABILITY & EHLERS-DANLOS SYNDROME ABOUT DR. MITAKIDES & THE TMJ TREATMENT CENTER Dedicated to the diagnosis
Clinical Psychopharmacology
 Clinical Psychopharmacology Antiparkinsonian drugs Department of Pharmacy, GGZ WNB Chair on Pharmacotherapy in Psychiatric Patients/Anton Loonen May 2015 2 Basal ganglia diseases Parkinson s disease and
Clinical Psychopharmacology Antiparkinsonian drugs Department of Pharmacy, GGZ WNB Chair on Pharmacotherapy in Psychiatric Patients/Anton Loonen May 2015 2 Basal ganglia diseases Parkinson s disease and
Drugs for MS.Drug fact box cannabis extract (Sativex) Version 1.0 Author
 Version History Policy Title Drugs for MS.Drug fact box cannabis extract (Sativex) Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further
Version History Policy Title Drugs for MS.Drug fact box cannabis extract (Sativex) Version 1.0 Author West Midlands Commissioning Support Unit Publication Date Jan 2013 Review Date Supersedes/New (Further
Parkinson's disease. Definition. Symptoms
 Parkinson's disease Definition Parkinson's disease is a progressive disorder of the nervous system that affects your movement. It develops gradually, sometimes starting with a barely noticeable tremor
Parkinson's disease Definition Parkinson's disease is a progressive disorder of the nervous system that affects your movement. It develops gradually, sometimes starting with a barely noticeable tremor
Medical Treatment Guidelines Washington State Department of Labor and Industries
 Complex regional pain syndrome (CRPS) Formerly known as reflex sympathetic dystrophy 1. Introduction This bulletin outlines the Department of Labor and Industries guidelines for diagnosing and treating
Complex regional pain syndrome (CRPS) Formerly known as reflex sympathetic dystrophy 1. Introduction This bulletin outlines the Department of Labor and Industries guidelines for diagnosing and treating
Multiple System Atrophy
 Multiple System Atrophy U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Multiple System Atrophy What is multiple system atrophy? Multiple system atrophy
Multiple System Atrophy U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES Public Health Service National Institutes of Health Multiple System Atrophy What is multiple system atrophy? Multiple system atrophy
Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas
 Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Billing and Coding in Neurology and Headache Stuart B Black MD, FAAN Chief of Neurology Co-Medical Director: Neuroscience Center Baylor University Medical Center at Dallas CPT Codes vs. ICD Codes Category
Botulinum Toxins (BOTOX, DYSPORT, MYOBLOC and XEOMIN)
 Botulinum Toxins (BOTOX, DYSPORT, MYOBLOC and XEOMIN) Policy Number: Original Effective Date: MM.04.004 03/14/2006 Line(s) of Business: Current Effective Date: HMO; PPO 10/01/2012 Section: Prescription
Botulinum Toxins (BOTOX, DYSPORT, MYOBLOC and XEOMIN) Policy Number: Original Effective Date: MM.04.004 03/14/2006 Line(s) of Business: Current Effective Date: HMO; PPO 10/01/2012 Section: Prescription
Botulinum Toxins in Dentistry The New Paradigm for Masticatory Muscle Hypertonicity
 REVIEW ARTICLE Botulinum Toxins in Dentistry The New Paradigm for Masticatory Muscle Hypertonicity Howard Katz Dentofacial Treatment Center of San Diego (Private Practice), San Diego, California, U.S.A.
REVIEW ARTICLE Botulinum Toxins in Dentistry The New Paradigm for Masticatory Muscle Hypertonicity Howard Katz Dentofacial Treatment Center of San Diego (Private Practice), San Diego, California, U.S.A.
Lateral pterygoid muscle Medial pterygoid muscle
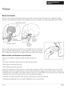 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Risk Factors for Blepharospasm
 Risk Factors for Blepharospasm Mark A. Stacy M.D. and Padma R. Mahant, M.D. The Barrow Neurological Institute Phoenix, AZ BACKGROUND Blepharospasm is a focal dystonia characterized by repetitive, sustained
Risk Factors for Blepharospasm Mark A. Stacy M.D. and Padma R. Mahant, M.D. The Barrow Neurological Institute Phoenix, AZ BACKGROUND Blepharospasm is a focal dystonia characterized by repetitive, sustained
Management in the pre-hospital setting
 Management in the pre-hospital setting Inflammation of the joints Two main types: Osteoarthritis - cartilage loss from wear and tear Rheumatoid arthritis - autoimmune disorder Affects all age groups,
Management in the pre-hospital setting Inflammation of the joints Two main types: Osteoarthritis - cartilage loss from wear and tear Rheumatoid arthritis - autoimmune disorder Affects all age groups,
Aetna Nerve Conduction Study Policy
 Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
Aetna Nerve Conduction Study Policy Policy Aetna considers nerve conduction velocity (NCV) studies medically necessary when both of the following criteria are met: 1. Member has any of the following indications:
How To Treat Sud
 May 8, 2010, Denver, Colorado Compiled by Pat Hill, NSDA Area Contact Persons Coordinator, and Mary Bifaro, NSDA Support Services Director The notes were taken informally to serve as a summary this NSDA
May 8, 2010, Denver, Colorado Compiled by Pat Hill, NSDA Area Contact Persons Coordinator, and Mary Bifaro, NSDA Support Services Director The notes were taken informally to serve as a summary this NSDA
NeuroStar TMS Therapy Patient Guide for Treating Depression
 NeuroStar TMS Therapy Patient Guide for Treating Depression This NeuroStar TMS Therapy Patient Guide for Treating Depression provides important safety and use information for you to consider about treating
NeuroStar TMS Therapy Patient Guide for Treating Depression This NeuroStar TMS Therapy Patient Guide for Treating Depression provides important safety and use information for you to consider about treating
3nd Biennial Contemporary Clinical Neurophysiological Symposium October 12, 2013 Fundamentals of NCS and NMJ Testing
 3nd Biennial Contemporary Clinical Neurophysiological Symposium October 12, 2013 Fundamentals of NCS and NMJ Testing Peter D. Donofrio, M.D. Professor of Neurology Vanderbilt University Medical Center
3nd Biennial Contemporary Clinical Neurophysiological Symposium October 12, 2013 Fundamentals of NCS and NMJ Testing Peter D. Donofrio, M.D. Professor of Neurology Vanderbilt University Medical Center
Drug-induced movement
 FEATURE Recognizing and managing drug-induced movement disorders Reprint from DUE Quarterly, July 2003 RICHARD CAMICIOLI, MD, Department of Medicine, University of Alberta, Edmonton, AB NOREEN VANDERBURGH,
FEATURE Recognizing and managing drug-induced movement disorders Reprint from DUE Quarterly, July 2003 RICHARD CAMICIOLI, MD, Department of Medicine, University of Alberta, Edmonton, AB NOREEN VANDERBURGH,
OHTAC Recommendation
 OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
OHTAC Recommendation Multiple Sclerosis and Chronic Cerebrospinal Venous Insufficiency Presented to the Ontario Health Technology Advisory Committee in May 2010 May 2010 Issue Background A review on the
UNIVERSITY OF FLORIDA
 UNIVERSITY OF FLORIDA center for movement disorders and neurorestoration A world leader in movement disorders and neurorestoration The University of Florida Center for Movement Disorders Tyler s Hope Center
UNIVERSITY OF FLORIDA center for movement disorders and neurorestoration A world leader in movement disorders and neurorestoration The University of Florida Center for Movement Disorders Tyler s Hope Center
Management of Parkinson s Disease in Primary Care
 Management of Parkinson s Disease in Primary Care Dr June Tan National University Hospital System (NUHS) Division of Neurology Senior Consultant Topics: Diagnosing PD Choice of medication in the de novo
Management of Parkinson s Disease in Primary Care Dr June Tan National University Hospital System (NUHS) Division of Neurology Senior Consultant Topics: Diagnosing PD Choice of medication in the de novo
ACUPUNCTURE AND FACIAL PAIN
 ACUPUNCTURE AND FACIAL PAIN About facial pain Facial pain commonly results from temporomandibular joint (TMJ) disorder. Many practitioners refer to TMJ disorder, or syndrome, as a single disorder but there
ACUPUNCTURE AND FACIAL PAIN About facial pain Facial pain commonly results from temporomandibular joint (TMJ) disorder. Many practitioners refer to TMJ disorder, or syndrome, as a single disorder but there
HEADACHES AND THE THIRD OCCIPITAL NERVE
 HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
HEADACHES AND THE THIRD OCCIPITAL NERVE Edward Babigumira M.D. FAAPMR. Interventional Pain Management, Lincoln. B. Pain Clinic, Ltd. Diplomate ABPMR. Board Certified Pain Medicine No disclosures Disclosure
Physical Medicine and Rehabilitation
 Physician Referral Center: (801) 581-2897 Toll-Free: (866) 850-8863 physicians.utah.edu Physical Medicine and The mission of the Division of Physical Medicine and is to provide compassionate, state-of-theart
Physician Referral Center: (801) 581-2897 Toll-Free: (866) 850-8863 physicians.utah.edu Physical Medicine and The mission of the Division of Physical Medicine and is to provide compassionate, state-of-theart
MOTION AND E-MOTION. Andrea Cavanna MD PhD FRCP
 MOTION AND E-MOTION Andrea Cavanna MD PhD FRCP Consultant in Behavioural Neurology, BSMHFT, Birmingham, UK Hon Professor in Neuropsychiatry, Aston University, Birmingham, UK Hon Reader in Neuropsychiatry,
MOTION AND E-MOTION Andrea Cavanna MD PhD FRCP Consultant in Behavioural Neurology, BSMHFT, Birmingham, UK Hon Professor in Neuropsychiatry, Aston University, Birmingham, UK Hon Reader in Neuropsychiatry,
A Definition of Multiple Sclerosis
 English 182 READING PRACTICE by Alyx Meltzer, Spring 2009 Vocabulary Preview (see bolded, underlined words) gait: (n) a particular way of walking transient: (adj) temporary; synonym = transitory remission:
English 182 READING PRACTICE by Alyx Meltzer, Spring 2009 Vocabulary Preview (see bolded, underlined words) gait: (n) a particular way of walking transient: (adj) temporary; synonym = transitory remission:
Treatment of Tension-Type Headache with Botox:
 Treatment of Tension-Type Headache with Botox: A Review of the Literature DIMA ROZEN, M.D. 1, AND JOYTI SHARMA, M.D. 2 Abstract Botulinum toxin has been shown to effectively treat several types of neurological
Treatment of Tension-Type Headache with Botox: A Review of the Literature DIMA ROZEN, M.D. 1, AND JOYTI SHARMA, M.D. 2 Abstract Botulinum toxin has been shown to effectively treat several types of neurological
*A discrete, hypersensitive nodule within tight band of muscle or fascia that present with classic pattern of pain referral that does not follow
 A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
Careful Coding: Headaches
 Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
Dynamic Chiropractic March 26, 2012, Vol. 30, Issue 07 Careful Coding: Headaches By K. Jeffrey Miller, DC, DABCO and Ray Tuck, DC Because s are among the most common reasons for seeking chiropractic care,
Clinical and Therapeutic Cannabis Information. Written by Cannabis Training University (CTU) All rights reserved
 Clinical and Therapeutic Cannabis Information Written by Cannabis Training University (CTU) All rights reserved Contents Introduction... 3 Chronic Pain... 6 Neuropathic Pain... 8 Movement Disorders...
Clinical and Therapeutic Cannabis Information Written by Cannabis Training University (CTU) All rights reserved Contents Introduction... 3 Chronic Pain... 6 Neuropathic Pain... 8 Movement Disorders...
Online Course Descriptions (degree seeking):
 Online Course Descriptions (degree seeking): BSC 6001 Foundations of Clinical Orthopaedics This is an online self study course discussing the foundations of orthopaedics and manipulative therapy. The history
Online Course Descriptions (degree seeking): BSC 6001 Foundations of Clinical Orthopaedics This is an online self study course discussing the foundations of orthopaedics and manipulative therapy. The history
Handicap after acute whiplash injury A 1-year prospective study of risk factors
 1 Handicap after acute whiplash injury A 1-year prospective study of risk factors Neurology 2001;56:1637-1643 (June 26, 2001) Helge Kasch, MD, PhD; Flemming W Bach, MD, PhD; Troels S Jensen, MD, PhD From
1 Handicap after acute whiplash injury A 1-year prospective study of risk factors Neurology 2001;56:1637-1643 (June 26, 2001) Helge Kasch, MD, PhD; Flemming W Bach, MD, PhD; Troels S Jensen, MD, PhD From
The Road to Rehabilitation
 The Road to Rehabilitation Part 7 Traveling Toward Relief: Dealing with Spasticity & Brain Injury Written by Cindy Ivanhoe, MD Elie Elovic, MD Content reveiwed by Gregory O Shanick, MD Brain Injury Association
The Road to Rehabilitation Part 7 Traveling Toward Relief: Dealing with Spasticity & Brain Injury Written by Cindy Ivanhoe, MD Elie Elovic, MD Content reveiwed by Gregory O Shanick, MD Brain Injury Association
Neurophysiological assessment of movement disorders. By Dr Carla Cordivari
 Neurophysiological assessment of movement disorders By Dr Carla Cordivari NEUROPHYSIOLOGICAL ASSESSMENT OF MOVEMENT DISORDERS Neurophysiological investigations in movement disorders are objective methods
Neurophysiological assessment of movement disorders By Dr Carla Cordivari NEUROPHYSIOLOGICAL ASSESSMENT OF MOVEMENT DISORDERS Neurophysiological investigations in movement disorders are objective methods
12/15/2008. Image from: http://www.emedicine.com/neuro/topic533.htm
 A non-progressive disorder Caused by brain injury pre (70-80%), peri, or post natally Injure occurs before CNS reaches maturity Patients often have great potential masked by their condition Image from:
A non-progressive disorder Caused by brain injury pre (70-80%), peri, or post natally Injure occurs before CNS reaches maturity Patients often have great potential masked by their condition Image from:
Differential Diagnosis of Craniofacial Pain
 1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
1. Differential Diagnosis of Craniofacial Pain 2. Headache Page - 1 3. International Headache Society International Classification... 4. The Primary Headaches (1-4) Page - 2 5. The Secondary Headaches
The Use of the Lokomat System in Clinical Research
 International Neurorehabilitation Symposium February 12, 2009 The Use of the Lokomat System in Clinical Research Keith Tansey, MD, PhD Director, Spinal Cord Injury Research Crawford Research Institute,
International Neurorehabilitation Symposium February 12, 2009 The Use of the Lokomat System in Clinical Research Keith Tansey, MD, PhD Director, Spinal Cord Injury Research Crawford Research Institute,
Sinus Headache vs. Migraine
 Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Sinus Headache vs. Migraine John M. DelGaudio, MD, FACS Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology Emory University School of Medicine 1 Sinus Headache Problems
Oral Motor Exercises for the Treatment of Motor Speech Disorders: Efficacy and Evidence Based Practice Issues
 Oral Motor Exercises for the Treatment of Motor Speech Disorders: Efficacy and Evidence Based Practice Issues A literature review based on a tutorial by Heather M. Clark (2003) Presented by Leslie Kubacki
Oral Motor Exercises for the Treatment of Motor Speech Disorders: Efficacy and Evidence Based Practice Issues A literature review based on a tutorial by Heather M. Clark (2003) Presented by Leslie Kubacki

![Bell s Palsy ]]> <![CDATA[Bell's Palsy]]> Bell s Palsy ]]> <![CDATA[Bell's Palsy]]>](/thumbs/27/10105461.jpg)